Solid Organ Transplantation Basic Immunology Basic Immunology
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

History of Lung Transplantation Akciğer Transplantasyonu Tarihçesi
REVIEW History of Lung Transplantation Akciğer Transplantasyonu Tarihçesi Gül Dabak Unit of Pulmonology, Kartal Kosuyolu Yüksek Ihtisas Teaching Hospital for Cardiovascular Diseases and Surgery, İstanbul ABSTRACT ÖZET History of lung transplantation in the world dates back to the early 20 Dünyada akciğer transplantasyonu tarihçesi, deneysel çalışmala- th century, continues to the first clinical transplantation performed rın yapılmaya başlandığı 20. yüzyılın ilk yıllarından itibaren Ja- by James Hardy in the United States of America in 1963 and comes mes Hardy’ nin Amerika Birleşik Devletleri’nde 1963’te yaptığı to the present with increased frequency. Over 40.000 heart-lung ilk klinik transplantasyona uzanır ve hızlanarak günümüze gelir. and lung transplantations were carried out in the world up to 2011 yılına kadar dünyada 40,000’in üzerinde kalp-akciğer ve 2011. The number of transplant centers and patients is flourishing akciğer transplantasyonu yapılmıştır. Transplantasyon alanındaki in accordance with the increasing demand and success rate in that artan ihtiyaca ve başarılara paralel olarak transplant merkezleri arena. Lung transplantations that started in Turkey at Sureyyapasa ve hasta sayıları da giderek artmaktadır. Türkiye’de 2009 yılında Teaching Hospital for Pulmonary Diseases and Thoracic Surgery Süreyyapaşa Göğüs Hastalıkları ve Cerrahisi Eğitim ve Araştırma in 2009 are being performed at two centers actively to date. This Hastanesi’ nde başlayan akciğer transplantasyonları günümüzde review covers a general outlook on lung transplantations both in iki merkezde aktif olarak yapılmaktadır. Bu derlemede, ülkemiz- the world and in Turkey with details of the first successful lung deki ilk başarılı akciğer transplantasyonu detaylandırılarak dün- transplantation in our country. yada ve ülkemizdeki akciğer transplantasyonu tarihçesi gözden Keywords: Lung transplantation, heart-lung transplantation, his- geçirilmektedir. -

Historical Perspectives of Lung Transplantation: Connecting the Dots
4531 Review Article Historical perspectives of lung transplantation: connecting the dots Tanmay S. Panchabhai1, Udit Chaddha2, Kenneth R. McCurry3, Ross M. Bremner1, Atul C. Mehta4 1Norton Thoracic Institute, St. Joseph’s Hospital and Medical Center, Phoenix, AZ, USA; 2Department of Pulmonary and Critical Care Medicine, Keck School of Medicine of University of Southern California, Los Angeles, CA, USA; 3Department of Cardiothoracic Surgery, Sydell and Arnold Miller Family Heart and Vascular Institute; 4Department of Pulmonary Medicine, Respiratory Institute, Cleveland Clinic, Cleveland, OH, USA Contributions: (I) Conception and design: TS Panchabhai, AC Mehta; (II) Administrative support: TS Panchabhai, RM Bremner, AC Mehta; (III) Provision of study materials or patients: TS Panchabhai, U Chaddha; (IV) Collection and assembly of data: TS Panchabhai, U Chaddha, AC Mehta; (V) Data analysis and interpretation: All authors; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Atul C. Mehta, MD, FCCP. Professor of Medicine, Cleveland Clinic Lerner College of Medicine, Cleveland, OH, USA; Staff Physician, Department of Pulmonary Medicine, Respiratory Institute, Cleveland Clinic, Cleveland, OH, USA. Email: [email protected]. Abstract: Lung transplantation is now a treatment option for many patients with end-stage lung disease. Now 55 years since the first human lung transplant, this is a good time to reflect upon the history of lung transplantation, to recognize major milestones in the field, and to learn from others’ unsuccessful transplant experiences. James Hardy was instrumental in developing experimental thoracic transplantation, performing the first human lung transplant in 1963. George Magovern and Adolph Yates carried out the second human lung transplant a few days later. -
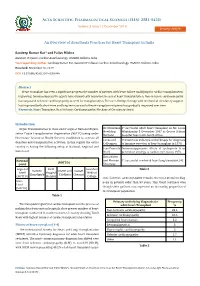
An Overview of Anesthesia Practices for Heart Transplant in India
Acta Scientific Pharmaceutical Sciences (ISSN: 2581-5423) Volume 3 Issue 12 December 2019 Review Article An Overview of Anesthesia Practices for Heart Transplant in India Sandeep Kumar Kar* and Pallav Mishra Assistant Professor, Cardiac Anesthesiology, IPGMER, Kolkata, India *Corresponding Author: Sandeep Kumar Kar, Assistant Professor, Cardiac Anesthesiology, IPGMER, Kolkata, India. Received: November 20, 2019 DOI: 10.31080/ASPS.2019.03.0449 Abstract is growing. Immunosuppressive agents have dramatically improved success of heart transplantation. Non-ischemic cardiomyopathy Heart transplant has seen a significant progress the number of patients with heart failure qualifying for cardiac transplantation has surpassed ischemic cardiomyopathy as need for transplantation. The use of bridge therapy with mechanical circulatory support has improved both short-term and long-term survival of heart transplant recipients has gradually improved over time Keywords: Heart Transplant; Non-Ischemic Cardiomyopathy; Mechanical Circulatory Assist Introduction st Organ Transplantation in India under aegis of National Organi- Dr. Christiaan 1 successful adult heart transplant on Mr. Louis Neethling Washkansky 3 December 1967 at Groote Schuur zation Tissue Transplantation Organization (NOTTO) setup under Barnard hospital Cape town, South Africa Directorate General of Health Services established to oversee all Caves and Transvenous endomyocardial biopsy for diagnosis donation and transplantation activities. In this regard, the entire Colleagues of immune rejection of heart transplant in 1970. country is having the following setup at National, Regional and Jean Francois Immunosuppressive effects of cyclosporin A as State Level. Borel preventive strategy to cardiac rejection in 1976. Bruce Reitz National and Norman 1st successful combined heart lung transplant [4]. (NOTTO) Level Shumway Regional KEM Guwahati Table 2 PGIMER IPGME and RGGGH Level Hospital Medical Chandigarh R Kolkata Chennai (ROTTO) Mumbai College ents. -

Lung Transplant Consideration: Anesthesiologist Perspective
ISSN: 2693-4965 DOI: 10.33552/OJCR.2020.04.000594 Online Journal of Cardiology Research & Reports Review Article Copyright © All rights are reserved by Sandeep Kumar Kar Lung Transplant Consideration: Anesthesiologist Perspective Sandeep Kumar Kar1* and Pallav Mishra2 Department of Cardiac Anesthesiology, Institute of Post Graduate Medical Education and Research, India *Corresponding author: Sandeep Kumar Kar, Department of Cardiac Received Date: August 07, 2020 Anesthesiology, Institute of Post Graduate Medical Education and Research, Kolkata, India. Published Date: October 21, 2020 Abstract Lung transplant has seen a significant progress since 1963 till this era. Worldwide lung transplant indications have broadened with time. Alpha 1 antitrypsin deficiency used to be the most common reason for transplant but now conditions like idiopathic pulmonary fibrosis, Cystic fibrosis, Non Cystic fibrosis bronchiectasis, lymphangioleiomyomatosis have become leading indications towards lung transplant. Relaxation of donor selection criteria management protocol preserving and optimizing lung function with development ex vivo perfusion techniques to recondition suboptimal lung has improved lung transplantation success. Post-transplant survival still poses challenge as median survival stands low around five years. Keywords: Lung transplant; Donor criteria; Ex vivo; Post-transplant Introduction country is having the following setup at National, Regional and Organ Transplantation in India under aegis of National State Level (Table 1 & 2). Lung transplant be considered for adults Organization Tissue Transplantation Organization (NOTTO) setup with chronic end stage lung disease meeting all of the following under Directorate General of Health Services established to oversee general criteria [5]. all donation and transplantation activities. In this regard, the entire Table 1: History of lung transplant. -

Thoracic and Cardiovascular Surgery
GREAT INSTITUTIONS One Hundred Years of History at Stanford University: Thoracic and Cardiovascular Surgery Y. Joseph Woo, MD, and Bruce A. Reitz, MD The history of thoracic and cardiovascular surgery at Stanford spans a century long period, beginning not long after the founding of Stanford University. Pioneering Stanford surgeons have made landmark discoveries and innovations in pulmonary, transplantation, thoracic aortic, mechanical circulatory support, minimally invasive, valvular, and congenital heart surgery. Fundamental research formed the foundation underlying these and many other advances. Educating and training the subsequent leaders of cardio- thoracic surgery has throughout this century-long history constituted a mission of the highest merit. New Stanford Adult Hospital Semin Thoracic Surg 27:388–397 I 2015 Elsevier Inc. All rights reserved. Central Message Keywords: History, Cardiovascular Surgery, Thoracic Surgery, Transplantation, Aortic Dissection Stanford: Upon a foundation of rigorous scien- tific investigation and dedicated teaching, Stan- ford thoracic and cardiovascular surgeons PRE-STANFORD UNIVERSITY Stanford Faculty in pioneered discoveries and innovations in pul- Lineage tracing of the history of Stanford Cardiothoracic 1914 and led the monary, transplantation, aortic, minimally inva- Surgery could be extended back to 1857, even before the Stanford surgical sive, and congenital heart surgery. founding of Stanford University. Elias Samuel Cooper, a San service at the San Francisco surgeon, authored “Report of an Operation to Francisco General Hospital2 (Fig. 2). Although he practiced a Remove a Foreign Body from Beneath the Heart” published broad spectrum of surgery, much of his clinical and experimental by the San Francisco Medico Chirurgical Association. The work and scholarly publications were in the arena of chest following year in 1858, Cooper founded the first medical surgery. -

Lung Transplantation in the Third Millennium Third the in Lung Transplantation in the Third Millennium
AME Medical Book 1A025 1A025 Lung Transplantation in the Third Millennium Transplantation Lung in the Third Millennium Editors: Dirk Van Raemdonck Federico Venuta www.amegroups.com Editors: Federico Venuta Raemdonck Dirk Van Lung Transplantation in the Third Millennium Editors: Dirk Van Raemdonck Federico Venuta AME Publishing Company Room C 16F, Kings Wing Plaza 1, NO. 3 on Kwan Street, Shatin, NT, Hong Kong Information on this title: www.amegroups.com For more information, contact [email protected] Copyright © AME Publishing Company. All rights reserved. This publication is in copyright. Subject to statutory exception and to the provisions of relevant collective licensing agreements, no reproduction of any part may take place without the written permission of AME Publishing Company. First published in 2018 Printed in China by AME Publishing Company Editors: Dirk Van Raemdonck, Federico Venuta Lung Transplantation in the Third Millennium (Hard Cover) ISBN: 978-988-77840-4-3 AME Publishing Company, Hong Kong AME Publishing Company has no responsibility for the persistence or accuracy of URLs for external or third-party internet websites referred to in this publication, and does not guarantee that any content on such websites is, or will remain, accurate or appropriate. The advice and opinions expressed in this book are solely those of the authors and do not necessarily represent the views or practices of the publisher. No representation is made by the publisher about the suitability of the information contained in this book, and there is no consent, endorsement or recommendation provided by the publisher, express or implied, with regard to its contents. I LUNG TRANSPLANTATION IN THE THIRD MILLENNIUM (FIRST EDITION) EDITORS Greg L. -

Norman Shumway
View metadata, citation and similar papers at core.ac.uk brought to you by CORE Baumgartner et al PRESIDENTIAL BIOGRAPHY Presidentialprovided by BiographyElsevier - Publisher Connector Norman E. Shumway, MD, PhD: Visionary, innovator, humorist William A. Baumgartner, MD,a Bruce A. Reitz, MD,b Vincent L. Gott, MD,a and Sara J. Shumway, MDc Born in Kalamazoo, Michigan, in 1923, Norman Edward sent back into the infantry. He then did three quarters of Shumway, Jr, and his parents (Laura Vandervliet Shumway premed at Baylor University in Waco, Texas. and Norman Edward Shumway, Sr) moved to Jackson, When it was time for Dr Shumway to matriculate to med- Michigan, when he was 1 year of age. His parents’ business ical school, all of the military slots were filled. He took an was operating ‘‘The Home Dairy,’’ which consisted of the interim job at Western State Mental Institution in Memphis, dairy in the back section and a diner up front. He went to Tennessee, where he was an orderly for 6 months. A slot be- the local grade school and was influenced early in a potential came open at Vanderbilt University in 1945, where he career in medicine when one of his classmates died of appen- started medical school. At Vanderbilt he was influenced dicitis. At Jackson High School, Dr Shumway was active on by 2 prominent surgeons of the time: Dr Barney Brooks, the debate team. His team was highly successful and won the Chief of Surgery, and Dr Cobb Pilcher, Chief of Neurosur- Michigan state championship in his senior year and then gery. -

Newsletteralumni News of the Newyork-Presbyterian Hospital/Columbia University Department of Surgery Volume 12 Number 1 Spring 2009
NEWSLETTERAlumni News of the NewYork-Presbyterian Hospital/Columbia University Department of Surgery Volume 12 Number 1 Spring 2009 Outliers All requires several iterative improvements and sometimes a leap of faith to cross a chasm of doubt and disappointment. This process is far more comfortable and promising if it is imbued with cross- discipline participation and basic science collaboration. Eric’s early incorporation of internist Ann Marie Schmidt’s basic science group within his Department continues to be a great example of the pro- ductivity that accrues from multidiscipline melding. Several speakers explored training in and acceptance of new techniques. The private practice community led the way in training and early adoption of laparoscopic cholecystectomy, which rapidly supplanted the open operation, despite an early unacceptable inci- dence of bile duct injuries. Mini-thoracotomies arose simultaneous- ly at multiple sites and are now well accepted as viable approaches to the coronaries and interior of the heart; whereas, more than a de- cade after their introduction, video assisted lobectomies for stage I, non-small-cell lung cancer account for <10% of US lobectomies. Os- tensibly, this reluctance reflects fear of uncontrollable bleeding and not doing an adequate cancer operation, neither of which has been a problem in the hands of VATS advocates. The May 8, 2009, 9th John Jones Surgical Day was a bit of an Lesions that are generally refractory to surgical treatment, outlier because the entire day was taken up by a single program, ex- such as glioblastomas and esophageal and pancreas cancers merit cept for a short business meeting and a lovely evening dinner party. -

Update on Lung Transplantation: Programmes, Patients and Prospects
Eur Respir Rev 2012; 21: 126, 271–305 DOI: 10.1183/09059180.00006312 CopyrightßERS 2012 EUROPEAN RESPIRATORY UPDATE Update on lung transplantation: programmes, patients and prospects Tom Kotsimbos*,#, Trevor J. Williams*,# and Gary P. Anderson" The will is infinite and the execution confined…the desire is (BLTx) from 1985 [3], this decade saw the true genesis of boundless and the act a slave to limit clinical lung transplant programmes. Shakespere W. Troilus and Cressida. Act III, Scene ii. HLTx became the early option for lung replacement with Stanford University (Stanford, CA, USA) leading the way Discovery consists of seeing what everyone has seen and thinking under the leadership of Bruce Reitz. A second key US centre in what nobody has thought Pittsburgh was also active. Europe, under the leadership of Anonymous Magdi Yacoub at Harefield Hospital (London, UK) and John Wallwork at Papworth Hospital (Cambridge, UK), developed t has been over 30 yrs since the modern era of lung very active HLTx programmes utilising donors from through- transplantation commenced and what was then the ‘‘new out the UK and the continent. Isolated lung transplantation I frontier and exceptional’’ has now become ‘‘routine and (SLT and BLTx) grew initially out of the Toronto programme expected’’. Strong vision, bold action and creative thinking and with the move of Cooper and Patterson to St Louis (Barnes have led to outstanding progress in the management of end- Hospital, Washington University, St Louis, MO, USA) by the stage lung and pulmonary vascular disease. The purpose of end of the 1980’s these were the dominant programmes. -

974-0947 1 United States of America Department
1 1 UNITED STATES OF AMERICA DEPARTMENT OF HEALTH AND HUMAN SERVICES FOOD AND DRUG ADMINISTRATION + + + CENTER FOR DEVICES AND RADIOLOGICAL HEALTH MEDICAL DEVICES ADVISORY COMMITTEE + + + GASTROENTEROLOGY AND UROLOGY DEVICES PANEL + + + May 17, 2017 8:00 a.m. Hilton Washington DC North 620 Perry Parkway Gaithersburg, Maryland PANEL MEMBERS: STEVEN SCHWAITZBERG, M.D. Panel Chair ABDELMONEM AFIFI, Ph.D. Voting Member DAVID YUH, M.D. Temporary Voting Member MICHAEL O'CONNOR, M.D. Temporary Voting Member ALFRED STAMMERS, M.S.A., CPBMT, CCP Temporary Voting Member JEFFREY B. RILEY, M.H.P.E., CCT Temporary Voting Member STEVEN NATHAN, M.D. Temporary Voting Member DAN MEYER, M.D. Temporary Voting Member JASON CONNOR, Ph.D. Temporary Voting Member ROGER YUSEN, M.D. Temporary Voting Member ALEXANDER KRUPNICK, M.D. Temporary Voting Member VICTOR VAN BERKEL, M.D., Ph.D. Temporary Voting Member JOHN HAMMON, JR., M.D. Temporary Voting Member MARC MOON, M.D. Temporary Voting Member TERESA BARNES Patient Representative NAFTALI FRANKEL, M.S. Consumer Representative NAVEEN THURAMALLA, M.S. Industry Representative ADEN ASEFA, M.P.H. Designated Federal Officer This transcript has not been edited or corrected, but appears as received from the commercial transcribing service. Accordingly, the Food and Drug Administration makes no representation as to its accuracy. Free State Reporting, Inc. 1378 Cape St. Claire Road Annapolis, MD 21409 (410) 974-0947 2 2 FDA REPRESENTATIVES: BENJAMIN FISHER, Ph.D. Director, Division of Reproductive, Gastro-Renal, and Urological Devices Office of Device Evaluation GEMA GONZALEZ, Ph.D. Renal Devices Branch Division of Reproductive, Gastro-Renal, and Urological Devices Office of Device Evaluation THERESA EISENMAN Press Contact FDA PRESENTERS: OWEN FARIS, Ph.D. -

Introduction
Notes Introduction 1. Telephone interview with Danelle DiCiantis, conducted by Annie Evans, November 19, 2000; Laura Rothenberg, “My So-Called Lungs,” in Sayantani DasGupta and Marsha Hurst (eds.), Stories of Illness and Healing; Women Write Their Bodies (Kent, OH: Kent State University Press, 2007), 44. The number of lung trans- plants in 1990 cited in “Report of the ATS Workshop on Lung Transplantation,” American Review of Respiratory Disease 147 (1993): 772–776; 2010 waiting list data cited in “Waiting List Additions 2000-2010 U.S.,” OPTN/UNOS 2011 Data Spring Regional Meetings, http://www.unos.org/docs/DataSlides_Spring_2011.pdf, accessed June 8, 2011. 2. For a critique of the assumptions and practices of modern medicine, see John D. Engel et al., Narrative in Health Care; Healing Patients, Practitioners, Profession, and Community (Oxford and New York: Radcliffe Publishing, 2008), 25–31; and Arthur W. Frank, The Wounded Storyteller: Body, Illness, and Ethics (University of Chicago Press, 1995), 54–56, 81–85, and 172. 3. These cost estimates were for first-year billed charges for a transplant; costs for immunosuppression drugs and other treatment continued well beyond the first year. Millman Research Report, “2008 U.S. Organ and Tissue Transplant Cost Estimates and Discussion,” http://publications.milliman.com/research/health-rr/pdfs/2008 -us-organ-tisse-RR4-1-08.pdf, accessed June 8, 2011. 4. Rhonda Bodfield, “Appeal for Transplant Patient,” Arizona Daily Star , December 17, 2010; Jane E. Allen, “Arizona Budget Cuts Put Some Organ Transplants Out of Reach,” ABC News/Health, November 18, 2010, http://abcnews.go.com/Health/Health_Care /medicaid-cuts-make-organ-transplants-unaffordable/story?id=12177059, accessed June 8, 2011. -

Preliminary Program
INTERNATIONAL SOCIETY FOR HEART AND LUNG TRANSPLANTATION Twenty-Second Annual Meeting and Scientific Sessions Final Program April 10-13, 2002 Convening at the Hilton Washington and Towers, Washington, DC PRESIDENT James B. Young, MD, Cleveland, OH PRESIDENT-ELECT Stephan Schueler, MD, Newcastle Upon Tyne, United Kingdom PAST PRESIDENT Anne Keogh, MBBS, MD, Sydney, Australia SECRETARY/TREASURER Alec Patterson, MD, St. Louis, MO DIRECTORS Robert C. Bourge, MD, Birmingham, AL Paul A. Corris, MB, FRCP, Newcastle Upon Tyne, United Kingdom F. Jay Fricker, MD, Gainesville, FL Axel Haverich, MD, Hannover, Germany Luigi Martinelli, MD, Genova, Italy Mehmet C. Oz, MD, New York, NY Sabina M. De Geest, RN, PhD, Basel, Switzerland W. Steves Ring, MD, Dallas, TX Robert C. Robbins, MD, Stanford, CA David O. Taylor, MD, Cleveland, OH Adriana Zeevi, PhD, Pittsburgh, PA JHLT EDITOR James K. Kirklin, MD, Birmingham, AL HEART AND LUNG TRANSPLANT REGISTRY MEDICAL DIRECTOR Marshall I. Hertz, MD, Minneapolis, MN MECHANICAL CIRCULATORY SUPPORT DEVICE DATABASE MEDICAL DIRECTOR Mario Deng, MD, New York, NY STAFF Amanda W. Rowe, Executive Director Phyllis Glenn, Director of Membership Services Lisa Edwards, Director of Meetings LeeAnn Mills, Director of Operations 14673 Midway Road, Suite 200 Addison, TX 75001 Phone: 972-490-9495 Fax: 972-490-9499 www.ishlt.org [email protected] INTERNATIONAL SOCIETY FOR HEART AND LUNG TRANSPLANTATION PAST PRESIDENTS 1981-1982 Michael Hess, MD 1982-1984 Jack Copeland, MD 1984-1986 Terence English, FRCS 1986-1988 Stuart Jamieson, MD 1988-1990 Bruno Reichart, MD 1990-1991 Margaret Billingham, MD 1991-1992 Christian Cabrol, MD 1992-1993 John O’Connell, MD 1993-1994 Eric Rose, MD 1994-1995 John Wallwork, FRCS 1995-1996 Sharon Hunt, MD 1996-1997 William Baumgartner, MD 1997-1998 Leslie Miller, MD 1998-1999 Alan Menkis, MD, FRCS(C) 1999-2000 Robert L.