Bariatric Surgical Procedure Guide
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Duodenal Switch. a Switch to the Duodenal Switch. A
Bariátrica & Metabólica Ibero-Americana (2019) 9.2.4: 2554-2563 Duodenal switch. A switch to the duodenal switch. A. Baltasar, N. Pérez, R. Bou, C. Serra Hospital "Virgen De Los Lirios De Alcoy”, Clínica San Jorge [email protected] 616.231.021 ABSTRACT: Background: The duodenal Switch (DS) combines a Sleeve-forming Keywords: gastrectomy (SFG) and a bilio-pancreatic diversion (BPD). Objectives: To report on 950 DS patients treated from 1994 to 2011. • Duodenal junction • Bariatric surgery Environment: Regional teaching hospital and private institution. • Vertical gastrectomy Methods: Prospective study of 950 consecutive patients treated with CD. • Bilio-pancreatic diversion • Poliphenols. Results: There were 518 open DS (ODS) and 432 laparoscopic DS (LDS). Surgical mortality of 0.73% (1.6% in CDA and 0.47% in CDL), 4.84% incidence of leakage, two liver failure (0.2%) and protein calorie malnutrition (PCM) in 3.1%. At 5 years, the %EWL drops by 80% and the Expected BMI by 100%. Conclusions: The CD is the most aggressive bariatric technique, with the best long-term weight loss. Operative complications and long-term follow-up guidelines are described. The aim is to change the bariatric techniques to accept the CD. 2555 Bariátrica & Metabólica Ibero-Americana (2019) 9.2.4: 2554-2563 Introduction Description of surgical techniques The Duodenal Switch (DS) is a mixed operation that consists Open DS (ODS) by transverse laparotomy of two techniques, a gastric surgery, the Sleeve-forming The patient is in Trendelenburg position. A transverse Vertical Gastrectomy (SFG) to reduce intake and also an supraumbilical incision is made between both costal intestinal surgery, the bilio-pancreatic diversion (BPD) that margins (Fig.2 a-b). -

Adjustable Gastric Banding
7 Review Article Page 1 of 7 Adjustable gastric banding Emre Gundogdu, Munevver Moran Department of Surgery, Medical School, Istinye University, Istanbul, Turkey Contributions: (I) Conception and design: All authors; (II) Administrative support: All authors; (III) Provision of study materials or patients: All authors; (IV) Collection and assembly of data: All authors; (V) Data analysis and interpretation: All authors; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Emre Gündoğdu, MD, FEBS. Assistant Professor of Surgery, Department of Surgery, Medical School, Istinye University, Istanbul, Turkey. Email: [email protected]; [email protected]. Abstract: Gastric banding is based on the principle of forming a small volume pouch near the stomach by wrapping the fundus with various synthetic grafts. The main purpose is to limit oral intake. Due to the fact that it is a reversible surgery, ease of application and early results, the adjustable gastric band (AGB) operation has become common practice for the last 20 years. Many studies have shown that the effectiveness of LAGB has comparable results with other procedures in providing weight loss. Early studies have shown that short term complications after LAGB are particularly low when compared to the other complicated procedures. Even compared to RYGB and LSG, short-term results of LAGB have been shown to be significantly superior. However, as long-term results began to emerge, such as failure in weight loss, increased weight regain and long-term complication rates, interest in the procedure disappeared. The rate of revisional operations after LAGB is rapidly increasing today and many surgeons prefer to convert it to another bariatric procedure, such as RYGB or LSG, for revision surgery in patients with band removed after LAGB. -

Clinical Policy: Bariatric Surgery Reference Number: NH
Clinical Policy: Bariatric Surgery Reference Number: NH. CP.MP.37 Coding Implications Effective Date: 06/09 Revision Log Last Review Date: 04/18 See Important Reminder at the end of this policy for important regulatory and legal information. Description There are two categories of bariatric surgery: restrictive procedures and malabsorptive procedures. Gastric restrictive procedures include procedures where a small pouch is created in the stomach to restrict the amount of food that can be eaten, resulting in weight loss. The laparoscopic adjustable gastric banding (LAGB) and laparoscopic sleeve gastrectomy (LSG) are examples of restrictive procedures. Malabsorptive procedures bypass portions of the stomach and intestines causing incomplete digestion and absorption of food. Duodenal switch is an example of a malabsorptive procedure. Roux-en-y gastric bypass (RYGB), biliopancreatic diversion with duodenal switch (BPD-DS), and biliopancreatic diversion with gastric reduction duodenal switch (BPD-GRDS) are examples of restrictive and malabsorptive procedures. LAGB devices are currently not FDA approved for adolescents less than 18 years, but an industry- sponsored prospective study is in progress, and numerous retrospective studies of adolescents have been published with favorable results. Policy/Criteria It is the policy of NH Healthy Families that the bariatric surgery procedures LAGB, LSG, and laparoscopic RYGB for adolescents and adults and laparoscopic BPD-DS/BPD-GRDS for adults are medically necessary when meeting the following criteria under section I through III: I. Participating providers that are MBSAQIP (Metabolic and Bariatric Surgery Accreditation and Quality Improvement Program for the American College of Surgeons) accredited have demonstrated a commitment to excellence in ethics, quality and patient care. -

A Matched Cohort Analysis of Single Anastomosis Loop Duodenal Switch Versus Roux-En-Y Gastric Bypass with 18-Month Follow-Up - Springer
A matched cohort analysis of single anastomosis loop duodenal switch versus Roux-en-Y gastric bypass with 18-month follow-up - Springer Search Submit Article Surgical Endoscopy pp 1-7 First online: 22 December 2015 A matched cohort analysis of single anastomosis loop duodenal switch versus Roux-en-Y gastric bypass with 18-month follow-up Austin Cottam, Daniel Cottam , Walter Medlin, Christina Richards, Samuel Cottam, Hinali Zaveri, Amit Surve 10.1007/s00464-015-4707-7 Copyright information Abstract Background The Roux-en-Y gastric bypass (GBP) has been considered the gold standard for many years. The loop duodenal switch (LDS) is a relatively new procedure that simplifies the complexity of the duodenal switch (BPDDS) by making it a single anastomosis procedure while at the same time giving it more intestinal absorption to reduce the rates of malnutrition associated with traditional BPDDS. This paper seeks to compare the 18-month weight loss outcomes and complications of the more standard GBP with the newer LDS in a single US center. Methods A retrospective matched cohort was analyzed on 108 patients who had either GBP (54 patients) or LDS (54 patients). Regression analysis was used to compare weight loss outcomes as measured by BMI and weight loss percentages. Complications gathered included bleeds, reoperations, diagnostic or therapeutic endoscopy (EGD), ulcers and chronic nausea. Results GBP and LDS have statistically similar weight loss at 18 months (39.6 vs 41 % weight loss, respectively). However, there were significantly more nausea complaints (26 vs 5), diagnostic endoscopies (EGD) (21 vs 3) and ulcers (6 vs 0) with the GBP than the LDS. -

Biliopancreatic Diversion with a Duodenal Switch
Obesity Surgeuy, 8, 267-282 Biliopancreatic Diversion with a Duodenal Switch Douglas S. Hess MD, FACS; Douglas W. Hess MD Wood County Hospital, Bowling Green, OH, USA Background: This paper evaluates biliopancreatic BPD without some of the associated problems. diversion combined with the duodenal switch, form- This operation is now used by us for all our ing a hybrid procedure which is a combination of bariatric patients, both in primary surgical proce- restriction and malabsorption. Methods: The evaluation is of the first 440 patients dures and reoperations. undergoing this procedure who had had no previous The difficulty of establishing an operation that bariatric surgery. The mean starting weight was has both long- and short-term success is well 183 kg, with 41% of our patients considered super known. Bariatric surgery is either restrictive or morbidly obese (BMI > 50). malabsorptive in nature, each with its own ad- Results: There was an average maximum weight loss of 80% excess weight by 24 months post- vantages, disadvantages and complications. While operation; this continued at a 70% level for 8 years. trying to find a procedure that would produce Major complications were found in almost 9% of the better long-term results and fewer failures, i.e. cases. There were two perioperative deaths, one regain of weight, we began to look at the from pulmonary embolism and one from acute Scopinaro BPD.l First of all we considered it pulmonary obstruction. There were 36 type II dia- betics, all of whom have discontinued medication only for reoperations on failed restrictive proce- following the surgery. -

OBESITY SURGERY: INDICATIONS, TECHNIQUES, WEIGHTLOSS and POSSIBLE COMPLICATIONS - Review Article
REFERENCES: 1. Makauchi M, Mori T, Gunven P, et 3. Belghiti J, Noun R, Malafosse R, et T, Sauvanet A. Portal triad clamping or al. Safety of hemihepatic vascular occlusion al. Continuous versus intermittent portal hepatic vascular exclusion for major liver during resection of the liver. Surg Gynecol triad clamping for liver resection. A resection. A controlled study. Ann Surg. Obstet 1989; 130:824–831. controlled study. Ann Surg 1999; 229:369 1996 Aug; 224(2):155-61 2. Wobbes T, Bemelmans BLH, –375. 6. PE Clavien, S Yadav, d. Syndram, R. Kuypers JHC, et al. Risk of postoperative 4. J.R. Hiatt J.Gabbay,R W. Busuttil. Bently. Protective Effects of Ischemic septic complications after abdominal Surgical Anatomy of the Hepatic Arteries Preconditioning for Liver Resection surgery treatment in relation to in 1000 Cases. Ann Surg.1994 Vol. 220, Performed Under Inflow Occlusion in preoperative blood transfusion. Surg No. 1, 50-52 Humans. Ann Surg Vol. 232, No. 2, 155– Gynecol Obstet 1990; 171: 5. Belghiti J, Noun R, Zante E, Ballet 162 Corresponding author: Ludmil Marinov Veltchev, MD PhD Mobile: +359 876 259 685 E-mail: [email protected] Journal of IMAB - Annual Proceeding (Scientific Papers) 2009, book 1 OBESITY SURGERY: INDICATIONS, TECHNIQUES, WEIGHTLOSS AND POSSIBLE COMPLICATIONS - Review article Ludmil M. Veltchev Fellow, Master’s Program in Hepatobiliary Pancreatic Surgery, Henri Bismuth Hepatobiliary Institute, 12-14, avenue Paul Vaillant-Couturier, 94804 Villejuif Cedex SUMMARY type of treatment is the only one leading to a lasting effect. In long-term perspective, the conservative treatment Basically, two mechanisms allow the unification of all of obesity is always doomed to failure and only the surgical known methods into three categories: method allows reducing obesity. -

Laparoscopic Bariatric Surgery Manual
Laparoscopic Bariatric Surgery Manual The Center for Bariatrics & Healthy Weight 11 Upper Riverdale Road, SW Surgery Suites – Women’s Center Ground Floor Riverdale, GA 30274 Office: 770-897-SLIM (7546) Fax: 770-996-3941 1 | P a g e Dr. Karleena Tuggle, M.D., F.A.C.S Board-certified Bariatric Surgeon 2 | P a g e What is the Process? Before Surgery • Information Seminar • Initial consultation • Insurance verified and clearances reviewed with Patient Advocate • Nutritional consultation and completion of any required weight loss visits • Completion of all other required appointments/clearances • Support group participation Around the time of Surgery • Pre-op appointment with Surgeon 2 weeks before surgery • Endoscopy (EGD) 1-2 weeks before surgery with surgeon • Bariatric surgery performed After Surgery • 2 week post-operative appointment with surgeon o When applicable 1 week appointment for drain removal • 6 week post-operative appointment with health care provider • 3-6 months: appointments with health care provider, nutritionist, exercise physiologist, mental health professional, support groups as needs are identified • 6 months and yearly appointments: check up with health care provider • At a minimum yearly appointments should be continued indefinitely where we check weight goals, blood lab work and overall health 3 | P a g e Table of Contents Page Morbid Obesity and Bariatric Surgery 5-6 Signs and Symptoms of Complications 6-8 Recommended Vitamin Regimen 8-11 How to Prepare for Weight Loss Surgery 11-12 2 Day Clear Liquid Diet 13 Morning -

ASMBS Position Statement on the Relationship Between Obesity And
Surgery for Obesity and Related Diseases 16 (2020) 713–724 ASMBS Guidelines/Statements ASMBS position statement on the relationship between obesity and cancer, and the role of bariatric surgery: risk, timing of treatment, effects on disease biology, and qualification for surgery Saber Ghiassi, M.D.a, Maher El Chaar, M.D.b, Essa M. Aleassa, M.D.c,d, Fady Moustarah, M.D.e, Sofiane El Djouzi, M.D.f, T. Javier Birriel, M.D.g, Ann M. Rogers, M.D.h,*, for the American Society for Metabolic and Bariatric Surgery Clinical Issues Committee aDepartment of Surgery, Yale University School of Medicine, New Haven, Connecticut bDepartment of Bariatric Surgery, St. Luke’s University Health Network, Allentown, Pennsylvania cDepartment of General Surgery, Bariatric and Metabolic Institute, Cleveland Clinic, Cleveland, Ohio dDepartment of Surgery, College of Medicine and Health Sciences, United Arab Emirates University, Al Ain, United Arab Emirates eAscension St. Mary’s Hospital, Saginaw, Michigan fAMITA Health, Hoffman Estates, Illinois gSt. Luke’s University Health Network, Stroudsburg, Pennsylvania hDivision of Minimally Invasive and Bariatric Surgery, Penn State Health, Hershey, Pennsylvania Received 13 March 2020; accepted 16 March 2020 Preamble bariatric surgery. In this statement, a summary of current, published, peer-reviewed scientific evidence, and expert The following position statement is issued by the Amer- opinion is presented. The intent of issuing such a statement ican Society for Metabolic and Bariatric Surgery in response is to provide available objective information about these to numerous inquiries made to the Society by patients, phy- topics. The statement is not intended as, and should not be sicians, Society members, hospitals, health insurance construed as, stating or establishing a local, regional, or na- payors, the media, and others, regarding the relationship be- tional standard of care. -

The Utility of Diagnostic Laparoscopy in Post-Bariatric Surgery Patients with Chronic Abdominal Pain of Unknown Etiology
OBES SURG (2017) 27:1924–1928 DOI 10.1007/s11695-017-2590-0 ORIGINAL CONTRIBUTIONS The Utility of Diagnostic Laparoscopy in Post-Bariatric Surgery Patients with Chronic Abdominal Pain of Unknown Etiology Mohammad Alsulaimy1,2 & Suriya Punchai1,3 & Fouzeyah A. Ali4 & Matthew Kroh1 & Philip R. Schauer1 & Stacy A. Brethauer 1 & Ali Aminian1 Published online: 22 February 2017 # Springer Science+Business Media New York 2017 Abstract Overall, 15 patients (43%) had symptomatic improvement Purpose Chronic abdominal pain after bariatric surgery is as- after laparoscopy; 14 of these patients had positive laparo- sociated with diagnostic and therapeutic challenges. The aim scopic findings requiring intervention (70% of the patients of this study was to evaluate the yield of laparoscopy as a with positive laparoscopy). Conversely, 20 (57%) patients re- diagnostic and therapeutic tool in post-bariatric surgery pa- quired long-term medical treatment for management of chron- tients with chronic abdominal pain who had negative imaging ic abdominal pain. and endoscopic studies. Conclusion Diagnostic laparoscopy, which is a safe proce- Methods A retrospective analysis was performed on post- dure, can detect pathological findings in more than half of bariatric surgery patients who underwent laparoscopy for di- post-bariatric surgery patients with chronic abdominal pain agnosis and treatment of chronic abdominal pain at a single of unknown etiology. About 40% of patients who undergo academic center. Only patients with both negative preopera- diagnostic laparoscopy and 70% of patients with positive find- tive CT scan and upper endoscopy were included. ings on laparoscopy experience significant symptom improve- Results Total of 35 post-bariatric surgery patients met the in- ment. -

Technic VERTICAL GASTROPLASTY WITH
ABCDDV/802 ABCD Arq Bras Cir Dig Technic 2011;24(3): 242-245 VERTICAL GASTROPLASTY WITH JEJUNOILEAL BYPASS - NEW TECHNICAL PROCEDURE Gastroplastia vertical com desvio jejunoileal - novo procedimento técnico Bruno ZILBERSTEIN, Arthur Sergio da SILVEIRA-FILHO, Juliana Abbud FERREIRA, Marnay Helbo de CARVALHO, Cely BUSSONS, Henrique JOAQUIM, Fernando RAMOS From Gastromed-Instituto Zilberstein, São ABSTRACT - Introduction - Vertical gastroplasty is increasingly used in the surgical Paulo, SP, Brasil. treatment of morbid obesity, being used alone or as part of the duodenal switch surgery or even in intestinal bipartition (Santoro technique). When used alone has only a restrictive character. Method - Is proposed association of jejunoileal bypass to vertical gastroplasty, in order to give a metabolic component to the procedure and eventually empower it to medium and long term. Eight morbidly obese patients were operated after removal of adjustable gastric band or as a primary procedure associated to vertical banded gastroplasty with jejunoileal bypass laterolateral and anastomosis between the jejunum 80 cm from duodenojejunal angle and the ileum at 120 cm from ileocecal valve, by laparoscopy. Results - The patients presented themselves without complications both in trans or in the immediate postoperative period, and also in the months that followed. The evolution BMI showed a significant reduction ranging from 39.57 kg/m2 to 28 kg/m2. No patient reported diarrhea or malabsorptive disorder in HEADINGS - Sleeve gastrectomy. Jejunoileal the period. Conclusion - It can be offered a new therapeutic option, with restraining diversion. Obesity. Surgery. and metabolic aspects, in which there are no consequences as the ones founded in procedures with duodenal diversion or intestinal transit alterations. -

Medical Policy Bariatric Surgery
Medical Policy Bariatric Surgery Subject: Bariatric Surgery Background: Morbid obesity (also called clinically severe obesity) is a serious health condition that can interfere with basic physical functions such as breathing or walking and reduce life expectancy. Individuals who are morbidly obese are at greater risk for serious medical complications including hypertension, coronary artery disease, type 2 diabetes mellitus, sleep apnea, gastroesophageal reflux disease and osteoarthritis. While the immediate cause of obesity is caloric intake that persistently exceeds caloric output, a limited number of cases may also be caused by illnesses such as hypothyroidism, Cushing's disease, and hypothalamic lesions. Nonsurgical strategies for achieving weight loss and weight maintenance (e.g., caloric restriction, increased physical activity, behavioral modification) are recommended for most overweight and obese persons. Bariatric (weight loss) surgery is a major surgical intervention and is indicated for adults and adolescents who have completed bone growth and are morbidly obese. Bariatric surgery procedures modify the anatomy of the gastrointestinal tract and cause weight loss by restricting the amount of food the stomach can hold, causing malabsorption of nutrients. Bariatric procedures can often cause hormonal and metabolic changes that result from gastric and intestinal surgery. Contraindications for bariatric surgeries include cardiac complications, significant respiratory dysfunction, non- compliance with medical treatment, psychological disorders that a psychologist/psychiatrist determines are likely to exacerbate or interfere with long-term management, significant eating disorders, and severe hiatal hernia/gastroesophageal reflux. Authorization: Prior authorization is required for bariatric surgeries provided to members enrolled in commercial (HMO, POS, PPO) products. Bariatric procedures can only be done at fully accredited centers. -
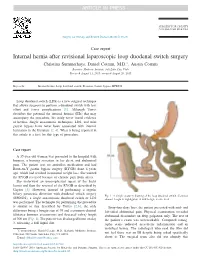
Internal Hernia After Revisional Laparoscopic Loop Duodenal Switch
Surgery for Obesity and Related Diseases ] (2015) 00–00 Case report Internal hernia after revisional laparoscopic loop duodenal switch surgery Christina Summerhays, Daniel Cottam, M.D.*, Austin Cottam Bariatric Medicine Institute, Salt Lake City, Utah Received August 11, 2015; accepted August 20, 2015 Keywords: Internal hernia; Loop duodenal switch; Revision; Gastric bypass; BPD/DS Loop duodenal switch (LDS) is a new surgical technique that allows surgeons to perform a duodenal switch with less effort and fewer complications [1]. Although Torres describes the potential for internal hernias (IHs) that may accompany the procedure, his study never found evidence of hernias. Single anastomotic techniques, LDS, and mini gastric bypass have never been associated with internal herniation in the literature [2–4]. What is being reported in this article is a first for this type of procedure. Case report A 35-year-old woman was presented to the hospital with burping, a burning sensation in her chest, and abdominal pain. The patient was on antireflux medication and had Roux-en-Y gastric bypass surgery (RYGB) done 6 years ago, which had resulted in minimal weight loss. She wanted the RYGB reversed because of chronic pain from ulcers. She underwent an uncomplicated repair of the hiatal hernia and then the reversal of the RYGB as described by Gagner [5]. However, instead of performing a regular biliary pancreatic diversion with duodenal switch surgery Fig. 1. A simple anatomy drawing of the loop duodenal switch. Common (BPD/DS), a single anastomosis duodenal switch or LDS channel length is highlighted. A 40F bougie is also used. was performed.