Teaching Home Exercises for the Rehabilitation of Upper Extremity Problems Scapular Dyskinesis, Rotator Cuff Impingement, and Adhesive Capsulitis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Shoulder Pain Advice and Exercises
Shoulder Pain Advice and Exercises 0523 - Oct 2018 (v1.2) April 2018 April 2021 Please note that if your shoulder pain started after a recent trauma please Simple Exercises contact your GP. Please complete all exercises below as your symptoms allow; aim for no more than 10-15 repetitions of each exercise, 2-3 times a day. Some exercises may cause This booklet has been produced by senior physiotherapists working for discomfort but should not cause significant pain. If your symptoms are not DynamicHealth. It offers simple advice and exercises to help you safely manage improving in 6 - 8 weeks or are worsening please call our Physio Advice Line for your shoulder problem, often the right advice and exercises are all that is needed. further support on 0300 555 0210. This leaflet has been made available to your GP, who may ask you to try the advice and exercises prior to physiotherapy assistance. About the Shoulder A. Shoulder Rolls The shoulder is the most mobile joint in the body. The main shoulder joint is a 1. Sit or stand. ball and socket joint, which allows a wide range of movement. The joint is surrounded by a tough fibrous sleeve called the capsule, which helps to support 2. Roll your shoulders backwards. the joint. A group of four muscles and their tendons make up the rotator cuff, which 3. Repeat up to 10-15 times. Frequency: 2-3 times per day. controls movement and also helps to support the joint. There’s another smaller joint where the top of the shoulder blade meets the collarbone. -

Rotator Cuff and Subacromial Impingement Syndrome: Anatomy, Etiology, Screening, and Treatment
Rotator Cuff and Subacromial Impingement Syndrome: Anatomy, Etiology, Screening, and Treatment The glenohumeral joint is the most mobile joint in the human body, but this same characteristic also makes it the least stable joint.1-3 The rotator cuff is a group of muscles that are important in supporting the glenohumeral joint, essential in almost every type of shoulder movement.4 These muscles maintain dynamic joint stability which not only avoids mechanical obstruction but also increases the functional range of motion at the joint.1,2 However, dysfunction of these stabilizers often leads to a complex pattern of degeneration, rotator cuff tear arthropathy that often involves subacromial impingement.2,22 Rotator cuff tear arthropathy is strikingly prevalent and is the most common cause of shoulder pain and dysfunction.3,4 It appears to be age-dependent, affecting 9.7% of patients aged 20 years and younger and increasing to 62% of patients of 80 years and older ( P < .001); odds ratio, 15; 95% CI, 9.6-24; P < .001.4 Etiology for rotator cuff pathology varies but rotator cuff tears and tendinopathy are most common in athletes and the elderly.12 It can be the result of a traumatic event or activity-based deterioration such as from excessive use of arms overhead, but some argue that deterioration of these stabilizers is part of the natural aging process given the trend of increased deterioration even in individuals who do not regularly perform overhead activities.2,4 The factors affecting the rotator cuff and subsequent treatment are wide-ranging. The major objectives of this exposition are to describe rotator cuff anatomy, biomechanics, and subacromial impingement; expound upon diagnosis and assessment; and discuss surgical and conservative interventions. -

Shoulder Pain: Differential Diagnosis with Mechanical Diagnosis and Therapy Extremity Assessment E a Case Report
Manual Therapy 18 (2013) 354e357 Contents lists available at SciVerse ScienceDirect Manual Therapy journal homepage: www.elsevier.com/math Case report Shoulder pain: Differential diagnosis with mechanical diagnosis and therapy extremity assessment e A case report A. Menon a,S.Mayb,* a Shri Giridhari Physical Therapy Center, Mumbai, India b Faculty of Health and Wellbeing, 38 Collegiate Crescent Campus, Sheffield Hallam University, Sheffield S10 2BP, UK article info abstract Article history: Mechanical Diagnosis and Therapy (MDT) is now probably the only non-specific classification system Received 29 May 2012 that can be used with both spinal and non-spinal patients. Derangement syndrome, which presents with Received in revised form rapid changes in symptoms or mechanical response with the use of repeated movements, appears to be 20 June 2012 common in both spinal and extremity cases. Shoulder problems can be attributed to specific shoulder Accepted 26 June 2012 problems, but may also be referred from the neck. The case report describes a patient presenting with shoulder pain and limitations to shoulder function, and who tested positive to functional shoulder tests. Keywords: However, repeated neck movements demonstrated the ability to worsen and improve the shoulder pain McKenzie ‘ ’ Mechanical diagnosis and therapy and limitations. MDT was an effective tool at making the differential diagnosis between genuine and Shoulder referred shoulder pain. Classification Ó 2012 Elsevier Ltd. All rights reserved. 1. Introduction prognosis and facilitates research (Long et al., 2004; Cook et al., 2005). Shoulder pain is reported to be the most common musculo- The McKenzie Method of Mechanical Diagnosis and Therapy skeletal disorder after spinal pain (Eltayeb et al., 2007). -

Shoulder Pain
Health News from Ponte Vedra Wellness Center Family Chiropractic Care in Ponte Vedra Beach & Nocatee Town Center Dr. Erika Hamer, DC, DIBCN, DIBE CHIROPRACTIC FROM HEAD TO TOE – SHOULDER PAIN he shoulder is a very unique and complex joint. It is the only articulation in the body whose stability is granted primarily by muscular balance instead of being held Ttogether by the integrity of its ligaments. Have you ever heard of the ROTATOR CUFF? This is the collection of four shoulder muscles that help perform this function: namely the supraspinatus, the infraspinatus, the teres minor and subscapularis. In addition, there are multiple bones that come togeth- er to make up the shoulder joint: the humerus (upper arm), the scapula (the shoulder blade) and the clavicle (the collar bone). Therefore, problems with the align- ment of any of these bones will directly aff ect shoulder function, potentially leading to dysfunction and painful symptoms in this joint. Finally, many nerves lead to the shoulder, infl uencing motor control of the shoulder and providing sensory feedback from the shoulder to the brain. The main source of these nerves is the cervical spine (the neck). How Chiropractic Helps Shoulders So, how can your chiropractor help when you have a shoulder problem? Just like every other joint in the body, the shoulder works best when all its moving parts are in proper alignment. As you will discover below, the most important factor contributing to the proper function of the shoulder is the alignment of your spine, with each major area of the spine contributing in a signifi cant way to the health of your shoulder. -

Spontaneous Septic Subacromial Bursitis Due to Streptococcus
A Case Report: Spontaneous Septic Subacromial Bursitis Due to Streptococcus anginosus Emily McGhee, MD, Mohammad Agha, MD, MHA University of Missouri – Columbia Department of Physical Medicine and Rehabilitation Introduction: Discussion: • 67 year old male presented to clinic with 1-2 weeks • Septic subacromial bursitis is rare due to the nature of right shoulder pain, 8/10 achy, no radiation, of the anatomic location of the deep bursa¹ worse with flexion and extension, improved with ice • It is usually seen in immunocompromised patients, • Gastroenteritis 3 days prior with fever of 102°F and after corticosteroid injections, or if there is a vomiting hematogenous spread from another source² • History is significant for HTN, T2DM, OA, bilateral • Of the cases reported in literature, 80% are caused total knee replacements, previous tobacco user, by Staphylococcus aureus² allergies to penicillin and sulfa • Streptococcus anginosus is part of the normal flora of the oral cavity and gastrointestinal tract • It can spread hematogenously and is known for its Clinical Course: ability to cause abscesses • Physical Exam: Vital signs within normal limits. • Streptococcus anginosus has been seen in pubic Right shoulder active abduction 30°, passive symphysis and sternoclavicular joint infections3,4 abduction 80°, 4/5 external and internal rotation, • There have been no reported cases of remainder of exam deferred due to pain. Normal left Figure 1: T2 weighted MRI Right Shoulder - large Streptococcus anginosus causing septic shoulder exam subacromial bursitis fluid collection in subacromial/subdeltoid bursa, • Diagnosed with rotator cuff tear and started physical appears ruptured with fluid extending laterally therapy Conclusion: • Initial x-ray negative, lab work unremarkable along humeral shaft, synovial thickening and • Pain continued, prompting a clinic visit the next day enhancement. -

Calcific Tendinitis of the Shoulder
CME Further Education Certified Advanced Training Orthopäde 2011 [jvn]:[afp]-[alp] P. Diehl1, 2 L. Gerdesmeyer3, 4 H. Gollwitzer3 W. Sauer2 T. Tischer1 DOI 10.1007/s00132-011-1817-3 1 Orthopaedic Clinic and Polyclinic, Rostock University 2 East Munich Orthopaedic Centre, Grafing 3 Orthopaedics and Sports Orthopaedics Clinic, Klinikum rechts der Isar, Online publication date: [OnlineDate] Munich Technical University Springer-Verlag 2011 4 Oncological and Rheumatological Orthopaedics Section, Schleswig-Holstein University Clinic, Kiel Campus Editors: R. Gradinger, Munich R. Graf, Stolzalpe J. Grifka, Bad Abbach A. Meurer, Friedrichsheim Calcific tendinitis of the shoulder Abstract Calcific tendinitis of the shoulder is a process involving crystal calcium deposition in the rotator cuff tendons, which mainly affects patients between 30 and 50 years of age. The etiology is still a matter of dispute. The diagnosis is made by history and physical examination with specific attention to radiologic and sonographic evidence of calcific deposits. Patients usually describe specific radiation of the pain to the lateral proximal forearm, with tenderness even at rest and during the night. Nonoperative management including rest, nonsteroidal anti-inflammatory drugs, subacromial corticosteroid injections, and shock wave therapy is still the treatment of choice. Nonoperative treatment is successful in up to 90 % of patients. When nonsurgical measures fail, surgical removal of the calcific deposit may be indicated. Arthroscopic treatment provides excellent results in more than 90 % of patients. The recovery process is very time consuming and may take up to several months in some cases. Keywords Rotator cuff Tendons Tendinitis Calcific tendinitis Calcification, pathologic English Translation oft he original article in German „Die Kalkschulter – Tendinosis calcarea“ in: Der Orthopäde 8 2011 733 This article explains the causes and development of calcific tendinitis of the shoulder, with special focus on the diagnosis of the disorder and the existing therapy options. -

Welcome Pack
Jing Certificate in Advanced Clinical Massage WELCOME PACK JING INSTITUTE OF ADVANCED MASSAGE TRAINING PO BOX 5291, BRIGHTON BN50 8AG l VAT NO: 866374290 CONTACT US www.jingmassage.com 1 2 Table of Contents Section 1: Syllabus and summary of modules Section 2: Guidance notes for students and contract Section 3: Reading list Section 4: Notes on assessment Section 5: Structuring your study; guidelines and sample quizzes 3 4 Certificate in Advanced Clinical Massage – Student syllabus Learning Assessment Criteria Underpinning knowledge Outcome UnitIntroduction to Advanced Massage Techniques – 120 learning hours 1 1.1 Utilise 1.1.1 Evaluate Client assessment – record taking based on appropriate assessment HOPRS; basic visual assessment; range of assessment techniques based movement; pain levels techniques for on HOPRS Client communication – explanation of presenting 1.1.2 Utilise correct treatment; importance of communication & client assessment conditions techniques for feedback; basic listening & questioning based on presenting client skills; non verbal communication in HOPRS conditions assessment 1.2 Demonstrate 1.2.1 Perform all specific Techniques – effleurage; petrissage; the ability to techniques tapotement; trigger point therapy; perform all correctly on neuromuscular techniques; muscle energy specific superficial muscles technique; myofascial release including techniques 1.2.2 Perform all specific indirect and direct fascial approaches, correctly and techniques appropriately appropriately using structural integration, basics of craniosacral -

WCAT Decision 2005-02580
WCAT Decision Number: WCAT-2005-02580 NOTEWORTHY DECISION SUMMARY Decision: WCAT-2005-02580 Panel: Joanne Kembel Decision Date: May 19, 2005 Pre-existing Conditions – Shoulder Dislocation – Wage Loss Benefits – Section 29(1) of the Workers Compensation Act – Section 30(1) of the Act – Policy Item #15.60 of the Rehabilitation Services and Claims Manual, Volume II (RSCM II) This case is noteworthy as an example of the application of those portions of policy item #15.60 of the Rehabilitation Services and Claims Manual, Volume II (RSCM II) which provide rules for the payment of benefits in shoulder dislocation claims where the worker has previously experienced a non-compensable shoulder dislocation. Item #15.60 of the RSCM II provides that if a worker has a prior non-compensable shoulder dislocation and suffers another dislocation at work, the later dislocation will only be compensable if there was a work incident of “sufficient causative significance to induce the further dislocation”. Once the claim is accepted the policy provides rules in respect of the payment of benefits. The policy provides, firstly, that temporary wage loss benefits will “normally endure no more than two weeks,” and secondly, that any surgery, after the injury, which is directed at repairing damage from the prior dislocation will not be compensable except in cases where: a) the shoulder has been stable for many years prior to the dislocation at work, or b) the dislocation at work was induced by “severe trauma.” In this case, the worker dislocated his left shoulder. The worker had a long history of left shoulder dislocations, and had surgery on his left shoulder three years earlier. -

SHOULDER PROBLEMS Yourphysio Ongoing Needs
SPRING 2011 Q: I suffer from back pain. Q: My mother fractured her wrist. The plaster has just 25 Wantirna Road What should I do? come off. When should she start physio? RINGWOOD25 Wantirna VIC Road 3134 PHRINGWOOD (03) 9870 VIC 8193 3134 A: Have your back problem www.physica.com.auPH (03) 9870 8193 assessed by a physio as soon as SPRING 2011 you can. Treatments such as manual therapy (to free up stiff and Dear Patient, www.physica.com.auHOURS painful spinal joints), mobilizing exercises and exercises aimed at WelcomeDear Patient,to our newsletter and The practiceHOURS hours are strengthening your core muscles can help a lot of back problems. Medications such as pain killers and anti-inflammatory can thanksWelcome for comingto our newsletter to see us for and your physio needs. MON-FRI:The practice 7.00am hours - 8.00pm are be useful but don’t actually fix the problem. Don’t rely on thanks for coming to see us for your SHOULDER PROBLEMS Yourphysio ongoing needs. health is very important MON-FRI:SAT: 8.00am 7.00am - 1pm- 8.00pm theses passive measures. Take control by consulting your A: Start physio straight away. Your mother needs to get the physiotherapist. wrist moving and to regain strength as soon as possible so that toYour all ofongoing us here health at the is clinic. very importantWe hope (Please SAT:ring for8.00am an appointment) - 1pm See your physiotherapist for a quick recovery she can get back to normal activity. Leaving physio off for too thatto all this of newsletterus here at thewill clinic.help keep We hopeyou (Please ring for an appointment) up to date with information about Q: I sit at a desk all day. -

Protocol for a Multi-Site Pilot and Feasibility Randomised Controlled Trial
Littlewood et al. Pilot and Feasibility Studies (2021) 7:17 https://doi.org/10.1186/s40814-020-00714-x STUDY PROTOCOL Open Access Protocol for a multi-site pilot and feasibility randomised controlled trial: Surgery versus PhysiothErapist-leD exercise for traumatic tears of the rotator cuff (the SPeEDy study) Chris Littlewood1,2* , Julia Wade3, Stephanie Butler-Walley1,4, Martyn Lewis1,4, David Beard5, Amar Rangan5,6, Gev Bhabra7, Socrates Kalogrianitis8, Cormac Kelly9, Saurabh Mehta10, Harvinder Pal Singh11, Matthew Smith12, Amol Tambe13, James Tyler14 and Nadine E. Foster1 Abstract Background: Clinically, a distinction is made between types of rotator cuff tear, traumatic and non-traumatic, and this sub-classification currently informs the treatment pathway. It is currently recommended that patients with traumatic rotator cuff tears are fast tracked for surgical opinion. However, there is uncertainty about the most clinically and cost-effective intervention for patients with traumatic rotator cuff tears and further research is required. SPeEDy will assess the feasibility of a fully powered, multi-centre randomised controlled trial (RCT) to test the hypothesis that, compared to surgical repair (and usual post-operative rehabilitation), a programme of physiotherapist-led exercise is not clinically inferior, but is more cost-effective for patients with traumatic rotator cuff tears. Methods: SPeEDy is a two-arm, multi-centre pilot and feasibility RCT with integrated Quintet Recruitment Intervention (QRI) and further qualitative investigation of patient experience. A total of 76 patients with traumatic rotator cuff tears will be recruited from approximately eight UK NHS hospitals and randomly allocated to either surgical repair and usual post-operative rehabilitation or a programme of physiotherapist-led exercise. -

Shoulder Instability Anatomy
Shoulder Instability The shoulder is your body’s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder is made up of bones, muscles, ligaments, and tendons. They work together so you can comfortably reach, swing, lift, and throw a ball. Learning about the parts of the shoulder will help you understand your shoulder problem. Anatomy Bones provide the foundation of the shoulder joint. The bones fit together in a way that allows the arm to move freely. • The humeral head is the ball at the top of the humerus (arm bone). • The glenoid is the shallow socket located on the scapula (shoulder blade). • The labrum is a ring of cartilage around the rim of the glenoid. Important ligaments attach to the labrum and connect to the humerus. The labrum and these ligaments provide stability to the shoulder joint. • The coracoid and acromion are two other parts of the scapula. Muscles attach on these structures. • The clavicle is the collar bone. The clavicle connects to the acromion, forming the acromioclavicular (AC) joint. Soft tissues include muscles, tendons, and ligaments. These connect the shoulder bones together, provide stability, and movement to the joint. • The capsule is a sheet of tough fibers that encloses the joint. The glenohumeralligaments are thickened parts of the Capsule capsule that connect the humerus to the labrum. The labrum is firmly attached to the rim of the glenoid. The capsule, ligaments, and labrum provide most of the stability to the shoulder joint. -
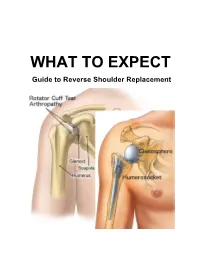
Guide to Reverse Shoulder Replacement TABLE of CONTENTS
WHAT TO EXPECT Guide to Reverse Shoulder Replacement TABLE OF CONTENTS 1. Introduction Welcome Letter Key Contacts Our Neighborhood 2. Surgery Preparation What is a Reverse Shoulder Replacement? Pre-Operation Checklist Planning Your Hospital Stay 3. Day of Surgery What to Expect on the Day of Surgery Your Anesthesiologist and Anesthesia Blood Transfusions 4. Initial Recovery in Post Anesthesia Care Unit Overview Relaxation Exercises Pain Management 5. Recovery & Rehabilitation Overview of Post-Operative Recovery Prevention of Post-Operative Complications Anticoagulation Therapy & Thrombosis Rehabilitation Overview 2 TABLE OF CONTENTS (continued) 6. Progress Guidelines Post Reverse Shoulder Replacement 7. Discharge Instructions Surgical Site Care Pain Management Protection Against Infection When Can You Begin Driving? Follow Up Appointments 8. Home Recovery & Exercise General Recovery Guidelines Bathing/Showering Dressing Rehabilitation 9. Nutrition Nutrition Before Surgery Nutrition on Day of Surgery Nutrition During Hospital Stay Nutrition After Discharge Food Guide Pyramid My Meal Plan: 1200 Calories 1800 Calories 2200 Calories . 10. Other Pastoral Care Other Educational Resources 3 Dear Patient, Welcome to Covenant Healthcare. In an effort to help you get the most out of your hospital experience, we have developed this guide to help you before, during, and after your hospital stay. The objectives of this guide are: 1) To help prepare you for your surgery and hospital experience 2) To optimize your recovery from your Reverse Shoulder Replacement while in the hospital and later at home. It is important to remember that this is only a general guide to recovery from your surgery. Keep in mind that not all patients have the same medical conditions or needs.