Liver/Gallbladder Cleanse DAY CLEANSE
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Mouth Esophagus Stomach Rectum and Anus Large Intestine Small
1 Liver The liver produces bile, which aids in digestion of fats through a dissolving process known as emulsification. In this process, bile secreted into the small intestine 4 combines with large drops of liquid fat to form Healthy tiny molecular-sized spheres. Within these spheres (micelles), pancreatic enzymes can break down fat (triglycerides) into free fatty acids. Pancreas Digestion The pancreas not only regulates blood glucose 2 levels through production of insulin, but it also manufactures enzymes necessary to break complex The digestive system consists of a long tube (alimen- 5 carbohydrates down into simple sugars (sucrases), tary canal) that varies in shape and purpose as it winds proteins into individual amino acids (proteases), and its way through the body from the mouth to the anus fats into free fatty acids (lipase). These enzymes are (see diagram). The size and shape of the digestive tract secreted into the small intestine. varies in each individual (e.g., age, size, gender, and disease state). The upper part of the GI tract includes the mouth, throat (pharynx), esophagus, and stomach. The lower Gallbladder part includes the small intestine, large intestine, The gallbladder stores bile produced in the liver appendix, and rectum. While not part of the alimentary 6 and releases it into the duodenum in varying canal, the liver, pancreas, and gallbladder are all organs concentrations. that are vital to healthy digestion. 3 Small Intestine Mouth Within the small intestine, millions of tiny finger-like When food enters the mouth, chewing breaks it 4 protrusions called villi, which are covered in hair-like down and mixes it with saliva, thus beginning the first 5 protrusions called microvilli, aid in absorption of of many steps in the digestive process. -

Acute Liver Failure J G O’Grady
148 Postgrad Med J: first published as 10.1136/pgmj.2004.026005 on 4 March 2005. Downloaded from REVIEW Acute liver failure J G O’Grady ............................................................................................................................... Postgrad Med J 2005;81:148–154. doi: 10.1136/pgmj.2004.026005 Acute liver failure is a complex multisystemic illness that account for most cases, but a significant number of patients have no definable cause and are evolves quickly after a catastrophic insult to the liver classified as seronegative or of being of indeter- leading to the development of encephalopathy. The minate aetiology. Paracetamol is the commonest underlying aetiology and the pace of progression strongly cause in the UK and USA.2 Idiosyncratic reac- tions comprise another important group. influence the clinical course. The commonest causes are paracetamol, idiosyncratic drug reactions, hepatitis B, and Viral seronegative hepatitis. The optimal care is multidisciplinary ALF is an uncommon complication of viral and up to half of the cases receive liver transplants, with hepatitis, occurring in 0.2%–4% of cases depend- ing on the underlying aetiology.3 The risk is survival rates around 75%–90%. Artificial liver support lowest with hepatitis A, but it increases with the devices remain unproven in efficacy in acute liver failure. age at time of exposure. Hepatitis B can be associated with ALF through a number of ........................................................................... scenarios (table 2). The commonest are de novo infection and spontaneous surges in viral repli- cation, while the incidence of the delta virus cute liver failure (ALF) is a complex infection seems to be decreasing rapidly. multisystemic illness that evolves after a Vaccination should reduce the incidence of Acatastrophic insult to the liver manifesting hepatitis A and B, while antiviral drugs should in the development of a coagulopathy and ameliorate replication of hepatitis B. -

Differential Metabolism of Alprazolam by Liver and Brain Cytochrome (P4503A) to Pharmacologically Active Metabolite
The Pharmacogenomics Journal (2002) 2, 243–258 2002 Nature Publishing Group All rights reserved 1470-269X/02 $25.00 www.nature.com/tpj ORIGINAL ARTICLE Differential metabolism of alprazolam by liver and brain cytochrome (P4503A) to pharmacologically active metabolite HV Pai1,2* ABSTRACT SC Upadhya1,2* Cytochrome P450 (P450) is a superfamily of enzymes which mediates metab- 1 olism of xenobiotics including drugs. Alprazolam, an anti-anxiety agent, is SJ Chinta * metabolized in rat and human liver by P4503A1 and P4503A4 respectively, SN Hegde1 to 4-hydroxy alprazolam (4-OHALP, pharmacologically less active) and ␣- V Ravindranath1,2 hydroxy alprazolam (␣-OHALP, pharmacologically more active). We exam- ined P450 mediated metabolism of alprazolam by rat and human brain 1Department of Neurochemistry, National microsomes and observed that the relative amount of ␣-OHALP formed in Institute of Mental Health & Neurosciences, brain was higher than liver. This biotransformation was mediated by a P450 Bangalore, India; 2National Brain Research Centre, ICGEB Campus, Aruna Asaf Ali Marg, isoform belonging to P4503A subfamily, which is constitutively expressed in New Delhi , India neuronal cells in rat and human brain. The formation of larger amounts of ␣-OHALP in neurons points to local modulation of pharmacological activity Correspondence: in brain, at the site of action of the anti-anxiety drug. Since hydroxy metab- V Ravindranath, National Brain Research olites of alprazolam are hydrophilic and not easily cleared through blood- Centre, ICGEB Campus, Aruna Asaf Ali ␣ Marg, New Delhi - 110 067, India CSF barrier, -OHALP would potentially have a longer half-life in brain. Tel: +91 124 630 8317 The Pharmacogenomics Journal (2002) 2, 243–258. -

Fact Sheet - Symptoms of Pancreatic Cancer
Fact Sheet - Symptoms of Pancreatic Cancer Diagnosis Pancreatic cancer is often difficult to diagnose, because the pancreas lies deep in the abdomen, behind the stomach, so tumors are not felt during a physical exam. Pancreatic cancer is often called the “silent” cancer because the tumor can grow for many years before it causes pressure, pain, or other signs of illness. When symptoms do appear, they can vary depending on the size of the tumor and where it is located on the pancreas. For these reasons, the symptoms of pancreatic cancer are seldom recognized until the cancer has progressed to an advanced stage and often spread to other areas of the body. General Symptoms Pain The first symptom of pancreatic cancer is often pain, because the tumors invade nerve clusters. Pain can be felt in the stomach area and/or in the back. The pain is generally worse after eating and when lying down, and is sometimes relieved by bending forward. Pain is more common in cancers of the body and tail of the pancreas. The abdomen may also be generally tender or painful if the liver, pancreas or gall bladder are inflamed or enlarged. It is important to keep in mind that there are many other causes of abdominal and back pain! Jaundice More than half of pancreatic cancer sufferers have jaundice, a yellowing of the skin and whites of the eyes. Jaundice is caused by a build-up bilirubin, a substance which is made in the liver and a component of bile. Bilirubin contains a lot of yellow pigment, and gives bile it’s color. -

Hepatitis B? HEPATITIS B Hepatitis B Is a Contagious Liver Disease That Results from Infection with the Hepatitis B Virus
What is Hepatitis B? HEPATITIS B Hepatitis B is a contagious liver disease that results from infection with the Hepatitis B virus. When first infected, a person can develop Are you at risk? an “acute” infection, which can range in severity from a very mild illness with few or no symptoms to a serious condition requiring hospitalization. Acute Hepatitis B refers to the first 6 months after someone is exposed to the Hepatitis B virus. Some people are able to fight the infection and clear the virus. For others, the infection remains and leads to a “chronic,” or lifelong, illness. Chronic Hepatitis B refers to the illness that occurs when the Hepatitis B virus remains in a person’s body. Over time, the infection can cause serious health problems. How is Hepatitis B spread? Hepatitis B is usually spread when blood, semen, or other body fluids from a person infected with the Hepatitis B virus enter the body of someone who is not infected. This can happen through having sex with an infected partner; sharing needles, syringes, or other injection drug equipment; or from direct contact with the blood or open sores of an infected person. Hepatitis B can also be passed from an infected mother to her baby at birth. Who should be tested for Hepatitis B? Approximately 1.2 million people in the United States and 350 million people worldwide have Hepatitis B. Testing for Hepatitis B is recommended for certain groups of people, including: Most are unaware of their infection. ■ People born in Asia, Africa, and other regions with moderate or high rates Is Hepatitis B common? of Hepatitis B (see map) Yes. -
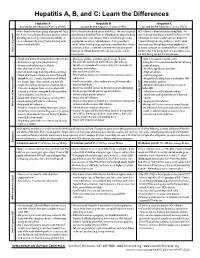
Hepatitis A, B, and C: Learn the Differences
Hepatitis A, B, and C: Learn the Differences Hepatitis A Hepatitis B Hepatitis C caused by the hepatitis A virus (HAV) caused by the hepatitis B virus (HBV) caused by the hepatitis C virus (HCV) HAV is found in the feces (poop) of people with hepa- HBV is found in blood and certain body fluids. The virus is spread HCV is found in blood and certain body fluids. The titis A and is usually spread by close personal contact when blood or body fluid from an infected person enters the body virus is spread when blood or body fluid from an HCV- (including sex or living in the same household). It of a person who is not immune. HBV is spread through having infected person enters another person’s body. HCV can also be spread by eating food or drinking water unprotected sex with an infected person, sharing needles or is spread through sharing needles or “works” when contaminated with HAV. “works” when shooting drugs, exposure to needlesticks or sharps shooting drugs, through exposure to needlesticks on the job, or from an infected mother to her baby during birth. or sharps on the job, or sometimes from an infected How is it spread? Exposure to infected blood in ANY situation can be a risk for mother to her baby during birth. It is possible to trans- transmission. mit HCV during sex, but it is not common. • People who wish to be protected from HAV infection • All infants, children, and teens ages 0 through 18 years There is no vaccine to prevent HCV. -

Gallbladder Removal
Patient Education Partners in Your Surgical Care AMericaN COLLege OF SUrgeoNS DIVisioN OF EDUcatioN Cholecystectomy Surgical Removal of the Gallbladder LaparoscopicLaparoscopic versus versus Open Open Cholecystectomy Cholecystectomy LLaparoscopicaparoscopic Cholecystectomy Cholecystectomy OpenOpen Cholecystectomy Cholecystectomy Patient Education This educational information is to help you be better informed about your operation and empower you with the skills and knowledge needed to actively participate in your care. Keeping You Informed Treatment Options Expectations Information that will help you further understand your operation. Surgery Before your operation— Evaluation usually Education is provided on: Laparoscopic cholecystectomy—The includes blood work, an gallbladder is removed with instruments abdominal ultrasound, Cholecystectomy Overview ............. 1 placed into 4 small slits in the abdomen. and an evaluation by your Condition, Symptoms, Tests ............ 2 Open cholecystectomy—The gallbladder surgeon and anesthesia Treatment Options ......................... 3 is removed through an incision on the provider to review your right side under the rib cage. health history and Risks and Possible Complications ..... 4 medications and to discuss Preparation and Expectations ......... 5 Nonsurgical pain control options. Your Recovery and Discharge ........... 6 Stone retrieval The day of your operation— Pain Control .................................. 7 For gallstones without symptoms You will not eat or drink for at least 4 hours -

The Spectrum of Gallbladder Disease
The Spectrum of Gallbladder Disease Rebecca Kowalski, M.D. October 18, 2017 Overview A (brief) history of gallbladder surgery Anatomy Anatomical variations Physiology Pathophysiology Diagnostic imaging of the gallbladder Natural history of cholelithiasis Case presentations of the spectrum of gallstone disease Summary History of Gallbladder Surgery Gallbladder Surgery: A Relatively Recent Change Prior to the late 1800s, doctors treated gallbladder disease with a cholecystostomy, due to the fear that removing the organ would kill patients Carl Johann August Langenbuch (director of the Lazarus Hospital in Berlin, Germany) practiced on a cadaver to remove the gallbladder, and in 1882, performed a cholecystectomy on a patient. He was discharged after 6 weeks in the hospital https://en.wikipedia.org/wiki/Carl_Langenbuch By 1897 over 100 cholecystectomies had been performed Gallbladder Surgery: A Relatively Recent Change In 1985, Erich Mühe removed a patient’s gallbladder laparoscopically in Germany Erich Muhe https://openi.nlm.ni h.gov/detailedresult. php?img=PMC30152 In 1987, Philippe Mouret (a 44_jsls-2-4-341- French gynecologic surgeon) g01&req=4 performed a laparoscopic cholecystectomy In 1992, the National Institutes of Health (NIH) created guidelines for laparoscopic cholecystectomy in the United Philippe Mouret States, essentially transforming https://www.pinterest.com surgical practice /pin/58195020154734720/ Anatomy and Abnormal Anatomy http://accesssurgery.mhmedical.com/content.aspx?bookid=1202§ionid=71521210 http://www.slideshare.net/pryce27/rsna-final-2 http://www.slideshare.net/pryce27/rsna-final-2 http://www.slideshare.net/pryce27/rsna-final-2 Physiology a http://www.nature.com/nrm/journal/v2/n9/fig_tab/nrm0901_657a_F3.html Simplified overview of the bile acid biosynthesis pathway derived from cholesterol Lisa D. -

Liver, Gallbladder, Bile Ducts, Pancreas
Liver, gallbladder, bile ducts, pancreas Coding issues Otto Visser May 2021 Anatomy Liver, gallbladder and the proximal bile ducts Incidence of liver cancer in Europe in 2018 males females Relative survival of liver cancer (2000 10% 15% 20% 25% 30% 35% 40% 45% 50% 0% 5% Bulgaria Latvia Estonia Czechia Slovakia Malta Denmark Croatia Lithuania N Ireland Slovenia Wales Poland England Norway Scotland Sweden Netherlands Finland Iceland Ireland Austria Portugal EUROPE - Germany 2007) Spain Switzerland France Belgium Italy five year one year Liver: topography • C22.1 = intrahepatic bile ducts • C22.0 = liver, NOS Liver: morphology • Hepatocellular carcinoma=HCC (8170; C22.0) • Intrahepatic cholangiocarcinoma=ICC (8160; C22.1) • Mixed HCC/ICC (8180; TNM: C22.1; ICD-O: C22.0) • Hepatoblastoma (8970; C22.0) • Malignant rhabdoid tumour (8963; (C22.0) • Sarcoma (C22.0) • Angiosarcoma (9120) • Epithelioid haemangioendothelioma (9133) • Embryonal sarcoma (8991)/rhabdomyosarcoma (8900-8920) Morphology*: distribution by sex (NL 2011-17) other other ICC 2% 3% 28% ICC 56% HCC 41% HCC 70% males females * Only pathologically confirmed cases Liver cancer: primary or metastatic? Be aware that other and unspecified morphologies are likely to be metastatic, unless there is evidence of the contrary. For example, primary neuro-endocrine tumours (including small cell carcinoma) of the liver are extremely rare. So, when you have a diagnosis of a carcinoid or small cell carcinoma in the liver, this is probably a metastatic tumour. Anatomy of the bile ducts Gallbladder -

How Is Alcohol Metabolized by the Body?
Overview: How Is Alcohol Metabolized by the Body? Samir Zakhari, Ph.D. Alcohol is eliminated from the body by various metabolic mechanisms. The primary enzymes involved are aldehyde dehydrogenase (ALDH), alcohol dehydrogenase (ADH), cytochrome P450 (CYP2E1), and catalase. Variations in the genes for these enzymes have been found to influence alcohol consumption, alcohol-related tissue damage, and alcohol dependence. The consequences of alcohol metabolism include oxygen deficits (i.e., hypoxia) in the liver; interaction between alcohol metabolism byproducts and other cell components, resulting in the formation of harmful compounds (i.e., adducts); formation of highly reactive oxygen-containing molecules (i.e., reactive oxygen species [ROS]) that can damage other cell components; changes in the ratio of NADH to NAD+ (i.e., the cell’s redox state); tissue damage; fetal damage; impairment of other metabolic processes; cancer; and medication interactions. Several issues related to alcohol metabolism require further research. KEY WORDS: Ethanol-to acetaldehyde metabolism; alcohol dehydrogenase (ADH); aldehyde dehydrogenase (ALDH); acetaldehyde; acetate; cytochrome P450 2E1 (CYP2E1); catalase; reactive oxygen species (ROS); blood alcohol concentration (BAC); liver; stomach; brain; fetal alcohol effects; genetics and heredity; ethnic group; hypoxia The alcohol elimination rate varies state of liver cells. Chronic alcohol con- he effects of alcohol (i.e., ethanol) widely (i.e., three-fold) among individ- sumption and alcohol metabolism are on various tissues depend on its uals and is influenced by factors such as strongly linked to several pathological concentration in the blood T chronic alcohol consumption, diet, age, consequences and tissue damage. (blood alcohol concentration [BAC]) smoking, and time of day (Bennion and Understanding the balance of alcohol’s over time. -

Recently Discovered Interstitial Cell Population of Telocytes: Distinguishing Facts from Fiction Regarding Their Role in The
medicina Review Recently Discovered Interstitial Cell Population of Telocytes: Distinguishing Facts from Fiction Regarding Their Role in the Pathogenesis of Diverse Diseases Called “Telocytopathies” Ivan Varga 1,*, Štefan Polák 1,Ján Kyseloviˇc 2, David Kachlík 3 , L’ubošDanišoviˇc 4 and Martin Klein 1 1 Institute of Histology and Embryology, Faculty of Medicine, Comenius University in Bratislava, 813 72 Bratislava, Slovakia; [email protected] (Š.P.); [email protected] (M.K.) 2 Fifth Department of Internal Medicine, Faculty of Medicine, Comenius University in Bratislava, 813 72 Bratislava, Slovakia; [email protected] 3 Institute of Anatomy, Second Faculty of Medicine, Charles University, 128 00 Prague, Czech Republic; [email protected] 4 Institute of Medical Biology, Genetics and Clinical Genetics, Faculty of Medicine, Comenius University in Bratislava, 813 72 Bratislava, Slovakia; [email protected] * Correspondence: [email protected]; Tel.: +421-90119-547 Received: 4 December 2018; Accepted: 11 February 2019; Published: 18 February 2019 Abstract: In recent years, the interstitial cells telocytes, formerly known as interstitial Cajal-like cells, have been described in almost all organs of the human body. Although telocytes were previously thought to be localized predominantly in the organs of the digestive system, as of 2018 they have also been described in the lymphoid tissue, skin, respiratory system, urinary system, meninges and the organs of the male and female genital tracts. Since the time of eminent German pathologist Rudolf Virchow, we have known that many pathological processes originate directly from cellular changes. Even though telocytes are not widely accepted by all scientists as an individual and morphologically and functionally distinct cell population, several articles regarding telocytes have already been published in such prestigious journals as Nature and Annals of the New York Academy of Sciences. -

Nomina Histologica Veterinaria, First Edition
NOMINA HISTOLOGICA VETERINARIA Submitted by the International Committee on Veterinary Histological Nomenclature (ICVHN) to the World Association of Veterinary Anatomists Published on the website of the World Association of Veterinary Anatomists www.wava-amav.org 2017 CONTENTS Introduction i Principles of term construction in N.H.V. iii Cytologia – Cytology 1 Textus epithelialis – Epithelial tissue 10 Textus connectivus – Connective tissue 13 Sanguis et Lympha – Blood and Lymph 17 Textus muscularis – Muscle tissue 19 Textus nervosus – Nerve tissue 20 Splanchnologia – Viscera 23 Systema digestorium – Digestive system 24 Systema respiratorium – Respiratory system 32 Systema urinarium – Urinary system 35 Organa genitalia masculina – Male genital system 38 Organa genitalia feminina – Female genital system 42 Systema endocrinum – Endocrine system 45 Systema cardiovasculare et lymphaticum [Angiologia] – Cardiovascular and lymphatic system 47 Systema nervosum – Nervous system 52 Receptores sensorii et Organa sensuum – Sensory receptors and Sense organs 58 Integumentum – Integument 64 INTRODUCTION The preparations leading to the publication of the present first edition of the Nomina Histologica Veterinaria has a long history spanning more than 50 years. Under the auspices of the World Association of Veterinary Anatomists (W.A.V.A.), the International Committee on Veterinary Anatomical Nomenclature (I.C.V.A.N.) appointed in Giessen, 1965, a Subcommittee on Histology and Embryology which started a working relation with the Subcommittee on Histology of the former International Anatomical Nomenclature Committee. In Mexico City, 1971, this Subcommittee presented a document entitled Nomina Histologica Veterinaria: A Working Draft as a basis for the continued work of the newly-appointed Subcommittee on Histological Nomenclature. This resulted in the editing of the Nomina Histologica Veterinaria: A Working Draft II (Toulouse, 1974), followed by preparations for publication of a Nomina Histologica Veterinaria.