Treatment of Multiple Skin Conditions with Advanced Broadband Lightbbl
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Update on Challenging Disorders of Pigmentation in Skin of Color Heather Woolery-Lloyd, M.D
Update on Challenging Disorders of Pigmentation in Skin of Color Heather Woolery-Lloyd, M.D. Director of Ethnic Skin Care Voluntary Assistant Professor Miller/University of Miami School of Medicine Department of Dermatology and Cutaneous Surgery What Determines Skin Color? What Determines Skin Color? No significant difference in the number of melanocytes between the races 2000 epidermal melanocytes/mm2 on head and forearm 1000 epidermal melanocytes/mm2 on the rest of the body differences present at birth Jimbow K, Quevedo WC, Prota G, Fitzpatrick TB (1999) Biology of melanocytes. In I. M. Freedberg, A.Z. Eisen, K. Wolff,K.F. Austen, L.A. Goldsmith, S. I. Katz, T. B. Fitzpatrick (Eds.), Dermatology in General Medicine 5th ed., pp192-220, New York, NY: McGraw Hill Melanosomes in Black and White Skin Black White Szabo G, Gerald AB, Pathak MA, Fitzpatrick TB. Nature1969;222:1081-1082 Jimbow K, Quevedo WC, Prota G, Fitzpatrick TB (1999) Biology of melanocytes. In I. M. Freedberg, A.Z. Eisen, K. Wolff, K.F. Austen, L.A. Goldsmith, S. I. Katz, T. B. Fitzpatrick (Eds.), Dermatology in General Medicine 5th ed., pp192- 220, New York, NY: McGraw Hill Role of Melanin-Advantages Melanin absorbs and scatters energy from UV and visible light to protect epidermal cells from UV damage Disadvantages Inflammation or injury to the skin is almost immediately accompanied by alteration in pigmentation Hyperpigmentation Hypopigmentation Dyschromias Post-Inflammatory hyperpigmentation Acne Melasma Lichen Planus Pigmentosus Progressive Macular Hypomelanosis -

Clinicopathological Correlation of Acquired Hyperpigmentary Disorders
Symposium Clinicopathological correlation of acquired Dermatopathology hyperpigmentary disorders Anisha B. Patel, Raj Kubba1, Asha Kubba1 Department of Dermatology, ABSTRACT Oregon Health Sciences University, Portland, Oregon, Acquired pigmentary disorders are group of heterogenous entities that share single, most USA, 1Delhi Dermatology Group, Delhi Dermpath significant, clinical feature, that is, dyspigmentation. Asians and Indians, in particular, are mostly Laboratory, New Delhi, India affected. Although the classic morphologies and common treatment options of these conditions have been reviewed in the global dermatology literature, the value of histpathological evaluation Address for correspondence: has not been thoroughly explored. The importance of accurate diagnosis is emphasized here as Dr. Asha Kubba, the underlying diseases have varying etiologies that need to be addressed in order to effectively 10, Aradhana Enclave, treat the dyspigmentation. In this review, we describe and discuss the utility of histology in the R.K. Puram, Sector‑13, diagnostic work of hyperpigmentary disorders, and how, in many cases, it can lead to targeted New Delhi ‑ 110 066, India. E‑mail: and more effective therapy. We focus on the most common acquired pigmentary disorders [email protected] seen in Indian patients as well as a few uncommon diseases with distinctive histological traits. Facial melanoses, including mimickers of melasma, are thoroughly explored. These diseases include lichen planus pigmentosus, discoid lupus erythematosus, drug‑induced melanoses, hyperpigmentation due to exogenous substances, acanthosis nigricans, and macular amyloidosis. Key words: Facial melanoses, histology of hyperpigmentary disorders and melasma, pigmentary disorders INTRODUCTION focus on the most common acquired hyperpigmentary disorders seen in Indian patients as well as a few Acquired pigmentary disorders are found all over the uncommon diseases with distinctive histological traits. -

Dermatologic Manifestations of Hermansky-Pudlak Syndrome in Patients with and Without a 16–Base Pair Duplication in the HPS1 Gene
STUDY Dermatologic Manifestations of Hermansky-Pudlak Syndrome in Patients With and Without a 16–Base Pair Duplication in the HPS1 Gene Jorge Toro, MD; Maria Turner, MD; William A. Gahl, MD, PhD Background: Hermansky-Pudlak syndrome (HPS) con- without the duplication were non–Puerto Rican except sists of oculocutaneous albinism, a platelet storage pool de- 4 from central Puerto Rico. ficiency, and lysosomal accumulation of ceroid lipofuscin. Patients with HPS from northwest Puerto Rico are homozy- Results: Both patients homozygous for the 16-bp du- gous for a 16–base pair (bp) duplication in exon 15 of HPS1, plication and patients without the duplication dis- a gene on chromosome 10q23 known to cause the disorder. played skin color ranging from white to light brown. Pa- tients with the duplication, as well as those lacking the Objective: To determine the dermatologic findings of duplication, had hair color ranging from white to brown patients with HPS. and eye color ranging from blue to brown. New findings in both groups of patients with HPS were melanocytic Design: Survey of inpatients with HPS by physical ex- nevi with dysplastic features, acanthosis nigricans–like amination. lesions in the axilla and neck, and trichomegaly. Eighty percent of patients with the duplication exhibited fea- Setting: National Institutes of Health Clinical Center, tures of solar damage, including multiple freckles, stel- Bethesda, Md (a tertiary referral hospital). late lentigines, actinic keratoses, and, occasionally, basal cell or squamous cell carcinomas. Only 8% of patients Patients: Sixty-five patients aged 3 to 54 years were di- lacking the 16-bp duplication displayed these findings. -

A Genome-Wide Association Study Reveals a Locus for Bilateral Iridal Hypopigmentation in Holstein Friesian Cattle Anne K
Hollmann et al. BMC Genetics (2017) 18:30 DOI 10.1186/s12863-017-0496-4 RESEARCHARTICLE Open Access A genome-wide association study reveals a locus for bilateral iridal hypopigmentation in Holstein Friesian cattle Anne K. Hollmann1, Martina Bleyer2, Andrea Tipold3, Jasmin N. Neßler3, Wilhelm E. Wemheuer1, Ekkehard Schütz1 and Bertram Brenig1* Abstract Background: Eye pigmentation abnormalities in cattle are often related to albinism, Chediak-Higashi or Tietz like syndrome. However, mutations only affecting pigmentation of coat color and eye have also been described. Herein 18 Holstein Friesian cattle affected by bicolored and hypopigmented irises have been investigated. Results: Affected animals did not reveal any ophthalmological or neurological abnormalities besides the specific iris color differences. Coat color of affected cattle did not differ from controls. Histological examination revealed a reduction of melanin pigment in the iridal anterior border layer and stroma in cases as cause of iris hypopigmentation. To analyze the genetics of the iris pigmentation differences, a genome-wide association study was performed using Illumina BovineSNP50 BeadChip genotypes of the 18 cases and 172 randomly chosen control animals. A significant association on bovine chromosome 8 (BTA8) was identified at position 60,990,733 with a -log10(p) = 9.17. Analysis of genotypic and allelic dependences between cases of iridal hypopigmentation and an additional set of 316 randomly selected Holstein Friesian cattle controls showed that allele A at position 60,990,733 on BTA8 (P =4.0e–08, odds ratio = 6.3, 95% confidence interval 3.02–13.17) significantly increased the chance of iridal hypopigmentation. Conclusions: The clinical appearance of the iridal hypopigmentation differed from previously reported cases of pigmentation abnormalities in syndromes like Chediak-Higashi or Tietz and seems to be mainly of cosmetic character. -

Hydroxychloroquine-Associated Hyperpigmentation Mimicking Elder Abuse
Dermatol Ther (Heidelb) (2013) 3:203–210 DOI 10.1007/s13555-013-0032-z CASE REPORT Hydroxychloroquine-Associated Hyperpigmentation Mimicking Elder Abuse Philip R. Cohen To view enhanced content go to www.dermtherapy-open.com Received: June 17, 2013 / Published online: August 14, 2013 Ó The Author(s) 2013. This article is published with open access at Springerlink.com ABSTRACT cleared of suspected elder abuse. A skin biopsy of the patient’s dyschromia confirmed the Background: Hydroxychloroquine may result diagnosis of hydroxychloroquine-associated in cutaneous dyschromia. Older individuals hyperpigmentation. who are the victims of elder abuse can present Conclusion: Hyperpigmentation of skin, with bruising and resolving ecchymoses. mucosa, and nails can be observed in patients Purpose: The features of hydroxychloroquine- treated with antimalarials, including associated hyperpigmentation are described, hydroxychloroquine. Elder abuse is a significant the mucosal and skin manifestations of elder and underreported problem in seniors. abuse are reviewed, and the mucocutaneous Cutaneous findings can aid in the discovery of mimickers of elder abuse are summarized. physical abuse, sexual abuse, and self-neglect in Case Report: An elderly woman being treated elderly individuals. However, medication- with hydroxychloroquine for systemic lupus associated effects, systemic conditions, and erythematosus developed drug-associated black accidental external injuries can mimic elder and blue pigmentation of her skin. The abuse. Therefore, a complete medical history dyschromia was misinterpreted by her and appropriate laboratory evaluation, including clinician as elder abuse and Adult Protective skin biopsy, should be conducted when the Services was notified. The family was eventually diagnosis of elder abuse is suspected. Keywords: Abuse; Dyschromia; Elderly; P. -

Pigmented Contact Dermatitis and Chemical Depigmentation
18_319_334* 05.11.2005 10:30 Uhr Seite 319 Chapter 18 Pigmented Contact Dermatitis 18 and Chemical Depigmentation Hideo Nakayama Contents ca, often occurs without showing any positive mani- 18.1 Hyperpigmentation Associated festations of dermatitis such as marked erythema, with Contact Dermatitis . 319 vesiculation, swelling, papules, rough skin or scaling. 18.1.1 Classification . 319 Therefore, patients may complain only of a pigmen- 18.1.2 Pigmented Contact Dermatitis . 320 tary disorder, even though the disease is entirely the 18.1.2.1 History and Causative Agents . 320 result of allergic contact dermatitis. Hyperpigmenta- 18.1.2.2 Differential Diagnosis . 323 tion caused by incontinentia pigmenti histologica 18.1.2.3 Prevention and Treatment . 323 has often been called a lichenoid reaction, since the 18.1.3 Pigmented Cosmetic Dermatitis . 324 presence of basal liquefaction degeneration, the ac- 18.1.3.1 Signs . 324 cumulation of melanin pigment, and the mononucle- 18.1.3.2 Causative Allergens . 325 ar cell infiltrate in the upper dermis are very similar 18.1.3.3 Treatment . 326 to the histopathological manifestations of lichen pla- 18.1.4 Purpuric Dermatitis . 328 nus. However, compared with typical lichen planus, 18.1.5 “Dirty Neck” of Atopic Eczema . 329 hyperkeratosis is usually milder, hypergranulosis 18.2 Depigmentation from Contact and saw-tooth-shape acanthosis are lacking, hyaline with Chemicals . 330 bodies are hardly seen, and the band-like massive in- 18.2.1 Mechanism of Leukoderma filtration with lymphocytes and histiocytes is lack- due to Chemicals . 330 ing. 18.2.2 Contact Leukoderma Caused Mainly by Contact Sensitization . -

Light-Based Treatment of Pigmented Lesions E
CosmetiC teChnique Light-Based Treatment of Pigmented Lesions E. Victor Ross, MD Pigmented lesions are common among patients presenting to dermatologists. Fortunately, a large arsenal of light-based technology is available for the reduction and removal of these lesions. By developing a comprehensive understanding of the microanatomy of dyschromia, physicians can optimize protocols based on principles of laser-tissue interactions and reports in the literature. This article will examine the author’s experience and preferences in treating specific types of pigmented lesions with various lasers and light devices. Cosmet Dermatol.COS 2011;24:515-522. DERM ermatologists commonly treat patients laser and nonlaser devices can be employed, sometimes with pigmented lesions. A large arsenal with different wavelengths, spot sizes, and pulse widths, of light-based devices are available for the but still achieve similar results.1 reduction and removal of these lesions. Chemical peels and cryotherapy at one time were wor- The most important factor to consider thy opponents of the laser but can present challenges Dwhen choosing the best light source for the treatment of related to damage confinement. For generalized superfi- pigmentedDo lesions is the microanatomy Not of the dyschro- cial pigmentCopy reduction, chemical peeling in experienced mia. A crucial factor in treatment of excessive pigment hands is quite sufficient. However, in focal destruction, is having an understanding of the pigment distribution the agent often will extend beyond the perimeter of the with the lesion. Lesion microanatomy should be con- lesion, even with careful application. Cryotherapy also is sidered when strategizing for optimal removal. It also notoriously challenging to control. -

Atypical Variants of Mycosis Fungoides
Altınışık et al. Atypical Variants of Mycosis Fungoides REVIEW DOI: 10.4274/jtad.galenos.2021.09719 J Turk Acad Dermatol 2021;15(2):30-33 Atypical Variants of Mycosis Fungoides Dursun Dorukhan Altınışık, Özge Aşkın, Tuğba Kevser Uzunçakmak, Burhan Engin Istanbul University-Cerrahpasa, Cerrahpasa Faculty of Medicine, Department of Dermatology, Istanbul, Turkey ABSTRACT Mycosis fungoides (MF) is the most common type of cutaneous T-cell lymphoma (CTCL) and it is characterised by specific histological features. MF is in a spectrum of disorders which includes Sezary syndrome and other CTCL subtypes. Clinically and histopathologically it can imitate other T-cell mediated dermatosis hence making its diagnosis difficult. Due to different prognosis and difference in treatment strategies other subtypes of CTCL must be differentiated from MF. MF is a clinically indolent low-grade lymphoma which is seen in people aged between 55- 60 and it’s seen more commonly in men (2:1 ratio). Meanwhile other subtypes of MF like folliculotropic variant may show relatively a more aggressive course and our treatment strategy may differ. Keywords: Mycosis fungoides, Cutaneous T-cell lymphoma, Phototherapy, PUVA Introduction follicles frequently causing alopecia and in the paediatric population Mycosis fungoides (MF) is the most common type of cutaneous T-cell it tends to accompany hypopigmented patches and plaques. FMF lymphoma (CTCL) and it is characterised by specific histological preferentially involves the head and neck region however it can features [1]. MF is in a spectrum of disorders which includes Sezary sometimes involve the trunk or the extremities [6]. Patients with syndrome and other CTCL subtypes. Clinically and histopathologically FMF have significant pruritus which may be overlapped by S. -

Albinism: Modern Molecular Diagnosis
British Journal of Ophthalmology 1998;82:189–195 189 Br J Ophthalmol: first published as 10.1136/bjo.82.2.189 on 1 February 1998. Downloaded from PERSPECTIVE Albinism: modern molecular diagnosis Susan M Carden, Raymond E Boissy, Pamela J Schoettker, William V Good Albinism is no longer a clinical diagnosis. The past cytes and into which melanin is confined. In the skin, the classification of albinism was predicated on phenotypic melanosome is later transferred from the melanocyte to the expression, but now molecular biology has defined the surrounding keratinocytes. The melanosome precursor condition more accurately. With recent advances in arises from the smooth endoplasmic reticulum. Tyrosinase molecular research, it is possible to diagnose many of the and other enzymes regulating melanin synthesis are various albinism conditions on the basis of genetic produced in the rough endoplasmic reticulum, matured in causation. This article seeks to review the current state of the Golgi apparatus, and translocated to the melanosome knowledge of albinism and associated disorders of hypo- where melanin biosynthesis occurs. pigmentation. Tyrosinase is a copper containing, monophenol, mono- The term albinism (L albus, white) encompasses geneti- oxygenase enzyme that has long been known to have a cally determined diseases that involve a disorder of the critical role in melanogenesis.5 It catalyses three reactions melanin system. Each condition of albinism is due to a in the melanin pathway. The rate limiting step is the genetic mutation on a diVerent chromosome. The cutane- hydroxylation of tyrosine into dihydroxyphenylalanine ous hypopigmentation in albinism ranges from complete (DOPA) by tyrosinase, but tyrosinase does not act alone. -

Leukemia Cutis Masquerading As Vitiligo
Leukemia Cutis Masquerading as Vitiligo Marissa D. Newman, MD; Sandy Milgraum, MD Chronic myelomonocytic leukemia (CMML) is a Case Report hematologic stem cell disorder with myelodys- A 57-year-old man presented with hypopigmented plastic and myeloproliferative characteristics. macules over his left forearm that had gradually Extramedullary leukemic infiltration of the skin, appeared over 2 months. The patient’s CMML although uncommon in CMML, has prognos- was diagnosed 4 months prior to his presentation tic relevance. We report a unique case of a to us. There was no personal or family history patient with CMML who clinically presented of autoimmune disease. At the time of CMML with vitiligo that was histologically diagnosed diagnosis, the peripheral blood showed a marked as leukemia cutis. This case underscores the monocytosis of 1.33109 cells/L (reference range, necessity of early recognition of skin changes 0.2–0.83109 cells/L) and abnormal granulocytic in patients with hematologic disorders and the maturation. Bone marrow aspirate demonstrated differentiation of nonspecific skin lesions from decalcified hypercellular marrow, maturing trilineage leukemia cutis. hematopoiesis, and dysplastic megakaryocytes. Immu- Cutis. 2008;81:163-165. nophenotyping by flow cytometry confirmed the pres- ence of a large monocytic cluster expressing abnormal CD56 and monocytic antigens CD14, CD64, CD33, hronic myelomonocytic leukemia (CMML) and CD4. Fluorescent in situ hybridization and poly- is a clonal disorder of hematopoietic stem merase chain reaction were both negative for the C cells with features of myelodysplastic breakpoint cluster region–Abelson gene, BCR-ABL. syndrome (MDS) characterized by monocytosis Cytogenetic analysis revealed trisomy 8, loss of Y, and and refractory anemia with excess blasts, as well rearrangement of the short arm of 1. -
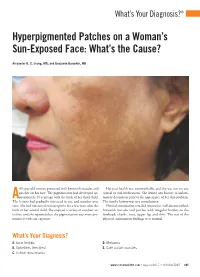
Hyperpigmented Patches on a Woman's Sun-Exposed Face
What’s Your Diagnosis?® Hyperpigmented Patches on a Woman’s Sun-Exposed Face: What’s the Cause? Alexander K. C. Leung, MD, and Benjamin Barankin, MD 45-year-old woman presented with brownish macules and Her past health was unremarkable, and she was not on any patches on her face. The pigmentation had developed ap- topical or oral medications. She denied any history of inflam- A proximately 10 years ago with the birth of her third child. matory dermatosis prior to the appearance of her skin problem. The lesions had gradually increased in size and number over The family history was not contributory. time. She had taken oral contraceptives for a few years after the Physical examination revealed symmetric, well-circumscribed, birth of her second child. She enjoyed a variety of outdoor ac- brownish macules and patches with irregular borders on the tivities, and she reported that the pigmentation was more pro- forehead, cheeks, nose, upper lip, and chin. The rest of the nounced with sun exposure. physical examination findings were normal. What’s Your Diagnosis? A. Solar lentigo D. Melasma B. Ephelides (freckles) E. Café au lait macules C. Actinic dyschromia www.consultant360.com • August 2017 • CONSULTANT 485 What’s Your Diagnosis?® Answer: Melasma A diagnosis of melasma was made. Wood lamp examination basement membrane disruption and dermal changes, indepen- showed accentuation of pigmentation suggestive of epidermal dent of UV radiation.1,17 pigmentation. The patient was treated with a series of trichlo- roacetic acid chemical peels, as well as a topical azelaic acid and HISTOPATHOLOGY a retinoid-hydroquinone-steroid (modified Kligman) formula- Three histologic patterns of pigmentation have been described: tion with significant, albeit incomplete, improvement. -

Review on Skin Hyperpigmentation: Etiology, Diagnosis and Treatment
J Pharm Sci Bioscientific Res. 2020. 10 (1):142-148 ISSN NO. 2271-3681 Review on Skin Hyperpigmentation: Etiology, Diagnosis and Treatment Sohan A. Patel*1, Jayant. B. Dave2, Timir Y. Mehta3 1. Assistant Professor, Department of Pharmacology, Smt. S M. Shah Pharmacy College, Amasaran, Mahedavad- Ahmedabad, Highway, Gujarat, India 2. Professor, Department of Quality Assurance, L. M. College of Pharmacy, Ahmedabad, Gujarat, India 3. Dermatologist, Samarpan Medical Research Organization, Modasa, Gujarat, India Article History: ABSTRACT: Received 29 April 2020 Hyperpigmentation is common dermatological condition. Skin color is determined Accepted 03 May 2020 Available online 11 May 2020 by melanin and other chromophores and is influenced by physical factors (ultraviolet radiation) and other endocrine, autocrine, and paracrine factors. Being Citation: the largest organ of the body, any abnormality in skin color can have impact on the Patel S. A., Dave J. B., Mehta T. Y., Review patients’ psychosocial impairment of life. In Indian population have verities of on Skin Hyperpigmentation: Etiology, Diagnosis and Treatment. J Pharm Sci hyperpigmentation condition on skin due to multifactorial region; hence, a Bioscientific Res. 2020. 10(1):142-148 multipronged approach is needed in such cases. The biggest challenge in such cases is to treat the hyperpigmentation itself; hence, counseling and general treatment *For Correspondence: (the use of broad-spectrum sunscreen, the avoidance of sun exposure, etc.) play Mr. Sohan A. Patel crucial role, and an interdisciplinary approach may be required, especially when Assistant professor, Department of the hyperpigmentation is due to a systemic cause. A thorough understanding of Pharmacology, Smt. S. M. Pharmacy the aetiology and management strategies of hyperpigmentation is of importance College, Amasaran, Bhumapura in caring for those afflicted and also in the development of new therapies.