Gastrointestinal Bleeding Gary A
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Provocative Testing and Localization in Video Capsule Endoscopy
1 2 The Role of Provocative 3 4 Testing and Localization of 5 6 the Video Capsule Endoscope in 7 the Management of Small 8 9 Intestinal Bleeding Q4 10 11 a, b 12 Daniel L. Raines, MD *, Douglas G. Adler, MD Q5 Q6 Q7 13 Q1 Q2 14 15 KEYWORDS 16 Small intestinal bleeding Provocative angiography Provocative endoscopy 17 Video capsule endoscopy Device-assisted enteroscopy 18 19 20 KEY POINTS 21 Cases of small intestinal bleeding (SIB) are commonly encountered in clinical practice 22 despite advancements in medical technology that allow consistent visualization of the 23 entire gastrointestinal tract. 24 The use of antithrombotic agents to provoke bleeding has been found to be revealing in 25 cases of SIB when used in combination with angiography as well as endoscopy. 26 The performance of endoscopic procedures, including video capsule endoscopy (VCE) 27 and device-assisted enteroscopy (DAE) on active antiplatelet and/or anticoagulant ther- 28 apy is considered low risk and may improve diagnostic yield. 29 The use of VCE for gastrointestinal bleeding in the inpatient setting has been found to 30 improve diagnostic yield and decrease hospital stay. 31 Because DAE is required for therapeutic intervention in patients with small bowel 32 bleeding, access to this technology is essential for effective management in many cases. 33 34 35 Video content accompanies this article at http://www.giendo.theclinics.com/. 36 37 Q8 38 OBSCURE GASTROINTESTINAL BLEEDING Definitions 39 40 Small intestinal bleeding (SIB) has been described as bleeding that is undefined in 41 cause despite evaluation by standard upper endoscopy, colonoscopy, and small Q9 42 bowel follow-through (SBFT). -

Clinical Audit on Management of Hematemesis in Children Admitted to Pediatric Gastroenterology and Hepatology Unit of Assiut
Med. J. Cairo Univ., Vol. 86, No. 8, December: 4531-4536, 2018 www.medicaljournalofcairouniversity.net Clinical Audit on Management of Hematemesis in Children Admitted to Pediatric Gastroenterology and Hepatology Unit of Assiut University Children Hospital ESRAA T. AHMED, M.Sc.; FATMA A. ALI, M.D. and NAGLA H. ABU FADDAN, M.D. The Department of Pediatrics, Faculty of Medicine, Assiut University, Assiut, Egypt Abstract Hematemesis: Indicates that the bleeding origin is above the Treitz angle, i.e., that it constitutes an Background: Hematemesis is an uncommon but potentially Upper Gastrointestinal Bleeding (UGIB) [3] . serious and life-threatening clinical condition in children. It indicates that the bleeding origin is above the Treitz angle, The etiology of upper GI bleeding varies by i.e., that it constitutes an Upper Gastrointestinal Bleeding (UGIB). age. The pathophysiology of upper GI bleeding is related to the source of the bleeding. Most clinically Aim of Study: To assess for how much the adopted proto- significant causes of upper GI bleeds are associated cols of management of children with upper gastrointestinal bleeding were applied at Gastroenterology & Hepatology Unit with ulcers, erosive esophagitis, gastritis, varices, of Assiut University Children Hospital. and/or Mallory-Weiss tears. While Physiologic Patients and Methods: This study is a an audit on man- stress, NSAIDs such as aspirin and ibuprofen, and agement of children with upper gastrointestinal bleeding infection with Helicobacter pylori are few of the admitted to pediatric Gastroenterology and Hepatology Unit, factors contributing to the imbalance leading to Assiut University Children Hospital during the period from ulcers and erosions in the GI tract [4] . -

The American Society of Colon and Rectal Surgeons' Clinical Practice
CLINICAL PRACTICE GUIDELINES The American Society of Colon and Rectal Surgeons’ Clinical Practice Guideline for the Evaluation and Management of Constipation Ian M. Paquette, M.D. • Madhulika Varma, M.D. • Charles Ternent, M.D. Genevieve Melton-Meaux, M.D. • Janice F. Rafferty, M.D. • Daniel Feingold, M.D. Scott R. Steele, M.D. he American Society of Colon and Rectal Surgeons for functional constipation include at least 2 of the fol- is dedicated to assuring high-quality patient care lowing symptoms during ≥25% of defecations: straining, Tby advancing the science, prevention, and manage- lumpy or hard stools, sensation of incomplete evacuation, ment of disorders and diseases of the colon, rectum, and sensation of anorectal obstruction or blockage, relying on anus. The Clinical Practice Guidelines Committee is com- manual maneuvers to promote defecation, and having less posed of Society members who are chosen because they than 3 unassisted bowel movements per week.7,8 These cri- XXX have demonstrated expertise in the specialty of colon and teria include constipation related to the 3 common sub- rectal surgery. This committee was created to lead inter- types: colonic inertia or slow transit constipation, normal national efforts in defining quality care for conditions re- transit constipation, and pelvic floor or defecation dys- lated to the colon, rectum, and anus. This is accompanied function. However, in reality, many patients demonstrate by developing Clinical Practice Guidelines based on the symptoms attributable to more than 1 constipation sub- best available evidence. These guidelines are inclusive and type and to constipation-predominant IBS, as well. The not prescriptive. -

Hemosuccus Pancreaticus: a Rare Cause of Upper Gastrointestinal Bleeding During Pregnancy Rani Akhil Bhat,1 Vani Ramkumar,1 K
Hemosuccus Pancreaticus: A Rare Cause Of Upper Gastrointestinal Bleeding During Pregnancy Rani Akhil Bhat,1 Vani Ramkumar,1 K. Akhil Krishnanand Bhat, 2 Rajgopal Shenoy2 Abstract Upper gastrointestinal bleeding is most commonly caused by From the 1Department of Department of Obstetrics and Gynaecology, Oman Medical 2 lesions in the esophagus, stomach or duodenum. Bleeding which College, Sohar, Sultanate of Oman, Department of Surgery, Oman Medical College, Sohar, Sultanate of Oma. originates from the pancreatic duct is known as hemosuccus pancreaticus. Only a few scattered case reports of hemosuccus Received: 06 Nov 2009 pancreaticus during pregnancy have been recorded in literature. Accepted: 31 Dec 2009 This is a case of a primigravida with 37 weeks of gestation Address correspondence and reprint request to: Dr. Rani A. Bhat,Department of with hemosuccus pancreaticus and silent chronic pancreatitis. Obstetrics and Gynaecology, Oman Medical College, P. O. Box 391, P. C. 321, Al- Evaluating pregnant women with upper gastrointestinal Tareef, Sohar, Sultanate of Oman. bleeding differs from that of non pregnant women as diagnostic E-mail: [email protected] modalities using radiation cannot be used. Therefore, Esophagogastroduodenoscopy should be performed at the time of active bleeding to diagnose hemosuccus pancreaticus. Bhat RA, et al. OMJ. 25 (2010); doi:10.5001/omj.2010.21 Introduction examination showed a combination of dark red blood and melena. Laboratory investigations revealed hemoglobin of 6.3 grams/dL, Hemosuccus pancreaticus is the term used to describe the liver function tests, serum amylase, glucose and prothrombin time syndrome of gastrointestinal bleeding into the pancreatic duct were within the normal range. -

Management of Hemorrhoid Complications in Persian Medicine
http://www.cjmb.org Open Access Review Article Crescent Journal of Medical and Biological Sciences Vol. 7, No. 4, October 2020, 457–466 eISSN 2148-9696 Management of Hemorrhoid Complications in Persian Medicine Khadijeh Hatami1, Amir-Hooman Kazemi-Motlagh1, Hossein Ajdarkosh2, Arman Zargaran1, Mehrdad Karimi1, Ali-Asghar Haeri Mehrizi3, Hoorieh Mohammadi Kenari4 Abstract Objectives: Hemorrhoid disease has been a common medical problem since ancient times. About 5%-10% of patients do not respond to conservative treatment, and surgical procedures have a 20%-25% complication rate including pain, stenosis, infection, incontinence, and the like. Thus, most patients and physicians seek alternative and complementary medicines. Persian medicine (PM) is one of the oldest traditional medicines that present different treatment methods for managing hemorrhoid complications. Accordingly, the present study reviewed these methods and their applications. Methods: This historical review surveyed the principle of management and different medicinal and non-medicinal treatments for each complication of hemorrhoid based on the main textbooks of disease-treatment and famous pharmacopoeias of PM from 10th to 18th century AD. Recent findings about their pharmaceutical properties and mechanisms of action were searched in Google Scholar, Science Direct, and PubMed databases. Results: In PM, it is believed that hemorrhoid disease is because of melancholic or sanguineous distemperament. Cleansing the body and then strengthening the gastrointestinal and the liver for more effective treatment and prevention of relapse are the first therapeutic approaches in this regard. They use herbal and non-herbal medicines with anti-oxidant and anti-inflammatory, analgesic, and phlebotonic properties. In addition, different methods of bloodletting are used for body cleansing, reducing pain, and treating bleeding or thrombotic hemorrhoids. -

Diagnostic Approach to Chronic Constipation in Adults NAMIRAH JAMSHED, MD; ZONE-EN LEE, MD; and KEVIN W
Diagnostic Approach to Chronic Constipation in Adults NAMIRAH JAMSHED, MD; ZONE-EN LEE, MD; and KEVIN W. OLDEN, MD Washington Hospital Center, Washington, District of Columbia Constipation is traditionally defined as three or fewer bowel movements per week. Risk factors for constipation include female sex, older age, inactivity, low caloric intake, low-fiber diet, low income, low educational level, and taking a large number of medications. Chronic constipa- tion is classified as functional (primary) or secondary. Functional constipation can be divided into normal transit, slow transit, or outlet constipation. Possible causes of secondary chronic constipation include medication use, as well as medical conditions, such as hypothyroidism or irritable bowel syndrome. Frail older patients may present with nonspecific symptoms of constipation, such as delirium, anorexia, and functional decline. The evaluation of constipa- tion includes a history and physical examination to rule out alarm signs and symptoms. These include evidence of bleeding, unintended weight loss, iron deficiency anemia, acute onset constipation in older patients, and rectal prolapse. Patients with one or more alarm signs or symptoms require prompt evaluation. Referral to a subspecialist for additional evaluation and diagnostic testing may be warranted. (Am Fam Physician. 2011;84(3):299-306. Copyright © 2011 American Academy of Family Physicians.) ▲ Patient information: onstipation is one of the most of 1,028 young adults, 52 percent defined A patient education common chronic gastrointes- constipation as straining, 44 percent as hard handout on constipation is 1,2 available at http://family tinal disorders in adults. In a stools, 32 percent as infrequent stools, and doctor.org/037.xml. -

081999 Disseminated Intravascular Coagulation
The New England Journal of Medicine Current Concepts Systemic activation+ of coagulation DISSEMINATED INTRAVASCULAR COAGULATION Intravascular+ Depletion of platelets+ deposition of fibrin and coagulation factors MARCEL LEVI, M.D., AND HUGO TEN CATE, M.D. Thrombosis of small+ Bleeding and midsize vessels+ ISSEMINATED intravascular coagulation is and organ failure characterized by the widespread activation Dof coagulation, which results in the intravas- Figure 1. The Mechanism of Disseminated Intravascular Coag- cular formation of fibrin and ultimately thrombotic ulation. occlusion of small and midsize vessels.1-3 Intravascu- Systemic activation of coagulation leads to widespread intra- lar coagulation can also compromise the blood sup- vascular deposition of fibrin and depletion of platelets and co- agulation factors. As a result, thrombosis of small and midsize ply to organs and, in conjunction with hemodynam- vessels may occur, contributing to organ failure, and there may ic and metabolic derangements, may contribute to be severe bleeding. the failure of multiple organs. At the same time, the use and subsequent depletion of platelets and coag- ulation proteins resulting from the ongoing coagu- lation may induce severe bleeding (Fig. 1). Bleeding may be the presenting symptom in a patient with disseminated intravascular coagulation, a factor that can complicate decisions about treatment. TABLE 1. COMMON CLINICAL CONDITIONS ASSOCIATED WITH DISSEMINATED ASSOCIATED CLINICAL CONDITIONS INTRAVASCULAR COAGULATION. AND INCIDENCE Sepsis Infectious Disease Trauma Serious tissue injury Disseminated intravascular coagulation is an ac- Head injury Fat embolism quired disorder that occurs in a wide variety of clin- Cancer ical conditions, the most important of which are listed Myeloproliferative diseases in Table 1. -

Post Hemorrhoidectomy Pain Relief; Outcome of Local Anesthesia
PAIN RELIEF POST HEMORRHOIDECTOMY The Professional Medical Journal www.theprofesional.com ORIGINAL PROF-2998 DOI: 10.17957/TPMJ/15.2998 POST HEMORRHOIDECTOMY PAIN RELIEF; OUTCOME OF LOCAL ANESTHESIA Dr. Syed Muhammad Maroof Hashmi1, Dr. Shua Nasir2, Dr. Lal Shehbaz3, Dr. Muhammad Absar Anwar4, Ahmed Ali5 1. Senior Registrar Department of Neurosurgery ABSTRACT… Background: The aim of my study is to evaluate post-operative pain relief K.M.D.C and Abbasi Shaheed on patients who had hemorrhoidectomy. Materials and Methods: 300 patients who had Hospital Karachi. hemorrhoidectomy were divided equally in to three groups, according to anesthesia type, 2. MD Resident Department of Emergency group 1 (local anesthesia and sedation), while spinal anesthesia was group 2 and general Medicine Ziauddin University anesthesia was considered to be group 3. Pain relief, post-operative complications, hospital Hospital Karachi. staying time were measured and compared between the three groups. Period: Study was 3. MD Resident performed between Jan 2012 to Dec 2014. Results: The study showed that patients who had Department of Emergency Medicine Ziauddin University local anesthesia infiltration and sedation a significant decrease of post-operative total pain Hospital Karachi. scores at 6/12/18/24 hours of more than 50%,200/240/300/320 out of 1000 points in group II 4. House Officer as compared to 420/500/540/580,700/680/660/660 in 3rd groups respectively. The total post- DUHS and Civil Hospital, Karachi 5. Research Fellow BMU operative analgesia doses in the 3 groups were 120:140:180 respectively, total hospital staying time were 130:210:260 days, headache in the ratio of 0:8:1, urine retention in 0:6:1 patients, Correspondence Address: nausea and vomiting in 0:1:5 patients were reduced by 30 %,. -

Hemorrhoids Brown Health Services Patient Education Series
Hemorrhoids Brown Health Services Patient Education Series What are hemorrhoids? Causes of Hemorrhoids Include: Hemorrhoids are swollen veins in the rectum. They ● Straining during bowel movements can cause itching, bleeding, and pain. Hemorrhoids ● Chronic diarrhea or constipation are very common. In some cases, you can see or ● Obesity feel hemorrhoids around the outside of the rectum. ● Pregnancy In other cases, you cannot see them because they ● Anal intercourse are hidden inside the rectum Diagnosis Hemorrhoids do not always cause symptoms. But To diagnose hemorrhoids, your clinician will when they do, they can include: examine your rectum and anus and may insert a ● Itching of the skin around the anus gloved finger into the rectum. Further evaluation ● Bleeding – Bleeding is usually painless and may include a procedure that allows your occurs during bowel movement. You might healthcare provider to look inside the anus (called see bright red blood after using the toilet on anoscopy), or evaluation by a proctologist. your toilet tissue or in the toilet bowl. ● Pain – If a blood clot forms inside a Management of Hemorrhoids hemorrhoid, this can cause pain. You may also experience: Initiate Lifestyle Changes: ● swelling around your anus One of the most important steps in treating ● A sensitive or painful lump near your anus hemorrhoids is avoiding constipation (hard or ● Leakage of feces infrequent stools). Hard stool can lead to rectal bleeding and/or a tear in the anus, called an anal Hemorrhoid symptoms usually depend on the fissure. In addition, pushing and straining to move location. Internal hemorrhoids lie inside the rectum. your bowels can worsen existing hemorrhoids and You can’t see or feel these hemorrhoids, and they increase the risk of developing new hemorrhoids. -

What Everyone Should Know to Stop Bleeding After an Injury
What Everyone Should Know to Stop Bleeding After an Injury THE HARTFORD CONSENSUS The Joint Committee to Increase Survival from Active Shooter and Intentional Mass Casualty Events was convened by the American College of Surgeons in response to the growing number and severity of these events. The committee met in Hartford Connecticut and has produced a number of documents with rec- ommendations. The documents represent the consensus opinion of a multi-dis- ciplinary committee involving medical groups, the military, the National Security Council, Homeland Security, the FBI, law enforcement, fire rescue, and EMS. These recommendations have become known as the Hartford Consensus. The overarching principle of the Hartford Consensus is that no one should die from uncontrolled bleeding. The Hartford Consensus recommends that all citizens learn to stop bleeding. Further information about the Hartford Consensus and bleeding control can be found on the website: Bleedingcontrol.org 2 SAVE A LIFE: What Everyone Should Know to Stop Bleeding After an Injury Authors: Peter T. Pons, MD, FACEP Lenworth Jacobs, MD, MPH, FACS Acknowledgements: The authors acknowledge the contributions of Michael Cohen and James “Brooks” Hart, CMI to the design of this manual. Some images adapted from Adam Wehrle, EMT-P and NAEMT. © 2017 American College of Surgeons CONTENTS SECTION 1 3 ■ Introduction ■ Primary Principles of Trauma Care Response ■ The ABCs of Bleeding SECTION 2 5 ■ Ensure Your Own Safety SECTION 3 6 ■ A – Alert – call 9-1-1 SECTION 4 7 ■ B – Bleeding – find the bleeding injury SECTION 5 9 ■ C – Compress – apply pressure to stop the bleeding by: ■ Covering the wound with a clean cloth and applying pressure by pushing directly on it with both hands, OR ■Using a tourniquet, OR ■ Packing (stuff) the wound with gauze or a clean cloth and then applying pressure with both hands SECTION 6 13 ■ Summary 2 SECTION 1: INTRODUCTION Welcome to the Stop the Bleed: Bleeding Control for the Injured information booklet. -

Why Is There Blood in My Cow's Manure?
Head office Mount Forest Tavistock 1805 Sawmill Road Tel: 519.323.1880 Tel: 519.655.3777BUSINESS NAME Conestogo, On, N0B 1N0: Fax: 519.323.3183 Fax: 519.655.3505 Tel: 519.664.2237 Fax: 519.664.1636 Toll Free 1.800.265.2203 Volume 14, Issue 2 Conestogo, Mount Forest, Tavistock APRIL—MAY 2014 WHY IS THERE BLOOD IN MY COW’S MANURE? WE WILL BE CLOSED There are several things that really seem to get the attention of dairy producers. One such situation is seeing blood in the manure of mature dairy cows. In order to figure out what is APRIL 18TH FOR going on, several considerations should be addressed. How many cows are affected? Do af- GOOD FRIDAY. fected cows appear really sick or are they otherwise fairly normal? Do the cows have diar- PLEASE ORDER YOUR rhea? Is the blood digested or undigested? FEED ACCORDINGLY. Manure containing digested blood has a dark brown or black, tar-like appearance and is called melena. The presence of undigested blood (still red in colour) in manure is referred to as hematochezia. Whether blood is digested or not depends on its point of origin in the gastro- intestinal (GI) tract. Generally speaking, digested blood comes from the rumen, abomasums, or beginning of the small intestine. Common causes of melena include rumen ulcers, abomasal FUTURES MARKET ulcers, abomasal torsion, and intussusceptions of the small intestine (a condition where a por- tion of the bowel telescopes on itself). Melena can also be caused by oak (acorn) toxicity, BEEF overdoses of certain drugs and consumption of some chemicals. -
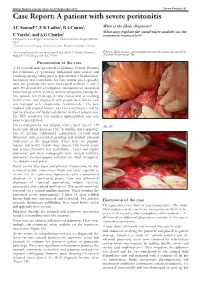
Case Report: a Patient with Severe Peritonitis
Malawi Medical Journal; 25(3): 86-87 September 2013 Severe Peritonitis 86 Case Report: A patient with severe peritonitis J C Samuel1*, E K Ludzu2, B A Cairns1, What is the likely diagnosis? 2 1 What may explain the small white nodules on the C Varela , and A G Charles transverse mesocolon? 1 Department of Surgery, University of North Carolina, Chapel Hill NC USA 2 Department of Surgery, Kamuzu Central Hospital, Lilongwe Malawi Corresponding author: [email protected] 4011 Burnett Womack Figure1. Intraoperative photograph showing the transverse mesolon Bldg CB 7228, Chapel Hill NC 27599 (1a) and the pancreas (1b). Presentation of the case A 42 year-old male presented to Kamuzu Central Hospital for evaluation of worsening abdominal pain, nausea and vomiting starting 3 days prior to presentation. On admission, his history was remarkable for four similar prior episodes over the previous five years that lasted between 3 and 5 days. He denied any constipation, obstipation or associated hematemesis, fevers, chills or urinary symptoms. During the first episode five years ago, he was evaluated at an outlying health centre and diagnosed with peptic ulcer disease and was managed with omeprazole intermittently . His past medical and surgical history was non contributory and he had no allergies and he denied alcohol intake or tobacco use. His HIV serostatus was negative approximately one year prior to presentation. On examination he was afebrile, with a heart rate of 120 (Fig 1B) beats/min, blood pressure 135/78 mmHg and respiratory rate of 22/min. Abdominal examination revealed mild distension with generalized guarding and marked rebound tenderness in the epigastrium.