Fever and a Rash
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Bacterial Skin Infections an Observational Study
RESEARCH Geoffrey Spurling Deborah Askew David King Geoffrey K Mitchell MBBS, DTM&H, FRACGP, is Senior PhD, is Senior Research Fellow, MBBS, MPH, FRACGP, is Senior Lecturer, MBBS, PhD, FRACGP, FAChPM, Lecturer, Discipline of General Practice, Discipline of General Practice, Discipline of General Practice, University is Associate Professor, Discipline University of Queensland. g.spurling@ University of Queensland. of Queensland. of General Practice, University of uq.edu.au Queensland. Bacterial skin infections An observational study Bacterial skin infections such as impetigo and boils are Background common, contagious, often painful, and have the potential to We aimed to determine the feasibility of measuring resolution rates of recur. They are caused by Staphylococcus aureus and bacterial skin infections in general practice. occasionally by Streptococcus pyogenes, and are transmitted Methods by skin-to-skin contact, fomite contact or contact with nasal Fifteen general practitioners recruited patients from March 2005 to carriers.1 In the United Kingdom, incidence of skin infections October 2007 and collected clinical and sociodemographic data at in children in 2005 was approximately 75 per 100 000.2 Skin baseline. Patients were followed up at 2 and 6 weeks to assess lesion infection rates are likely to be higher in warmer climates. The resolution. only Australian data we found were for one Northern Territory Results Aboriginal Medical Service (Danila Dilba), which recorded 7.5 Of 93 recruited participants, 60 (65%) were followed up at 2 and 6 per 100 consultations for localised skin infections.3 weeks: 50% (30) had boils, 37% (22) had impetigo, 83% (50) were prescribed antibiotics, and active follow up was suggested for 47% Suggested risk factors for impetigo include: household crowding, (28). -

Skin Cancer in the Immunocompromised Patient
Dermatologic Risks and Transplantation Allison Hanlon, MD, PhD Vanderbilt University School of Medicine Department of Medicine Division of Dermatology I have no relevant conflicts of interest to disclose. Dermatologic Risks and Transplantation • Acne • Folliculitis • Sebaceous hyperplasia • Overgrowth of hair • Infections – warts, molluscum contagiosum • Skin thinning and increased bruising • Skin cancer Folliculitis and Acne Folliculitis Sebaceous Hyperplasia Overgrowth of Hair Cyclosporine associated Gingival Hyperplasis Molluscum Contagiosum Verruca Easy Bruising and Skin Thinning Overview of Skin Cancer in SOTR • Clinical appearance of most common skin cancers • Risk factors for developing skin cancer • Skin cancer prevention • Multidisciplinary care Basal Cell Carcinoma Basal Cell Carcinoma Nodular Basal Cell Carcinoma Basal Cell Carcinoma Squamous Cell Carcinoma Squamous Cell Carcinoma Field Cancerization Immunocompromised patients at risk for metastasis Melanoma Nail Unit Melanoma Nodular Melanoma Melanoma Benign Seborrheic Keratosis Skin cancer is the most common malignancy in solid organ transplant recipients • Skin cancer accounts for 40% of malignancies in solid organ transplant recipients (SOTR) • 50% of Caucasian SOTR will develop skin cancer • Non-melanoma skin cancer (NMSC) > melanoma Euvrard S, Kanitakis J, Claudy A. Skin cancers after organ transplantation. N Engl J Med 2003;348:1681 Skin Cancer in SOTR • Squamous cell carcinoma (SCC) is the most common cutaneous malignancy in transplant patient • Basal cell carcinoma (BCC) is second most common skin cancer in transplant patient • Melanoma risk 3.6 times greater likelihood in SOTR Hollenbeak CS et al. Cancer 2005; 104:1962 than the general Euvrard S et.al. N Engl J Med 2003;348:1681 population Lanov E et.al. Int J Cancer. 2010;126:1724 Proposed Mechanisms Of Immunosuppression relationship to Skin Cancer Development • Direct carcinogenic effects of immunosuppression medications • Proliferation of oncogenic viruses • Reduced immune surveillance within transplant skin cancers Carucci et.al.PLoS One. -

Molluscum Contagiosum
Partners in Pediatrics, PC 7110 Forest Ave Suite 105 Richmond, VA 23226 804-377-7100 Molluscum Contagiosum Although molluscum contagiosum is a common skin rash in kids, many parents have never heard of it. The most important thing to know about it is that, for most children, the rash is no big deal and goes away on its own over time. About Molluscum Contagiosum Molluscum contagiosum is a viral infection that causes a mild skin rash. The rash looks like one or more small growths or wart-like bumps (called mollusca) that are usually pink, white, or skin-colored. The bumps are usually soft and smooth and may have an indented center. Infection is most common among kids between 1 and 12 years old, but also occurs in: teens and adults some athletes, such as wrestlers, swimmers, and gymnasts people whose immune systems have been weakened by HIV, cancer treatment, or long-term steroid use As you might guess by its name, this skin disorder is contagious, and can be passed from one person to another. It is unknown how long the rash and virus may be contagious. Causes Molluscum contagiosum is caused by the molluscum contagiosum virus (MCV), a member of the poxvirus family. This virus thrives in warm, humid climates and in areas where people live very close together. Infection with MCV occurs when the virus enters a small break in the skin's surface. Many people who come in contact with the virus have immunity against it, and do not develop any growths. For those not resistant to it, growths usually appear 2 to 8 weeks after infection. -

Inflammatory Or Infectious Hair Disease? a Case of Scalp Eschar and Neck Lymph Adenopathy After a Tick Bite
Case Report ISSN: 2574 -1241 DOI: 10.26717/BJSTR.2021.35.005688 Adherent Serous Crust of the Scalp: Inflammatory or Infectious Hair Disease? A Case of Scalp Eschar and Neck Lymph Adenopathy after a Tick Bite Starace M1, Vezzoni R*2, Alessandrini A1 and Piraccini BM1 1Dermatology - IRCCS, Policlinico Sant’Orsola, Department of Specialized, Experimental and Diagnostic Medicine, Alma Mater Studiorum, University of Bologna, Italy 2Dermatology Clinic, Maggiore Hospital, University of Trieste, Italy *Corresponding author: Roberta Vezzoni, Dermatology Clinic, Maggiore Hospital, University of Trieste, Italy ARTICLE INFO ABSTRACT Received: Published: April 17, 2021 The appearance of a crust initially suggests inflammatory scalp diseases, although infectious diseases such as impetigo or insect bites should also be considered among April 27, 2021 the differential diagnoses. We report a case of 40-year-old woman presentedB. Burgdorferi to our, Citation: Starace M, Vezzoni R, Hair Disease Outpatient Service with an adherent serous crust on the scalp and lymphadenopathy of the neck. Serological tests confirmed the aetiology of while rickettsia infection was excluded. Lyme borreliosis can mimic rickettsia infection Alessandrini A, Piraccini BM. Adherent and may present as scalp eschar and neck lymphadenopathy after a tick bite (SENLAT). Serous Crust of the Scalp: Inflammatory Appropriate tests should be included in the diagnostic workup of patients with necrotic or Infectious Hair Disease? A Case of Scalp scalpKeywords: eschar in order to promptly set -

Dermatology DDX Deck, 2Nd Edition 65
63. Herpes simplex (cold sores, fever blisters) PREMALIGNANT AND MALIGNANT NON- 64. Varicella (chicken pox) MELANOMA SKIN TUMORS Dermatology DDX Deck, 2nd Edition 65. Herpes zoster (shingles) 126. Basal cell carcinoma 66. Hand, foot, and mouth disease 127. Actinic keratosis TOPICAL THERAPY 128. Squamous cell carcinoma 1. Basic principles of treatment FUNGAL INFECTIONS 129. Bowen disease 2. Topical corticosteroids 67. Candidiasis (moniliasis) 130. Leukoplakia 68. Candidal balanitis 131. Cutaneous T-cell lymphoma ECZEMA 69. Candidiasis (diaper dermatitis) 132. Paget disease of the breast 3. Acute eczematous inflammation 70. Candidiasis of large skin folds (candidal 133. Extramammary Paget disease 4. Rhus dermatitis (poison ivy, poison oak, intertrigo) 134. Cutaneous metastasis poison sumac) 71. Tinea versicolor 5. Subacute eczematous inflammation 72. Tinea of the nails NEVI AND MALIGNANT MELANOMA 6. Chronic eczematous inflammation 73. Angular cheilitis 135. Nevi, melanocytic nevi, moles 7. Lichen simplex chronicus 74. Cutaneous fungal infections (tinea) 136. Atypical mole syndrome (dysplastic nevus 8. Hand eczema 75. Tinea of the foot syndrome) 9. Asteatotic eczema 76. Tinea of the groin 137. Malignant melanoma, lentigo maligna 10. Chapped, fissured feet 77. Tinea of the body 138. Melanoma mimics 11. Allergic contact dermatitis 78. Tinea of the hand 139. Congenital melanocytic nevi 12. Irritant contact dermatitis 79. Tinea incognito 13. Fingertip eczema 80. Tinea of the scalp VASCULAR TUMORS AND MALFORMATIONS 14. Keratolysis exfoliativa 81. Tinea of the beard 140. Hemangiomas of infancy 15. Nummular eczema 141. Vascular malformations 16. Pompholyx EXANTHEMS AND DRUG REACTIONS 142. Cherry angioma 17. Prurigo nodularis 82. Non-specific viral rash 143. Angiokeratoma 18. Stasis dermatitis 83. -

Skin Manifestation of SARS-Cov-2: the Italian Experience
Journal of Clinical Medicine Article Skin Manifestation of SARS-CoV-2: The Italian Experience Gerardo Cazzato 1 , Caterina Foti 2, Anna Colagrande 1, Antonietta Cimmino 1, Sara Scarcella 1, Gerolamo Cicco 1, Sara Sablone 3, Francesca Arezzo 4, Paolo Romita 2, Teresa Lettini 1 , Leonardo Resta 1 and Giuseppe Ingravallo 1,* 1 Section of Pathology, University of Bari ‘Aldo Moro’, 70121 Bari, Italy; [email protected] (G.C.); [email protected] (A.C.); [email protected] (A.C.); [email protected] (S.S.); [email protected] (G.C.); [email protected] (T.L.); [email protected] (L.R.) 2 Section of Dermatology and Venereology, University of Bari ‘Aldo Moro’, 70121 Bari, Italy; [email protected] (C.F.); [email protected] (P.R.) 3 Section of Forensic Medicine, University of Bari ‘Aldo Moro’, 70121 Bari, Italy; [email protected] 4 Section of Gynecologic and Obstetrics Clinic, University of Bari ‘Aldo Moro’, 70121 Bari, Italy; [email protected] * Correspondence: [email protected] Abstract: At the end of December 2019, a new coronavirus denominated Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) was identified in Wuhan, Hubei province, China. Less than three months later, the World Health Organization (WHO) declared coronavirus disease-19 (COVID-19) to be a global pandemic. Growing numbers of clinical, histopathological, and molecular findings were subsequently reported, among which a particular interest in skin manifestations during the course of the disease was evinced. Today, about one year after the development of the first major infectious foci in Italy, various large case series of patients with COVID-19-related skin Citation: Cazzato, G.; Foti, C.; manifestations have focused on skin specimens. -
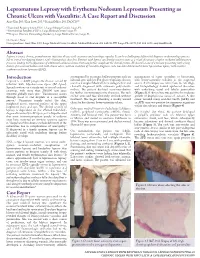
Lepromatous Leprosy with Erythema Nodosum Leprosum Presenting As
Lepromatous Leprosy with Erythema Nodosum Leprosum Presenting as Chronic Ulcers with Vasculitis: A Case Report and Discussion Anny Xiao, DO,* Erin Lowe, DO,** Richard Miller, DO, FAOCD*** *Traditional Rotating Intern, PGY-1, Largo Medical Center, Largo, FL **Dermatology Resident, PGY-2, Largo Medical Center, Largo, FL ***Program Director, Dermatology Residency, Largo Medical Center, Largo, FL Disclosures: None Correspondence: Anny Xiao, DO; Largo Medical Center, Graduate Medical Education, 201 14th St. SW, Largo, FL 33770; 510-684-4190; [email protected] Abstract Leprosy is a rare, chronic, granulomatous infectious disease with cutaneous and neurologic sequelae. It can be a challenging differential diagnosis in dermatology practice due to several overlapping features with rheumatologic disorders. Patients with leprosy can develop reactive states as a result of immune complex-mediated inflammatory processes, leading to the appearance of additional cutaneous lesions that may further complicate the clinical picture. We describe a case of a woman presenting with a long history of a recurrent bullous rash with chronic ulcers, with an evolution of vasculitic diagnoses, who was later determined to have lepromatous leprosy with reactive erythema nodosum leprosum (ENL). Introduction accompanied by an intense bullous purpuric rash on management of sepsis secondary to bacteremia, Leprosy is a slowly progressive disease caused by bilateral arms and face. For these complaints she was with lower-extremity cellulitis as the suspected infection with Mycobacterium leprae (M. leprae). seen in a Complex Medical Dermatology Clinic and source. A skin biopsy was taken from the left thigh, Spread continues at a steady rate in several endemic clinically diagnosed with cutaneous polyarteritis and histopathology showed epidermal ulceration countries, with more than 200,000 new cases nodosa. -

Bacterial Infections Diseases Picture Cause Basic Lesion
page: 117 Chapter 6: alphabetical Bacterial infections diseases picture cause basic lesion search contents print last screen viewed back next Bacterial infections diseases Impetigo page: 118 6.1 Impetigo alphabetical Bullous impetigo Bullae with cloudy contents, often surrounded by an erythematous halo. These bullae rupture easily picture and are rapidly replaced by extensive crusty patches. Bullous impetigo is classically caused by Staphylococcus aureus. cause basic lesion Basic Lesions: Bullae; Crusts Causes: Infection search contents print last screen viewed back next Bacterial infections diseases Impetigo page: 119 alphabetical Non-bullous impetigo Erythematous patches covered by a yellowish crust. Lesions are most frequently around the mouth. picture Lesions around the nose are very characteristic and require prolonged treatment. ß-Haemolytic streptococcus is cause most frequently found in this type of impetigo. basic lesion Basic Lesions: Erythematous Macule; Crusts Causes: Infection search contents print last screen viewed back next Bacterial infections diseases Ecthyma page: 120 6.2 Ecthyma alphabetical Slow and gradually deepening ulceration surmounted by a thick crust. The usual site of ecthyma are the legs. After healing there is a permanent scar. The pathogen is picture often a streptococcus. Ecthyma is very common in tropical countries. cause basic lesion Basic Lesions: Crusts; Ulcers Causes: Infection search contents print last screen viewed back next Bacterial infections diseases Folliculitis page: 121 6.3 Folliculitis -

Erythema Nodosum (En)
Buffalo Medical Group, P.C. Robert E. Kalb, M.D. Phone: (716) 630-1102 Fax: (716) 633-6507 Department of Dermatology 325 Essjay Road Williamsville, New York 14221 ERYTHEMA NODOSUM (EN) Erythema Nodosum (EN) is a relatively uncommon reaction in the skin consisting of red shiny tender nodular lesions most commonly found on the legs. The erythema refers to the red color that is seen at the surface of the skin. The nodosum refers to the fact that these lesions feel like bumps or nodules underneath the skin surface. Erythema nodosum is a reaction pattern occurring in the subcutaneous tissue and fat. It may be preceded by a low grade fever, fatigue, and joint pains. In about half of the cases, there is an internal condition occurring in the body which contributes to its formation. These include the use of certain medications, certain infections, and a number of other less likely causes. In order to identify cause for the erythema nodosum, it may be necessary to perform blood and laboratory tests. At times, however, the cause cannot be determined and erythema nodosum is considered to be idiopathic in nature. Erythema nodosum often runs an acute course lasting for a brief period from weeks to months. In a small percentage of cases, it can be a more chronic condition. The red nodules are usually confined to the lower legs, but can develop anywhere there is fat under the skin including the thighs, arms, and trunk. Initially, the lesions are more red and inflamed in appearance, but with time become more bruise like. -

MYELOPATHY ASSOCIATED with SYSTEMIC LUPUS ERYTHEMATOSUS (Erythema Nodosum)
Paraplegia 16 (1978-79) 282-294 Original Articles MYELOPATHY ASSOCIATED WITH SYSTEMIC LUPUS ERYTHEMATOSUS (Erythema Nodosum) L. S. KEWALRAMANI, M.D., M.S.Orth., S. SALEEM, M.D. and D. BERTRAND, M.T. (ASCP) Texas Institute for Rehabilitation and Research and Department of Pathology, Baylor College of Medicine, Houston, Texas 77030, U.S.A. Abstract. Two patients with sudden onset of myelopathy associated with Systemic Lupus Erythematosus (Erythema Nodosum) are described. Pertinent literature is extensively reviewed and these two new patients are added to previously reported 26 patients. Key words: Myelopathy; Meningoencephalomyelopathy; Systemic lupus erythematosus. NEUROLOGICAL manifestations of systemic lupus erythematosus (SLE) have only recently been emphasised although they were mentioned by Kaposi in 1875, who observed stupor and coma as terminal manifestations of the disease. But focal neurological abnormalities were first reported by Osler (1903) and since then there have been several reports in the literature. Most commonly reported entities have been acute organic brain syndrome, seizures and cerebrovascular disorders. Chorea, Guillain Barre syndrome, subarachnoid haemorrhage, peripheral neuro pathy and cranial nerve palsies associated with SLE have also been reported on a few occasions. Myelopathy, however, has not received adequate emphasis as a complication of SLE. Fisher and Gilmour reported the first case of flaccid paraplegia in a female with SLE in 1939. Since then only 25 additional cases have been reported in the medical literature over the past 38 years. Twenty cases have been described in sufficient detail and six briefly, to permit a meaningful review of the spinal cord involvement in this disease. We feel that there are probably many more unreported cases of myelopathy associated with SLE. -

022291S015 Eltrombopag Clinical BPCA
CLINICAL REVIEW Application Type sNDA Application Number(s) 022291, S-015 Priority or Standard Priority Submit Date(s) December 19, 2014 Received Date(s) December 19, 2014 PDUFA Goal Date June 19, 2015 Division / Office Division of Hematology Products/OHOP Reviewer Name(s) Lori A. Ehrlich Review Completion Date May 26, 2015 Established Name Eltrombopag Trade Name Promacta® Therapeutic Class Thrombopoietin Agonist Applicant Glaxo SmithKline Formulation(s) Tablet Dosing Regimen 50 mg once daily Indication(s) Chronic ITP Intended Population(s) Pediatric patients ≥6 years old with chronic ITP Template Version: March 6, 2009 Reference ID: 3765521 Clinical Review Lori A. Ehrlich, MD, PhD NDA 022291, S-015 Promacta® (eltrombopag) tablets Table of Contents 1 RECOMMENDATIONS/RISK BENEFIT ASSESSMENT ......................................... 8 1.1 Recommendation on Regulatory Action ............................................................. 8 1.2 Risk Benefit Assessment.................................................................................... 9 1.3 Recommendations for Postmarket Risk Evaluation and Mitigation Strategies . 11 1.4 Recommendations for Postmarket Requirements and Commitments .............. 11 2 INTRODUCTION AND REGULATORY BACKGROUND ...................................... 11 2.1 Product Information .......................................................................................... 12 2.2 Tables of Currently Available Treatments for Proposed Indications ................. 12 2.3 Availability of Proposed Active Ingredient -

Eyelid Conjunctival Tumors
EYELID &CONJUNCTIVAL TUMORS PHOTOGRAPHIC ATLAS Dr. Olivier Galatoire Dr. Christine Levy-Gabriel Dr. Mathieu Zmuda EYELID & CONJUNCTIVAL TUMORS 4 EYELID & CONJUNCTIVAL TUMORS Dear readers, All rights of translation, adaptation, or reproduction by any means are reserved in all countries. The reproduction or representation, in whole or in part and by any means, of any of the pages published in the present book without the prior written consent of the publisher, is prohibited and illegal and would constitute an infringement. Only reproductions strictly reserved for the private use of the copier and not intended for collective use, and short analyses and quotations justified by the illustrative or scientific nature of the work in which they are incorporated, are authorized (Law of March 11, 1957 art. 40 and 41 and Criminal Code art. 425). EYELID & CONJUNCTIVAL TUMORS EYELID & CONJUNCTIVAL TUMORS 5 6 EYELID & CONJUNCTIVAL TUMORS Foreword Dr. Serge Morax I am honored to introduce this Photographic Atlas of palpebral and conjunctival tumors,which is the culmination of the close collaboration between Drs. Olivier Galatoire and Mathieu Zmuda of the A. de Rothschild Ophthalmological Foundation and Dr. Christine Levy-Gabriel of the Curie Institute. The subject is now of unquestionable importance and evidently of great interest to Ophthalmologists, whether they are orbital- palpebral specialists or not. Indeed, errors or delays in the diagnosis of tumor pathologies are relatively common and the consequences can be serious in the case of malignant tumors, especially carcinomas. Swift diagnosis and anatomopathological confirmation will lead to a treatment, discussed in multidisciplinary team meetings, ranging from surgery to radiotherapy.