Closed Reduction, Traction, and Casting Techniques
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
Ankle Fractures
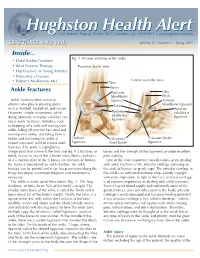
HughstonHughston HealthHealth AlertAlert 6262 Veterans Parkway, PO Box 9517, Columbus, GA 31908-9517 • www.hughston.com/hha FRACTURES AND YOU Volume 19, Number 2 - Spring 2007 Inside... Fig. 1. Normal anatomy of the ankle • Distal Radius Fractures • Wrist Fracture Therapy Posterior (back) view • Hip Fractures in Young Athletes • Protecting a Fracture Lateral (outside) view • Robert J. McAlindon, MD Tibia Fibula Ankle Fractures Posterior Tibia tibiofibular Fibula Ankle fractures often occur in ligament Anterior athletes who play in pivoting sports Talus tibiofibular ligament such as football, basketball, and soccer. Anterior However, simple movements while Posterior talofibular doing common, everyday activities can talofibular ligament ligament cause ankle fractures. Activities, such as stepping off a curb and turning your ankle, falling off your kitchen stool and twisting your ankle, and falling from a ladder and fracturing the ankle at Deltoid Calcaneus Calcaneofibular impact can cause mild to serious ankle ligament (heel bone) ligament fractures. The ankle is a ginglymus (hinge) joint that connects the foot and leg. If a fracture, or bones and the strength of the ligaments provide excellent break, occurs in any of the 3 bones (tibia, fibula, and talus) joint stability. or if a combination of the 3 bones are cracked, or broken, One of the most important considerations when dealing the injury is considered an ankle fracture. An ankle with ankle fractures is the articular cartilage (covering on fracture can be painful and it can keep you from doing the the ends of bones), or gristle caps. The articular cartilage in things you enjoy, so prompt diagnosis and treatment is the ankle can withstand multiple times a body’s weight necessary. -

Pediatric Ankle Fractures
CHAPTER 26 PEDIATRIC ANKLE FRACTURES Sofi e Pinney, DPM, MS INTRODUCTION stronger than both the physis and bone. As a result, there is a greater capacity for plastic deformation and less chance of The purpose of this review is to examine the current intra-articular fractures, joint dislocation, and ligamentous literature on pediatric ankle fractures. I will discuss the disruptions. However, ligamentous injury may be more anatomic considerations of a pediatric patient, how to common than originally believed (1). A case-control study evaluate and manage these fractures, and when to surgically by Zonfrillo et al found an association between an increased repair them. Surgical techniques and complications will be risk of athletic injury in obese children, and concluded a briefl y reviewed. higher body mass index risk factor for ankle sprains (4). Ankle fractures are the third most common fractures in Secondary ossifi cation centers are located in the children, after the fi nger and distal radial physeal fracture. epiphysis. The distal tibial ossifi cation center appears at 6-24 Approximately 20-30% of all pediatric fractures are ankle months of age and closes asymmetrically over an 18-month fractures. Most ankle fractures occur at 8-15 years old. The period fi rst central, then medial and posterior, with the peak injury age is 11-12 years, and is relatively uncommon anterolateral portion closing last at 15 and 17 years of age for under the age 5. This injury is more common in boys. females and males, respectively. The distal fi bula ossifi cation The most common cause of pediatric ankle fractures is a center appears at 9-24 months of age and closes 1-2 years rotational force, and is often seen in sports injuries associated after the distal tibial. -

Ankle Fracture Protocol: Operative Treatment
53880 Carmichael Drive ● South Bend, IN 46635 60160 Bodnar Boulevard ● Mishawaka, IN 46544 Phone 574-247-9441 ● Fax: 574-247-9442 ● www.sbortho.com ANKLE FRACTURE PROTOCOL: OPERATIVE TREATMENT Ankle fractures are common injuries both in young and older patient populations caused by both low energy (trip or fall) and high energy (automobile accident) trauma. Although there are multiple ways of describing ankle fractures and no two fractures are exactly alike, the most important aspect of how we treat your ankle fracture depends on whether the ankle fracture is stable or unstable. The “stability” of the ankle is often determined by whether or not there is an injury to the ankle syndesmosis (the joint between the tibia and fibula). Your treatment plan will be dictated partly by whether or not this is injury which is evaluated intraoperatively at the time of surgery. There are two basic types of ankle fractures: 1) High Energy Axial Injuries: Pilon 2) Rotational Injuries: - Malleolar – either medial or lateral - Bimalleolar – both medial and lateral - Trimalleolar – includes posterior malleolus The goal of treatment is to maximize the long term function of the ankle by restoring and maintaining alignment. If surgery is not required then patients may be treated with closed reduction and immobilization in the form of a splint, cast, pneumatic walker, or air splint. If surgery required then patients may be treated with open reduction and internal fixation. The amount of weightbearing allowed is based on the quality of the fixation, quality of the bone and the healing status of the fracture. If the fixation is secure and stable, the expectation is for the patient to begin early AROM once the wounds are healed ~ two weeks status post. -

Physiotherapy Following Your Ankle Fracture
Physiotherapy following your ankle fracture This leaflet has been given to you to assist you in returning back to normal following your fractured ankle. If you have any queries after reading it, please discuss with your physiotherapist or contact the physiotherapy department on 0118 322 7812 Monday to Friday 8am to 4pm. What is an ankle fracture? • A fracture is the same as a break. • The broken bone often occurs in just the fibula (the thinner bone on the outside of your lower leg). The break may be below, at the same level or above your ankle joint. These fractures may be referred to as a Weber fracture and are classified as A, B or C dependent on the site of the break (see below). • Occasionally the tibia (the thicker bone in your lower leg may also be involved. Weber fractures of the ankle. How is it treated? • Most fractures will heal themselves but do need a period of protected immobilisation to allow this healing to occur. • Occasionally your ankle may need to be manipulated prior to being immobilised to ensure it heals in the correct position. • Your ankle may be immobilised in a plaster cast or a boot. This usually lasts for up to six weeks but may be shorter or longer depending how well healing occurs. • Occasionally your ankle may require surgery to stabilise the fracture with pins and plates. • While the plaster is on, it is important to keep your toes and knees moving to prevent them becoming stiff. Physiotherapy following your ankle fracture, August 2021 1 Physiotherapy Department / Physiotherapy following your ankle fracture • When your consultant thinks you are ready the plaster cast will be removed and you can then start to move your ankle. -

Ankle Fracture
NHS Forth Valley Ankle Fracture Patient Information Leaflet Introduction l A fracture is the same as a break. l A simple fracture will be treated in a plaster. l More complicated fractures may be fixed with pins and plates. Bones of the Tibia Foot and Ankle Fibula Navicular Metatarsals Talus Cuneiforms Phalanges Cuboid Calcaneus 2 What should I expect when my plaster is taken off? 1. SKIN CHANGES – dry skin, colour changes and increased hair growth. 2. STIFFNESS – because your ankle has been held in one position by the plaster for a period of time. 3. SWELLING – your foot and ankle will be swollen, this may increase at the end of the day or if you have been upright too long. 4. DISCOMFORT – you may feel more pain as you begin to move and walk on your ankle. This is normal and will ease. The above symptoms can restrict your walking initially. You may require to continue using a stick or crutches. You will be advised on this. 3 What should I do to help these symptoms? 5. ELEVATION – keep your leg elevated when you are not walking. Support your leg with pillows/cushions; make sure your foot is above the level of your hip. Doing your exercises in this position reduces swelling. 6. COMPRESSION – You may have been given tubigrip to use on your ankle/foot during the day. Make sure there are no wrinkles. Take it off at night. 7. DRY SKIN/EXCESSIVE HAIR GROWTH – wash the foot/ankle with warm water. Use a bland moisturiser (aqueous cream) for the first few days. -

Ankle Fractures 3
Ankle Fracture Update OTA RESIDENT CORE CURRICULUM LECTURE SERIES Christopher Lee, M.D. UCLA Core Curriculum V5 Objectives Following this session, you should be able to: 1. Understand normal versus abnormal radiographic parameters 2. Indications for surgical fixation of ankle fractures 3. Define articular pathology associated with the Lauge-Hansen classification 4. Define common posterior malleolus pathology 5. Indications for posterior malleolus fixation 6. Understand syndesmosis evaluation and treatment principles Core Curriculum V5 Outline • Evaluation: Clinical and Radiographic • Classification: Weber Lauge-Hansen • Specific Problem Areas: Posterior Malleolus and Syndesmosis • Outcome • Diabetic Ankle Fractures Core Curriculum V5 Evaluation: Clinical HISTORY PHYSICAL EXAM • Mechanism • Skin • Timing • Nerves • Soft-tissue Injury • Vasculature • Bony Quality • Pain • Comorbidities • Deformity • Associated Injuries • Instability: Does the ankle easily re-dislocate? Core Curriculum V5 Physical Exam • Look at the soft tissue! • Open versus tenting versus closed Core Curriculum V5 Radiographic Evaluation • Ensure adequate films • Joint above and below • Ankle series (AP/LAT/MORTISE) • Special films • Manual stress • Gravity stress • CT • For specific pathology Core Curriculum V5 AP Ankle • Tib/Fib overlap: ~10 mm • Tib/Fib clear space: <5 mm • End on view of fibula • Can evaluate if screw through fibular plate going into incisura or not Core Curriculum V5 Mortise View • Tib/fib overlap: >1 mm • Talocrural angle: <8 or >15 degrees Core Curriculum -

Residents Comprehensive Fracture Course Faculty: Lunch /Spinesymposium Wednesday - Friday, October 5 - 7
RESIDENTS COMPREHENSIVE FRACTURE COURSE • Wednesday – Friday, Modules Module One October 5 – 7, 2016 Articular Fractures Module Leaders: Frank A. Liporace, MD Toni M. McLaurin, MD & Marcus F. Sciadini, MD, Timothy S. Achor, MD Program Chairs Topics Distal Humerus Course Description Anatomy/Approaches (incl. Osteotomy) Post-Operative Treatment Reduction and Implant Techniques Total Elbow Arthroplasty The Residents Comprehensive Fracture Course will be presented Elbow in six (6) separate small group modules, with 22 - 24 residents Anatomy and Radiographs Olecranon Fractures and 5 experienced faculty educators per module. Monteggia Fractures Terrible Triad Wednesday - Friday, October 5 - 7 - Friday, Wednesday The modules will have a rapid-fire series of mini-lectures, an Tibial Plateau extensive open case-based discussion, video demonstrations of Fragment Specific Fixation Classification techniques, and hands-on skills lab exercises. Modules will cover Medial/Posteromedial Fragment Lateral Articular Fragment fundamental principles of fracture care distributed among six topics: Treatment Algorithms: Low Energy - High Energy articular, diaphyseal, foot & ankle, geriatrics, pediatrics, and Supracondylar Femur pelvis/polytrauma/acetabulum, plus a lunch-time spine session. ORIF - Intramedullary Nailing Anatomy Implant Position and Surgical Techniques Radiography This course offers pre-course educational on-demand video materials. Details will be sent with registration confirmation as Case-Based Discussions well as an online basic science pre-test and an onsite clinical Intra-articular Distal Humerus Fracture Monteggia Fracture post test. Olecranon Fracture Terrible Triad Residents Comprehensive Fracture Course Fracture Residents Comprehensive Intercondylar Femur Fracture Lateral Plateau Fracture Bicondylar Plateau Fracture B3 Distal Femur Fracture Target Audience Hands-on Skills Labs This course is targeted for PGY2 – PGY4’s, others who feel they Olecranon Tension Banding and Plating Tibial Plateau will benefit will not be excluded. -

Three Week Versus Six Week Immobilisation for Stable Weber BMJ: First Published As 10.1136/Bmj.K5432 on 23 January 2019
RESEARCH Three week versus six week immobilisation for stable Weber BMJ: first published as 10.1136/bmj.k5432 on 23 January 2019. Downloaded from B type ankle fractures: randomised, multicentre, non-inferiority clinical trial Tero Kortekangas,1,2 Heidi Haapasalo,3 Tapio Flinkkilä,1,2 Pasi Ohtonen,2,4 Simo Nortunen,1,2 Heikki-Jussi Laine,3 Teppo LN Järvinen,5,6 Harri Pakarinen1,2 1Department of Surgery, ABSTRACT three week cast group, and 89.8 (SD 18.4) in the three Division of Orthopaedic and OBJECTIVE week orthosis group. The between group difference Trauma Surgery, Oulu University To determine whether treatment of isolated stable at 52 weeks for the three week cast versus six week Hospital, Kajaanintie 50, PO Box 21, FI 90029 OYS, Oulu, Weber B type ankle fractures with a cast or a simple cast was 3.6 points (95% confidence interval −1.9 to Finland orthotic device for three weeks produces non-inferior 9.1, P=0.20), and for the three week orthosis versus 2Medical Research Centre outcomes compared with conventional immobilisation six week cast was 1.7 points (−4.0 to 7.3, P=0.56). (MRC) Oulu, Oulu, Finland in a cast for six weeks. In both comparisons, the confidence intervals did 3 Department of Orthopaedics, not include the predefined inferiority margin of −8.8 Tampere University Hospital, DESIGN Tampere, Finland Randomised, pragmatic, non-inferiority, clinical trial points. The only statistically significant between group 4Division of Operative Care, with blinded outcome assessment. differences observed in the secondary outcomes and Oulu University Hospital, Oulu, harms in the two primary comparisons were slight SETTING Finland improvement in ankle plantar flexion and incidence of 5 Two major trauma centres in Finland, 22 December Finnish Centre for Evidence- deep vein thrombosis, both in the three week orthosis 2012 to 6 June 2016. -

Role of Regional Bone Mineral Density on Ankle Fracture Pattern Hannah Sahli, Dpmb, Cody J
Folds here Folds here Role of Regional Bone Mineral Density on Ankle Fracture Pattern Hannah Sahli, DPMb, Cody J. Togher, DPMa, Stephanie L. Golding, DPMa, Jordan Butterfield, DPMa, Joshua A. Sebag, DPMb, Christopher L. Reeves, MS, DPM, FACFASc, Amber M. Shane, DPM, FACFASc aCurrent Resident, AdventHealth East Orlando, Florida bImmediate Past Resident, AdventHealth East Orlando, Florida cAttending Faculty, Department of Podiatric Surgery, AdventHealth East Orlando Residency, Florida Introduction & Literature Review Results Discussion Ankle fractures are a common injury treated by foot and ankle surgeons, frequently Of the 108 subjects, 39 were male, 69 were female. Average age was Rotational mechanism of injury has been described with the Lauge-Hansen classified on plain film radiographs using the Lauge-Hansen system (1). In each stage, 50.7 years. Average BMI was 30.9 ± 32 kg/m^2; tobacco use in 26 system. Injury pattern includes malleolar or ligamentous injury. We investigated malleolar fracture or ligamentous rupture is sustained. However, it is unclear what factors (24.1%), and diabetes mellitus in 18 (16.7%) patients. Average BMD a correlation between BMD and fracture severity. account for this difference. We suspect bone mineral density (BMD) is a contributing The influence CTs have on surgical treatment of ankle fractures has been factor. was 233.18 ± 233 HU. When divided by malleolar involvement there Decreased BMD is a known risk factor for fragility fractures, often hip, wrist and spine were 8 unimalleolar, 33 bimalleolar, and 67 trimalleolar fractures. The discussed by numerous authors (5,6). We had more trimalleolar versus fractures in the elderly (2). The correlation between BMD and ankle fractures has not majority of fractures were supination-external rotation injuries (n=60). -

Diagnosis and Treatment of Ankle Fractures
CE .................................................................................................. DIRECTED READING Diagnosis and Treatment Of Ankle Fractures ANNE M SCOTT, BSRS, R.T.(R) Ankle fractures are common After reading this article, readers should be able to: among all populations, ■ Review ankle joint anatomy and the role of ligament structures in providing stability. ■ although incidence increases Describe the role of imaging in patient diagnosis, treatment planning and follow-up. ■ in the elderly. They are most Discuss classification systems for ankle injury patterns. ■ often the result of simple falls Determine when surgical reduction and internal fixation of ankle fractures is required and complications that may result from surgery. and athletic injuries but also ■ may be caused by underlying Describe rehabilitation techniques and functional recovery prognosis. pathology. A thorough patient evaluation with description of njuries to the ankle are common used to evaluate these injuries may the mechanism of injury is key in the general population and in include conventional radiography, mag- to proper diagnosis. 1,2 athletes. It is estimated that netic resonance (MR) imaging, comput- 260 000 Americans sustain an ed tomography (CT), radionuclide bone This article examines the ankle fracture each year and scanning and ultrasonography. use of radiography and I that ankle fractures occur in about 100 Stable fractures are effectively treat- other imaging modalities in per 100 000 people in major cities.3,4 ed with casts and removable braces.9 diagnosing ankle injuries, as They constitute 21% of all sports-relat- Unstable fractures must be reduced well as several classification ed injuries.1 One study reported that promptly and accurately to optimize systems available to describe the incidence of ankle fractures has healing and minimize the length of the pattern of injury and increased in recent decades, especially hospital stay.4 When surgery is required, aid in treatment planning. -

Ankle Fracture Patient Education Handbook
Ankle Fracture Patient Education Handbook Orlando EDUPT.080.0001 Ankle Fracture: Patient Education Handbook AdventHealth Orlando AdventHealth Orlando is a cornerstone of Central Florida’s epicenter for arts, science and medicine. Around us, neighborhoods have flourished, a small town became the city beautiful and a hospital is becoming part of Health Village. Same doctors you trust. Same care you love. Now coming together as AdventHealth — one unified system with one collaborative focus on your whole-person health. Whether you live in a large city or a rural town, whole-person health means a more personal level of care than ever before — physically, emotionally and spiritually. Our whole-hearted commitment to your well-being means we may have a new name, but we still know yours. Experience compassion, expertise and world-class resources with access to some of the nation’s best services, right here in Florida. ADDRESS: 601 E. Rollins Street, Orlando, FL 32803 Main Phone: (407) 303-5600 Important Phone Numbers Orthopaedic Traumatology Office- (407) 895-8890 Phone calls are answered Monday through Friday from 8:00AM to 5:00PM AdventHealth Orlando Orthopedic Institute - (407) 609-3049 2 Ankle Fracture: Patient Education Handbook Table of Contents Page Section 4 Introduction 5 Understanding the Ankle and Ankle Surgery 6 What to Expect: Plan of Care • Closed Reduction • Surgical Treatment: Open Reduction and Internal Fixation 8 Discharge and When to Call Your Doctor 9 Going Home With a Nerve Block ****** 10 Healing & Recovery After Ankle Surgery • Pain Management: Elevation, Ice, Medication, Sleep • Exercise • Therapy • Fracture Boot • Showering 12 Taking Pain Medications at Home 13 Dressing Changes at Home 14 Constipation 16 Home Safety 17 Therapy/Exercise Program This printed copy for temporary use only. -
ANTHEM® Ankle Fracture System Technique Guide
ANTHEM® Ankle Fracture System SURGICAL TECHNIQUE GUIDE GLOBUSMEDICAL.COM/TRAUMA | Our mission is to deliver cutting-edge technology, research, and innovative solutions to promote healing in patients with musculoskeletal disorders. The Surgical Technique shown is for illustrative purposes only. The technique(s) actually employed in each case always depends on the medical judgment of the surgeon exercised before and during surgery as to the best mode of treatment for each patient. Additionally, as instruments may occasionally be updated, the instruments depicted in this Surgical Technique may not be exactly the same as the instruments currently available. Please consult with your sales representative or contact Globus directly for more information. SURGICAL TECHNIQUE GUIDE ANTHEM® Ankle Fracture System System Overview .................................................................................4 Implant Overview . 6 Screw Compatibility ............................................................................... 8 Distal Fibula Plating: Surgical Technique 1. Preoperative Planning .......................................................................11 2. Patient Positioning ..........................................................................11 3. Approach ..................................................................................11 4. Fracture Reduction . .13 5. Plate Selection . .14 6. Plate Placement ...........................................................................14 7. Screw Insertion . .15 OPTIONAL: Syndesmosis