BCMA) As a Target for New Drug Development in Relapsed And/Or Refractory Multiple Myeloma
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

BAFF-Neutralizing Interaction of Belimumab Related to Its Therapeutic Efficacy for Treating Systemic Lupus Erythematosus
ARTICLE DOI: 10.1038/s41467-018-03620-2 OPEN BAFF-neutralizing interaction of belimumab related to its therapeutic efficacy for treating systemic lupus erythematosus Woori Shin1, Hyun Tae Lee1, Heejin Lim1, Sang Hyung Lee1, Ji Young Son1, Jee Un Lee1, Ki-Young Yoo1, Seong Eon Ryu2, Jaejun Rhie1, Ju Yeon Lee1 & Yong-Seok Heo1 1234567890():,; BAFF, a member of the TNF superfamily, has been recognized as a good target for auto- immune diseases. Belimumab, an anti-BAFF monoclonal antibody, was approved by the FDA for use in treating systemic lupus erythematosus. However, the molecular basis of BAFF neutralization by belimumab remains unclear. Here our crystal structure of the BAFF–belimumab Fab complex shows the precise epitope and the BAFF-neutralizing mechanism of belimumab, and demonstrates that the therapeutic activity of belimumab involves not only antagonizing the BAFF–receptor interaction, but also disrupting the for- mation of the more active BAFF 60-mer to favor the induction of the less active BAFF trimer through interaction with the flap region of BAFF. In addition, the belimumab HCDR3 loop mimics the DxL(V/L) motif of BAFF receptors, thereby binding to BAFF in a similar manner as endogenous BAFF receptors. Our data thus provides insights for the design of new drugs targeting BAFF for the treatment of autoimmune diseases. 1 Department of Chemistry, Konkuk University, 120 Neungdong-ro, Gwangjin-gu, Seoul 05029, Republic of Korea. 2 Department of Bio Engineering, Hanyang University, 222 Wangsimni-ro, Seongdong-gu, Seoul 04763, Republic of Korea. These authors contributed equally: Woori Shin, Hyun Tae Lee, Heejin Lim, Sang Hyung Lee. -

Monoclonal Antibody: a New Treatment Strategy Against Multiple Myeloma
antibodies Review Monoclonal Antibody: A New Treatment Strategy against Multiple Myeloma Shih-Feng Cho 1,2,3, Liang Lin 3, Lijie Xing 3,4, Tengteng Yu 3, Kenneth Wen 3, Kenneth C. Anderson 3 and Yu-Tzu Tai 3,* 1 Division of Hematology & Oncology, Department of Internal Medicine, Kaohsiung Medical University Hospital, Kaohsiung Medical University, Kaohsiung 807, Taiwan; [email protected] 2 Faculty of Medicine, College of Medicine, Kaohsiung Medical University, Kaohsiung 807, Taiwan 3 LeBow Institute for Myeloma Therapeutics and Jerome Lipper Multiple Myeloma Center, Dana-Farber Cancer Institute, Harvard Medical School, Boston, MA 02215, USA; [email protected] (L.L.); [email protected] (L.X.); [email protected] (T.Y.); [email protected] (K.W.); [email protected] (K.C.A.) 4 Department of Hematology, Shandong Provincial Hospital Affiliated to Shandong University, No. 324, Jingwu Road, Jinan 250021, China * Correspondence: [email protected]; Tel.: +1-617-632-3875; Fax: +1-617-632-2140 Received: 20 October 2017; Accepted: 10 November 2017; Published: 14 November 2017 Abstract: 2015 was a groundbreaking year for the multiple myeloma community partly due to the breakthrough approval of the first two monoclonal antibodies in the treatment for patients with relapsed and refractory disease. Despite early disappointments, monoclonal antibodies targeting CD38 (daratumumab) and signaling lymphocytic activation molecule F7 (SLAMF7) (elotuzumab) have become available for patients with multiple myeloma in the same year. Specifically, phase 3 clinical trials of combination therapies incorporating daratumumab or elotuzumab indicate both efficacy and a very favorable toxicity profile. These therapeutic monoclonal antibodies for multiple myeloma can kill target cells via antibody-dependent cell-mediated cytotoxicity, complement-dependent cytotoxicity, and antibody-dependent phagocytosis, as well as by direct blockade of signaling cascades. -

Blincyto Pi Hcp English.Pdf
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use BLINCYTO® safely and effectively. See full prescribing information for BLINCYTO. - Premedicate with dexamethasone. (2.2) BLINCYTO® (blinatumomab) for injection, for intravenous use • Refer to Full Prescribing Information for important preparation and Initial U.S. Approval: 2014 administration information. (2.4, 2.5, 2.6) • Administer as a continuous intravenous infusion at a constant flow rate using an infusion pump. (2.5, 2.6) WARNING: CYTOKINE RELEASE SYNDROME and - See Section 2.5 for infusion over 24 hours or 48 hours. NEUROLOGICAL TOXICITIES - See Section 2.6 for infusion over 7 days using Bacteriostatic 0.9% See full prescribing information for complete boxed warning. Sodium Chloride Injection, USP (containing 0.9% benzyl alcohol). This option is not recommended for patients weighing less than 22 kg. • Cytokine Release Syndrome (CRS), which may be life-threatening or fatal, occurred in patients receiving BLINCYTO. Interrupt or ---------------------DOSAGE FORMS AND STRENGTHS---------------------- discontinue BLINCYTO and treat with corticosteroids as For injection: 35 mcg of lyophilized powder in a single-dose vial for recommended. (2.3, 5.1) reconstitution. (3) • Neurological toxicities, which may be severe, life-threatening, or fatal, occurred in patients receiving BLINCYTO. Interrupt or discontinue -------------------------------CONTRAINDICATIONS------------------------------ BLINCYTO as recommended. (2.3, 5.2) Known hypersensitivity -

BCMA-Targeted Immunotherapy for Multiple Myeloma Bo Yu1, Tianbo Jiang2 and Delong Liu2*
Yu et al. Journal of Hematology & Oncology (2020) 13:125 https://doi.org/10.1186/s13045-020-00962-7 REVIEW Open Access BCMA-targeted immunotherapy for multiple myeloma Bo Yu1, Tianbo Jiang2 and Delong Liu2* Abstract B cell maturation antigen (BCMA) is a novel treatment target for multiple myeloma (MM) due to its highly selective expression in malignant plasma cells (PCs). Multiple BCMA-targeted therapeutics, including antibody-drug conjugates (ADC), chimeric antigen receptor (CAR)-T cells, and bispecific T cell engagers (BiTE), have achieved remarkable clinical response in patients with relapsed and refractory MM. Belantamab mafodotin-blmf (GSK2857916), a BCMA-targeted ADC, has just been approved for highly refractory MM. In this article, we summarized the molecular and physiological properties of BCMA as well as BCMA-targeted immunotherapeutic agents in different stages of clinical development. Keywords: B cell maturation antigen, BCMA, Belantamab mafodotin, CAR-T, Antibody-drug conjugate, Bispecific T cell engager Introduction B cell maturation antigen (BCMA) Recent advances in novel therapeutics such as prote- BCMA is encoded by a 2.92-kb TNFRSF17 gene located asome inhibitors (PI) and immunomodulatory drugs on the short arm of chromosome 16 (16p13.13) and (IMiD) have significantly improved the treatment out- composed of 3 exons separated by 2 introns (Fig. 1). comes in patients with multiple myeloma (MM) [1–8]. BCMA is a 184 amino acid and 20.2-kDa type III trans- However, most MM patients eventually relapse due to membrane glycoprotein, with the extracellular N the development of drug resistance [9]. In addition, terminus containing a conserved motif of 6 cysteines many of the current popular target antigens, such as [18–21]. -

The Potential of Adoptive Transfer of Γ9δ2 T Cells to Enhance
www.nature.com/scientificreports OPEN The potential of adoptive transfer of γ9δ2 T cells to enhance blinatumomab’s antitumor activity against B‑cell malignancy Yun‑Hsiang Chen1, Yun Wang2, Cheng‑Hao Liao3 & Shu‑Ching Hsu4,5,6,7,8,9* Blinatumomab, a bispecifc T cell engager (BiTE) antibody targeting CD19 and CD3ε, can redirect T cells toward CD19‑positive tumor cells and has been approved to treat relapsed/refractory B‑cell acute lymphoblastic leukemia (R/R B‑ALL). However, chemotherapeutic regimens can severely reduce T cells’ number and cytotoxic function, leading to an inadequate response to blinatumomab treatment in patients. In addition, it was reported that a substantial portion of R/R B‑ALL patients failing blinatumomab treatment had the extramedullary disease, indicating the poor ability of blinatumomab in treating extramedullary disease. In this study, we investigated whether the adoptive transfer of ex vivo expanded γ9δ2 T cells could act as the efector of blinatumomab to enhance blinatumomab’s antitumor activity against B‑cell malignancies in vivo. Repeated infusion of blinatumomab and human γ9δ2 T cells led to more prolonged survival than that of blinatumomab or human γ9δ2 T cells alone in the mice xenografted with Raji cells. Furthermore, adoptive transfer of γ9δ2 T cells reduced tumor mass outside the bone marrow, indicating the potential of γ9δ2 T cells to eradicate the extramedullary disease. Our results suggest that the addition of γ9δ2 T cells to the blinatumomab treatment regimens could be an efective approach to enhancing blinatumomab’s therapeutic efcacy. The concept of this strategy may also be applied to other antigen‑specifc BiTE therapies for other malignancies. -

Targeting BAFF and APRIL in Systemic Lupus Erythemathosis a Comparison of Trials of Three BAFF/APRIL Inhibitors
Targeting BAFF and APRIL in Systemic Lupus Erythemathosis A comparison of trials of three BAFF/APRIL inhibitors Figure 1: B-cell targeting therapies to treat systemic lupus erythemathosis (1) Abstract: Systemic Lupus Erythemathosis (SLE) is a complex autoimmune disease. Diagnosis and prognosis are difficult and have a lot of confounders. Progress of the disease is thus followed by a number of measures, such as damage indices like SELENA/SLEDAI and BILAG, B-cell numbers, immunoglobulin levels, in particular autoantibodies such as anti-dsDNA antibodies, and complement C3 and C4 levels. B-cell proliferation and activation are overstimulated in SLE, particularly through the BAFF/APRIL stimulated pathways. A number of BAFF/APRIL targeting biologicals have been approved for use in treatment of SLE or are currently in clinical trials. Three of these are highlighted here: Belimumab, Blisibimod and Atacicept. Belimumab, a fully humanized anti-BAFF antibody, is already approved by the USFDA. In clinical studies it has been show to lower the damage index, B-cell numbers and immunoglobulin levels, it increases complement levels and may reduce the need for steroids. Blisibimod, a synthetic peptibody, is in stage II trials. Like Belimumab, Blisbimod lowers the damage index and B-cell numbers, increases complement levels and may reduce the need for steroids. Ataticept, a fusion protein, is in stage III trials. Atacicept also lowers the damage index, B-cell numbers and immunoglobulin levels, increases complement and may reduce the need for steroids. The differences are relatively small and to determine the most promising of these treatments close attention has to be paid to the data from trials. -

An Update on the Current State of Management and Clinical Trials for Iga Nephropathy
Journal of Clinical Medicine Review An Update on the Current State of Management and Clinical Trials for IgA Nephropathy Chee Kay Cheung 1,2 , Arun Rajasekaran 3 , Jonathan Barratt 1,2,† and Dana V. Rizk 3,*,† 1 Department of Cardiovascular Sciences, University of Leicester, Leicester LE1 7RH, UK; [email protected] (C.K.C.); [email protected] (J.B.) 2 John Walls Renal Unit, University Hospitals of Leicester NHS Trust, Leicester LE5 4PW, UK 3 Division of Nephrology, Department of Medicine, University of Alabama at Birmingham, ZRB 614, 1720 2nd Avenue South, Birmingham, AL 35294, USA; [email protected] * Correspondence: [email protected] † Both authors contributed equally to this work. Abstract: IgA nephropathy remains the most common primary glomerular disease worldwide. It affects children and adults of all ages, and is a leading cause of end-stage kidney disease, making it a considerable public health issue in many countries. Despite being initially described over 50 years ago, there are still no disease specific treatments, with current management for most patients being focused on lifestyle measures and renin-angiotensin-aldosterone system blockade. However, significant advances in the understanding of its pathogenesis have been made particularly over the past decade, leading to great interest in developing new therapeutic strategies, and a significant rise in the number of interventional clinical trials being performed. In this review, we will summarise the current state of management of IgAN, and then describe major areas of interest where new therapies are at their most advanced stages of development, that include the gut mucosal immune system, B cell signalling, the complement system and non-immune modulators. -

High Risk Therapy Made Easy: Supporting High Risk Patients Through Complex Therapy
8/21/2018 High Risk Therapy Made Easy: Supporting high risk patients through complex therapy Lori Ranney, MSN, APRN, CPNP, CPHON Mylynda Livingston, MSN, APRN, AC PC-PNP, CPON Teresa Herriage, DNP, APRN, CPNP, CPHON Children’s Minnesota Disclaimers and Confidentiality Protections Children’s Minnesota makes no representations or warranties about the accuracy, reliability, or completeness of the content. Content is provided “as is” and is for informational use only. It is not a substitute for professional medical advice, diagnosis, or treatment. Children’s disclaims all warranties, express or implied, statutory or otherwise, including without limitation the implied warranties of merchantability, non-infringement of third parties’ rights, and fitness for a particular purpose. This content was developed for use in Children’s patient care environment and may not be suitable for use in other patient care environments. Children’s does not endorse, certify, or assess third parties’ competency. You hold all responsibility for your use or nonuse of the content. Children’s shall not be liable for claims, losses, or damages arising from or related to any use or misuse of the content. This content and its related discussions are privileged and confidential under Minnesota’s peer review statute (Minn. Stat. § 145.61 et. seq.). Do not disclose unless appropriately authorized. Notwithstanding the foregoing, content may be subject to copyright or trademark law; use of such information requires Children’s permission. This content may include patient protected health information. You agree to comply with all applicable state and federal laws protecting patient privacy and security including the Minnesota Health Records Act and the Health Insurance Portability and Accountability Act and its implementing regulations as amended from time to time. -

The Future of B-Cell Activating Factor Antagonists in the Treatment of Systemic Lupus Erythematosus
pISSN: 2093-940X, eISSN: 2233-4718 Journal of Rheumatic Diseases Vol. 24, No. 2, April, 2017 https://doi.org/10.4078/jrd.2017.24.2.65 Review Article The Future of B-cell Activating Factor Antagonists in the Treatment of Systemic Lupus Erythematosus William Stohl Division of Rheumatology, Department of Medicine, University of Southern California Keck School of Medicine, Los Angeles, CA, USA To review B-cell activating factor (BAFF)-antagonist therapy in systemic lupus erythematosus (SLE), literature was searched us- ing the search words and phrases, “BAFF”, “B lymphocyte stimulator (BLyS)”, “a proliferation-inducing ligand (APRIL)”, “B-cell maturation antigen (BCMA)”, “transmembrane activator and calcium-modulating and cyclophilin ligand interactor (TACI)”, “BLyS receptor 3 (BR3)”, “belimumab”, “atacicept”, “blisibimod”, “tabalumab”, and “lupus clinical trial”. In addition, papers from the author’s personal library were searched. BAFF-antagonist therapy in SLE has a checkered past, with four late-stage clin- ical trials meeting their primary endpoints and four failing to do so. Additional late-stage clinical trials are enrolling subjects to address some of the remaining unresolved questions, and novel approaches are proposed to improve results. The BAFF-centric pathway is a proven therapeutic target in SLE. As the only pathway in the past 50+ years to have yielded an United States Food and Drug Administration-approved drug for SLE, it occupies a unique place in the armamentarium of the practicing rheumatologist. The challenges facing clinicians and investigators are how to better tweak the BAFF-centric pathway and im- prove on the successes realized. (J Rheum Dis 2017;24:65-73) Key Words. -

BAFF Suppresses IL-15 Expression in B Cells
BAFF Suppresses IL-15 Expression in B Cells Ning Ma, Chen Xing, He Xiao, Youdi He, Gencheng Han, Guojiang Chen, Chunmei Hou, Bernadette Marrero, Yujuan Wang, Shengquan Zhang, Beifen Shen, Yan Li and Renxi This information is current as Wang of September 28, 2021. J Immunol 2014; 192:4192-4201; Prepublished online 26 March 2014; doi: 10.4049/jimmunol.1302132 http://www.jimmunol.org/content/192/9/4192 Downloaded from Supplementary http://www.jimmunol.org/content/suppl/2014/03/26/jimmunol.130213 Material 2.DCSupplemental http://www.jimmunol.org/ References This article cites 39 articles, 14 of which you can access for free at: http://www.jimmunol.org/content/192/9/4192.full#ref-list-1 Why The JI? Submit online. • Rapid Reviews! 30 days* from submission to initial decision by guest on September 28, 2021 • No Triage! Every submission reviewed by practicing scientists • Fast Publication! 4 weeks from acceptance to publication *average Subscription Information about subscribing to The Journal of Immunology is online at: http://jimmunol.org/subscription Permissions Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html Email Alerts Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts The Journal of Immunology is published twice each month by The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. The Journal of Immunology BAFF Suppresses IL-15 Expression in B Cells Ning Ma,*,†,1 Chen Xing,*,1 He Xiao,*,1 Youdi He,‡ Gencheng Han,* Guojiang Chen,* Chunmei Hou,* Bernadette Marrero,x Yujuan Wang,{ Shengquan Zhang,‖ Beifen Shen,* Yan Li,* and Renxi Wang* Clinical trials have shown that BAFF inhibitors do not reduce memory B cell levels but can reduce the number of mature B cells. -
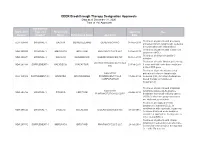
CDER Breakthrough Therapy Designation Approvals Data As of December 31, 2020 Total of 190 Approvals
CDER Breakthrough Therapy Designation Approvals Data as of December 31, 2020 Total of 190 Approvals Submission Application Type and Proprietary Approval Use Number Number Name Established Name Applicant Date Treatment of patients with previously BLA 125486 ORIGINAL-1 GAZYVA OBINUTUZUMAB GENENTECH INC 01-Nov-2013 untreated chronic lymphocytic leukemia in combination with chlorambucil Treatment of patients with mantle cell NDA 205552 ORIGINAL-1 IMBRUVICA IBRUTINIB PHARMACYCLICS LLC 13-Nov-2013 lymphoma (MCL) Treatment of chronic hepatitis C NDA 204671 ORIGINAL-1 SOVALDI SOFOSBUVIR GILEAD SCIENCES INC 06-Dec-2013 infection Treatment of cystic fibrosis patients age VERTEX PHARMACEUTICALS NDA 203188 SUPPLEMENT-4 KALYDECO IVACAFTOR 21-Feb-2014 6 years and older who have mutations INC in the CFTR gene Treatment of previously untreated NOVARTIS patients with chronic lymphocytic BLA 125326 SUPPLEMENT-60 ARZERRA OFATUMUMAB PHARMACEUTICALS 17-Apr-2014 leukemia (CLL) for whom fludarabine- CORPORATION based therapy is considered inappropriate Treatment of patients with anaplastic NOVARTIS lymphoma kinase (ALK)-positive NDA 205755 ORIGINAL-1 ZYKADIA CERITINIB 29-Apr-2014 PHARMACEUTICALS CORP metastatic non-small cell lung cancer (NSCLC) who have progressed on or are intolerant to crizotinib Treatment of relapsed chronic lymphocytic leukemia (CLL), in combination with rituximab, in patients NDA 206545 ORIGINAL-1 ZYDELIG IDELALISIB GILEAD SCIENCES INC 23-Jul-2014 for whom rituximab alone would be considered appropriate therapy due to other co-morbidities -

5.01.582 Antibody-Drug Conjugates
MEDICAL POLICY – 5.01.582 Antibody-Drug Conjugates Effective Date: June 1, 2021 RELATED MEDICAL POLICIES: Last Revised: May 11, 2021 None Replaces: N/A Select a hyperlink below to be directed to that section. POLICY CRITERIA | CODING | RELATED INFORMATION EVIDENCE REVIEW | REFERENCES | HISTORY ∞ Clicking this icon returns you to the hyperlinks menu above. Introduction An antibody is a blood protein. When the immune system detects an unhealthy cell, antibodies link to a molecule, known as an antigen, on the unhealthy cell. Monoclonal antibodies are produced in a laboratory. They are made to link to antigens usually found in high numbers on cancer cells. Antibody-drug conjugates combine monoclonal antibodies with certain chemotherapy drugs. The monoclonal antibodies find the cancer cells and the chemotherapy drug is released directly into those cells. The goal with this treatment is to target only cancer cells and spare nearby healthy cells. This policy describes when specific antibody-drug conjugates may be considered medically necessary. Note: The Introduction section is for your general knowledge and is not to be taken as policy coverage criteria. The rest of the policy uses specific words and concepts familiar to medical professionals. It is intended for providers. A provider can be a person, such as a doctor, nurse, psychologist, or dentist. A provider also can be a place where medical care is given, like a hospital, clinic, or lab. This policy informs them about when a service may be covered. Policy Coverage Criteria Drug Medical