Female Sexual Function and Urinary Incontinence Bekker, M.D
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Vulvodynia: a Common and Underrecognized Pain Disorder in Women and Female Adolescents Integrating Current
21/4/2017 www.medscape.org/viewarticle/877370_print www.medscape.org This article is a CME / CE certified activity. To earn credit for this activity visit: http://www.medscape.org/viewarticle/877370 Vulvodynia: A Common and UnderRecognized Pain Disorder in Women and Female Adolescents Integrating Current Knowledge Into Clinical Practice CME / CE Jacob Bornstein, MD; Andrew Goldstein, MD; Ruby Nguyen, PhD; Colleen Stockdale, MD; Pamela Morrison Wiles, DPT Posted: 4/18/2017 This activity was developed through a comprehensive review of the literature and best practices by vulvodynia experts to provide continuing education for healthcare providers. Introduction Slide 1. http://www.medscape.org/viewarticle/877370_print 1/69 21/4/2017 www.medscape.org/viewarticle/877370_print Slide 2. Historical Perspective Slide 3. http://www.medscape.org/viewarticle/877370_print 2/69 21/4/2017 www.medscape.org/viewarticle/877370_print Slide 4. What we now refer to as "vulvodynia" was first documented in medical texts in 1880, although some believe that the condition may have been described as far back as the 1st century (McElhiney 2006). Vulvodynia was described as "supersensitiveness of the vulva" and "a fruitful source of dyspareunia" before mention of the condition disappeared from medical texts for 5 decades. Slide 5. http://www.medscape.org/viewarticle/877370_print 3/69 21/4/2017 www.medscape.org/viewarticle/877370_print Slide 6. Slide 7. http://www.medscape.org/viewarticle/877370_print 4/69 21/4/2017 www.medscape.org/viewarticle/877370_print Slide 8. Slide 9. Magnitude of the Problem http://www.medscape.org/viewarticle/877370_print 5/69 21/4/2017 www.medscape.org/viewarticle/877370_print Slide 10. -

A Step Towards Stereotactic Navigation During Pelvic Surgery: 3D Nerve Topography
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Erasmus University Digital Repository Surgical Endoscopy and Other Interventional Techniques https://doi.org/10.1007/s00464-018-6086-3 A step towards stereotactic navigation during pelvic surgery: 3D nerve topography A. R. Wijsmuller1,2 · C. Giraudeau3 · J. Leroy4 · G. J. Kleinrensink5 · E. Rociu6 · L. G. Romagnolo7 · A. G. F. Melani7,8,9 · V. Agnus2 · M. Diana3 · L. Soler3 · B. Dallemagne2 · J. Marescaux2 · D. Mutter2 Received: 10 May 2017 / Accepted: 1 February 2018 © The Author(s) 2018. This article is an open access publication Abstract Background Long-term morbidity after multimodal treatment for rectal cancer is suggested to be mainly made up by nerve- injury-related dysfunctions. Stereotactic navigation for rectal surgery was shown to be feasible and will be facilitated by highlighting structures at risk of iatrogenic damage. The aim of this study was to investigate the ability to make a 3D map of the pelvic nerves with magnetic resonance imaging (MRI). Methods A systematic review was performed to identify a main positional reference for each pelvic nerve and plexus. The nerves were manually delineated in 20 volunteers who were scanned with a 3-T MRI. The nerve identifiability rate and the likelihood of nerve identification correctness were determined. Results The analysis included 61 studies on pelvic nerve anatomy. A main positional reference was defined for each nerve. On MRI, the sacral nerves, the lumbosacral plexus, and the obturator nerve could be identified bilaterally in all volunteers. The sympathetic trunk could be identified in 19 of 20 volunteers bilaterally (95%). -

How to Ensure Clitoral Bud Survival in a Sexual Reassignment Surgery for Transsexualism
How We Do It J Cosmet Med 2018;2(1):57-62 https://doi.org/10.25056/JCM.2018.2.1.57 pISSN 2508-8831, eISSN 2586-0585 How to ensure clitoral bud survival in a sexual reassignment surgery for transsexualism Juthapot Pumsup, MD Juthapot Clinics,Trad, Thailand Background: Sexual reassignment surgery (SRS) is the complicated procedure as it has a very high risk of complications. The loss of clitoris is the ones. Accordingly, surgeons should carefully consider the surgical technique and ensure no mistakes during operation. Although most surgeons perform the operation carefully, a considerable incidence of clitoral bud necrosis has been reported. Thus, finding techniques that improve the success rates in surgeries is very important. Objective: We aimed to study the cause of neo-clitoral bud necrosis after SRS in order to devise a mechanism to avoid neo-clitoral bud necrosis, and to find a surgical technique for ensuring the survival of the clitoral bud. Methods: The study was conducted in 20 patients, who underwent a male-to-female SRS via Author technique From Juthapot Clinics, Trad Hospital, and Private Hospital (couldn’t mention) during September 2016 to August 2017. This intervention included various factors as mention below. Results: Of the 20 patients who underwent the procedure with this technique, 18 patients were without clitoral bud necrosis and 2 patients had partial clitoral bud necrosis at the tip. Sensation was preserved in these patients, although it was decreased. The sensation has 2 part: the 1st part is neoclitoris and the 2nd is at the anterior vagina, that made by the urethral lining after spatulation, that can serve the sensation. -

Unit #2 - Abdomen, Pelvis and Perineum
UNIT #2 - ABDOMEN, PELVIS AND PERINEUM 1 UNIT #2 - ABDOMEN, PELVIS AND PERINEUM Reading Gray’s Anatomy for Students (GAFS), Chapters 4-5 Gray’s Dissection Guide for Human Anatomy (GDGHA), Labs 10-17 Unit #2- Abdomen, Pelvis, and Perineum G08- Overview of the Abdomen and Anterior Abdominal Wall (Dr. Albertine) G09A- Peritoneum, GI System Overview and Foregut (Dr. Albertine) G09B- Arteries, Veins, and Lymphatics of the GI System (Dr. Albertine) G10A- Midgut and Hindgut (Dr. Albertine) G10B- Innervation of the GI Tract and Osteology of the Pelvis (Dr. Albertine) G11- Posterior Abdominal Wall (Dr. Albertine) G12- Gluteal Region, Perineum Related to the Ischioanal Fossa (Dr. Albertine) G13- Urogenital Triangle (Dr. Albertine) G14A- Female Reproductive System (Dr. Albertine) G14B- Male Reproductive System (Dr. Albertine) 2 G08: Overview of the Abdomen and Anterior Abdominal Wall (Dr. Albertine) At the end of this lecture, students should be able to master the following: 1) Overview a) Identify the functions of the anterior abdominal wall b) Describe the boundaries of the anterior abdominal wall 2) Surface Anatomy a) Locate and describe the following surface landmarks: xiphoid process, costal margin, 9th costal cartilage, iliac crest, pubic tubercle, umbilicus 3 3) Planes and Divisions a) Identify and describe the following planes of the abdomen: transpyloric, transumbilical, subcostal, transtu- bercular, and midclavicular b) Describe the 9 zones created by the subcostal, transtubercular, and midclavicular planes c) Describe the 4 quadrants created -

Uva-DARE (Digital Academic Repository)
UvA-DARE (Digital Academic Repository) Development of the pelvic floor : implications for clinical anatomy Wallner, C. Publication date 2008 Document Version Final published version Link to publication Citation for published version (APA): Wallner, C. (2008). Development of the pelvic floor : implications for clinical anatomy. General rights It is not permitted to download or to forward/distribute the text or part of it without the consent of the author(s) and/or copyright holder(s), other than for strictly personal, individual use, unless the work is under an open content license (like Creative Commons). Disclaimer/Complaints regulations If you believe that digital publication of certain material infringes any of your rights or (privacy) interests, please let the Library know, stating your reasons. In case of a legitimate complaint, the Library will make the material inaccessible and/or remove it from the website. Please Ask the Library: https://uba.uva.nl/en/contact, or a letter to: Library of the University of Amsterdam, Secretariat, Singel 425, 1012 WP Amsterdam, The Netherlands. You will be contacted as soon as possible. UvA-DARE is a service provided by the library of the University of Amsterdam (https://dare.uva.nl) Download date:27 Sep 2021 APPENDIX LETTERS TO THE EDITOR 183 184 BUTTOCK PAIN AFTER SACROSPINOUS HYSTEROPEXY Published as: Wallner C (2008). Buttock pain after sacrospinous hysteropexy. Int Urogynecol J Pelvic Floor Dysfunct. DOI: 10.1007/s00192-008-0646-3. 185 Dear Editor, With great interest I read the recent publication of Dietz et al [1] in your journal. The authors describe that buttock pain occurred post-operatively in ~18% of patients undergoing sacrospinous hysteropexy for pelvic organ prolapse. -

Award Winning Paper Ð Tanagho Prize Signi®Cant Physiological
International Journal of Impotence Research (2001) 13, 82±88 ß 2001 Nature Publishing Group All rights reserved 0955-9930/01 $15.00 www.nature.com/ijir Award Winning Paper Ð Tanagho Prize Signi®cant physiological roles of ancillary penile nerves on increase in intracavernous pressure in rats: experiments using electrical stimulation of the medial preoptic area YSato1, J Rehman1, C Santizo1, A Melman1, and GJ Christ1;2* 1Department of Urology, Institute for Smooth Muscle Biology, Albert Einstein College of Medicine, New York, USA; and 2Department of Physiology and Biophysics, Institute for Smooth Muscle Biology, Albert Einstein College of Medicine, New York, USA The objectives of this work were to evaluate the contributions of the ancillary penile nerves to penile erection in male rats in vivo. We investigated the effects of unilateral and bilateral transection of the cavernous nerve (main penile nerve) on the increase in intracavernous pressure (ICP) following electrical stimulation of the medial preoptic area (MPOA) in male rats in vivo. After unilateral or bilateral transection of the cavernous nerve (main penile nerve), the ICP responses showed decreases of 28% and 55%, respectively compared to those ICP responses before transection. In other words, even after bilateral transection of the cavernous nerve, signi®cant increases in the ICP response following central stimulation were observed. In contrast to these ®ndings, the ICP response was completely eliminated following bilateral pelvic nerve transection. These data suggested that the ancillary penile nerves, which originate from the major pelvic ganglia, have a complementary role to the cavernous nerves in the autonomic motor innervation of the penis. -

Specific Targeting of Ganglion Cell Sprouts Provides an Additional
The Journal of Neuroscience, October 1, 1998, 18(19):7987–7995 Specific Targeting of Ganglion Cell Sprouts Provides an Additional Mechanism for Restoring Peripheral Motor Circuits in Pelvic Ganglia after Spinal Nerve Damage Mark E. Kepper and Janet R. Keast Department of Physiology and Pharmacology, The University of Queensland, St. Lucia, Queensland, 4072, Australia The pelvic ganglia contain both sympathetic and parasympa- which grow profusely within just a few days. These arise from thetic neurons and provide an interesting model in which to each of the main chemical classes of pelvic neurons but grow study the effects of a distributed spinal nerve lesion. Previous at different rates and have different distributions. Importantly, animal studies have suggested that after either lumbar or sacral some chemical classes of sprouts preferentially supply neurons nerve injury, some functional connections are restored between of dissimilar histochemistry, suggesting the presence of very preganglionic and postganglionic neurons. It has been pro- specific targeting mechanisms rather than random growth. posed that this is because of intact preganglionic axons sprout- These sprouts are transient, however, those formed after partial ing collaterals to supply denervated ganglion cells. However, decentralization appear to be maintained. Moreover, after le- this has never been demonstrated, and our study has investi- sion of either lumbar or sacral spinal nerves, many sprouts arise gated whether the ganglion cells themselves contribute to axo- from neurons with intact spinal connections and innervate neu- genesis and restoration of peripheral circuitry. We have moni- rons that have lost their preganglionic inputs. This provides a tored the growth of axons from pelvic ganglion cells after very different alternative mechanism to reestablish communi- lumbar or sacral nerve injury (partial decentralization), or a cation between preganglionic and postganglionic neurons. -

Pelvic Floor Physical Therapy for Vulvodynia a Clinician’S Guide
Pelvic Floor Physical Therapy for Vulvodynia A Clinician’s Guide Stephanie A. Prendergast, MPT KEYWORDS Vulvodynia Vestibulodynia Dyspareunia Pelvic floor dysfunction Pelvic floor physical therapy KEY POINTS Most women with complaints of vulvar pain have pelvic floor dysfunction. Pelvic floor screenings can be easily incorporated into a gynecology examination to iden- tify pelvic floor dysfunction. Successful treatment plans for vulvodynia are multimodal and include pelvic floor physical therapy. INTRODUCTION OF NEW NOMENCLATURE In 2003, the International Society for the Study of Vulvovaginal Disease (ISSVD) defined vulvodynia as ‘vulvar discomfort, most often described as burning pain, occurring in the absence of relevant visible findings or a specific, clinically identifiable, neurologic disorder’. This terminology served to acknowledge vulvar pain as a real disorder but fell short of classifying the syndrome as anything more than idiopathic pain. At that time, little was known about the pathophysiologic mechanisms that cause vulvodynia and treatment options were limited. Over the past decade, researchers have identified several causes of vulvodynia as well as associated factors/impair- ments. This identification resulted in the need to develop a new classification system to guide physicians toward better diagnosis and treatment. Last year the ISSVD, the International Society for the Study of Women’s Sexual Health, and the International Pelvic Pain Society came together to review the evidence and publish the 2015 Consensus Terminology -

Plasticity of Neurons in Mouse Major Pelvic Ganglia in Response to Loss of Physiological
Plasticity of neurons in mouse major pelvic ganglia in response to loss of physiological input in cases of nerve injury and spinal cord injury A Dissertation Presented to The Faculty of the Graduate School At the University of Missouri In Partial Fulfillment Of the Requirements for the Degree Doctor of Philosophy By Cindy Kyi Dr. David Schulz, Dissertation Advisor May 2018 i The undersigned, appointed by the dean of the Graduate School, have examined the dissertation entitled PLASTICITY OF NEURONS IN MOUSE MAJOR PELVIC GANGLIA IN RESPONSE TO LOSS OF PHYSIOLOGICAL INPUT IN CASES OF NERVE INJURY AND SPINAL CORD INJURY Presented by Kyi, Cindy (MU-Student) A candidate for the degree of Doctor of Philosophy And hereby certify that, in their opinion, it is worthy of acceptance. Dr. David J. Schulz Dr. Michael L. Garcia Dr. Andrew D. McClellan Dr. Kevin J. Cummings Dedicated to Mom and Dad iii ACKNOWLEDGEMENTS First of all, I would like to thank God for guiding me and being with me and my family since the day I left Myanmar (Burma). He has been my rock and shelter through all the challenges along the way. I am very grateful to my advisor Dr. David Schulz for granting me with the opportunity to work in his laboratory and believing in me to take on a new project. Thank you very much for all your guidance, patience, training, and for giving me room to grow under your mentorship. I would also like to thank my committee members Dr. Andrew McClellan, Dr. Michael Garcia, and Dr. Kevin Cummings for all of their support in providing me with feedback not only on the details of experimental protocols but also helping me relate my experimental findings to a big picture context. -
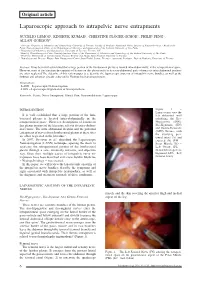
Laparoscopic Approach to Intrapelvic Nerve Entrapments
4-Lemos - Laparoscopic.qxp_treatment 05/03/18 12:11 Pagina 6 Original article Laparoscopic approach to intrapelvic nerve entrapments NUCELIO LEMOS 1, KINSHUK KUMAR 2, CHRISTINE PLÖGER-SCHOR 3, PHILIP PENG 4, ALLAN GORDON 5 1 Associate Professor of Obstetrics and Gynaecology University of Toronto, Faculty of Medicine Functional Pelvic Surgery & Neuropelveology - Head of the Pelvic Neurodysfunction Clinic of the Department of Obstetrics and Gynecology of the Federal University of São Paulo 2 Department of Obstetrics and Gynaecology, University of Toronto, Toronto, ON 3 Head of Physiotherapy in Pelvic Neurodysfunction Clinic of the Department of Obstetrics and Gynecology of the Federal University of São Paulo 4 Professor, Department of Anesthesiology Toronto Western and Mount Sinai Hospital University of Toronto 5 Neurologist and Director Wasser Pain Management Centre Sinai Health System, Toronto - Asscociate Professor, Dept of Medicine, University of Toronto Abstract: It has been well-established that a large portion of the lumbosacral plexus is located intra-abdominally, in the retroperitoneal space. However, most of the literature descriptions of lesions on this plexus refer to its extra-abdominal parts whereas its intra-abdominal portions are often neglected.The objective of this review paper is to describe the laparoscopic anatomy of intrapelvic nerve bundles, as well as the findings and advances already achieved by Neuropelveology practitioners. Abreviations: - LANN – Laparoscopic Neuronavigation - LION – Laparoscopic Implantation of Neuroprosthesis Keywords: Sciatic; Nerve Entrapment; Gluteal Pain; Neuromodulation; Laparoscopy. INTRODUCTION Figure 1. – Laparoscopic view the It is well established that a large portion of the lum - left abdominal wall bosacral plexus is located intra-abdominally in the exhibiting the Ilio- retroperitoneal space 1. -

The Innervation of the Pelvic Floor Muscles: a Reappraisal for the Levator Ani Nerve
UvA-DARE (Digital Academic Repository) Development of the pelvic floor : implications for clinical anatomy Wallner, C. Publication date 2008 Document Version Final published version Link to publication Citation for published version (APA): Wallner, C. (2008). Development of the pelvic floor : implications for clinical anatomy. General rights It is not permitted to download or to forward/distribute the text or part of it without the consent of the author(s) and/or copyright holder(s), other than for strictly personal, individual use, unless the work is under an open content license (like Creative Commons). Disclaimer/Complaints regulations If you believe that digital publication of certain material infringes any of your rights or (privacy) interests, please let the Library know, stating your reasons. In case of a legitimate complaint, the Library will make the material inaccessible and/or remove it from the website. Please Ask the Library: https://uba.uva.nl/en/contact, or a letter to: Library of the University of Amsterdam, Secretariat, Singel 425, 1012 WP Amsterdam, The Netherlands. You will be contacted as soon as possible. UvA-DARE is a service provided by the library of the University of Amsterdam (https://dare.uva.nl) Download date:01 Oct 2021 CHAPTER 3 THE INNERVATION OF THE PELVIC FLOOR MUSCLES: A REAPPRAISAL FOR THE LEVATOR ANI NERVE Published as: Wallner C, Maas CP, Dabhoiwala NF, Lamers WH, DeRuiter MC (2006). The Innervation of the Pelvic Floor Muscles: A Reappraisal for the Levator Ani Nerve. Obstet Gynecol, 108(3): 529-534. 75 CHAPTER 3 - INNERVATION OF THE PELVIC FLOOR MUSCLES: THE LEVATOR ANI NERVE Abstract Objective: A recent study, published in this journal suggested that a transvaginal pudendal nerve blockade selectively affects the pudendal nerve without blocking the direct sacral branches to the levator ani muscle (the levator ani nerve, LAN). -

An Introduction to Pelvic Floor Physical Therapy
Anatomy of the Pelvis Presented by Julie Peterson, PT, DPT, WCS, BCB- PMD Acknowledgements: Ruth M. Maher, PT, PhD, DPT, WCS, BCB-PMD October 2019 • Material presented in this webinar cannot be reproduced without consent of original authors. 2 Objectives • Understand pelvic anatomy – male/female – Osteology – Ligamentous – Viscera – Blood supply/lymphatics – Musculature/fascia – Innervation – lumbo sacral plexus, branches and structures innervated 3 The Politics of the Pelvis 4 Who’s looking after this system? Osteology 6 Pelvic (Hip) Girdle • Each coxal (hip) bone consists of three bones that fuse together: ilium, pubis, and ischium. • The two coxal bones are joined anteriorly by the pubic symphysis (fibrocartilage). • Joined posteriorly by the sacrum forming the sacroiliac joint (SIJ). • The os coxa (hip bone) initially begins life as three individual bones: – Ilium – Ischium – Pubis The Ilium • Largest of the three hip bones • Ilium is the superior part of the hip bone • Consists of a superior ala and inferior body which forms the acetabulum (the socket for the head of the femur) • Superior border - iliac crest • Greater sciatic notch - allows passage of sciatic nerve Ischium and Pubis • Ischium - inferior and posterior part of the hip bone • Most prominent feature is the ischial tuberosity, it is the part that meets the chair when you are sitting • Pubis - inferior and anterior part of the hip bone • Superior and inferior rami and body Anterior Pelvis Posterior Pelvis Superior View False and True Pelves • Pelvic brim/inlet - a line