Shigellosis Outbreak Associated with an Unchlorinated Fill-And-Drain
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Distribution of Tick-Borne Diseases in China Xian-Bo Wu1, Ren-Hua Na2, Shan-Shan Wei2, Jin-Song Zhu3 and Hong-Juan Peng2*
Wu et al. Parasites & Vectors 2013, 6:119 http://www.parasitesandvectors.com/content/6/1/119 REVIEW Open Access Distribution of tick-borne diseases in China Xian-Bo Wu1, Ren-Hua Na2, Shan-Shan Wei2, Jin-Song Zhu3 and Hong-Juan Peng2* Abstract As an important contributor to vector-borne diseases in China, in recent years, tick-borne diseases have attracted much attention because of their increasing incidence and consequent significant harm to livestock and human health. The most commonly observed human tick-borne diseases in China include Lyme borreliosis (known as Lyme disease in China), tick-borne encephalitis (known as Forest encephalitis in China), Crimean-Congo hemorrhagic fever (known as Xinjiang hemorrhagic fever in China), Q-fever, tularemia and North-Asia tick-borne spotted fever. In recent years, some emerging tick-borne diseases, such as human monocytic ehrlichiosis, human granulocytic anaplasmosis, and a novel bunyavirus infection, have been reported frequently in China. Other tick-borne diseases that are not as frequently reported in China include Colorado fever, oriental spotted fever and piroplasmosis. Detailed information regarding the history, characteristics, and current epidemic status of these human tick-borne diseases in China will be reviewed in this paper. It is clear that greater efforts in government management and research are required for the prevention, control, diagnosis, and treatment of tick-borne diseases, as well as for the control of ticks, in order to decrease the tick-borne disease burden in China. Keywords: Ticks, Tick-borne diseases, Epidemic, China Review (Table 1) [2,4]. Continuous reports of emerging tick-borne Ticks can carry and transmit viruses, bacteria, rickettsia, disease cases in Shandong, Henan, Hebei, Anhui, and spirochetes, protozoans, Chlamydia, Mycoplasma,Bartonia other provinces demonstrate the rise of these diseases bodies, and nematodes [1,2]. -

Recognizing and Treating New and Emerging Infections Encountered in Everyday Practice
Recognizing and treating new and emerging infections encountered in everyday practice STEVEN M. GORDON, MD NFECTIOUS DISEASES, pre- MiikWirj:« Although infectious diseases were once considered a dicted earlier in this cen- diminishing threat, new pathogens are constantly challenging tury to be eliminated as a the health care system. This article reviews the clinical presen- public health problem, re- tation, diagnosis, and treatment of seven emerging infections I main the chief cause of death that primary care physicians are likely to encounter. worldwide and a significant cause of death and morbidity in i Parvovirus B19 attacks erythrocyte precursors; the United States.1 Challenging infection is usually benign and self-limiting but can cause the US public health system are aplastic crises in patients with chronic hemolytic disorders. several newly identified patho- Hemorrhagic colitis due to Escherichia coli 0157:H7 infection gens (eg, human immunodefi- can lead to the hemolytic-uremic syndrome, especially in chil- ciency virus [HIV], Escherichia dren; it also can cause thrombotic thrombocytopenia purpura. coli 0157:H7, hepatitis C) and a Chlamydia pneumoniae causes a mild pneumonia that resem- resurgence of old diseases pre- bles mycoplasmal pneumonia. Bacillary angiomatosis primar- sumed to be under control (eg, ily affects immunocompromised patients, especially those tuberculosis, syphilis). Further, infected with human immunodeficiency virus (HIV). At least multiple-drug resistance in two organisms can cause bacillary angiomatosis: Bartonella hense- strains of pneumococci, gono- lae and Bartonella quintana. Hantavirus pulmonary syndrome cocci, enterococci, staphylo- is spread by exposure to the droppings of infected rodents. cocci, salmonella, and mycobac- Contrary to previous thought, HIV continues to replicate teria undermines efforts to throughout the course of the illness and does not have a latency control the diseases they cause.2 phase. -

Q Fever in Small Ruminants and Its Public Health Importance
Journal of Dairy & Veterinary Sciences ISSN: 2573-2196 Review Article Dairy and Vet Sci J Volume 9 Issue 1 - January 2019 Copyright © All rights are reserved by Tolera Tagesu Tucho DOI: 10.19080/JDVS.2019.09.555752 Q Fever in Small Ruminants and its Public Health Importance Tolera Tagesu* School of Veterinary Medicine, Jimma University, Ethiopia Submission: December 01, 2018; Published: January 11, 2019 *Corresponding author: Tolera Tagesu Tucho, School of Veterinary Medicine, Jimma University, Jimma Oromia, Ethiopia Abstract Query fever is caused by Coxiella burnetii, it’s a worldwide zoonotic infectious disease where domestic small ruminants are the main reservoirs for human infections. Coxiella burnetii, is a Gram-negative obligate intracellular bacterium, adapted to thrive within the phagolysosome of the phagocyte. Humans become infected primarily by inhaling aerosols that are contaminated with C. burnetii. Ingestion (particularly drinking raw milk) and person-to-person transmission are minor routes. Animals shed the bacterium in urine and feces, and in very high concentrations in birth by-products. The bacterium persists in the environment in a resistant spore-like form which may become airborne and transported long distances by the wind. It is considered primarily as occupational disease of workers in close contact with farm animals or processing their be commenced immediately whenever Q fever is suspected. To prevent both the introduction and spread of Q fever infection, preventive measures shouldproducts, be however,implemented it may including occur also immunization in persons without with currently direct contact. available Doxycycline vaccines drugof domestic is the first small line ruminant of treatment animals for Q and fever. -

Coxiella Burnetii
SENTINEL LEVEL CLINICAL LABORATORY GUIDELINES FOR SUSPECTED AGENTS OF BIOTERRORISM AND EMERGING INFECTIOUS DISEASES Coxiella burnetii American Society for Microbiology (ASM) Revised March 2016 For latest revision, see web site below: https://www.asm.org/Articles/Policy/Laboratory-Response-Network-LRN-Sentinel-Level-C ASM Subject Matter Expert: David Welch, Ph.D. Medical Microbiology Consulting Dallas, TX [email protected] ASM Sentinel Laboratory Protocol Working Group APHL Advisory Committee Vickie Baselski, Ph.D. Barbara Robinson-Dunn, Ph.D. Patricia Blevins, MPH University of Tennessee at Department of Clinical San Antonio Metro Health Memphis Pathology District Laboratory Memphis, TN Beaumont Health System [email protected] [email protected] Royal Oak, MI BRobinson- Erin Bowles David Craft, Ph.D. [email protected] Wisconsin State Laboratory of Penn State Milton S. Hershey Hygiene Medical Center Michael A. Saubolle, Ph.D. [email protected] Hershey, PA Banner Health System [email protected] Phoenix, AZ Christopher Chadwick, MS [email protected] Association of Public Health Peter H. Gilligan, Ph.D. m Laboratories University of North Carolina [email protected] Hospitals/ Susan L. Shiflett Clinical Microbiology and Michigan Department of Mary DeMartino, BS, Immunology Labs Community Health MT(ASCP)SM Chapel Hill, NC Lansing, MI State Hygienic Laboratory at the [email protected] [email protected] University of Iowa [email protected] Larry Gray, Ph.D. Alice Weissfeld, Ph.D. TriHealth Laboratories and Microbiology Specialists Inc. Harvey Holmes, PhD University of Cincinnati College Houston, TX Centers for Disease Control and of Medicine [email protected] Prevention Cincinnati, OH om [email protected] [email protected] David Welch, Ph.D. -

Antibiotic Resistance in the European Union Associated with Therapeutic Use of Veterinary Medicines
The European Agency for the Evaluation of Medicinal Products Veterinary Medicines Evaluation Unit EMEA/CVMP/342/99-Final Antibiotic Resistance in the European Union Associated with Therapeutic use of Veterinary Medicines Report and Qualitative Risk Assessment by the Committee for Veterinary Medicinal Products 14 July 1999 Public 7 Westferry Circus, Canary Wharf, London, E14 4HB, UK Switchboard: (+44-171) 418 8400 Fax: (+44-171) 418 8447 E_Mail: [email protected] http://www.eudra.org/emea.html ãEMEA 1999 Reproduction and/or distribution of this document is authorised for non commercial purposes only provided the EMEA is acknowledged TABLE OF CONTENTS Page 1. INTRODUCTION 1 1.1 DEFINITION OF ANTIBIOTICS 1 1.1.1 Natural antibiotics 1 1.1.2 Semi-synthetic antibiotics 1 1.1.3 Synthetic antibiotics 1 1.1.4 Mechanisms of Action 1 1.2 BACKGROUND AND HISTORY 3 1.2.1 Recent developments 3 1.2.2 Authorisation of Antibiotics in the EU 4 1.3 ANTIBIOTIC RESISTANCE 6 1.3.1 Microbiological resistance 6 1.3.2 Clinical resistance 6 1.3.3 Resistance distribution in bacterial populations 6 1.4 GENETICS OF RESISTANCE 7 1.4.1 Chromosomal resistance 8 1.4.2 Transferable resistance 8 1.4.2.1 Plasmids 8 1.4.2.2 Transposons 9 1.4.2.3 Integrons and gene cassettes 9 1.4.3 Mechanisms for inter-bacterial transfer of resistance 10 1.5 METHODS OF DETERMINATION OF RESISTANCE 11 1.5.1 Agar/Broth Dilution Methods 11 1.5.2 Interpretative criteria (breakpoints) 11 1.5.3 Agar Diffusion Method 11 1.5.4 Other Tests 12 1.5.5 Molecular techniques 12 1.6 MULTIPLE-DRUG RESISTANCE -
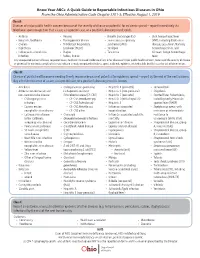
Know Your Abcs: a Quick Guide to Reportable Infectious Diseases in Ohio
Know Your ABCs: A Quick Guide to Reportable Infectious Diseases in Ohio From the Ohio Administrative Code Chapter 3701-3; Effective August 1, 2019 Class A: Diseases of major public health concern because of the severity of disease or potential for epidemic spread – report immediately via telephone upon recognition that a case, a suspected case, or a positive laboratory result exists. • Anthrax • Measles • Rubella (not congenital) • Viral hemorrhagic fever • Botulism, foodborne • Meningococcal disease • Severe acute respiratory (VHF), including Ebola virus • Cholera • Middle East Respiratory syndrome (SARS) disease, Lassa fever, Marburg • Diphtheria Syndrome (MERS) • Smallpox hemorrhagic fever, and • Influenza A – novel virus • Plague • Tularemia Crimean-Congo hemorrhagic infection • Rabies, human fever Any unexpected pattern of cases, suspected cases, deaths or increased incidence of any other disease of major public health concern, because of the severity of disease or potential for epidemic spread, which may indicate a newly recognized infectious agent, outbreak, epidemic, related public health hazard or act of bioterrorism. Class B: Disease of public health concern needing timely response because of potential for epidemic spread – report by the end of the next business day after the existence of a case, a suspected case, or a positive laboratory result is known. • Amebiasis • Carbapenemase-producing • Hepatitis B (perinatal) • Salmonellosis • Arboviral neuroinvasive and carbapenem-resistant • Hepatitis C (non-perinatal) • Shigellosis -

Tick-Borne Diseases in Maine a Physician’S Reference Manual Deer Tick Dog Tick Lonestar Tick (CDC Photo)
tick-borne diseases in Maine A Physician’s Reference Manual Deer Tick Dog Tick Lonestar Tick (CDC PHOTO) Nymph Nymph Nymph Adult Male Adult Male Adult Male Adult Female Adult Female Adult Female images not to scale know your ticks Ticks are generally found in brushy or wooded areas, near the DEER TICK DOG TICK LONESTAR TICK Ixodes scapularis Dermacentor variabilis Amblyomma americanum ground; they cannot jump or fly. Ticks are attracted to a variety (also called blacklegged tick) (also called wood tick) of host factors including body heat and carbon dioxide. They will Diseases Diseases Diseases transfer to a potential host when one brushes directly against Lyme disease, Rocky Mountain spotted Ehrlichiosis anaplasmosis, babesiosis fever and tularemia them and then seek a site for attachment. What bites What bites What bites Nymph and adult females Nymph and adult females Adult females When When When April through September in Anytime temperatures are April through August New England, year-round in above freezing, greatest Southern U.S. Coloring risk is spring through fall Adult females have a dark Coloring Coloring brown body with whitish Adult females have a brown Adult females have a markings on its hood body with a white spot on reddish-brown tear shaped the hood Size: body with dark brown hood Unfed Adults: Size: Size: Watermelon seed Nymphs: Poppy seed Nymphs: Poppy seed Unfed Adults: Sesame seed Unfed Adults: Sesame seed suMMer fever algorithM ALGORITHM FOR DIFFERENTIATING TICK-BORNE DISEASES IN MAINE Patient resides, works, or recreates in an area likely to have ticks and is exhibiting fever, This algorithm is intended for use as a general guide when pursuing a diagnosis. -

Communicable Diseases Weekly Report
Communicable Diseases Weekly Report Week 08, 21 February to 27 February 2021 In summary, we report: • Chancroid – one new case in a returned traveller • Rodent-borne disease risks • Novel coronavirus 2019 (COVID-19) • Summary of notifiable conditions activity in NSW For further information see NSW Health infectious diseases page. This includes links to other NSW Health infectious disease surveillance reports and a diseases data page for a range of notifiable infectious diseases. Chancroid One case of chancroid was notified this reporting week in a traveller returning from overseas. Chancroid is an acute sexually transmitted bacterial infection that causes painful genital ulcers. The condition is now rarely seen in Australia and only one other case has been notified in NSW during the past decade. Although the incidence of chancroid is decreasing globally, it is still reported in some regions within Africa, Asia, the Caribbean and South Pacific. Chancroid genital ulcer disease is a known risk factor for the transmission of HIV. The bacterium that causes chancroid, Haemophilus ducreyi, is usually transmitted through anal, oral, or vaginal sex with an infected person. After infection, one or more ulcers (sores) develop on the genitals or around the anus. Non-genital skin infections have also been reported globally, through non-sexual skin-to-skin contact with an infected person. The ulcers are usually painful, but rarely can be asymptomatic. Swelling in the groin (due to enlarged painful lymph nodes that can liquify and develop into buboes) can also occur. Other symptoms may include pain during sexual intercourse or while urinating. An infected person can spread the infection from their genital region to other parts of their body. -

Zoonotic Diseases Fact Sheet
ZOONOTIC DISEASES FACT SHEET s e ion ecie s n t n p is ms n e e s tio s g s m to a a o u t Rang s p t tme to e th n s n m c a s a ra y a re ho Di P Ge Ho T S Incub F T P Brucella (B. Infected animals Skin or mucous membrane High and protracted (extended) fever. 1-15 weeks Most commonly Antibiotic melitensis, B. (swine, cattle, goats, contact with infected Infection affects bone, heart, reported U.S. combination: abortus, B. suis, B. sheep, dogs) animals, their blood, tissue, gallbladder, kidney, spleen, and laboratory-associated streptomycina, Brucellosis* Bacteria canis ) and other body fluids causes highly disseminated lesions bacterial infection in tetracycline, and and abscess man sulfonamides Salmonella (S. Domestic (dogs, cats, Direct contact as well as Mild gastroenteritiis (diarrhea) to high 6 hours to 3 Fatality rate of 5-10% Antibiotic cholera-suis, S. monkeys, rodents, indirect consumption fever, severe headache, and spleen days combination: enteriditis, S. labor-atory rodents, (eggs, food vehicles using enlargement. May lead to focal chloramphenicol, typhymurium, S. rep-tiles [especially eggs, etc.). Human to infection in any organ or tissue of the neomycin, ampicillin Salmonellosis Bacteria typhi) turtles], chickens and human transmission also body) fish) and herd animals possible (cattle, chickens, pigs) All Shigella species Captive non-human Oral-fecal route Ranges from asymptomatic carrier to Varies by Highly infective. Low Intravenous fluids primates severe bacillary dysentery with high species. 16 number of organisms and electrolytes, fevers, weakness, severe abdominal hours to 7 capable of causing Antibiotics: ampicillin, cramps, prostration, edema of the days. -

Bartonella Henselae and Coxiella Burnetii Infection and the Kawasaki Disease
GALLEY PROOF J. Appl. Sci. Environ. Mgt. 2004 JASEM ISSN 1119-8362 Available Online at All rights reserved http:// www.bioline.org.br/ja Vol. 8 (1) 11 - 12 Bartonella henselae and Coxiella burnetii Infection and the Kawasaki Disease KEI NUMAZAKI, M D Department of Pediatrics, Sapporo Medical University School of Medicine, S.1 W.16 Chuo-ku Sapporo, 060-8543 Japan Phone: +81-611-2111 X3413 Fax: +81-611-0352 E-mail: [email protected] ABSTRACT: It was reported that Bartonella henselae, B. quintana and Coxiella burnetii was not strongly associated with coronary artery disease but on the basis of geometric mean titer, C. burnetii infection might have a modest association with coronary artery disease. Serum antibodies to B. henselae from 14 patients with acute phase of Kawasaki disease were determined by the indirect fluorescence antibody assay . Serum antibodies to C. burnetii were also tried to detect. However, no positive results were obtained. I also examined 10 children and 10 pregnant women who had serum IgG antibody to B. henselae or to C. burnetii. No one showed abnormal findings of coronary artery. @JASEM Several Bartonella species cause illness and associated with several infections, including asymptotic infection in humans. B. henselae has Chlamydia pneumoniae, cytomegalovirus, been associated with an increasing spectrum of Helicobacter pylori and other intercellular bacteria clinical syndromes including cat scratch disease. (Danesh et al., 1997). Previous studies supported Although the clinical spectrum has not been the possibility of certain populations having an completely clarified, B. quintana may cause association of infections and coronary artery disease blood-culture negative endocarditis in children Kawasaki disease (KD). -

Screening of Pharmaceuticals in San Francisco Bay Wastewater
Screening of Pharmaceuticals in San Francisco Bay Wastewater Prepared by Diana Lin Rebecca Sutton Jennifer Sun John Ross San Francisco Estuary Institute CONTRIBUTION NO. 910 / October 2018 Pharmaceuticals in Wastewater Technical Report Executive Summary Previous studies have shown that pharmaceuticals are widely detected in San Francisco Bay, and some compounds occasionally approach levels of concern for wildlife. In 2016 and 2017, seven wastewater treatment facilities located throughout the Bay Area voluntarily collected wastewater samples and funded analyses for 104 pharmaceutical compounds. This dataset represents the most comprehensive analysis of pharmaceuticals in wastewater to date in this region. On behalf of the Regional Monitoring Program for Water Quality in San Francisco Bay (RMP), the complete dataset was reviewed utilizing RMP quality assurance methods. An analysis of influent and effluent information is summarized in this report, and is intended to inform future monitoring recommendations for the Bay. Influent and effluent concentration ranges measured were generally within the same order of magnitude as other US studies, with a few exceptions for effluent. Effluent concentrations were generally significantly lower than influent concentrations, though estimated removal efficiency varied by pharmaceutical, and in some cases, by treatment type. These removal efficiencies were generally consistent with those reported in other studies in the US. Pharmaceuticals detected at the highest concentrations and with the highest frequencies in effluent were commonly used drugs, including treatments for diabetes and high blood pressure, antibiotics, diuretics, and anticonvulsants. For pharmaceuticals detected in discharged effluent, screening exercises were conducted to determine which might be appropriate candidates for further examination and potential monitoring in the Bay. -

Fluoroquinolones in the Management of Acute Lower Respiratory Infection
Thorax 2000;55:83–85 83 Occasional review Thorax: first published as 10.1136/thorax.55.1.83 on 1 January 2000. Downloaded from The next generation: fluoroquinolones in the management of acute lower respiratory infection in adults Peter J Moss, Roger G Finch Lower respiratory tract infections (LRTI) are ing for up to 40% of isolates in Spain19 and 33% the leading infectious cause of death in most in the United States.20 In England and Wales developed countries; community acquired the prevalence is lower; in the first quarter of pneumonia (CAP) and acute exacerbations of 1999 6.5% of blood/cerebrospinal fluid isolates chronic bronchitis (AECB) are responsible for were reported to the Public Health Laboratory the bulk of the adult morbidity. Until recently Service as showing intermediate sensitivity or quinolone antibiotics were not recommended resistance (D Livermore, personal communi- for the routine treatment of these infections.1–3 cation). Pneumococcal resistance to penicillin Neither ciprofloxacin nor ofloxacin have ad- is not specifically linked to quinolone resist- equate activity against Streptococcus pneumoniae ance and, in general, penicillin resistant in vitro, and life threatening invasive pneumo- pneumococci are sensitive to the newer coccal disease has been reported in patients fluoroquinolones.11 21 treated for respiratory tract infections with Resistance to ciprofloxacin develops rela- these drugs.4–6 The development of new fluoro- tively easily in both S pneumoniae and H influ- quinolone agents with increased activity enzae, requiring only a single mutation in the against Gram positive organisms, combined parC gene.22 23 Other quinolones such as with concerns about increasing microbial sparfloxacin and clinafloxacin require two resistance to â-lactam agents, has prompted a mutations in the parC and gyrA genes.11 23 re-evaluation of the use of quinolones in LRTI.