**No Patient Handout Erythema Annulare Centrifugum
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Inflammatory Or Infectious Hair Disease? a Case of Scalp Eschar and Neck Lymph Adenopathy After a Tick Bite
Case Report ISSN: 2574 -1241 DOI: 10.26717/BJSTR.2021.35.005688 Adherent Serous Crust of the Scalp: Inflammatory or Infectious Hair Disease? A Case of Scalp Eschar and Neck Lymph Adenopathy after a Tick Bite Starace M1, Vezzoni R*2, Alessandrini A1 and Piraccini BM1 1Dermatology - IRCCS, Policlinico Sant’Orsola, Department of Specialized, Experimental and Diagnostic Medicine, Alma Mater Studiorum, University of Bologna, Italy 2Dermatology Clinic, Maggiore Hospital, University of Trieste, Italy *Corresponding author: Roberta Vezzoni, Dermatology Clinic, Maggiore Hospital, University of Trieste, Italy ARTICLE INFO ABSTRACT Received: Published: April 17, 2021 The appearance of a crust initially suggests inflammatory scalp diseases, although infectious diseases such as impetigo or insect bites should also be considered among April 27, 2021 the differential diagnoses. We report a case of 40-year-old woman presentedB. Burgdorferi to our, Citation: Starace M, Vezzoni R, Hair Disease Outpatient Service with an adherent serous crust on the scalp and lymphadenopathy of the neck. Serological tests confirmed the aetiology of while rickettsia infection was excluded. Lyme borreliosis can mimic rickettsia infection Alessandrini A, Piraccini BM. Adherent and may present as scalp eschar and neck lymphadenopathy after a tick bite (SENLAT). Serous Crust of the Scalp: Inflammatory Appropriate tests should be included in the diagnostic workup of patients with necrotic or Infectious Hair Disease? A Case of Scalp scalpKeywords: eschar in order to promptly set -

Skin Manifestation of SARS-Cov-2: the Italian Experience
Journal of Clinical Medicine Article Skin Manifestation of SARS-CoV-2: The Italian Experience Gerardo Cazzato 1 , Caterina Foti 2, Anna Colagrande 1, Antonietta Cimmino 1, Sara Scarcella 1, Gerolamo Cicco 1, Sara Sablone 3, Francesca Arezzo 4, Paolo Romita 2, Teresa Lettini 1 , Leonardo Resta 1 and Giuseppe Ingravallo 1,* 1 Section of Pathology, University of Bari ‘Aldo Moro’, 70121 Bari, Italy; [email protected] (G.C.); [email protected] (A.C.); [email protected] (A.C.); [email protected] (S.S.); [email protected] (G.C.); [email protected] (T.L.); [email protected] (L.R.) 2 Section of Dermatology and Venereology, University of Bari ‘Aldo Moro’, 70121 Bari, Italy; [email protected] (C.F.); [email protected] (P.R.) 3 Section of Forensic Medicine, University of Bari ‘Aldo Moro’, 70121 Bari, Italy; [email protected] 4 Section of Gynecologic and Obstetrics Clinic, University of Bari ‘Aldo Moro’, 70121 Bari, Italy; [email protected] * Correspondence: [email protected] Abstract: At the end of December 2019, a new coronavirus denominated Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) was identified in Wuhan, Hubei province, China. Less than three months later, the World Health Organization (WHO) declared coronavirus disease-19 (COVID-19) to be a global pandemic. Growing numbers of clinical, histopathological, and molecular findings were subsequently reported, among which a particular interest in skin manifestations during the course of the disease was evinced. Today, about one year after the development of the first major infectious foci in Italy, various large case series of patients with COVID-19-related skin Citation: Cazzato, G.; Foti, C.; manifestations have focused on skin specimens. -

Erythema Marginatum
Figurative Erythemas Michelle Goedken, DO Affiliated Dermatology Scottsdale, AZ Figurative Erythemas • Erythema annulare centrifugum • Erythema marginatum • Erythema migrans • Erythema gyratum repens • Erythema multiforme Erythemas • Erythemas represent a change in the color of the skin that is due to the dilation of blood vessels, especially those in the papillary and reticular dermis • The color is blanchable and most last for days to months • Figurative erythemas have an annular, arciform or polycyclic appearance ERYTHEMA ANNULARE CENTRIFUGUM ERYTHEMA ANNULARE CENTRIFUGUM • Pathogenesis: EAC represents a reaction pattern or hypersensitivity to one of many antigens – IL-2 and TNF-alpha may have a role – Most patients do not have an underlying disease identified ERYTHEMA ANNULARE CENTRIFUGUM • Associated with: – Infection » Dermatophytes and other fungi (Candida and Penicillium in blue cheese) » Viruses: poxvirus, EBV, VZV, HIV » Parasites and ectoparasites – Drugs: diuretics, antimalarials, gold, NSAIDs, finasteride, amitriptyline, etizolam, Ustekinumab (2012) ERYTHEMA ANNULARE CENTRIFUGUM – Foods – Autoimmune endocrinopathies – Neoplasms (lymphomas and leukemias) – Pregnancy – Hypereosinophilic syndrome – Lupus (2014) ERYTHEMA ANNULARE CENTRIFUGUM http://www.dermaamin.com Rongioletti, F., Fausti, V., & Parodi, A ERYTHEMA ANNULARE CENTRIFUGUM • 2 major forms: – Superficial: classic trailing scale, may have associated pruritus – Deep: infiltrated borders, usually no scale, edges are elevated, usually not pruritic ERYTHEMA ANNULARE CENTRIFUGUM -
Belly Button…
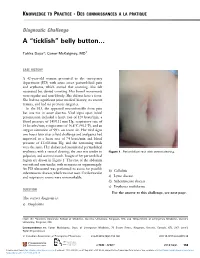
KNOWLEDGE TO PRACTICE DES CONNAISSANCES À LA PRATIQUE Diagnostic Challenge A “ticklish” belly button… Tahira Daya*; Conor McKaigney, MD† CASE HISTORY A 42-year-old woman presented to the emergency department (ED) with acute onset periumbilical pain and erythema, which started that morning. She felt nauseated but denied vomiting. Her bowel movements were regular and non-bloody. She did not have a fever. She had no significant prior medical history, no recent trauma, and had no previous surgeries. In the ED, she appeared uncomfortable from pain but was not in acute distress. Vital signs upon initial presentation included a heart rate of 120 beats/min, a blood pressure of 145/111 mm Hg, respiratory rate of 16 breaths/min, temperature of 36.8°C (98.2°F), and an oxygen saturation of 99% on room air. Her vital signs two hours later after a fluid challenge and analgesics had improved to a heart rate of 74 beats/min and blood pressure of 132/83 mm Hg, and the remaining vitals were the same. Her abdomen demonstrated periumbilical erythema, with a central clearing; the area was tender to Figure 1. Periumbilical rash with central clearing. palpation, and warm to touch. Images of her periumbilical region are shown in Figure 1. The rest of the abdomen was soft and non-tender, with no masses or organomegaly. An ED ultrasound was performed to assess for possible b) Cellulitis subcutaneous abscess, which was not seen. Cardiovascular and respiratory exams were unremarkable. c) Lyme disease d) Subcutaneous abscess e) Erythema multiforme QUESTION For the answer to this challenge, see next page. -

Lyme Disease Diagnostic Support Tool
1 / 11 For further details, click on the DIAGNOSTIC SUPPORT TOOL underlined words. Localized and disseminated stages of Lyme disease This diagnostic support tool is intended mainly for primary care clinicians. It is provided for information purposes only and should not replace the judgement of the clinician who performs the activities reserved under a statute or regulation. The recommendations in this tool were developed using a systematic process and are supported by the scientific literature and the knowledge and experience of Québec health professionals, experts and patients. For further details, go to the “Publications” section of INESSS’s website inesss.qc.ca. This tool does not deal with other tick-borne infections or with the much-debated form of Lyme disease, which is sometimes referred to as the chronic form. WHAT IS LYME DISEASE ? WHAT ARE THE DIFFERENT STAGES OF THE DISEASE? GENERAL INFORMATION • Lyme disease is an infectious disease caused by bacterial Localized stage (sometimes called the early stage): Beginning Patient with a tick genospecies of Borrelia burgdorferi, which are transmitted of the infection before dissemination of the bacteria in the • If tick is attached, refer to the procedure for removing it. to humans by black-legged ticks that are carriers. bloodstream. • Refer to the tick surveillance procedure. • Main manifestation observed: • It is a notifiable disease (MADO) • Consult the decision support tool or the Québec’s national and is on the increase in Québec. Not always present or noticed. medical protocol on post-exposure prophylaxis. • It can affect several anatomical systems at the same time. If present, usually appears • Identifying the tick and obtaining proof that it carries of Lym 3 to 30 days after infection or e d B. -

Diagnosis, Classification, and Management of Erythema
Arch Dis Child 2000;83:347–352 347 Diagnosis, classification, and management of Arch Dis Child: first published as 10.1136/adc.83.4.347 on 1 October 2000. Downloaded from erythema multiforme and Stevens–Johnson syndrome C Léauté-Labrèze, T Lamireau, D Chawki, J Maleville, A Taïeb Abstract become widely accepted that EM and SJS, as Background—In adults, erythema multi- well as toxic epidermal necrolysis, are all part of forme (EM) is thought to be mainly a single “EM spectrum”. In both EM and SJS, related to herpes infection and Stevens– pathological changes in the earliest skin lesion Johnson syndrome (SJS) to drug reac- consist of the accumulation of mononuclear tions. cells around the superficial dermal blood Aims—To investigate this hypothesis in vessels; epidermal damage is more characteris- children, and to review our experience in tic of EM with keratinocyte necrosis leading to the management of these patients. multilocular intraepidermal blisters.5 In fact, Methods—A retrospective analysis of 77 there is little clinical resemblance between paediatric cases of EM or SJS admitted to typical EM and SJS, and recently some authors the Children’s Hospital in Bordeaux be- have proposed a reconsideration of the “spec- tween 1974 and 1998. trum” concept and a return to the original Results—Thirty five cases, inadequately description.15–17 According to these authors, the documented or misdiagnosed mostly as term EM should be restricted to acrally urticarias or non-EM drug reactions were distributed typical targets or raised oedema- excluded. Among the remaining 42 pa- tous papules. Depending on the presence or tients (14 girls and 28 boys), 22 had EM (11 absence of mucous membrane erosions the EM minor and 11 EM major), 17 had SJS, cases may be classified as EM major or EM 16 and three had isolated mucous membrane minor. -

Fundamentals of Dermatology Describing Rashes and Lesions
Dermatology for the Non-Dermatologist May 30 – June 3, 2018 - 1 - Fundamentals of Dermatology Describing Rashes and Lesions History remains ESSENTIAL to establish diagnosis – duration, treatments, prior history of skin conditions, drug use, systemic illness, etc., etc. Historical characteristics of lesions and rashes are also key elements of the description. Painful vs. painless? Pruritic? Burning sensation? Key descriptive elements – 1- definition and morphology of the lesion, 2- location and the extent of the disease. DEFINITIONS: Atrophy: Thinning of the epidermis and/or dermis causing a shiny appearance or fine wrinkling and/or depression of the skin (common causes: steroids, sudden weight gain, “stretch marks”) Bulla: Circumscribed superficial collection of fluid below or within the epidermis > 5mm (if <5mm vesicle), may be formed by the coalescence of vesicles (blister) Burrow: A linear, “threadlike” elevation of the skin, typically a few millimeters long. (scabies) Comedo: A plugged sebaceous follicle, such as closed (whitehead) & open comedones (blackhead) in acne Crust: Dried residue of serum, blood or pus (scab) Cyst: A circumscribed, usually slightly compressible, round, walled lesion, below the epidermis, may be filled with fluid or semi-solid material (sebaceous cyst, cystic acne) Dermatitis: nonspecific term for inflammation of the skin (many possible causes); may be a specific condition, e.g. atopic dermatitis Eczema: a generic term for acute or chronic inflammatory conditions of the skin. Typically appears erythematous, -

Isotretinoin and the Risk of Erythema Multiforme Final SPC and PL
Isotretinoin and the risk of erythema multiforme Final SPC and PL wording agreed by the PhVWP in June 2010 Doc. Ref.: CMDh/PhVWP/021/2010 Rev 1 July 2010 SUMMARY OF PRODUCT CHARACTERISTICS Section 4.4 There have been post-marketing reports of severe skin reactions (e.g. erythema multiforme (EM), Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN)) associated with isotretinoin use. As these events may be difficult to distinguish from other skin reactions that may occur (see section 4.8), patients should be advised of the signs and symptoms and monitored closely for severe skin reactions. If a severe skin reaction is suspected, isotretinoin treatment should be discontinued. Section 4.8 Skin and subcutaneous tissues Cheilitis, dermatitis, dry skin, localised exfoliation, pruritus, rash disorders: erythematous, skin fragility (risk of frictional trauma) Very common (≥ 1/10) Rare (≥ 1/10 000,< 1/1000) Alopecia Acne fulminans, acne aggravated (acne flare), erythema (facial), exanthema, hair disorders, hirsutism, nail dystrophy, paronychia, Very Rare (≤ 1/10 000) photosensitivity reaction, pyogenic granuloma, skin hyperpigmentation, sweating increased, ∗ Erythema multiforme, Stevens-Johnson Syndrome, toxic Unknown epidermal necrolysis. PACKAGE LEAFLET Possible side effects Skin and hair problems Unknown frequency Serious skin rashes (erythema multiforme, Stevens- Johnson syndrome, and toxic epidermal necrolysis), which are potentially life-threatening and require immediate medical attention. These appear initially as circular patches often with central blisters usually on arms and hands or legs and feet, more severe rashes may include blistering of the chest and back. Additional symptoms such as infection of the eye (conjunctivitis) or ulcers of the mouth, throat or nose may occur. -

04Amersoncommondermatoses
Conflicts of Interest None Common Dermatoses in Children & Adults Erin Amerson, MD Department of Dermatology UC San Francisco Outline Impetigo Infections & Infestations Organism 50-70% staphylococcus aureus Remainder group A beta- Skin cancer hemolytic streptococcus or both 2 Forms: Common dermatologic disorders Honey-colored crusts Less common but important diseases Bullous Impetigo- staphylococcus 1 Impetigo Treatment Systemic Abx + topical therapy is best Soak off thick crusts, may use mupirocin oint Beta-lactamase resistant antibiotics x 7 days Dicloxacillin Cephalexin To eradicate nasal Staph carriage Rifampin 600 mg qd X 5 days with your other Abx OR Mupirocin (Bactroban) to nares bid Methicillin Resistant Staph Aureus (MRSA) 40-59% MRSA at UCSF/SFGH Culture for organism and sensitivities Consider if recurrent infection Oral antibiotics that still work: Doxycycline or minocycline Trimethoprim-sulfamethoxazole Clindamycin Can combine any of the above with rifampin Save IV Vanco or Linezolid for MRSA resistant to EVERYTHING 2 Groin Fold Rash DDx Tinea cruris Seborrheic dermatitis Erythrasma Intertrigo Candida Inverse psoriasis Fungal/Yeast Infections of the Groin Tinea Cruris Dermatophyte and Scaly, crusted plaque with central clearing Nystatin not effective Yeast Infections Imidizole/Allylamines x 2-4 weeks as for tinea corporis Candida Moister, more red, satellite pustules Drying agents like Domeboro’s soaks, then Nystatin/Imidizoles 3 Treatment of Onychomycosis Trichophyton rubrum Why treat? Confirm fungal infection before treating DDx: psoriasis, trauma, lichen planus No longer use Griseofulvin: 12-18 months rx & poor efficacy Ketoconazole: risk ↑ LFT’s with long-term use Treatment of Onychomycosis Nail Psoriasis Terbinafine (Lamisil) 250 mg/day x 3-4 months Pulsing being studied Liver toxicity Itraconazole (Sporonox) Pulse at 400 mg/day x 7 days/ mo x 3 months Drug-drug interactions Liver toxicity/CHF/$$$$ 4 Tinea Capitis Tinea Capitis Treatment What to look for: p.o. -

Lyme Disease
Volume 91 No. 7 July 2008 Lyme Disease UNDER THE JOINT VOLUME 91 NO. 7 July 2008 EDITORIAL SPONSORSHIP OF: Medicine Health The Warren Alpert Medical School of Brown University HODE SLAND Edward J. Wing, MD, Dean of Medicine R I & Biological Science PUBLICATION OF THE RHODE ISLAND MEDICAL SOCIETY Rhode Island Department of Health David R. Gifford, MD, MPH, Director Quality Partners of Rhode Island Richard W. Besdine, MD, Chief Medical Officer COMMENTARIES Rhode Island Medical Society Nick Tsiongas, MD, MPH, President 206 When Is a Somatic Disorder Psychiatric? Joseph H. Friedman, MD EDITORIAL STAFF Joseph H. Friedman, MD 207 The Awkward Birth Pangs of Bolero Editor-in-Chief Stanley M. Aronson, MD Joan M. Retsinas, PhD Managing Editor CONTRIBUTIONS Stanley M. Aronson, MD, MPH SPECIAL ISSUE: Lyme Disease Editor Emeritus Guest Editors: Jerome Larkin, MD, and Jennifer Mitty, MD, MPH EDITORIAL BOARD 208 Introduction: Lyme Disease Stanley M. Aronson, MD, MPH Jerome Larkin, MD, and Jennifer Mitty, MD, MPH Jay S. Buechner, PhD John J. Cronan, MD 209 Ticks and Tick-Related Illness James P. Crowley, MD Jerome M. Larkin, MD Edward R. Feller, MD 212 Lyme Disease In Children and Pregnant Women John P. Fulton, PhD Peter A. Hollmann, MD Jerome M. Larkin, MD Sharon L. Marable, MD, MPH 213 Musculoskeletal Manifestations of Lyme Disease Anthony E. Mega, MD Imad Bitar, MD, and Edward V. Lally, MD Marguerite A. Neill, MD Frank J. Schaberg, Jr., MD 216 Neurological Complications of Lyme Disease Lawrence W. Vernaglia, JD, MPH Syed Rizvi, MD, and Amanda Diamond, MD Newell E. Warde, PhD 219 Updates and Controversy In the Treatment of Lyme Disease OFFICERS Jennifer Mitty, MD, MPH, and David Margolius Nick Tsiongas, MD, MPH President COLUMNS Diane R. -

Oral Diseases Associated with Human Herpes Viruses: Aetiology, Clinical Features, Diagnosis and Management
www.sada.co.za / SADJ Vol 71 No. 6 CLINICAL REVIEW < 253 Oral diseases associated with human herpes viruses: aetiology, clinical features, diagnosis and management SADJ July 2016, Vol 71 no 6 p253 - p259 R Ballyram1, NH Wood2, RAG Khammissa3, J Lemmer4, L Feller5 ABSTRACT Human herpesviruses (HHVs) are very prevalent DNA ACRONYMS viruses that can cause a variety of orofacial diseases. EM: erythema multiforme Typically they are highly infectious, are contracted early in HHV: human herpes virus life, and following primary infection, usually persist in a latent form. Primary oral infections are often subclinical, but may PCR: polymerase chain reaction be symptomatic as in the case of herpes simplex virus- HSV, HHV-1: herpes simplex virus induced primary herpetic gingivostomatitis. Reactivation VZV, HHV-3: varicella-zoster virus of the latent forms may result in various conditions: herpes EBV, HHV-4: Epstein-Barr virus simplex virus (HSV) can cause recurrent herpetic orolabial CMV, HHV-5: cytomegalovirus lesions; varicella zoster virus (VZV) can cause herpes zoster; Epstein-Barr virus (EBV) can cause oral hairy Key words: herpes simplex virus, human herpes virus-8, leukoplakia; and reactivation of HHV-8 can cause Kaposi varicella zoster virus, Epstein-Barr virus, recurrent herpes sarcoma. In immunocompromised subjects, infections labialis, recurrent intraoral herpetic ulcers, treatment, val- with human herpesviruses are more extensive and aciclovir, aciclovir, famcicylovir. severe than in immunocompetent subjects. HSV and VZV infections are treated with nucleoside analogues aciclovir, valaciclovir, famciclovir and penciclovir. These agents INTRODucTION have few side effects and are effective when started The human herpesvirus (HHV) family comprises a diverse early in the course of the disease. -

Erythema Multiforme: Recognition and Management Kathryn P
Erythema Multiforme: Recognition and Management Kathryn P. Trayes, MD; Gillian Love, MD; and James S. Studdiford, MD Thomas Jefferson University Hospital, Philadelphia, Pennsylvania Erythema multiforme is an immune-mediated reaction that involves the skin and sometimes the mucosa. Classically described as target-like, the erythema multiforme lesions can be isolated, recur- rent, or persistent. Most commonly, the lesions of erythema multiforme present symmetrically on the extremities (especially on extensor surfaces) and spread centripetally. Infections, especially herpes simplex virus and Mycoplasma pneumoniae, and medications constitute most of the causes of erythema multiforme; immunizations and autoimmune diseases have also been linked to erythema multiforme. Erythema multiforme can be differentiated from urticaria by the duration of individual lesions. Ery- thema multiforme lesions are typically fixed for a minimum of seven days, whereas individual urticarial lesions often resolve within one day. Erythema multiforme can be confused with the more serious con- dition, Stevens-Johnson syndrome; however, Stevens-Johnson syndrome usually contains widespread erythematous or purpuric macules with blisters. The management of erythema multiforme involves symptomatic treatment with topical steroids or antihistamines and treating the underlying etiology, if known. Recurrent erythema multiforme associated with the herpes simplex virus should be treated with prophylactic antiviral therapy. Severe mucosal erythema multiforme can require hospitalization