EANM Procedure Guidelines for 131I-Meta-Iodobenzylguanidine (131I-Mibg) Therapy
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Landscape Analysis of Phase 2/3 Clinical Trials of Targeted
Journal of Nuclear Medicine, published on February 12, 2021 as doi:10.2967/jnumed.120.258103 Landscape analysis of Phase 2/3 clinical trials for Targeted Radionuclide Therapy Erik Mittra1, Amanda Abbott2, and Lisa Bodei3 Affiliations 1. Division of Nuclear Medicine & Molecular Imaging, Oregon Health & Science University, Portland, OR 2. Clinical Trials Network, Society of Nuclear Medicine & Molecular Imaging, Reston, VA 3. Molecular Imaging and Therapy Service, Memorial Sloan Kettering Cancer Center, New York, NY Word count without figure: 880 Word count with figure: 971 Key Words: radioisotope therapy, radiopharmaceutical therapy and radioligand therapy Text Within Nuclear Medicine, theranostics has revitalized the field of Targeted Radionuclide Therapy (TRT) and there is a growing number of investigator-initiated and industry-sponsored clinical trials of TRT. This article summarizes the current trials available in the NIH database, the largest trial repository, to provide both an overview of the current landscape and a glimpse towards an undeniably exciting future of theranostics. This landscape analysis was completed by searching the terms “radionuclide therapy”, “radioisotope therapy”, “radiopharmaceutical therapy” and “radioligand therapy” on ClinicalTrials.gov in November 2020. Other terms may provide different results. Phase 1/2, 2, and 3 trials that are currently recruiting and those not yet recruiting were included. Studies. Overall, the results showed 42 clinical trials including 13 Phase 1/2, 26 Phase 2, and three Phase 3. Given this range of phases, the planned enrollment varies widely from 10-813, with an average of 147 participants. Five different radioisotopes, 12 ligands or targets, and 11 different cancer types are represented (Figure 1). -

RADIO PHARMACEUTICALS Production Control Safety Precautions Applications Storage
RADIO PHARMACEUTICALS Production control Safety precautions Applications Storage. Presented by: K. ARSHAD AHMED KHAN M.Pharm, (Ph.D) Department of Pharmaceutics, Raghavendra Institute of Pharmaceutical Education and Research [RIPER] Anantapur. 1 DEFINITION: Radiopharmaceuticals are the radioactive substances or radioactive drugs for diagnostic or therapeutic interventions. or Radiopharmaceuticals are medicinal formulations containing radioisotopes which are safe for administration in humans for diagnosis or for therapy. 2 COMPOSITION: • A radioactive isotope that can be injected safely into the body, and • A carrier molecule which delivers the isotope to the area to be treated or examined. 3 USAGE/WORKING: 4 BASICS Nuclide: This is a particular nuclear species characterized by its atomic number (No. of protons) and mass 12 23 number (No. of protons + neutrons). 6C , 11Na Isotopes: These are nuclides with same atomic number and different mass number. 1 2 3 Hydrogen has 3 isotopes --- 1H , 1H , 1H . 10 11 12 13 14 Carbon has 5 isotopes ------6C , 6C , 6C , 6C , 6C . 5 • ISOTOPES MAY BE STABLE OR UNSTABLE. • The nucleus is unstable if the number of neutrons is less or greater than the number of protons. • If they are unstable, they under go radioactive decay or disintegration and are known as radioactive isotopes/ radioactive nuclides. Radioactivity: The property of unstable nuclides of emitting radiation by spontaneous transformation of nuclei into other nuclides is called radioactivity. •Radioactive isotopes emit radiations or rays like α, β, γ rays. 6 PRODUCTION CONTROL 7 8 9 10 11 12 13 14 15 Radiopharmaceuticals production occurs in machines like 1. Cyclotron (low energy, high energy) 2. -

Targeted Radiotherapeutics from 'Bench-To-Bedside'
RadiochemistRy in switzeRland CHIMIA 2020, 74, No. 12 939 doi:10.2533/chimia.2020.939 Chimia 74 (2020) 939–945 © C. Müller, M. Béhé, S. Geistlich, N. P. van der Meulen, R. Schibli Targeted Radiotherapeutics from ‘Bench-to-Bedside’ Cristina Müllera, Martin Béhéa, Susanne Geistlicha, Nicholas P. van der Meulenab, and Roger Schibli*ac Abstract: The concept of targeted radionuclide therapy (TRT) is the accurate and efficient delivery of radiation to disseminated cancer lesions while minimizing damage to healthy tissue and organs. Critical aspects for success- ful development of novel radiopharmaceuticals for TRT are: i) the identification and characterization of suitable targets expressed on cancer cells; ii) the selection of chemical or biological molecules which exhibit high affin- ity and selectivity for the cancer cell-associated target; iii) the selection of a radionuclide with decay properties that suit the properties of the targeting molecule and the clinical purpose. The Center for Radiopharmaceutical Sciences (CRS) at the Paul Scherrer Institute in Switzerland is privileged to be situated close to unique infrastruc- ture for radionuclide production (high energy accelerators and a neutron source) and access to C/B-type labora- tories including preclinical, nuclear imaging equipment and Swissmedic-certified laboratories for the preparation of drug samples for human use. These favorable circumstances allow production of non-standard radionuclides, exploring their biochemical and pharmacological features and effects for tumor therapy and diagnosis, while investigating and characterizing new targeting structures and optimizing these aspects for translational research on radiopharmaceuticals. In close collaboration with various clinical partners in Switzerland, the most promising candidates are translated to clinics for ‘first-in-human’ studies. -

Bispecific Antibody Pretargeting of Radionuclides for Immuno^ Single
Bispecific Antibody Pretargeting of Radionuclides for Immuno ^ Single-Photon Emission Computed Tomography and Immuno ^ Positron Emission Tomography Molecular Imaging:An Update Robert M. Sharkey,1Habibe Karacay,1William J. McBride,2 Edmund A. Rossi,3 Chien-Hsing Chang,3 and David M. Goldenberg1 Abstract Molecular imaging is intended to localize disease based on distinct molecular/functional characteristics. Much of today’s interest in molecular imaging is attributed to the increased acceptance and role of 18F-flurodeoxyglucose (18F-FDG) imaging in a variety of tumors. The clinical acceptance of 18F-FDG has stimulated research for other positron emission tomography (PET) agents with improved specificity to aid in tumor detection and assessment. In this regard, a number of highly specific antibodies have been described for different cancers. Although scintigraphic imaging with antibodies in the past was helpful in patient management, most antibody-based imaging products have not been able to compete successfully with the sensitivity afforded by 18F-FDG-PET, especially when used in combination with computed tomography. Recently, however, significant advances have been made in reengineering antibodies to improve their targeting properties. Herein, we describe progress being made in using a bispecific antibody pretargeting method for immuno ^ single-photon emission computed tomography and immunoPETapplications, as contrasted to directly radiolabeled antibodies.This approach not only significantly enhances tumor/nontumor ratios but also provides high signal intensity in the tumor, making it possible to visualize micrometastases of colonic cancer as small as 0.1to 0.2 mm in diameter using an anti ^ carcinoembryonic antigen bispecific antibody, whereas FDG failed to localize these lesions in a nude mouse model. -
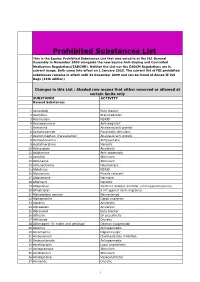
Prohibited Substances List
Prohibited Substances List This is the Equine Prohibited Substances List that was voted in at the FEI General Assembly in November 2009 alongside the new Equine Anti-Doping and Controlled Medication Regulations(EADCMR). Neither the List nor the EADCM Regulations are in current usage. Both come into effect on 1 January 2010. The current list of FEI prohibited substances remains in effect until 31 December 2009 and can be found at Annex II Vet Regs (11th edition) Changes in this List : Shaded row means that either removed or allowed at certain limits only SUBSTANCE ACTIVITY Banned Substances 1 Acebutolol Beta blocker 2 Acefylline Bronchodilator 3 Acemetacin NSAID 4 Acenocoumarol Anticoagulant 5 Acetanilid Analgesic/anti-pyretic 6 Acetohexamide Pancreatic stimulant 7 Acetominophen (Paracetamol) Analgesic/anti-pyretic 8 Acetophenazine Antipsychotic 9 Acetylmorphine Narcotic 10 Adinazolam Anxiolytic 11 Adiphenine Anti-spasmodic 12 Adrafinil Stimulant 13 Adrenaline Stimulant 14 Adrenochrome Haemostatic 15 Alclofenac NSAID 16 Alcuronium Muscle relaxant 17 Aldosterone Hormone 18 Alfentanil Narcotic 19 Allopurinol Xanthine oxidase inhibitor (anti-hyperuricaemia) 20 Almotriptan 5 HT agonist (anti-migraine) 21 Alphadolone acetate Neurosteriod 22 Alphaprodine Opiod analgesic 23 Alpidem Anxiolytic 24 Alprazolam Anxiolytic 25 Alprenolol Beta blocker 26 Althesin IV anaesthetic 27 Althiazide Diuretic 28 Altrenogest (in males and gelidngs) Oestrus suppression 29 Alverine Antispasmodic 30 Amantadine Dopaminergic 31 Ambenonium Cholinesterase inhibition 32 Ambucetamide Antispasmodic 33 Amethocaine Local anaesthetic 34 Amfepramone Stimulant 35 Amfetaminil Stimulant 36 Amidephrine Vasoconstrictor 37 Amiloride Diuretic 1 Prohibited Substances List This is the Equine Prohibited Substances List that was voted in at the FEI General Assembly in November 2009 alongside the new Equine Anti-Doping and Controlled Medication Regulations(EADCMR). -

The Evolving Landscape of Therapeutic and Diagnostic Radiopharmaceuticals
ARTICLE THE EVOLVING LANDSCAPE OF THERAPEUTIC AND DIAGNOSTIC RADIOPHARMACEUTICALS Therapeutic and diagnostic approaches involving the use of radiation and radioactive compounds have a long- standing history in the fields of science and medicine. Radiotherapy was first used in cancer treatments in 1896.1 Since then, the field of radiation has advanced to further understand how radioactive compounds interact with biological tissues and how they can be used in both diagnostic and therapeutic applications. Radiopharmaceuticals are compounds used for medicinal purposes that contain radioactive isotopes (also known as radionuclides) and can be diagnostic or therapeutic in nature, or both.2 They represent a unique category of pharmaceuticals due to their radioactive properties. As such, there are specific guidelines and regulations that impact and direct the study and use of these compounds. Radiopharmaceutical drug development has rapidly expanded over the last decade. Radiopharmaceuticals are widely used in the field of imaging for diagnosis, staging, and follow up; in the realm of therapeutics, their use has increased, most notably, in the area of oncology. In a recent webinar, experts from Medpace’s radiation oncology, imaging, regulatory, and operational teams discussed the growing space of radiopharmaceutical development with respect to their biological use and application, regulatory frameworks that govern their evaluation in support of approvals, operational manufacturing considerations, and associated imaging approaches. BIOLOGICAL MECHANISMS OF ACTION OF RADIONUCLIDES According to Dr. Jess Guarnaschelli, Medical Director, Radiation Oncology, the radioactivity of radionuclides can be employed for both diagnostic and therapeutic medical uses. While external beam ionizing radiation involves radiation emitted in the form of electromagnetic waves or particles, radiopharmaceuticals use radionuclides to deliver localized radiation to specific targets. -

Radiotoxicity After Iodine-131 Therapy for Thyroid Cancer Using the Micronucleus Assay
Radiotoxicity After Iodine-131 Therapy for Thyroid Cancer Using the Micronucleus Assay Naoto Watanabe, Kunihiko Yokoyama, Seigo Kinuya, Noriyuki Shuke, Masashi Shimizu, Ryusuke Futatsuya, Takatoshi Michigishi, Norihisa Tonami, Hikaru Seto and David A. Goodwin Departments of Radiology and Radiological Science, Toyama Medical and Pharmaceutical University, Toyama; Department of Nuclear Medicine, Kanazawa University, Kanazawa; Department of Radiology, Asahikawa Medical University, Asahikawa, Japan; Nuclear Medicine Service, Veterans Affairs Health Sciences, Palo Alto, California; and Department of Radiology, Stanford University School of Medicine, Stanford, California thrombocytopenia have been reported (6,7). Therefore, in most The purpose of the present study was to evaluate the degree of patients who are treated with a large amount of I3il, the limiting cytological radiation damage to lymphocytes after1311therapy using the cytokinesis-blocked micronucleus assay. The chromosomal factor is the radiation dose to the blood and the bone marrow damage to lymphocytes induced by 131I ¡nvivo should result in (8). Dosimetrie studies have estimated the radiation dose to the augmentation of the cells with micronuclei. Methods: We studied 25 blood and bone marrow with a large amount of radioiodine (3 ). patients with differentiated thyroid carcinoma who were treated with Previous work has been done on cytogenetic changes (9). 3.7 GBq of 131I.Isolated lymphocytes collected from patients 1 wk However, the cytological effects of radiation exposure on the after therapy were harvested and treated according to the cytoki lymphocytes in vivo with large therapeutic doses of radioiodine nesis-blocked method of Fenech and Morley. The micronucleus have not been extensively examined. number of micronuclei per 500 binucleated cells were scored by The purpose of our study was to evaluate the degree of visual inspection. -

(Mibg) Scintigraphy: Procedure Guidelines for Tumour Imaging
Eur J Nucl Med Mol Imaging (2010) 37:2436–2446 DOI 10.1007/s00259-010-1545-7 GUIDELINES 131I/123I-Metaiodobenzylguanidine (mIBG) scintigraphy: procedure guidelines for tumour imaging Emilio Bombardieri & Francesco Giammarile & Cumali Aktolun & Richard P. Baum & Angelika Bischof Delaloye & Lorenzo Maffioli & Roy Moncayo & Luc Mortelmans & Giovanna Pepe & Sven N. Reske & Maria R. Castellani & Arturo Chiti Published online: 20 July 2010 # EANM 2010 Abstract The aim of this document is to provide general existing procedures for neuroendocrine tumours. The information about mIBG scintigraphy in cancer patients. guidelines should therefore not be taken as exclusive of The guidelines describe the mIBG scintigraphy protocol other nuclear medicine modalities that can be used to obtain currently used in clinical routine, but do not include all comparable results. It is important to remember that the The European Association has written and approved guidelines to promote the use of nuclear medicine procedures with high quality. These general recommendations cannot be applied to all patients in all practice settings. The guidelines should not be deemed inclusive of all proper procedures and exclusive of other procedures reasonably directed to obtaining the same results. The spectrum of patients seen in a specialized practice setting may be different than the spectrum usually seen in a more general setting. The appropriateness of a procedure will depend in part on the prevalence of disease in the patient population. In addition, resources available for patient care may vary greatly from one European country or one medical facility to another. For these reasons, guidelines cannot be rigidly applied. These guidelines summarize the views of the Oncology Committee of the EANM and reflect recommendations for which the EANM cannot be held responsible. -

The Use of Stems in the Selection of International Nonproprietary Names (INN) for Pharmaceutical Substances
WHO/PSM/QSM/2006.3 The use of stems in the selection of International Nonproprietary Names (INN) for pharmaceutical substances 2006 Programme on International Nonproprietary Names (INN) Quality Assurance and Safety: Medicines Medicines Policy and Standards The use of stems in the selection of International Nonproprietary Names (INN) for pharmaceutical substances FORMER DOCUMENT NUMBER: WHO/PHARM S/NOM 15 © World Health Organization 2006 All rights reserved. Publications of the World Health Organization can be obtained from WHO Press, World Health Organization, 20 Avenue Appia, 1211 Geneva 27, Switzerland (tel.: +41 22 791 3264; fax: +41 22 791 4857; e-mail: [email protected]). Requests for permission to reproduce or translate WHO publications – whether for sale or for noncommercial distribution – should be addressed to WHO Press, at the above address (fax: +41 22 791 4806; e-mail: [email protected]). The designations employed and the presentation of the material in this publication do not imply the expression of any opinion whatsoever on the part of the World Health Organization concerning the legal status of any country, territory, city or area or of its authorities, or concerning the delimitation of its frontiers or boundaries. Dotted lines on maps represent approximate border lines for which there may not yet be full agreement. The mention of specific companies or of certain manufacturers’ products does not imply that they are endorsed or recommended by the World Health Organization in preference to others of a similar nature that are not mentioned. Errors and omissions excepted, the names of proprietary products are distinguished by initial capital letters. -

Molecular Imaging and Radionuclide Therapy of Pheochromocytoma and Paraganglioma in the Era of Genomic Characterization of Disease Subgroups
26 11 Theranostics of D Taïeb et al. 26:11 R627–R656 Endocrine-Related pheochromocytoma and Cancer paraganglioma REVIEW Molecular imaging and radionuclide therapy of pheochromocytoma and paraganglioma in the era of genomic characterization of disease subgroups David Taïeb1,*, Abhishek Jha2,*, Giorgio Treglia3,4,5 and Karel Pacak2 1Department of Nuclear Medicine, La Timone University Hospital, CERIMED, Aix-Marseille University, Marseille, France 2Section on Medical Neuroendocrinology, Eunice Kennedy Shriver National Institute of Child Health and Human Development, National Institutes of Health, Bethesda, Maryland, USA 3Clinic of Nuclear Medicine and PET/CT Center, Ente Ospedaliero Cantonale, Bellinzona, Switzerland 4Department of Nuclear Medicine and Molecular Imaging, Lausanne University Hospital, Lausanne, Switzerland 5Health Technology Assessment Unit, General Directorate, Ente Ospedaliero Cantonale, Bellinzona, Switzerland Correspondence should be addressed to K Pacak: [email protected] *(D Taïeb and A Jha contributed equally to this work) Abstract In recent years, advancement in genetics has profoundly helped to gain a more Key Words comprehensive molecular, pathogenic, and prognostic picture of pheochromocytomas f pheochromocytoma and paragangliomas (PPGLs). Newly discovered molecular targets, particularly those f paraganglioma that target cell membranes or signaling pathways have helped move nuclear medicine f PPGL in the forefront of PPGL precision medicine. This is mainly based on the introduction f succinate dehydrogenase and increasing experience of various PET radiopharmaceuticals across PPGL genotypes complex quickly followed by implementation of novel radiotherapies and revised imaging f SDHB algorithms. Particularly, 68Ga-labeled-SSAs have shown excellent results in the diagnosis f 18F-FDOPA and staging of PPGLs and in selecting patients for PRRT as a potential alternative to f 68Ga-DOTATATE 123/131I-MIBG theranostics. -

Getting Oral Or Systemic Radiation Therapy
cancer.org | 1.800.227.2345 Getting Oral or Systemic Radiation Therapy What is systemic radiation therapy? Systemic therapy involves treatment that travels through your entire body rather than being aimed at one area. Systemic radiation therapy uses radioactive drugs (called radiopharmaceuticals or radionuclides) to treat certain types of cancer, including thyroid, bone, and prostate cancer. These are liquid drugs made up of a radioactive substance. They can be given by mouth or put into a vein; they then travel throughout the body. Although these drugs travel through your whole body, they can find and collect in places where the cancer cells are located. This helps them deliver radiation doses exactly to the tumor or area where the cancer cells are found. In some cases, a radioactive drug might be used to help find cancer, such as bone metastasis (when cancer has spread to the bone). There are also radioactive drugs that are used to help diagnose other non-cancer health problems. Radioimmunotherapy One type of radiopharmaceutical is called radioimmunotherapy. This treatment combines a small amount of radioactive material with a special drug called a monoclonal antibody1. The radioactive material acts as a tracer that can find and attach to cancer cells, then the monoclonal antibody is delivered directly to the cells. Peptide receptor radionuclide therapy (PRRT) Another type of radiopharmaceutical is called peptide receptor radionuclide therapy (PRRT). This treatment combines radioactive material with a special protein called a peptide to make a radiopeptide. When given, the radiopeptide finds and attaches to 1 ____________________________________________________________________________________American Cancer Society cancer.org | 1.800.227.2345 certain types of cancer cells, then delivers a high dose of radiation directly to the cells. -

Dosimetry and Dosimetric Tools in Radionuclide Therapy, Including Results from a European Survey
Dosimetry and dosimetric tools in radionuclide therapy, including results from a European survey KATARINA SJÖGREEN GLEISNER MEDICAL RADIATION PHYSICS, LUND UNIVERSITY, SWEDEN Radionuclide therapies • Thyroid – 131I NaI for benign conditions – 131I NaI for thyroid cancer Oral • Adult neuroendocrine disease – 131I mIBG, 177Lu or 90Y radiopeptides intravenous • Neuroblastoma - 131I mIBG • Non-Hodgkins lymphoma – 177Lu or 90Y labelled mAbs • Bone metastases - 153Sm, 89Sr, 223Ra • Prostate cancer - 177Lu-PSMA (trial) • Myeloproliferative disease - 32P • Intra-arterial treatment in liver : – 90Y microspheres, 166Ho Local administration • Joints - Radiation synovectomy 90Y, 186Re, 169Er • 169Er, 67Cu, 188Re,227Th, 225Ac, 211At …. Systemically administered • Thyroid – 131I NaI for benign conditions – 131I NaI for thyroid cancer • Adult neuroendocrine disease – 131I mIBG, 177Lu or 90Y radiopeptides • Neuroblastoma - 131I mIBG • Non-Hodgkins lymphoma – 177Lu or 90Y labelled mAbs • Bone metastases - 153Sm, 89Sr, 223Ra • Prostate cancer - 177Lu-PSMA (trial) • Myeloproliferative disease - 32P • Intra-arterial treatment in liver : – 90Y microspheres, 166Ho • Joints - Radiation synovectomy 90Y, 186Re, 169Er • 169Er, 67Cu, 188Re,227Th, 225Ac, 211At …. Systemically administered Systemically administered Autoradiography: intratumoral distribution of monoclonal antibody in rat Örbom et al J Nucl Med 2013 AD Definition of absorbed dose (ICRU 85 and 86) • The absorbed dose is the mean energy imparted, , to the matter in an infinitesimal volume, , with mass unit gray (Gy) ; 1 Gy = 1 J/kg. • The mean absorbed dose in a target region with mass ) ℳ ICRU Report 85: Fundamental quantities and units for ionizing radiation, Journal of the ICRU 11 1 (2011). ICRU Report 86: Quantification and reporting of low-dose and other heterogeneous exposures, Journal of the ICRU 11 2 (2011). Internal dosimetry - The absorbed fraction Source * Target is the absorbed fraction, i.e.