Suctioning Nonvigorous Infants Through
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

PLANNED OUT-OF-HOSPITAL BIRTH Approved 11/12/15
HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: PLANNED OUT-OF-HOSPITAL BIRTH Approved 11/12/15 HERC COVERAGE GUIDANCE Planned out-of-hospital (OOH) birth is recommended for coverage for women who do not have high- risk coverage exclusion criteria as outlined below (weak recommendation). This coverage recommendation is based on the performance of appropriate risk assessments1 and the OOH birth attendant’s compliance with the consultation and transfer criteria as outlined below. Planned OOH birth is not recommended for coverage for women who have high risk coverage exclusion criteria as outlined below, or when appropriate risk assessments are not performed, or where the attendant does not comply with the consultation and transfer criteria as outlined below (strong recommendation). High-risk coverage exclusion criteria: Complications in a previous pregnancy: Maternal surgical history Cesarean section or other hysterotomy Uterine rupture Retained placenta requiring surgical removal Fourth-degree laceration without satisfactory functional recovery Maternal medical history Pre-eclampsia requiring preterm birth Eclampsia HELLP syndrome Fetal Unexplained stillbirth/neonatal death or previous death related to intrapartum difficulty Baby with neonatal encephalopathy Placental abruption with adverse outcome Complications of current pregnancy: Maternal Induction of labor Prelabor rupture of membranes > 24 hours 1 Pre-existing chronic hypertension; Pregnancy-induced hypertension with diastolic blood pressure greater than -

Aspirin Use to Prevent Preeclampsia and Related Morbidity and Mortality: an Evidence Update for the U.S
Evidence Synthesis Number 205 Aspirin Use to Prevent Preeclampsia and Related Morbidity and Mortality: An Evidence Update for the U.S. Preventive Services Task Force Prepared for: Agency for Healthcare Research and Quality U.S. Department of Health and Human Services 5600 Fishers Lane Rockville, MD 20857 www.ahrq.gov Contract No. HHSA-290-2015-00007-I-EPC5, Task Order No. 6 Prepared by: Kaiser Permanente Research Affiliates Evidence-based Practice Center Kaiser Permanente Center for Health Research Portland, OR Investigators: Jillian T. Henderson, PhD, MPH Kimberly K. Vesco, MD, MPH Caitlyn A. Senger, MPH Rachel G. Thomas, MPH Nadia Redmond, MSPH AHRQ Publication No. 21-05274-EF-1 February 2021 This report is based on research conducted by the Kaiser Permanente Research Affiliates Evidence-based Practice Center (EPC) under contract to the Agency for Healthcare Research and Quality (AHRQ), Rockville, MD (Contract No. HHSA-290-2015-00007-I-EPC5, Task Order No. 6). The findings and conclusions in this document are those of the authors, who are responsible for its contents; the findings and conclusions do not necessarily represent the views of AHRQ. Therefore, no statement in this report should be construed as an official position of AHRQ or of the U.S. Department of Health and Human Services. The information in this report is intended to help health care decisionmakers—patients and clinicians, health system leaders, and policymakers, among others—make well-informed decisions and thereby improve the quality of healthcare services. This report is not intended to be a substitute for the application of clinical judgment. Anyone who makes decisions concerning the provision of clinical care should consider this report in the same way as any medical reference and in conjunction with all other pertinent information (i.e., in the context of available resources and circumstances presented by individual patients). -

Rotation Objectives
Rotation Objectives Obstetrical Ward (Caseroom) Medical Expert 1. Be able to diagnose and manage the following antenatal complications a. Gestational Hypertension and preeclampsia b. Gestational diabetes c. Premature rupture of membranes d. Antepartum Bleeding (after 20 weeks gestation) e. Maternal hypothyroidism f. Intrauterine growth retardation 2. Demonstrate the following skills during antenatal visits: a. Fundal height measurements, b. Leopold manoeuvres, c. Fetal Doppler heart monitoring, d. Cervical exam 3. Be able to assess and triage risk associated with a trial of labour after Cesarian 4. Be able to assess the factors that will influence the decision to induce labour 5. Be able to perform normal risk labour and vaginal deliveries a. Demonstrate accurate cervical exams to determine the stage of labour b. Be able to evaluate for spontaneous rupture of membranes c. Fetal surveillance during labour d. Be able to diagnose non-cephalic fetal presentation using appropriate techniques 6. Be able to recognize and manage the following complications of labour and delivery a. Labour dystocia b. Shoulder dystocia c. Postpartum hemorrhage d. Perineal lacerations e. Vacuum assisted delivery f. Non-cephalic presentation g. Peripartum fever 7. Be able to manage pain in labour Postnatal and neonatal Care *The following objectives are relevant to services in which the resident is responsible for newborn assessments 8. Be able to describe and perform neonatal resuscitation 9. Demonstrate a comprehensive evaluation of a newborn in the first few days of life that will identify complications specific to the newborn period a. Hypoglycemia b. Hyperbilirubinemia c. Neonatal respiratory distress d. Congenital anomalies 10. Be able to provide support for breastfeeding, and anticipatory guidance for new mothers 11. -

Antepartum Haemorhhage(Aph)
ANTEPARTUM HAEMORHHAGE(APH) MAJ SAMIA NASREEN CLASSIFIED GYNAECOLOGIST CMH OBJECTIVES OF PRESENTATION • Identify serious causes of vaginal bleeding in the second half of pregnancy • Describe a systematic approach to identify the cause of bleeding • Describe specific treatment options based on diagnosis DEFINITION • Vaginal bleeding after 24weeks and before the delivery of the fetus. • It complicates (3-4%) of all pregnancies. • It is an obstetric emergency because it endanger the life of both the mother and fetus. • Hemorrhage remain the most frequent cause of maternal deaths. • Mild= <50 mL loss of blood, Major= 50-1000mL loss, Massive= >1000mL loss. • Bleeding >1 occasion regarded as recurrent APH. Causes of Late Pregnancy Bleeding • Placenta previa • Placental abruption • Uterine scar disruption Life Threatening • Ruptured vasa previa • Cervical polyp • Bloody show/cervical change • Cervicitis or cervical ectropion • Vaginal trauma • Cervical cancer INITIAL MANAGEMENT • Same initial steps regardless of etiology in all cases of APH • Assess vital signs, circulatory stability • Secure intravenous access, administer fluids HISTORY & EXAMINATION • Targeted history and physical • Abdominal examination for estimated fetal weight (EFW), estimated gestational age (EGA), and fetal presentation Localize tenderness Palpate for uterine contractions • Gentle speculum examination is safe • NO digital vaginal exam unless placental location is known DIAGNOSTIC EVALUATION • Continuous electronic fetal monitoring (CTG) and tocodynamometry • Ultrasound for placental location, presence of clots, and fetal presentation • Obtain baseline laboratory tests Complete blood count Blood type and antibody screen Consider: coagulation studies, blood urea nitrogen (BUN), creatinine, liver function testing, and type and cross • Prepare for possible emergent cesarean delivery PLACENTA PREVIA Grading of placenta previa Grade .1 (lateral placenta): The placenta implanted in the lower uterine segment but not reach the internal os. -

Third Trimester Bleeding
Third Trimester Bleeding Nicole Sprawka, MD Maternal Fetal Medicine Causes of antepartum bleeding Labor Cervical bleeding Placental abruption Placenta previa Bleeding from a site above the cervix Vasa previa Bleeding in Labor Bleeding during labor is common Effacement and dilation of the cervix causes tearing of small vessels Often called “bloody show” Cervical bleeding Cervix my be friable due pregnancy or infection Cervical polyps Ask about recent intercourse Placental abruption Separation from it’s site of implantation before delivery Occurs 1 in 200 deliveries Cause of fetal death 1 in 1600 10% of all 3rd trimester stillbirth due to abruption Pathology of abruption Initiated by hemorrhage in to the decidua basalis The decidual hematoma leads to separation, compression, and destruction of the adjacent placenta In the early stages there may be no clinical symptoms The blood may dissect the membranes from the uterine wall and escape through the cervix Placental abruption The blood can be retained between the placenta and uterus resulting in a concealed abruption Concealed abruption likely go undiagnosed till delivery and are associated with a higher rate of DIC Risk factors for abruption Prior abruption 10 - 25 Preterm ruptured membranes 2.4 – 4.9 Preeclampsia 2.1 – 4.0 Chronic hypertension 1.8 – 3.0 Multifetal gestation 2.1 Polyhydramnios 2.0 Cigarette smoking 1.4 – 1.9 Increased age and parity 1.3 – 1.5 Cocaine use Uterine fibroids (esp. if behind placental implantation site) Hypertension and abruption Most common -

Management of Obstetric Hemorrhage
MANAGEMENT OF OBSTETRIC HEMORRHAGE AMITAVA RUDRA*, SUMAN CHATTERJEE**, SAIKAT SENGUPTA***, RAVI WANKHEDE***, BIswaJIT NANDI****, GAURAB MAITRA***, AND JAYANTA MITRA**** Abstract Major obstetric hemorrhage is an extremely challenging obstetric emergency associated with significant morbidity and mortality. Pharmacological treatment of uterine atony has not altered much in recent years apart from the increasing use of misoprostol, although controversy surrounds its advantages over other uterotonics. Placenta accreta is becoming more common, a sequel to the rising caesarean section rate. Interventional radiology may reduce blood loss in these cases. Uterine compression sutures, intrauterine tamponade balloons and cell salvage have been introduced in the last decade. Keywords: Antepartum hemorrhage, postpartum hemorrhage, uterotonics. Obstetric hemorrhage is the world’s leading cause of maternal mortality1. Postpartum hemorrhage (PPH) accounts for the majority of these deaths1. The global maternal ratio of 402 deaths per 100,000 live births2 obscures the fact that 99% of these deaths occur in the developing world3. In addition, even in many developed countries, it is also the maternal complication for which the highest rate of substandard care is observed4. Furthermore, Zeeman’s5 study of obstetric critical care provision identifies hemorrhage as one of the most frequent reasons for admission to intensive care unit. Major obstetric hemorrhage accounts for 30% of cases6. Obstetric hemorrhage is often sudden, unexpected, and may be associated with coagulopathy. Blood loss can be notoriously difficult to assess in obstetric bleeds. Bleeding may sometimes be concealed and the presence of amniotic fluid makes accurate estimation challenging. Hence, early recognition and treatment are essential to ensure the best outcome. Therefore, it is important to have a thorough knowledge of the pathophysiology, etiology, and management strategies of obstetric hemorrhage. -

Board-Review-Series-Obstetrics-Gynecology-Pearls.Pdf
ObstetricsandGynecology BOARDREVIEW Third Edition Stephen G. Somkuti, MD, PhD Associate Professor Department of Obstetrics and Gynecology and Reproductive Sciences Temple University School of Medicine School Philadelphia, Pennsylvania Director, The Toll Center for Reproductive Sciences Division of Reproductive Endocrinology Department of Obstetrics and Gynecology Abington Memorial Hospital Abington Reproductive Medicine Abington, Pennsylvania New York Chicago San Francisco Lisbon London Madrid Mexico City Milan New Delhi San Juan Seoul Singapore Sydney Toronto Copyright © 2008 by the McGraw-Hill Companies, Inc. All rights reserved. Manufactured in the United States of America. Except as permitted under the United States Copyright Act of 1976, no part of this publication may be reproduced or distributed in any form or by any means, or stored in a database or retrieval system, without the prior written permission of the publisher. 0-07-164298-6 The material in this eBook also appears in the print version of this title: 0-07-149703-X. All trademarks are trademarks of their respective owners. Rather than put a trademark symbol after every occurrence of a trademarked name, we use names in an editorial fashion only, and to the benefit of the trademark owner, with no intention of infringement of the trademark. Where such designations appear in this book, they have been printed with initial caps. McGraw-Hill eBooks are available at special quantity discounts to use as premiums and sales promotions, or for use in corporate training programs. For more information, please contact George Hoare, Special Sales, at [email protected] or (212) 904-4069. TERMS OF USE This is a copyrighted work and The McGraw-Hill Companies, Inc. -

Nursethink® for Students NCLEX-RN Conceptual Review Guide
NurseThink® for Students NCLEX-RN Conceptual Review Guide Clinical-Based for Next Gen Learning ONLY,Resale / Concept-Based USEBONUS: Mobile-Ready Quizzes and Videos Testing SuccessSample Over 1,000 Questions for 35 Patient Assignments Clinical Judgment Audio/Video for Stream/Download Prioritization Power Over 160 Exemplars for Prioritization Power Clinical Judgment Questions Focus on the New NCLEX® NurseThink® ThroughoutNot Tim J. Bristol Judith W. Herrman Winsome Stephenson PhD, RN, CNE, ANEF, FAAN PhD, RN, ANEF, FAAN PhD, RN, CNE NurseThink® for Students: The NoteBook Clinical-Based Note Taking Helps You Save Time Studying NurseThink® for Students: The NoteBook is a tool that develops clinical judgment in students by habitually applying a methodical way of analyzing information. This is a product that has shown consistent student success through outcome measures! Order Today! Visit NurseThink.com to learn more and order. ONLY,Resale / Thank you for purchasing the NurseThinkUSE ® for Students: ® Sample NCLEX-RN Conceptual Reviewfor Guide. Don’t forget to use the online resources! Step 1: Scratch off the code ý Over 1,000 Questions Step 2: Visit nursethink.com/NCLEX-RN-book ý 35 Patient Assignments Not to register your book ý Audio/Video to Stream/Download Step 3: Study, study, study! Your Access Code: Gently scratch to reveal access code. This access code is only valid for one registration. If the code is visible, it may have been used and cannot be re-used for registration. Once the access code has been exposed, the book cannot be returned. For technical assistance, please contact [email protected] NurseThink® for Students NCLEX-RN® Conceptual Review Guide Clinical-Based for Next Gen Learning ONLY,Resale / Tim J. -

Placental Contribution to Obstetric Hemorrhage
PLACENTAL CONTRIBUTION TO OBSTETRIC HEMORRHAGE Ware Branch, MD Medical Director of Women and Newborn Clinical Program for the Urban Central Region of Intermountain Healthcare Professor of Obstetrics and Gynecology, University of Utah, Salt Lake City Third Stage of Labor Sudden decrease in uterine size and area of implantation site Formation of retroplacental hematoma Uterine contraction Secondary clot formation Placental Contribution to Obstetric Hemorrhage • Placental abruption • Placenta previa • Placenta accreta (spectrum) Placental Contribution to Obstetric Hemorrhage • Uterine bleeding after 20 weeks complicates 5-10% of pregnancies; of these: – Abruption ~ 15% – Previa ~ 10% – Accreta ~? – Other (local / focal bleeding) Placental Contribution to Obstetric Hemorrhage Placental Abruption • Bleeding at the decidual-placental interface (maternal vessels in decidua basalis) à premature separation • Occurs in about 0.5-1% of pregnancies • Adverse outcomes: – Fetus/neonate: FGR, LBW, PTB, HIE, perinatal death – Mother: DIC, transfusion, hysterectomy, renal failure, death Placental Contribution to Obstetric Hemorrhage Placental Abruption • Estimated to be the cause of ~10% of preterm births and ~10% of perinatal deaths • Maternal mortality – In about about 1% of serious abruption cases – Attributable cause of 7 maternal deaths in UK, 2000-2005 Placental Contribution to Obstetric Hemorrhage Placental Abruption Risk Factors for Abruption Demographic or Historical Current Medical Behavioral •Prior abrupon •Hypertensive dise ase • Maternal age -

Impact of Placenta Previa with Placenta Accreta Spectrum Disorder on Fetal Growth
Ultrasound Obstet Gynecol 2019; 54: 643–649 Published online in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.20244 Impact of placenta previa with placenta accreta spectrum disorder on fetal growth E. JAUNIAUX1 ,I.DIMITROVA2, N. KENYON3, M. MHALLEM4,N.A.KAMETAS2, N. ZOSMER2, C. HUBINONT4,K.H.NICOLAIDES2 andS.L.COLLINS3 1EGA Institute for Women’s Health, Faculty of Population Health Sciences, University College London, London, UK; 2Fetal Medicine Research Institute, King’s College Hospital, Harris Birthright Research Centre, London, UK; 3Nuffield Department of Women’s and Reproductive Health, University of Oxford, Oxford, UK; 4Department of Obstetrics, Saint Luc University Hospital, Universite´ Catholique de Louvain, Brussels, Belgium KEYWORDS: birth weight; fetal growth; increta; percreta; placenta previa accreta CONTRIBUTION and invasive (n = 47) PAS subgroups, and 146 women What are the novel findings of this work? with placenta previa without PAS disorder. There Placenta previa accreta does not impact on fetal growth. were 64 controls with a low-lying placenta. There was no significant difference in the incidence of ≤ th What are the clinical implications of this work? small-for-gestational age (SGA) (birth weight 10 As placenta previa accreta does not pose a risk to fetal percentile) and large-for-gestational age (LGA) (birth ≥ th development other than those linked to premature birth, weight 90 percentile) between the study groups. serial ultrasound examinations should not be required to Median gestational age at diagnosis was significantly evaluate fetal wellbeing in the second half of pregnancy lower in pregnancies with placenta previa without PAS = in women presenting with placenta previa accreta. -

Placental Abruption an Obstetric Emergency: Management and Outcomes in 180 Cases
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Devabhaktuni P et al. Int J Reprod Contracept Obstet Gynecol. 2020 Aug;9(8):3188-3195 www.ijrcog.org pISSN 2320-1770 | eISSN 2320-1789 DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20203294 Original Research Article Placental abruption an obstetric emergency: management and outcomes in 180 cases Pratibha Devabhaktuni1*, Aruna Kumari Konkathi2 1Department of Obstetrics and Gynecology, Modern Government Maternity Hospital/Osmania Medical College, Hyderabad, Telangana, India 2Department of Obstetrics and Gynecology, Niloufer Hospital for Women and Children/Osmania Medical College, Hyderabad, Telangana, India Received: 13 July 2020 Accepted: 18 July 2020 *Correspondence: Dr. Pratibha Devabhaktuni, E-mail: [email protected] Copyright: © the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Background: During a period of eight months, 180 cases of abruption that occurred from January 2007 to August 2007 at GMH, Nayapool, Hyderabad were analysed. Total number of deliveries during the study period of eight months were 14004. Incidence of abruption cases delivered was - 1.3%. In this series 88% were unbooked in our hospital, were referrals. Objective of this study was to study maternal fetal outcome of placental abruption. Methods: Initial clinical assessment, investigations for maternal fetal wellbeing, expedite delivery, manage complications as per accepted protocol. In this series of cases, ARM was done in 85 cases (47.22%), ARM was done and oxytocin drip was started in 36 (20%), ARM was done and PGE1 tablet 25 mcg. -
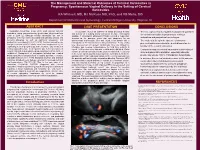
ABSTRACT Introduction the Management and Maternal Outcomes of Cervical Varicosities in Pregnancy: Spontaneous Vaginal Delivery I
The Management and Maternal Outcomes of Cervical Varicosities in Pregnancy: Spontaneous Vaginal Delivery in the Setting of Cervical Varicosities KA Whitsell, MD, MJ McKuen MD, PhD, and VB Mello, DO Department of Obstetrics and Gynecology, Central Michigan University, Saginaw, MI ABSTRACT CASE PRESENTATION CONCLUSIONS Postpartum hemorrhage is one of the most common maternal A Caucasian 18-year-old G2P0101 at 30w2d presented to labor • There is a great need to establish management guidelines morbidities, which has increased by greater than fifty percent from and delivery at a outlying facility with pelvic pressure and vaginal for cervical varicosities in pregnancy to minimize 1993 to 2014 [2]. Although cervical varicosities are rare in spotting. A transvaginal ultrasound (TVUS) revealed a hypoechoic pregnancy, they have been associated with placenta previas and structure in the posterior cervix that was suspicious for an antepartum and postpartum hemorrhages. low-lying placentas as well as significant antepartum and arteriovenous malformation. She was found to be anemic with a • The mode of delivery in the absence of abnormal postpartum hemorrhage[1-3,8-9,11-13,15]. Cervical varicosities are hemoglobin of 7.7 and received a blood transfusion. A few weeks placental implantation should be decided based on the thought to be the result of inferior vena cava compression by the later, she returned with preterm contractions. She was initiated on location of the cervical varicosities. expanding uterus in pregnancy [6]. In the literature, only 17 cases of nifedipine and received betamethasone for fetal lung maturity. A cervical varicosities have been reported. Due to the rare nature of repeat TVUS performed by Maternal Fetal Medicine (MFM) at 33w3d • Cesarean section for cervical varicosities in the setting of cervical varicosities in pregnancy, proper management has not been confirmed cervical varicosities on the posterior wall of the cervix and abnormal placental implantation, especially placenta established.