2019 National Conference Planning Materials
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

7. Kansas Vision Screening Referral & Eye Care Professional Report
7. Kansas Vision Screening Referral & Eye Care Professional Report (Return completed report to school health clinic or nurse) Child’s Name: Date of Birth: Date of Referral: School: Grade: Met referral criteria (check applicable boxes): [ ] With Glasses/Contacts [ ] Without Correction [ ] Unable to Screen [ ] Based on Observation. Provide Symptoms/Concerns: [ ] Distance Visual Acuity [ ] R [ ] L Circle screening tool/distance: Sloan Chart, LEA Symbols, HOTV Symbols, Chart 5 or 10 feet [ ] Near Visual Acuity [ ] R [ ] L (or) if Near Binocular Testing [ ] Both [ ] Stereopsis (PASS 2) Instrument Screening (screener may attach instrument report): [ ] With Glasses/Contacts [ ] Without Correction Circle Instrument (WA Spot™ / Plusoptix S12C / WA SureSight 2.25) Met referral criteria: [ ] R [ ] L Eye Care Professional Findngs Date of Exam:____________ Without Correction With Current Prescription With New Prescription [ ] Normal R_______ L_______ R_______ L_______ R_______ L_______ Summary of vision problem & diagnosis: [ ] Hyperopia: Indicate eye R_______ L_______ [ ] Myopia: Indicate eye? R_______ L_______ [ ] Astigmatism: Indicate eye R_______ L_______ [ ] Amblyopia: Indicate eye R_______ L_______ [ ] Eye Alignment: Indicate eye? R_______ L_______ Esophoria / Esotropia / Exophoria / Exotropia / Other [ ] Binocularity (Stereovision, Near Point of Convergence): ______________________________ [ ] Other Ocular Conditions or Neurological/ Cortical Vision Impairment – Explain: Recommendations & Treatment: Glasses Prescribed: [ ] No [ ] Yes [ ] Constant -

Eyeglasses Product Narrative
Increasing Access to Eyeglasses in Low- and Middle-Income Countries PRODUCT NARRATIVE: EYEGLASSES aatscale2030.orgtscale2030.org MARCH 2020 ACKNOWLEDGEMENTS This report was delivered by the Clinton Health Access Initiative under the AT2030 programme in support of the ATscale Strategy. The AT2030 programme is funded by UK aid from the UK government and led by the Global Disability Innovation (GDI) Hub. The authors wish to acknowledge and thank vision sector experts, practitioners and users, and the partners from the AT2030 programme and Founding Partners of ATscale, the Global Partnership for Assistive Technology, for their contributions. The ATscale Founding Partners are: China Disabled Persons’ Federation, Clinton Health Access Initiative, GDI Hub, Government of Kenya, International Disability Alliance, Norwegian Agency for Development Cooperation, Office of the UN Secretary-General’s Envoy for Financing the Health Millennium Development Goals and for Malaria, UK Department for International Development, UNICEF, United States Agency for International Development, World Health Organization. The views and opinions expressed within this report are those of the authors and do not necessarily reflect the official policies or position of ATscale Founding Partners, partners of the AT2030 programme, or funders. Please use the following form (https://forms.gle/QVVKAbYMG73UVeFB8) to register any comments or questions about the content of this document. Please direct any questions about ATscale, the Global Partnership for Assistive Technology, to [email protected] or visit atscale2030.org. To learn more about the AT2030 Programme, please visit a https://at2030.org/. II PRODUCT NARRATIVE: EYEGLASSES TABLE OF CONTENTS Acronyms iii Executive Summary 1 Introduction 3 1. Assistive Technology and Market Shaping 3 2. -

FAQ: Cataracts
Don’t lose sight of Cataracts Information for people at risk What is cataract? 1 When the lens of your eye gets cloudy, it is called a cataract. It can cause vision loss in one or both eyes. It cannot spread from one eye to the other. What causes a cataract? 2 The lenses of the eyes are made mostly of water and protein. As we age, some of this protein may clump together and cloud the lenses of our eyes. Over time, this “cloud” may grow and cover more of the lens. This makes it harder to see. Smoking, alcohol use, diabetes, and prolonged exposure to the sun can also cause cataract. When are you most likely to have a cataract? 3 Older people mostly get cataracts. But people in their 40s and 50s may get them, especially if the eye has been injured. The risk of having a cataract increases after age 60, and by age 80, more than half of all Americans will have a cataract or will have had cataract surgery. Normal vision. What are the symptoms of a cataract? A scene as it might be viewed by a 4 When you first get a cataract, you may not notice much person with a cataract. change. Your vision may become blurry, as if looking through a foggy window. Or colors may not appear as bright as they once did. As the “cloud” over the lens of your eye grows, it may be harder for you to read. You may also see more glare from a lamp or car headlights at night. -

Finding an Eye Care Professional
Finding an Eye Care Professional You may have recently had your vision screened and failed the screening, you may have noticed changes in your vision, or you may be at risk for developing glaucoma or diabetic retinopathy. Even if you are not experiencing vision problems, it is important to get regular eye exams. If you are thinking about seeing an eye care professional, but don’t know where to begin, this fact sheet can help. Referrals are often helpful in choosing an eye care professional. Ask trusted friends or contact a hospital or university with a medical school for names and references. You can also call one of the following organizations for a referral to someone in your area. The following are the definitions given by each professional organization with their contact information. Ophthalmologists Definition provided by the American Academy of Ophthalmology. For more information, contact the AAO at (415) 561-8540 or www.aao.org. A physician (doctor of medicine or doctor of osteopathy) who specializes in the refractive, medical and surgical care of the eyes and visual system and in the prevention of eye disease and injury. The ophthalmologist has completed four or more years of college premedical education, four or more years of medical school, and four or more years of residency, including at least three years of residency in ophthalmology. The ophthalmologist is a specialist who is qualified by lengthy medical education, training, and experience to diagnose, treat, and manage all eye and visual system problems and is licensed by a state regulatory board to practice medicine and surgery. -

Do You Know Your Eye Care Jargon? an OPTOMETRIST
Do you know your eye care jargon? Optometrists, Orthoptists and Opthalmologists all work in the field of eye care and often work as a team in the same practice. These various professional “categories” can cause quite a lot of confusion though. Not only do they sound similarbut some of their roles can overlap, thus making the differentiation even harder. One great example is that all these experts can recommend glasses. In this article, I will aim to overview the role of each specialty and so make it easier to identify who does what! The levels of training and what they are permitted to do for youas a patientare an important differentiator between these specialties. It will definitely help you make the best-informed decision when looking for help regarding your specific eye care issue. AN OPTOMETRIST In South Africa, Optometrists need to complete a four-year Bachelor of Optometry degree before they are permitted to practice. Once qualified, they provide vital primary vision care. They conduct vision tests and eye examinations on patients in order to detect visual errors, such as near-sightedness, long-sightedness and astigmatism. Optometrists also do testing to determine the patient's ability to focus and coordinate their eyes, judge depth perception, and see colors accurately. Once a visual „problem‟ has been identified andanalyzed, the optometristeffectively corrects them and their related problems, by providing comfortable glasses and or contact lenses. They are also responsible for the maintenance of these “devices”. Optometrists also play an important role in the diagnosis and rehabilitation of patients suffering from Low-vision. -

A Breakthrough in Myopia Control for Your Child
USER GUIDE FOR MiYOSMART MiYOSMART OPTOMETRIC PROTOCOL FOR MiYOSMART MiYOSMART MiYOSMART: A SMART APPROACH TO MYOPIA MiYOSMART The user guide identies what new MiyoSmart wearers should take note of during the adaptation period. To ensure maximized benets of MiyoSmart are experienced, it is recommended to follow the optometric protocol. If you had a way to halt or slow down the progression of myopia, surely you would want to know how. Adaption to new lenses MiyoSmart delivers on this promise and lls a rapidly growing market need. MiyoSmart is an innovative 1ST VISIT 1. It always takes time to get used to your new lenses. The time needed really depends on the individual but wearers can ophthalmic lens for myopia control developed by Hoya Vision Care in cooperation with its research expect about one to two weeks to adapt. collaborator, The Hong Kong Polytechnic University (PolyU). Engineered specically to correct myopic During the rst visit, all visual functions of the child should be assessed to get a clear overview of the current status. A few 2. During the adaptation time, the wearer should avoid: factors are examined to ascertain if the wearer is suitable for MiyoSmart. refractive error and slow down myopia progression, MiyoSmart comes to market at a time when the 1 It is also essential to know the child and his/her parents' ocular and optical history. incidence of myopia is on the rise. Preliminary investigation will also have to be done, where it is compulsory to conduct the following tests and examinations: An estimated 5 billion Research shows that Intensive sport Operating any Using the new lenses Using them on high people, or activities, e.g. -

Care of the Patient with Accommodative and Vergence Dysfunction
OPTOMETRIC CLINICAL PRACTICE GUIDELINE Care of the Patient with Accommodative and Vergence Dysfunction OPTOMETRY: THE PRIMARY EYE CARE PROFESSION Doctors of optometry are independent primary health care providers who examine, diagnose, treat, and manage diseases and disorders of the visual system, the eye, and associated structures as well as diagnose related systemic conditions. Optometrists provide more than two-thirds of the primary eye care services in the United States. They are more widely distributed geographically than other eye care providers and are readily accessible for the delivery of eye and vision care services. There are approximately 36,000 full-time-equivalent doctors of optometry currently in practice in the United States. Optometrists practice in more than 6,500 communities across the United States, serving as the sole primary eye care providers in more than 3,500 communities. The mission of the profession of optometry is to fulfill the vision and eye care needs of the public through clinical care, research, and education, all of which enhance the quality of life. OPTOMETRIC CLINICAL PRACTICE GUIDELINE CARE OF THE PATIENT WITH ACCOMMODATIVE AND VERGENCE DYSFUNCTION Reference Guide for Clinicians Prepared by the American Optometric Association Consensus Panel on Care of the Patient with Accommodative and Vergence Dysfunction: Jeffrey S. Cooper, M.S., O.D., Principal Author Carole R. Burns, O.D. Susan A. Cotter, O.D. Kent M. Daum, O.D., Ph.D. John R. Griffin, M.S., O.D. Mitchell M. Scheiman, O.D. Revised by: Jeffrey S. Cooper, M.S., O.D. December 2010 Reviewed by the AOA Clinical Guidelines Coordinating Committee: David A. -

Page 1 of 8 Questions and Answers from the “Year of Children's Vision
Questions and Answers from the “Year of Children’s Vision: Developing a Strong Vision Health System (Part I)” Webinar (Presented February 26, 2014) QUESTION: I don't feel comfortable not referring for vision screening at 20/33 or greater but the acuity numbers for referral were quoted as 20/40 (ages 3-5). ANSWER: The referral guidelines example in the Webinar from the American Academy of Pediatrics, the American Association for Pediatric Ophthalmology and Strabismus, the American Academy of Ophthalmology, and the American Association of Certified Orthoptists state that children ages 3 through 5 years should be rescreened or referred if they cannot identify the majority (3 of 5) of optotypes on the 20/40 line. Children ages 6 years and older should be rescreened or referred if they cannot pass the majority of optotypes on the 20/30 (20/32) line. Some states, for example, Massachusetts, do have 20/32 as a referral line for ages 3, 4, and 5. QUESTION: Is there a preference to refer to an ophthalmologist as opposed to an optometrist especially for younger children never have been screened before? ANSWER: We do not have a preference. You want to refer to a pediatric eye care professional (optometrist or ophthalmologist) with training and experience treating young children. QUESTION: Why would we get charged for direct referral? We don’t have many choices in our area who take Medicaid. ANSWER: If a child is entitled to an eye examination to identify a disability, to determine eligibility for special education services, to develop an Individualized Education Program (IEP), or as a related service under the IEP, the eye exam must occur at no cost to the family. -

Treatment of Convergence Insufficiency in Childhood: a Current Perspective
1040-5488/09/8605-0420/0 VOL. 86, NO. 5, PP. 420–428 OPTOMETRY AND VISION SCIENCE Copyright © 2009 American Academy of Optometry REVIEW Treatment of Convergence Insufficiency in Childhood: A Current Perspective Mitchell Scheiman*, Michael Rouse†, Marjean Taylor Kulp†, Susan Cotter†, Richard Hertle‡, and G. Lynn Mitchell§ ABSTRACT Purpose. To provide a current perspective on the management of convergence insufficiency (CI) in children by summarizing the findings and discussing the clinical implications from three recent randomized clinical trials in which we evaluated various treatments for children with symptomatic CI. We then present an evidence-based treatment approach for symptomatic CI based on the results of these trials. Finally, we discuss unanswered questions and suggest directions for future research in this area. Methods. We reviewed three multi-center randomized clinical trials comparing treatments for symptomatic (CI) in children 9 to 17 years old (one study 9 to 18 years old). Two trials evaluated active therapies for CI. These trials compared the effectiveness of office-based vergence/accommodative therapy, office-based placebo therapy, and home-based therapy [pencil push-ups alone (both trials), home-based computer vergence/accommodative therapy, and pencil push-ups (large-scale study)]. One trial compared the effectiveness of base-in prism reading glasses to placebo reading glasses. All studies included well-defined criteria for the diagnosis of CI, a placebo group, and masked examiners. The primary outcome measure was the Convergence Insufficiency Symptom Survey score. Secondary outcomes were near point of convergence and positive fusional vergence at near. Results. Office-based vergence/accommodative therapy was significantly more effective than home-based or placebo therapies. -
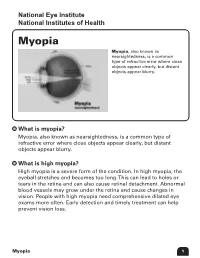
Myopia Myopia, Also Known As Nearsightedness, Is a Common Type of Refractive Error Where Close Objects Appear Clearly, but Distant Objects Appear Blurry
National Eye Institute Eye Institute National Institutes Institutes of Health of Health Myopia Myopia, also known as nearsightedness, is a common type of refractive error where close objects appear clearly, but distant objects appear blurry. What is myopia? Myopia, also known as nearsightedness, is a common type of refractive error where close objects appear clearly, but distant objects appear blurry. What is high myopia? High myopia is a severe form of the condition. In high myopia, the eyeball stretches and becomes too long. This can lead to holes or tears in the retina and can also cause retinal detachment. Abnormal blood vessels may grow under the retina and cause changes in vision. People with high myopia need comprehensive dilated eye exams more often. Early detection and timely treatment can help prevent vision loss. Myopia 1 What is refraction? Refraction is the bending of light as it passes through one object to another. Vision occurs when light rays are bent (refracted) as they pass through the cornea and the lens. The light is then focused on the retina. The retina converts the light-rays into messages that are sent through the optic nerve to the brain. The brain interprets these messages into the images we see. What are refractive errors? In refractive errors, the shape of the eye prevents light from focusing on the retina. The length of the eyeball (longer or shorter), changes in the shape of the cornea, or aging of the lens can cause refractive errors. How does myopia develop? Myopia develops in eyes that focus images in front of the retina instead of on the retina, which results in blurred vision. -

COMPLEMENTARY THERAPY ASSESSMENT VISUAL TRAINING for REFRACTIVE ERRORS August 2013
COMPLEMENTARY THERAPY ASSESSMENT VISUAL TRAINING FOR REFRACTIVE ERRORS August 2013 SUMMARY DESCRIPTION OF VISUAL TRAINING Vision training consists of a variety of programs designed to enhance visual efficiency and processing. Vision training, or orthoptics, typically addresses how well both eyes work together. Eye exercises may include, muscle relaxation techniques, biofeedback, eye patches, eye massages, the use of under-corrected prescription lenses, and/or nutritional supplements. Training is most often provided by an optometrist. BENEFITS One randomized controlled trial (RCT) of biofeedback training for control of accommodation for myopia reported no statistically significant benefits from training (Level I evidence). Another RCT (2013), which investigated vision training modalities to evaluate changes in peripheral refraction profiles in myopes, also found no evidence of benefits (Level 1 evidence). In other studies undertaken over the last 60 years, an improvement in subjective visual acuity (VA) in myopes with no corresponding improvement in objective VA has been reported (Level II/III evidence). RISKS The only risk attributable to visual training is financial. Most health insurers do not cover visual training programs. At the start of treatment, the optometrist should provide a reasonable estimate of what improvement to expect and how long it will take. CONCLUSIONS There is Level I evidence that visual training for control of accommodation has no effect on myopia. In other studies (Level II/III evidence), an improvement in subjective VA for patients with myopia that have undertaken visual training has been shown, but no corresponding physiological cause for the improvement has been demonstrated. It is postulated that the improvements in myopic patients noted in these studies were due to improvements in interpreting blurred images, changes in mood or motivation, creation of an artificial contact lens by tear film changes, or a pinhole effect from miosis of the pupil. -

Speaker's Guide
Speaker’s Guide Living With Low Vision: What you should know Slide 1 Presenter Instructions: • Introduce yourself to the group. • Tell your audience how long the presentation will last. • Engage the audience by asking them to introduce themselves and to name one thing they would like to learn from this presentation. Talking Points: • The purpose of this presentation is to provide information about low vision, what can be done about it, and where to get more information. • After attending this presentation, you will be able to do the following: ❍❍ Identify signs that may signal vision loss. ❍❍ Define low vision and vision rehabilitation. ❍❍ Outline what you can do if you have low vision. ❍❍ List questions that are good to ask an eye care professional and/or specialist in low vision. Living With Low Vision Speaker’s Guide 1 7/14 Slide 2 Talking Point: • Many changes to vision are normal and common as you age. But losing vision or going blind is not a normal part of aging. Living With Low Vision Speaker’s Guide 7/14 Slide 3 Talking Points: • As we get older, our eyes and vision change. Some of these normal changes include: ❍❍ Losing the ability to focus, which makes it harder to perform tasks such as reading, writing, playing cards, and working on the computer. ❍❍ Noticing declining contrast and color sensitivity, making it harder to distinguish colors such as blue and black or distinguish where an object ends and its background begins. ❍❍ Needing more light to see well and more time to adjust to changing levels of light.