Z-Palatoplasty (ZPP): a Technique for Patients Without Tonsils
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Surgical Treatment of Snoring and Obstructive Sleep Apnea Syndrome
Medical Policy Surgical Treatment of Snoring and Obstructive Sleep Apnea Syndrome Table of Contents Policy: Commercial Coding Information Information Pertaining to All Policies Policy: Medicare Description References Authorization Information Policy History Policy Number: 130 BCBSA Reference Number: 7.01.101 Related Policies None Policy Commercial Members: Managed Care (HMO and POS), PPO, and Indemnity Medicare HMO BlueSM and Medicare PPO BlueSM Members Uvulopalatopharyngoplasty (UPPP) may be MEDICALLY NECESSARY for the treatment of clinically significant obstructive sleep apnea syndrome (OSAS) in appropriately selected adult patients who have failed an adequate trial of continuous positive airway pressure (CPAP) or failed an adequate trial of an oral appliance (OA). Clinically significant OSA is defined as those patients who have: Apnea/hypopnea Index (AHI) or Respiratory Disturbance Index (RDI) 15 or more events per hour, or AHI or RDI 5 or more events and 14 or less events per hour with documented symptoms of excessive daytime sleepiness, impaired cognition, mood disorders or insomnia, or documented hypertension, ischemic heart disease, or history of stroke. Hyoid suspension, surgical modification of the tongue, and/or maxillofacial surgery, including mandibular- maxillary advancement (MMA), may be MEDICALLY NECESSARY in appropriately selected adult patients with clinically significant OSA and objective documentation of hypopharyngeal obstruction who have failed an adequate trial of continuous positive airway pressure (CPAP) or failed an adequate trial of an oral appliance (OA). Clinically significant OSA is defined as those patients who have: AHI or RDI 15 or more events per hour, or AHI or RDI 5 or more events and 14 or less events per hour with documented symptoms of excessive daytime sleepiness, impaired cognition, mood disorders or insomnia, or documented hypertension, ischemic heart disease, or history of stroke. -
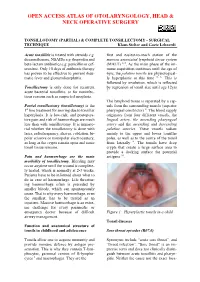
Tonsillotomy (Partial) and Complete Tonsillectomy
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY TONSILLOTOMY (PARTIAL) & COMPLETE TONSILLECTOMY - SURGICAL TECHNIQUE Klaus Stelter and Goetz Lehnerdt Acute tonsillitis is treated with steroids e.g. first and easiest-to-reach station of the dexamethasone, NSAIDs e.g. ibuprofen and mucosa associated lymphoid tissue system beta-lactam antibiotics e.g. penicillin or cef- (MALT) 2-4. As the main phase of the im- uroxime. Only 10 days of antibiotic therapy mune acquisition continues until the age of has proven to be effective to prevent rheu- 6yrs, the palatine tonsils are physiological- matic fever and glomerulonephritis. ly hyperplastic at this time 5, 6. This is followed by involution, which is reflected Tonsillectomy is only done for recurrent by regression of tonsil size until age 12yrs acute bacterial tonsillitis, or for noninfec- 7. tious reasons such as suspected neoplasia. The lymphoid tissue is separated by a cap- Partial tonsillectomy (tonsillotomy) is the sule from the surrounding muscle (superior 1st line treatment for snoring due to tonsillar pharyngeal constrictor) 8. The blood supply hyperplasia. It is low-risk, and postopera- originates from four different vessels, the tive pain and risk of haemorrhage are much lingual artery, the ascending pharyngeal less than with tonsillectomy. It is immate- artery and the ascending and descending rial whether the tonsillotomy is done with palatine arteries. These vessels radiate laser, radiofrequency, shaver, coblation, bi- mainly to the upper and lower tonsillar polar scissors or monopolar electrocautery, poles, as well as to the centre of the tonsil as long as the crypts remain open and some from laterally 9. -

Read Full Article
PEDIATRIC/CRANIOFACIAL Pharyngeal Flap Outcomes in Nonsyndromic Children with Repaired Cleft Palate and Velopharyngeal Insufficiency Stephen R. Sullivan, M.D., Background: Velopharyngeal insufficiency occurs in 5 to 20 percent of children M.P.H. following repair of a cleft palate. The pharyngeal flap is the traditional secondary Eileen M. Marrinan, M.S., procedure for correcting velopharyngeal insufficiency; however, because of M.P.H. perceived complications, alternative techniques have become popular. The John B. Mulliken, M.D. authors’ purpose was to assess a single surgeon’s long-term experience with a Boston, Mass.; and Syracuse, N.Y. tailored superiorly based pharyngeal flap to correct velopharyngeal insufficiency in nonsyndromic patients with a repaired cleft palate. Methods: The authors reviewed the records of all children who underwent a pharyngeal flap performed by the senior author (J.B.M.) between 1981 and 2008. The authors evaluated age of repair, perceptual speech outcome, need for a secondary operation, and complications. Success was defined as normal or borderline sufficient velopharyngeal function. Failure was defined as borderline insufficiency or severe velopharyngeal insufficiency with recommendation for another procedure. Results: The authors identified 104 nonsyndromic patients who required a pharyngeal flap following cleft palate repair. The mean age at pharyngeal flap surgery was 8.6 Ϯ 4.9 years. Postoperative speech results were available for 79 patients. Operative success with normal or borderline sufficient velopharyngeal function was achieved in 77 patients (97 percent). Obstructive sleep apnea was documented in two patients. Conclusion: The tailored superiorly based pharyngeal flap is highly successful in correcting velopharyngeal insufficiency, with a low risk of complication, in non- syndromic patients with repaired cleft palate. -

New Surgical Technique That Stabilizes Uvulopalatinal Segment in Patients with Loud Snore
Global Journal of Otolaryngology ISSN 2474-7556 Review Article Glob J Otolaryngol Volume 8 Issue 5 - July 2017 Copyright © All rights are reserved by Jon Garito DOI: 10.19080/GJO.2017.08.555748 New Surgical Technique That Stabilizes Uvulopalatinal Segment in Patients with Loud Snore Novak Vukoje1 and Jon Garito2* 1ENT office “dr Vukoje”, Petrovaradin, Serbia 2PhD, Inventer the dual Frequency device and the RF electrodes, USA Submission: July 01, 2017; Published: July 13, 2017 *Corresponding author: Jon Garito, PhD, Inventer the dual Frequency device and the RF electrodes, 1111 Crandon, BLVD, FL 33149, USA, Tel: ; Email: Abstract This method is author’s innovative technique which follows number of applied surgical procedures on palate and uvula with only goal to advance functional results and avoid complications like velofaringeal insufficiency. Task of this method is to solve uvulopalato lateral obstruction and to expand oropharyngeal airway. It was introduced in the year 2000 by Dr. Vukoje. It requires strict indications for application and correct selection of patients. Author has done this surgical procedure in the period from 2000 to 2004, on 36 patients (19 males and 17 females) with the average age of 45.3 years. Patient selection followed thorough diagnostic procedure (Figure 1). Figure 1: Ellman Surgitron 4.0 Dual RF, patented by Ellman International Company, Oceanside, New York, USA. (US Patent reference number # 5.954.686-Inventor dr Jon C. Garito). Interventions have been executed using radio wave surgical apparatus “Ellman Sugitron 4.0MHz combined with classical surgical technique. Follow-up, done two years after the surgery, imply that noisy sleep ceased to exist in 72.2% of cases (26) and in 19.4% of cases (7) it was reduced to tolerable level. -

Surgical Treatments for Obstructive Sleep Apnea (OSA) Policy Number: PG0056 ADVANTAGE | ELITE | HMO Last Review: 06/01/2021
Surgical Treatments for Obstructive Sleep Apnea (OSA) Policy Number: PG0056 ADVANTAGE | ELITE | HMO Last Review: 06/01/2021 INDIVIDUAL MARKETPLACE | PROMEDICA MEDICARE PLAN | PPO GUIDELINES This policy does not certify benefits or authorization of benefits, which is designated by each individual policyholder terms, conditions, exclusions and limitations contract. It does not constitute a contract or guarantee regarding coverage or reimbursement/payment. Self-Insured group specific policy will supersede this general policy when group supplementary plan document or individual plan decision directs otherwise. Paramount applies coding edits to all medical claims through coding logic software to evaluate the accuracy and adherence to accepted national standards. This medical policy is solely for guiding medical necessity and explaining correct procedure reporting used to assist in making coverage decisions and administering benefits. SCOPE X Professional _ Facility DESCRIPTION Sleep apnea is a disorder where breathing nearly or completely stops for periods of time during sleep. In obstructive sleep apnea (OSA), the brain sends the message to breathe, but there is a blockage to air flowing into the chest. It is a condition in which repetitive episodes of upper airway obstruction occur during sleep. The obstruction may be localized to one or two areas, or may encompass the entire upper airway passages to include the nasal cavity (nose), oropharynx (palate, tonsils, tonsillar pillars) and hypopharynx (tongue base). The hallmark symptom of OSA is excessive daytime sleepiness, and the typical clinical sign of OSA is snoring, which can abruptly cease and be followed by gasping associated with a brief arousal from sleep. The snoring resumes when the patient falls back to sleep, and the cycle of snoring/apnea/arousal may be repeated as frequently as every minute throughout the night. -

32 Surgical Treatment of Sleep-Related Breathing Disorders Donald M
32 Surgical Treatment of Sleep-Related Breathing Disorders Donald M. Sesso Department of Otolaryngology/Head and Neck Surgery, Stanford University Medical Center, Stanford, California, U.S.A. Nelson B. Powell and Robert W. Riley Department of Otolaryngology/Head and Neck Surgery, Stanford University Medical Center and Department of Behavioral Sciences, Division of Sleep Medicine, Stanford University School of Medicine, Stanford, California, U.S.A. INTRODUCTION Snoring, upper airway resistance syndrome (UARS), obstructive sleep apnea (OSA), and obstructive sleep apnea-hypopnea syndrome (OSAHS) are collectively referred to as sleep- related breathing disorders (SRBD). These terms describe a partial or complete obstruction of the upper airway during sleep. Patency of the pharyngeal airway is maintained by two opposing forces: negative intraluminal pressure and the activity of the upper airway musculature. Anatomical or central neural abnormalities can disrupt this delicate balance and result in compromise of the upper airway. This reduction of airway caliber may cause sleep fragmentation and subsequent behavioral derangements, such as excessive daytime sleepiness (EDS) (1–3). The goal of medical and surgical therapy is to alleviate this obstruction and increase airway patency. The first therapeutic modality employed to treat SRBD was surgery. Kuhlo described placement of a tracheotomy tube in an attempt to bypass upper airway obstruction in Pickwickian patients (4). Although effective, tracheotomy does not address the specific sites of pharyngeal collapse and is not readily accepted by most patients. These sites include the nasal cavity/nasopharynx, oropharynx, and hypopharynx. Often, multilevel obstruction is present. Consequently, the surgical armamentarium has evolved to create techniques that correct the specific anatomical sites of obstruction. -
Stanford University
STANFORD UNIVERSITY CURRICULUM VITAE Updated September 2019 NAME Stanley Yung-Chuan Liu, MD, DDS POSITION Assistant Professor of Otolaryngology Stanford University School of Medicine Co-Director, Sleep Surgery Fellowship EDUCATION Date Attended Institution Degree, Title Major 9/25/96 - 6/11/00 Stanford University B.S. Biology 8/28/02 - 6/17/07 University of California – San D.D.S. Dentistry Francisco (UCSF), School of Dentistry 9/12/07 - 6/10/11 University of California – San M.D. Medicine Francisco (UCSF), School of Medicine ACADEMIC APPOINTMENTS 6/2013 – 6/2014 Clinical Instructor Department of Otolaryngology, Stanford University School of Medicine Stanford, CA, USA 9/2014 – Present Assistant Professor (Medical Center Line) Department of Otolaryngology, Stanford University School of Medicine Stanford, CA, USA 9/2015 – Present Preceptor Department of Ophthalmology, Stanford University School of Medicine Stanford, CA, USA HOSPITAL APPOINTMENTS/AFFILIATIONS 6/2013 – Present Stanford Hospital and Clinics, Stanford, CA, USA 9/2015 – Present San Francisco Veterans Affairs Hospital, Palo Alto, CA, USA CERTIFICATION 4/2018 – Present Diplomate, American Board of Oral & Maxillofacial Surgery 4/2018 – Present Candidate, American College of Surgeons LICENSURE 2010 – Present California Dental License #59319 2012 – Present California Medical License # A122495 HONORS AND AWARDS 2004 Howard Hughes Medical Institute – NIH Research Scholarship (Cloister Program) 2009 Advanced Training Clinical Research Fellowship, UCSF School of Medicine, 2010 Lightowler -

DENTAL and ORAL SURGICAL PROCEDURES Policy Number: DENTAL 002.28 T2 Effective Date: March 1, 2017
UnitedHealthcare® Oxford Administrative Policy DENTAL AND ORAL SURGICAL PROCEDURES Policy Number: DENTAL 002.28 T2 Effective Date: March 1, 2017 Table of Contents Page Related Policy INSTRUCTIONS FOR USE .......................................... 1 Temporomandibular Joint Disorders BENEFIT CONSIDERATIONS ...................................... 2 PURPOSE ................................................................ 2 POLICY ................................................................... 2 PROCEDURES AND RESPONSIBILITIES ....................... 2 APPLICABLE CODES ................................................. 3 REFERENCES ........................................................... 7 POLICY HISTORY/REVISION INFORMATION ................. 7 INSTRUCTIONS FOR USE The services described in Oxford policies are subject to the terms, conditions and limitations of the member's contract or certificate. Unless otherwise stated, Oxford policies do not apply to Medicare Advantage members. Oxford reserves the right, in its sole discretion, to modify policies as necessary without prior written notice unless otherwise required by Oxford's administrative procedures or applicable state law. The term Oxford includes Oxford Health Plans, LLC and all of its subsidiaries as appropriate for these policies. Certain policies may not be applicable to Self-Funded members and certain insured products. Refer to the member specific benefit plan document or Certificate of Coverage to determine whether coverage is provided or if there are any exclusions or benefit -

Uvula in Snoring and Obstructive Sleep Apnea: Role and Surgical Intervention
Opinion American Journal of Otolaryngology and Head and Neck Surgery Published: 13 Apr, 2020 Uvula in Snoring and Obstructive Sleep Apnea: Role and Surgical Intervention Elbassiouny AM* Department of Otolaryngology, Cairo University, Egypt Abstract Objective: Currently, the consideration of the enlarged uvula as a cause of snoring and Obstructive Sleep Apnea (OSA) lacks data for objective interpretation. This article focused on some concepts on how we can manage the enlarged uvula in cases of snoring and OSA. The purpose of the present article is to discuss the cost benefits of uvular surgery versus its preservation. Conclusion: The direct correlation between the uvula and OSA needs to be reevaluated to maintain a balance between reserving its anatomical and physiological functions and surgically manipulating it as a part of palatopharyngeal surgery, yet further objective studies are needed to reach optimal results. Keywords: Uvula; Snoring; Obstructive sleep apnea Introduction The palatine uvula, usually referred to as simply the uvula, is that part of the soft palate that has an anatomical structure and serves some functions. Anatomically, the uvula, a conic projection from the back edge of the middle of the soft palate, is composed of connective tissue containing several racemose glands, and some muscular fibers, musculus uvulae muscle; arises from the posterior nasal spine and the palatine aponeurosis and inserts into the mucous membrane of the uvula. It contains many serous glands, which produce thin saliva [1]. Physiologically, the uvula serves several functions. First during swallowing, the soft palate and the uvula move together to close off the nasopharynx OPEN ACCESS and prevent food from entering the nasal cavity. -

CPC® Certification Review
CPC® Certification Review 1 CPT® CPT® copyright 2011 American Medical Association. All rights reserved. Fee schedules, relative value units, conversion factors and/or related components are not assigned by the AMA, are not part of CPT®, and the AMA is not recommending their use. The AMA does not directly or indirectly practice medicine or dispense medical services. The AMA assumes no liability for data contained or not contained herein. CPT is a registered trademark of the American Medical Association. 2 ICD-9-CM Coding 3 NEC vs. NOS • NEC Not elsewhere classifiable “We know what’s wrong, but there isn’t a specific code for it.” • NOS Not otherwise specified “We aren’t sure what’s wrong.” 4 Punctuation [ ] Brackets: in tabular enclose synonyms or alternate wording Example: 008.0 Escherichia coli [E. coli] [ ] Slanted brackets: in index identifies manifestations and indicates sequence. Example: Diabetes, diabetic 250.0x cataract 250.5x [366.41] 5 Punctuation ( ) Parentheses: enclose supplementary words that may be present in the description Example: Cyst (mucus)(retention)(serous)(simple) 6 Additional Terms 599.0 Urinary tract infection, site not specified Excludes candidiasis of urinary tract (112.2) urinary tract infection of newborn (771.82) 280 Iron deficiency anemias anemia Includes asiderotic hypochromic-microcytic sideropenic 7 Use Additional Code 282.42 Sickle-cell thalassemia with crisis Sickle-cell thalassemia with vaso-occlusive pain Thalassemia Hb-S disease with crisis Use additional code for the type of crisis, such as: acute chest sydrome (517.3) splenic sequestration (289.52) 8 Use Additional Code, if Applicable 416.2 Chronic pulmonary embolism Use additional code, if applicable, for associated long-term (current) use of anticoagulants (V58.61) 9 Combination Codes Single codes: 787.02 Nausea alone 787.03 Vomiting alone Combination code: 787.01 Nausea with vomiting 10 Steps to Look Up a Diagnosis Code 1. -

Medical Management Prenotification Certification/Prior Authorization
Guideline Name: Medical Management ¾ Prenotification ¾ Certification/Prior Authorization ¾ Predetermination of Benefits Pre-Notification: Pre-note is a non-penalty request made of enrollees/providers to advise of any upcoming hospital admissions. This provides our clinical staff with possible case management/disease management opportunities based on our criteria. The general categories frequently requiring pre-notification: ¾ In Care System or in the Care System “Family” for In Patient Hospitalization and Rehabilitation. ¾ In Care System or in the Care System “family” for In Patient Mental Health/Chemical Dependency. No letters are sent. Certification/Prior Authorization: A determination as to whether a service, treatment, supply or facility is approved as Medically Necessary by the Claims Administrator, on behalf of the Plan , before payment can be made. The general categories frequently required by the Employer’s Summary Plan Description ( SPD) for certification include the following: ¾ All out of area ( not participating in any Care System) for the following: In Patient Hospitalization and Rehabilitation In Patient Mental Health/Chemical Dependency Skilled Nursing and Extended Care Admissions- NOTE: BHCAG requires pre- authorization for In Care Systems and certification for out of area Home Health Care Transplant Care- Note: this applies to both In/Out of Care Systems Durable Medical Equipment over $750 In/ $1500 out of area Letters are generated and sent to Employee, Provider and Facility per URAC requirements. Pre-Determination: A determination of benefits by the Claims Administrator, on behalf of the Plan, prior to services being provided when individuals want to know if the procedure/service is Medically Necessary and/or Covered under the Plan. -

Robert S. Glade, MD, FAAP Co-Director, VPI Multidisciplinary Clinic of Oklahoma Pediatric ENT of Oklahoma
Robert S. Glade, MD, FAAP Co-Director, VPI Multidisciplinary Clinic of Oklahoma Pediatric ENT of Oklahoma Velopharyngeal dysfunction Velopharyngeal Velopharyngeal Velopharyngeal mislearning incompetance insufficiency (pharyngeal sound (neurolophysiologic (structural or substitution for oral dysfunction causing anatomic deficiency) sound) poor movement) Velopharyngeal Mislearning Speech Therapy Velopharyngeal Incompetence Ideal Patient Pharyngeal Flap-Surgery Incompetent palate, surgical candidate Pharyngeal Bulb Poor surgical candidate, short palate Pharyngeal Lift Poor surgical candidate, long palate Velopharyngeal Insufficiency - Surgery Ideal patient Posterior wall augmentation Small central gap, post adenoidectomy VPI Furlow palatoplasty Submucous , occult submucous cleft palate, and secondary cleft palate repair with small gap (less than 5mm-1cm) Sphincter pharyngoplasty Coronal or bowtie closure pattern with lateral gaps Pharyngeal flap Sagittal or central closure pattern with large, central gap, inadequate palatal length, palatal hypotonia • Muscles of VP closure – Levator veli palatini • Principle elevator (most important for VP closure) – Tensor veli palatini • Opens eustachian tube • ? Tension to velum – Musculus uvulae • Only intrinsic velar muscle • Adds bulk to dorsal uvula – Superior constrictor • Produces inward movement of lateral pharyngeal walls • Passavants ridge – Not universal Passavant’s Ridge Velopharyngeal Dysfunction Robert Glade, MD FAAP After repair – 20-50% develop VPD •Levator orientation •Scar tissue •Palatal