Definitions, Pathophysiology, and Epidemiology of Acute Cholangitis and Cholecystitis: Tokyo Guidelines
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Print This Article
International Surgery Journal Lew D et al. Int Surg J. 2021 May;8(5):1575-1578 http://www.ijsurgery.com pISSN 2349-3305 | eISSN 2349-2902 DOI: https://dx.doi.org/10.18203/2349-2902.isj20211831 Case Report Acute gangrenous appendicitis and acute gangrenous cholecystitis in a pregnant patient, a difficult diagnosis: a case report David Lew, Jane Tian*, Martine A. Louis, Darshak Shah Department of Surgery, Flushing Hospital Medical Center, Flushing, New York, USA Received: 26 February 2021 Accepted: 02 April 2021 *Correspondence: Dr. Jane Tian, E-mail: [email protected] Copyright: © the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Abdominal pain is a common complaint in pregnancy, especially given the physiological and anatomical changes that occur as the pregnancy progresses. The diagnosis and treatment of common surgical pathologies can therefore be difficult and limited by the special considerations for the fetus. While uncommon in the general population, concurrent or subsequent disease processes should be considered in the pregnant patient. We present the case of a 36 year old, 13 weeks pregnant female who presented with both acute appendicitis and acute cholecystitis. Keywords: Appendicitis, Cholecystitis, Pregnancy, Pregnant INTRODUCTION population is rare.5 Here we report a case of concurrent appendicitis and cholecystitis in a pregnant woman. General surgeons are often called to evaluate patients with abdominal pain. The differential diagnosis list must CASE REPORT be expanded in pregnant woman and the approach to diagnosing and treating certain diseases must also be A 36 year old, 13 weeks pregnant female (G2P1001) adjusted to prevent harm to the fetus. -

Choledochoduodenal Fistula Complicatingchronic
Gut: first published as 10.1136/gut.10.2.146 on 1 February 1969. Downloaded from Gut, 1969, 10, 146-149 Choledochoduodenal fistula complicating chronic duodenal ulcer in Nigerians E. A. LEWIS AND S. P. BOHRER From the Departments ofMedicine and Radiology, University ofIbadan, Nigeria Peptic ulceration was thought to be rare in Nigerians SOCIAL CLASS All the patients were in the lower until the 1930s when Aitken (1933) and Rose (1935) socio-economic class. This fact may only reflect the reported on this condition. Chronic duodenal ulcers, patients seen at University College Hospital. in particular, are being reported with increasing frequency (Ellis, 1948; Konstam, 1959). The symp- AETIOLOGY Twelve (92.3 %) of the fistulas resulted toms and complications of duodenal ulcers in from chronic duodenal ulcer and in only one case Nigerians are the same as elsewhere, but the relative from gall bladder disease. incidence of these complications differs markedly. Pyloric stenosis is the commonest complication CLINICAL FEATURES There were no special symp- followed by haematemesis and malaena in that order toms or signs for this complication. All patients (Antia and Solanke, 1967; Solanke and Lewis, except the one with gall bladder disease presented 1968). Perforation though present is not very com- with symptoms of chronic duodenal ulcer or with mon. those of pyloric stenosis of which theie were four A remarkable complication found in some of our cases. In the case with gall bladder disease the history patients with duodenal ulcer who present them- was short and characterized by fever, right-sided selves for radiological examination is the formation abdominal pain, jaundice, and dark urine. -

Imaging of Biliary Infections
3 Imaging of Biliary Infections Onofrio Catalano, MD1 Ronald S. Arellano, MD2 1 Division of Abdominal Imaging, Department of Radiology, Address for correspondence Onofrio Catalano, MD, Division of Massachusetts General Hospital, Harvard Medical School, Abdominal Imaging, Department of Radiology, Massachusetts Boston, Massachusetts General Hospital, Harvard Medical School, 55 Fruit Street, White 270, 2 Division of Interventional Radiology, Department of Radiology, Boston, MA 02114 (e-mail: [email protected]). Massachusetts General Hospital, Harvard Medical School, Boston, Massachusetts Dig Dis Interv 2017;1:3–7. Abstract Biliary tract infections cover a wide spectrum of etiologies and clinical presentations. Imaging plays an important role in understanding the etiology and as well as the extent Keywords of disease. Imaging also plays a vital role in assessing treatment response once a ► biliary infections diagnosis is established. This article will review the imaging findings of commonly ► cholangitides encountered biliary tract infectious diseases. ► parasites ► immunocompromised ► echinococcal Infections of the biliary tree can have a myriad of clinical and duodenum can lead toa cascade ofchanges tothehost immune imaging manifestations depending on the infectious etiolo- defense mechanisms of chemotaxis and phagocytosis.7 The gy, underlying immune status of the patient and extent of resultant lackof bile and secretory immunoglobulin A from the involvement.1,2 Bacterial infections account for the vast gastrointestinal tract lead -
Cholecystitis
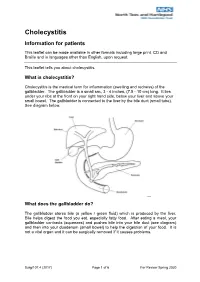
Cholecystitis Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about cholecystitis. What is cholecystitis? Cholecystitis is the medical term for inflammation (swelling and redness) of the gallbladder. The gallbladder is a small sac, 3 - 4 inches, (7.5 - 10 cm) long. It lies under your ribs at the front on your right hand side, below your liver and above your small bowel. The gallbladder is connected to the liver by the bile duct (small tube). See diagram below. What does the gallbladder do? The gallbladder stores bile (a yellow / green fluid) which is produced by the liver. Bile helps digest the food you eat, especially fatty food. After eating a meal, your gallbladder contracts (squeezes) and pushes bile into your bile duct (see diagram) and then into your duodenum (small bowel) to help the digestion of your food. It is not a vital organ and it can be surgically removed if it causes problems. Surg/107.4 (2017) Page 1 of 6 For Review Spring 2020 Cholecystitis What causes cholecystitis? Inflammation of the gallbladder is often caused when gallstones irritate the gallbladder and sometimes cause an infection. Gallstones are formed in the gallbladder or bile duct and develop when bile forms crystals. Over time these crystals become hardened and eventually grow into stones but they do not always cause problems. However, gallstones can cause: jaundice. If the stones move from your gallbladder and block your bile duct jaundice can occur. -

Clinical Biliary Tract and Pancreatic Disease
Clinical Upper Gastrointestinal Disorders in Urgent Care, Part 2: Biliary Tract and Pancreatic Disease Urgent message: Upper abdominal pain is a common presentation in urgent care practice. Narrowing the differential diagnosis is sometimes difficult. Understanding the pathophysiology of each disease is the key to making the correct diagnosis and providing the proper treatment. TRACEY Q. DAVIDOFF, MD art 1 of this series focused on disorders of the stom- Pach—gastritis and peptic ulcer disease—on the left side of the upper abdomen. This article focuses on the right side and center of the upper abdomen: biliary tract dis- ease and pancreatitis (Figure 1). Because these diseases are regularly encountered in the urgent care center, the urgent care provider must have a thorough understand- ing of them. Biliary Tract Disease The gallbladder’s main function is to concentrate bile by the absorption of water and sodium. Fasting retains and concentrates bile, and it is secreted into the duodenum by eating. Impaired gallbladder contraction is seen in pregnancy, obesity, rapid weight loss, diabetes mellitus, and patients receiving total parenteral nutrition (TPN). About 10% to 15% of residents of developed nations will form gallstones in their lifetime.1 In the United States, approximately 6% of men and 9% of women 2 have gallstones. Stones form when there is an imbal- ©Phototake.com ance in the chemical constituents of bile, resulting in precipitation of one or more of the components. It is unclear why this occurs in some patients and not others, Tracey Q. Davidoff, MD, is an urgent care physician at Accelcare Medical Urgent Care in Rochester, New York, is on the Board of Directors of the although risk factors do exist. -

Abdominal Pain
10 Abdominal Pain Adrian Miranda Acute abdominal pain is usually a self-limiting, benign condition that irritation, and lateralizes to one of four quadrants. Because of the is commonly caused by gastroenteritis, constipation, or a viral illness. relative localization of the noxious stimulation to the underlying The challenge is to identify children who require immediate evaluation peritoneum and the more anatomically specific and unilateral inner- for potentially life-threatening conditions. Chronic abdominal pain is vation (peripheral-nonautonomic nerves) of the peritoneum, it is also a common complaint in pediatric practices, as it comprises 2-4% usually easier to identify the precise anatomic location that is produc- of pediatric visits. At least 20% of children seek attention for chronic ing parietal pain (Fig. 10.2). abdominal pain by the age of 15 years. Up to 28% of children complain of abdominal pain at least once per week and only 2% seek medical ACUTE ABDOMINAL PAIN attention. The primary care physician, pediatrician, emergency physi- cian, and surgeon must be able to distinguish serious and potentially The clinician evaluating the child with abdominal pain of acute onset life-threatening diseases from more benign problems (Table 10.1). must decide quickly whether the child has a “surgical abdomen” (a Abdominal pain may be a single acute event (Tables 10.2 and 10.3), a serious medical problem necessitating treatment and admission to the recurring acute problem (as in abdominal migraine), or a chronic hospital) or a process that can be managed on an outpatient basis. problem (Table 10.4). The differential diagnosis is lengthy, differs from Even though surgical diagnoses are fewer than 10% of all causes of that in adults, and varies by age group. -

Problems in Family Practice Acute Abdominal Pain in Children
dysuria. The older child may start bed wetting with or without dysuria. A problems in Family Practice drop of fresh, clean unspun urine will usually reveal pyuria, but in the early case relatively few white blood cells may be seen compared to gross bacillu- Acute Abdominal Pain ria. The infection may have underlying urinary tract abnormality, stone, in Children hydronephrosis, polycystic kidney or renal neoplasms. The IVP is important Hyman Shrand, M D in detecting these underlying prob lems. Cambridge, M assachusetts 4. Viral Hepatitis. Malaise, anorexia, abdominal pain, and tenderness over Acute abdominal pain in children is a common and challenging prob the liver occur with hepatitis A or B. lem for the family physician. The many causes of this problem require Later, patients who become jaundiced a systematic approach to making the diagnosis and planning specific have dark urine and pale stools. In therapy. A careful history and physical examination, together with a teenagers, “needle tracks” suggest sy ringe transmitted Type B (H.A.A.) small number of selected laboratory studies, provide a rational basis hepatitis. Youngsters with infectious for effective management in most cases. This paper reviews the more mononucleosis may present as hepati common causes of acute abdominal pain in children with special em tis. phasis on their clinical differentiation. 5. Upper Respiratory Tract. Strepto coccal pharyngitis, a common cause of Abdominal pain in a child is always followed by vomiting is more likely an vomiting and abdominal pain, can be an emergency. The primary physician intra-abdominal disorder. recognized by looking at the throat must identify a “medical” cause in or with confirmatory throat culture. -

General Medicine - Surgery IV Year
1 General Medicine - Surgery IV year 1. Overal mortality rate in case of acute ESR – 24 mm/hr. Temperature 37,4˚C. Make appendicitis is: the diagnosis? A. 10-20%; A. Appendicular colic; B. 5-10%; B. Appendicular hydrops; C. 0,2-0,8%; C. Appendicular infiltration; D. 1-5%; D. Appendicular abscess; E. 25%. E. Peritonitis. 2. Name the destructive form of appendicitis. 7. A 34-year-old female patient suffered from A. Appendicular colic; abdominal pain week ago; no other B. Superficial; gastrointestinal problems were noted. On C. Appendix hydrops; clinical examination, a mass of about 6 cm D. Phlegmonous; was palpable in the right lower quadrant, E. Catarrhal appendicitis. appeared hard, not reducible and fixed to the parietal muscle. CBC: leucocyts – 3. Koher sign is: 7,5*109/l, ESR – 24 mm/hr. Temperature A. Migration of the pain from the 37,4˚C. Triple antibiotic therapy with epigastrium to the right lower cefotaxime, amikacin and tinidazole was quadrant; very effective. After 10 days no mass in B. Pain in the right lower quadrant; abdominal cavity was palpated. What time C. One time vomiting; term is optimal to perform appendectomy? D. Pain in the right upper quadrant; A. 1 week; E. Pain in the epigastrium. B. 2 weeks; C. 3 month; 4. In cases of appendicular infiltration is D. 1 year; indicated: E. 2 years. A. Laparoscopic appendectomy; B. Concervative treatment; 8. What instrumental method of examination C. Open appendectomy; is the most efficient in case of portal D. Draining; pyelophlebitis? E. Laparotomy. A. Plain abdominal film; B. -

Or Ascending Cholangitis) Is a Clinical Syndrome That Is Classically Characterized by the Triad Of
ACUTE ASCENDING CHOLANGITIS Introduction Acute cholangitis (or ascending cholangitis) is a clinical syndrome that is classically characterized by the triad of: ● Fever ● Abdominal pain ● Jaundice The condition occurs as a result of obstruction/ stasis and subsequent infection within the biliary tract. In the absence of appropriate treatment the condition has significant potential for mortality and morbidity. It is a medical emergency that requires prompt antibiotic treatment and urgent relief of biliary obstruction (usually by endoscopic retrograde cholangiopancreatography ERCP). History Jean M. Charcot was the first to describe this illness in 1877. He described a triad of fever, jaundice, and right upper quadrant pain. Epidemiology Acute cholangitis is predominantly seen in adults, most commonly around 40-70 years of age. Physiology Normal barrier mechanisms to cholangitis infection include ● The sphincter of Oddi, which normally forms an effective mechanical barrier to duodenal reflux and ascending bacterial infection. ● Continuous flushing action of bile plus the bacteriostatic activity of bile salts which help maintain bile sterility. ● Secretory IgA and biliary mucous probably also function as anti-adherence factors, preventing bacterial colonization Pathology Organisms: Ascending cholangitis is usually associated with Gram-negative or anaerobic sepsis. ● Aerobic organisms include Escherichia coli and Klebsiella and Enterococcus species. ● The most common anaerobic organism is Bacteroides fragilis. Clostridia may also cause serious infection. Causes: Ascending cholangitis essentially occurs as consequence of obstruction of the biliary tract. Stasis leads to secondary bacterial infection; the organisms typically ascending from the duodenum. Biliary obstruction raises intrabiliary pressure and leads to increased permeability of bile ductules, permitting translocation of bacteria and toxins from the portal circulation into the biliary tract. -

Risk for Appendicitis, Cholecystitis, Or Diverticulitis in Patients with Psoriasis
ORIGINAL RESEARCH Risk for Appendicitis, Cholecystitis, or Diverticulitis in Patients With Psoriasis Erica B. Lee, BS; Mina Amin, BS; Lewei Duan, MS; Alexander Egeberg, MD, PhD; Jashin J. Wu, MD soriasis is a chronic skin condition affecting approx- PRACTICE POINTS imately 2% to 3% of the population.1,2 Beyond • Patients with psoriasis may have elevated risk of P cutaneous manifestations, psoriasis is a systemic diverticulitis compared to healthy patients. However, copy inflammatory state that is associated with an increased psoriasis patients do not appear to have increased risk for cardiovascular disease, including obesity,3,4 type 2 risk of appendicitis or cholecystitis. diabetes mellitus,5,6 hypertension,5 dyslipidemia,3,7 meta- • Clinicians treating psoriasis patients should consider bolic syndrome,7 atherosclerosis,8 peripheral vascular assessing for other risk factors of diverticulitis at disease,9 coronary artery calcification,10 myocardial infarc- regular intervals. tion,11-13 stroke,9,14 and cardiac death.15,16 Psoriasis also has been associated with inflammatory bowel notdisease (IBD), possibly because of similar auto- Numerous comorbidities have been associated with psoriasis; immune mechanisms in the pathogenesis of both dis- however, no studies have considered the relationship between eases.17,18 However, there is no literature regarding the risk psoriasis and appendicitis, cholecystitis, or diverticulitis. To deter- for acute gastrointestinal pathologies such as appendicitis, mine the incidence rate and hazard risk (HR) -

Cholestatic Liver Diseases: Patterns of Disease and Challenges
6/24/2015 Cholestatic liver diseases: Patterns of disease and challenges Joseph Misdraji, MD GI pathology unit Massachusetts General Hospital Cholestatic Disorders The differential in biopsies with tissue cholestasis Chronic cholestatic conditions Ductopenia 1 6/24/2015 Case 1 67 year old woman on multiple medications, diagnosed with drug induced autoimmune hepatitis 5 months earlier. While on steroids, the transaminases improved but the LFT pattern became cholestatic with increasing bilirubin. The clinical team did a biopsy to evaluate for overlap PBC/AIH. 2 6/24/2015 3 6/24/2015 Cholestatic Disorders Usually shows bile stasis. Often no bile stasis. The differential for acute The differential for chronic cholestatic reaction cholestatic disorder Drug reaction Primary Biliary Cirrhosis Large bile duct obstruction Primary Sclerosing Ascending cholangitis Cholangitis Gram negative infection, sepsis IgG4 cholangitis Paraneoplastic (lymphoma, Sarcoidosis renal cell carcinoma) Cystic fibrosis Some infections: Hepatitis A, Other small duct hepatitis E, (syphilis) cholangiopathies Familial cholestatic disorder Chronic outflow obstruction Total parenteral nutrition Chronic rejection 4 6/24/2015 Drug Induced Cholestatic Hepatitis Most common pattern of drug induced injury – a primary consideration in adults with cholestasis Presents acutely and mimics obstructive jaundice Features that favor drugs – Eosinophils – Granulomas 5 6/24/2015 6 6/24/2015 7 6/24/2015 8 6/24/2015 Large Duct Obstruction Mechanical obstruction – Strictures – Tumors – Stones – PSC – Many others Abdominal pain, fever, rigors, prior biliary surgery, and older age suggest obstruction. Ultrasound detects dilated ducts in about a quarter of patients. 9 6/24/2015 10 6/24/2015 Sepsis Cholangiolar cholestasis – Bile in neocholangioles (as opposed to bile inspissated in the actual duct) – Paradoxically, not typical of obstruction – Sepsis, severe drug reactions, catastrophic illness Neutrophils in portal tracts 11 6/24/2015 Our case Cholestatic hepatic parenchyma. -

Gallstone Disease: the Big Picture
GALLSTONE DISEASE: THE BIG PICTURE UNR ECHO PROJECT CLARK A. HARRISON, MD GASTROENTEROLOGY CONSULTANTS RENO, NEVADA DEFINITIONS CHOLELITHIASIS = stones or sludge in the gallbladder CHOLEDOCHOLITHIASIS = stones/sludge in the bile ducts CHOLECYSTITIS = inflamed gallbladder usually in the presence of stones or sludge CHOLANGITIS = stasis and infection in the bile ducts as a result of stones, benign stenosis, or malignancy GALLSTONE PANCREATITIS = acute pancreatitis related to choledocholithiasis with obstruction at the papilla GALLBLADDER AND BILIARY ANATOMY Gallbladder Cystic Duct Right and Left Intraheptics Common Hepatic Duct Common Bile Duct Ampulla of Vater Major Papilla BILIARY ANATOMY GALLSTONE EPIDEMIOLOGY • A common and costly disease • US estimates are 6.3 million men and 14.2 million women between ages of 20-74. • Prevalence among non-Hispanic white men and women is 8-16%. • Prevalence among Hispanic men and women is 9-27%. • Prevalence among African Americans is lower at 5-14%. • More common among Western Caucasians, Hispanics and Native Americans • Less common among Eastern Europeans, African Americans, and Asians GALLSTONE RISK FACTORS • Ethnicity • Female > Male • Pregnancy • Older age • Obesity • Rapid weight loss/bariatric surgery GALLSTONES: NATURAL HISTORY • 15%-20% will develop symptoms • *Once symptoms develop, there is an increased risk of complications. • Incidental or silent gallstones do not require treatment. • Special exceptions due to increased risk of gallbladder cancer: Large gallstone > 3cm, porcelain gallbladder, gallbladder polyp/adenoma 10mm or bigger, and anomalous pancreatic duct drainage GALLSTONES: CLINICAL SYMPTOMS • Biliary colic which is a misnomer and not true colic • Episodic steady epigastric or RUQ pain often radiating to the R scapular area • Peaks rapidly within 5-10 minutes and lasts 30 minutes to 6 hours or more • Frequently associated with N/V • Fatty meal is a common trigger, but symptoms may occur day or night without a meal.