Evicore Pediatric Musculoskeletal Imaging Guidelines
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Occult Fracture of the Femoral Neck Associated with Extensive
CASE REPORT – OPEN ACCESS International Journal of Surgery Case Reports 14 (2015) 136–140 Contents lists available at ScienceDirect International Journal of Surgery Case Reports j ournal homepage: www.casereports.com Occult fracture of the femoral neck associated with extensive osteonecrosis of the femoral head: A case report ∗ Kiyokazu Fukui , Ayumi Kaneuji, Tadami Matsumoto Department of Orthopaedic Surgery, Kanazawa Medical University, Kahoku-gun, Japan a r a t i b s c t l e i n f o r a c t Article history: INTRODUCTION: Although the subchondral portion of the femoral head is a common site for collapse in Received 4 April 2015 osteonecrosis of the femoral head (ONFH), femoral-neck fracture rarely occurs during the course of ONFH. Received in revised form 24 July 2015 We report a case of occult insufficiency fracture of the femoral neck without conditions predisposing to Accepted 26 July 2015 insufficiency fractures, occurring in association with ONFH. Available online 31 July 2015 PRESENTATION OF CASE: We report a case of occult fracture of the femoral neck due to extensive ONFH in a 60-year-old man. No abnormal findings suggestive of ONFH were identified on radiographs, and Keywords: the fracture occurred spontaneously without any trauma or unusual increase in activity. The patient’s Occult fracture medical history, age, and good bone quality suggested ONFH as a possible underlying cause. Contrast- Femoral neck enhanced magnetic resonance imaging was useful in determining whether the fracture was caused by Osteonecrosis of the femoral head ONFH or was instead a simple insufficiency fracture caused by steroid use. -

Isolated Trapezoid Fractures a Case Report with Compilation of the Literature
Bulletin of the NYU Hospital for Joint Diseases 2008;66(1):57-60 57 Isolated Trapezoid Fractures A Case Report with Compilation of the Literature Konrad I. Gruson, M.D., Kevin M. Kaplan, M.D., and Nader Paksima, D.O., M.P.H. Abstract as an axial load5,6 or bending stress7 transmitted indirectly Isolated fractures of the trapezoid bone have been rarely to the trapezoid through the second metacarpal. We present reported in the literature, the mechanism of injury being a case of an acute, isolated trapezoid fracture that resulted an axial or bending load transmitted through the second from direct trauma to the distal carpus and that was treated metacarpal. We report a case of an isolated, nondisplaced nonoperatively. Additionally, strategies for diagnosis and trapezoid fracture that was sustained by direct trauma treatment, as well as a synthesis of the published results and subsequently treated successfully in a short-arm cast. for both isolated and concomitant trapezoid fractures, are Diagnostic and treatment strategies for isolated fractures presented. of the trapezoid bone are reviewed as well as the results of operative and nonoperative treatment. Case Report A 25-year-old right-hand dominant male presented to the ractures of the carpus most commonly involve the emergency room (ER) complaining of isolated right-wrist scaphoid,1 with typical physical examination findings pain and swelling of 1 day’s duration. The patient stated Fof “snuffbox” tenderness. This presentation is fre- that a heavy metal door at work had closed onto the back quently the result of the patient falling onto an outstretched of his wrist causing an immediate onset of swelling and hand. -

Occult Fractures of the Proximal Femur
Deleanu et al. World Journal of Emergency Surgery (2015) 10:55 DOI 10.1186/s13017-015-0049-y WORLD JOURNAL OF EMERGENCY SURGERY RESEARCH ARTICLE Open Access Occult fractures of the proximal femur: imaging diagnosis and management of 82 cases in a regional trauma center Bogdan Deleanu1,2, Radu Prejbeanu1,2, Eleftherios Tsiridis6, Dinu Vermesan1,2, Dan Crisan1* , Horia Haragus1, Vlad Predescu4,5 and Florin Birsasteanu2,3 Abstract Background: Occult hip fractures are often difficult to identify in busy trauma units. We aimed to present our institutions experience in the diagnosis and treatment of occult fractures around the hip and to help define a clinical and radiological management algorithm. Method: We conducted a seven-year retrospective hospital medical record analysis. The electronic database was searched for ICD-10 CM codes S72.0 and S72.1 used for proximal femoral fractures upon patient discharge. We identified 34 (4.83 %) femoral neck fractures and 48 (4.42 %) trochanteric fractures labeled as occult. Results: The majority of the cases were diagnosed by primary MRI scan (57.4 %) and 12 were diagnosed by emergency CT scan (14.6 %). For the remaining cases the final diagnosis was confirmed by 72 h CT scan in 9 patients (representing 39 % of the false negative cases) or by MRI in the rest of 14 patients. MRI was best at detecting incomplete pertrochanteric fracture patterns (13.45 % of total) and incomplete fractures of the greater trochanter (3.65 % of total) respectively. It also detected the majority of Garden I femoral neck fractures (20.7 % of total). CT scanning accurately detected 100 % of Garden 2 fractures (2.44 %) and 25 % (3.65 %) of the complete pertrochanteric fractures (false negative 25 %). -

ACR Appropriateness Criteria® Acute Hand and Wrist Trauma
Revised 2018 American College of Radiology ACR Appropriateness Criteria® Acute Hand and Wrist Trauma Variant 1: Acute blunt or penetrating trauma to the hand or wrist. Initial imaging. Procedure Appropriateness Category Relative Radiation Level Radiography area of interest Usually Appropriate Varies CT area of interest with IV contrast Usually Not Appropriate Varies CT area of interest without and with IV Usually Not Appropriate Varies contrast CT area of interest without IV contrast Usually Not Appropriate Varies MRI area of interest without and with IV Usually Not Appropriate contrast O MRI area of interest without IV contrast Usually Not Appropriate O Bone scan area of interest Usually Not Appropriate ☢☢☢ US area of interest Usually Not Appropriate O Variant 2: Suspect acute hand or wrist trauma. Initial radiographs negative or equivocal. Next imaging study. Procedure Appropriateness Category Relative Radiation Level MRI area of interest without IV contrast Usually Appropriate O Radiography area of interest repeat in 10-14 Usually Appropriate Varies days CT area of interest without IV contrast Usually Appropriate Varies CT area of interest with IV contrast Usually Not Appropriate Varies CT area of interest without and with IV Usually Not Appropriate Varies contrast MRI area of interest without and with IV Usually Not Appropriate contrast O Bone scan area of interest Usually Not Appropriate ☢☢☢ US area of interest Usually Not Appropriate O ACR Appropriateness Criteria® 1 Acute Hand and Wrist Trauma Variant 3: Acute wrist fracture on -

ACR Appropriateness Criteria Acute Hip Pain-Suspected Fracture
Revised 2018 American College of Radiology ACR Appropriateness Criteria® Acute Hip Pain-Suspected Fracture Variant 1: Acute hip pain. Fall or minor trauma. Suspect fracture. Initial imaging. Procedure Appropriateness Category Relative Radiation Level Radiography hip Usually Appropriate ☢☢☢ Radiography pelvis Usually Appropriate ☢☢ Radiography pelvis and hips Usually Appropriate ☢☢☢ CT pelvis and hips with IV contrast Usually Not Appropriate ☢☢☢ CT pelvis and hips without and with IV Usually Not Appropriate contrast ☢☢☢☢ CT pelvis and hips without IV contrast Usually Not Appropriate ☢☢☢ MRI pelvis and affected hip without and Usually Not Appropriate with IV contrast O MRI pelvis and affected hip without IV Usually Not Appropriate contrast O Bone scan hips Usually Not Appropriate ☢☢☢ US hip Usually Not Appropriate O Variant 2: Acute hip pain. Fall or minor trauma. Negative radiographs. Suspect fracture. Next imaging study. Procedure Appropriateness Category Relative Radiation Level MRI pelvis and affected hip without IV Usually Appropriate contrast O CT pelvis and hips without IV contrast Usually Appropriate ☢☢☢ CT pelvis and hips with IV contrast Usually Not Appropriate ☢☢☢ CT pelvis and hips without and with IV Usually Not Appropriate contrast ☢☢☢☢ MRI pelvis and affected hip without and with Usually Not Appropriate IV contrast O Bone scan hips Usually Not Appropriate ☢☢☢ US hip Usually Not Appropriate O ACR Appropriateness Criteria® 1 Acute Hip Pain-Suspected Fracture Acute Hip Pain-Suspected Fracture Expert Panel on Musculoskeletal Imaging: Andrew B. Ross, MD, MPHa; Kenneth S. Lee, MD, MBAb; Eric Y. Chang, MDc; Behrang Amini, MD, PhDd; Jennifer K. Bussell, MDe; Tetyana Gorbachova, MDf; Alice S. Ha, MDg; Bharti Khurana, MDh; Alan Klitzke, MDi; Pekka A. -
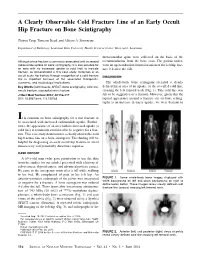
A Clearly Observable Cold Fracture Line of an Early Occult Hip Fracture on Bone Scintigraphy
A Clearly Observable Cold Fracture Line of an Early Occult Hip Fracture on Bone Scintigraphy Zhiyun Yang, Tameron Reed, and Alberto A. Simoncini Department of Radiology, Louisiana State University Health Sciences Center, Shreveport, Louisiana thoracolumbar spine were collected on the basis of the Although a true fracture is commonly associated with increased recommendation from the bone scan. The patient under- radionuclide uptake on bone scintigraphy, it is also possible for went an open-reduction internal fixation of the left hip frac- an area with no increased uptake (a cold line) to indicate ture 9 d after the fall. fracture, as demonstrated in this case study. Detection of an occult acute hip fracture through recognition of a cold fracture DISCUSSION line is important because of the associated therapeutic, economic, and medicolegal implications. The whole-body bone scintigram revealed a clearly Key Words: joint/muscle; SPECT; bone scintigraphy; cold line; defined linear area of no uptake, or the so-called cold line, occult fracture; subcapital neck fracture crossing the left femoral neck (Fig. 1). This cold line was J Nucl Med Technol 2014; 42:116–117 felt to be suggestive of a fracture. However, given that the DOI: 10.2967/jnmt.113.130765 typical appearance around a fracture site on bone scintig- raphy is an increase in tracer uptake, we were hesitant to It is common on bone scintigraphy for a true fracture to be associated with increased radionuclide uptake. Further- more, the appearance of an area with no increased uptake (a cold line) is commonly considered to be negative for a frac- ture. -

Imaging Choices in Occult Hip Fracture
Introduction Imaging Choices in High dependence on the integrity of this structure for people to function in their Occult Hip Fracture daily lives A delay of just 2 days in surgical treatment for an acute hip fracture Jesse Cannon, MD; Salvatore Silvestri, MD; Mark Munro, MD J Emerg Med. 2009;32(3):144-152 doubles mortality Reporter PGY 宋兆家 Unrecognized non-displaced fracture Supervisor VS 侯勝文 may displace, requiring surgery of much 990220 higher risk Introduction Plain Radiography Suspicion of hip fracture despite Occult fracture as the proximal femur negative X-ray studies Æ additional High percentage of trabecular bone imaging to detect or exclude pathology. Difficult to detect than in cortical bone Computed tomography (CT), bone scanning, and magnetic resonance imaging (MRI). Plain Radiography Overall, 4.4% (95% confidence interval 3.0-6.5%) of patients with negative X-ray studies had an occult fracture, or 3.1% of all ED patients having hip X-ray studies occult intertrochanteric fracture 2 days after missed occult fracture 1 Sensitivity of Radiographs Sensitivity of Radiographs Standard radiographic hip imaging Several factors could lead to the lower sensitivity in the ED (90.1%) relative to Sensitivity of these projections for hip other settings (average = 95.5%) fracture between 90% and 98% Emergently obtained Æ improper Dominguez et al. noted a sensitivity of technique 90.1% of plain radiographs for hip Re-imaged after coming to the specialists fracture in the ED More views may have increased overall sensitivity -

Acs Tqip Best Practices Guidelines in Imaging
ACS TQIP BEST PRACTICES GUIDELINES IN IMAGING AS ER 1988 THE AMERICAN SOCIETY OF Released October 2018 Table of Contents Introduction ............................................................................................... 3 1. Overview ................................................................................................ 4 Part 1: General Issues ........................................................................... 4 Part 2: Contrast Considerations .............................................................. 8 Part 3: Sedation .................................................................................10 2. Brain Imaging .........................................................................................15 3. Cervical Spine Imaging .............................................................................21 4. Imaging for Blunt Cerebrovascular Injury .....................................................32 5. Chest Imaging ........................................................................................36 6. Abdominal Imaging ................................................................................ 40 7. Genitourinary Imaging .............................................................................45 8. Thoracic and Lumbar Spine Imaging .......................................................... 48 9. Whole-Body CT Imaging ...........................................................................51 10. Imaging in Orthopaedic Trauma ...............................................................56 -

Femoral Neck Fractures
Femoral Neck Fractures Carol Lin, MD & Brad Merk, MD Original Authors: Brian Boyer, MD; March 2004 Steven A. Olson, MD; March 2006 James C. Krieg, MD; May 2011 Revised: March 2016 Epidemiology • > 300,000 Hip fractures annually in the US – Accounts for 30% of all hospitalizations – Expected to surpass 6 million annually worldwide by 2050 • Significant morbidity, mortality, expense – $10-15 billion/year in the US www.ahrq.gov/data/hcup; Kannus et al, Bone 1996; Dy et al, JBJS 2011 Epidemiology: Bimodal Distribution • Elderly – incidence doubles each decade beyond age 50 – higher in caucasians – smokers, lower BMI, excessive caffeine & ETOH • Young – high energy trauma Anatomy • Physeal closure age 16 • Neck-shaft angle 130° ± 7° • Anteversion 10° ± 7° • Calcar Femorale Posteromedial calcar dense plate of bone Images from: Court-Brown, C. et al. Rockwood & Greens Fractures in Adults. Philadelphia: Lippincott Williams & Wilkins, 2014 Blood Supply • Lateral epiphysel artery – terminal branch MFC artery – predominant blood supply to weight bearing dome of head • After fracture, blood supply depends on retinacular vessels Images from: Court-Brown, C. et al. Rockwood & Greens Fractures in Adults. Philadelphia: Lippincott Williams & Wilkins, 2014 Blood Supply • Greater fracture displacement = greater risk of retinacular vessel disruption • Tamponade effect of blood in intact capsule – Theoretical risk of AVN with increased pressure Diagnosis • Plain Film – Consider traction-internal rotation view if comminuted • CT scan – Displacement – comminution -

Clinical Appropriateness Guidelines: Advanced Imaging
Clinical Appropriateness Guidelines: Advanced Imaging Appropriate Use Criteria: Imaging of the Extremities Effective Date: September 5, 2017 Proprietary Date of Origin: 03/30/2005 Last revised: 07/26/2016 Last reviewed: 07/26/2016 8600 W Bryn Mawr Avenue South Tower - Suite 800 Chicago, IL 60631 P. 773.864.4600 Copyright © 2017. AIM Specialty Health. All Rights Reserved www.aimspecialtyhealth.com Table of Contents Description and Application of the Guidelines Description and Application of the Guidelines ........................................................................................................3 Administrative Guidelines Ordering of Multiple Studies ...................................................................................................................................4 Pre-test Requirements ...........................................................................................................................................5 Extremity Imaging CT of the Upper Extremity ......................................................................................................................................6 MRI of the Upper Extremity (Any Joint) ..................................................................................................................9 MRI of the Upper Extremity (Non-Joint) ...............................................................................................................15 CTA/MRA of the Upper Extremity .........................................................................................................................18 -

Acr–Spr–Ssr Practice Parameter for the Performance of Radiography of the Extremities
The American College of Radiology, with more than 30,000 members, is the principal organization of radiologists, radiation oncologists, and clinical medical physicists in the United States. The College is a nonprofit professional society whose primary purposes are to advance the science of radiology, improve radiologic services to the patient, study the socioeconomic aspects of the practice of radiology, and encourage continuing education for radiologists, radiation oncologists, medical physicists, and persons practicing in allied professional fields. The American College of Radiology will periodically define new practice parameters and technical standards for radiologic practice to help advance the science of radiology and to improve the quality of service to patients throughout the United States. Existing practice parameters and technical standards will be reviewed for revision or renewal, as appropriate, on their fifth anniversary or sooner, if indicated. Each practice parameter and technical standard, representing a policy statement by the College, has undergone a thorough consensus process in which it has been subjected to extensive review and approval. The practice parameters and technical standards recognize that the safe and effective use of diagnostic and therapeutic radiology requires specific training, skills, and techniques, as described in each document. Reproduction or modification of the published practice parameter and technical standard by those entities not providing these services is not authorized. Revised 2018 (Resolution 6)* ACR–SPR–SSR PRACTICE PARAMETER FOR THE PERFORMANCE OF RADIOGRAPHY OF THE EXTREMITIES PREAMBLE This document is an educational tool designed to assist practitioners in providing appropriate radiologic care for patients. Practice Parameters and Technical Standards are not inflexible rules or requirements of practice and are not intended, nor should they be used, to establish a legal standard of care1. -

ADVANCED IMAGING Appropriate Use Criteria: Imaging of the Extremities
CLINICAL APPROPRIATENESS GUIDELINES ADVANCED IMAGING Appropriate Use Criteria: Imaging of the Extremities EFFECTIVE MARCH 14, 2021 Proprietary Approval and implementation dates for specific health plans may vary. Please consult the applicable health plan for more details. AIM Specialty Health disclaims any responsibility for the completeness or accuracy of the information contained herein. 8600 West Bryn Mawr Avenue Appropriate.Safe.Affordable South Tower – Suite 800 Chicago, IL 60631 © 2017 ©©©© 2021 AIM Specialty Health www.aimspecialtyhealth.com RBM03-0321.1 Imaging of the Extremities Table of Contents Description and Application of the Guidelines .......................................................................................................... 4 General Clinical Guideline ........................................................................................................................................... 5 Clinical Appropriateness Framework .................................................................................................................... 5 Simultaneous Ordering of Multiple Diagnostic or Therapeutic Interventions .................................................... 5 Repeat Diagnostic Intervention .............................................................................................................................. 5 Repeat Therapeutic Intervention ............................................................................................................................ 6 Imaging of the Extremities