Paediatric Cookbook
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Inflammatory Or Infectious Hair Disease? a Case of Scalp Eschar and Neck Lymph Adenopathy After a Tick Bite
Case Report ISSN: 2574 -1241 DOI: 10.26717/BJSTR.2021.35.005688 Adherent Serous Crust of the Scalp: Inflammatory or Infectious Hair Disease? A Case of Scalp Eschar and Neck Lymph Adenopathy after a Tick Bite Starace M1, Vezzoni R*2, Alessandrini A1 and Piraccini BM1 1Dermatology - IRCCS, Policlinico Sant’Orsola, Department of Specialized, Experimental and Diagnostic Medicine, Alma Mater Studiorum, University of Bologna, Italy 2Dermatology Clinic, Maggiore Hospital, University of Trieste, Italy *Corresponding author: Roberta Vezzoni, Dermatology Clinic, Maggiore Hospital, University of Trieste, Italy ARTICLE INFO ABSTRACT Received: Published: April 17, 2021 The appearance of a crust initially suggests inflammatory scalp diseases, although infectious diseases such as impetigo or insect bites should also be considered among April 27, 2021 the differential diagnoses. We report a case of 40-year-old woman presentedB. Burgdorferi to our, Citation: Starace M, Vezzoni R, Hair Disease Outpatient Service with an adherent serous crust on the scalp and lymphadenopathy of the neck. Serological tests confirmed the aetiology of while rickettsia infection was excluded. Lyme borreliosis can mimic rickettsia infection Alessandrini A, Piraccini BM. Adherent and may present as scalp eschar and neck lymphadenopathy after a tick bite (SENLAT). Serous Crust of the Scalp: Inflammatory Appropriate tests should be included in the diagnostic workup of patients with necrotic or Infectious Hair Disease? A Case of Scalp scalpKeywords: eschar in order to promptly set -

Erythema Marginatum
Figurative Erythemas Michelle Goedken, DO Affiliated Dermatology Scottsdale, AZ Figurative Erythemas • Erythema annulare centrifugum • Erythema marginatum • Erythema migrans • Erythema gyratum repens • Erythema multiforme Erythemas • Erythemas represent a change in the color of the skin that is due to the dilation of blood vessels, especially those in the papillary and reticular dermis • The color is blanchable and most last for days to months • Figurative erythemas have an annular, arciform or polycyclic appearance ERYTHEMA ANNULARE CENTRIFUGUM ERYTHEMA ANNULARE CENTRIFUGUM • Pathogenesis: EAC represents a reaction pattern or hypersensitivity to one of many antigens – IL-2 and TNF-alpha may have a role – Most patients do not have an underlying disease identified ERYTHEMA ANNULARE CENTRIFUGUM • Associated with: – Infection » Dermatophytes and other fungi (Candida and Penicillium in blue cheese) » Viruses: poxvirus, EBV, VZV, HIV » Parasites and ectoparasites – Drugs: diuretics, antimalarials, gold, NSAIDs, finasteride, amitriptyline, etizolam, Ustekinumab (2012) ERYTHEMA ANNULARE CENTRIFUGUM – Foods – Autoimmune endocrinopathies – Neoplasms (lymphomas and leukemias) – Pregnancy – Hypereosinophilic syndrome – Lupus (2014) ERYTHEMA ANNULARE CENTRIFUGUM http://www.dermaamin.com Rongioletti, F., Fausti, V., & Parodi, A ERYTHEMA ANNULARE CENTRIFUGUM • 2 major forms: – Superficial: classic trailing scale, may have associated pruritus – Deep: infiltrated borders, usually no scale, edges are elevated, usually not pruritic ERYTHEMA ANNULARE CENTRIFUGUM -
Belly Button…
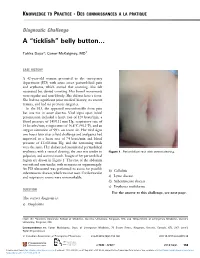
KNOWLEDGE TO PRACTICE DES CONNAISSANCES À LA PRATIQUE Diagnostic Challenge A “ticklish” belly button… Tahira Daya*; Conor McKaigney, MD† CASE HISTORY A 42-year-old woman presented to the emergency department (ED) with acute onset periumbilical pain and erythema, which started that morning. She felt nauseated but denied vomiting. Her bowel movements were regular and non-bloody. She did not have a fever. She had no significant prior medical history, no recent trauma, and had no previous surgeries. In the ED, she appeared uncomfortable from pain but was not in acute distress. Vital signs upon initial presentation included a heart rate of 120 beats/min, a blood pressure of 145/111 mm Hg, respiratory rate of 16 breaths/min, temperature of 36.8°C (98.2°F), and an oxygen saturation of 99% on room air. Her vital signs two hours later after a fluid challenge and analgesics had improved to a heart rate of 74 beats/min and blood pressure of 132/83 mm Hg, and the remaining vitals were the same. Her abdomen demonstrated periumbilical erythema, with a central clearing; the area was tender to Figure 1. Periumbilical rash with central clearing. palpation, and warm to touch. Images of her periumbilical region are shown in Figure 1. The rest of the abdomen was soft and non-tender, with no masses or organomegaly. An ED ultrasound was performed to assess for possible b) Cellulitis subcutaneous abscess, which was not seen. Cardiovascular and respiratory exams were unremarkable. c) Lyme disease d) Subcutaneous abscess e) Erythema multiforme QUESTION For the answer to this challenge, see next page. -

Lyme Disease Diagnostic Support Tool
1 / 11 For further details, click on the DIAGNOSTIC SUPPORT TOOL underlined words. Localized and disseminated stages of Lyme disease This diagnostic support tool is intended mainly for primary care clinicians. It is provided for information purposes only and should not replace the judgement of the clinician who performs the activities reserved under a statute or regulation. The recommendations in this tool were developed using a systematic process and are supported by the scientific literature and the knowledge and experience of Québec health professionals, experts and patients. For further details, go to the “Publications” section of INESSS’s website inesss.qc.ca. This tool does not deal with other tick-borne infections or with the much-debated form of Lyme disease, which is sometimes referred to as the chronic form. WHAT IS LYME DISEASE ? WHAT ARE THE DIFFERENT STAGES OF THE DISEASE? GENERAL INFORMATION • Lyme disease is an infectious disease caused by bacterial Localized stage (sometimes called the early stage): Beginning Patient with a tick genospecies of Borrelia burgdorferi, which are transmitted of the infection before dissemination of the bacteria in the • If tick is attached, refer to the procedure for removing it. to humans by black-legged ticks that are carriers. bloodstream. • Refer to the tick surveillance procedure. • Main manifestation observed: • It is a notifiable disease (MADO) • Consult the decision support tool or the Québec’s national and is on the increase in Québec. Not always present or noticed. medical protocol on post-exposure prophylaxis. • It can affect several anatomical systems at the same time. If present, usually appears • Identifying the tick and obtaining proof that it carries of Lym 3 to 30 days after infection or e d B. -

Lyme Disease
Volume 91 No. 7 July 2008 Lyme Disease UNDER THE JOINT VOLUME 91 NO. 7 July 2008 EDITORIAL SPONSORSHIP OF: Medicine Health The Warren Alpert Medical School of Brown University HODE SLAND Edward J. Wing, MD, Dean of Medicine R I & Biological Science PUBLICATION OF THE RHODE ISLAND MEDICAL SOCIETY Rhode Island Department of Health David R. Gifford, MD, MPH, Director Quality Partners of Rhode Island Richard W. Besdine, MD, Chief Medical Officer COMMENTARIES Rhode Island Medical Society Nick Tsiongas, MD, MPH, President 206 When Is a Somatic Disorder Psychiatric? Joseph H. Friedman, MD EDITORIAL STAFF Joseph H. Friedman, MD 207 The Awkward Birth Pangs of Bolero Editor-in-Chief Stanley M. Aronson, MD Joan M. Retsinas, PhD Managing Editor CONTRIBUTIONS Stanley M. Aronson, MD, MPH SPECIAL ISSUE: Lyme Disease Editor Emeritus Guest Editors: Jerome Larkin, MD, and Jennifer Mitty, MD, MPH EDITORIAL BOARD 208 Introduction: Lyme Disease Stanley M. Aronson, MD, MPH Jerome Larkin, MD, and Jennifer Mitty, MD, MPH Jay S. Buechner, PhD John J. Cronan, MD 209 Ticks and Tick-Related Illness James P. Crowley, MD Jerome M. Larkin, MD Edward R. Feller, MD 212 Lyme Disease In Children and Pregnant Women John P. Fulton, PhD Peter A. Hollmann, MD Jerome M. Larkin, MD Sharon L. Marable, MD, MPH 213 Musculoskeletal Manifestations of Lyme Disease Anthony E. Mega, MD Imad Bitar, MD, and Edward V. Lally, MD Marguerite A. Neill, MD Frank J. Schaberg, Jr., MD 216 Neurological Complications of Lyme Disease Lawrence W. Vernaglia, JD, MPH Syed Rizvi, MD, and Amanda Diamond, MD Newell E. Warde, PhD 219 Updates and Controversy In the Treatment of Lyme Disease OFFICERS Jennifer Mitty, MD, MPH, and David Margolius Nick Tsiongas, MD, MPH President COLUMNS Diane R. -

Research Article Bull's-Eye and Nontarget Skin Lesions of Lyme
Hindawi Publishing Corporation Dermatology Research and Practice Volume 2012, Article ID 451727, 6 pages doi:10.1155/2012/451727 Research Article Bull’s-Eye and Nontarget Skin Lesions of Lyme Disease: An Internet Survey of Identification of Erythema Migrans John N. Aucott,1 Lauren A. Crowder,2 Victoria Yedlin,2 and Kathleen B. Kortte3 1 Department of Medicine, Johns Hopkins University, 10755 Falls Road, Suite 200, Lutherville, MD 21093, USA 2 Division of Clinical Research, Lyme Disease Research Foundation, 10755 Falls Road, Suite 200, Lutherville, MD 21093, USA 3 Department of Physical Medicine and Rehabilitation, Johns Hopkins University School of Medicine, Phipps 174, 600 North Wolfe Street, Baltimore, MD 21287, USA Correspondence should be addressed to John N. Aucott, [email protected] Received 27 June 2012; Accepted 15 August 2012 Academic Editor: Jag Bhawan Copyright © 2012 John N. Aucott et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Introduction. Lyme disease is an emerging worldwide infectious disease with major foci of endemicity in North America and regions of temperate Eurasia. The erythema migrans rash associated with early infection is found in approximately 80% of patients and can have a range of appearances including the classic target bull’s-eye lesion and nontarget appearing lesions. Methods.Asurvey was designed to assess the ability of the general public to distinguish various appearances of erythema migrans from non-Lyme rashes. Participants were solicited from individuals who visited an educational website about Lyme disease. -

Dermatology from the Outside in Rob Danoff, DO, MS, FACOFP, FAAFP
Dermatology from the Outside In Rob Danoff, DO, MS, FACOFP, FAAFP + A Pictorial Review of Primary Care Dermatology ACOFP Intensive Review Update 8-22-15 Rob Danoff, DO, MS, FACOFP, FAAFP + In the Beginning Proof that babies are delivered by storks + What’s the diagnosis? 1 + Erythema Toxicum Neonatorum “E-Tox” Benign transient self-limiting eruption in the newborn seen in 40% of healthy full-term infants Follicular aggregation of eosinophils and neutrophils Resemble flea bites (yellow/beige papule on an erythematous base) Presents within first four days of life, peak at 48 hours Most cases resolve within five to fourteen days No treatment necessary + What is the diagnosis? + Distribution Crawling Children in diapers – typicaly seen on elbows and knees Older children and adults – typically present in folds of skin opposite to the elbow and kneecap, but spares armpits Other areas commonly involved include the cheeks, neck, wrists, and ankles. 2 + Atopic Dermatitis / Eczema Treatment: Avoid triggers—cold, wet, irritants, emotional stress Aggressive hydration with cream based or petrolatum based moisturizer to restore skin barrier Less irritating soap Infants--Low potency corticosteroid ointments for maintenance Older children and adults—medium potency corticosteroid ointments, sparing the face Stronger corticosteroids ointments should be used for flares or refractory plaques short term only to avoid thinning of skin Calcineurin inhibitors (tacrolimus or picrolimus) –useful on face or eyelids Short course oral Prednisone only -

Annular Erythema As a Cutaneous Sign of Recurrent Ductal Breast Carcinoma, Misdiagnosed As Erythema Chronicum Migrans
Volume 26 Number 9| September 2020| Dermatology Online Journal || Case Presentation 26(9):7 Annular erythema as a cutaneous sign of recurrent ductal breast carcinoma, misdiagnosed as erythema chronicum migrans Zoltan Szep1-3, Juraj Majtan3 Affiliations: 1Department of Dermatovenerology, St. Elisabeth´s Oncological Institute and Slovak Medical University, Bratislava, Slovakia, 2Alpha Medical Ltd, Diagnostic Center of Clinical Pathology, Bratislava, Slovakia, 3Institute of Molecular Biology, Slovak Academy of Sciences, Bratislava, Slovakia Corresponding Author: Dr. Juraj Majtan, Institute of Molecular Biology, Slovak Academy of Sciences, Dubravska cesta 21, 845 06, Bratislava, Slovakia. Email: [email protected] axilla. After mastectomy, dissection of axillary lymph Abstract nodes, radiotherapy, and chemotherapy, the patient Annular erythema as a clinical manifestation of was in complete remission on long-term tamoxifen locoregional recurrence of breast cancer is extremely treatment. Five years later, a solitary 6×6cm annular rare. Only three papers with the description of five erythematous plaque with a raised red border was cases have been published in the current literature to detected in the left pectoral area (Figure 1A). The our knowledge. Herein, we describe two additional patient reported a tick bite at the site of the lesion; cases of annular erythema as a cutaneous sign of recurrent ductal breast carcinoma; both were serological examination (ELISA method) detected misdiagnosed as erythema chronicum migrans. IgM positivity and IgG negativity of anti-Borrelia antibodies. The dermatologist diagnosed erythema chronicum migrans and put the patient on oral Keywords: annular erythema breast cancer, metastasis, doxycycline with a dosage of 200mg daily for 21 erythema migrans Introduction Annular erythema as a clinical manifestation of locoregional recurrence of malignant tumor disease is extremely rare. -

RASH in INFECTIOUS DISEASES of CHILDREN Andrew Bonwit, M.D
RASH IN INFECTIOUS DISEASES OF CHILDREN Andrew Bonwit, M.D. Infectious Diseases Department of Pediatrics OBJECTIVES • Develop skills in observing and describing rashes • Recognize associations between rashes and serious diseases • Recognize rashes associated with benign conditions • Learn associations between rashes and contagious disease Descriptions • Rash • Petechiae • Exanthem • Purpura • Vesicle • Erythroderma • Bulla • Erythema • Macule • Enanthem • Papule • Eruption Period of infectivity in relation to presence of rash • VZV incubates 10 – 21 days (to 28 d if VZIG is given • Contagious from 24 - 48° before rash to crusting of all lesions • Fifth disease (parvovirus B19 infection): clinical illness & contagiousness pre-rash • Rash follows appearance of IgG; no longer contagious when rash appears • Measles incubates 7 – 10 days • Contagious from 7 – 10 days post exposure, or 1 – 2 d pre-Sx, 3 – 5 d pre- rash; to 4th day after onset of rash Associated changes in integument • Enanthems • Measles, varicella, group A streptoccus • Mucosal hyperemia • Toxin-mediated bacterial infections • Conjunctivitis/conjunctival injection • Measles, adenovirus, Kawasaki disease, SJS, toxin-mediated bacterial disease Pathophysiology of rash: epidermal disruption • Vesicles: epidermal, clear fluid, < 5 mm • Varicella • HSV • Contact dermatitis • Bullae: epidermal, serous/seropurulent, > 5 mm • Bullous impetigo • Neonatal HSV • Bullous pemphigoid • Burns • Contact dermatitis • Stevens Johnson syndrome, Toxic Epidermal Necrolysis Bacterial causes of rash -

Ectopic Erythema Migrans in an Adolescent with a Skin Disorder
Pediatric Oral Pathology Ectopic erythema migrans in an adolescent with a skin disorder Catherine M. Flaitz, DDS, MS Dr. Flaitz is a professor, Oral and Maxillofacial Pathology and Pediatric Dentistry, Department of Stomatology, University of Texas at Houston Health Science Center Dental Branch, Houston, Texas. Abstract Red and white circular lesions of the buccal and labial mucosa were observed in an adolescent. Periodically, these nontender patches would resolve and move to other oral sites. Detection of ectopic erythema migrans aided in the diagnosis of a bothersome skin condition. (Pediatr Dent 22:63-64, 2000.) Case history uring a routine oral examination, multiple red and white patches were observed on the buccal and labial Dmucosa in a healthy 16 year-old African-American female. Review of her medical history was positive for envi- ronmental allergies, chronic sinusitis, and eczema. Hypoallergenic soaps and lotions, loratadine, naproxen and oral Fig 1. Ectopic erythema migrans presenting as a circinate red and white contraceptives were the medications used by this teenager. In- lesion of the manibular labial mucosa. traoral examination revealed oval to circinate red patches with slightly raised white margins on the mandibular labial mucosa (figure 1) and bilateral, coalescing, red patches of the anterior buccal mucosa (figures 2 a, b). The patient was aware of in- creased surface roughness at these sites, but denied having any oral tenderness. These recurrent oral lesions would resolve in a couple weeks and then reappear at different mucosal sites. Except for localized gingivitis and a coated tongue, no other intraoral soft tissue abnormalities were observed. Mildly pru- ritic, hyperpigmented papules and plaques with scaly surfaces were noted around the hairline, hands and elbows. -

Overview of Tick-Borne Diseases
TAKE-HOME MEDICAL GRAND ROUNDS WILLIAM S. WILKE, MD, EDITOR POINTS FROM LECTURES BY CLEVELAND CLINIC AND VISITING FACULTY Tick trouble: Overview of tickrborne diseases ALAN J. TAEGE, MD positive until several weeks after the patient Department of Infectious Diseases, Cleveland Clinic has been infected; therefore, these tests must be used for confirmation, not screening. • ABSTRACT It is important for physicians to learn Tick-borne diseases can be severe or about the varying clinical characteristics and even fatal, but when identified early, the epidemiology of these diseases. In this most can be easily treated. Tick-borne article, I will first call attention to three of the diseases often present with nonspecific less familiar tick-borne diseases: Rocky symptoms. Therefore it is important for Mountain spotted fever, ehrlichiosis, and the primary care physician to be familiar babesiosis. I will conclude with an update on with the epidemiology of these diseases the most common of the tick-borne diseases, and their presentations. Although Lyme Lyme borreliosis. disease is the most common and well- • ROCKY MOUNTAIN SPOTTED FEVER known of the many tick-borne diseases, Rocky Mountain spotted fever, An acute febrile illness, Rocky Mountain ehrlichiosis, and babesiosis are also spotted fever is caused by Rickettsia rickettsii, a More threats throughout the United States. gram-negative intracellular bacillus transmit- Americans are ted by tick bites. The disease is misnamed: not S SUBURBS EXPAND and deer populations all patients develop rash, and fewer than 2% coming into 0continue to increase, more Americans of cases occur in Rocky Mountain states. contact with are coming into contact with rural problems Symptoms and course. -

Derm World: a Journey Through a "Rash" of Clinical Presentations
Derm World: A Journey Through a "Rash" of Clinical Presentations Rob Danoff, DO, MS, FACOFP, FAAFP Derm World: + A Journey Through a “Rash” of Clinical Presentations Rob Danoff DO, MS, FACOFP, FAAFP OMED 2015 + Cutaneous findings in the Newborn Or, what is this? 1 + What is this? + Cutis Marmorata Mottling of skin Transient phenomena Vascular response to cold with immature nervous system Superficial small blood vessels in the skin dilating (red color) and contracting (pale color) at the same time May persist for months Re-warming usually restores the skin to its normal appearance Occurs in about 50% of infants Generally resolves with increasing age and of no significance for most infants 2 + In the Beginning Proof that babies are delivered by storks + What’s the Diagnosis? 3 + Nevus simplex = Stork bite= Salmon patch Red dilitation of blood vessels often on eyelid, face, or nape of neck (stork bite) They are usually small flat patches of pink or red skin with poorly defined borders These exanthems are very common and occur in over 40% of all newborns The facial patches are sometimes referred to as an “angel's kiss” and tend to fade over the first year of life + Nevus simplex = Stork bite= Salmon patch Often deepen in color with crying, straining with defecation, breath holding or with changes in ambient temperature Not painful or itchy Benign course, reassurance, lighten with age Those on the eyelids and below towards the nose usually disappear by 2 to 3 years of age Salmon patches are rarely detected after age 6 years