Deep Vein Thrombosis (DVT)
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Deep Vein Thrombosis in Behcet's Disease
BRIEF PAPER Clinical and Experimental Rheumatology 2001; 19 (Suppl. 24): S48-S50. Deep vein thrombosis ABSTRACT stitute the most frequent vascular mani- Objective festation seen in 6.2 to 33 % cases of in Behcet’s disease We aimed to describe the epidemiologi - BD (1, 2). We carried out this study to cal and clinical aspects of deep vein d e t e rmine the fre q u e n cy, the cl i n i c a l M.H. Houman1 thrombosis (DVT) in Behçet’s disease characteristics and course of deep vein 1 (BD) and to determine the patients at thrombosis (DVT) in BD patients and I. Ben Ghorbel high risk for this complication. to define a subgroup of patients at high I. Khiari Ben Salah1 Methods risk for this complication. M. Lamloum1 Among 113 patients with BD according 2 to the international criteria for classifi - Patients and methods M. Ben Ahmed cation of BD, those with DVT were ret - The medical records of one hundred M. Miled1 rospectively studied.The diagnosis of and thirteen patients with BD were re- DVT was made in all cases using con - viewed in order to investigate the pa- 1Department of Internal Medicine. La ventional venous angiography, venous tient’s medical history, the clinical ma- Rabta Hospital, 2Department of Immuno- ultrasonography and/or thoracic or ab - nifestations and outcome of the disease logy, Institute Pasteur. Tunis, Tunisia. dominal computed tomograp hy. Pa - as well as the treatment prescribed.The Houman M Habib, MD; Ben Ghorbel tients were divided in two subgroups diagnosis of BD was made based on the Imed, MD; Khiari Ben Salah Imen; a c c o rding to the occurrence of DV T criteria established by the international Lamloum Mounir, MD; Ben Ahmed other than cereb ral thromboses. -

Lower Extremity Deep Venous Thrombosis
SECTION 5 Vascular System CHAPTER 34 Lower Extremity Deep Venous Thrombosis Ariel L. Shiloh KEY POINTS • Providers can accurately detect lower extremity deep venous thrombosis with point-of- care ultrasound after limited training. • Compression ultrasound exams are as accurate as traditional duplex and triplex vascular ultrasound exams. • Compression ultrasound exam at only two sites, the common femoral vein and popliteal vein, permits rapid and accurate assessment of deep venous thrombosis. Background care providers can perform lower extremity compression ultrasonography exams rapidly Venous thromboembolic disease (VTE) is a and with high diagnostic accuracy to detect common cause of morbidity and mortality in DVT. 7–13 A meta-analysis of 16 studies showed hospitalized patients and is especially preva- that point-of-care ultrasound can accurately lent in critically ill patients.1–3 Approximately diagnose lower extremity DVTs with a pooled 70% to 90% of patients with an identified source sensitivity of 96% and specificity of 97%.14 of pulmonary embolism (PE) have a proxi- Traditional vascular studies, the duplex mal lower extremity deep venous thrombosis and triplex exams, use a combination of (DVT). Conversely, 40% to 50% of patients two-dimensional (2D) imaging with compres- with a proximal DVT have a concurrent pul- sion along with the use of color and/or spectral monary embolism at presentation, and simi- Doppler ultrasound. More recent studies have larly, in only 50% of patients presenting with a demonstrated that 2D compression ultrasound PE can a DVT be found.4–6 exams alone yield similar accuracy as tradi- Point-of-care ultrasound is readily available tional duplex or triplex vascular studies.9,11,15–17 as a diagnostic tool for VTE. -

Skin Injuries – Can We Determine Timing and Mechanism?
Skin injuries – can we determine timing and mechanism? Jo Tully VFPMS Seminar 2016 What skin injuries do we need to consider? • Bruising • Commonest accidental and inflicted skin injury • Basic principles that can be applied when formulating opinion • Abrasions • Lacerations }we need to be able to tell the difference • Incisions • Stabs/chops • Bite marks – animal v human / inflicted v ‘accidental’ v self-inflicted Our role…. We are often/usually/always asked…………….. • “What type of injury is it?” • “When did this injury occur?” • “How did this injury occur?” • “Was this injury inflicted or accidental?” • IS THIS CHILD ABUSE? • To be able to answer these questions (if we can) we need knowledge of • Anatomy/physiology/healing - injury interpretation • Forces • Mechanisms in relation to development, plausibility • Current evidence Bruising – can we really tell which bruises are caused by abuse? Definitions – bruising • BLUNT FORCE TRAUMA • Bruise =bleeding beneath intact skin due to BFT • Contusion = bruise in deeper tissues • Haematoma - extravasated blood filling a cavity (or potential space). Usually associated with swelling • Petechiae =Pinpoint sized (0.1-2mm) hemorrhages into the skin due to acute rise in venous pressure • medical causes • direct forces • indirect forces Medical Direct Indirect causes mechanical mechanical forces forces Factors affecting development and appearance of a bruise • Properties of impacting object or surface • Force of impact • Duration of impact • Site - properties of body region impacted (blood supply, -
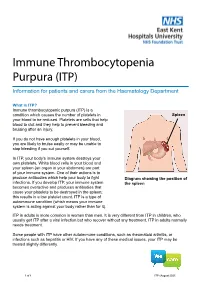
Immune Thrombocytopenia Purpura (ITP)
Immune Thrombocytopenia Purpura (ITP) Information for patients and carers from the Haematology Department What is ITP? Immune thrombocytopenic purpura (ITP) is a condition which causes the number of platelets in Spleen your blood to be reduced. Platelets are cells that help blood to clot and they help to prevent bleeding and bruising after an injury. If you do not have enough platelets in your blood, you are likely to bruise easily or may be unable to stop bleeding if you cut yourself. In ITP, your body’s immune system destroys your own platelets. White blood cells in your blood and your spleen (an organ in your abdomen) are part of your immune system. One of their actions is to produce antibodies which help your body to fight Diagram showing the position of infections. If you develop ITP, your immune system the spleen becomes overactive and produces antibodies that cause your platelets to be destroyed in the spleen; this results in a low platelet count. ITP is a type of autoimmune condition (which means your immune system is acting against your body rather than for it). ITP in adults is more common in women than men. It is very different from ITP in children, who usually get ITP after a viral infection but who recover without any treatment. ITP in adults normally needs treatment. Some people with ITP have other autoimmune conditions, such as rheumatoid arthritis, or infections such as hepatitis or HIV. If you have any of these medical issues, your ITP may be treated slightly differently. 1 of 8 ITP (August 2021) A normal platelet count is between 150 and 400 thousand million platelets per litre of blood. -

Difference Between Vein and Venule Key Difference - Vein Vs Venule
Difference Between Vein and Venule www.differencebetween.com Key Difference - Vein vs Venule The veins are the blood vessels that carry blood towards the heart. It always has a low blood pressure. Except the pulmonary and the umbilical veins, all the remaining veins carry the deoxygenated blood. On the contrary, the arteries carry blood away from the heart. The veins have valves in them to prevent the black flow of blood and to maintain unidirectional blood flow. They are less muscular, larger and are located closer to the skin. Venules are very smaller veins. They are the ones that collect blood from the capillaries. The collected blood will be directed to the larger and medium veins where the blood is transported towards the heart again. Many venules unite to form larger veins. The key difference between Vein and Venule is, the vein is a larger blood vessel that carries blood towards the heart while, the venule is a smaller minute blood vessel that drains blood from capillaries to the veins. What is a Vein? The veins are larger blood vessels present in throughout the body. The main function of veins is to carry oxygen-poor blood back into the heart. Veins are classified into some categories such as, superficial veins, pulmonary veins, deep veins, perforator veins, communicating veins and systematic veins. The wall of the vein is thinner and less elastic than the wall of an artery. The walls of the veins consist three layers of tissues which are named as tunica externa, tunica media, and tunica intima. Veins also have larger and irregular lumen. -

Peripheral Vascular Disease (PVD) Fact Sheet
FACT SHEET FOR PATIENTS AND FAMILIES Peripheral Vascular Disease (PVD) What is peripheral vascular disease? Vascular disease is disease of the blood vessels (arteries and veins). Peripheral vascular disease (PVD) affects The heart receives blood, the areas that are “peripheral,” or outside your heart. sends it to The most common types of PVD are: the lungs to get oxygen, • Carotid artery disease affects the arteries and pumps that carry blood to your brain. It occurs when it back out. one or more arteries are narrowed or blocked by plaque, a fatty substance that builds up inside artery walls. Carotid artery disease can increase Veins carry Arteries carry your risk of stroke. It can also cause transient blood to your oxygen-rich [TRANZ-ee-ent] ischemic [iss-KEE-mik] attacks (TIAs). heart to pick blood from up oxygen. your heart TIAs are temporary changes in brain function to the rest of that are sometimes called “mini-strokes.” your body. • Peripheral arterial disease (PAD) often affects the arteries to your legs and feet. It is also caused by Healthy blood vessels provide oxygen plaque buildup, and can for every part of your body. cause pain that feels like a dull cramp or heavy tiredness in your hips or legs when • Venous insufficiency affects the veins, usually you exercise or climb stairs. in your legs or feet. Your veins have valves that This pain is sometimes Damaged Healthy keepvalve blood fromvalve flowing backward as it moves called claudication. If PAD toward your heart. If the valves stop working, blood worsens, it can cause cold Plaque can build backs up in your body, usually in your legs. -

Bleeds and Bruises in Children with Haemophilia
Bleeds and Bruises in CHildren WiTH HaeMOPHilia MusCle ANd/or JoiNt Bleeds Call the parent/guardian P.r.i.C.e. siGNs oF A serious HeAd Bleed P : Protection * Headache. Lower Limb: Take weight off the joint or muscle * drowsiness. Upper Limb: No carrying using affected arm * Nausea. r : rest * Vomiting. • Rest means rest! * unsteady Balance. • Try not to allow use of the joint or muscle where * irritability. possible. * Confusion. * seizures. i : ice * loss of consciousness. • Regular ice packs can help with pain & reduce swelling. • Put an ice pack over the affected area for 20 minutes. Repeat every two hours. DO NOT leave the ice pack on for more than 20 minutes siGNs oF A soFt tissue DO NOT place ice pack directly on skin (Use a tea Bleed towel/cold pack cover) * Bruising, discolouring of skin. C : Compression * Mild swelling. • Use an elasticated bandage to compress the affected area to reduce swelling. e : elevation • Elevate the affected limb to help reduce swelling. siGNs oF AN ABdoMiNAl • Keep the affected joint or muscle above the level of the Bleed heart. * Bloody, black or tar-like First Aid bowel motions. * red or brown urine. Mouth & Gum Bleeds * Pain. These can be hard to control because clots that form are * Vomiting of blood (blood washed away by saliva or knocked off by the tongue or food. Try giving the child an ice cube or ice pop to suck. may be red or black). These bleeds may need treatment by parents or the treatment centre. Nosebleeds siGNs oF BleediNG iNto tHe Tilt head forward and pinch the bridge of the nose below the bone for 10 - 20 minutes and / or put an ice-pack on JoiNts or MusCles the bridge of the nose for not more than 5 minutes. -

Anatomy of the Large Blood Vessels-Veins
Anatomy of the large blood vessels-Veins Cardiovascular Block - Lecture 4 Color index: !"#$%&'(& !( "')*+, ,)-.*, $()/ Don’t forget to check the Editing File !( 0*"')*+, ,)-.*, $()/ 1$ ($&*, 23&%' -(0$%"'&-$(4 *3#)'('&-$( Objectives: ● Define veins, and understand the general principles of venous system. ● Describe the superior & inferior Vena Cava and their tributaries. ● List major veins and their tributaries in the body. ● Describe the Portal Vein. ● Describe the Portocaval Anastomosis Veins ◇ Veins are blood vessels that bring blood back to the heart. ◇ All veins carry deoxygenated blood. with the exception of the pulmonary veins(to the left atrium) and umbilical vein(umbilical vein during fetal development). Vein can be classified in two ways based on Location Circulation ◇ Superficial veins: close to the surface of the body ◇ Veins of the systemic circulation: NO corresponding arteries Superior and Inferior vena cava with their tributaries ◇ Deep veins: found deeper in the body ◇ Veins of the portal circulation: With corresponding arteries Portal vein Superior Vena Cava ◇Formed by the union of the right and left Brachiocephalic veins. ◇Brachiocephalic veins are formed by the union of internal jugular and subclavian veins. Drains venous blood from : ◇ Head & neck ◇ Thoracic wall ◇ Upper limbs It Passes downward and enter the right atrium. Receives azygos vein on its posterior aspect just before it enters the heart. Veins of Head & Neck Superficial veins Deep vein External jugular vein Anterior Jugular Vein Internal Jugular Vein Begins just behind the angle of mandible It begins in the upper part of the neck by - It descends in the neck along with the by union of posterior auricular vein the union of the submental veins. -

Isolated Plantar Vein Thrombosis Resembling a Corn with a Bruise
JE Hahm, et al pISSN 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 31, No. 1, 2019 https://doi.org/10.5021/ad.2019.31.1.66 CASE REPORT Isolated Plantar Vein Thrombosis Resembling a Corn with a Bruise Ji Eun Hahm, Kang Su Kim, Jae Won Ha, Chul Woo Kim, Sang Seok Kim Department of Dermatology, Kangdong Sacred Heart Hospital, College of Medicine, Hallym University, Seoul, Korea Plantar vein thrombosis, rarely-reported disease, is usually or callus, plantar fibromatosis, or plantar verruca1. Among accompanied by pain and tenderness in the plantar region laborers, they may develop from excess pressure on the and should be differentiated from other dermatological con- bony prominences of the feet, repetitive uneven friction ditions causing plantar pain, such as hemorrhagic corn/cal- from footwear, or gait abnormalities. Plantar vein throm- lus, plantar epidermal cyst, verruca, or plantar fibromatosis. bosis is a rare condition causing plantar pain. The exact A 52-year-old man presented with a violaceous tender sub- cause of plantar vein thrombosis is yet unclear, but predis- cutaneous nodule overlying a hyperkeratotic plaque on his posing conditions, such as prior trauma, surgery, paraneo- sole. Initially, he thought it was a corn and applied keratolytic plastic syndromes, or coagulation disorders have been agents, which failed to work. Sonography revealed a well-de- described. To date, there is no established treatment ex- marcated mass with increased peripheral vascularity. His cept surgical excision, but reportedly, nonsteroidal anti-in- pain was relieved after a complete wide excision, which con- flammatory drug or heparin with elastic bandage is known firmed the mass to be plantar vein thrombosis after histo- to be effective for symptomatic control2-5. -

Incidence of Deep Venous Thrombosis and Stratification of Risk Groups in A
ORIGINAL ARTICLE Incidence of deep venous thrombosis and stratification of risk groups in a university hospital vascular surgery unit Incidência de trombose venosa profunda e estratificação dos grupos de risco em serviço de cirurgia vascular de hospital universitário 1 1 1 2 Alberto Okuhara *, Túlio Pinho Navarro , Ricardo Jayme Procópio , José Oyama Moura de Leite Abstract Background: There is a knowledge gap with relation to the true incidence of deep vein thrombosis among patients undergoing vascular surgery procedures in Brazil. This study is designed to support the implementation of a surveillance system to control the quality of venous thromboembolism prophylaxis in our country. Investigations in specific institutions have determined the true incidence of deep vein thrombosis and identified risk groups, to enable measures to be taken to ensure adequate prophylaxis and treatment to prevent the condition. Objective: To study the incidence of deep venous thrombosis in patients admitted to hospital for non-venous vascular surgery procedures and stratify them into risk groups. Method: This was a cross-sectional observational study that evaluated 202 patients from a university hospital vascular surgery clinic between March 2011 and July 2012. The incidence of deep venous thrombosis was determined using vascular ultrasound examinations and the Caprini scale. Results: The mean incidence of deep venous thrombosis in vascular surgery patients was 8.5%. The frequency distribution of patients by venous thromboembolism risk groups was as follows: 8.4% were considered low risk, 17.3% moderate risk, 29.7% high risk and 44.6% were classified as very high risk. Conclusion: The incidence of deep venous thrombosis in vascular surgery patients was 8.5%, which is similar to figures reported in the international literature. -

Understanding Haemophilia
Understanding haemophilia Understanding haemophilia Contents Introduction 3 Haemophilia and your child 4 What is haemophilia? 5 What causes haemophilia? 5 Can females have haemophilia? 6 Carriers 8 Who is affected by haemophilia? 9 How severe is haemophilia? 9 Signs and symptoms of haemophilia 11 How is haemophilia diagnosed? 14 Diagnosis 14 Treatment 16 Port-a-cath 19 Managing joint bleeds with PRICE 19 Gene therapy 21 Possible complications of haemophilia 22 Inhibitors 22 Joint damage 22 Medical and dental treatment 23 Surgery Circumcision Dental care Medicines Vaccinations Bleeding disorder card Living with haemophilia 26 Sport and exercise 27 School, college and work 28 Travel 29 Pregnancy and haemophilia 30 Glossary of terms 32 About The Haemophilia Society 33 2 Understanding haemophilia Introduction This booklet is about haemophilia A and B. It gives a general overview of haemophilia and information on diagnosing, treating and living with the condition that we hope will answer your main questions. It has been written for people directly affected by haemophilia and for anyone interested in learning about haemophilia. If you are a parent and your child has recently been diagnosed with haemophilia you may be feeling quite overwhelmed. Remember, you’re not alone and many families are facing the same concerns and issues. Please do get in touch – we have lots of support and information available as well as services for parents and children. You can find out more via our website or Facebook pages, by emailing [email protected] or calling us on 020 7939 0780. The outlook is now the best it has ever been for people with haemophilia in the UK. -

What Is Dvt? Deep Vein Thrombosis (DVT) Occurs When an Abnormal Blood Clot Forms in a Large Vein
What is DVt? Deep vein thrombosis (DVT) occurs when an abnormal blood clot forms in a large vein. These clots usually develop in the lower leg, thigh, or pelvis, but can also occur in other large veins in the body. If you develop DVT and it is diagnosed correctly and quickly, it can be treated. However, many people do not know if they are at risk, don’t know the symptoms, and delay seeing a healthcare professional if they do have symptoms. CAn DVt hAppen to me? Anyone may be at risk for DVT but the more risk factors you have, the greater your chances are of developing DVT. Knowing your risk factors can help you prevent DVt: n Hospitalization for a medical illness n Recent major surgery or injury n Personal history of a clotting disorder or previous DVT n Increasing age this is serious n Cancer and cancer treatments n Pregnancy and the first 6 weeks after delivery n Hormone replacement therapy or birth control products n Family history of DVT n Extended bed rest n Obesity n Smoking n Prolonged sitting when traveling (longer than 6 to 8 hours) DVt symptoms AnD signs: the following are the most common and usually occur in the affected limb: n Recent swelling of the limb n Unexplained pain or tenderness n Skin that may be warm to the touch n Redness of the skin Since the symptoms of DVT can be similar to other conditions, like a pulled muscle, this often leads to a delay in diagnosis. Some people with DVT may have no symptoms at all.