Solitary Nodule with White Hairs
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
Another Rashmanaging ? Common Skin Problems in Primary Care: Ugh….Another Rash Kathleen Haycraft, DNP, FNP/PNP-BC, DCNP, FAANP Objectives
Another RashManaging ? Common Skin Problems in Primary Care: Ugh….Another Rash Kathleen Haycraft, DNP, FNP/PNP-BC, DCNP, FAANP Objectives At the completion of this session the learner will be able to: 1. Identify common skin rashes seen in dermatology 2. Differentiate between rashes that require urgent treatment and those that require monitored therapy. 3. Determine an appropriate treatment plan for common rashes Financial Disclosures and COI The speaker is on the advisory committee for: ABVIE CELGENE LILLY NOVARTIS PFIZER VALEANT Significance Dermatologic conditions are the number one reason to enter ambulatory walk in clinics The skin it the largest organ of the body and frequently is a measure of what is occurring internally Take a good history Duration What did it look like in the beginning and how has it progressed? Does anyone else in your immediate family or workers have a similar rash? Have you been ill and in what way? What have you treated the rash with prescription or over the counter medications? Take a good history Have they seen anyone and what diagnosis where you given? What is your medical history? What medicines do you take? Does it itch, hurt, scale, or asymptomatic? Give it a scale. How did it begin and what does has it changed (tie this into treatment history)? Is the patient sick? What does it looks like? Macule vs. Patch Papule, nodule, pustule, tumor Vesicle or Bulla Petechial or purpura Indurated vs. non-indurated Is it crusted…deep or superficial What pattern…. Blaschkos vs. dermatome,, symmetrical, central vs. caudal, reticular, annular vs. -
Dermoscopic Features of Trichoadenoma
Dermatology Practical & Conceptual Broadening the List of Basal Cell Carcinoma Mimickers: Dermoscopic Features of Trichoadenoma Riccardo Pampena1, Stefania Borsari1, Simonetta Piana2, Caterina Longo1,3 1 Centro Oncologico ad Alta Tecnologia Diagnostica, Azienda Unità Sanitaria Locale - IRCCS di Reggio Emilia, Italy 2 Pathology Unit, Azienda Unità Sanitaria Locale - IRCCS di Reggio Emilia, Italy 3 Department of Dermatology, University of Modena and Reggio Emilia, Modena, Italy Key words: trichoadenoma, basal cell carcinoma, adnexal tumors, dermoscopy Citation: Pampena R, Borsari S, Piana S, Longo C. Broadening the list of basal cell carcinoma mimickers: dermoscopic features of trichoadenoma. Dermatol Pract Concept. 2019;9(2):160-161. DOI: https://doi.org/10.5826/dpc.0902a17 Accepted: January 10, 2019; Published: April 30, 2019 Copyright: ©2019 Pampena et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Funding: This research was supported by Italian Ministry of Health (Project Code: NET-2011-02347213). Competing interests: The authors have no conflicts of interest to disclose. Authorship: All authors have contributed significantly to this publication. Corresponding author: Riccardo Pampena, MD, Centro Oncologico ad Alta Tecnologia Diagnostica, Azienda Unità Sanitaria Locale – IRCCS, Viale Risorgimento 80, 42123, Reggio Emilia, Italy. Email: [email protected] Introduction Case Presentation A wide spectrum of skin tumors may mimic basal cell carci- Dermoscopic evaluation was performed with a contact polar- noma (BCC) on both clinical and dermoscopic appearance. ized dermatoscope (DermLite Foto, 3Gen LLC, Dana Point, Among these, adnexal skin neoplasms and in particular CA, USA) and showed a general BCC-like appearance. -
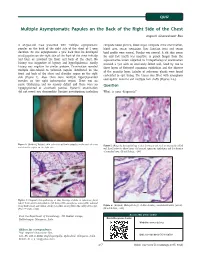
Multiple Asymptomatic Papules on the Back of the Right Side of the Chest Angoori Gnaneshwar Rao
QUIZ Multiple Asymptomatic Papules on the Back of the Right Side of the Chest Angoori Gnaneshwar Rao A 43-year-old male presented with multiple asymptomatic complete blood picture, blood sugar, complete urine examination, papules on the back of the right side of the chest of 1 year blood urea, serum creatinine, liver function tests and serum duration. He was asymptomatic a year back then he developed lipid profile were normal. Fundus was normal. A slit skin smear small papules on the right side of the front of the chest initially for acid fast bacilli was negative. A punch biopsy from the and later on involved the front and back of the chest. No representative lesion subjected to histopathological examination history was suggestive of leprosy and hyperlipidemias. Family revealed a cyst with an intricately folded wall, lined by two to history was negative for similar problem. Examination revealed three layers of flattened squamous epithelium and the absence multiple skin-colored to yellowish papules distributed on the of the granular layer. Lobules of sebaceous glands were found front and back of the chest and shoulder region on the right embedded in cyst lining. The lumen was filled with amorphous side [Figure 1]. Also, there were multiple hyperpigmented eosinophilic material and multiple hair shafts [Figures 2-4]. macules on the right infrascapular region. There was no nerve thickening and no sensory deficit and there were no Question hypopigmented or anesthetic patches. Systemic examination did not reveal any abnormality. Routine investigations including What is your diagnosis? (Original) Multiple skin-colored to yellowish papules on the back of chest Figure 1: Figure 2: (Original) Histopathology of skin showing a cyst with an intricately folded and shoulder region on the right side wall lined by two to three layers of flattened squamous epithelium and the absence of granular layer. -

Metastasis of Meningioma: a Rare Differential Diagnosis In
logy: Op go en n y A Lunger et al., Otolaryngol (Sunnyvale) 2017, 7:6 r c a c l e o s t DOI: 10.4172/2161-119X.1000333 s O Otolaryngology: Open Access ISSN: 2161-119X Case Report OpenOpen Access Access Metastasis of Meningioma: A Rare Differential Diagnosis in Subcutaneous Masses of the Scalp Alexander Lunger1*, Tarek Ismail1#, Adrian Dalbert2, Kirsten Mertz3, Thomas Weikert4, Dirk Johannes Schaefer1 and Ilario Fulco1 1Department of Plastic, Reconstructive, Aesthetic and Hand Surgery, University Hospital Basel, Basel, Switzerland 2Department of Otorhinolaryngology-Head and Neck Surgery, University Hospital Zurich, Zurich, Switzerland 3Department of Pathology, Kantonsspital Basel Land, Liestal, Switzerland 4Department of Radiology, University Hospital Basel, Switzerland Abstract Background: Subcutaneous masses of the scalp have a wide range of differential diagnosis. After removal of a meningioma in the patient’s history, scalp metastasis from the previously resected meningioma should be considered. Methods: A 86 year old patient presented with a local swelling on the left temporal forehead and no other clinical symptoms. Eleven years earlier an extra-axial meningioma was resected. The patient was receiving immunosuppressive therapy subsequent to kidney transplantation. After clinical examination and MRI, a lipoma was suspected. The mass was resected under local anesthesia. Results: Histopathology revealed a metastasis of the previously removed meningioma (WHO grade II). No further treatment was recommended. Clinical follow-up was without pathological findings so far. Conclusion: Scalp metastases of meningiomas are a rare finding. However, if patient history reveals removal of a meningioma, scalp metastasis must be a differential diagnosis for subcutaneous masses even years after the initial surgery. -

Eyelid Conjunctival Tumors
EYELID &CONJUNCTIVAL TUMORS PHOTOGRAPHIC ATLAS Dr. Olivier Galatoire Dr. Christine Levy-Gabriel Dr. Mathieu Zmuda EYELID & CONJUNCTIVAL TUMORS 4 EYELID & CONJUNCTIVAL TUMORS Dear readers, All rights of translation, adaptation, or reproduction by any means are reserved in all countries. The reproduction or representation, in whole or in part and by any means, of any of the pages published in the present book without the prior written consent of the publisher, is prohibited and illegal and would constitute an infringement. Only reproductions strictly reserved for the private use of the copier and not intended for collective use, and short analyses and quotations justified by the illustrative or scientific nature of the work in which they are incorporated, are authorized (Law of March 11, 1957 art. 40 and 41 and Criminal Code art. 425). EYELID & CONJUNCTIVAL TUMORS EYELID & CONJUNCTIVAL TUMORS 5 6 EYELID & CONJUNCTIVAL TUMORS Foreword Dr. Serge Morax I am honored to introduce this Photographic Atlas of palpebral and conjunctival tumors,which is the culmination of the close collaboration between Drs. Olivier Galatoire and Mathieu Zmuda of the A. de Rothschild Ophthalmological Foundation and Dr. Christine Levy-Gabriel of the Curie Institute. The subject is now of unquestionable importance and evidently of great interest to Ophthalmologists, whether they are orbital- palpebral specialists or not. Indeed, errors or delays in the diagnosis of tumor pathologies are relatively common and the consequences can be serious in the case of malignant tumors, especially carcinomas. Swift diagnosis and anatomopathological confirmation will lead to a treatment, discussed in multidisciplinary team meetings, ranging from surgery to radiotherapy. -

A Clinico-Histopathological Study of Cutaneous Appendageal Tumours
IP Indian Journal of Clinical and Experimental Dermatology 5 (2019) 206–210 Content available at: iponlinejournal.com IP Indian Journal of Clinical and Experimental Dermatology Journal homepage: www.innovativepublication.com Original Research Article A clinico-histopathological study of cutaneous appendageal tumours Gowda Monika M1, S Sathish K1, M Basavarajaiah D2,* 1Kempegowda Institute of Medical Sciences, Bengaluru, Karnataka, India 2Dept. of Dermatology, KVAFSU B Hebbal, Bidar, Karnataka, India ARTICLEINFO ABSTRACT Article history: The cutaneous appendageal tumors are an ideal subject for study from clinical and morphological point Received 01-08-2019 of view and so ubiquitous that they can affect people of all age group A histopathological study of 100 Accepted 13-08-2019 cases of cutaneous appendageal tumors was carried out at tertiary care hospital over 18 months. A Total Available online 14-09-2019 95 cases were benign and 5 cases were malignant tumors, constituting 95.0 % p<0.01 and 5.0 % p>0.01 respectively. Sweat gland tumors were the most common manifestation (79.0% ) p<0.01, followed by hair follicle tumors (20%) and eccrine duct tumors 1(1%). Male and female ratio was 27:73. The commonest Keywords: affected body site was head and neck region . The mean age was 36.58 1.22 years . Out of 95 cases cutaneous appendageal tumors of benign tumors, syringoma accounted for 48% (48), trichoepithelioma12 p<0.01, eccrine hydrocystoma malignant (11) p<0.01 ,trichofolliculoma, Apocrine hydrocystoma and nodular hidradenomaeach (4)p>0.01. Total histopathologically (39) p<0.01 are correlating both clinically and histopathologically and (61) p<0.01 are not correlating clinically clinically and histopathologically. -

The Way We Were the New Style Always Get an Informed Consent Always Ask About Allergies!
6/3/2019 The Way We Were The Expanding Optometric Scope: 1045-02-.12 PRIMARY EYE CARE PROCEDURES. For the Minor Surgical Procedures purpose of 1993 Public Acts Chapter 295 • The performance of primary eye care procedures rational to the Needles, Blades and Radio ‐ Waves treatment of conditions or diseases of the eye or eyelid is determined by the board to be those procedures that could be performed in the optometrist’s office or other health care facilities that would require no more than a topical anesthetic. Laser Jason Duncan, OD, FAAO surgery and radial keratotomy are excluded. • Authority: T.C.A. §§4-5-202, 4-5-204, 63-8-12, and Public Diplomate, American Board of Optometry Chapter 295, Acts of 1993. Administrative Associate Professor, Southern College of Optometry • History: Original rule filed February 14, 1993; effective April 30, 1994. The New Style • An optometrist who uses a local anesthetic in the manner allowed by this subsection shall provide to • The use of a local anesthetic in conjunction with the primary care the board of optometry proof that the optometrist treatment of an eyelid lesion; provided, however, no optometrist has current CPR certification by an organization shall use a local anesthetic for this purpose unless that optometrist has met the certification requirements set forth in 63‐8‐112(4) and approved by the board; provide, that the optometrist in the rules of the board of optometry for the administration of may meet this requirement by providing proof to the pharmaceutical agents in the performance of primary eye care procedures. -

The Best Diagnosis Is: H&E, Original Magnification 2
Dermatopathology Diagnosis The best diagnosis is: H&E, original magnification 2. a. adenoid cysticcopy carcinoma arising within a spiradenoma b. cylindroma and spiradenoma collision tumor c. microcysticnot change within a spiradenoma d. mucinous carcinoma arising within a spiradenoma Doe. trichoepithelioma and spiradenoma collision tumor CUTIS H&E, original magnification 100. PLEASE TURN TO PAGE 211 FOR DERMATOPATHOLOGY DIAGNOSIS DISCUSSION Amanda F. Marsch, MD; Jeffrey B. Shackelton, MD; Dirk M. Elston, MD Dr. Marsch is from the Department of Dermatology, University of Illinois at Chicago. Drs. Shackelton and Elston are from the Ackerman Academy of Dermatopathology, New York, New York. The authors report no conflict of interest. Correspondence: Amanda F. Marsch, MD, University of Illinois at Chicago, 808 S Wood St, Chicago, IL 60612 ([email protected]). 192 CUTIS® WWW.CUTIS.COM Copyright Cutis 2015. No part of this publication may be reproduced, stored, or transmitted without the prior written permission of the Publisher. Dermatopathology Diagnosis Discussion Trichoepithelioma and Spiradenoma Collision Tumor he coexistence of more than one cutaneous adnexal neoplasm in a single biopsy specimen Tis unusual and is most frequently recognized in the context of a nevus sebaceous or Brooke-Spiegler syndrome, an autosomal-dominant inherited disease characterized by cutaneous adnexal neoplasms, most commonly cylindromas and trichoepitheliomas.1-3 Brooke-Spiegler syndrome is caused by germline muta- tions in the cylindromatosis gene, CYLD, located on band 16q12; it functions as a tumor suppressor gene and has regulatory roles in development, immunity, and inflammation.1 Weyers et al3 first recognized the tendency for adnexal collision tumors to present in patients with Brooke-Spiegler syndrome; they reported a patient with Brooke-Spiegler syndrome with spirad- Figure 1. -

Pilomatricoma: a Case Report
Open Access Austin Journal of Dermatology Case Report Pilomatricoma: A Case Report Jayakar Thomas*, Tamilarasi S, Asha D and Zohra Begum C Abstract Department of Dermatology, Sree Balaji Medical College Pilomatricoma is a benign tumor that arises from hair follicle matrical cells. & Bharath University, India Involvement of the upper limb is relatively uncommon and can be mistaken for *Corresponding author: Jayakar Thomas, other soft tissue tumors. We report the case of a 12 year old boy, who presented Department of Dermatology, Sree Balaji Medical College with an asymptomatic firm nodule over the left arm whose histology was & Bharath University, Chennai 600044, India, Email: suggestive of Pilomatricoma. [email protected] Keywords: Pilomatricoma; Shadow cells; Ghost cells; Basaloid cells Received: April 05, 2015; Accepted: May 29, 2015; Published: June 02, 2015 Introduction 1). The neurovascular status of the left hand was noted to be intact; there were no other palpable masses in the extremities and no axillary Pilomatricoma also known as Pilomatrixoma or calcifying adenopathy was present. Excision biopsy was performed under epithelioma of Malherbe is a benign neoplasm, which is derived regional anesthesia. Grossly the tumor was white in appearance and from hair follicle matrix cells. These tumors are typically present well circumscribed. in the head and neck region, but also occur in the upper limbs and are rarely reported in other sites[1].Pilomatricoma represents as an Histopathology revealed a capsulated benign neoplasm over asymptomatic, solitary, firm to hard, freely mobile nodule of the the subcutis, composed of lobules ofirregularly shaped masses of dermis or subcutaneous tissue. These tumors are generally exhibits ghost or shadow cells, scattered basophilic cells that undergo abrupt no fixation to neighbouring tissues and have an osseous- or cartilage- keratinization forming ghost [shadow] cells and areas of calcification. -

2016 Essentials of Dermatopathology Slide Library Handout Book
2016 Essentials of Dermatopathology Slide Library Handout Book April 8-10, 2016 JW Marriott Houston Downtown Houston, TX USA CASE #01 -- SLIDE #01 Diagnosis: Nodular fasciitis Case Summary: 12 year old male with a rapidly growing temple mass. Present for 4 weeks. Nodular fasciitis is a self-limited pseudosarcomatous proliferation that may cause clinical alarm due to its rapid growth. It is most common in young adults but occurs across a wide age range. This lesion is typically 3-5 cm and composed of bland fibroblasts and myofibroblasts without significant cytologic atypia arranged in a loose storiform pattern with areas of extravasated red blood cells. Mitoses may be numerous, but atypical mitotic figures are absent. Nodular fasciitis is a benign process, and recurrence is very rare (1%). Recent work has shown that the MYH9-USP6 gene fusion is present in approximately 90% of cases, and molecular techniques to show USP6 gene rearrangement may be a helpful ancillary tool in difficult cases or on small biopsy samples. Weiss SW, Goldblum JR. Enzinger and Weiss’s Soft Tissue Tumors, 5th edition. Mosby Elsevier. 2008. Erickson-Johnson MR, Chou MM, Evers BR, Roth CW, Seys AR, Jin L, Ye Y, Lau AW, Wang X, Oliveira AM. Nodular fasciitis: a novel model of transient neoplasia induced by MYH9-USP6 gene fusion. Lab Invest. 2011 Oct;91(10):1427-33. Amary MF, Ye H, Berisha F, Tirabosco R, Presneau N, Flanagan AM. Detection of USP6 gene rearrangement in nodular fasciitis: an important diagnostic tool. Virchows Arch. 2013 Jul;463(1):97-8. CONTRIBUTED BY KAREN FRITCHIE, MD 1 CASE #02 -- SLIDE #02 Diagnosis: Cellular fibrous histiocytoma Case Summary: 12 year old female with wrist mass. -

Hidrocystoma Multiplex
Case Reports Hidrocystoma Multiplex Dr. W. K. Yu and puncture resulted in collapse of the cyst with Date: 13 October, 1999 drainage of clear watery fluid. Venue: Yaumatei Skin Centre Organizer: Social Hygiene Service, DH; Clinico-pathological Seminar Differential diagnoses The possible diagnoses for numerous asymptomatic small facial papules included hidrocystoma, plane warts, seborrhoeic keratoses, milia, CASE SUMMARY xanthelasma, syringoma, trichoepithelioma, tricholemmoma and sebaceous hyperplasia. History A 48-year-old housewife complained of multiple asymptomatic papules on her face for over ten years, Investigations and diagnosis gradually becoming more numerous. There was an Biopsy was done on one of the biggest papules increase in size and number of the papules on exposure beneath the left eye. Histology showed a small cyst of to heat or after exercise. The condition was worse in 0.2 cm in the dermis. The cyst was lined by a double summer. She had no family history of similar facial layer of polygonal cuboidal epithelial cells of the sweat eruption. gland with irregular border. No papillary invagination or tadpole-like strand was seen. The features were consistent with hidrocystoma multiplex (Figures 2 and Physical examination 3). There were numerous skin-coloured, small, smooth, oval or round papules of 1-3 mm in diameter on the face (Figure 1). They were most numerous around Management the eyes. Some of the lesions had a cystic appearance The patient was advised about the benign nature Figure 1: Multiple small cystic papules on the face Vol.8 No.2, June 2000 71 Case Reports Figure 2: Low power view showing a cystic tumour in the mid dermis. -

Epidermoid Cyst: Highlights on Diagnosis and Magnetic Resonance Imaging Features
EpidermoidCase cyst Report Epidermoid cyst: highlights on diagnosis and magnetic resonance imaging features Cisto epidermóide: processo de diagnóstico e características das imagens por ressonância magnética Abstract Larissa Santana Arantes Elias a Angélica Ferreira Oton-Leite a b Purpose: Epidermoid and dermoid cysts are extremely rare developmental cysts of a benign Clóvis Martins Silva a nature, which may occur anywhere in the body, although about 7% are found in the head Rejane Faria Ribeiro-Rotta Aline Carvalho Batista a and neck. This article reports a clinical case of a patient who had an epidermoid cyst and its Elismauro Francisco de Mendonça a magnetic resonance imaging (MRI) features. Case report: This case discusses an epidermoid cyst in a 36-year-old woman complaining about speech difficulty. Clinical examination revealed an extensive swelling on the floor of the mouth. MRI findings showed a cystic homogenous lesion located underneath the mylohyoid a Department of Oral Medicine (Oral Pathology), muscle which was removed by surgery. Histological examination of the mass confirmed the Dental School, Federal University of Goiás, diagnosis of an epidermoid cyst. Goiânia, GO, Brazil b Araújo Jorge Hospital, Association of Cancer Conclusion: We concluded that MRI was considered useful for a more accurate diagnosis Combat of Goiás, Goiânia, GO, Brazil prior to treatment. Key words: Epidermoid cyst; dermoid cyst; magnetic resonance images; differential diagnosis Resumo Proposta: Cistos epidermóide e dermóide são cistos de desenvolvimento extremamente raros, de natureza benigna, que podem ocorrer em qualquer região do corpo e somente 7% são encontrados na região de cabeça e pescoço. Este artigo apresenta o caso clínico de uma paciente que possuía um cisto epidermóide juntamente com as características das imagens por ressonância magnética.