Glioblastoma & Anaplastic Astrocytoma
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Neurofibromatosis Type 2 (NF2)
International Journal of Molecular Sciences Review Neurofibromatosis Type 2 (NF2) and the Implications for Vestibular Schwannoma and Meningioma Pathogenesis Suha Bachir 1,† , Sanjit Shah 2,† , Scott Shapiro 3,†, Abigail Koehler 4, Abdelkader Mahammedi 5 , Ravi N. Samy 3, Mario Zuccarello 2, Elizabeth Schorry 1 and Soma Sengupta 4,* 1 Department of Genetics, Cincinnati Children’s Hospital, Cincinnati, OH 45229, USA; [email protected] (S.B.); [email protected] (E.S.) 2 Department of Neurosurgery, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] (S.S.); [email protected] (M.Z.) 3 Department of Otolaryngology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] (S.S.); [email protected] (R.N.S.) 4 Department of Neurology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] 5 Department of Radiology, University of Cincinnati, Cincinnati, OH 45267, USA; [email protected] * Correspondence: [email protected] † These authors contributed equally. Abstract: Patients diagnosed with neurofibromatosis type 2 (NF2) are extremely likely to develop meningiomas, in addition to vestibular schwannomas. Meningiomas are a common primary brain tumor; many NF2 patients suffer from multiple meningiomas. In NF2, patients have mutations in the NF2 gene, specifically with loss of function in a tumor-suppressor protein that has a number of synonymous names, including: Merlin, Neurofibromin 2, and schwannomin. Merlin is a 70 kDa protein that has 10 different isoforms. The Hippo Tumor Suppressor pathway is regulated upstream by Merlin. This pathway is critical in regulating cell proliferation and apoptosis, characteristics that are important for tumor progression. -

Pathologic and Molecular Aspects of Anaplasia in Circumscribed Gliomas and Glioneuronal Tumors
Brain Tumor Pathology (2019) 36:40–51 https://doi.org/10.1007/s10014-019-00336-z REVIEW ARTICLE Pathologic and molecular aspects of anaplasia in circumscribed gliomas and glioneuronal tumors Elisabet Pujadas1 · Liam Chen1,2 · Fausto J. Rodriguez1,3 Received: 6 February 2019 / Accepted: 28 February 2019 / Published online: 11 March 2019 © The Japan Society of Brain Tumor Pathology 2019 Abstract Many breakthroughs have been made in the past decade regarding our knowledge of the biological basis of the diffuse glio- mas, the most common primary central nervous system (CNS) tumors. These tumors as a group are aggressive, associated with high mortality, and have a predilection for adults. However, a subset of CNS glial and glioneuronal tumors are char- acterized by a more circumscribed pattern of growth and occur more commonly in children and young adults. They tend to be indolent, but our understanding of anaplastic changes in these tumors continues to improve as diagnostic classifications evolve in the era of molecular pathology and more integrated and easily accessible clinical databases. The presence of ana- plasia in pleomorphic xanthoastrocytomas and gangliogliomas is assigned a WHO grade III under the current classification, while the significance of anaplasia in pilocytic astrocytomas remains controversial. Recent data highlight the association of the latter with aggressive clinical behavior, as well as the presence of molecular genetic features of both pilocytic and dif- fuse gliomas, with the recognition that the precise terminology remains to be defined. We review the current concepts and advances regarding histopathology and molecular understanding of pilocytic astrocytomas, pleomorphic xanthoastrocytomas, and gangliogliomas, with a focus on their anaplastic counterparts. -

Risk Factors for Gliomas and Meningiomas in Males in Los Angeles County1
[CANCER RESEARCH 49, 6137-6143. November 1, 1989] Risk Factors for Gliomas and Meningiomas in Males in Los Angeles County1 Susan Preston-Martin,2 Wendy Mack, and Brian E. Henderson Department of Preventive Medicine, University of Southern California School of Medicine, Los Angeles, California 90033 ABSTRACT views with proxy respondents, we were unable to include a large proportion of otherwise eligible cases because they were deceased or Detailed job histories and information about other suspected risk were too ill or impaired to participate in an interview. The Los Angeles factors were obtained during interviews with 272 men aged 25-69 with a County Cancer Surveillance Program identified the cases (26). All primary brain tumor first diagnosed during 1980-1984 and with 272 diagnoses had been microscopically confirmed. individually matched neighbor controls. Separate analyses were con A total of 478 patients were identified. The hospital and attending ducted for the 202 glioma pairs and the 70 meningioma pairs. Meningi- physician granted us permission to contact 396 (83%) patients. We oma, but not glioma, was related to having a serious head injury 20 or were unable to locate 22 patients, 38 chose not to participate, and 60 more years before diagnosis (odds ratio (OR) = 2.3; 95% confidence were aphasie or too ill to complete the interview. We interviewed 277 interval (CI) = 1.1-5.4), and a clear dose-response effect was observed patients (74% of the 374 patients contacted about the study or 58% of relating meningioma risk to number of serious head injuries (/' for trend the initial 478 patients). -

Central Nervous System Tumors General ~1% of Tumors in Adults, but ~25% of Malignancies in Children (Only 2Nd to Leukemia)
Last updated: 3/4/2021 Prepared by Kurt Schaberg Central Nervous System Tumors General ~1% of tumors in adults, but ~25% of malignancies in children (only 2nd to leukemia). Significant increase in incidence in primary brain tumors in elderly. Metastases to the brain far outnumber primary CNS tumors→ multiple cerebral tumors. One can develop a very good DDX by just location, age, and imaging. Differential Diagnosis by clinical information: Location Pediatric/Young Adult Older Adult Cerebral/ Ganglioglioma, DNET, PXA, Glioblastoma Multiforme (GBM) Supratentorial Ependymoma, AT/RT Infiltrating Astrocytoma (grades II-III), CNS Embryonal Neoplasms Oligodendroglioma, Metastases, Lymphoma, Infection Cerebellar/ PA, Medulloblastoma, Ependymoma, Metastases, Hemangioblastoma, Infratentorial/ Choroid plexus papilloma, AT/RT Choroid plexus papilloma, Subependymoma Fourth ventricle Brainstem PA, DMG Astrocytoma, Glioblastoma, DMG, Metastases Spinal cord Ependymoma, PA, DMG, MPE, Drop Ependymoma, Astrocytoma, DMG, MPE (filum), (intramedullary) metastases Paraganglioma (filum), Spinal cord Meningioma, Schwannoma, Schwannoma, Meningioma, (extramedullary) Metastases, Melanocytoma/melanoma Melanocytoma/melanoma, MPNST Spinal cord Bone tumor, Meningioma, Abscess, Herniated disk, Lymphoma, Abscess, (extradural) Vascular malformation, Metastases, Extra-axial/Dural/ Leukemia/lymphoma, Ewing Sarcoma, Meningioma, SFT, Metastases, Lymphoma, Leptomeningeal Rhabdomyosarcoma, Disseminated medulloblastoma, DLGNT, Sellar/infundibular Pituitary adenoma, Pituitary adenoma, -

SOMATIC MUTATIONS AS a FACTOR in the PRODUC- TION of CANCER for Nearly Thirty Years the Phenomenon Known by Von Hanse- Mann's
SOMATIC MUTATIONS AS A FACTOR IN THE PRODUC- TION OF CANCER A CRITICAL REVIEW OF v. HANSEMANN’S THEORY OF ANAPLASIA IN THE LIGHT OF MODERN KNOWLEDGE OF GENETICS R. C. WHITMAN From the Henry S. Denison Research Laboratories of the University of Colorado, Received for publication, March 4, 1918 For nearly thirty years the phenomenon known by von Hanse- mann’s term, anaplasia, has been widely used among patholog- ists to describe and exphin the origin of cancer cells. Any well established facts, therefore, which throw added light upon the nature of the process of anaplasia itself and any possible relation it may have to cancer genesis must be important and significant. The term anaplasia has been, however, so loosely used that it will be worth while to review at length von Hansemann’s theory in order that we may start with a clear conception of what the word really means. The pleomorphism of cancer cells and the irregular, atypical mitoses so characteristic of their nuclei had been observed and carefully studied since the middle of the nine- teenth century. Arnold (Virch. Arch., vol. 79, cited by von Hansemann (l)),observing irregularities in the mitotic process itself, had inferred that thesemight be of fundamental significance. A voluminous literature dealing with the mitoses in cancer cells and other forms of rapidly proliferating tissues had already ac- cumulated when von Hansemann (1) undertook a further inves- tigation in the same field. In a carcinoma of the larynx he found besides a great abundance of normal mitotic figures, large numbers of tripolar and multipolar divisions and other departures from the normal type already observed and described by earlier writers; and in addition many hyperchromatic and hypochromatic mitoses, the hypochromatism consisting not merely in a reduction of the amount of chromatin in the chromosoines but rather in an 181 182 R. -

Cerebellar Anaplastic Astrocytoma in Adult Patients: 15 Consecutive Cases from a Single Institution and Literature Review
medRxiv preprint doi: https://doi.org/10.1101/2020.09.09.20188938; this version posted September 14, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted medRxiv a license to display the preprint in perpetuity. All rights reserved. No reuse allowed without permission. Cerebellar anaplastic astrocytoma in adult patients: 15 consecutive cases from a single institution and literature review Artem Belyaev1, Dmitry Usachev1, Marina Ryzhova1, Gleb Gulida1, Vasilisa Skvortsova2,3, Igor Pronin1, Grigory Kobiakov1. 1 Burdenko Neurosurgery Center, 4th Tverskaya-Yamskaya, 16, Moscow, 125047, Russia 2 Wellcome Trust Centre for Neuroimaging, University College London, London, United Kingdom; 3 Max Planck University College London Centre for Computational Psychiatry and Ageing Research, London, United Kingdom; Abstract: Adult cerebellar anaplastic astrocytomas (cAA) are rare entities and their clinical and genetic appearances are still ill defined. Previously, malignant gliomas of the cerebellum were combined and reviewed together (cAA and cerebellar glioblastomas (cGB), that could have possibly affected overall results. We present characteristics of 15 adult patients with cAA and compared them to a series of 45 patients with a supratentorial AA (sAA). The mean age at cAA diagnosis was 39.3 years (range 19-72). A history of neurofibromatosis type I was noted in 1 patient (6.7%). An IDH-1 mutation was identified in 6/15 cases and a methylated MGMT promoter in 5/15 cases. Patients in study and control groups were matched in age, sex and IDH- 1 mutation status. Patients in a study group tended to have a more frequent multifocal presentation at diagnosis (13% vs. -
A Case of Intramedullary Spinal Cord Astrocytoma Associated with Neurofibromatosis Type 1
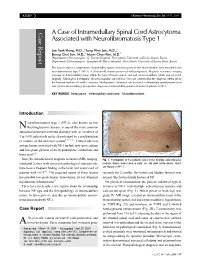
KISEP J Korean Neurosurg Soc 36 : 69-71, 2004 Case Report A Case of Intramedullary Spinal Cord Astrocytoma Associated with Neurofibromatosis Type 1 Jae Taek Hong, M.D.,1 Sang Won Lee, M.D.,1 Byung Chul Son, M.D.,1 Moon Chan Kim, M.D.2 Department of Neurosurgery,1 St. Vincent Hospital, The Catholic University of Korea, Suwon, Korea Department of Neurosurgery,2 Kangnam St. Mary's Hospital, The Catholic University of Korea, Seoul, Korea The authors report a symptomatic intramedullary spinal cord astrocytoma in the thoracolumbar area associated with neurofibromatosis type 1 (NF-1). A 38-year-old woman presented with paraparesis. Magnetic resonance imaging revealed an intramedullary lesion within the lower thoracic spinal cord and conus medullaris, which was removed surgically. Pathological investigation showed anaplastic astrocytoma. This case confirms that the diagnosis criteria set by the National Institute of Health Consensus Development Conference can be useful to differentiate ependymoma from astrocytoma when making a preoperative diagnosis of intramedullary spinal cord tumor in patients of NF-1. KEY WORDS : Astrocytoma·Intramedullary cord tumor·Neurofibromatosis. Introduction eurofibromatosis type 1 (NF-1), also known as von N Recklinghausen's disease, is one of the most common autosomal dominant inherited disorders with an incidence of 1 in 3,000 individuals and is characterized by a predisposition to tumors of the nervous system5,6,12,16). Central nervous system lesions associated with NF-1 include optic nerve glioma and low-grade gliomas of the hypothalamus, cerebellum and brain stem6,10). Since the introduction of magnetic resonance(MR) imaging, Fig. 1. Photograph of the patient's back shows multiple subcutaneous incidental lesions with uncertain pathological characteristic nodules (black arrow) and a cafe-au-lait spot (white arrow), which have been a frequent finding in the brain and spinal cord of are typical of NF-1. -

Inhibition of Mir-1193 Leads to Synthetic Lethality in Glioblastoma
Zhang et al. Cell Death and Disease (2020) 11:602 https://doi.org/10.1038/s41419-020-02812-3 Cell Death & Disease ARTICLE Open Access Inhibition of miR-1193 leads to synthetic lethality in glioblastoma multiforme cells deficient of DNA-PKcs Jing Zhang1,LiJing1,SubeeTan2, Er-Ming Zeng3, Yingbo Lin4, Lingfeng He 1, Zhigang Hu 1, Jianping Liu1 and Zhigang Guo1 Abstract Glioblastoma multiforme (GBM) is the most malignant primary brain tumor and has the highest mortality rate among cancers and high resistance to radiation and cytotoxic chemotherapy. Although some targeted therapies can partially inhibit oncogenic mutation-driven proliferation of GBM cells, therapies harnessing synthetic lethality are ‘coincidental’ treatments with high effectiveness in cancers with gene mutations, such as GBM, which frequently exhibits DNA-PKcs mutation. By implementing a highly efficient high-throughput screening (HTS) platform using an in-house-constructed genome-wide human microRNA inhibitor library, we demonstrated that miR-1193 inhibition sensitized GBM tumor cells with DNA-PKcs deficiency. Furthermore, we found that miR-1193 directly targets YY1AP1, leading to subsequent inhibition of FEN1, an important factor in DNA damage repair. Inhibition of miR-1193 resulted in accumulation of DNA double-strand breaks and thus increased genomic instability. RPA-coated ssDNA structures enhanced ATR checkpoint kinase activity, subsequently activating the CHK1/p53/apoptosis axis. These data provide a preclinical theory for the application of miR-1193 inhibition as a potential synthetic lethal approach targeting GBM cancer cells with DNA-PKcs fi 1234567890():,; 1234567890():,; 1234567890():,; 1234567890():,; de ciency. Introduction In response to DNA damage, cells activate the DNA Glioblastoma multiforme (GBM), exhibits highly damage response (DDR) network, allowing DNA repair aggressive invasion, a high mortality rate, and high resis- through the regulation of cell-cycle progression, DNA tance to radiation and cytotoxic chemotherapy, and thus damage repair or apoptosis4. -

Nodal Metastases from Laryngeal Carcinoma and Their Correlation with Certain Characteristics of the Primary Tumor
NODAL METASTASES FROM LARYNGEAL CARCINOMA AND THEIR CORRELATION WITH CERTAIN CHARACTERISTICS OF THE PRIMARY TUMOR Kamaljit Kaur ~, Nishi Sonkhya 2, A.S. Bapna 3 Key Words : Carcinoma larynx, nodal metastases. INTRODUCTION nodal metastases progresses in an orderly manner with Cancer of the larynx represents about 2% of the total the first site of metastasis being the sentinel node. cancer risk and is the most common head and neck cancer (skin excluded). It has been consistently observed by Lymphatic metastasis is the most important mechanism various authors that the status of cervical lymph nodes is in the spread of head and neck squamous cell carcinoma. the single most important prognostic factor in laryngeal Multiple clinical studies have demonstrated that the carcinoma and the probability of 5 year survival, regardless distribution of cervical lymph node metastases is indeed of the treatment rendered, reduces by 50% once the tumor predictable in patients with previously untreated squamous dissemination to the regional lymph nodes has taken place. cell carcinoma of the upper aerodigestive tract. The rate For this reason, studies dealing with the probability of of metastasis probably reflects the aggressiveness of the nodal metastases are important in making therapeutic primary tumor and is an important prognosticator. Not decisions. only the presence, but also the number of nodal metastases, their level in the neck, the size of the nodes and the presence Although the credit for first injection studies of laryngeal of extra-capsular spread are important prognostic feature. lymphatics goes to Hajek in 1891, it was the monumental study of laryngeal lymphatics by injections of dyes and There is a need to identify pretreatment factors that can radioisotopes by Pressman et al in 1956 that provided differentiate high risk from low risk patients with respect excellent documentation of the anatomical to occult metastases. -

Survival and Functional Outcome of Childhood Spinal Cord Low-Grade Gliomas
J Neurosurg Pediatrics 4:000–000,254–261, 2009 Survival and functional outcome of childhood spinal cord low-grade gliomas Clinical article KATRIN SCHEINEMANN, M.D.,1 UTE BARTELS, M.D.,2 ANNIE HUANG, M.D., PH.D.,2 CYNTHIA HAWKINS, M.D., PH.D.,3 ABHAYA V. KULKARNI, M.D., PH.D.,4 ERIC BOUFFET, M.D.,2 AND URI TABORI, M.D.2 1Division of Hematology/Oncology, McMaster Children’s Hospital, Hamilton; and Divisions of 2Hematology/ Oncology, 3Pathology, and 4Neurosurgery, The Hospital for Sick Children, Toronto, Ontario, Canada Object. Intramedullary spinal cord low-grade gliomas (LGGs) are rare CNS neoplasms in pediatric patients, and there is little information on therapy for and outcome of these tumors in this population. Furthermore, most patient series combine adult and pediatric patients or high- and low-grade tumors, resulting in controversial data regarding optimal treatment of these children. To clarify these issues, the authors performed a regional population-based study of spinal cord LGGs in pediatric patients. Methods.$OOSHGLDWULFSDWLHQWVZLWK/**VWUHDWHGGXULQJWKH05LPDJLQJHUD ² ZHUHLGHQWLÀHGLQ the comprehensive database of the Hospital for Sick Children in Toronto. Data on demographics, pathology, treat- ment details, and outcomes were collected. Results. Spinal cord LGGs in pediatric patients constituted 29 (4.6%) of 635 LGGs. Epidemiological and clini- cal data in this cohort were different than in patients with other spinal tumors and strikingly similar to data from pediatric patients with intracranial LGGs. The authors observed an age peak at 2 years and a male predominance in patients with these tumors. Histological testing revealed a Grade I astrocytoma in 86% of tumors. -

Grading Evolution and Contemporary Prognostic Biomarkers of Clinically Significant Prostate Cancer
cancers Review Grading Evolution and Contemporary Prognostic Biomarkers of Clinically Significant Prostate Cancer Konrad Sopyllo 1, Andrew M. Erickson 2 and Tuomas Mirtti 1,3,* 1 Research Program in Systems Oncology, Faculty of Medicine, University of Helsinki, 00014 Helsinki, Finland; konrad.sopyllo@helsinki.fi 2 Nuffield Department of Surgical Sciences, University of Oxford, Oxford OX3 9DU, UK; [email protected] 3 Department of Pathology, HUS Diagnostic Centre, Helsinki University Hospital, 00029 Helsinki, Finland * Correspondence: tuomas.mirtti@helsinki.fi Simple Summary: Prostate cancer treatment decisions are based on clinical stage and histological diagnosis, including Gleason grading assessed by a pathologist, in biopsies. Prior to staging and grading, serum or blood prostate-specific antigen (PSA) levels are measured and often trigger diagnostic examinations. However, PSA is best suited as a marker of cancer relapse after initial treatment. In this review, we first narratively describe the evolution of histological grading, the current status of Gleason pattern-based diagnostics and glance into future methodology of risk assessment by histological examination. In the second part, we systematically review the biomarkers that have been shown, independent from clinical characteristics, to correlate with clinically relevant end-points, i.e., occurrence of metastases, disease-specific mortality and overall survival after initial treatment of localized prostate cancer. Abstract: Gleason grading remains the strongest prognostic parameter in localized prostate ade- nocarcinoma. We have here outlined the evolution and contemporary practices in pathological evaluation of prostate tissue samples for Gleason score and Grade group. The state of more observer- Citation: Sopyllo, K.; Erickson, A.M.; Mirtti, T. Grading Evolution and independent grading methods with the aid of artificial intelligence is also reviewed. -

Astrocytoma: a Hormone-Sensitive Tumor?
International Journal of Molecular Sciences Review Astrocytoma: A Hormone-Sensitive Tumor? Alex Hirtz 1, Fabien Rech 1,2,Hélène Dubois-Pot-Schneider 1 and Hélène Dumond 1,* 1 Université de Lorraine, CNRS, CRAN, F-54000 Nancy, France; [email protected] (A.H.); [email protected] (F.R.); [email protected] (H.D.-P.-S.) 2 Université de Lorraine, CHRU-Nancy, Service de Neurochirurgie, F-54000 Nancy, France * Correspondence: [email protected]; Tel.: +33-372746115 Received: 29 October 2020; Accepted: 27 November 2020; Published: 30 November 2020 Abstract: Astrocytomas and, in particular, their most severe form, glioblastoma, are the most aggressive primary brain tumors and those with the poorest vital prognosis. Standard treatment only slightly improves patient survival. Therefore, new therapies are needed. Very few risk factors have been clearly identified but many epidemiological studies have reported a higher incidence in men than women with a sex ratio of 1:4. Based on these observations, it has been proposed that the neurosteroids and especially the estrogens found in higher concentrations in women’s brains could, in part, explain this difference. Estrogens can bind to nuclear or membrane receptors and potentially stimulate many different interconnected signaling pathways. The study of these receptors is even more complex since many isoforms are produced from each estrogen receptor encoding gene through alternative promoter usage or splicing, with each of them potentially having a specific role in the cell. The purpose of this review is to discuss recent data supporting the involvement of steroids during gliomagenesis and to focus on the potential neuroprotective role as well as the mechanisms of action of estrogens in gliomas.