Principles for Health Care Reform
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Definition of a Person Under Investigation (PUI)
Definition of a Person Under Investigation (PUI) Epidemiologic Risk (Exposure) & Clinical Features Close contact^ with a person that has laboratory-confirmed Asymptomatic§ COVID-19 OR Developed one or more of the following symptoms within 14 days of last exposure: • fever* • chills • rigors • myalgia Travel to locations on the KDHE Travel Related Quarantine Table • malaise https://www.coronavirus.kdheks.gov/175/Travel-Exposure-Related- and • headache Isolation-Quaran • sore throat • lower respiratory illness (cough, shortness of breath, or difficulty breathing) • new olfactory and taste disorders • congestion or runny nose • nausea or vomiting • diarrhea without an alternate more likely diagnosis. One or more of the following symptoms: • fever* and • chills • rigors No source of exposure has been identified • myalgia • malaise • headache • sore throat • lower respiratory illness (cough, shortness of breath, or difficulty breathing) 1 | Page • new olfactory and taste disorders • congestion or runny nose • nausea or vomiting • diarrhea without an alternate more likely diagnosis. ^ You are a "close contact" if any of the following situations happened while you spent time with a person with COVID-19, even if they didn't have symptoms: • Were within 6 feet of the person for 10 consecutive minutes or more • Had contact with the person's respiratory secretions (for example, coughed or sneezed on; kissed; contact with a dirty tissue; shared a drinking glass, food, towels, or other personal items) • Live with the person or stayed overnight for at least one night in a house with the person. The chance of spreading the virus is greater the longer an infected person or persons are close to someone. -

Hospice and COVID-19
Hospice and COVID-19 For a profession whose mission is to help terminally ill patients plan their final days and guide them and their loved ones through the passage emotionally and spiritually, a global pandemic presented the ultimate challenge. ASPR TRACIE met with Sarah McSpadden, RN, MSN, MHA, President and Chief Executive Officer of The Elizabeth Hospice, to learn more about her experiences during the COVID-19 pandemic. HIGHLIGHT ASPR TRACIE Sarah, can you please tell us more about your work and the clients Related Resources you serve? COVID-19 Home-based Healthcare Sarah McSpadden (SM) and Hospice Resource Collection Our mission is to enhance the lives of those nearing the end of Engagement of Home Health life’s journey and to care for those who grieve. As a community- and Hospice Agencies in Medical based organization, we ensure that hospice care, palliative care, Surge Activities and bereavement support are available for all who face advanced Homecare and Hospice Topic serious illness. Our Elizabeth Supportive Medical Specialists provide Collection personalized medical care for adults and children who need palliative support. The Elizabeth Hospice is one of the few organizations across Medical Surge and the Role of the nation with a dedicated team specializing in perinatal and pediatric Home Health and Hospice Agencies hospice. Our comprehensive grief support program serves families from (Full Report) the community no matter how their person died or whether their person Hospice and Emergency was on service with us. Preparedness: Experiences from We were founded in 1978 when hospice was an all-volunteer program. the Field In 1982, there was a significant shift: hospice became Medicare- reimbursable and we could hire permanent staff. -

China's Health System Reform and Global Health Strategy in The
Testimony China’s Health System Reform and Global Health Strategy in the Context of COVID-19 Jennifer Bouey CT-A321-1 Testimony presented before the U.S.-China Economic and Security Review Commission on May 7, 2020. C O R P O R A T I O N For more information on this publication, visit www.rand.org/pubs/testimonies/CTA321-1.html Testimonies RAND testimonies record testimony presented or submitted by RAND associates to federal, state, or local legislative committees; government-appointed commissions and panels; and private review and oversight bodies. ChapterTitle 1 Published by the RAND Corporation, Santa Monica, Calif. © Copyright 2020 RAND Corporation RA® is a registered trademark. Limited Print and Electronic Distribution Rights This document and trademark(s) contained herein are protected by law. This representation of RAND intellectual property is provided for noncommercial use only. Unauthorized posting of this publication online is prohibited. Permission is given to duplicate this document for personal use only, as long as it is unaltered and complete. Permission is required from RAND to reproduce, or reuse in another form, any of its research documents for commercial use. For information on reprint and linking permissions, please visit www.rand.org/pubs/permissions.html. www.rand.org China’s Health System Reform and Global Health Strategy in the Context of COVID-19 Testimony of Jennifer Bouey1 The RAND Corporation2 Before the U.S.-China Economic and Security Review Commission May 7, 2020 hairman Cleveland, Commissioner Lee, and members of the Commission, thank you for inviting me to assess China’s pandemic-related issues regarding its public health C system, health care system, and global health strategy in the context of COVID-19. -

The French Health Care System
The french health care system The french health care system VICTOR RODWIN PROFESSOR OF HEALTH POLICY AND MANAGEMENT WAGNER SCHOOL OF PUBLIC SERVICE, NEW YORK UNIVERSITY NEW YORK, USA ABSTRACT: The French health care system is a model of national health insurance (NHI) that provides health care coverage to all legal residents. It is an example of public social security and private health care financing, combined with a public-private mix in the provision of health care services. The French health care system reflects three underlying political values: liberalism, pluralism and solidarity. This article provides a brief overview of how French NHI evolved since World War II; its financing health care organization and coverage; and most importantly, its overall performance. ntroduction. Evolution, coverage, financing and organization The French health care system is a model of national health Evolution: French NHI evolved in stages and in response to Iinsurance (NHI) that provides health care coverage to all legal demands for extension of coverage. Following its original passage, residents. It is not an example of socialized medicine, e.g. Cuba. in 1928, the NHI program covered salaried workers in industry and It is not an example of a national health service, as in the United commerce whose wages were under a low ceiling (Galant, 1955). Kingdom, nor is it an instance of a government-run health care In 1945, NHI was extended to all industrial and commercial workers system like the United States Veterans Health Administration. and their families, irrespective of wage levels. The extension of French NHI, in contrast, is an example of public, social security and coverage took the rest of the century to complete. -

Guidelines for Pharmacists and the Pharmacy Workforce
UPDATED 14 JULY 2020 FIP HEALTH ADVISORY COVID-19: GUIDELINES FOR PHARMACISTS AND THE PHARMACY WORKFORCE INTERNATIONAL PHARMACEUTICAL FEDERATION COVID-19: GUIDELINES FOR PHARMACISTS AND THE PHARMACY WORKFORCE FIP will update this interim guidance as more information becomes available. Table of contents Purpose of this document 2 Responsibilities and role of community pharmacy 2 Responsibilities and role of hospital pharmacy 4 Pharmacy activities 5 Pharmacy staff 5 Pharmacy operations and facilities: ensuring safety and continuity of service 5 Preventive measures 8 Use of masks: Recommendations for pharmacy staff and the public 9 Advice to the community 14 Recommendation for outpatient care 14 Patient isolation and referral 15 Home care for patients with suspected COVID-19 presenting with mild symptoms 15 Diagnostic testing for COVID-19 in suspected human cases 15 Ensuring stock and access to key medicines, equipment and facilities 17 Cleaning and disinfection management 17 Infection control: other precautions 18 Infection control: hand washing and hand rubbing 19 How to prepare alcohol-based handrub formulations 19 Pharmacy as an information resource 19 Addressing travel concerns 20 Bibliography 21 ANNEX 1: List of key facilities, equipment, and personal protective equipment using during COVID-19 infections 24 ANNEX 2: Viability of SARS-CoV-2 in aerosols and on different surfaces, and list of disinfectants for commonly contaminated objects 25 ANNEX 3: WHO guide to local production of handrub formulations 26 Validity 29 Acknowledgements 29 COVID-19 pandemic: Guidelines for pharmacists and the pharmacy workforce | Page 1 of 29 Purpose of this Since December 2019, an outbreak of a new human coronavirus has spread to many document countries, causing millions of cases and hundreds of thousands of deaths. -

Expensive Patients, Reinsurance, and the Future of Health Care Reform
Emory Law Journal Volume 69 Issue 6 2020 Expensive Patients, Reinsurance, and the Future of Health Care Reform Govind Persad Follow this and additional works at: https://scholarlycommons.law.emory.edu/elj Recommended Citation Govind Persad, Expensive Patients, Reinsurance, and the Future of Health Care Reform, 69 Emory L. J. 1153 (2020). Available at: https://scholarlycommons.law.emory.edu/elj/vol69/iss6/1 This Article is brought to you for free and open access by the Journals at Emory Law Scholarly Commons. It has been accepted for inclusion in Emory Law Journal by an authorized editor of Emory Law Scholarly Commons. For more information, please contact [email protected]. PERSAD_8.21.20 8/24/2020 11:43 AM EXPENSIVE PATIENTS, REINSURANCE, AND THE FUTURE OF HEALTH CARE REFORM Govind Persad* ABSTRACT In 2017, Americans spent over $3.4 trillion—nearly 18% of gross domestic product—on health care. This spending is unevenly distributed: Almost a quarter is spent on the costliest 1% of patients, and almost half on the costliest 5%. Most of these patients soon return to a lower percentile, but many continue to incur health care costs in the top percentiles year after year. This Article focuses on the challenges that persistently expensive patients present for health law and policy, and how fairly dividing their medical costs among payers illuminates fundamental normative choices about the design and reform of health insurance. In doing so, this Article draws on bioethical and health policy analyses of the fair distribution of medical costs, and examines how legal doctrine shapes health systems’ options for responding to expensive patients. -

Barrier Isolation Technology: a Labor-Efficient Alternative to Cleanrooms
Barrier Isolation Technology: A Labor-Efficient Alternative To Cleanrooms Paul Mosko, MS. FASHP and Hank Rahe, BSIM, MSE Abstract - Barrier isolation technology has been recognized by the Food and Drug Administration for a number of years as a sage and effective way to process parenteral products aseptically. Pharmaceutical companies have shown that this method of processing increases the sterility assurance level of their products and reduces manufacturing costs. Hospital pharmacies in Europe have used this technology for more than 10 years as a means of product and personnel protection. In the United States, the technology is becoming accepted because of its capital cost effectiveness and because it increases safety during the preparation of cytotoxic compounds. Some pharmacists, however, have expressed concerns about the efficiency of such systems in the pharmacy setting. Using work measurement techniques, the authors tested a barrier isolator system at the University of Cincinnati Hospital. The results are presented here. Key Words - barrier/isolator technology: cleanrooms: parenteral drugs Hosp Pharm - 1999:34:834-838 Providing a facility for the manipulation of parenteral drugs within the pharmacy is a significant concern for health care organizations because of the costs, space requirements, and potential lack of flexibility this preparation often entails. The American Society of Health-System Pharmacists (ASHP) has focused on quality working conditions in health system pharmacies by upgrading the guidelines for cleanliness in prepatory work environments. (1) Some have interpreted these guidelines simply to mean laminar flow hoods or "cleanrooms," because these have been the conventional particulate-control technology for more than 40 years. (2) Some states have taken steps to upgrade the quality of the environment in which IV admixtures and cytotoxic compounds are prepared recognizing new technologies that can achieve this goal. -

Addressing Health Care Market Consolidation and High Prices the Role of the States
HEALTH POLICY CENTER RESEARCH REPORT Addressing Health Care Market Consolidation and High Prices The Role of the States Robert A. Berenson Jaime S. King Katherine L. Gudiksen Roslyn Murray URBAN INSTITUTE UC HASTINGS LAW UC HASTINGS LAW GEORGETOWN UNIVERSITY Adele Shartzer URBAN INSTITUTE January 2020 ABOUT THE URBAN INSTITUTE The nonprofit Urban Institute is a leading research organization dedicated to developing evidence-based insights that improve people’s lives and strengthen communities. For 50 years, Urban has been the trusted source for rigorous analysis of complex social and economic issues; strategic advice to policymakers, philanthropists, and practitioners; and new, promising ideas that expand opportunities for all. Our work inspires effective decisions that advance fairness and enhance the well-being of people and places. Copyright © January 2020. Urban Institute. Permission is granted for reproduction of this file, with attribution to the Urban Institute. Cover image by Tim Meko. Contents Acknowledgments iv Executive Summary v 1. Introduction 1 2. Employee Retirement Income Security’s Act 8 3. State Efforts to Promote Transparency 11 4. State Efforts to Regulate Consolidation and Promote Competition 17 5. State Options for Overseeing and Regulating Prices 44 6. Conclusion 68 Notes 69 References 79 About the Authors 86 Statement of Independence 87 Acknowledgments This report was funded by the Commonwealth Fund. We are grateful to them and to all our funders, who make it possible for Urban to advance its mission. The views expressed are those of the authors and should not be attributed to the Urban Institute or UC Hastings Law, its trustees, or its funders. -

Hand Hygiene: Clean Hands for Healthcare Personnel
Core Concepts for Hand Hygiene: Clean Hands for Healthcare Personnel 1 Presenter Russ Olmsted, MPH, CIC Director, Infection Prevention & Control Trinity Health, Livonia, MI Contributions by Heather M. Gilmartin, NP, PhD, CIC Denver VA Medical Center University of Colorado Laraine Washer, MD University of Michigan Health System 2 Learning Objectives • Outline the importance of effective hand hygiene for protection of healthcare personnel and patients • Describe proper hand hygiene techniques, including when various techniques should be used 3 Why is Hand Hygiene Important? • The microbes that cause healthcare-associated infections (HAIs) can be transmitted on the hands of healthcare personnel • Hand hygiene is one of the MOST important ways to prevent the spread of infection 1 out of every 25 patients has • Too often healthcare personnel do a healthcare-associated not clean their hands infection – In fact, missed opportunities for hand hygiene can be as high as 50% (Chassin MR, Jt Comm J Qual Patient Saf, 2015; Yanke E, Am J Infect Control, 2015; Magill SS, N Engl J Med, 2014) 4 Environmental Surfaces Can Look Clean but… • Bacteria can survive for days on patient care equipment and other surfaces like bed rails, IV pumps, etc. • It is important to use hand hygiene after touching these surfaces and at exit, even if you only touched environmental surfaces Boyce JM, Am J Infect Control, 2002; WHO Guidelines on Hand Hygiene in Health Care, WHO, 2009 5 Hands Make Multidrug-Resistant Organisms (MDROs) and Other Microbes Mobile (Image from CDC, Vital Signs: MMWR, 2016) 6 When Should You Clean Your Hands? 1. Before touching a patient 2. -

Body Substance Isolation PERSONAL PROTECTIVE
CACC Standard 6A Body Substance Isolation AND UNIVERSAL PRECAUTIONS TRAINING PERSONAL PROTECTIVE EQUIPMENT • Blocks entry of an organism into the body – Gloves are most common • Make sure all first aid kits contain several pairs of vinyl, laytex, or Nitrile gloves • Protective eyewear, standard surgical masks, and/or respirators may be necessary • Mouth to barrier (breathing masks) are also recommended PERSONAL PROTECTIVE EQUIPMENT (PPE) • No case of disease transmission to a rescuer as a result of performing unprotected CPR in an infected victim has been documented (only 15 cases of infection reported in last 30 years!) . However, mouth to barrier devices are still strongly recommended! 1 CACC Training Aid 39-H-7 Last Modified 10 Oct 07 CACC Standard 6A UNIVERSAL PRECAUTIONS • Individuals infected with Hepatitis B Virus (HBV) or HIV may not show symptoms and may not even know they are infectious. • All human blood and body fluids should be considered infectious, and precautions should be taken to avoid contact. UNIVERSAL PRECAUTIONS • The Body Substance Isolation (BSI) technique assumes that all body fluids are a potential risk. • Follow BSI procedures even when blood and/or body fluids are not visible UNIVERSAL PRECAUTIONS • Wear appropriate PPE, such as gloves • Use absorbent barriers to soak up blood or other infectious materials • Clean the spill area with an appropriate disinfecting solution, such as bleach • Discard contaminated materials in an appropriate waste disposal container 2 CACC Training Aid 39-H-7 Last Modified 10 Oct -
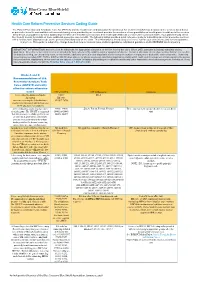
Health Care Reform Preventive Services Coding Guide
Health Care Reform Preventive Services Coding Guide The Patient Protection and Affordable Care Act (PPACA) and the Health Care and Education Reconciliation Act of 2010 (HCERA) has designated the services listed below as preventive benefits and available with no cost-sharing when provided by an in-network provider for members of non-grandfathered health plans. In addition to the services listed below, your patient may have additional preventive care benefits covered under their health plan that may or may not be covered at 100%. Your patient should check their benefit booklet for details on these additional preventive care benefits. The following tables provide a quick reference guide for submitting claims for preventive services with a “well-person” diagnosis code as the primary (first) diagnosis on the claim. This information is intended as a reference tool for your convenience and is not a guarantee of payment. This guide is subject to change based on new or revised laws and/or regulations, additional guidance and/or BCBSNC medical policy. IMPORTANT INFORMATION: Services must be billed with the appropriate diagnosis, at the line level of the claim (Block 24E), pursuant to industry standard coding guidelines. Preventive or screening services are intended for those who currently exhibit no signs or symptoms of disease. Services otherwise deemed preventive that are received in an inpatient setting, an emergency room, or that include additional procedures or diagnostic services may be subject to copayment, deductible and coinsurance. Submitting screening service codes (CPT, HCPCs, ICD-9 or ICD-10) when signs or symptoms are present constitutes inappropriate coding which could result in recoupment of monies paid to the provider for those services. -

Chapter 9: Monitoring, Surveillance, and Investigation of Health Threats
Chapter 9: Monitoring, surveillance, and investigation of health threats SUMMARY POINTS · Monitoring, surveillance and investigation of health threats are vital capabilities for an effective health system. The International Health Regulations (2005) require countries to maintain an integrated, national system for public health surveillance and response, and set out the core capabilities that countries are required to achieve. · Systematic monitoring of serious infectious diseases and other conditions is typically achieved through notifiable diseases legislation based on clinical observation and laboratory confirmation. Clinical and laboratory-based surveillance also provides the basis for systematic collection of vital statistics (births, deaths, causes of death), and may extend to the reporting and analysis of risk factors for noncommunicable diseases and injuries. Systematic collection of these data informs the allocation of resources and facilitates evaluation of community-based and population-level prevention strategies. · Clinical and laboratory surveillance are passive systems that may be enhanced by sentinel surveillance and/or community-based surveillance strategies that rely on a wider range of people, including non-medical personnel. Suspected cases identified in this way must be treated with respect, protected from discrimination, with diagnosis confirmed by qualified health workers at the earliest opportunity. · A significant degree of stigma may attach to some diseases, such as HIV, sexually transmitted infections and diabetes. Notifiable diseases legislation should require the protection of personal information, and clearly define any exceptions. Concerns about discrimination and breach of privacy may be addressed by requiring certain diseases to be reported on an anonymous or de- identified basis. · In some countries, legislation or regulations may be used to establish or enhance a comprehensive public health surveillance system.