What Are Pituitary Tumors?
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Synchronous Morphologically Distinct Craniopharyngioma and Pituitary
orders & is T D h e n r Bhatoe et al., Brain Disord Ther 2016, 5:1 i a a p r y B Brain Disorders & Therapy DOI: 10.4172/2168-975X.1000207 ISSN: 2168-975X Case Report Open Access Synchronous Morphologically Distinct Craniopharyngioma and Pituitary Adenoma: A Rare Collision Entity Harjinder S Bhatoe*, Prabal Deb and Sudip Kumar Sengupta Institute of Neuroscience, Max Super Speciality Hospital, New Delhi, India Abstract While pituitary tumors and craniopharyngiomas share a common lineage, their simultaneous occurrence is distinctly rare. We present one such patient, an adult male with two distinct tumors, that were excised by two different approaches. Relevant literature is briefly reviewed. Keywords: Brain tumor; Collision tumor; Craniopharyngioma; Pituitary tumor Introduction Simultaneous occurrence of morphological distinct, discreet intracranial tumors sharing the same cell lineage is a rarity. Pituitary tumors and craniopharyngiomas share a common lineage. Simultaneous occurrence of these two tumors in the same patient is rare and has been reported only nine times so far (Table 1). While pituitary tumours are centred in the sella, craniopharyngiomas may occur anywhere from the pituitary gland to the third ventricle. Association of intra-third ventricular craniopharyngioma and growth hormone- Figure 1: Contrast MRI (T1-weighted sagittal) showing intra-third-ventricular secreting pituitary macroadenoma as two distinct, unconnected tumors craniopharyngioma and pituitary adenoma. occurring synchronously has not been reported so far. Case Report A 35-year-old male was admitted with six-month-history of generalized headache, gradual loss of vision and intermittent generalized tonic clonic seizures. Clinically, he had acromegaly and optic atrophy with no perception of light. -

Incidental Pituitary Adenomas
Neurosurg Focus 31 (6):E18, 2011 Incidental pituitary adenomas WALAVAN SIVAKUMAR, M.D.,1 ROUKOZ CHAMOUN, M.D.,1 VINH NGUYEN, M.D.,2 AND WILLIAM T. COULdwELL, M.D., PH.D.1 Departments of 1Neurosurgery and 2Radiology, University of Utah, Salt Lake City, Utah Object. Pituitary incidentalomas are a common finding with a poorly understood natural history. Over the last few decades, numerous studies have sought to decipher the optimal evaluation and treatment of these lesions. This paper aims to elucidate the current evidence regarding their prevalence, natural history, evaluation, and management. Methods. A search of articles on PubMed (National Library of Medicine) and reference lists of all relevant ar- ticles was conducted to identify all studies pertaining to the incidence, natural history, workup, treatment, and follow- up of incidental pituitary and sellar lesions, nonfunctioning pituitary adenomas, and incidentalomas. Results. The reported prevalence of pituitary incidentalomas has increased significantly in recent years. A com- plete history, physical, and endocrinological workup with formal visual field testing in the event of optic apparatus involvement constitutes the basics of the initial evaluation. Although data regarding the natural history of pituitary incidentalomas remain sparse, they seem to suggest that progression to pituitary apoplexy (0.6/100 patient-years), visual field deficits (0.6/100 patient-years), and endocrine dysfunction (0.8/100 patient-years) remains low. In larger lesions, apoplexy risk may be higher. Conclusions. While the majority of pituitary incidentalomas can be managed conservatively, involvement of the optic apparatus, endocrine dysfunction, ophthalmological symptoms, and progressive increase in size represent the main indications for surgery. -

Multiple Endocrine Neoplasia Type 1 (MEN1)
Lab Management Guidelines v2.0.2019 Multiple Endocrine Neoplasia Type 1 (MEN1) MOL.TS.285.A v2.0.2019 Introduction Multiple Endocrine Neoplasia Type 1 (MEN1) is addressed by this guideline. Procedures addressed The inclusion of any procedure code in this table does not imply that the code is under management or requires prior authorization. Refer to the specific Health Plan's procedure code list for management requirements. Procedures addressed by this Procedure codes guideline MEN1 Known Familial Mutation Analysis 81403 MEN1 Deletion/Duplication Analysis 81404 MEN1 Full Gene Sequencing 81405 What is Multiple Endocrine Neoplasia Type 1 Definition Multiple Endocrine Neoplasia Type 1 (MEN1) is an inherited form of tumor predisposition characterized by multiple tumors of the endocrine system. Incidence or Prevalence MEN1 has a prevalence of 1/10,000 to 1/100,000 individuals.1 Symptoms The presenting symptom in 90% of individuals with MEN1 is primary hyperparathyroidism (PHPT). Parathyroid tumors cause overproduction of parathyroid hormone which leads to hypercalcemia. The average age of onset is 20-25 years. Parathyroid carcinomas are rare in individuals with MEN1.2,3,4 Pituitary tumors are seen in 30-40% of individuals and are the first clinical manifestation in 10% of familial cases and 25% of simplex cases. Tumors are typically solitary and there is no increased prevalence of pituitary carcinoma in individuals with MEN1.2,5 © eviCore healthcare. All Rights Reserved. 1 of 9 400 Buckwalter Place Boulevard, Bluffton, SC 29910 (800) 918-8924 www.eviCore.com Lab Management Guidelines v2.0.2019 Prolactinomas are the most commonly seen pituitary subtype and account for 60% of pituitary adenomas. -

Findings of Brain Magnetic Resonance Imaging in Girls with Central Precocious Puberty Compared with Girls with Chronic Or Recurrent Headache
Journal of Clinical Medicine Article Findings of Brain Magnetic Resonance Imaging in Girls with Central Precocious Puberty Compared with Girls with Chronic or Recurrent Headache Shin-Hee Kim 1, Moon Bae Ahn 2 , Won Kyoung Cho 2 , Kyoung Soon Cho 2, Min Ho Jung 3,* and Byung-Kyu Suh 2 1 Department of Pediatrics, Incheon St. Mary’s Hospital, College of Medicine, The Catholic University of Korea, Incheon 21431, Korea; [email protected] 2 Department of Pediatrics, College of Medicine, The Catholic University of Korea, Seoul 06591, Korea; [email protected] (M.B.A.); [email protected] (W.K.C.); [email protected] (K.S.C.); [email protected] (B.K.S.) 3 Department of Pediatrics, Yeouido St. Mary’s Hospital, College of Medicine, The Catholic University of Korea, Seoul 07345, Korea * Correspondence: [email protected] Abstract: In the present study, the results of brain magnetic resonance imaging (MRI) in girls with central precocious puberty (CPP) were compared those in with girls evaluated for headaches. A total of 295 girls with CPP who underwent sellar MRI were enrolled. A total of 205 age-matched girls with chronic or recurrent headaches without neurological abnormality who had brain MRI were included as controls. The positive MRI findings were categorized as incidental non-hypothalamic–pituitary (H–P), incidental H–P, or pathological. Positive MRI findings were observed in 39 girls (13.2%) with Citation: Kim, S.-H.; Ahn, M.B.; Cho, CPP; 8 (2.7%) were classified as incidental non-H–P lesions, 30 (10.2%) as incidental H–P lesions, and 1 W.K.; Cho, K.S.; Jung, M.H.; Suh, B.-K. -
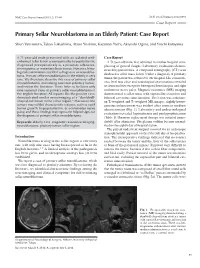
Primary Sellar Neuroblastoma in an Elderly Patient: Case Report
NMC Case Report Journal 2015; 2: 57–60 DOI: 10.2176/nmccrj.2014-0091 Case Report Primary Sellar Neuroblastoma in an Elderly Patient: Case Report Shun Yamamuro, Takao Fukushima, Atsuo Yoshino, Kazunari Yachi, Akiyoshi Ogino, and Yoichi Katayama A 71-year-old male presented with an isolated well- Case Report enhanced sellar lesion accompanied by hypopituitarism, A 71-year-old male was admitted to another hospital com- diagnosed preoperatively as a pituitary adenoma, plaining of general fatigue. Laboratory evaluations demon- meningioma, or metastatic brain tumor. However, histo- strated hyponatremia. A computed tomography (CT) scan logical examinations yielded a diagnosis of neuroblas- disclosed a sellar mass lesion. Under a diagnosis of pituitary toma. Primary sellar neuroblastoma in the elderly is very rare. We therefore describe this case of primary sellar tumor, the patient was referred to our hospital. His conscious- neuroblastoma, mimicking common pituitary tumor, ness level was clear and neurological examinations revealed and review the literature. There have so far been only no abnormalities except for bitemporal hemianopsia and right nine reported cases of primary sellar neuroblastoma in oculomotor nerve palsy. Magnetic resonance (MR) imaging the English literature. All reports like the present case, demonstrated a sellar mass with suprasellar extension and demonstrated similar neuroimaging of a “dumbbell- bilateral cavernous sinus invasion. The lesion was isointense shaped extension in the sellar region.” Moreover, the on T1-weighted and T2-weighted MR images; slightly hetero- tumors may exhibit characteristic features, such as rapid geneous enhancement was evident after contrast medium tumor growth, hypopituitarism, or oculomotor nerve administration (Fig. 1). Laboratory and endocrinological palsy, and these findings may represent helpful signs for evaluations revealed hyponatremia and panhypopituitarism the diagnosis of primary sellar neuroblastoma. -

Hypothalamic Hamartomas Causing Gelastic Epilepsy: Two Cases and a Review of the Literature
Seizure 1998; 7:167-171 CASE REPORT Hypothalamic hamartomas causing gelastic epilepsy: Two cases and a review of the literature N. GEORGAKOULIAS*, C. VIZE*, A. JENKINS* & E. SINGOUNAS t * Department of Neurosurgery, Newcastle General Hospital, UK; t Evangelismos General Hospital, Athens, Greece Correspondence to: N. Georgakoulias, Department of Neurosurgery, Middlesbrough General Hospital, Ayresome Green Lane, Middlesbrough, Cleveland, TS5 5AZ, UK Two cases of hypothalamic hamartomas causing gelastic epilepsy are described. The clinical presentations and the radiological features are presented, and the mechanisms involved in laughing attacks are discussed. The literature is reviewed and it is suggested the complete extirpation of the hamartomas is the treatment of choice in gelastic epilepsy. Key words: hypothalamic hamartomas; gelastic epilepsy. INTRODUCTION improvement. One month later, he was admitted fol- lowing a generalized seizure and vigabritin 500 mg Gelastic epilepsy, or laughter attacks (Greek gelos = bd was added. laugh), may occur in association with hypothalamic Unfortunately his fits continued to increase until hamartomas. The management of affected patients is he was having between 10 and 20 seizures per day. difficult and controversial. In this report we present These were sometimes spontaneous but oftenprecipi- two patients to illustrate dilemmas in management, tated by laughing and consisted of a short period of and have reviewed the literature associated with this laughter followed by hand-clapping and various au- condition. -

Pituitary Adenomas: from Diagnosis to Therapeutics
biomedicines Review Pituitary Adenomas: From Diagnosis to Therapeutics Samridhi Banskota 1 and David C. Adamson 1,2,3,* 1 School of Medicine, Emory University, Atlanta, GA 30322, USA; [email protected] 2 Department of Neurosurgery, Emory University, Atlanta, GA 30322, USA 3 Neurosurgery, Atlanta VA Healthcare System, Decatur, GA 30322, USA * Correspondence: [email protected] Abstract: Pituitary adenomas are tumors that arise in the anterior pituitary gland. They are the third most common cause of central nervous system (CNS) tumors among adults. Most adenomas are benign and exert their effect via excess hormone secretion or mass effect. Clinical presentation of pituitary adenoma varies based on their size and hormone secreted. Here, we review some of the most common types of pituitary adenomas, their clinical presentation, and current diagnostic and therapeutic strategies. Keywords: pituitary adenoma; prolactinoma; acromegaly; Cushing’s; transsphenoidal; CNS tumor 1. Introduction The pituitary gland is located at the base of the brain, coming off the inferior hy- pothalamus, and weighs no more than half a gram. The pituitary gland is often referred to as the “master gland” and is the most important endocrine gland in the body because it regulates vital hormone secretion [1]. These hormones are responsible for vital bodily Citation: Banskota, S.; Adamson, functions, such as growth, blood pressure, reproduction, and metabolism [2]. Anatomically, D.C. Pituitary Adenomas: From the pituitary gland is divided into three lobes: anterior, intermediate, and posterior. The Diagnosis to Therapeutics. anterior lobe is composed of several endocrine cells, such as lactotropes, somatotropes, and Biomedicines 2021, 9, 494. https: corticotropes, which synthesize and secrete specific hormones. -
Onc26. Pituitary Tumors, Apoplexy, Empty Sella.Pdf
PITUITARY TUMORS Onc26 (1) Pituitary Tumors Last updated: December 22, 2020 Differential Diagnosis of Sellar and Parasellar Tumors ................................................................... 1 PITUITARY ADENOMAS ................................................................................................................... 1 PATHOPHYSIOLOGY, PATHOLOGY, ETIOLOGY ....................................................................................... 2 CLASSIFICATION .................................................................................................................................... 2 Size ........................................................................................................................................ 2 Hormonal secretion ............................................................................................................... 2 Histology ............................................................................................................................... 2 EPIDEMIOLOGY ...................................................................................................................................... 4 CLINICAL FEATURES .............................................................................................................................. 4 1. Hormonal function control ................................................................................................ 4 2. Mass effect ....................................................................................................................... -

Management of Hypopituitarism
Journal of Clinical Medicine Review Management of Hypopituitarism Krystallenia I. Alexandraki 1 and Ashley B. Grossman 2,3,* 1 Endocrine Unit, 1st Department of Propaedeutic Medicine, School of Medicine, National and Kapodistrian University of Athens, 115 27 Athens, Greece; [email protected] 2 Department of Endocrinology, Oxford Centre for Diabetes, Endocrinology and Metabolism, Churchill Hospital, University of Oxford, Oxford OX3 7LE, UK 3 Centre for Endocrinology, Barts and the London School of Medicine, London EC1M 6BQ, UK * Correspondence: [email protected] Received: 18 November 2019; Accepted: 2 December 2019; Published: 5 December 2019 Abstract: Hypopituitarism includes all clinical conditions that result in partial or complete failure of the anterior and posterior lobe of the pituitary gland’s ability to secrete hormones. The aim of management is usually to replace the target-hormone of hypothalamo-pituitary-endocrine gland axis with the exceptions of secondary hypogonadism when fertility is required, and growth hormone deficiency (GHD), and to safely minimise both symptoms and clinical signs. Adrenocorticotropic hormone deficiency replacement is best performed with the immediate-release oral glucocorticoid hydrocortisone (HC) in 2–3 divided doses. However, novel once-daily modified-release HC targets a more physiological exposure of glucocorticoids. GHD is treated currently with daily subcutaneous GH, but current research is focusing on the development of once-weekly administration of recombinant GH. Hypogonadism is targeted with testosterone replacement in men and on estrogen replacement therapy in women; when fertility is wanted, replacement targets secondary or tertiary levels of hormonal settings. Thyroid-stimulating hormone replacement therapy follows the rules of primary thyroid gland failure with L-thyroxine replacement. -

Multiple Endocrine Neoplasia Type 1: the Potential Role of Micrornas in the Management of the Syndrome
International Journal of Molecular Sciences Review Multiple Endocrine Neoplasia Type 1: The Potential Role of microRNAs in the Management of the Syndrome Simone Donati 1, Simone Ciuffi 1 , Francesca Marini 1, Gaia Palmini 1 , Francesca Miglietta 1, Cinzia Aurilia 1 and Maria Luisa Brandi 1,2,3,* 1 Department of Experimental and Clinical Biomedical Sciences “Mario Serio”, University of Study of Florence, Viale Pieraccini 6, 50139 Florence, Italy; [email protected] (S.D.); simone.ciuffi@unifi.it (S.C.); francesca.marini@unifi.it (F.M.); gaia.palmini@unifi.it (G.P.); [email protected] (F.M.); [email protected] (C.A.) 2 Unit of Bone and Mineral Diseases, University Hospital of Florence, Largo Palagi 1, 50139 Florence, Italy 3 Fondazione Italiana Ricerca Sulle Malattie Dell’Osso (FIRMO Onlus), 50141 Florence, Italy * Correspondence: marialuisa.brandi@unifi.it; Tel.: +39-055-7946304 Received: 24 September 2020; Accepted: 12 October 2020; Published: 14 October 2020 Abstract: Multiple endocrine neoplasia type 1 (MEN1) is a rare inherited tumor syndrome, characterized by the development of multiple neuroendocrine tumors (NETs) in a single patient. Major manifestations include primary hyperparathyroidism, gastro-entero-pancreatic neuroendocrine tumors, and pituitary adenomas. In addition to these main NETs, various combinations of more than 20 endocrine and non-endocrine tumors have been described in MEN1 patients. Despite advances in diagnostic techniques and treatment options, which are generally similar to those of sporadic tumors, patients with MEN1 have a poor life expectancy, and the need for targeted therapies is strongly felt. MEN1 is caused by germline heterozygous inactivating mutations of the MEN1 gene, which encodes menin, a tumor suppressor protein. -

Small (And Large) Blue Cell Tumors of the Skull Base
Small (and large) Blue Cell Tumors of the Skull Base Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University of Arkansas for Medical Sciences [email protected] 1 Sino-Nasal Lesions • High Grade Epithelial Tumors • Tumors with neuroendocrine differentiation • Other lesions in the differential diagnosis 2 Sinonasal Undifferentiated Carcinoma • Incidence: Rare • Clinical • Present with large invasive tumors • Metastases are frequent • Symptoms include nasal obstruction, epistaxis, visual and headache • Prognosis is poor • ~20-25% overall survival at 5 years 3 Sinonasal Undifferentiated Carcinoma • Histopathology • Undifferentiated tumor cells • Mitoses and necrosis • Vascular invasion and adjacent structures • Immunohistochemistry • Positive for Cytokeratin • Controversy: Neuroendocrine marker positivity 4 SNUC, H&E 5 SNUC, H&E 6 SNUC, H&E 7 SNUC, H&E 8 Differential Diagnosis • Melanoma • Ewings/PNET • Rhabdomyosarcoma • NUT midline carcinoma • Lymphoepithelial carcinoma • Lymphoma • Neuroendocrine carcinoma 9 Mucosal Melanoma, H&E 10 Ewing’s, H&E 11 Rhabdomyosarcoma, H&E Work-Up of High Grade Tumor • Cytokeratin stains • Neuroendocrine stains • S100 • HMB45 • CD99 • Myogenin • Desmin • Lymphoma markers 13 NUT Midline Carcinoma • Nut midline carcinomas • More common in young people • Average age 17 years • Very aggressive (lethal) tumors • Histology • Undifferentiated morphology • Abrupt keratinization in 82% • NUT-BRD4 translocation French CA, JCO, 22(20):4135, 2004 14 NUT midline carcinoma, H&E SNUC and NUT Translocation • Stelow, et al • Undifferentiated carcinomas of UADT • NUT rearrangement in 5/28 cases • NUT IHC positive in 3/5 cases • Bishop, et al • NUT IHC in 151 primary sinonasal carcinomas • 2 of 13 SNUCs positive • 1/87 squamous cell carcinomas positive Stelow E, et al. -

Differential Diagnosis of Sellar Masses
~~ ~~ ~ ADVANCES IN PITUITARY TUMOR THERAPY 0889-8529/99 $8.00 + .OO DIFFERENTIAL DIAGNOSIS OF SELLAR MASSES Pamela U. Freda, MD, and Kalmon D. Post, MD Pituitary adenomas are the most common cause of a mass in the sella. In as many as 9% of cases, other etiologies are responsible for mass lesions in the sellar regions4,13' (Table 1). The differential diagnosis of nonpituitary sellar masses is broad and includes cell rest tumors, germ cell tumors, gliomas, menin- giomas, metastatic tumors, vascular lesions, and granulomatous, infectious, and inflammatory processes (Table 2). Differentiating among these potential etiolo- gies may not always be straightforward because many of these lesions, tumorous and nontumorous, may mimic the clinical, endocrinologic, and radiographic presentations of pituitary adenomas. In some cases, there are no features that clearly distinguish the unusual etiologies from the clinically nonfunctioning pituitary adenoma. In others, certain endocrine, neurologic, and radiographic findings that are more characteristic of patients with a nonpituitary sellar mass may be present and can help in their differentiation. Correct preoperative diag- nosis is clinically important because the treatment of choice for many of these nonpituitary sellar masses differs from that of a pituitary tumor. This article provides an overview of the clinical and radiographic characteristics of both pituitary tumors and the nonpituitary lesions found in the sellar/parasellar region and discusses in detail the specific nonpituitary etiologies of the sellar mass. SIGNS AND SYMPTOMS OF PITUITARY TUMORS Pituitary tumors vary in presentation. Clinical findings depend largely on whether the tumor is hormone secreting or clinically nonfunctioning, on the size and pattern of tumor growth, and on whether normal pituitary gland function is disrupted.