Anatomy of Brachial and Lumbosacral Plexus
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Intrapartum Lesions to the Lumbar Portion of the Lumbosacral Plexus: an Anatomical Review
REVIEW Eur. J. Anat. 23 (2): 83-90 (2019) Intrapartum lesions to the lumbar portion of the lumbosacral plexus: an anatomical review Shanna E. Williams, Asa C. Black, Jr. Department of Biomedical Sciences, University of South Carolina School of Medicine Greenville, Greenville, SC, USA SUMMARY Key words: Plexopathy – Radiculopathy – Neu- The lumbosacral plexus is formed by the ventral ropathy – Pregnancy – Foot drop rami of L2-S3 and provides sensory and motor branches to the lower extremity. The spatial orien- INTRODUCTION tation of the lumbar portion of the plexus above the pelvic brim leaves it particularly susceptible to in- The lumbosacral plexus is formed by the ventral trapartum injury by the fetal head. Such lesions are rami of the L2-S3 segments, with some contribu- subdivided into two groups: upper lumbar plexus tions from L1 and S4 segments. It gives rise to six (L1-L4) and lumbosacral trunk (L4-L5). Given the sensory nerves of the thigh and leg, and six major root levels involved, upper lumbar plexus lesions sensorimotor nerves responsible for innervating 43 produce symptoms suggestive of iliohypogastric, muscles of the lower extremity (Van Alfen and ilioinguinal, genitofemoral, femoral, and obturator Malessy, 2013). As the name would suggest, it neuropathies or L4 radiculopathies. Alternatively, consists of two components, the lumbar plexus involvement of the lumbosacral trunk can imitate a and the sacral plexus, which are spatially separat- common fibular (peroneal) neuropathy or L5 ed. This anatomical separation results in a clinical radiculopathy. This symptomatic overlap with vari- division of lumbosacral plexus lesions into those ous neuropathies and radiculopathies, makes di- affecting the lumbar plexus and those affecting the agnosis of such lesions particularly challenging. -

Ischaemic Lumbosacral Plexopathy in Acute Vascular Compromise:Case Report
Parapkgia 29 (1991) 70-75 © 1991 International Medical Soci<ty of Paraplegia Paraplegia L-_________________________________________________ � Ischaemic Lumbosacral Plexopathy in Acute Vascular Compromise: Case Report D.X. Cifu, MD, K.D. Irani, MD Department of Physical Medicine, Baylor College of Medicine, Houston, Texas, USA. Summary Anterior spinal artery syndrome (ASAS) is a well reported cause of spinal cord injury (SCI) following thoracoabdominal aortic surgery. The resultant deficits are often incom plete, typically attributed to the variable nature of the vascular distribution. Our Physi cal Medicine and Rehabilitation (PM and Rehabilitation) service was consulted about a 36-year-old patient with generalised deconditioning, 3 months after a stab wound to the left ventricle. Physical examination revealed marked lower extremity weakness, hypo tonia, hyporeflexia, and a functioning bowel and bladder. Further questioning disclosed lower extremity dysesthesias. Nerve conduction studies showed slowed velocities, pro longed distal latencies and decreased amplitudes of all lower extremity nerves. Electro myography revealed denervation of all proximal and distal lower extremity musculature, with normal paraspinalis. Upper extremity studies were normal. Recently, 3 cases of ischaemic lumbosacral plexopathy, mimicking an incomplete SCI, have been reported. This distinction is particularly difficult in the poly trauma patient with multiple musculo skeletal injuries or prolonged recuperation time, in addition to a vascular insult, as in this patient. The involved anatomical considerations will be discussed. A review of the elec trodiagnostic data from 30 patients, with lower extremity weakness following acute ischaemia, revealed a 20% incidence of spinal cord compromise, but no evidence of a plexopathy. Key words: Ischaemia; Lumbosacral plexopathy; Electromyography. Recent advances in cardiovascular and trauma surgery have led to increased survi val of patients following cardiac and great vessel trauma or insult. -

Clinical Presentations of Lumbar Disc Degeneration and Lumbosacral Nerve Lesions
Hindawi International Journal of Rheumatology Volume 2020, Article ID 2919625, 13 pages https://doi.org/10.1155/2020/2919625 Review Article Clinical Presentations of Lumbar Disc Degeneration and Lumbosacral Nerve Lesions Worku Abie Liyew Biomedical Science Department, School of Medicine, Debre Markos University, Debre Markos, Ethiopia Correspondence should be addressed to Worku Abie Liyew; [email protected] Received 25 April 2020; Revised 26 June 2020; Accepted 13 July 2020; Published 29 August 2020 Academic Editor: Bruce M. Rothschild Copyright © 2020 Worku Abie Liyew. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Lumbar disc degeneration is defined as the wear and tear of lumbar intervertebral disc, and it is mainly occurring at L3-L4 and L4-S1 vertebrae. Lumbar disc degeneration may lead to disc bulging, osteophytes, loss of disc space, and compression and irritation of the adjacent nerve root. Clinical presentations associated with lumbar disc degeneration and lumbosacral nerve lesion are discogenic pain, radical pain, muscular weakness, and cutaneous. Discogenic pain is usually felt in the lumbar region, or sometimes, it may feel in the buttocks, down to the upper thighs, and it is typically presented with sudden forced flexion and/or rotational moment. Radical pain, muscular weakness, and sensory defects associated with lumbosacral nerve lesions are distributed on -
4-Brachial Plexus and Lumbosacral Plexus (Edited).Pdf
Color Code Brachial Plexus and Lumbosacral Important Doctors Notes Plexus Notes/Extra explanation Please view our Editing File before studying this lecture to check for any changes. Objectives At the end of this lecture, the students should be able to : Describe the formation of brachial plexus (site, roots) List the main branches of brachial plexus Describe the formation of lumbosacral plexus (site, roots) List the main branches of lumbosacral plexus Describe the important Applied Anatomy related to the brachial & lumbosacral plexuses. Brachial Plexus Formation Playlist o It is formed in the posterior triangle of the neck. o It is the union of the anterior rami (or ventral) of the 5th ,6th ,7th ,8th cervical and the 1st thoracic spinal nerves. o The plexus is divided into 5 stages: • Roots • Trunks • Divisions • Cords • Terminal branches Really Tired? Drink Coffee! Brachial Plexus A P A P P A Brachial Plexus Trunks Divisions Cords o Upper (superior) trunk o o Union of the roots of Each trunk divides into Posterior cord: C5 & C6 anterior and posterior From the 3 posterior division divisions of the 3 trunks o o Middle trunk Lateral cord: From the anterior Continuation of the divisions of the upper root of C7 Branches and middle trunks o All three cords will give o Medial cord: o Lower (inferior) trunk branches in the axilla, It is the continuation of Union of the roots of the anterior division of C8 & T1 those will supply their respective regions. the lower trunk The Brachial Plexus Long Thoracic (C5,6,7) Anterior divisions Nerve to Subclavius(C5,6) Posterior divisions Dorsal Scapular(C5) Suprascapular(C5,6) upper C5 trunk Lateral Cord C6 middle (2LM) trunk C7 lower C8 trunk T1 Posterior Cord (ULTRA) Medial Cord (4MU) In the PowerPoint presentation this slide is animated. -

Lumbosacral Plexus Entrapment Syndrome. Part One: a Common Yet Little-Known Cause of Chronic Pelvic and Lower Extremity Pain
3-A Running head: ANAESTHESIA, PAIN & INTENSIVE CARE www.apicareonline.com ORIGINAL ARTICLE Lumbosacral plexus entrapment syndrome. Part one: A common yet little-known cause of chronic pelvic and lower extremity pain Kjetil Larsen, CES, George C. Chang Chien, D O2 ABSTRACT Corrective exercise specialist, Training & Rehabilitation, Oslo Lumbosacral plexus entrapment syndrome (LPES) is a little-known but common cause Norway of chronic lumbopelvic and lower extremity pain. The lumbar plexus, including the 2 Director of pain management, lumbosacral tunks emerge through the fibers of the psoas major, and the proximal Ventura County Medical Center, sciatic nerve beneath the piriformis muscles. Severe weakness of these muscles may Ventura, CA 93003, USA. lead to entrapment plexopathy, resulting in diffuse and non-specific pain patterns Correspondence: Kjetil Larsen, CES, Corrective throughout the lumbopelvic complex and lower extremities (LPLE), easily mimicking Exercise Specialist, Training & other diagnoses and is therefore likely to mislead the interpreting clinician. It is a Rehabilitation, Oslo Norway; pathology very similar to that of thoracic outlet syndrome, but for the lower body. This Kjetil@trainingandrehabilitation. two part manuscript series was written in an attempt to demonstrate the existence, com; pathophysiology, diagnostic protocol as well as interventional strategy for LPES, and Tel.: +47 975 45 192 its efficacy. Received: 23 November 2018, Reviewed & Accepted: 28 Key words: Pelvic girdle; Pain, Pelvic girdle; Lumbosacral plexus entrapment syndrome; February 2019 Piriformis syndrome; Nerve entrapment; Double-crush; Pain, Chronic; Fibromyalgia Citation: Larsen K, Chien GCC. Lumbosacral plexus entrapment syndrome. Part one: A common yet little-known cause of chronic pelvic and lower extremity pain. -

LECTURE (SACRAL PLEXUS, SCIATIC NERVE and FEMORAL NERVE) Done By: Manar Al-Eid Reviewed By: Abdullah Alanazi
CNS-432 LECTURE (SACRAL PLEXUS, SCIATIC NERVE AND FEMORAL NERVE) Done by: Manar Al-Eid Reviewed by: Abdullah Alanazi If there is any mistake please feel free to contact us: [email protected] Both - Black Male Notes - BLUE Female Notes - GREEN Explanation and additional notes - ORANGE Very Important note - Red CNS-432 Objectives: By the end of the lecture, students should be able to: . Describe the formation of sacral plexus (site & root value). List the main branches of sacral plexus. Describe the course of the femoral & the sciatic nerves . List the motor and sensory distribution of femoral & sciatic nerves. Describe the effects of lesion of the femoral & the sciatic nerves (motor & sensory). CNS-432 The Mind Maps Lumber Plexus 1 Branches Iliohypogastric - obturator ilioinguinal Femoral Cutaneous branches Muscular branches to abdomen and lower limb 2 Sacral Plexus Branches Pudendal nerve. Pelvic Splanchnic Sciatic nerve (largest nerves nerve), divides into: Tibial and divides Fibular and divides into : into: Medial and lateral Deep peroneal Superficial planter nerves . peroneal CNS-432 Remember !! gastrocnemius Planter flexion – knee flexion. soleus Planter flexion Iliacus –sartorius- pectineus – Hip flexion psoas major Quadriceps femoris Knee extension Hamstring muscles Knee flexion and hip extension gracilis Hip flexion and aids in knee flexion *popliteal fossa structures (superficial to deep): 1-tibial nerve 2-popliteal vein 3-popliteal artery. *foot drop : planter flexed position Common peroneal nerve injury leads to Equinovarus Tibial nerve injury leads to Calcaneovalgus CNS-432 Lumbar Plexus Formation Ventral (anterior) rami of the upper 4 lumbar spinal nerves (L1,2,3 and L4). Site Within the substance of the psoas major muscle. -
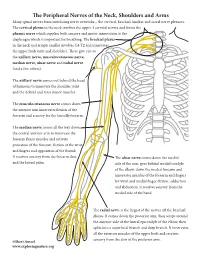
The Peripheral Nerves of the Neck, Shoulders and Arms Many Spinal Nerves Form Interlacing Nerve Networks – the Cervical, Brachial, Lumbar and Sacral Nerve Plexuses
The Peripheral Nerves of the Neck, Shoulders and Arms Many spinal nerves form interlacing nerve networks – the cervical, brachial, lumbar and sacral nerve plexuses. The cervical plexus in the neck involves the upper 4 cervical nerves and forms the phrenic nerve which supplies both sensory and motor innervation to the diaphragm which is important for breathing. The brachial plexus in the neck and armpit (axilla) involves C4-T2 and innervates the upper limb (arm and shoulder). These give rise to the axillary nerve, musculocutaneous nerve, median nerve, ulnar nerve and radial nerve (and a few others). The axillary nerve comes out behind the head of humerus to innervate the shoulder joint and the deltoid and teres minor muscles. The musculocutaneous nerve comes down the anterior arm innervates flexion of the forearm and sensory for the laterally forearm. The median nerve comes all the way down the central anterior arm to innervate the forearm flexor muscles and activate pronation of the forearm, flexion of the wrist and fingers and opposition of the thumb. It receives sensory from the forearm skin The ulnar nerve comes down the medial and the lateral palm. side of the arm, goes behind medial condyle of the elbow, down the medial forearm and innervates muscles of the forearm and fingers for wrist and medial finger flexion, adduction and abduction. It receives sensory from the medial side of the hand. The radial nerve is the largest of the nerves off the brachial plexus. It comes down the posterior arm, then wraps around the anterior aide of the lateral epicondyle of the elbow, then splits into a superficial branch and deep branch. -

Anatomy of Spinal Nerves in the First Turkish Illustrated Anatomy Handwritten Textbook
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by DSpace@HKU Childs Nerv Syst DOI 10.1007/s00381-016-3136-9 COVER EDITORIAL Anatomy of spinal nerves in the first Turkish illustrated anatomy handwritten textbook Murat Çetkin1 & Mustafa Orhan1 & İlhan Bahşi1 & Begümhan Turhan2 Received: 26 May 2016 /Accepted: 30 May 2016 # Springer-Verlag Berlin Heidelberg 2016 BTeşrih-ül Ebdan ve Tercümânı Kıbale-i Feylesûfan^ is the the book, İtâḳî acknowledges the contributions of the Grand first handwritten anatomy textbook with illustrations written Vizier [4, 7]. in Turkish in 17th century by Şemseddîn-i İtâḳî. BTeşrih^ has Not many textbooks about anatomy existed in the Islamic different meanings such as anatomy, skeleton, and cutting a World and the Ottoman Empire until İtâḳî’sbook[9]. In other corpse into pieces [1]. BTeşrih-ül Ebdan ve Tercümânı Kıbale- medical textbooks, anatomy occupies only a few pages in i Feylesûfan ^ means dissection of the body and scholars’ different sections [4]. İtâḳî’s book is a pioneer in its area as birth knowledge [2]. Since this is the first handwritten text- it is written in Turkish, and it is supported with illustrations book in Turkish, it has great importance in the development of [4]. In addition to Turkish, the book contains mostly Arabic medicine in Ottoman Empire. This book was written while and rarely Persian terms as well [4, 6, 7]. Some editions of this Grand Vizier Recep Pasha was in power, and it was dedicated book which was written in the 17th century were reprinted in to the Sultan of that period, Murat the IVth [3, 4]. -

The Spinal Nerves That Constitute the Plexus Lumbosacrales of Porcupines (Hystrix Cristata)
Original Paper Veterinarni Medicina, 54, 2009 (4): 194–197 The spinal nerves that constitute the plexus lumbosacrales of porcupines (Hystrix cristata) A. Aydin, G. Dinc, S. Yilmaz Faculty of Veterinary Medicine, Firat University, Elazig, Turkey ABSTRACT: In this study, the spinal nerves that constitute the plexus lumbosacrales of porcupines (Hystrix cristata) were investigated. Four porcupines (two males and two females) were used in this work. Animals were appropriately dissected and the spinal nerves that constitute the plexus lumbosacrales were examined. It was found that the plexus lumbosacrales of the porcupines was formed by whole rami ventralis of L1, L2, L3, L4, S1 and a fine branch from T15 and S2. The rami ventralis of T15 and S2 were divided into two branches. The caudal branch of T15 and cranial branch of S2 contributed to the plexus lumbosacrales. At the last part of the plexus lumbosacrales, a thick branch was formed by contributions from the whole of L4 and S1, and a branch from each of L3 and S2. This root gives rise to the nerve branches which are disseminated to the posterior legs (caudal glu- teal nerve, caudal cutaneous femoral nerve, ischiadic nerve). Thus, the origins of spinal nerves that constitute the plexus lumbosacrales of porcupine differ from rodantia and other mammals. Keywords: lumbosacral plexus; nerves; posterior legs; porcupines (Hystrix cristata) List of abbreviations M = musculus, T = thoracal, L = lumbal, S = sacral, Ca = caudal The porcupine is a member of the Hystricidae fam- were opened by an incision made along the linea ily, a small group of rodentia (Karol, 1963; Weichert, alba and a dissection of the muscles. -

Study of Anatomical Pattern of Lumbar Plexus in Human (Cadaveric Study)
54 Az. J. Pharm Sci. Vol. 54, September, 2016. STUDY OF ANATOMICAL PATTERN OF LUMBAR PLEXUS IN HUMAN (CADAVERIC STUDY) BY Prof. Gamal S Desouki, prof. Maged S Alansary,dr Ahmed K Elbana and Mohammad H Mandor FROM Professor Anatomy and Embryology Faculty of Medicine - Al-Azhar University professor of anesthesia Faculty of Medicine - Al-Azhar University Anatomy and Embryology Faculty of Medicine - Al-Azhar University Department of Anatomy and Embryology Faculty of Medicine of Al-Azhar University, Cairo Abstract The lumbar plexus is situated within the substance of the posterior part of psoas major muscle. It is formed by the ventral rami of the frist three nerves and greater part of the fourth lumbar nerve with or without a contribution from the ventral ramus of last thoracic nerve. The pattern of formation of lumbar plexus is altered if the plexus is prefixed (if the third lumbar is the lowest nerve which enters the lumbar plexus) or postfixed (if there is contribution from the 5th lumbar nerve). The branches of the lumbar plexus may be injured during lumbar plexus block and certain surgical procedures, particularly in the lower abdominal region (appendectomy, inguinal hernia repair, iliac crest bone graft harvesting and gynecologic procedures through transverse incisions). Thus, a better knowledge of the regional anatomy and its variations is essential for preventing the lesions of the branches of the lumbar plexus. Key Words: Anatomical variations, Lumbar plexus. Introduction The lumbar plexus formed by the ventral rami of the upper three nerves and most of the fourth lumbar nerve with or without a contribution from the ventral ramous of last thoracic nerve. -

Lower Extremity Focal Neuropathies
LOWER EXTREMITY FOCAL NEUROPATHIES Lower Extremity Focal Neuropathies Arturo A. Leis, MD S.H. Subramony, MD Vettaikorumakankav Vedanarayanan, MD, MBBS Mark A. Ross, MD AANEM 59th Annual Meeting Orlando, Florida Copyright © September 2012 American Association of Neuromuscular & Electrodiagnostic Medicine 2621 Superior Drive NW Rochester, MN 55901 Printed by Johnson Printing Company, Inc. 1 Please be aware that some of the medical devices or pharmaceuticals discussed in this handout may not be cleared by the FDA or cleared by the FDA for the specific use described by the authors and are “off-label” (i.e., a use not described on the product’s label). “Off-label” devices or pharmaceuticals may be used if, in the judgment of the treating physician, such use is medically indicated to treat a patient’s condition. Information regarding the FDA clearance status of a particular device or pharmaceutical may be obtained by reading the product’s package labeling, by contacting a sales representative or legal counsel of the manufacturer of the device or pharmaceutical, or by contacting the FDA at 1-800-638-2041. 2 LOWER EXTREMITY FOCAL NEUROPATHIES Lower Extremity Focal Neuropathies Table of Contents Course Committees & Course Objectives 4 Faculty 5 Basic and Special Nerve Conduction Studies of the Lower Limbs 7 Arturo A. Leis, MD Common Peroneal Neuropathy and Foot Drop 19 S.H. Subramony, MD Mononeuropathies Affecting Tibial Nerve and its Branches 23 Vettaikorumakankav Vedanarayanan, MD, MBBS Femoral, Obturator, and Lateral Femoral Cutaneous Neuropathies 27 Mark A. Ross, MD CME Questions 33 No one involved in the planning of this CME activity had any relevant financial relationships to disclose. -

The Neuroanatomy of Female Pelvic Pain
Chapter 2 The Neuroanatomy of Female Pelvic Pain Frank H. Willard and Mark D. Schuenke Introduction The female pelvis is innervated through primary afferent fi bers that course in nerves related to both the somatic and autonomic nervous systems. The somatic pelvis includes the bony pelvis, its ligaments, and its surrounding skeletal muscle of the urogenital and anal triangles, whereas the visceral pelvis includes the endopelvic fascial lining of the levator ani and the organ systems that it surrounds such as the rectum, reproductive organs, and urinary bladder. Uncovering the origin of pelvic pain patterns created by the convergence of these two separate primary afferent fi ber systems – somatic and visceral – on common neuronal circuitry in the sacral and thoracolumbar spinal cord can be a very dif fi cult process. Diagnosing these blended somatovisceral pelvic pain patterns in the female is further complicated by the strong descending signals from the cerebrum and brainstem to the dorsal horn neurons that can signi fi cantly modulate the perception of pain. These descending systems are themselves signi fi cantly in fl uenced by both the physiological (such as hormonal) and psychological (such as emotional) states of the individual further distorting the intensity, quality, and localization of pain from the pelvis. The interpretation of pelvic pain patterns requires a sound knowledge of the innervation of somatic and visceral pelvic structures coupled with an understand- ing of the interactions occurring in the dorsal horn of the lower spinal cord as well as in the brainstem and forebrain. This review will examine the somatic and vis- ceral innervation of the major structures and organ systems in and around the female pelvis.