Activated and Exhausted MAIT Cells Foster Disease Progression and Indicate
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

ENSG Gene Encodes Effector TCR Pathway Costimulation Inhibitory/Exhaustion Synapse/Adhesion Chemokines/Receptors
ENSG Gene Encodes Effector TCR pathway Costimulation Inhibitory/exhaustion Synapse/adhesion Chemokines/receptors ENSG00000111537 IFNG IFNg x ENSG00000109471 IL2 IL-2 x ENSG00000232810 TNF TNFa x ENSG00000271503 CCL5 CCL5 x x ENSG00000139187 KLRG1 Klrg1 x ENSG00000117560 FASLG Fas ligand x ENSG00000121858 TNFSF10 TRAIL x ENSG00000134545 KLRC1 Klrc1 / NKG2A x ENSG00000213809 KLRK1 Klrk1 / NKG2D x ENSG00000188389 PDCD1 PD-1 x x ENSG00000117281 CD160 CD160 x x ENSG00000134460 IL2RA IL-2 receptor x subunit alpha ENSG00000110324 IL10RA IL-10 receptor x subunit alpha ENSG00000115604 IL18R1 IL-18 receptor 1 x ENSG00000115607 IL18RAP IL-18 receptor x accessory protein ENSG00000081985 IL12RB2 IL-12 receptor x beta 2 ENSG00000186810 CXCR3 CXCR3 x x ENSG00000005844 ITGAL CD11a x ENSG00000160255 ITGB2 CD18; Integrin x x beta-2 ENSG00000156886 ITGAD CD11d x ENSG00000140678 ITGAX; CD11c x x Integrin alpha-X ENSG00000115232 ITGA4 CD49d; Integrin x x alpha-4 ENSG00000169896 ITGAM CD11b; Integrin x x alpha-M ENSG00000138378 STAT4 Stat4 x ENSG00000115415 STAT1 Stat1 x ENSG00000170581 STAT2 Stat2 x ENSG00000126561 STAT5a Stat5a x ENSG00000162434 JAK1 Jak1 x ENSG00000100453 GZMB Granzyme B x ENSG00000145649 GZMA Granzyme A x ENSG00000180644 PRF1 Perforin 1 x ENSG00000115523 GNLY Granulysin x ENSG00000100450 GZMH Granzyme H x ENSG00000113088 GZMK Granzyme K x ENSG00000057657 PRDM1 Blimp-1 x ENSG00000073861 TBX21 T-bet x ENSG00000115738 ID2 ID2 x ENSG00000176083 ZNF683 Hobit x ENSG00000137265 IRF4 Interferon x regulatory factor 4 ENSG00000140968 IRF8 Interferon -

Cd160 Mouse Shrna Plasmid (Locus ID 54215) – TR514223 | Origene
OriGene Technologies, Inc. 9620 Medical Center Drive, Ste 200 Rockville, MD 20850, US Phone: +1-888-267-4436 [email protected] EU: [email protected] CN: [email protected] Product datasheet for TR514223 Cd160 Mouse shRNA Plasmid (Locus ID 54215) Product data: Product Type: shRNA Plasmids Product Name: Cd160 Mouse shRNA Plasmid (Locus ID 54215) Locus ID: 54215 Synonyms: AU045688; By55 Vector: pRS (TR20003) Format: Retroviral plasmids Components: Cd160 - Mouse, 4 unique 29mer shRNA constructs in retroviral untagged vector(Gene ID = 54215). 5µg purified plasmid DNA per construct Non-effective 29-mer scrambled shRNA cassette in pRS Vector, TR30012, included for free. RefSeq: BC021596, NM_001163496, NM_001163497, NM_018767 Summary: CD160 antigen: Receptor on immune cells capable to deliver stimulatory or inhibitory signals that regulate cell activation and differentiation. Exists as a GPI-anchored and as a transmembrane form, each likely initiating distinct signaling pathways via phosphoinositol 3- kinase in activated NK cells and via LCK and CD247/CD3 zeta chain in activated T cells (By similarity). Receptor for both classical and non-classical MHC class I molecules (PubMed:16177084). Receptor or ligand for TNF superfamily member TNFRSF14, participating in bidirectional cell-cell contact signaling between antigen presenting cells and lymphocytes. Upon ligation of TNFRSF14, provides stimulatory signal to NK cells enhancing IFNG production and anti-tumor immune response (PubMed:25711213). On activated CD4+ T cells, interacts with TNFRSF14 and downregulates CD28 costimulatory signaling, restricting memory and alloantigen-specific immune response (By similarity). In the context of bacterial infection, acts as a ligand for TNFRSF14 on epithelial cells, triggering the production of antimicrobial proteins and proinflammatory cytokines (PubMed:22801499).[UniProtKB/Swiss-Prot Function] shRNA Design: These shRNA constructs were designed against multiple splice variants at this gene locus. -

Human and Mouse CD Marker Handbook Human and Mouse CD Marker Key Markers - Human Key Markers - Mouse
Welcome to More Choice CD Marker Handbook For more information, please visit: Human bdbiosciences.com/eu/go/humancdmarkers Mouse bdbiosciences.com/eu/go/mousecdmarkers Human and Mouse CD Marker Handbook Human and Mouse CD Marker Key Markers - Human Key Markers - Mouse CD3 CD3 CD (cluster of differentiation) molecules are cell surface markers T Cell CD4 CD4 useful for the identification and characterization of leukocytes. The CD CD8 CD8 nomenclature was developed and is maintained through the HLDA (Human Leukocyte Differentiation Antigens) workshop started in 1982. CD45R/B220 CD19 CD19 The goal is to provide standardization of monoclonal antibodies to B Cell CD20 CD22 (B cell activation marker) human antigens across laboratories. To characterize or “workshop” the antibodies, multiple laboratories carry out blind analyses of antibodies. These results independently validate antibody specificity. CD11c CD11c Dendritic Cell CD123 CD123 While the CD nomenclature has been developed for use with human antigens, it is applied to corresponding mouse antigens as well as antigens from other species. However, the mouse and other species NK Cell CD56 CD335 (NKp46) antibodies are not tested by HLDA. Human CD markers were reviewed by the HLDA. New CD markers Stem Cell/ CD34 CD34 were established at the HLDA9 meeting held in Barcelona in 2010. For Precursor hematopoetic stem cell only hematopoetic stem cell only additional information and CD markers please visit www.hcdm.org. Macrophage/ CD14 CD11b/ Mac-1 Monocyte CD33 Ly-71 (F4/80) CD66b Granulocyte CD66b Gr-1/Ly6G Ly6C CD41 CD41 CD61 (Integrin b3) CD61 Platelet CD9 CD62 CD62P (activated platelets) CD235a CD235a Erythrocyte Ter-119 CD146 MECA-32 CD106 CD146 Endothelial Cell CD31 CD62E (activated endothelial cells) Epithelial Cell CD236 CD326 (EPCAM1) For Research Use Only. -

Tools for Cell Therapy and Immunoregulation
RnDSy-lu-2945 Tools for Cell Therapy and Immunoregulation Target Cell TIM-4 SLAM/CD150 BTNL8 PD-L2/B7-DC B7-H1/PD-L1 (Human) Unknown PD-1 B7-1/CD80 TIM-1 SLAM/CD150 Receptor TIM Family SLAM Family Butyrophilins B7/CD28 Families T Cell Multiple Co-Signaling Molecules Co-stimulatory Co-inhibitory Ig Superfamily Regulate T Cell Activation Target Cell T Cell Target Cell T Cell B7-1/CD80 B7-H1/PD-L1 T cell activation requires two signals: 1) recognition of the antigenic peptide/ B7-1/CD80 B7-2/CD86 CTLA-4 major histocompatibility complex (MHC) by the T cell receptor (TCR) and 2) CD28 antigen-independent co-stimulation induced by interactions between B7-2/CD86 B7-H1/PD-L1 B7-1/CD80 co-signaling molecules expressed on target cells, such as antigen-presenting PD-L2/B7-DC PD-1 ICOS cells (APCs), and their T cell-expressed receptors. Engagement of the TCR in B7-H2/ICOS L 2Ig B7-H3 (Mouse) the absence of this second co-stimulatory signal typically results in T cell B7-H1/PD-L1 B7/CD28 Families 4Ig B7-H3 (Human) anergy or apoptosis. In addition, T cell activation can be negatively regulated Unknown Receptors by co-inhibitory molecules present on APCs. Therefore, integration of the 2Ig B7-H3 Unknown B7-H4 (Mouse) Receptors signals transduced by co-stimulatory and co-inhibitory molecules following TCR B7-H5 4Ig B7-H3 engagement directs the outcome and magnitude of a T cell response Unknown Ligand (Human) B7-H5 including the enhancement or suppression of T cell proliferation, B7-H7 Unknown Receptor differentiation, and/or cytokine secretion. -

Molecular Profile of Tumor-Specific CD8+ T Cell Hypofunction in a Transplantable Murine Cancer Model
Downloaded from http://www.jimmunol.org/ by guest on September 25, 2021 T + is online at: average * The Journal of Immunology , 34 of which you can access for free at: 2016; 197:1477-1488; Prepublished online 1 July from submission to initial decision 4 weeks from acceptance to publication 2016; doi: 10.4049/jimmunol.1600589 http://www.jimmunol.org/content/197/4/1477 Molecular Profile of Tumor-Specific CD8 Cell Hypofunction in a Transplantable Murine Cancer Model Katherine A. Waugh, Sonia M. Leach, Brandon L. Moore, Tullia C. Bruno, Jonathan D. Buhrman and Jill E. Slansky J Immunol cites 95 articles Submit online. Every submission reviewed by practicing scientists ? is published twice each month by Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts http://jimmunol.org/subscription Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html http://www.jimmunol.org/content/suppl/2016/07/01/jimmunol.160058 9.DCSupplemental This article http://www.jimmunol.org/content/197/4/1477.full#ref-list-1 Information about subscribing to The JI No Triage! Fast Publication! Rapid Reviews! 30 days* Why • • • Material References Permissions Email Alerts Subscription Supplementary The Journal of Immunology The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 Copyright © 2016 by The American Association of Immunologists, Inc. All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. This information is current as of September 25, 2021. The Journal of Immunology Molecular Profile of Tumor-Specific CD8+ T Cell Hypofunction in a Transplantable Murine Cancer Model Katherine A. -

Transcriptional Control of Tissue-Resident Memory T Cell Generation
Transcriptional control of tissue-resident memory T cell generation Filip Cvetkovski Submitted in partial fulfillment of the requirements for the degree of Doctor of Philosophy in the Graduate School of Arts and Sciences COLUMBIA UNIVERSITY 2019 © 2019 Filip Cvetkovski All rights reserved ABSTRACT Transcriptional control of tissue-resident memory T cell generation Filip Cvetkovski Tissue-resident memory T cells (TRM) are a non-circulating subset of memory that are maintained at sites of pathogen entry and mediate optimal protection against reinfection. Lung TRM can be generated in response to respiratory infection or vaccination, however, the molecular pathways involved in CD4+TRM establishment have not been defined. Here, we performed transcriptional profiling of influenza-specific lung CD4+TRM following influenza infection to identify pathways implicated in CD4+TRM generation and homeostasis. Lung CD4+TRM displayed a unique transcriptional profile distinct from spleen memory, including up-regulation of a gene network induced by the transcription factor IRF4, a known regulator of effector T cell differentiation. In addition, the gene expression profile of lung CD4+TRM was enriched in gene sets previously described in tissue-resident regulatory T cells. Up-regulation of immunomodulatory molecules such as CTLA-4, PD-1, and ICOS, suggested a potential regulatory role for CD4+TRM in tissues. Using loss-of-function genetic experiments in mice, we demonstrate that IRF4 is required for the generation of lung-localized pathogen-specific effector CD4+T cells during acute influenza infection. Influenza-specific IRF4−/− T cells failed to fully express CD44, and maintained high levels of CD62L compared to wild type, suggesting a defect in complete differentiation into lung-tropic effector T cells. -
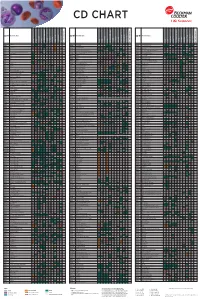
Flow Reagents Single Color Antibodies CD Chart
CD CHART CD N° Alternative Name CD N° Alternative Name CD N° Alternative Name Beckman Coulter Clone Beckman Coulter Clone Beckman Coulter Clone T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells CD1a T6, R4, HTA1 Act p n n p n n S l CD99 MIC2 gene product, E2 p p p CD223 LAG-3 (Lymphocyte activation gene 3) Act n Act p n CD1b R1 Act p n n p n n S CD99R restricted CD99 p p CD224 GGT (γ-glutamyl transferase) p p p p p p CD1c R7, M241 Act S n n p n n S l CD100 SEMA4D (semaphorin 4D) p Low p p p n n CD225 Leu13, interferon induced transmembrane protein 1 (IFITM1). p p p p p CD1d R3 Act S n n Low n n S Intest CD101 V7, P126 Act n p n p n n p CD226 DNAM-1, PTA-1 Act n Act Act Act n p n CD1e R2 n n n n S CD102 ICAM-2 (intercellular adhesion molecule-2) p p n p Folli p CD227 MUC1, mucin 1, episialin, PUM, PEM, EMA, DF3, H23 Act p CD2 T11; Tp50; sheep red blood cell (SRBC) receptor; LFA-2 p S n p n n l CD103 HML-1 (human mucosal lymphocytes antigen 1), integrin aE chain S n n n n n n n l CD228 Melanotransferrin (MT), p97 p p CD3 T3, CD3 complex p n n n n n n n n n l CD104 integrin b4 chain; TSP-1180 n n n n n n n p p CD229 Ly9, T-lymphocyte surface antigen p p n p n -

Haematopoiesis During Native Conditions and Immune Thrombocytopenia Progression
Haematopoiesis During Native Conditions and Immune Thrombocytopenia Progression Oliver Herd Doctor of Philosophy University of York Biology March 2021 i Abstract The maintenance of haematopoietic stem cell (HSC) self-renewal and differentiation throughout life is essential for ongoing haematopoiesis and is highly dependent upon cytokine-cytokine receptor interactions and direct cell-cell contact between the HSC and components of the perivascular bone marrow (BM) microenvironment. Thrombopoietin (TPO) is one of two such cytokines essential for HSC self-renewal. Although the majority of TPO is produced distally by the liver, lower amounts of TPO are thought to be produced locally in the BM, directly at the site of utilisation. However, the exact cellular sources of BM derived TPO are unclear and remains an active area of research. Contrary to previous studies, the results in this thesis indicate that megakaryocytes do not express Thpo, and instead LepR+/Cxcl12-DsRedhigh BM stromal cells (BMSCs) are major sources of Thpo in mice. Immune thrombocytopenia (ITP) is an acquired autoimmune condition characterised by reduced platelet production and increased platelet destruction by sustained immune attack. In this thesis, a novel mouse model of sustained ITP was generated and the effect on the immune and haematopoietic system was assessed. Platelet destruction was antibody dependent and appeared to be primarily driven by splenic macrophages. Additionally, ITP progression was associated with considerable progenitor expansion and BM remodelling. Single cell assays using Lin-Sca1+c-Kit+CD48-CD150+ long-term HSCs (LT-HSCs) revealed elevated LT-HSC activation and proliferation in vitro. However, LT-HSC functionality was maintained as measured by in vivo serial transplantations. -

Role for Expression of CD200 in Multiparameter Flow Cytometric Differential Diagnosis of Mature B-Cell Neoplasms
Editorial Page 1 of 4 Role for expression of CD200 in multiparameter flow cytometric differential diagnosis of mature B-cell neoplasms Reginald M. Gorczynski1,2 1Department of Immunology, Faculty of Medicine, University of Toronto, Toronto, ON, Canada; 2Institute of Medical Science, University of Toronto, Toronto, ON, Canada Correspondence to: Reginald M. Gorczynski, MD, PhD. Department of Immunology, Faculty of Medicine, University of Toronto, Toronto, ON, Canada. Email: [email protected]. Provenance: This is a Guest Editorial commissioned by the Section Editor Baohong Yue (Hematology lab in Department of Clinical Laboratory Medicine, The First Affiliated Hospital, College of Medicine, Zhengzhou University, Zhengzhou, China). Comment on: Sandes AF, de Lourdes Chauffaille M, Oliveira CR, et al. CD200 has an important role in the differential diagnosis of mature B-cell neoplasms by multiparameter flow cytometry. Cytometry B Clin Cytom 2014;86:98-105. Received: 01 July 2017; Accepted: 24 July 2017; Published: 09 August 2017. doi: 10.21037/jlpm.2017.07.14 View this article at: http://dx.doi.org/ 10.21037/jlpm.2017.07.14 Introduction in differential diagnosis. Analysis of CD200 expression seems to fulfill just this need, as indicated in previous This issue of the journal includes an important study by reports of its expression in typical CLL and MCL (5-8). Sandes et al. (1), which explores whether inclusion of The study by Sandes et al. confirmed this analysis in analysis of CD200 expression can contribute to improved other cases of MBN, and includes atypical CLL cases for classification of mature B cell neoplasms (MBN). Currently, comparison also. -

Expanded Antigen-Experienced CD160+CD8+Effector T Cells Exhibit
Open access Original research J Immunother Cancer: first published as 10.1136/jitc-2020-002189 on 30 April 2021. Downloaded from Expanded antigen- experienced CD160+CD8+effector T cells exhibit impaired effector functions in chronic lymphocytic leukemia Najmeh Bozorgmehr,1 Isobel Okoye,1 Olaide Oyegbami,1 Lai Xu,1 Amelie Fontaine,2 Nanette Cox- Kennett,2 Loree M Larratt,3 Mark Hnatiuk,3 Andrei Fagarasanu,2 3 2 1,2,4 Joseph Brandwein, Anthea C Peters, Shokrollah Elahi To cite: Bozorgmehr N, ABSTRACT BACKGROUND Okoye I, Oyegbami O, et al. Background T cell exhaustion compromises antitumor Chronic lymphocytic leukemia (CLL), the Expanded antigen- experienced immunity, and a sustained elevation of co- inhibitory + + most common leukemia among adults in CD160 CD8 effector T cells receptors is a hallmark of T cell exhaustion in solid tumors. exhibit impaired effector Western countries, is identified by the clonal Similarly, upregulation of co- inhibitory receptors has + functions in chronic lymphocytic expansion of CD5 mature B lymphocytes in leukemia. Journal for been reported in T cells in hematological cancers such as chronic lymphocytic leukemia (CLL). However, the the blood, bone marrow (BM), and secondary ImmunoTherapy of Cancer lymphoid organs.1 2 The disease fate is highly 2021;9:e002189. doi:10.1136/ role of CD160, a glycosylphosphatidylinositol-anchored jitc-2020-002189 protein, as one of these co-inhibitor y receptors has been influenced by the advanced clinical stage (ie, contradictory in T cell function. Therefore, we decided to Rai stage), the broad range of genetic factors ► Additional supplemental elucidate how CD160 expression and/or co-expression and remarkable contributions from the tumor material is published online only. -

CD200 in Hematological Malignancies: Just a Diagnostic Tool Or More?
Editorial Page 1 of 4 CD200 in hematological malignancies: just a diagnostic tool or more? Daniela Damiani, Mario Tiribelli Division of Hematology and Stem Cell Transplantation, Department of Medical Area, Azienda Sanitaria Universitaria Integrata di Udine, Udine, Italy Correspondence to: Prof. Daniela Damiani. Division of Hematology and Stem Cell Transplantation Department of Medical Area, Azienda Sanitaria Universitaria Integrata di Udine, 33100 Udine, Italy. Email: [email protected]. Provenance: This is a Guest Editorial commissioned by the Section Editor Baohong Yue (Hematology lab in Department of Clinical Laboratory Medicine, The First Affiliated Hospital, College of Medicine, Zhengzhou University, Zhengzhou, China). Comment on: Sandes AF, de Lourdes Chauffaille M, Oliveira CR, et al. CD200 has an important role in the differential diagnosis of mature B cell neoplasms by multiparameter flow cytometry. Cytometry B Clin Cytom 2014;86:98-105. Received: 28 July 2017; Accepted: 08 August 2017; Published: 15 September 2017. doi: 10.21037/jlpm.2017.08.08 View this article at: http://dx.doi.org/10.21037/jlpm.2017.08.08 Over the past two decades, the increased number of monoclonal Cytometry, Sandes and colleagues tested the diagnostic antibodies and the constantly expanding availability of utility of CD200 in differential diagnosis of 159 patients fluorescence probes significantly improved the efficiency with mature B lymphoproliferative diseases (3). They and the accuracy of flow cytometric analysis, providing not only added CD200 to a conventional MFC panel, relevant information for the diagnosis, classification and evaluating its dichotomous expression, but also compared follow up of various hematological malignancies. As a the fluorescence intensity in the tested cases, with the aim to diagnostic tool, together with morphology and molecular create a reference pool of CD200 expression intensity that genetics, flow cytometry has become a gold standard in may further discriminate within the CD200-positive group. -

Molecular Programming of Tumor-Infiltrating CD8 T Cells and IL15 Resistance
Published OnlineFirst August 2, 2016; DOI: 10.1158/2326-6066.CIR-15-0178 Research Article Cancer Immunology Research Molecular Programming of Tumor-Infiltrating CD8þ T Cells and IL15 Resistance Andrew L. Doedens1, Mark P. Rubinstein1,2, Emilie T. Gross3, J. Adam Best1, David H. Craig2, Megan K. Baker2, David J. Cole2, Jack D. Bui3, and Ananda W. Goldrath1 Abstract Despite clinical potential and recent advances, durable immu- in the lung and spleen were activated and dramatically expanded. þ notherapeutic ablation of solid tumors is not routinely achieved. Tumor-infiltrating CD8 T cells exhibited cell-extrinsic and cell- IL15expandsnaturalkillercell(NK),naturalkillerTcell(NKT)and intrinsic resistance to IL15. Our data showed that in the case of þ CD8 T-cell numbers and engages the cytotoxic program, and thus persistent viral or tumor antigen, single-agent systemic IL15cx is under evaluation for potentiation of cancer immunotherapy. We treatment primarily expanded antigen-irrelevant or extratumoral þ found that short-term therapy with IL15 bound to soluble IL15 CD8 Tcells.Weidentified exhaustion, tissue-resident memory, þ receptor a–Fc (IL15cx; a form of IL15 with increased half-life and and tumor-specific molecules expressed in tumor-infiltrating CD8 activity) was ineffective in the treatment of autochthonous PyMT T cells, which may allow therapeutic targeting or programming þ murine mammary tumors, despite abundant CD8 T-cell infiltra- of specific subsets to evade loss of function and cytokine resist- tion. Probing of this poor responsiveness revealed that IL15cx ance, and, in turn, increase the efficacy of IL2/15 adjuvant cytokine þ only weakly activated intratumoral CD8 T cells, even though cells therapy.