New Aspects of Cutaneous Mosaicism
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The National Economic Burden of Rare Disease Study February 2021
Acknowledgements This study was sponsored by the EveryLife Foundation for Rare Diseases and made possible through the collaborative efforts of the national rare disease community and key stakeholders. The EveryLife Foundation thanks all those who shared their expertise and insights to provide invaluable input to the study including: the Lewin Group, the EveryLife Community Congress membership, the Technical Advisory Group for this study, leadership from the National Center for Advancing Translational Sciences (NCATS) at the National Institutes of Health (NIH), the Undiagnosed Diseases Network (UDN), the Little Hercules Foundation, the Rare Disease Legislative Advocates (RDLA) Advisory Committee, SmithSolve, and our study funders. Most especially, we thank the members of our rare disease patient and caregiver community who participated in this effort and have helped to transform their lived experience into quantifiable data. LEWIN GROUP PROJECT STAFF Grace Yang, MPA, MA, Vice President Inna Cintina, PhD, Senior Consultant Matt Zhou, BS, Research Consultant Daniel Emont, MPH, Research Consultant Janice Lin, BS, Consultant Samuel Kallman, BA, BS, Research Consultant EVERYLIFE FOUNDATION PROJECT STAFF Annie Kennedy, BS, Chief of Policy and Advocacy Julia Jenkins, BA, Executive Director Jamie Sullivan, MPH, Director of Policy TECHNICAL ADVISORY GROUP Annie Kennedy, BS, Chief of Policy & Advocacy, EveryLife Foundation for Rare Diseases Anne Pariser, MD, Director, Office of Rare Diseases Research, National Center for Advancing Translational Sciences (NCATS), National Institutes of Health Elisabeth M. Oehrlein, PhD, MS, Senior Director, Research and Programs, National Health Council Christina Hartman, Senior Director of Advocacy, The Assistance Fund Kathleen Stratton, National Academies of Science, Engineering and Medicine (NASEM) Steve Silvestri, Director, Government Affairs, Neurocrine Biosciences Inc. -

Neonatal Dermatology Review
NEONATAL Advanced Desert DERMATOLOGY Dermatology Jennifer Peterson Kevin Svancara Jonathan Bellew DISCLOSURES No relevant financial relationships to disclose Off-label use of acitretin in ichthyoses will be discussed PHYSIOLOGIC Vernix caseosa . Creamy biofilm . Present at birth . Opsonizing, antibacterial, antifungal, antiparasitic activity Cutis marmorata . Reticular, blanchable vascular mottling on extremities > trunk/face . Response to cold . Disappears on re-warming . Associations (if persistent) . Down syndrome . Trisomy 18 . Cornelia de Lange syndrome PHYSIOLOGIC Milia . Hard palate – Bohn’s nodules . Oral mucosa – Epstein pearls . Associations . Bazex-Dupre-Christol syndrome (XLD) . BCCs, follicular atrophoderma, hypohidrosis, hypotrichosis . Rombo syndrome . BCCs, vermiculate atrophoderma, trichoepitheliomas . Oro-facial-digital syndrome (type 1, XLD) . Basal cell nevus (Gorlin) syndrome . Brooke-Spiegler syndrome . Pachyonychia congenita type II (Jackson-Lawler) . Atrichia with papular lesions . Down syndrome . Secondary . Porphyria cutanea tarda . Epidermolysis bullosa TRANSIENT, NON-INFECTIOUS Transient neonatal pustular melanosis . Birth . Pustules hyperpigmented macules with collarette of scale . Resolve within 4 weeks . Neutrophils Erythema toxicum neonatorum . Full term . 24-48 hours . Erythematous macules, papules, pustules, wheals . Eosinophils Neonatal acne (neonatal cephalic pustulosis) . First 30 days . Malassezia globosa & sympoidalis overgrowth TRANSIENT, NON-INFECTIOUS Miliaria . First weeks . Eccrine -

42Th. Brazilian Congress of Oral Medicine and Oral Patology Manaus, Amazonas, Brazil
42TH. BRAZILIAN CONGRESS OF ORAL MEDICINE AND ORAL PATOLOGY MANAUS, AMAZONAS, BRAZIL. JULY 4-8, 2016 538 ABSTRACTS OP – ORAL PRESENTATION 043 CPP – CLINICAL POSTER PRESENTATION 344 RESEARCH POSTER 151 OP01 - BROWN TUMOR OF THE JAW MIMICKING MALIGNANT NEOPLASM. Paulo de Camargo MORAES. Rubens GONÇALVESTEIXEIRA. Luis Alexandre THOMAZ. Claudio Roberto Pacheco JODAS. Victor Angelo MONTALLI. Marcelo SPERANDIO. Amy Louise BROWN. Brown tumors are an unusual manifestation of primary hyperparathyroidism, a disease characterized by excessive secretion of parathyroid hormone (PTH). With the exception of bone loss, skeletal manifestations are rare, occurring in less than 2% of patients. The presence of multiple lesions may imitate a malignant neoplasm, hence posing a real diagnostic challenge. We describe a 50-year-old wheelchair-bound Brazilian woman, presenting multiple expansive lytic lesions. The clinical differential diagnosis included metastatic disease and multiple myeloma. Intra-oral examination revealed a large ulcerating proliferative brown mass on the left side of the mandible, with significant bone destruction. Serum calcium, alkaline phosphatase and PTH (was seven times above the upper limit of normal). A combination of physical examination, and radiological and histopathologyc investigations were performed. A parathyroid nodule was detected and surgically excised. Two months later the patient no longer wheelchair-bound. In addition, after 15 months of follow-up the brown tumour has significantly decreased. OP02 - LEISHMANIOSE IN ORAL CAVITY - A CASE CLINICAL REPORT. Carlos Deyver de Souza QUEIROZ. Helio Massaiochi TANIMOTO. Raphael HAIKEL JUNIOR. Edmundo Carvalho MAUAD. André Lopes CARVALHO. José Humberto FRAGNANI. Adhemar LONGATTO FILHO. Leishmaniasis is an infectious disease A, non-contagious, caused by different species of Leishmania protozoa, which can affect the skin and / or mucous membranes. -
Epidermal Nevus Syndrome): a Case Report Arun Joshi, MD,1 Sudha Agrawal, MD,1 Kuldeep Singh, MD,2 Shatrughan Prasad Sah, MD3 Arun Agarwalla, MD,1 Sanjay K
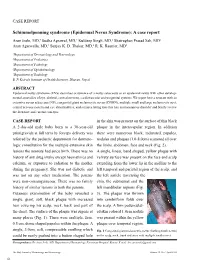
CASE REPORT Schimmelpenning syndrome (Epidermal Nevus Syndrome): A case report Arun Joshi, MD,1 Sudha Agrawal, MD,1 Kuldeep Singh, MD,2 Shatrughan Prasad Sah, MD3 Arun Agarwalla, MD,1 Sanjay K. D. Thakur, MD,4 R. K. Rauniar, MD5 1Department of Dermatology and Venereology 2Department of Pediatrics 3Department of Pathology 4Department of Ophthalmology 5Department of Radiology B. P. Koirala Institute of Health Sciences, Dharan, Nepal ABSTRACT Epidermal nevus syndrome (ENS) describes occurrence of a nevus sebaceous or an epidermal nevus with other develop- mental anomalies of eye, skeletal, central nervous, cardiovascular and urogenital systems. We report here a neonate with an extensive nevus sebaceous (NS), congenital giant melanocytic nevus (CGMN), multiple small and large melanocytic nevi, central nervous system and eye abnormalities, and seizures fitting into this rare neurocutaneus disorder and briefly review the literature and current concepts. CASE REPORT in the skin was present on the surface of this black A 2-day-old male baby born to a 30-year-old plaque in the interscapular region. In addition primigravida at full term by forceps delivery was there were numerous black, indurated, papules, referred by the pediatric department for dermato- nodules and plaques (1.0-8.0cm) scattered all over logic consultation for the multiple extensive skin the limbs, abdomen, face and neck (Fig. 2). lesions the neonate had since birth. There was no A single, linear, band shaped, yellow plaque with history of any drug intake except haematinics and velvety surface was present on the face and scalp calcium, or exposure to radiation to the mother extending from the lower lip in the midline to the during the pregnancy. -

Hair Loss in Infancy
SCIENCE CITATIONINDEXINDEXED MEDICUS INDEX BY (MEDLINE) EXPANDED (ISI) OFFICIAL JOURNAL OF THE SOCIETÀ ITALIANA DI DERMATOLOGIA MEDICA, CHIRURGICA, ESTETICA E DELLE MALATTIE SESSUALMENTE TRASMESSE (SIDeMaST) VOLUME 149 - No. 1 - FEBRUARY 2014 Anno: 2014 Lavoro: 4731-MD Mese: Febraury titolo breve: Hair loss in infancy Volume: 149 primo autore: MORENO-ROMERO No: 1 pagine: 55-78 Rivista: GIORNALE ITALIANO DI DERMATOLOGIA E VENEREOLOGIA Cod Rivista: G ITAL DERMATOL VENEREOL G ITAL DERMATOL VENEREOL 2014;149:55-78 Hair loss in infancy J. A. MORENO-ROMERO 1, R. GRIMALT 2 Hair diseases represent a signifcant portion of cases seen 1Department of Dermatology by pediatric dermatologists although hair has always been Hospital General de Catalunya, Barcelona, Spain a secondary aspect in pediatricians and dermatologists 2Universitat de Barcelona training, on the erroneous basis that there is not much in- Universitat Internacional de Catalunya, Barcelona, Spain formation extractable from it. Dermatologists are in the enviable situation of being able to study many disorders with simple diagnostic techniques. The hair is easily ac- cessible to examination but, paradoxically, this approach is often disregarded by non-dermatologist. This paper has Embryology and normal hair development been written on the purpose of trying to serve in the diag- nostic process of daily practice, and trying to help, for ex- ample, to distinguish between certain acquired and some The full complement of hair follicles is present genetically determined hair diseases. We will focus on all at birth and no new hair follicles develop thereafter. the data that can be obtained from our patients’ hair and Each follicle is capable of producing three different try to help on using the messages given by hair for each types of hair: lanugo, vellus and terminal. -

Nevus Sebaceous
Open Access Austin Journal of Pediatrics A Austin Full Text Article Publishing Group Review Article Nevus Sebaceous Alexander K. C. Leung1* and Benjamin Barankin2 Abstract 1Department of Pediatrics, University of Calgary, Canada 2Toronto Dermatology Centre, Canada Nevus sebaceous, a hamartoma of the skin and its adnexa, is characterized *Corresponding author: Alexander KC Leung, by epidermal, follicular, sebaceous, and apocrine gland abnormalities. Nevus Department of Pediatrics, The University of Calgary, sebaceous occurs in approximately 0.3% of all newborns. Both sexes are Pediatric Consultant, The Alberta Children’s Hospital, equally affected. The early infantile stage is characterized by papillomatous Calgary, Alberta, T2M 0H5, #200, 233 – 16th Avenue epithelial hyperplasia. The hair follicles are underdeveloped and the sebaceous NW, Canada, Tel: 403 230-3322; Fax: 403 230-3322; glands are not prominent. During puberty, sebaceous glands become numerous Email: [email protected] and hyperplastic, apocrine glands become hyperplastic and cystic, and the epidermis becomes verrucous. The hair follicles remain small and primordial Received: April 28, 2014; Accepted: May 26, 2014; and may disappear altogether. During adulthood, epidermal hyperplasia, large Published: May 27, 2014 sebaceous glands, and ectopic apocrine glands are characteristic histological findings. At birth, nevus sebaceous typically presents as a solitary, well- circumscribed, smooth to velvety, yellow to orange, round or oval, minimally raised plaque. The scalp and face are sites of predilection. Lesions on the scalp are typically hairless. At or just before puberty, the lesion grows more rapidly, becomes more thickened and protuberant, and at times acquires a verrucous or even a nodular appearance. Nevus sebaceous may be complicated by the development of benign and malignant nevoid tumors in the original nevus. -

Current Diagnosis and Treatment Options for Cutaneous Adnexal Neoplasms with Apocrine and Eccrine Differentiation
International Journal of Molecular Sciences Review Current Diagnosis and Treatment Options for Cutaneous Adnexal Neoplasms with Apocrine and Eccrine Differentiation Iga Płachta 1,2,† , Marcin Kleibert 1,2,† , Anna M. Czarnecka 1,* , Mateusz Spałek 1 , Anna Szumera-Cie´ckiewicz 3,4 and Piotr Rutkowski 1 1 Department of Soft Tissue/Bone Sarcoma and Melanoma, Maria Sklodowska-Curie National Research Institute of Oncology, 02-781 Warsaw, Poland; [email protected] (I.P.); [email protected] (M.K.); [email protected] (M.S.); [email protected] (P.R.) 2 Faculty of Medicine, Medical University of Warsaw, 02-091 Warsaw, Poland 3 Department of Pathology and Laboratory Diagnostics, Maria Sklodowska-Curie National Research Institute of Oncology, 02-781 Warsaw, Poland; [email protected] 4 Department of Diagnostic Hematology, Institute of Hematology and Transfusion Medicine, 00-791 Warsaw, Poland * Correspondence: [email protected] or [email protected] † Equally contributed to the work. Abstract: Adnexal tumors of the skin are a rare group of benign and malignant neoplasms that exhibit morphological differentiation toward one or more of the adnexal epithelium types present in normal skin. Tumors deriving from apocrine or eccrine glands are highly heterogeneous and represent various histological entities. Macroscopic and dermatoscopic features of these tumors are unspecific; therefore, a specialized pathological examination is required to correctly diagnose patients. Limited Citation: Płachta, I.; Kleibert, M.; treatment guidelines of adnexal tumor cases are available; thus, therapy is still challenging. Patients Czarnecka, A.M.; Spałek, M.; should be referred to high-volume skin cancer centers to receive an appropriate multidisciplinary Szumera-Cie´ckiewicz,A.; Rutkowski, treatment, affecting their outcome. -
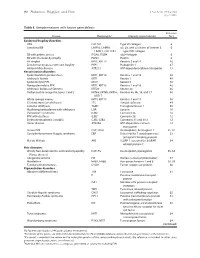

Table I. Genodermatoses with Known Gene Defects 92 Pulkkinen
92 Pulkkinen, Ringpfeil, and Uitto JAM ACAD DERMATOL JULY 2002 Table I. Genodermatoses with known gene defects Reference Disease Mutated gene* Affected protein/function No.† Epidermal fragility disorders DEB COL7A1 Type VII collagen 6 Junctional EB LAMA3, LAMB3, ␣3, 3, and ␥2 chains of laminin 5, 6 LAMC2, COL17A1 type XVII collagen EB with pyloric atresia ITGA6, ITGB4 ␣64 Integrin 6 EB with muscular dystrophy PLEC1 Plectin 6 EB simplex KRT5, KRT14 Keratins 5 and 14 46 Ectodermal dysplasia with skin fragility PKP1 Plakophilin 1 47 Hailey-Hailey disease ATP2C1 ATP-dependent calcium transporter 13 Keratinization disorders Epidermolytic hyperkeratosis KRT1, KRT10 Keratins 1 and 10 46 Ichthyosis hystrix KRT1 Keratin 1 48 Epidermolytic PPK KRT9 Keratin 9 46 Nonepidermolytic PPK KRT1, KRT16 Keratins 1 and 16 46 Ichthyosis bullosa of Siemens KRT2e Keratin 2e 46 Pachyonychia congenita, types 1 and 2 KRT6a, KRT6b, KRT16, Keratins 6a, 6b, 16, and 17 46 KRT17 White sponge naevus KRT4, KRT13 Keratins 4 and 13 46 X-linked recessive ichthyosis STS Steroid sulfatase 49 Lamellar ichthyosis TGM1 Transglutaminase 1 50 Mutilating keratoderma with ichthyosis LOR Loricrin 10 Vohwinkel’s syndrome GJB2 Connexin 26 12 PPK with deafness GJB2 Connexin 26 12 Erythrokeratodermia variabilis GJB3, GJB4 Connexins 31 and 30.3 12 Darier disease ATP2A2 ATP-dependent calcium 14 transporter Striate PPK DSP, DSG1 Desmoplakin, desmoglein 1 51, 52 Conradi-Hu¨nermann-Happle syndrome EBP Delta 8-delta 7 sterol isomerase 53 (emopamil binding protein) Mal de Meleda ARS SLURP-1 -

When the Skin Falls Apart……. Neonatal Blistering Disorders
When the Skin Falls Apart……. Neonatal Blistering Disorders Steven Teich, M.D. Neonatal Blistering Disorders • Suction blisters • Staphylococcal scalded skin syndrome • Aplasia cutis congenita • Congenital herpes simplex virus infection • Bullous congenital ichthyosiform erythroderma • Epidermolysis bullosa Suction Blisters Suction Blisters • Presumed to be induced by vigorous sucking on the affected part in utero • Seen in up to 0.5% of normal newborns at birth • 0.5- to 2-cm oval bullae or erosions on the dorsal aspect of the fingers, thumbs, wrists, lips, or radial aspect of the forearms • Spontaneous resolution without sequelae Staphylococcal Scalded Skin Syndrome (SSSS) Staphylococcal Scalded Skin Syndrome (SSSS) • Blistering skin disorder caused by the epidermolytic toxin- producing S. aureus • Occurs at 2-30 days of life • Abrupt onset of erythema followed by blistering and exfoliation Staphylococcal Scalded Skin Syndrome (SSSS) • SSSS generally begins with localized infection of the conjunctivae, nares, peri-oral region, perineum, or umbilicus • Fever, malaise, lethargy, and poor feeding subsequently develop, and the generalized eruption begins • The rash is characterized by erythema that progresses to large, superficial fragile blisters that rupture easily, leaving behind denuded, erythematous, and tender skin Staphylococcal Scalded Skin Syndrome (SSSS) • Eruption most marked in flexural creases but may involve entire skin • With extensive denudation neonate may have decreased thermoregulatory ability, extensive fluid losses, and -
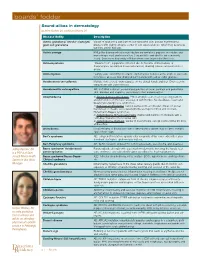

Boards' Fodder
boards’ fodder Sound-alikes in dermatology by Jeffrey Kushner, DO, and Kristen Whitney, DO Disease Entity Description Actinic granuloma/ Annular elastolytic Variant of granuloma annulare on sun-damaged skin; annular erythematous giant cell granuloma plaques with slightly atrophic center in sun-exposed areas, which may be precipi- tated by actinic damage. Actinic prurigo PMLE-like disease with photodistributed erythematous papules or nodules and hemorrhagic crust and excoriation. Conjunctivitis and cheilitis are commonly found. Seen more frequently in Native Americans (especially Mestizos). Actinomycetoma “Madura Foot”; suppurative infection due to Nocaria, Actinomadura, or Streptomyces resulting in tissue tumefaction, draining sinuses and extrusion of grains. Actinomycosis “Lumpy Jaw”; Actinomyces israelii; erythematous nodules at the angle of jaw leads to fistulous abscess that drain purulent material with yellow sulfur granules. Acrokeratosis verruciformis Multiple skin-colored, warty papules on the dorsal hands and feet. Often seen in conjunction with Darier disease. Acrodermatitis enteropathica AR; SLC39A4 mutation; eczematous patches on acral, perineal and periorificial skin; diarrhea and alopecia; secondary to zinc malabsorption. Atrophoderma 1) Atrophoderma vermiculatum: Pitted atrophic scars in a honeycomb pattern around follicles on the face; associated with Rombo, Nicolau-Balus, Tuzun and Braun-Falco-Marghescu syndromes. 2) Follicular atrophoderma: Icepick depressions at follicular orifices on dorsal hands/feet or cheeks; associated with Bazex-Dupré-Christol and Conradi- Hünermann-Happle syndromes. 3) Atrophoderma of Pasini and Pierini: Depressed patches on the back with a “cliff-drop” transition from normal skin. 4) Atrophoderma of Moulin: Similar to Pasini/Pierini, except lesions follow the lines of Blaschko. Anetoderma Localized area of flaccid skin due to decreased or absent elastic fibers; exhibits “buttonhole” sign. -

Ocular Manifestations of Inherited Diseases Maya Eibschitz-Tsimhoni
10 Ocular Manifestations of Inherited Diseases Maya Eibschitz-Tsimhoni ecognizing an ocular abnormality may be the first step in Ridentifying an inherited condition or syndrome. Identifying an inherited condition may corroborate a presumptive diagno- sis, guide subsequent management, provide valuable prognostic information for the patient, and determine if genetic counseling is needed. Syndromes with prominent ocular findings are listed in Table 10-1, along with their alternative names. By no means is this a complete listing. Two-hundred and thirty-five of approxi- mately 1900 syndromes associated with ocular or periocular manifestations (both inherited and noninherited) identified in the medical literature were chosen for this chapter. These syn- dromes were selected on the basis of their frequency, the char- acteristic or unique systemic or ocular findings present, as well as their recognition within the medical literature. The boldfaced terms are discussed further in Table 10-2. Table 10-2 provides a brief overview of the common ocular and systemic findings for these syndromes. The table is organ- ized alphabetically; the boldface name of a syndrome is followed by a common alternative name when appropriate. Next, the Online Mendelian Inheritance in Man (OMIM™) index num- ber is listed. By accessing the OMIM™ website maintained by the National Center for Biotechnology Information at http://www.ncbi.nlm.nih.gov, the reader can supplement the material in the chapter with the latest research available on that syndrome. A MIM number without a prefix means that the mode of inheritance has not been proven. The prefix (*) in front of a MIM number means that the phenotype determined by the gene at a given locus is separate from those represented by other 526 chapter 10: ocular manifestations of inherited diseases 527 asterisked entries and that the mode of inheritance of the phe- notype has been proven. -

Dystrophic Epidermolysis Bullosa
NLM Citation: Pfendner EG, Lucky AW. Dystrophic Epidermolysis Bullosa. 2006 Aug 21 [Updated 2018 Sep 13]. In: Adam MP, Ardinger HH, Pagon RA, et al., editors. GeneReviews® [Internet]. Seattle (WA): University of Washington, Seattle; 1993-2019. Bookshelf URL: https://www.ncbi.nlm.nih.gov/books/ Dystrophic Epidermolysis Bullosa Synonyms: DEB, Epidermolysis Bullosa Dystrophica Ellen G Pfendner, PhD1 and Anne W Lucky, MD2 Created: August 21, 2006; Updated: September 13, 2018. Summary Clinical characteristics Dystrophic epidermolysis bullosa (DEB) is a genetic skin disorder affecting skin and nails that usually presents at birth. DEB is divided into two major types depending on inheritance pattern: recessive dystrophic epidermolysis bullosa (RDEB) and dominant dystrophic epidermolysis bullosa (DDEB). Each type is further divided into multiple clinical subtypes. Absence of a known family history of DEB does not preclude the diagnosis. Clinical findings in severe generalized RDEB include skin fragility manifest by blistering with minimal trauma that heals with milia and scarring. Blistering and erosions affecting the whole body may be present in the neonatal period. Oral involvement may lead to mouth blistering, fusion of the tongue to the floor of the mouth, and progressive diminution of the size of the oral cavity. Esophageal erosions can lead to webs and strictures that can cause severe dysphagia. Consequently, malnutrition and vitamin and mineral deficiency may lead to growth restriction in young children. Corneal erosions can lead to scarring and loss of vision. Blistering of the hands and feet followed by scarring fuses the digits into "mitten" hands and feet, with contractures and pseudosyndactyly. The lifetime risk of aggressive squamous cell carcinoma is higher than 90%.