(ET) Dysfunction Eustachian Tube (ET) Dysfunction
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Lumps and Swellings
Clinical Oral medicine for the general practitioner: lumps and swellings Crispian Scully 1 his series of five papers summarises some of the most important oral medicine problems likely to be Tencountered by practitioners. Some are common, others rare. The practitioner cannot be expected to diagnose all, but has been trained to recognise oral health and disease, and should be competent to recognise normal variants, and common orofacial disorders. In any case of doubt, the practitioner is advised to seek a second opinion from a colleague. The series is not intended to be comprehensive in coverage either of the conditions encountered, or all aspects of Figure 1: Torus mandibularis. diagnosis or treatment: further details are available in standard texts, in the further reading section, or from the internet. The present article discusses aspects of lumps through fear, perhaps after hearing of someone with and swellings. ‘mouth cancer’. Thus some individuals discover and worry about normal anatomical features such as tori, the parotid Lumps and swellings papilla, foliate papillae on the tongue, or the pterygoid Lumps and swellings in the mouth are common, but of hamulus. The tongue often detects even a very small diverse aetiologies (Table 1), and some represent swelling, or the patient may first notice it because it is sore malignant neoplasms. Therefore, this article will discuss (Figure 1). In contrast, many oral cancers are diagnosed far lumps and swellings in general terms, but later focus on too late, often after being present several months, usually the particular problems of oral cancer and of orofacial because the patient ignores the swelling. -

WHAT HAPPENED? CDR, a 24-Year-Old Chinese Male
CHILDHOOD DEVELOPMENTAL SCREENING 2020 https://doi.org/10.33591/sfp.46.5.up1 FINDING A MASS WITHIN THE ORAL CAVITY: WHAT ARE THE COMMON CAUSES AND 4-7 GAINING INSIGHT: WHAT ARE THE ISSUES? In Figure 2 below, a list of masses that could arise from each site Figure 3. Most common oral masses What are the common salivary gland pathologies Salivary gland tumours (Figure 7) commonly present as channel referrals to appropriate specialists who are better HOW SHOULD A GP MANAGE THEM? of the oral cavity is given and elaborated briey. Among the that a GP should be aware of? painless growing masses which are usually benign. ey can equipped in centres to accurately diagnose and treat these Mr Tan Tai Joum, Dr Marie Stella P Cruz CDR had a slow-growing mass in the oral cavity over one year more common oral masses are: torus palatinus, torus occur in both major and minor salivary glands but are most patients, which usually involves surgical excision. but sought treatment only when he experienced a sudden acute mandibularis, pyogenic granuloma, mucocele, broma, ere are three pairs of major salivary glands (parotid, commonly found occurring in the parotid glands. e most 3) Salivary gland pathology may be primary or secondary to submandibular and sublingual) as well as hundreds of minor ABSTRACT onset of severe pain and numbness. He was fortunate to have leukoplakia and squamous cell carcinoma – photographs of common type of salivary gland tumour is the pleomorphic systemic causes. ese dierent diseases may present with not sought treatment as it had not caused any pain. -

Abscesses Apicectomy
BChD, Dip Odont. (Mondchir.) MBChB, MChD (Chir. Max.-Fac.-Med.) Univ. of Pretoria Co Reg: 2012/043819/21 Practice.no: 062 000 012 3323 ABSCESSES WHAT IS A TOOTH ABSCESS? A dental/tooth abscess is a localised acute infection at the base of a tooth, which requires immediate attention from your dentist. They are usually associated with acute pain, swelling and sometimes an unpleasant smell or taste in the mouth. More severe infections cause facial swelling as the bacteria spread to the nearby tissues of the face. This is a very serious condition. Once the swelling begins, it can spread rapidly. The pain is often made worse by drinking hot or cold fluids or biting on hard foods and may spread from the tooth to the ear or jaw on the same side. WHAT CAUSES AN ABSCESS? Damage to the tooth, an untreated cavity, or a gum disease can cause an abscessed tooth. If the cavity isn’t treated, the inside of the tooth can become infected. The bacteria can spread from the tooth to the tissue around and beneath it, creating an abscess. Gum disease causes the gums to pull away from the teeth, leaving pockets. If food builds up in one of these pockets, bacteria can grow, and an abscess may form. An abscess can cause the bone around the tooth to dissolve. WHY CAN'T ANTIBIOTIC TREATMENT ALONE BE USED? Antibiotics will usually help the pain and swelling associated with acute dental infections. However, they are not very good at reaching into abscesses and killing all the bacteria that are present. -

Recognition and Management of Oral Health Problems in Older Adults by Physicians: a Pilot Study
J Am Board Fam Pract: first published as 10.3122/jabfm.11.6.474 on 1 November 1998. Downloaded from BRIEF REPORTS Recognition and Management of Oral Health Problems in Older Adults by Physicians: A Pilot Study Thomas V. Jones, MD, MPH, Mitchel J Siegel, DDS, andJohn R. Schneider, A1A Oral health problems are among the most com of the nation's current and future health care mon chronic health conditions experienced by needs, the steady increase in the older adult popu older adults. Healthy People 2000, an initiative to lation, and the generally high access elderly per improve the health of America, has selected oral sons have to medical care provided by family health as a priority area. l About 11 of 100,000 physicians and internists.s,7,8 Currently there is persons have oral cancer diagnosed every year.2 very little information about the ability of family The average age at which oral cancer is diagnosed physicians or internists, such as geriatricians, to is approximately 65 years, with the incidence in assess the oral health of older patients. We con creasing from middle adulthood through the sev ducted this preliminary study to determine how enth decade of life. l-3 Even though the mortality family physicians and geriatricians compare with rate associated with oral cancer (7700 deaths an each other and with general practice dentists in nually)4 ranks among the lowest compared with their ability to recognize, diagnose, and perform other cancers, many deaths from oral cancer initial management of a wide spectrum of oral might be prevented by improved case finding and health problems seen in older adults. -

Oral Health and Disease
Downloaded from bmj.com on 19 August 2005 ABC of oral health: Oral health and disease Ruth Holt, Graham Roberts and Crispian Scully BMJ 2000;320;1652-1655 doi:10.1136/bmj.320.7250.1652 Updated information and services can be found at: http://bmj.com/cgi/content/full/320/7250/1652 These include: Rapid responses One rapid response has been posted to this article, which you can access for free at: http://bmj.com/cgi/content/full/320/7250/1652#responses You can respond to this article at: http://bmj.com/cgi/eletter-submit/320/7250/1652 Email alerting Receive free email alerts when new articles cite this article - sign up in the box at service the top right corner of the article Topic collections Articles on similar topics can be found in the following collections Dentistry and Oral Medicine (79 articles) Notes To order reprints of this article go to: http://www.bmjjournals.com/cgi/reprintform To subscribe to BMJ go to: http://bmj.bmjjournals.com/subscriptions/subscribe.shtml Clinical review Downloaded from bmj.com on 19 August 2005 ABC of oral health Oral health and disease Ruth Holt, Graham Roberts, Crispian Scully A healthy dentition and mouth is important to both quality of life and nutrition, and oral disease may affect systemic health, as Enamel covering crown Gingival crevice discussed in later articles in this series. (gingival sulcus) Dentine Development of the dentition Gingiva Pulp chamber Teeth form mainly from neuroectoderm and comprise a crown of insensitive enamel surrounding sensitive dentine and a root Periodontal ligament that has no enamel covering. -

QUICK ORAL HEALTH FACTS ABOUT the YOUNG Dr Ng Jing Jing, Dr Wong Mun Loke
ORAL health IN PRIMARY CARE UNIT NO. 2 QUICK ORAL HEALTH FACTS ABOUT THE YOUNG Dr Ng Jing Jing, Dr Wong Mun Loke ABSTRACT Table 1. Eruption sequence of Primary Dentition This article sheds light on the sequence of teeth eruption Primary Upper Teeth Primary Lower Teeth in the young and teething problems; highlights the importance and functions of the primary dentition and Central Incisors: 8-13 months Central Incisors: 6-10 months provides a quick overview of common developmental Lateral Incisors: 8-13 months Lateral Incisors: 10-16 months dental anomalies and other dental conditions in Canines: 16-23 months Canines: 16-23 months children. First Molars: 16-23 months First Molars: 13-19 months Second Molars: 25-33 months Second Molars: 23-31 months SFP2011; 37(1) Supplement : 10-13 Table 2. Eruption sequence of Adult Dentition Adult Upper Teeth Adult Lower Teeth INTRODUCTION Central Incisors: 7-8 years Central Incisors: 6-7 years The early years are always full of exciting moments as we observe Lateral Incisors: 8-9 years Lateral Incisors: 7-8 years our children grow and develop. One of the most noticeable Canines: 11-12 years Canines: 9-10 years aspects of their growth and development is the eruption of First Premolars: 10-11 years First Premolars: 10-11 years teeth. The first sign of a tooth in the mouth never fails to Second Premolars: 11-12 years Second Premolars: 11-12 years attract the attention of the parent and child. For the parent, it First Molars: 6-7 years First Molars: 6-7 years marks an important developmental milestone of the child but Second Molars: 12-13 years Second Molars: 11-13 years for the child, it can be a source of irritation brought on by the Third Molars: 18-25 years Third Molars: 18-25 years whole process of teething. -

Concurrence of Torus Palatinus, Torus Mandibularis and Buccal Exostosis Sarfaraz Khan1, Syed Asif Haider Shah2, Farman Ali3 and Dil Rasheed4
CASE REPORT Concurrence of Torus Palatinus, Torus Mandibularis and Buccal Exostosis Sarfaraz Khan1, Syed Asif Haider Shah2, Farman Ali3 and Dil Rasheed4 ABSTRACT Torus palatinus (TP), torus mandibularis (TM), and buccal exostosis are localised, benign, osseous projections, occurring in maxilla and mandible. Etiology is multifactorial and not well established. Tori and exostoses have been associated with parafunctional occlusal habits, temporomandibular joint (TMJ) disorders, migraine and consumption of fish. Concurrence of TP, TM, and exostosis in the same individual is very rare. Concurrence of TP and TM has not been reported from Pakistan. We report a case of a 22-year female patient manifesting concurrence of TP, bilateral TM, and maxillary buccal exostoses; with possible association of abnormal occlusal stresses and use of calcium and vitamin D supplements. Key Words: Torus palatinus. Torus mandibularis. Exostoses. INTRODUCTION upper teeth, for the last one year. She noticed a gradual Torus palatinus (TP) is a localised, benign, osseous increase in the severity of her symptoms. The patient projection in midline of the hard palate. Torus denied any associated pain or ulceration. She had mandibularis (TM) is a benign, bony protuberance, on remained under orthodontic treatment for 2 years for the lingual aspect of the mandible, usually bilaterally, at correction of her crooked teeth. After completion of the the canine-premolar area, above the mylohyoid line. treatment, she was advised to wear removable retainer appliance; but owing to her admittedly non-compliant Exostoses are multiple small bony nodules occurring attitude towards treatment, malalignment of her teeth along the buccal or palatal aspects of maxilla and buccal recurred within the next 2 years. -

Torus Palatinus and Torus Mandibularis in Edentulous Patients
Torus Palatinus and Torus Mandibularis in Edentulous Patients Abstract Aim: To determine the prevalence of tori in Jordanian edentulous patients, the sex variation in their distribution, and their clinical characteristics. Methods: Three hundred and thirty eight patients were examined in the Prosthodontic Clinic in the Department of Restorative Dentistry at Jordan University of Science and Technology. The location, extent, and clinical presentation of tori were recorded related to the age and sex of patients. Results: The overall prevalence of tori was 13.9%. The prevalence of torus palatinus was 29.8% (14/47), while that of torus mandibularis was significantly higher 42.6%(20/47). Both types of tori were associated with each other in 27.7% of cases (13/47). Conclusions: There was no significant difference in the prevalence of tori between males and females. There seems to be a strong association between mandibular and palatal tori. Keywords: Tori, torus palatinus, torus mandibularis Citation: Al Quran FAM, Al-Dwairi ZN. Torus Palatinus and Torus Mandibularis in Edentulous Patients. J Contemp Dent Pract 2006 May;(7)2:112-119. 1 The Journal of Contemporary Dental Practice, Volume 7, No. 2, May 1, 2006 Introduction Tori are benign anatomical bony prominences occurring in the hard palate and the lingual aspect of the mandible. Although they are generally asymptomatic, surgical intervention may be required in some cases for prosthodontic purposes.1 Currently, tori are considered to be an interplay of genetic and environmental factors with a familial occurrence suggesting autosomal dominant inheritance with reduced penetrance.2 Suzuki and Saki10 suggested the two anomalies are due to the same autosomal dominant gene. -
DIAGNOSIS ICD-9 ICD-10 a Abscess
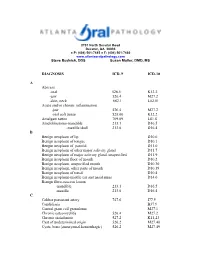
2701 North Decatur Road Decatur, GA 30033 ● P: (404) 501-7445 ● F: (404) 501-7460 www.atlantaoralpathology.com Steve Budnick, DDS Susan Muller, DMD, MS DIAGNOSIS ICD-9 ICD-10 A Abscess -oral 528.5 K12.2 -jaw 526.4 M27.2 -skin, neck 682.1 L02.01 Acute and/or chronic inflammation -jaw 526.4 M27.2 -oral soft tissue 528.00 K12.2 Amalgam tattoo 709.09 L81.8 Ameloblastoma-mandible 213.1 D16.5 -maxilla/skull 213.0 D16.4 B Benign neoplasm of lip D10.0 Benign neoplasm of tongue D10.1 Bengin neoplasm of parotid D11.0 Benign neoplasm of other major salivary gland D11.7 Benign neoplasm of major salivary gland, unspecified D11.9 Benign neoplasm floor of mouth D10.2 Benign neoplasm, unspecified mouth D10.30 Benign neoplasm, other parts of mouth D10.39 Benign neoplasm of tonsil D10.4 Benign neoplasm-middle ear and nasal sinus D14.0 Benign fibro-osseous lesion -mandible 213.1 D16.5 -maxilla 213.0 D16.4 C Caliber persistent artery 747.6 I77.9 Candidiasis B37.9 Central giant cell granuloma M27.1 Chronic osteomyelitis 526.4 M27.2 Chronic sialadenitis 527.2 K11.23 Cyst of undetermined origin 526.2 M27.40 Cysts, bone{aneurysmal,hemorrhagic) 526.2 M27.49 D Dental follicle (enlarged) 526.9 M27.0 Dentigerous cyst 526.0 K09.0 Dental granuloma 526.4 M27.2 Developmental cyst NOS 526.1 K09.0 Dysplasia – mid 528.79 K13.29 -moderate 528.79 K13.29 -severe 528.79 K13.29 E Epidermoid cyst – mouth 528.4 K09.9 - skin 706.2 L72.0 Epulis fissuratum 528.9 K13.70 Eruption cyst 526.0 K09.0 Erythema migrans 529.1 K14.1 Erythema multiforme 695.1 L51.8 Exostosis 526.81 M27.8 F -

Description Concept ID Synonyms Definition
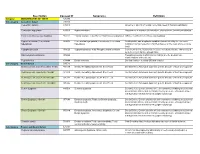
Description Concept ID Synonyms Definition Category ABNORMALITIES OF TEETH 426390 Subcategory Cementum Defect 399115 Cementum aplasia 346218 Absence or paucity of cellular cementum (seen in hypophosphatasia) Cementum hypoplasia 180000 Hypocementosis Disturbance in structure of cementum, often seen in Juvenile periodontitis Florid cemento-osseous dysplasia 958771 Familial multiple cementoma; Florid osseous dysplasia Diffuse, multifocal cementosseous dysplasia Hypercementosis (Cementation 901056 Cementation hyperplasia; Cementosis; Cementum An idiopathic, non-neoplastic condition characterized by the excessive hyperplasia) hyperplasia buildup of normal cementum (calcified tissue) on the roots of one or more teeth Hypophosphatasia 976620 Hypophosphatasia mild; Phosphoethanol-aminuria Cementum defect; Autosomal recessive hereditary disease characterized by deficiency of alkaline phosphatase Odontohypophosphatasia 976622 Hypophosphatasia in which dental findings are the predominant manifestations of the disease Pulp sclerosis 179199 Dentin sclerosis Dentinal reaction to aging OR mild irritation Subcategory Dentin Defect 515523 Dentinogenesis imperfecta (Shell Teeth) 856459 Dentin, Hereditary Opalescent; Shell Teeth Dentin Defect; Autosomal dominant genetic disorder of tooth development Dentinogenesis Imperfecta - Shield I 977473 Dentin, Hereditary Opalescent; Shell Teeth Dentin Defect; Autosomal dominant genetic disorder of tooth development Dentinogenesis Imperfecta - Shield II 976722 Dentin, Hereditary Opalescent; Shell Teeth Dentin Defect; -

Prevalence of Torus Mandibularis in Viking Age Icelanders
Richter and Eliasson ORIGINAL SCIENTIFIC PAPER Prevalence of Torus Mandibularis in Viking Age Icelanders • Richter S, Eliasson ST • University of Iceland, Faculty of Odontology, Vatnsmyravegi 16, 101 Reykjavik, Iceland Address for correspondence: Svend Richter University of Iceland Faculty of Odontology Vatnsmyravegi 16, 101 Reykjavik, Iceland E-mail: [email protected] Bull Int Assoc Paleodont. 2012;6(2):40-50. Abstract Of 48 available crania dated older than 1104AD, from the archaeological site of Skeljastadir in Thorsardalur, Iceland, 24 (50%) had torus mandibularis. There was no sex difference observed. The prevalence is similar among other populations in the northern hemisphere from the same time period. According to a number of authors, environmental and functional factors, particularly high masticatory activity, play a predominant part in the etiology. People from artic- and subartic areas survived on an animal diet, mostly fish and meat, but people living further south in a more temperate climate had more of an agricultural diet. Higher prevalence was found in the age group above 36 years than in the group 35 years and below. The majority of the tori were small or medium in size. The most frequently occurring variant was the multiple bilateral form, followed by the multiple unilateral form. The prevalence of torus mandibularis in the study was much higher than found in modern Iceland. Keywords: Torus Mandibularis; Viking Age Icelanders Introduction Torus mandibularis is a bony protruberance or exostosis on the lingual surface of the mandible, above the mylohyoid ridge, generally situated in the canine and the premolar region. The trait can occur unilaterally or bilaterally, with symmetrical occurrence visible as either as a single elevation or Bull Int Assoc Paleodont. -

Partnering General Practitioners to Advance Community Oral Health
E D I T O R I A L PartNERING GENERAL PRACTITIONERS to ADVANCE CoMMUNITY ORAL Health SFP2011; 37(1) Supplement : 4 In Unit 3 – “Recognising Common Adult Oral Conditions” – Dr Rahul Nair, Dr Adeline Wong, Dr Joanna Ngo and Dr Wong Mun Loke highlight the common oral problems in the Oral health has long been overlooked in the medical adult population which are dental caries, and periodontal community. We are not well versed in anything more disease. The prevention of oral diseases has now taken on than the rudimentary aspects of oral health. The medical the strategy of targeting a small set of risk factors that are school curriculum is also lacking in coverage of this area of important for a large number of diseases. This Common Risk medicine. This is despite the fact that oral health and hygiene Factor Approach aims to reduce risk factors in diet, stress, is often one of the first indicators of the general health of hygiene, smoking, alcohol, lack of exercise and injuries to the individual, and of disease. prevent the onset of a range of diseases including dental caries and periodontal disease. Many of us in Family Practice see the very young in our daily work. Neonates, infants and toddlers make up, for some of In Unit 4 – “Ageing and its Influence on the Oral us, a large part of our clinical responsibilities. We are often Environment” – Dr Hilary Thean and Dr Wong Mun Loke faced with questions from anxious parents such as teething cover issues which are specific to the ageing process and issues, new tooth eruption, tongue tie and the list goes on.