Body Part Key of ICD-10-PCS for the Nerves of the Head, Neck, and Trunk
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Intrapartum Lesions to the Lumbar Portion of the Lumbosacral Plexus: an Anatomical Review
REVIEW Eur. J. Anat. 23 (2): 83-90 (2019) Intrapartum lesions to the lumbar portion of the lumbosacral plexus: an anatomical review Shanna E. Williams, Asa C. Black, Jr. Department of Biomedical Sciences, University of South Carolina School of Medicine Greenville, Greenville, SC, USA SUMMARY Key words: Plexopathy – Radiculopathy – Neu- The lumbosacral plexus is formed by the ventral ropathy – Pregnancy – Foot drop rami of L2-S3 and provides sensory and motor branches to the lower extremity. The spatial orien- INTRODUCTION tation of the lumbar portion of the plexus above the pelvic brim leaves it particularly susceptible to in- The lumbosacral plexus is formed by the ventral trapartum injury by the fetal head. Such lesions are rami of the L2-S3 segments, with some contribu- subdivided into two groups: upper lumbar plexus tions from L1 and S4 segments. It gives rise to six (L1-L4) and lumbosacral trunk (L4-L5). Given the sensory nerves of the thigh and leg, and six major root levels involved, upper lumbar plexus lesions sensorimotor nerves responsible for innervating 43 produce symptoms suggestive of iliohypogastric, muscles of the lower extremity (Van Alfen and ilioinguinal, genitofemoral, femoral, and obturator Malessy, 2013). As the name would suggest, it neuropathies or L4 radiculopathies. Alternatively, consists of two components, the lumbar plexus involvement of the lumbosacral trunk can imitate a and the sacral plexus, which are spatially separat- common fibular (peroneal) neuropathy or L5 ed. This anatomical separation results in a clinical radiculopathy. This symptomatic overlap with vari- division of lumbosacral plexus lesions into those ous neuropathies and radiculopathies, makes di- affecting the lumbar plexus and those affecting the agnosis of such lesions particularly challenging. -

Cranial Nerves 9Th & 10Th
Cranial Nerves 9th & 10th Neuroanatomy block-Anatomy-Lecture 8 Editing file Objectives At the end of the lecture, students should be able to: ● Define the deep origin of both Glossopharyngeal and Vagus Nerves. ● Locate the exit of each nerve from the brain stem. ● Describe the course and distribution of each nerve . ● List the branches of both nerves. Color guide ● Only in boys slides in Green ● Only in girls slides in Purple ● important in Red ● Notes in Grey Glossopharyngeal (IX) 9th Cranial Nerve ● it's mixed nerve, a Sensory nerve with preganglionic parasympathetic and few motor fibers ● It has no real nucleus to itself. Instead it shares nuclei with VII (facial) and X (vagus). Superficial attachment Course ● It arises from the ventral aspect of the 1. It Passes forwards between medulla by a linear series of small Internal jugular vein and rootlets, in groove between olive and External carotid artery. inferior cerebellar peduncle. ● It leaves the cranial cavity by passing 2. Lies Deep to Styloid process. through the jugular foramen in company with the Vagus , and the Accessory 3. Passes between external and nerves and the Internal jugular vein. internal carotid arteries at the posterior border of Stylopharyngeus then lateral to it. 4. It reaches the pharynx by passing between middle and inferior constrictors, deep to Hyoglossus, where it breaks into terminal branches. 3 Glossopharyngeal (IX) 9th Cranial Nerve Ganglia & Communications ● Small with no branches. Superior Ganglion ● It is connected to the Superior Cervical sympathetic ganglion. ● Large and carries general sensations from pharynx, soft palate and tonsil. Inferior ● ganglion It is connected to Auricular Branch of Vagus. -

Clinical Presentations of Lumbar Disc Degeneration and Lumbosacral Nerve Lesions
Hindawi International Journal of Rheumatology Volume 2020, Article ID 2919625, 13 pages https://doi.org/10.1155/2020/2919625 Review Article Clinical Presentations of Lumbar Disc Degeneration and Lumbosacral Nerve Lesions Worku Abie Liyew Biomedical Science Department, School of Medicine, Debre Markos University, Debre Markos, Ethiopia Correspondence should be addressed to Worku Abie Liyew; [email protected] Received 25 April 2020; Revised 26 June 2020; Accepted 13 July 2020; Published 29 August 2020 Academic Editor: Bruce M. Rothschild Copyright © 2020 Worku Abie Liyew. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Lumbar disc degeneration is defined as the wear and tear of lumbar intervertebral disc, and it is mainly occurring at L3-L4 and L4-S1 vertebrae. Lumbar disc degeneration may lead to disc bulging, osteophytes, loss of disc space, and compression and irritation of the adjacent nerve root. Clinical presentations associated with lumbar disc degeneration and lumbosacral nerve lesion are discogenic pain, radical pain, muscular weakness, and cutaneous. Discogenic pain is usually felt in the lumbar region, or sometimes, it may feel in the buttocks, down to the upper thighs, and it is typically presented with sudden forced flexion and/or rotational moment. Radical pain, muscular weakness, and sensory defects associated with lumbosacral nerve lesions are distributed on -

Vagus Nerve (CN X) That Supply All of the Thoracic and Abdominal Viscera, Except the Descending and Sigmoid Colons and Other Pelvic Viscera
DR. HAYTHEM ALI ALSAYIGH Assistant prof. BOARD CLINICAL SURGICAL ANATOMY F.I.M.B.S.-MB.CH,B COLLEGE OF MEDICINE –UNIVERSITY OF BABYLON III. Autonomic Nervous System in the Thorax Is composed of motor, or efferent, nerves through which cardiac muscle, smooth muscle , and glands are innervated. Involves two neurons: preganglionic and postganglionic. It may include general visceral afferent (GVA) fibers because they run along with general visceral efferent (GVE) fibers . Consists of sympathetic (or thoracolumbar outflow) and parasympathetic (or craniosacral outflow)systems. Consists of cholinergic fibers (sympathetic preganglionic, parasympathetic preganglionic, and postganglionic) that use acetylcholine as the neurotransmitter and adrenergic fibers (sympathetic postganglionic) that use norepinephrine as the neurotransmitter (except those to sweat glands [cholinergic]). A. Sympathetic nervous system Enables the body to cope with crises or emergencies and thus often is referred to as the fight-or-flight division. Contains preganglionic cell bodies that are located in the lateral horn or intermediolateral cell column of the spinal cord segments between T1 and L2. Has preganglionic fibers that pass through the white rami communicantes and enter the sympathetic chain ganglion, where they synapse. Has postganglionic fibers that join each spinal nerve by way of the gray rami communicantes and supply the blood vessels, hair follicles (arrector pili muscles), and sweat glands. Increases the heart rate , dilates the bronchial lumen , and dilates the coronary arteries. 1. Sympathetic trunk Is composed primarily of ascending and descending preganglionic sympathetic fibers and visceral afferent fibers, and contains the cell bodies of the postganglionic sympathetic (GVE) fibers. Descends in front of the neck of the ribs and the posterior intercostal vessels. -

The Sympathetic and the Parasympathetic Nervous System
The sympathetic and the parasympathetic nervous system Zsuzsanna Tóth, PhD Institute of Anatomy, Histology and Embryology Semmelweis University The role of the autonomic nervous system Claude Bernard • „milieu intérieur” concept; every organism lives in its internal environment that is constant and independent form the external environment Walter Bradford Cannon homeostasis; • an extension of the “milieu interieur” concept • consistence in an open system requires mechanisms that act to maintain that consistency • steady-state conditions require that any tendency toward change automatically meets with factors that resist that change • regulating systems that determine the homeostatic state : o autonomic nervous system ( sympathetic, parasympathetic, enteral) o endocrine system General structure of the autonomic nervous system craniosacral thoracolumbar Anatomy Neurotransmittersof the gut autonomic nervous system. symp. gangl pregangl. fiber pregangl. postgangl. fiber fiber (PoR) PoR enteral ganglion PoR PoR smooth muscle smooth muscle Kuratani S Development 2009;136:1585-1589 Sympathetic activation: Fight or flight reaction • energy mobilization • preparation for escape, or fight vasoconstriction • generalized Parasympathetic activation: adrenal • energy saving and restoring • „rest and digest” system • more localized vasoconstriction Paravertebral ganglia and the sympathetic chains pars cervicalis superius ganglion medium cervicale stellatum pars vertebrae • from the base of the skull to the caudal end thoracalis thoracalis of the sacrum • paravertebral ganglia (ganglia trunci sympathici) • rami interganglionares pars vertebrae • the two chains fuses at the ganglion impar abdominalis lumbalis sacrum pars pelvina foramen sacralia anteriora ganglion impar Anatomy of the cervical part of the sympathetic trunk superior cervical ganglion • behind the seath of the carotid, fusiform ggl. cervicale superius • IML T1-3 vegetative motoneurons- preganglionic fibers truncus symp. -

Netter's Anatomy Flash Cards – Section 7 – List 4Th Edition
Netter's Anatomy Flash Cards – Section 7 – List 4th Edition https://www.memrise.com/course/1577594/ Section 7 Lower Limb (72 cards) Plate 7-1 Hip (Coxal) Bone: Lateral View 1.1 Posterior superior iliac spine 1.2 Posterior inferior iliac spine 1.3 Greater sciatic notch 1.4 Body of ilium 1.5 Body of ischium 1.6 Ischial tuberosity 1.7 Pubic tubercle 1.8 Acetabulum 1.9 Iliac crest Plate 7-2 Hip (Coxal) Bone: Medial View 2.1 Wing (ala) of ilium (iliac fossa) 2.2 Pecten pubis (pectineal line) 2.3 Ramus of ischium 2.4 Lesser sciatic notch 2.5 Ischial spine 2.6 Articular surface (for sacrum) 2.7 Iliac tuberosity Plate 7-3 Hip Joint: Lateral View 3.1 Lunate (articular) surface of acetabulum 3.2 Articular cartilage 3.3 Head of femur 3.4 Ligament of head of femur (cut) 3.5 Obturator membrane 3.6 Acetabular labrum (fibrocartilaginous) Plate 7-4 Hip Joint: Anterior and Posterior Views 4.1 Iliofemoral ligament (Y ligament of Bigelow) 4.2 Pubofemoral ligament 4.3 Iliofemoral ligament 4.4 Ischiofemoral ligament Plate 7-5 Femur 5.1 Greater trochanter 5.2 Shaft (body) 5.3 Lateral epicondyle 5.4 Lateral condyle 5.5 Medial condyle 5.6 Medial epicondyle 5.7 Adductor tubercle 5.8 Linea aspera (Medial lip; Lateral lip) 5.9 Lesser trochanter 5.10 Intertrochanteric crest 5.11 Neck 5.12 Head Plate 7-6 Tibia and Fibula 6.1 Lateral condyle 6.2 Apex, Head, and Neck of fibula 6.3 Fibula 6.4 Lateral malleolus 6.5 Medial malleolus 6.6 Tibia 6.7 Tibial tuberosity 6.8 Medial condyle 6.9 Superior articular surfaces (medial and lateral facets) 6.10 Malleolar fossa of lateral -

33. Spinal Nerves. Cervical Plexus
GUIDELINES Students’ independent work during preparation to practical lesson Academic discipline HUMAN ANATOMY Topic SPINAL NERVES. CERVICAL PLEXUS. 1. Relevance of the topic: The knowledge of structures of the peripheral nervous system, particularly cervical plexus and its branches is the base of clinical thinking in terms of differential diagnosis for the doctor of any specialty, but above all a neurologist, vertebroneurologist, traumatologist, dermatologist, general practitioner. 2. Specific objectives of practical lesson - Analyse the composition of fibres of anterior and posterior roots of spinal nerves. - Explain the formation of spinal nerve. - Suggest the definition of spinal nerve. - Classify spinal nerve branches. - Explain functional anatomy of thoracic spinal nerve branches. - Define term "plexus of somatic nerves" including the formation of cervical plexus. - Draw a scheme of spinal nerve: o а - in cervical region of spinal cord (except for the CVIII); o b - in thoracic region of spinal cord; o c - on the level of SII – SIV. - Analyse the connection of somatic nerve (thoracic spinal nerve) with ganglia of sympathetic trunk. - Create the conception of grey and white connecting branches in the functional aspect. 3. Basic level of preparation (interdisciplinary integration) of the student includes knowledge of medical biology and histology of the development of nervous system in phylogenesis and ontogenesis. Name of previous disciplines Obtained skills 1. Medical Biology and Histology Know ontogenesis and phylogenesis of nervous system. The structure of the neuron. 2. Sections of Human Anatomy: - osteology The student should have skills to describe the structure of - myology the spine in general, to be able to demonstrate structural features of the cervical vertebrae, their connections with each other and with the bones of the skull. -

Simple Ways to Dissect Ciliary Ganglion for Orbital Anatomical Education
OkajimasDetection Folia Anat. of ciliary Jpn., ganglion94(3): 119–124, for orbit November, anatomy 2017119 Simple ways to dissect ciliary ganglion for orbital anatomical education By Ming ZHOU, Ryoji SUZUKI, Hideo AKASHI, Akimitsu ISHIZAWA, Yoshinori KANATSU, Kodai FUNAKOSHI, Hiroshi ABE Department of Anatomy, Akita University Graduate School of Medicine, Akita, 010-8543 Japan –Received for Publication, September 21, 2017– Key Words: ciliary ganglion, orbit, human anatomy, anatomical education Summary: In the case of anatomical dissection as part of medical education, it is difficult for medical students to find the ciliary ganglion (CG) since it is small and located deeply in the orbit between the optic nerve and the lateral rectus muscle and embedded in the orbital fat. Here, we would like to introduce simple ways to find the CG by 1): tracing the sensory and parasympathetic roots to find the CG from the superior direction above the orbit, 2): transecting and retracting the lateral rectus muscle to visualize the CG from the lateral direction of the orbit, and 3): taking out whole orbital structures first and dissecting to observe the CG. The advantages and disadvantages of these methods are discussed from the standpoint of decreased laboratory time and students as beginners at orbital anatomy. Introduction dissection course for the first time and with limited time. In addition, there are few clear pictures in anatomical The ciliary ganglion (CG) is one of the four para- textbooks showing the morphology of the CG. There are sympathetic ganglia in the head and neck region located some scientific articles concerning how to visualize the behind the eyeball between the optic nerve and the lateral CG, but they are mostly based on the clinical approaches rectus muscle in the apex of the orbit (Siessere et al., rather than based on the anatomical procedure for medical 2008). -

Shoulder Anatomy & Clinical Exam
MSK Ultrasound - Spine - Incheon Terminal Orthopedic Private Clinic Yong-Hyun, Yoon C,T-spine Basic Advanced • Medial branch block • C-spine transforaminal block • Facet joint block • Thoracic paravertebral block • C-spine intra-discal injection • Superficial cervical plexus block • Vagus nerve block • Greater occipital nerve block(GON) • Third occipital nerve block(TON) • Hydrodissection • Brachial plexus(1st rib level) • Suboccipital nerve • Stellate ganglion block(SGB) • C1, C2 nerve root, C2 nerve • Brachial plexus block(interscalene) • Recurrent laryngeal nerve • Serratus anterior plane • Cervical nerve root Cervical facet joint Anatomy Diagnosis Cervical facet joint injection C-arm Ultrasound Cervical medial branch Anatomy Nerve innervation • Medial branch • Same level facet joint • Inferior level facet joint • Facet joint • Dual nerve innervation Cervical medial branch C-arm Ultrasound Cervical nerve root Anatomy Diagnosis • Motor • Sensory • Dermatome, myotome, fasciatome Cervical nerve root block C-arm Ultrasound Stallete ganglion block Anatomy Injection Vagus nerve Anatomy Injection L,S-spine Basic Advanced • Medial branch block • Lumbar sympathetic block • Facet joint block • Lumbar plexus block • Superior, inferior hypogastric nerve block • Caudal block • Transverse abdominal plane(TAP) block • Sacral plexus block • Epidural block • Hydrodissection • Interlaminal • Pudendal nerve • Transforaminal injection • Genitofemoral nerve • Superior, inferior cluneal nerve • Rectus abdominal sheath • Erector spinae plane Lumbar facet -

Anatomy of Spinal Nerves in the First Turkish Illustrated Anatomy Handwritten Textbook
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by DSpace@HKU Childs Nerv Syst DOI 10.1007/s00381-016-3136-9 COVER EDITORIAL Anatomy of spinal nerves in the first Turkish illustrated anatomy handwritten textbook Murat Çetkin1 & Mustafa Orhan1 & İlhan Bahşi1 & Begümhan Turhan2 Received: 26 May 2016 /Accepted: 30 May 2016 # Springer-Verlag Berlin Heidelberg 2016 BTeşrih-ül Ebdan ve Tercümânı Kıbale-i Feylesûfan^ is the the book, İtâḳî acknowledges the contributions of the Grand first handwritten anatomy textbook with illustrations written Vizier [4, 7]. in Turkish in 17th century by Şemseddîn-i İtâḳî. BTeşrih^ has Not many textbooks about anatomy existed in the Islamic different meanings such as anatomy, skeleton, and cutting a World and the Ottoman Empire until İtâḳî’sbook[9]. In other corpse into pieces [1]. BTeşrih-ül Ebdan ve Tercümânı Kıbale- medical textbooks, anatomy occupies only a few pages in i Feylesûfan ^ means dissection of the body and scholars’ different sections [4]. İtâḳî’s book is a pioneer in its area as birth knowledge [2]. Since this is the first handwritten text- it is written in Turkish, and it is supported with illustrations book in Turkish, it has great importance in the development of [4]. In addition to Turkish, the book contains mostly Arabic medicine in Ottoman Empire. This book was written while and rarely Persian terms as well [4, 6, 7]. Some editions of this Grand Vizier Recep Pasha was in power, and it was dedicated book which was written in the 17th century were reprinted in to the Sultan of that period, Murat the IVth [3, 4]. -
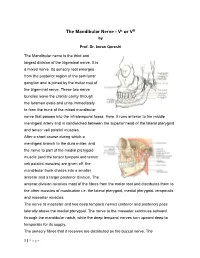
The Mandibular Nerve - Vc Or VIII by Prof
The Mandibular Nerve - Vc or VIII by Prof. Dr. Imran Qureshi The Mandibular nerve is the third and largest division of the trigeminal nerve. It is a mixed nerve. Its sensory root emerges from the posterior region of the semilunar ganglion and is joined by the motor root of the trigeminal nerve. These two nerve bundles leave the cranial cavity through the foramen ovale and unite immediately to form the trunk of the mixed mandibular nerve that passes into the infratemporal fossa. Here, it runs anterior to the middle meningeal artery and is sandwiched between the superior head of the lateral pterygoid and tensor veli palatini muscles. After a short course during which a meningeal branch to the dura mater, and the nerve to part of the medial pterygoid muscle (and the tensor tympani and tensor veli palatini muscles) are given off, the mandibular trunk divides into a smaller anterior and a larger posterior division. The anterior division receives most of the fibres from the motor root and distributes them to the other muscles of mastication i.e. the lateral pterygoid, medial pterygoid, temporalis and masseter muscles. The nerve to masseter and two deep temporal nerves (anterior and posterior) pass laterally above the medial pterygoid. The nerve to the masseter continues outward through the mandibular notch, while the deep temporal nerves turn upward deep to temporalis for its supply. The sensory fibres that it receives are distributed as the buccal nerve. The 1 | P a g e buccal nerve passes between the medial and lateral pterygoids and passes downward and forward to emerge from under cover of the masseter with the buccal artery. -

Association of Arrhythmia in Patients with Cervical Spondylosis: a Nationwide Population-Based Cohort Study
Journal of Clinical Medicine Article Association of Arrhythmia in Patients with Cervical Spondylosis: A Nationwide Population-Based Cohort Study Shih-Yi Lin 1,2, Wu-Huei Hsu 1,3, Cheng-Chieh Lin 1,4, Cheng-Li Lin 5,6, Chun-Hao Tsai 1,7, Chih-Hsueh Lin 1,4, Der-Cherng Chen 7, Tsung-Chih Lin 8, Chung-Y. Hsu 1 and Chia-Hung Kao 1,9,10,* ID 1 Graduate Institute of Biomedical Sciences and School of Medicine, College of Medicine, China Medical University, No. 2, Yuh-Der Road, Taichung 404, Taiwan; [email protected] (S.-Y.L.); [email protected] (W.-H.H.); [email protected] (C.-C.L.); [email protected] (C.-H.T.); [email protected] (C.-H.L.); [email protected] (C.-Y.H.) 2 Division of Nephrology and Kidney Institute, China Medical University Hospital, Taichung 404, Taiwan 3 Division of Pulmonary and Critical Care Medicine, China Medical University Hospital and China Medical University, Taichung 404, Taiwan 4 Department of Family Medicine, China Medical University Hospital, Taichung 404, Taiwan 5 Management Office for Health Data, China Medical University Hospital, Taichung 404, Taiwan; [email protected] 6 College of Medicine, China Medical University, Taichung 404, Taiwan 7 Department of Orthopedics, China Medical University Hospital, Taichung 404, Taiwan; [email protected] 8 Department of Orthopedics, St. Martin De Porres Hospital, Chiayi 600, Taiwan; [email protected] 9 Department of Nuclear Medicine, China Medical University Hospital, Taichung 404, Taiwan 10 Department of Bioinformatics and Medical Engineering, Asia University, Taichung 413, Taiwan * Correspondence: [email protected]; Tel.: +886-4-2205-2121 (ext.