Two-Part Fractures of the Proximal Humerus
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Isolated Avulsion Fracture of the Lesser Tuberosity of The
(aspects of trauma) Isolated Avulsion Fracture of the Lesser Tuberosity of the Humerus in an Adult: Case Report and Literature Review Aman Dhawan, MD, Kevin Kirk, DO, Thomas Dowd, MD, and William Doukas, MD solated avulsion fractures of also describe our operative technique, comminuted 3-cm lesser tuberosity the lesser tuberosity of the including use of heavy, nonabsorb- fracture fragment retracted approxi- proximal humerus are rare. able suture. mately 2 cm from the donor site We report the case of a right- (Figures 1B–1D). No biceps tendon Ihand–dominant woman in her early ASE EPORT subluxation or injury and no intra- C R 30s who sustained such an injury, A right-hand–dominant woman in articular pathology were noted. with an intact subscapularis tendon her early 30s presented with right The lesser tuberosity fracture was attached to the lesser tuberosity frag- shoulder pain 1 day after a fall down surgically repaired less than 2 weeks ment. Treatment included surgery to a flight of stairs. During the acci- after injury. Through a deltopectoral restore tension to the subscapularis dent, as her feet slipped out from approach, the rotator interval and muscle and maintain the force couple underneath her and her torso fell the 3×2-cm fracture fragment were about the shoulder joint. One year after injury, the patient reported no pain, excellent range of motion, and “[To be diagnosed] this injury...requires... return to activities. This case demonstrates the diag- careful review of orthogonal radiographs nostic challenge of this injury, which requires a high index of suspicion and and advanced imaging.” careful review of orthogonal radio- graphs and advanced imaging. -

Fragility Fractures and Imminent Fracture Risk in Hong Kong: One of the Cities with Longest Life Expectancies
Archives of Osteoporosis (2019) 14:104 https://doi.org/10.1007/s11657-019-0648-4 ORIGINAL ARTICLE Fragility fractures and imminent fracture risk in Hong Kong: one of the cities with longest life expectancies Ronald Man Yeung Wong1 & Wing Tung Ho1 & Law Sheung Wai1 & Wilson Li2 & Wai Wang Chau1 & Kwoon-Ho Simon Chow1 & Wing-Hoi Cheung1 Received: 6 May 2019 /Accepted: 27 August 2019 # International Osteoporosis Foundation and National Osteoporosis Foundation 2019 Abstract Introduction Imminent fracture risk, or fractures within 2 years of an initial fracture, is a pressing issue worldwide. Hong Kong is a city with one of the longest life expectancies. The concern of fragility fractures and the imminent risk of a subsequent fracture is becoming a top priority. The objective of this study was to present the epidemiology of incident fragility fractures of all public acute hospitals and the imminent risk of a subsequent fracture in Hong Kong. Methodology This was a retrospective population-based analysis. Patient records from all acute hospitals in Hong Kong from 1 January 2004 to 31 December 2018 were retrieved for patients ≥ 50 years of age with hip, distal radius, or proximal humerus fractures. Secondary fractures and falls were identified in the subsequent 5 years. Post hoc analysis in recent 2013–2018 period was performed. Overall survival (re-fracture incidence) on age subgroups using Kaplan survival analysis and variables was compared using the log-rank test. Cox proportional hazard regressions, obtaining the hazard ratios (HR) and their respective 95% confidence intervals (CI), were used. Results There is an overall increasing trend of fragility fractures (hip, distal radius, proximal humerus) from 5596 in 2004 to 8465 in 2018. -

Distal Humerus Nonunion After Failed Internal Fixation: Reconstruction with Total Elbow Arthroplasty Dawn M
(aspects of trauma • an original study) Distal Humerus Nonunion After Failed Internal Fixation: Reconstruction With Total Elbow Arthroplasty Dawn M. LaPorte, MD, Michael S. Murphy, MD, and J. Russell Moore, MD ABSTRACT onunion occurs in 2% ing treatment option. In the 1980s, In nonunion after distal humerus to 5% of distal humerus TEA for nonunion with tightly con- fracture, osteoporosis, devas- fractures.1 The condition strained or custom prostheses had cularized fracture fragments, is difficult to treat, and fair to moderately good results but and periarticular fibrosis limit Nno single treatment modality has a high complication rates (4/7, 57%6; potential reconstructive options. high success rate with few compli- 5/14, 36%10). According to a recent We assessed pain relief, func- 2-6 11 tional gains, and complications cations. Without intervention, the review, however, 31 (86%) of 36 in 12 patients whose long-stand- patient is left with a painful, unstable, patients had a satisfactory result with ing, painful nonunions after previ- and often flail extremity and with a semiconstrained prosthesis, and ous treatment with rigid internal limitations in activities of daily liv- only 7 (19%) of the 36 patients had fixation were reconstructed with ing. Frequently, there is an associ- complications. a semiconstrained total elbow ated ulnar neuropathy. Osteoporosis, In the current study, we assessed arthroplasty, frequently with a devascularized fracture fragments, outcomes (complications, symptoms, triceps-sparing approach and and periarticular fibrosis limit poten- function) after semiconstrained anterior ulnar nerve transposition. tial reconstructive options for long- TEA for long-standing distal humer- At mean follow-up of 63 months, 11 patients had good pain relief and standing distal humerus nonunions. -

Body Mechanics As the Rotator Cuff Gether in a Cuff-Shape Across the Greater and Lesser Tubercles the on Head of the Humerus
EXPerT CONTENT Body Mechanics by Joseph E. Muscolino | Artwork Giovanni Rimasti | Photography Yanik Chauvin Rotator Cuff Injury www.amtamassage.org/mtj WORKING WITH CLieNTS AFFecTED BY THIS COmmON CONDITION ROTATOR CUFF GROUP as the rotator cuff group because their distal tendons blend and attach to- The four rotator cuff muscles are gether in a cuff-shape across the greater and lesser tubercles on the head of the supraspinatus, infraspinatus, the humerus. Although all four rotator cuff muscles have specific concen- teres minor, and subscapularis (Fig- tric mover actions at the glenohumeral (GH) joint, their primary functional ure 1). These muscles are described importance is to contract isometrically for GH joint stabilization. Because 17 Before practicing any new modality or technique, check with your state’s or province’s massage therapy regulatory authority to ensure that it is within the defined scope of practice for massage therapy. the rotator cuff group has both mover and stabilization roles, it is extremely functionally active and therefore often physically stressed and injured. In fact, after neck and low back conditions, the shoulder is the most com- Supraspinatus monly injured joint of the human body. ROTATOR CUFF PATHOLOGY The three most common types of rotator cuff pathology are tendinitis, tendinosus, and tearing. Excessive physi- cal stress placed on the rotator cuff tendon can cause ir- ritation and inflammation of the tendon, in other words, tendinitis. If the physical stress is chronic, the inflam- matory process often subsides and degeneration of the fascial tendinous tissue occurs; this is referred to as tendinosus. The degeneration of tendinosus results in weakness of the tendon’s structure, and with continued Teres minor physical stress, whether it is overuse microtrauma or a macrotrauma, a rotator cuff tendon tear might occur. -

Broken Bones: Common Pediatric Lower Extremity Fractures—Part III
10173-06_ON2506-Hart.qxd 11/9/06 3:51 PM Page 390 Broken Bones: Common Pediatric Lower Extremity Fractures—Part III Erin S. Hart ▼ Brenda Luther ▼ Brian E. Grottkau Lower extremity injuries and fractures occur frequently in young usually have pain with hamstring stretching and hip flex- children and adolescents. Nurses are often one of the first ion/abduction). Patients also frequently demonstrate an healthcare providers to assess a child with an injury or fracture. antalgic gait and have pain during their activity or sport. Although basic fracture care and principles can be applied, An anteroposterior radiograph of the pelvis usually reveals nurses caring for these young patients must have a good under- the avulsed fragment. Comparative views of the contralat- standing of normal bone growth and development as well as eral side are often helpful in confirming the diagnosis and avoiding further unnecessary advanced imaging studies. common mechanisms of injury and fracture patterns seen in This injury is usually treated symptomatically and often children. Similar to many of the injuries in the upper extremity, involves rest, application of ice, and relaxation of the in- fractures in the lower extremity in children often can be treated volved tendon (O’Kane, 1999). Conservative treatment of nonoperatively with closed reduction and casting. However, this pelvic avulsion fractures is usually successful. Crutches are article will also review several lower extremity fractures that often needed for several weeks to reduce symptoms and frequently require surgical intervention to obtain a precise rest the extremity involved. Complications following pelvic anatomical reduction. Common mechanisms of injury, fracture avulsion fractures in children are rare, and most patients patterns, and current management techniques will be discussed. -

5Th Metatarsal Fracture
FIFTH METATARSAL FRACTURES Todd Gothelf MD (USA), FRACS, FAAOS, Dip. ABOS Foot, Ankle, Shoulder Surgeon Orthopaedic You have been diagnosed with a fracture of the fifth metatarsal bone. Surgeons This tyPe of fracture usually occurs when the ankle suddenly rolls inward. When the ankle rolls, a tendon that is attached to the fifth metatarsal bone is J. Goldberg stretched. Because the bone is weaker than the tendon, the bone cracks first. A. Turnbull R. Pattinson A. Loefler All bones heal in a different way when they break. This is esPecially true J. Negrine of the fifth metatarsal bone. In addition, the blood suPPly varies to different I. PoPoff areas, making it a lot harder for some fractures to heal without helP. Below are D. Sher descriPtions of the main Patterns of fractures of the fifth metatarsal fractures T. Gothelf and treatments for each. Sports Physicians FIFTH METATARSAL AVULSION FRACTURE J. Best This fracture Pattern occurs at the tiP of the bone (figure 1). These M. Cusi fractures have a very high rate of healing and require little Protection. Weight P. Annett on the foot is allowed as soon as the Patient is comfortable. While crutches may helP initially, walking without them is allowed. I Prefer to Place Patients in a walking boot, as it allows for more comfortable walking and Protects the foot from further injury. RICE treatment is initiated. Pain should be exPected to diminish over the first four weeks, but may not comPletely go away for several months. Follow-uP radiographs are not necessary if the Pain resolves as exPected. -

Fractures of the Proximal Humerus
Fractures of the Proximal Humerus David Rothberg, MDa,*, Thomas Higgins, MDb KEYWORDS Proximal humerus fracture Neer classification Fibular strut Shoulder arthroplasty KEY POINTS Proximal humeral fractures are common. Classification systems have evolved to develop treatment guidelines. Bone quality must be considered for treatment. Surgical stabilization may require augmentation. Arthroplasty must be considered especially in the elderly. INTRODUCTION common osteoporotic extremity fracture after hip fractures and distal radius fractures.1 Greater Proximal humeral fractures are common, with low- than 70% of these fractures occur in patients older energy injuries occurring in the elderly population than 60 years, with a 4:1 female/male ratio and an and less frequent higher-energy fractures striking incidence steadily increasing after the age of 40 young people. The decision to pursue operative years. or nonoperative treatment is driven by the func- Independent risk factors for proximal humeral tional goals and the degree of displacement of fractures include a recent decline in health status, the proximal humeral anatomic parts. Operative insulin-dependent diabetes mellitus, infrequent management is based on the ability to obtain walking, indicators of neuromuscular weakness, and maintain reduction, vascularity of the articular diminished femoral neck bone density, height/ segment, quality of soft-tissue attachments, and weight loss, previous falls, impaired balance, and bone porosity. Despite much study, the optimal maternal history of hip fractures.2 In a 3-decade treatment of significantly displaced fracture population-based study of osteoporotic proximal patterns remains controversial. humeral fractures, Palvanen and colleagues3 found that the incidence in patients older than 60 EPIDEMIOLOGY years increased by 13.7% per year of age. -

Non-Union Humeral Shaft Fracture with Hardware Failure
Non-Union Humeral Shaft Fracture with Hardware Failure Molly Hovendick, MAT, ATC, LAT., Northeastern State University Dylan Morris, DO., Oklahoma State University- Center for Health Sciences Matthew O’Brien, PhD, ATC, LAT., Oklahoma State University- Center for Health Sciences Introduction: Humeral shaft fractures account for three to five percent of all fractures. The unique aspect of this case was the patient suffered from a nonunion humeral fracture and subsequently suffered from surgical hardware failure as well. Background: The patient is a right hand dominant 66-year-old male who presented to the emergency department with left arm pain and disability due to a fall from standing height. Initially, he was treated conservatively and placed into a functional brace. At the follow up visit approximately one month later, he reported continued pain and discomfort in his upper extremity. Although there was concern of a possible delayed union due to a history of cigarette smoking and possible noncompliance with post- operative restrictions the patient elected to proceed with open reduction internal fixation (ORIF) the following day. Shortly following surgery, the patient reported a fall reinjuring his left shoulder while mowing his lawn. Previous symptoms were aggravated and signs of hardware failure through the locking plate was suspected. The decision to perform revision ORIF of the fracture using interfragmentary compression plating with lag screw fixation and bone grafting was made and performed approximately seven months following the initial surgery. Discussion: This case report highlights that while the majority of humeral shaft fractures can successfully be treated conservatively, this method may fail and require delayed open reduction internal fixation. -

Role of Antibiotics in Open Fractures of the Finger
Vol. 15A, No. 5 September 1990 Fasciectomy for treatment qf Dupuyren’s diseaw 16. Hueston JT. ‘Firebreak’ grafts in Dupuytren’s contrac- 20 Honner R, Lamb DW, James JIP. Dupuytren’s contrac- ture. Aust N Z J Surg 1984;54:277-81. ture. long term results after fasiectomy. J Bone Joint Surg 17. Strickland JW. The coverage of difficult digital defects 1971;53B:240-6. with local rotation flaps. In: Strickland JW, Steichen WB, 21 Green TL, Strickland JW, Torstrick RF. The proximal eds. Difficult problems in hand surgery. St. Louis: The interphalangeal joint in Dupuytren’s contracture. In: CV Mosby Company, 1982:38&l. Strickland JW, Steichen WB, eds. Difficult problems in 18. Hueston JT. Limited fasciectomy for Dupuytren’s con- hand surgery. St. Louis: The CV Mosby Company, tracture. Plast Reconstr Surg 1961;27:569-85. 1982:414-18. 19. Zachariae-L. Extensive versus limited fasciectomy for Dupuytren’s contracture. Stand J Plast Reconstr Surg 1967;1:150-3. Role of antibiotics in open fractures of the finger The role of antibiotics was investigated prospectively in 91 open fractures of the finger. Antibiotics were administered to alternate patients with open phalangeal fractures. Only finger fractures distal to the metacarpophalangeal joint were included. Both groups were treated with aggressive surgical irrigation and debridement. In four patients in each group clinical signs of infection eventually developed; osteomyelitis did not develop in any patients, and no secondary surgical procedures were required in either group. This data indicates that vigorous irrigation and debridement is adequate primary treatment for open phalangeal fractures in fingers with intact digital arteries. -

Bone Limb Upper
Shoulder Pectoral girdle (shoulder girdle) Scapula Acromioclavicular joint proximal end of Humerus Clavicle Sternoclavicular joint Bone: Upper limb - 1 Scapula Coracoid proc. 3 angles Superior Inferior Lateral 3 borders Lateral angle Medial Lateral Superior 2 surfaces 3 processes Posterior view: Acromion Right Scapula Spine Coracoid Bone: Upper limb - 2 Scapula 2 surfaces: Costal (Anterior), Posterior Posterior view: Costal (Anterior) view: Right Scapula Right Scapula Bone: Upper limb - 3 Scapula Glenoid cavity: Glenohumeral joint Lateral view: Infraglenoid tubercle Right Scapula Supraglenoid tubercle posterior anterior Bone: Upper limb - 4 Scapula Supraglenoid tubercle: long head of biceps Anterior view: brachii Right Scapula Bone: Upper limb - 5 Scapula Infraglenoid tubercle: long head of triceps brachii Anterior view: Right Scapula (with biceps brachii removed) Bone: Upper limb - 6 Posterior surface of Scapula, Right Acromion; Spine; Spinoglenoid notch Suprspinatous fossa, Infraspinatous fossa Bone: Upper limb - 7 Costal (Anterior) surface of Scapula, Right Subscapular fossa: Shallow concave surface for subscapularis Bone: Upper limb - 8 Superior border Coracoid process Suprascapular notch Suprascapular nerve Posterior view: Right Scapula Bone: Upper limb - 9 Acromial Clavicle end Sternal end S-shaped Acromial end: smaller, oval facet Sternal end: larger,quadrangular facet, with manubrium, 1st rib Conoid tubercle Trapezoid line Right Clavicle Bone: Upper limb - 10 Clavicle Conoid tubercle: inferior -
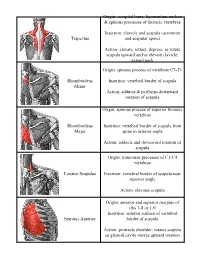
Trapezius Origin: Occipital Bone, Ligamentum Nuchae & Spinous Processes of Thoracic Vertebrae Insertion: Clavicle and Scapul
Origin: occipital bone, ligamentum nuchae & spinous processes of thoracic vertebrae Insertion: clavicle and scapula (acromion Trapezius and scapular spine) Action: elevate, retract, depress, or rotate scapula upward and/or elevate clavicle; extend neck Origin: spinous process of vertebrae C7-T1 Rhomboideus Insertion: vertebral border of scapula Minor Action: adducts & performs downward rotation of scapula Origin: spinous process of superior thoracic vertebrae Rhomboideus Insertion: vertebral border of scapula from Major spine to inferior angle Action: adducts and downward rotation of scapula Origin: transverse precesses of C1-C4 vertebrae Levator Scapulae Insertion: vertebral border of scapula near superior angle Action: elevates scapula Origin: anterior and superior margins of ribs 1-8 or 1-9 Insertion: anterior surface of vertebral Serratus Anterior border of scapula Action: protracts shoulder: rotates scapula so glenoid cavity moves upward rotation Origin: anterior surfaces and superior margins of ribs 3-5 Insertion: coracoid process of scapula Pectoralis Minor Action: depresses & protracts shoulder, rotates scapula (glenoid cavity rotates downward), elevates ribs Origin: supraspinous fossa of scapula Supraspinatus Insertion: greater tuberacle of humerus Action: abduction at the shoulder Origin: infraspinous fossa of scapula Infraspinatus Insertion: greater tubercle of humerus Action: lateral rotation at shoulder Origin: clavicle and scapula (acromion and adjacent scapular spine) Insertion: deltoid tuberosity of humerus Deltoid Action: -

Open Supracondylar Humerus Fractures in Children
Open Access Original Article DOI: 10.7759/cureus.13903 Open Supracondylar Humerus Fractures in Children Tommy Pan 1 , Matthew R. Widner 1 , Michael M. Chau 2 , William L. Hennrikus 3 1. Department of Orthopaedics and Rehabilitation, Penn State College of Medicine, Hershey, USA 2. Department of Orthopaedic Surgery, University of Minnesota Twin Cities, Minneapolis, USA 3. Department of Orthopaedics and Rehabilitation, Penn State Health Milton S. Hershey Medical Center, Hershey, USA Corresponding author: Tommy Pan, [email protected] Abstract Purpose: Supracondylar humerus (SCH) fractures are the most common elbow fracture in children; however, they rarely occur as open injuries. Open fractures are associated with higher rates of infection, neurovascular injury, compartment syndrome, and nonunion. The purpose of this study was to evaluate the treatment and outcomes of open SCH fractures in children. Methods: Between 2008 and 2015, four children (1%) had open injuries among 420 treated for SCH fractures at a single center. The mean patient age was six years (range, four to eight years). Two patients had Gustilo- Anderson grade 1 open fractures and two had grade 2 fractures. Tetanus immunization was up-to-date in all. First dose of intravenous antibiotics was given on average 3hr 7min after onset of injury (range, 1hr 38min to 8hr 15min). Time from injury to irrigation and debridement (I&D) and closed reduction and percutaneous pinning (CRPP) was on average 8hr 16min (range, 4hr 19min to 13hr 15min). All patients received 24-hour intravenous antibiotics. Pins were removed at four weeks and bony union occurred by six weeks. Results: After an average follow-up period of 12 months (range, 6 to 22 months), there were no infections, neurovascular deficits, compartment syndromes, cubitus varus deformities, or range of motion losses.