10 Bile Diverting Operations for Management of Esophageal Disease
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Duodenal Switch. a Switch to the Duodenal Switch. A
Bariátrica & Metabólica Ibero-Americana (2019) 9.2.4: 2554-2563 Duodenal switch. A switch to the duodenal switch. A. Baltasar, N. Pérez, R. Bou, C. Serra Hospital "Virgen De Los Lirios De Alcoy”, Clínica San Jorge [email protected] 616.231.021 ABSTRACT: Background: The duodenal Switch (DS) combines a Sleeve-forming Keywords: gastrectomy (SFG) and a bilio-pancreatic diversion (BPD). Objectives: To report on 950 DS patients treated from 1994 to 2011. • Duodenal junction • Bariatric surgery Environment: Regional teaching hospital and private institution. • Vertical gastrectomy Methods: Prospective study of 950 consecutive patients treated with CD. • Bilio-pancreatic diversion • Poliphenols. Results: There were 518 open DS (ODS) and 432 laparoscopic DS (LDS). Surgical mortality of 0.73% (1.6% in CDA and 0.47% in CDL), 4.84% incidence of leakage, two liver failure (0.2%) and protein calorie malnutrition (PCM) in 3.1%. At 5 years, the %EWL drops by 80% and the Expected BMI by 100%. Conclusions: The CD is the most aggressive bariatric technique, with the best long-term weight loss. Operative complications and long-term follow-up guidelines are described. The aim is to change the bariatric techniques to accept the CD. 2555 Bariátrica & Metabólica Ibero-Americana (2019) 9.2.4: 2554-2563 Introduction Description of surgical techniques The Duodenal Switch (DS) is a mixed operation that consists Open DS (ODS) by transverse laparotomy of two techniques, a gastric surgery, the Sleeve-forming The patient is in Trendelenburg position. A transverse Vertical Gastrectomy (SFG) to reduce intake and also an supraumbilical incision is made between both costal intestinal surgery, the bilio-pancreatic diversion (BPD) that margins (Fig.2 a-b). -

Laparoscopic Truncal Vagotomy and Gatrojejunostomy for Pyloric Stenosis
ORIGINAL ARTICLE pISSN 2234-778X •eISSN 2234-5248 J Minim Invasive Surg 2015;18(2):48-52 Journal of Minimally Invasive Surgery Laparoscopic Truncal Vagotomy and Gatrojejunostomy for Pyloric Stenosis Jung-Wook Suh, M.D.1, Ye Seob Jee, M.D., Ph.D.1,2 Department of Surgery, 1Dankook University Hospital, 2Dankook University School of Medicine, Cheonan, Korea Purpose: Peptic ulcer disease (PUD) remains one of the most prevalent gastrointestinal diseases and Received January 27, 2015 an important target for surgical treatment. Laparoscopy applies to most surgical procedures; however Revised 1st March 9, 2015 its use in elective peptic ulcer surgery, particularly in cases of pyloric stenosis, has not been popular. 2nd March 28, 2015 The aim of this study was to describe the role of laparoscopic surgery and an easily performed Accepted April 20, 2015 procedure for pyloric stenosis. We accordingly performed laparoscopic truncal vagotomy with gastrojejunostomy in 10 consecutive patients with pyloric stenosis. Corresponding author Ye Seob Jee Methods: Data were collected prospectively from all patients who underwent laparoscopic truncal Department of Surgery, Dankook vagotomy with gastrojejunostomy from August 2009 to May 2014 and reviewed retrospectively. University Hospital, Dankook Results: A total of 10 patients underwent laparoscopic trucal vagotomy with gastrojejunostomy for University School of Medicine, 119, peptic ulcer obstruction from August 2009 to May 2014 in ○○ university hospital. The mean age was Dandae-ro, Dongnam-gu, Cheonan 62.6 (±16.4) years old and mean BMI was 19.3 (±2.5) kg/m2. There were no conversions to open 330-714, Korea surgery and no occurrence of intra-operative complications. -

Thoracoscopic Truncal Vagotomy Versus Surgical Revision of the Gastrojejunal Anastomosis for Recalcitrant Marginal Ulcers
Surgical Endoscopy (2019) 33:607–611 and Other Interventional Techniques https://doi.org/10.1007/s00464-018-6386-7 2018 SAGES ORAL DYNAMIC Thoracoscopic truncal vagotomy versus surgical revision of the gastrojejunal anastomosis for recalcitrant marginal ulcers Alicia Bonanno1 · Brandon Tieu2 · Elizabeth Dewey1 · Farah Husain3 Received: 1 May 2018 / Accepted: 10 August 2018 / Published online: 21 August 2018 © Springer Science+Business Media, LLC, part of Springer Nature 2018 Abstract Introduction Marginal ulcer is a common complication following Roux-en-Y gastric bypass with incidence rates between 1 and 16%. Most marginal ulcers resolve with medical management and lifestyle changes, but in the rare case of a non-healing marginal ulcer there are few treatment options. Revision of the gastrojejunal (GJ) anastomosis carries significant morbidity with complication rates ranging from 10 to 50%. Thoracoscopic truncal vagotomy (TTV) may be a safer alternative with decreased operative times. The purpose of this study is to evaluate the safety and effectiveness of TTV in comparison to GJ revision for treatment of recalcitrant marginal ulcers. Methods A retrospective chart review of patients who required surgical intervention for non-healing marginal ulcers was performed from 1 September 2012 to 1 September 2017. All underwent medical therapy along with lifestyle changes prior to intervention and had preoperative EGD that demonstrated a recalcitrant marginal ulcer. Revision of the GJ anastomosis or TTV was performed. Data collected included operative time, ulcer recurrence, morbidity rate, and mortality rate. Results Twenty patients were identified who underwent either GJ revision (n = 13) or TTV (n = 7). There were no 30-day mortalities in either group. -

Effects of Sleeve Gastrectomy Plus Trunk Vagotomy Compared with Sleeve Gastrectomy on Glucose Metabolism in Diabetic Rats
Submit a Manuscript: http://www.f6publishing.com World J Gastroenterol 2017 May 14; 23(18): 3269-3278 DOI: 10.3748/wjg.v23.i18.3269 ISSN 1007-9327 (print) ISSN 2219-2840 (online) ORIGINAL ARTICLE Basic Study Effects of sleeve gastrectomy plus trunk vagotomy compared with sleeve gastrectomy on glucose metabolism in diabetic rats Teng Liu, Ming-Wei Zhong, Yi Liu, Xin Huang, Yu-Gang Cheng, Ke-Xin Wang, Shao-Zhuang Liu, San-Yuan Hu Teng Liu, Ming-Wei Zhong, Xin Huang, Yu-Gang Cheng, reviewers. It is distributed in accordance with the Creative Ke-Xin Wang, Shao-Zhuang Liu, San-Yuan Hu, Department Commons Attribution Non Commercial (CC BY-NC 4.0) license, of General Surgery, Qilu Hospital of Shandong University, Jinan which permits others to distribute, remix, adapt, build upon this 250012, Shandong Province, China work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and Yi Liu, Health and Family Planning Commission of Shandong the use is non-commercial. See: http://creativecommons.org/ Provincial Medical Guidance Center, Jinan 250012, Shandong licenses/by-nc/4.0/ Province, China Manuscript source: Unsolicited manuscript Author contributions: Liu T, Liu SZ and Hu SY designed the study and wrote the manuscript; Liu T and Zhong MW instructed Correspondence to: San-Yuan Hu, Professor, Department of on the whole study and prepared the figures; Liu Y and Wang KX General Surgery, Qilu Hospital of Shandong University, No. 107, collected and analyzed the data; Liu T, Huang X and Cheng YG Wenhua Xi Road, Jinan 250012, Shandong Province, performed the operations and performed the observational study; China. -

A Matched Cohort Analysis of Single Anastomosis Loop Duodenal Switch Versus Roux-En-Y Gastric Bypass with 18-Month Follow-Up - Springer
A matched cohort analysis of single anastomosis loop duodenal switch versus Roux-en-Y gastric bypass with 18-month follow-up - Springer Search Submit Article Surgical Endoscopy pp 1-7 First online: 22 December 2015 A matched cohort analysis of single anastomosis loop duodenal switch versus Roux-en-Y gastric bypass with 18-month follow-up Austin Cottam, Daniel Cottam , Walter Medlin, Christina Richards, Samuel Cottam, Hinali Zaveri, Amit Surve 10.1007/s00464-015-4707-7 Copyright information Abstract Background The Roux-en-Y gastric bypass (GBP) has been considered the gold standard for many years. The loop duodenal switch (LDS) is a relatively new procedure that simplifies the complexity of the duodenal switch (BPDDS) by making it a single anastomosis procedure while at the same time giving it more intestinal absorption to reduce the rates of malnutrition associated with traditional BPDDS. This paper seeks to compare the 18-month weight loss outcomes and complications of the more standard GBP with the newer LDS in a single US center. Methods A retrospective matched cohort was analyzed on 108 patients who had either GBP (54 patients) or LDS (54 patients). Regression analysis was used to compare weight loss outcomes as measured by BMI and weight loss percentages. Complications gathered included bleeds, reoperations, diagnostic or therapeutic endoscopy (EGD), ulcers and chronic nausea. Results GBP and LDS have statistically similar weight loss at 18 months (39.6 vs 41 % weight loss, respectively). However, there were significantly more nausea complaints (26 vs 5), diagnostic endoscopies (EGD) (21 vs 3) and ulcers (6 vs 0) with the GBP than the LDS. -

Biliopancreatic Diversion with a Duodenal Switch
Obesity Surgeuy, 8, 267-282 Biliopancreatic Diversion with a Duodenal Switch Douglas S. Hess MD, FACS; Douglas W. Hess MD Wood County Hospital, Bowling Green, OH, USA Background: This paper evaluates biliopancreatic BPD without some of the associated problems. diversion combined with the duodenal switch, form- This operation is now used by us for all our ing a hybrid procedure which is a combination of bariatric patients, both in primary surgical proce- restriction and malabsorption. Methods: The evaluation is of the first 440 patients dures and reoperations. undergoing this procedure who had had no previous The difficulty of establishing an operation that bariatric surgery. The mean starting weight was has both long- and short-term success is well 183 kg, with 41% of our patients considered super known. Bariatric surgery is either restrictive or morbidly obese (BMI > 50). malabsorptive in nature, each with its own ad- Results: There was an average maximum weight loss of 80% excess weight by 24 months post- vantages, disadvantages and complications. While operation; this continued at a 70% level for 8 years. trying to find a procedure that would produce Major complications were found in almost 9% of the better long-term results and fewer failures, i.e. cases. There were two perioperative deaths, one regain of weight, we began to look at the from pulmonary embolism and one from acute Scopinaro BPD.l First of all we considered it pulmonary obstruction. There were 36 type II dia- betics, all of whom have discontinued medication only for reoperations on failed restrictive proce- following the surgery. -

Gastroenterostomy and Vagotomy for Chronic Duodenal Ulcer
Gut, 1969, 10, 366-374 Gut: first published as 10.1136/gut.10.5.366 on 1 May 1969. Downloaded from Gastroenterostomy and vagotomy for chronic duodenal ulcer A. W. DELLIPIANI, I. B. MACLEOD1, J. W. W. THOMSON, AND A. A. SHIVAS From the Departments of Therapeutics, Clinical Surgery, and Pathology, The University ofEdinburgh The number of operative procedures currently in Kingdom answered a postal questionnaire. Eight had vogue in the management of chronic duodenal ulcer died since operation, and three could not be traced. The indicates that none has yet achieved definitive status. patients were questioned particularly with regard to Until recent years, partial gastrectomy was the eating capacity, dumping symptoms, vomiting, ulcer-type dyspepsia, diarrhoea or other change in bowel habit, and favoured operation, but an increasing awareness of a clinical assessment was made based on a modified its significant operative mortality and its metabolic Visick scale. The mean time since operation was 6-9 consequences, along with Dragstedt and Owen's years. demonstration of the effectiveness of vagotomy in Thirty-five patients from this group were admitted to reducing acid secretion (1943), has resulted in the hospital for a full investigation of gastrointestinal and widespread use of vagotomy and gastric drainage. related function two to seven years following their The success of duodenal ulcer surgery cannot be operation. Most were volunteers, but some were selected judged only on low stomal (or recurrent) ulceration because of definite complaints. There were more females rates; the other sequelae of gastric operations must than males (21 females and 14 males). The following be considered. -

Technic VERTICAL GASTROPLASTY WITH
ABCDDV/802 ABCD Arq Bras Cir Dig Technic 2011;24(3): 242-245 VERTICAL GASTROPLASTY WITH JEJUNOILEAL BYPASS - NEW TECHNICAL PROCEDURE Gastroplastia vertical com desvio jejunoileal - novo procedimento técnico Bruno ZILBERSTEIN, Arthur Sergio da SILVEIRA-FILHO, Juliana Abbud FERREIRA, Marnay Helbo de CARVALHO, Cely BUSSONS, Henrique JOAQUIM, Fernando RAMOS From Gastromed-Instituto Zilberstein, São ABSTRACT - Introduction - Vertical gastroplasty is increasingly used in the surgical Paulo, SP, Brasil. treatment of morbid obesity, being used alone or as part of the duodenal switch surgery or even in intestinal bipartition (Santoro technique). When used alone has only a restrictive character. Method - Is proposed association of jejunoileal bypass to vertical gastroplasty, in order to give a metabolic component to the procedure and eventually empower it to medium and long term. Eight morbidly obese patients were operated after removal of adjustable gastric band or as a primary procedure associated to vertical banded gastroplasty with jejunoileal bypass laterolateral and anastomosis between the jejunum 80 cm from duodenojejunal angle and the ileum at 120 cm from ileocecal valve, by laparoscopy. Results - The patients presented themselves without complications both in trans or in the immediate postoperative period, and also in the months that followed. The evolution BMI showed a significant reduction ranging from 39.57 kg/m2 to 28 kg/m2. No patient reported diarrhea or malabsorptive disorder in HEADINGS - Sleeve gastrectomy. Jejunoileal the period. Conclusion - It can be offered a new therapeutic option, with restraining diversion. Obesity. Surgery. and metabolic aspects, in which there are no consequences as the ones founded in procedures with duodenal diversion or intestinal transit alterations. -

A Case Report
LAPAROSCOPIC POSTERIOR TRUNCAL VAGOTOMY AND ANTERIOR HIGHLY SELECTIVE VAGOTOMY - A CASE REPORT C K Kum, P Goh ABSTRACT Laparoscopie vagotomy provides a viable alternative to expensive long-term treatment with 112 antagonists in patients with intractable peptic ulcer disease. The minimally invasive procedure offers reduced postoperative discomfort and improved cosmesis. Here, we report our first case of a posterior truncal vagotomy and anterior highly selective vagotmny performed laparoscopicallyfor the first time in Asia. The surgery was uneventful. Diet was resumed on day 3 and the patient was discharged on day 4. Post-vagotomy acid secretion tests on the third week revealed a dramatic decrease in acid production. With further experience, laparoscopic vagotomy can be an attractive alternative to long tern medication in peptic ulcer disease. Keywords: Laparoscopy, Vagotomy, Laparoscopic vagotomy, Highly selective vagotomy, Peptic ulcer. SINGAPORE MED J 1992; Vol 33: 302-303 INTRODUCTION ration of the procedure was 150 mins. Postoperatively, the The advent of laparoscopic highly selective vagotomy has pro- patient was able to have feeds on the second day and normal vided patients with ulcer diasthesis a viable alternative to long diet the next day. He was discharged on the fourth day. Acid term dependency on H2 antagonists. Laparoscopic surgery, in secretion tests with insulin stimulation three weeks later re- contrast to conventional open surgery, is characterized by short vealed a dramatic improvement (Table 1). recovery, brief hospitalization and negligible postoperative Operative Procedure scars. We report our first case of laparoscopie highly selective The objective was to denervate the acid -secreting parietal cells vagotomy performed with minimal discomfort to the patient. -
Internal Hernia After Revisional Laparoscopic Loop Duodenal Switch
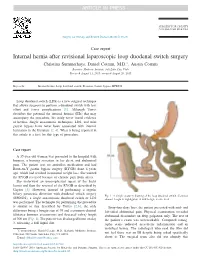
Surgery for Obesity and Related Diseases ] (2015) 00–00 Case report Internal hernia after revisional laparoscopic loop duodenal switch surgery Christina Summerhays, Daniel Cottam, M.D.*, Austin Cottam Bariatric Medicine Institute, Salt Lake City, Utah Received August 11, 2015; accepted August 20, 2015 Keywords: Internal hernia; Loop duodenal switch; Revision; Gastric bypass; BPD/DS Loop duodenal switch (LDS) is a new surgical technique that allows surgeons to perform a duodenal switch with less effort and fewer complications [1]. Although Torres describes the potential for internal hernias (IHs) that may accompany the procedure, his study never found evidence of hernias. Single anastomotic techniques, LDS, and mini gastric bypass have never been associated with internal herniation in the literature [2–4]. What is being reported in this article is a first for this type of procedure. Case report A 35-year-old woman was presented to the hospital with burping, a burning sensation in her chest, and abdominal pain. The patient was on antireflux medication and had Roux-en-Y gastric bypass surgery (RYGB) done 6 years ago, which had resulted in minimal weight loss. She wanted the RYGB reversed because of chronic pain from ulcers. She underwent an uncomplicated repair of the hiatal hernia and then the reversal of the RYGB as described by Gagner [5]. However, instead of performing a regular biliary pancreatic diversion with duodenal switch surgery Fig. 1. A simple anatomy drawing of the loop duodenal switch. Common (BPD/DS), a single anastomosis duodenal switch or LDS channel length is highlighted. A 40F bougie is also used. was performed. -

A History of Bariatric Surgery the Maturation of a Medical Discipline
A History of Bariatric Surgery The Maturation of a Medical Discipline Adam C. Celio, MD, Walter J. Pories, MD* KEYWORDS Bariatric Obesity Metabolic surgery Intestinal bypass Gastric bypass Gastric sleeve Gastric band Gastric balloon KEY POINTS The history of bariatric surgery, one of the great medical advances of the last century, again documents that science progresses not as a single idea by one person, but rather in small collaborative steps that take decades to accept. Bariatric surgery, now renamed “metabolic surgery,” has, for the first time, provided cure for some of the most deadly diseases, including type 2 diabetes, hypertension, severe obesity, NASH, and hyperlipidemias, among others, that were previously considered incurable and for which there were no effective therapies. With organization, a common database, and certification of centers of excellence, bariat- ric surgery, once one of the most dangerous operations, is now performed throughout the United States with the same safety as a routine cholecystectomy. RECOGNITION Obesity is now a worldwide public health problem, an epidemic, with increasing inci- dence and prevalence, high costs, and associated comorbidities.1 Although the genes from our ancestors were helpful in times of potential famine, now in times of plenty, they have contributed to obesity.1–4 The history of obesity is related to the history of food; the human diet has changed considerably over the last 700,000 years. Our an- cestors at one time were hunter-gatherers, consuming large and small game along with nuts and berries. Their diets were high in protein and their way of life was stren- uous; they were well suited for times of famine. -

Vagotomy with Pyloroplasty Or Antrectomy: a Comparison of Results in the Treatment of Duodenal Ulcer Richard L
Henry Ford Hospital Medical Journal Volume 22 Number 3 Laurence S. Fallis, M.D. Commemorative Article 9 Issue 9-1974 Vagotomy with Pyloroplasty or Antrectomy: A Comparison of Results in the Treatment of Duodenal Ulcer Richard L. Collier John H. Wylie Jr. Follow this and additional works at: https://scholarlycommons.henryford.com/hfhmedjournal Part of the Life Sciences Commons, Medical Specialties Commons, and the Public Health Commons Recommended Citation Collier, Richard L. and Wylie, John H. Jr. (1974) "Vagotomy with Pyloroplasty or Antrectomy: A Comparison of Results in the Treatment of Duodenal Ulcer," Henry Ford Hospital Medical Journal : Vol. 22 : No. 3 , 149-152. Available at: https://scholarlycommons.henryford.com/hfhmedjournal/vol22/iss3/9 This Article is brought to you for free and open access by Henry Ford Health System Scholarly Commons. It has been accepted for inclusion in Henry Ford Hospital Medical Journal by an authorized editor of Henry Ford Health System Scholarly Commons. Henry Ford Hosp. Med. Journal Vol. 22, No. 3, 1974 Vagotomy with Pyloroplasty or Antrectomy A Comparison of Results in the Treatment of Duodenal Ulcer Richard L. Collier, MD* and John H. Wylie, Jr, MD** DURING the past several decades, there have been changes in the surgical treatment of peptic ulcer. More knowl edge of the physiology of the stomach has given direction to these trends. Dur ing his many years of surgical practice, Dr. Laurence Fallis found the surgical During the years 1970-73, 776 operations treatment of peptic ulcer to be one of his were performed for the relief of duodenal chief interests.