MRI of the Small Joints and Extremities/ Illustrative Cases
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
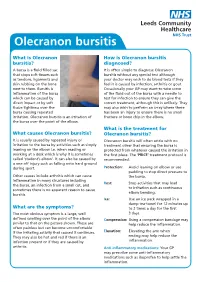
Olecranon Bursitis
Olecranon bursitis What is Olecranon How is Olecranon bursitis bursitis? diagnosed? A bursa is a fluid filled sac It is often simple to diagnose Olecranon that stops soft tissues such bursitis without any special test although as tendons, ligaments and your doctor may wish to do blood tests if they skin rubbing on the bone feel it is caused by infection, arthritis or gout. next to them. Bursitis is Occasionally your GP may want to take some inflammation of the bursa of the fluid out of the bursa with a needle to which can be caused by test for infection to ensure they can give the direct impact or by soft correct treatment, although this is unlikely. They tissue tightness over the may also wish to perform an x-ray where there bursa causing repeated has been an injury to ensure there is no small irritation. Olecranon bursitis is an irritation of fracture or bone chip in the elbow. the bursa over the point of the elbow. What is the treatment for What causes Olecranon bursitis? Olecranon bursitis? It is usually caused by repeated injury or Olecranon bursitis will often settle with no irritation to the bursa by activities such as simply treatment other that ensuring the bursa is leaning on the elbow i.e. when reading or protected from whatever caused the irritation in working at a desk which is why it is sometimes the first place. The ‘PRICE’ treatment protocol is called ‘student’s elbow’. It can also be caused by recommended: a one off injury such as falling onto hard ground during sport. -

OES Site Color Scheme 1
Nuisance Problems You will Grow to Love Thomas V Gocke, MS, ATC, PA-C, DFAAPA President & Founder Orthopaedic Educational Services, Inc. Boone, NC [email protected] www.orthoedu.com Orthopaedic Educational Services, Inc. © 2016 Orthopaedic Educational Services, Inc. all rights reserved. Faculty Disclosures • Orthopaedic Educational Services, Inc. Financial Intellectual Property No off label product discussions American Academy of Physician Assistants Financial PA Course Director, PA’s Guide to the MSK Galaxy Urgent Care Association of America Financial Intellectual Property Faculty, MSK Workshops Ferring Pharmaceuticals Consultant Orthopaedic Educational Services, Inc. © 2016 Orthopaedic Educational Services, Inc. all rights reserved. 2 LEARNING GOALS At the end of this sessions you will be able to: • Recognize nuisance conditions in the Upper Extremity • Recognize nuisance conditions in the Lower Extremity • Recognize common Pediatric Musculoskeletal nuisance problems • Recognize Radiographic changes associates with common MSK nuisance problems • Initiate treatment plans for a variety of MSK nuisance conditions Orthopaedic Educational Services, Inc. © 2016 Orthopaedic Educational Services, Inc. all rights reserved. Inflammatory Response Orthopaedic Educational Services, Inc. © 2016 Orthopaedic Educational Services, Inc. all rights reserved. Inflammatory Response* When does the Inflammatory response occur: • occurs when injury/infection triggers a non-specific immune response • causes proliferation of leukocytes and increase in blood flow secondary to trauma • increased blood flow brings polymorph-nuclear leukocytes (which facilitate removal of the injured cells/tissues), macrophages, and plasma proteins to injured tissues *Knight KL, Pain and Pain relief during Cryotherapy: Cryotherapy: Theory, Technique and Physiology, 1st edition, Chattanooga Corporation, Chattanooga, TN 1985, p 127-137 Orthopaedic Educational Services, Inc. © 2016 Orthopaedic Educational Services, Inc. -

Bony Bankart Lesions and Shoulder Dislocations
Shoulder Dislocations and Bony Bankart Lesions The shoulder is the most mobile and the most commonly dislocated large joint in the body. Dislocation means that the joint is moved out of position, such that the joint surfaces at the ends of the bones are no longer in contact. In the shoulder, most dislocations are anterior (moving forward from the body); however, they can occur in several directions. When a dislocation occurs, the soft tissues that stabilize the shoulder can be torn, and the bone that forms the socket also can be broken at the same time. Traumatic dislocations of the shoulder can result in a Bankart lesion (tear). The head of the humerus (ball of upper arm bone) is stabilized against the glenoid (socket of the shoulder joint) using a combination of muscles, labrum, and ligaments. Ligaments run from the glenoid to the humeral head, and they blend with fibrous tissue called the capsule that encloses the entire joint. When the humeral head is forced forward in a dislocation, the soft tissues stretch or tear, and in some cases, bone is fractured off the glenoid rim, resulting in a bony Bankart lesion. X-ray of a patient with a bony Bankart facture of 3-D scan of the same patient more clearly the glenoid (socket), secondary to shoulder recreating the fracture. dislocation. Orthopaedic Surgery & Sports Medicine 630-324-0402 ⚫ [email protected] Teaching & Research Foundation stevenchudikmd.com otrfund.org Schedule online now © 2018 Steven Chudik MD Shoulder, Knee & Sports Medicine. All rights reserved. Frequent Signs and -

Sports Medicine Examination Outline
Sports Medicine Examination Content I. ROLE OF THE TEAM PHYSICIAN 1% A. Ethics B. Medical-Legal 1. Physician responsibility 2. Physician liability 3. Preparticipation clearance 4. Return to play 5. Waiver of liability C. Administrative Responsibilities II. BASIC SCIENCE OF SPORTS 16% A. Exercise Physiology 1. Training Response/Physical Conditioning a.Aerobic b. Anaerobic c. Resistance d. Flexibility 2. Environmental a. Heat b.Cold c. Altitude d.Recreational diving (scuba) 3. Muscle a. Contraction b. Lactate kinetics c. Delayed onset muscle soreness d. Fiber types 4. Neuroendocrine 5. Respiratory 6. Circulatory 7. Special populations a. Children b. Elderly c. Athletes with chronic disease d. Disabled athletes B. Anatomy 1. Head/Neck a.Bone b. Soft tissue c. Innervation d. Vascular 2. Chest/Abdomen a.Bone b. Soft tissue c. Innervation d. Vascular 3. Back a.Bone b. Soft tissue c. Innervation 1 d. Vascular 4. Shoulder/Upper arm a. Bone b. Soft tissue c. Innervation d. Vascular 5. Elbow/Forearm a. Bone b. Soft tissue c. Innervation d. Vascular 6. Hand/Wrist a. Bone b. Soft tissue c. Innervation d. Vascular 7. Hip/Pelvis/Thigh a. Bone b. Soft tissue c. Innervation d. Vascular 8. Knee a. Bone b. Soft tissue c. Innervation d. Vascular 9. Lower Leg/Foot/Ankle a. Bone b. Soft tissue c. Innervation d. Vascular 10. Immature Skeleton a. Physes b. Apophyses C. Biomechanics 1. Throwing/Overhead activities 2. Swimming 3. Gait/Running 4. Cycling 5. Jumping activities 6. Joint kinematics D. Pharmacology 1. Therapeutic Drugs a. Analgesics b. Antibiotics c. Antidiabetic agents d. Antihypertensives e. -

34Th Annual Meeting of the Japan Shoulder Society
34TH ANNUAL MEETING OF THE JAPAN SHOULDER SOCIETY 1 F Wave Monitoring After Arthroscopic Shoulder Surgery gers may be used to evaluate the functions of the shoulder joint. It is IWATA Yoshio, Department of Orthopaedics, Uji Takeda Hospital also believed that people can perform approximately half of the ac- MORIHARA Toru, HAYASHIDA Tatsurou, OGURA Akiko, KUBO tions even if the diseased hand is on their dominant side. Toshikazu, Department of Orthopaedics, Kyoto Prefectural Univer- sity of Medicine, Graduate School of Medical Science HORII Motoyuki, Department of Orthopaedic Surgery, Kyoto Inter- 3 The Shoulder Function of Congenital Clavicle Anomalies disciplinary Institute Hospital of Community Medicine KENMOKU Tomonori, Department of Orthopaedics Surgery, Chiba KUROKAWA Masao, Department of Orthopaedic Surgery, Saisei- Univercity Graduate School of Medicine kai Suita Hospital SAISU Takashi, KAMEGAYA Makoto, Division of Orthopaedics Sur- The purpose of this study was to evaluate the modulation of excit- gery, Chiba Children’s Hospital ability of spinal motor neuron function. We investigated F waves af- MIKASA Motohiko, Matsudo Orthopaedic Hospital ter arthroscopic shoulder surgery. We evaluated 7 subjects who There was no report on the shoulder function of congenital clav- underwent an arthroscopic shoulder surgery. There were 5 men icle anomalies. Our purpose was to clarify the role of the clavicle, and 2 women; the mean age at the time of surgery was 33.6 years investigating the shoulder function in patients with clavicle defect old. In our study, F waves were recorded from the abductor pollicis or pseudoarthrosis. muscle after transcutaneous median nerve stimulation at bilateral Thirteen shoulders of 9 patients with congenital clavicle anoma- wrists. -

Presentations
7/4/2019 30th Brucosport Football Medicine: What’s New 2017 Bruges, Belgium 11 March 2017 Aspetar Orthopaedic and Sports Medicine Hospital 1 Dr. Scott Gillogly Chief Medical Officer 26 February 2017 2 1 7/4/2019 Articular Cartilage Injuries in the Knee: Evaluation and Surgical Treatment Options based on Return to Play Scott D. Gillogly, MD 34th FIMS World Sports Medicine Congress Ljubljana, Slovenia 29 September - 2 October 2016 Aspetar Orthopaedic and Sports Medicine Hospital 3 ICRS Annual Meeting 29 September 2016 Aspetar Orthopaedics and Sorrento, Italy Sports Medicine Hospital 4 2 7/4/2019 Articular Cartilage Injuries in the Knee: Evaluation and Surgical Treatment Options based on Return to Play Scott D. Gillogly, MD AFC Team Physiotherapist Sports Medicine Course Doha, Qatar 13-15 June 2016 Aspetar Orthopaedic and Sports Medicine Hospital 5 Cartilage Defects in Athletes: Return To Play (RTP) Scott D. Gillogly, MD 1st GCC Sports Medicine Conference Doha, Qatar 23 April 2016 Aspetar Orthopaedic and Sports Medicine Hospital 6 3 7/4/2019 AAOS Articular Cartilage Restoration: The Modern Frontier 1 April 2016 Aspetar Orthopaedics and Sports Medicine Hospital Chicago, Illinois 7 AAOS Articular Cartilage Restoration: The Modern Frontier 2 April 2016 Aspetar Orthopaedics and Chicago, Illinois Sports Medicine Hospital 8 4 7/4/2019 8 April 2016 Aspetar Orthopaedics and Washington, D.C. Sports Medicine Hospital 9 8 April 2016 Aspetar Orthopaedics and Washington, D.C. Sports Medicine Hospital 10 5 7/4/2019 Return to Play (RTP) After Cartilage Repair of the Knee Scott D. Gillogly, MD Challenges in Football Injuries Doha, Qatar 11‐12 February, 2016 Aspetar Orthopaedic and Sports Medicine Hospital 11 Partial Osteochondral Fractures of the Condyles (Osteochondral Defects) Scott D. -

An Overview of Common Injuries and Imaging Findings
SPORTS RADIOLOGY SHOULDER DISLOCATION AMONG ATHLETES AN OVERVIEW OF COMMON INJURIES AND IMAGING FINDINGS – Written by Nima Hafezi–Nejad, Shadpour Demehri and John A Carrino, USA The Glenohumeral (GH) joint has a mobility is often termed hyperlaxity, a during sports activities. Second, SD may arise large range of motion that leaves it prone common feature among many athletes. as a result of chronic injuries, mostly in the to shoulder instability, ranging from Hyperlaxity may help athletes by enhancing form of recurrent microtrauma and overuse. subluxation to frank shoulder dislocation their range of motion. However, this may Secondary forms of impingement and (SD). Due to the shallow depth of the glenoid’s become a problem when it is accompanied injury to the dynamic soft tissue stabilisers osseous structure, shoulder stability is by a functional deficit and pathological may arise from recurrent microtrauma as achieved through a number of additional symptoms. Typical symptoms include well2. soft tissue stabilisers (including the glenoid pain and a subjective feeling of instability labrum). Rotator cuff muscles are the most or apprehension. While instability and ADVANCED IMAGING FINDINGS – AN important dynamic stabilisers of the GH hyperlaxity are two distinct phenomena, OVERVIEW joint. Other muscles that cross the GH joint, they frequently occur together in athletes Radiography remains the primary such as pectoralis major and latissimus dorsi, suffering from SD1. modality of choice when SD is suspected may potentially act as stabilisers as well. SD While purely atraumatic causes may (Figure 1). However, advanced imaging may arise from abnormal function of either account for a number of SDs among athletes, modalities including computed tomo- osseous (glenoid fossa and coracoacromial there are two main etiologies, behind athlete graphy (CT) and magnetic resonance arch) or soft tissue (glenoid labrum, articular SD. -

Download Versus Arthritis
Elbow pain Elbow pain information booklet Contents How does the elbow work? 4 What causes elbow pain and stiffness? 6 Should I see a healthcare professional? 8 What can I do to help myself? 9 How are elbow problems diagnosed? 12 What treatments are there for elbow pain? 14 Specific elbow conditions 18 Glossary 26 Research and new developments 27 Keeping active with elbow pain 28 Where can I find out more? 32 We’re the 10 million people living with arthritis. We’re the carers, researchers, health professionals, friends and parents all united in Talk to us 33 our ambition to ensure that one day, no one will have to live with the pain, fatigue and isolation that arthritis causes. We understand that every day is different. We know that what works for one person may not help someone else. Our information is a collaboration of experiences, research and facts. We aim to give you everything you need to know about your condition, the treatments available and the many options you can try, so you can make the best and most informed choices for your lifestyle. We’re always happy to hear from you whether it’s with feedback on our information, to share your story, or just to find out more about the work of Versus Arthritis. Contact us at [email protected] Words shown are explained in the glossary on p.26. Registered office: Versus Arthritis, Copeman House, St Mary’s Gate, Chesterfield S41 7TD in bold Registered Charity England and Wales No. 207711, Scotland No. SC041156. -

Malignant Olecranon Bursitis in the Setting of Multiple Myeloma Relapse
Case Report Malignant olecranon bursitis in the setting of multiple myeloma relapse Maxwell M Krem, MD, PhD,a Samer Z Al-Quran, MD,b Craig L Silverman, MD,c Vallejo Miller, RN,a and William Tse, MD, FACPa aDivision of Blood and Bone Marrow Transplantation, Department of Medicine, and Departments of bPathology and cRadiation Oncology, at the James Graham Brown Cancer Center, University of Louisville School of Medicine, Louisville, Kentucky ultiple myeloma is the most common Case presentation and summary plasma cell neoplasm, with an esti- A 46-year-old man with a longstanding history mated 24,000 cases occurring annu- of multiple myeloma developed swelling of the Mally. 1 Symptomatic multiple myeloma most com- left elbow that was initially painless in September monly presents with one or more of the cardinal 2016. He had been diagnosed with IgA kappa mul- CRAB phenomena of hypercalcemia, renal dys- tiple myeloma and AL deposition in 2011. Over the function, anemia, or lytic bone lesions.2 Less com- course of his disease, he was treated with the follow- monly, patients may present with plasmacytomas ing sequence of therapies: cyclophosphamide, bort- (focal lesions of malignant plasma cells), which may ezomib, and dexamethasone, followed by melphalan- involve bony or soft tissues.1 conditioned autologous peripheral blood stem cell Plasma cell neoplasms occasionally involve the joints, transplant; lenalidomide and dexamethasone; car lzo- including the elbows, typically as plasmacytomas. e mib and dexamethasone; pomalidomide, bortezomib, elbow is an unusual but reported location of plasma- and dexamethasone; and bortezomib, lenalidomide, cytomas.3,4 A case of multiple myeloma and amyloid dexamethasone, doxorubicin, cyclophosphamide, and light-chain (AL) amyloidosis has been reported, with etoposide, followed by second melphalan-conditioned manifestations including pseudomyopathy, bone mar- autologous peripheral blood stem cell transplant. -

Olecranon Bursitis As Initial Presentation of Gout in Asymptomatic Normouricemic Patients
CORE Metadata, citation and similar papers at core.ac.uk Provided by Elsevier - Publisher Connector The Egyptian Rheumatologist (2014) 36, 47–50 Egyptian Society for Joint Diseases and Arthritis The Egyptian Rheumatologist www.rheumatology.eg.net www.sciencedirect.com CASE REPORT Olecranon bursitis as initial presentation of gout in asymptomatic normouricemic patients Yasser Emad a,b,*, Yasser Ragab c,d, Nashwa El-Shaarawy e, J.J. Rasker f a Rheumatology and Rehabilitation Department, Faculty of Medicine, Cairo University, Cairo, Egypt b Rheumatology and Rehabilitation Department, Dr. Erfan and Bagedo General Hospital, Jeddah, Saudi Arabia c Radiology Department, Faculty of Medicine, Cairo University, Cairo, Egypt d Radiology Department, Dr. Erfan and Bagedo General Hospital, Jeddah, Saudi Arabia e Rheumatology and Rehabilitation Department, Suez Canal University, Ismailia, Egypt f Rheumatology Department, University of Twente, The Netherlands Received 25 August 2013; accepted 25 August 2013 Available online 4 October 2013 KEYWORDS Abstract Background: Acute bursitis is a less frequent presentation of gout, especially in Olecranon gouty bursitis; normouricemic subjects compared to the typical pattern of acute gouty arthritis. Olecranon bursitis; Aim of the work: The aim of the current case reports is to describe the clinical and the magnetic Gout; resonance imaging features of acute gouty olecranon bursitis as initial presentation of acute gouty MRI features attack. Case report: In this report we describe the clinical and MRI features of three cases presenting with acute gouty olecranon bursitis, in spite of normal serum uric acid and stable renal function. For all cases diagnostic aspiration was carried out to exclude septic bursitis as initial first step of management. -

ESR-Endorsed ESSR DIPLOMA CORRECT ANSWERS (In Bold)
ESR-endorsed ESSR DIPLOMA Examination Session at ESSR 2015 York, June 19, 2015 CORRECT ANSWERS (in bold) 1. In the Erdheim-Chester disease, which of the following statements is true: a) it is a frequent disease in Western Europe b) is a Langerhans cell histiocytosis c) bone involvement is almost universal d) it essentially affects the axial skeleton and only rarely the long bones 2. In the POEMS syndrome, which of the following statements is false: a) affected patients are older than patients with standard multiple myeloma b) sclerotic bone lesions are found in the majority of the patients c) sclerotic bone lesions can be mistaken for bone islands d) as a consequence of treatment response, sclerotic bone lesions may to decrease in size 3) Taking into account ankle sprains, the highest incidence of injury can be found in the: a) calcaneofibular ligament b) posterior talofibular ligament c) anterior talofibular ligament d) tibiocalcaneal ligament 4) HIV-positive patients have a higher incidence of: a) bacillary angiomatosis b) thoracic cage tuberculosis c) reiter’s syndrome d) all of the previous entities 5) On MRI, the structures of the rotator cuff interval can be best evaluated on: a) oblique sagittal and oblique coronal images b) axial and oblique coronal images. c) oblique sagittal and axial images d) ABER position. 6) Which structure does not belong to the rotator cuff interval? a) coraco-acromial ligament b) long head of the biceps tendon c) coracohumeral ligament d) superior glenohumeral ligament 7) Most people under the age of -

10 Soft Tissue Injections
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Repositório Institucional dos Hospitais da Universidade de... Best Practice & Research Clinical Rheumatology Vol. 19, No. 3, pp. 503–527, 2005 doi:10.1016/j.berh.2005.01.003 available online at http://www.sciencedirect.com 10 Soft tissue injections Luı´s P.B.S. Ineˆs MD Rheumatologist Jose´ Anto´nio P. da Silva* MD, PhD Consultant Rheumatologist and Professor of Rheumatology Hospitais da Universidade de Coimbra, 3000-075 Coimbra, Portugal Soft tissue rheumatism includes a wide spectrum of common lesions of the tendons, enthesis, tendon sheaths, bursae, ligaments and fasciae as well as nerve compression syndromes. Studies on the pathogenesis of these lesions do not support a major role for inflammation, thus questioning the rationale for glucocorticoid injections. This chapter reviews current indications for local glucocorticoid injections and available evidence on its efficacy, as well as contra- indications and potential risks. Randomised controlled studies of good methodological quality are rare and there is limited scientific evidence to support the superiority of glucocorticoid injections over alternative treatments. The basic principles of the glucocorticoid injection method are outlined, together with a description of the practical procedure for the more common conditions. Key words: soft tissue rheumatism; treatment; glucocorticoid injection. Periarticular soft tissue rheumatic disorders include a wide spectrum of localised lesions of the tendons, enthesis, tendon sheaths, bursae, ligaments and fasciae as well as nerve compression syndromes. They are extremely common in daily practice and result in significant morbidity and socioeconomic impact. These aspects, together with their tendency to chronicity and recurrence, make the treatment of these conditions an important health care issue.