Abnormal Head Positions in the Eye Clinic Overview General
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Vertical Perspective Medical Assistance Program
Kansas Vertical Perspective Medical Assistance Program December 2006 Provider Bulletin Number 688 General Providers Emergent and Nonemergent Diagnosis Code List Attached is a list of diagnosis codes and whether the Kansas Medical Assistance Program (KMAP) considers the code to be emergent or nonemergent. Providers are responsible for validating whether a particular diagnosis code is covered by KMAP under the beneficiary’s benefit plan and that all program requirements are met. This list does not imply or guarantee payment for listed diagnosis codes. Information about the Kansas Medical Assistance Program as well as provider manuals and other publications are on the KMAP Web site at https://www.kmap-state-ks.us. If you have any questions, please contact the KMAP Customer Service Center at 1-800-933-6593 (in-state providers) or (785) 274-5990 between 7:30 a.m. and 5:30 p.m., Monday through Friday. EDS is the fiscal agent and administrator of the Kansas Medical Assistance Program for the Kansas Health Policy Authority. Page 1 of 347 Emergency Indicators as noted by KMAP: N – Never considered emergent S – Sometimes considered emergent (through supporting medical documentation) Y – Always considered emergent Diagnosis Emergency Diagnosis Code Description Code Indicator 0010 Cholera due to Vibrio Cholerae S 0011 Cholera due to Vibrio Cholerae El Tor S 0019 Unspecified Cholera S 019 Late Effects of Tuberculosis N 0020 Typhoid Fever S 0021 Paratyphoid Fever A S 0022 Paratyphoid Fever B S 0023 Paratyphoid Fever C S 024 Glanders Y 025 Melioidosis -

Code Description
Code Description 0061 Chronic intestinal amebiasis without mention of abscess 0062 Amebic nondysenteric colitis 0063 Amebic liver abscess 0064 Amebic lung abscess 00642 West Nile fever with other neurologic manifestation 00649 West Nile fever with other complications 0065 Amebic brain abscess 0066 Amebic skin ulceration 0068 Amebic infection of other sites 0069 Amebiasis, unspecified 0070 Other protozoal intestinal diseases, balantidiasis (Infection by Balantidium coli) 0071 Other protozoal intestinal diseases, giardiasis 0072 Other protozoal intestinal diseases, coccidiosis 0073 Other protozoal intestinal diseases, trichomoniasis 0074 Other protozoal intestinal diseases, cryptosporidiosis 0075 Other protozoal intestional disease cyclosporiasis 0078 Other specified protozoal intestinal diseases 0079 Unspecified protozoal intestinal disease 01000 Primary tuberculous infection, unspecified 01001 Primary tuberculous infection bacteriological or histological examination not done 01002 Primary tuberculous infection, bacteriological or histological examination results unknown 01003 Primary tuberculous infection, tubercle bacilli found by microscopy 01004 Primary tuberculous infection, tubercle bacilli found by bacterial culture 01005 Primary tuberculous infection, tubercle bacilli confirmed histolgically 01006 Primary tuberculous infection, tubercle bacilli found by other methods 01010 Tuberculous pleurisy in primary progressive tuberculosis unspecified 01011 Tuberculous pleurisy bacteriological or histological examination not done 01012 Tuberculous -

Strabismus: a Decision Making Approach
Strabismus A Decision Making Approach Gunter K. von Noorden, M.D. Eugene M. Helveston, M.D. Strabismus: A Decision Making Approach Gunter K. von Noorden, M.D. Emeritus Professor of Ophthalmology and Pediatrics Baylor College of Medicine Houston, Texas Eugene M. Helveston, M.D. Emeritus Professor of Ophthalmology Indiana University School of Medicine Indianapolis, Indiana Published originally in English under the title: Strabismus: A Decision Making Approach. By Gunter K. von Noorden and Eugene M. Helveston Published in 1994 by Mosby-Year Book, Inc., St. Louis, MO Copyright held by Gunter K. von Noorden and Eugene M. Helveston All rights reserved. No part of this publication may be reproduced, stored in a retrieval system, or transmitted, in any form or by any means, electronic, mechanical, photocopying, recording, or otherwise, without prior written permission from the authors. Copyright © 2010 Table of Contents Foreword Preface 1.01 Equipment for Examination of the Patient with Strabismus 1.02 History 1.03 Inspection of Patient 1.04 Sequence of Motility Examination 1.05 Does This Baby See? 1.06 Visual Acuity – Methods of Examination 1.07 Visual Acuity Testing in Infants 1.08 Primary versus Secondary Deviation 1.09 Evaluation of Monocular Movements – Ductions 1.10 Evaluation of Binocular Movements – Versions 1.11 Unilaterally Reduced Vision Associated with Orthotropia 1.12 Unilateral Decrease of Visual Acuity Associated with Heterotropia 1.13 Decentered Corneal Light Reflex 1.14 Strabismus – Generic Classification 1.15 Is Latent Strabismus -

Visual Function Following Congenital Cataract Surgery
Visual Function Following Congenital Cataract Surgery Misao Yamamoto, Murat Dogru, Makoto Nakamura, Hiroko Shirabe, Yasutomo Tsukahara, Yoshibumi Sekiya Department of Ophthalmology, Kobe University School of Medicine, Kobe, Japan Abstract: To evaluate the results of congenital cataract extraction and postoperative visual function, we retrospectively reviewed the records of 95 patients who underwent pars plana (plicata) lensectomy or aspiration surgery. Forty-nine percent of the patients with bilateral aphakia and 25% with bilateral pseudophakia had a Landolt visual acuity of 0.5 or above at the final visit. The figures were 31% and 66% for patients with unilateral aphakia and pseudophakia, respectively. Eight patients (16.3%) with bilateral and 2 patients (5.8%) with unilateral cataract for whom contact lenses were prescribed after surgery attained fine stere- opsis. Five of 8 patients (62.5%) with unilateral cataract who had intraocular lens implanta- tion ended up with gross or fine stereopsis. We stress that very early surgery and optical cor- rection in the sensitive period of binocular visual development should be instituted, especially in the presence of dense opacities. A good postoperative visual outcome can be achieved in patients undergoing late surgery if the opacities are light or partial in nature. We also reemphasize the importance of aggressive and diligent visual rehabilitation and occlu- sion therapy against amblyopia. Jpn J Ophthalmol 1998;42:411–416 © 1998 Japanese Ophthalmological Society Key Words: Amblyopia, aphakia, congenital cataract, pars plana lensectomy, stereopsis. Introduction tients who received either contact lens fitting or pos- An infantile cataract not only blurs the retinal im- terior chamber intraocular lens implantation. -

PEDIATRIC OPHTHALMOLOGY of a Round Table
PEDIATRIC OPHTHALMOLOGY Summary of a Round Table By James E. Miller, M.D. Department of Ophthalmology, School of Medicine, Washington University T HE ROUND TABLE covered two principal The lacnimal glands in the upper part topics : first, external diseases of the of the lid are seldom involved in an inflam- eye, especially in relation to infection and matory process, except occasionally in to lid and conjunctival lesions; and, second, mumps or sarcoid. growth and development of the eye with Herpes simplex of the lid, consisting of stress upon eye movements, refractive er- a vesicle which crusts and then heals, is rors, and strabismus. often seen with concomitant mouth lesions. External diseases of the eye are often Involvement of the conjunctivae is also primary, but pathology in this area fre- seen. quently is found to reflect systemic illness. Herpes zoster may affect the lid when it involves the first division of the tnigeminal LID nerve. Intraocular involvement usually fol- Various glands of the lid were defined lows skin manifestations on the tip of the and the pathology of each reviewed. In the nose. Topical use of adrenal steroids is fibrous tarsal portion of the lid lies the sometimes employed in the treatment of Meibomian gland, the sebaceous secretion herpes zoster. Varicella is closely related of which prevents the spillage of tears and or may be due to the same virus as herpes protects the lid margin. The acute inflam- zoster; it also produces vesicles on the con- rnation is usually staphylococcal, and tends junctivae, but these usually resolve them- to persist to produce a granuloma sur- selves without any sequelae. -

931 Brain Imaging CPT, HCPCS and Diagnoses Codes
Medical Policy Brain Imaging CPT, HCPCS and Diagnoses Codes Policy Number: 931 BCBSA Reference Number: N/A NCD/LCD: N/A Related Policies • Medicare Advantage: Advanced Imaging/Radiology and Sleep Disorder Management Clinical and Utilization Guidance Redirect, #923 • Advanced Imaging/Radiology CPT and HCPCS Codes, #900 • Advanced Imaging/Radiology, #968 • Oncologic Imaging CPT, HCPCS and Diagnoses Codes, #929 • Abdomen and Pelvic Imaging CPT, HCPCS and Diagnoses Codes, #930 • Chest Imaging CPT, HCPCS and Diagnoses Codes, #932 • Extremity Imaging CPT, HCPCS and Diagnoses Codes, #933 • Head and Neck Imaging CPT, HCPCS and Diagnoses Codes, #934 • Spine Imaging CPT, HCPCS and Diagnoses Codes, #935 • Vascular Imaging CPT, HCPCS and Diagnoses Codes, #936 Table of Contents Commercial Products .................................................................................................................................... 1 Medicare Advantage Products ...................................................................................................................... 2 CPT Codes / HCPCS Codes / ICD Codes .................................................................................................... 2 CPT Codes: 70450, 70460, 70470 CT head/brain ....................................................................................... 2 CPT codes: 70551, 70552, 70553 MRI brain............................................................................................ 115 CPT codes: 70554, 70555 MRI brain functional ...................................................................................... -

Asthenopia in Schoolchildren � �
Thesis for doctoral degree (Ph.D.) 2007 Asthenopia in Schoolchildren Saber Abdi From SECTION OF OPHTHALMOLOGY AND VISION DEPARTMENT OF CLINICAL NEUROSCIENCE, St. Erik Eye Hospital Karolinska Institutet, Stockholm, Sweden Asthenopia in Schoolchildren Saber Abdi Stockholm 2007 Papers II, III, IV, are reproduced by the permission of the journals. Published and printed by Karolinska University Press Box 200, SE-171 77 Stockholm, Sweden © Saber Abdi, 2007 IBSN 978-91-7357-180 In dear memory of my mother SUMMARY Asthenopia is a term used to describe different symptoms associated with the use of the eyes, such as pain, blurred vision, diplopia, headaches. Asthenopia is most often reported in association with near vision. Children with asthenopia complain of such symptoms particularly when reading and writing. Asthenopia is often divided into two main categories: refractive including refractive errors and anisometropia, and muscular, comprising strabismus and convergence insufficiency. Asthenopia due to accommodative problems has in the present studies been regarded as muscular asthenopia. In paper I the prevalence of asthenopia, refractive errors and binocular disorders was determined in a representative population of 216 Swedish schoolchildren aged 6 – 15 years. The prevalence of asthenopia was 23.1 %. The prevalence of hypermetropia and myopia changed with age, while astigmatism, convergence ability and strabismus did not. Accommodative insufficiency was more common in the older schoolchildren. Asthenopia was related to uncorrected visual acuity and refractive errors, and to accommodative insufficiency. Paper II described the orthoptic and ophthalmological findings in a group of 120 schoolchildren with asthenopia. The effect of asthenopia treatment was also evaluated. The most frequently occurring findings related to asthenopia were refractive errors, heterophoria and accommodative insufficiency. -

Global Burden of Eye and Vision Disease As Reflected in the Cochrane Database of Systematic Reviews
Research Original Investigation Global Burden of Eye and Vision Disease as Reflected in the Cochrane Database of Systematic Reviews Lindsay N. Boyers, BA; Chante Karimkhani, BA; John Hilton, MSc, MPhil; William Richheimer, MD; Robert P. Dellavalle, MD, PhD, MSPH Supplemental content at IMPORTANCE Eye and vision disease burden should help guide ophthalmologic research jamaophthalmology.com prioritization. The Global Burden of Disease (GBD) Study 2010 compiled data from 1990 to 2010 on 291 diseases and injuries, 1160 disease and injury sequelae, and 67 risk factors in 187 countries. The Cochrane Database of Systematic Reviews (CDSR) is a resource for systematic reviews in health care, with peer-reviewed systematic reviews that are published by Cochrane Review Groups. OBJECTIVE To determine whether systematic review and protocol topics in the CDSR reflect disease burden, measured by disability-adjusted life-years (DALYs), from the GBD 2010 project. This is one of a series of projects mapping GBD 2010 medical field disease burdens to corresponding systematic reviews in the CDSR. DESIGN AND SETTING Two investigators independently assessed 8 ophthalmologic conditions in the CDSR for systematic review and protocol representation according to subject content. The 8 diseases were matched to their respective DALYs from the GBD 2010 project. MAIN OUTCOMES AND MEASURES Cochrane Database of Systematic Reviews systematic review and protocol representation and percentage of total 2010 DALYs. RESULTS All 8 ophthalmologic conditions were represented by at least 1 systematic review in the CDSR. A total of 91.4% of systematic reviews and protocols focused on these conditions were from the Cochrane Eyes and Vision Group. Comparing the number of reviews and protocols with disability, only cataract was well matched; glaucoma, macular degeneration, and other vision loss were overrepresented. -

Binocular Vision and Ocular Motility SIXTH EDITION
Binocular Vision and Ocular Motility SIXTH EDITION Binocular Vision and Ocular Motility THEORY AND MANAGEMENT OF STRABISMUS Gunter K. von Noorden, MD Emeritus Professor of Ophthalmology Cullen Eye Institute Baylor College of Medicine Houston, Texas Clinical Professor of Ophthalmology University of South Florida College of Medicine Tampa, Florida Emilio C. Campos, MD Professor of Ophthalmology University of Bologna Chief of Ophthalmology S. Orsola-Malpighi Teaching Hospital Bologna, Italy Mosby A Harcourt Health Sciences Company St. Louis London Philadelphia Sydney Toronto Mosby A Harcourt Health Sciences Company Editor-in-Chief: Richard Lampert Acquisitions Editor: Kimberley Cox Developmental Editor: Danielle Burke Project Manager: Agnes Byrne Production Manager: Peter Faber Illustration Specialist: Lisa Lambert Book Designer: Ellen Zanolle Copyright ᭧ 2002, 1996, 1990, 1985, 1980, 1974 by Mosby, Inc. All rights reserved. No part of this publication may be reproduced or transmit- ted in any form or by any means, electronic or mechanical, including photo- copy, recording, or any information storage and retrieval system, without per- mission in writing from the publisher. NOTICE Ophthalmology is an ever-changing field. Standard safety precautions must be followed, but as new research and clinical experience broaden our knowledge, changes in treatment and drug therapy may become necessary or appropriate. Readers are advised to check the most current product information provided by the manufacturer of each drug to be administered to verify the recommended dose, the method and duration of administration, and contraindications. It is the responsibility of the treating physician, relying on experience and knowledge of the patient, to determine dosages and the best treatment for each individual pa- tient. -

Surgical Management of Strabismus
SURGICAL MANAGEMENT OF STRABISMUS EUGENE M. HELVESTON, M.D. Emeritus Professor of Ophthalmology Indiana University School of Medicine Department of Ophthalmology Section of Pediatric Ophthalmology and Strabismus Indianapolis, Indiana FIFTH EDITION With 852 illustrations With love and gratitude to my wife Barbara Preface to the fifth edition The 33 years since the publication of the Atlas of around the world. These patients' consultations were Strabismus Surgery has seen a steady growth in the made possible by ORBIS Telemedicine, Cyber-Sight number of ophthalmologists specializing in the diag- that is supported by the server at Flight Safety in New nosis and treatment of strabismus. Membership in the York and provided through the generosity of Mr. American Association for Pediatric Ophthalmology Albert Ueltschi. By viewing these images and read- and Strabismus has grown to more than 500 mem- ing the discussion that accompanies each, it is my bers and the International Strabismological hope that the reader will by critical analysis along Association boasts 300 members in 25 countries. with comparison of the patients seen in his or her clin- Several journals deal exclusively or largely with the ic hone skills for a more effective personal approach subject of strabismus and several high quality texts to the whole patient leading to better outcome. have been published dealing with strabismus diagno- This book represents the 'full circle' in that it is sis and management. Moreover, an explosion in the based on experience during a professional lifetime in field of information technology has brought people the care of patients with strabismus. It is my hope together and facilitated the distribution of information that what I have learned and then shared here will be in a way not dreamed of when the first edition of this of use to those who follow. -
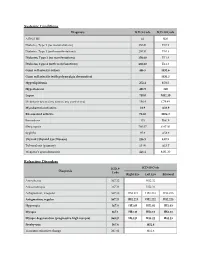
Systemic Conditions Refractive Disorders
Systemic Conditions Diagnosis ICD-9 Code ICD-10 Code AIDS/HIV 42 B20 Diabetes, Type 1 (no manifestations) 250.01 E10.9 Diabetes, Type 1 (with manifestations) 250.51 E10.3 Diabetes, Type 2 (no manifestations) 250.00 E11.9 Diabetes, Type 2 (with manifestations) 250.50 E11.3 Giant cell arteritis (other) 446.5 M31.6 Giant cell arteritis (with polymyalgia rheumatica) M31.5 Hyperlipidemia 272.4 E78.5 Hypertension 401.9 I10 Lupus 710.0 M32.10 Metastasis to eye (any cancer, any part of eye) 198.4 C79.49 Mycobacteria infection 31.9 A31.9 Rheumatoid arthritis 714.0 M06.9 Sarcoidosis 135 D86.9 Sleep apnea 780.57 G47.30 Syphilis 97.9 A53.9 Thyroid (Thyroid Eye Disease) 246.9 E07.9 Tuberculosis (primary) 10.00 A15.7 Wegener’s granulomatosis 446.4 M31.30 Refractive Disorders ICD-9 ICD-10 Code Diagnosis Code Right Eye Left Eye Bilateral Aniseikonia 367.32 H52.32 Anisometropia 367.31 H52.31 Astigmatism, irregular 367.22 H52.211 H52.212 H52.213 Astigmatism, regular 367.21 H52.221 H52.222 H52.223 Hyperopia 367.0 H52.01 H52.02 H52.03 Myopia 367.1 H52.11 H52.12 H52.13 Myopic degeneration (progressive high myopia) 360.21 H44.21 H44.22 H44.23 Presbyopia 367.4 H52.4 Transient refractive change 367.81 H52.6 General Eye-Related Codes ICD-9 ICD-10 Code Diagnosis Code Right Eye Left Eye Bilateral Color deficiency: Achromatopsia H53.51 Color deficiency: Acquired color vision deficiency H53.52 Color deficiency: Deuteranomaly H53.53 Color deficiency: Protanomaly H53.54 Color deficiency: Tritanomaly H53.55 Day blindness (hemeralopia) H53.11 Diplopia 368.2 H53.2 Glare -

Abstract Book
AAPOS 45TH ANNUAL MEETING ABSTRACT BOOK 27–31 HILTON BAYFRONT Table of Contents Lectures Costenbader page 3 Helveston page 4 Papers page 5 Posters page 44 Session 1 page 45 Session 2 page 145 Workshops page 245 The Costenbader Lecture Making the Superior Oblique Great Again David A. Plager, MD Purpose/Relevance: To review the history and bring up to date clinically relevant knowledge about the anatomy and physiology of the superior oblique Target Audience: Strabismus surgeons Current Practice: Varies widely among strabismologists according to their training and personal experience Best Practice: Evaluation and treatment algorithms based on the author’s 30 years of learning from others, personal experience and mistakes. There will be emphasis on the importance of relative tendon laxity, how it is easily evaluated and how it can be applied to surgical decision making. When torsion should be specifically addressed or perhaps can be willfully ignored will be discussed. Expected Outcomes: Audience will have an appreciation of the history of strabismologist attitudes toward operating on the superior oblique, the evolution of knowledge about its structure and function, and the author’s approach toward formulating individual surgical plans based on a combination of clinical and intraoperative findings. Format: Lecture supplemented with illustrations and videos Summary: The superior oblique is by far the most complicated extraocular muscle and the source of more angst and controversy when learning how best to approach its dysfunction than all the other EOMs combined. However, by applying a few basic principles and avoiding a few common pitfalls, surgeons can have many grateful patients whose annoying or even debilitating symptoms they have relieved.