TMJ Concepts Related Articles Page 1 of 14
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Pattern of Third Molar Impaction; Correlation with Malocclusion And
Pattern of Third Molar Impaction; Correlation with Malocclusion and Facial Growth SograYassaei1, Farhad O Wlia2, Zahra Ebrahimi Nik3 1Associate professor, Department of Orthodontics, Faculty of Dentistry, Shahid Sadoughi University of Medical Sciences, Yazd 89195/165, Iran. 2Faculty of Dentistry, Shahid Sadoughi University of Medical Sciences, Yazd, Iran.3Postgraduate student of orthodontics, Department of Orthodontics, Faculty of Dentistry, Shahid Sadoughi University of Medical Sciences, Yazd 89195/165, Iran. Abstract Background: The aim of the present study was to evaluate the type of mandibular and maxillary third molar impaction in different malocclusions and facial growth patterns. Method and materials: In this descriptive cross sectional study, 364 impacted third molars of patients referring to the orthodontic department of Yazd University were assessed radio graphically. Also, the type of malocclusion and the facial growth pattern was determined by analyzing their lateral cephalograms. Collected data were entered to a computer and statistical tests (Chi-square) were carried out using SPSS16. Results: Significant correlation was found between the type of mandibular third molar impaction (based on Pell Gregory classification) and different types of malocclusion. Also, the dominant form of impaction (based on winter classification) among different types of facial growth pattern was the vertical one. Conclusion According to the results of this study, the vertical level of mandibular third molar impaction relative to the adjacent second molar impaction was statistically associated to the type of malocclusion. Also, we found no correlation between the M3s impaction and the type of facial growth pattern. Key Words: Third molar Impaction, Malocclusion, Facial growth pattern Introduction (2010) found higher incidence of mandibular M3s impaction The impacted tooth is one that fails to erupt into the dental in malocclusion class III [3]. -

Tutankhamun's Dentition: the Pharaoh and His Teeth
Brazilian Dental Journal (2015) 26(6): 701-704 ISSN 0103-6440 http://dx.doi.org/10.1590/0103-6440201300431 1Department of Oral and Maxillofacial Tutankhamun’s Dentition: Surgery, University Hospital of Leipzig, Leipzig, Germany The Pharaoh and his Teeth 2Institute of Egyptology/Egyptian Museum Georg Steindorff, University of Leipzig, Leipzig, Germany 3Department of Orthodontics, University Hospital of Greifswald, Greifswald, Germany Niels Christian Pausch1, Franziska Naether2, Karl Friedrich Krey3 Correspondence: Dr. Niels Christian Pausch, Liebigstraße 12, 04103 Leipzig, Germany. Tel: +49- 341-97-21160. e-mail: niels. [email protected] Tutankhamun was a Pharaoh of the 18th Dynasty (New Kingdom) in ancient Egypt. Medical and radiological investigations of his skull revealed details about the jaw and teeth status of the mummy. Regarding the jaw relation, a maxillary prognathism, a mandibular retrognathism and micrognathism have been discussed previously. A cephalometric analysis was performed using a lateral skull X-ray and a review of the literature regarding Key Words: Tutankhamun’s King Tutankhamun´s mummy. The results imply diagnosis of mandibular retrognathism. dentition, cephalometric analysis, Furthermore, third molar retention and an incomplete, single cleft palate are present. mandibular retrognathism Introduction also been discussed (11). In 1922, the British Egyptologist Howard Carter found the undisturbed mummy of King Tutankhamun. The Case Report spectacular discovery enabled scientists of the following In the evaluation of Tutankhamun’s dentition and jaw decades to analyze the Pharaoh's remains. The mummy alignment, contemporary face reconstructions and coeval underwent multiple autopsies. Until now, little was artistic images can be of further use. However, the ancient published about the jaw and dentition of the King. -

Therapeutic Management of Patients with Class III Skeletal Malocclusion
Szpyt Justyna, Gębska Magdalena. Therapeutic management of patients with class III skeletal malocclusion. Mandibular prognathism, maxillary retrognathism – a case report. Journal of Education, Health and Sport. 2019;9(5):20-31. eISSN 2391-8306. DOI http://dx.doi.org/10.5281/zenodo.2656446 http://ojs.ukw.edu.pl/index.php/johs/article/view/6872 https://pbn.nauka.gov.pl/sedno-webapp/works/912455 The journal has had 7 points in Ministry of Science and Higher Education parametric evaluation. Part B item 1223 (26/01/2017). 1223 Journal of Education, Health and Sport eISSN 2391-8306 7 © The Authors 2019; This article is published with open access at Licensee Open Journal Systems of Kazimierz Wielki University in Bydgoszcz, Poland Open Access. This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author (s) and source are credited. This is an open access article licensed under the terms of the Creative Commons Attribution Non commercial license Share alike. (http://creativecommons.org/licenses/by-nc-sa/4.0/) which permits unrestricted, non commercial use, distribution and reproduction in any medium, provided the work is properly cited. The authors declare that there is no conflict of interests regarding the publication of this paper. Received: 15.04.2019. Revised: 25.04.2019. Accepted: 01.05.2019. Therapeutic management of patients with class III skeletal malocclusion. Mandibular prognathism, maxillary retrognathism – a case report Justyna Szpyt1, Magdalena Gębska2 1. Physiotherapy student, Faculty of Health Sciences, Pomeranian Medical University in Szczecin. -

Skeletal Malocclusion and Genetic Expression: an Evidence
JDSM REVIEW ARTICLES http://dx.doi.org/10.15331/jdsm.5720 Skeletal Malocclusion and Genetic Expression: An Evidence- Based Review Clarice Nishio, DDS, MSc, PhD; Nelly Huynh, PhD Faculty of Dentistry, University of Montreal, Quebec, Canada Altered dentofacial morphology is an important risk factor of obstructive sleep apnea by compromising the upper airway volume. Maxillary and/or mandibular retrognathia, narrow maxilla, and long face are the most common craniofacial risk factors of sleep- disordered breathing. The etiology of dentofacial variation and malocclusion is multifactorial, which includes the influence of genetic and environmental factors acting on the units of the craniofacial complex. There is very little evidence on the reverse relationship, where changes in malocclusion could affect gene expression. The advances in human genetics and molecular biology have contributed to the identification of relevant genetic markers associated with certain skeletal malocclusions and/or dental malformations. Since some studies have observed differences between siblings, between parents/children, and between monozygotic twin pairs, this evidence suggests a significant influence of environmental factors in the development of dentofacial structures. However, the skeletal craniofacial complex has been systematically documented to be more influenced by genetic factors than the dental malocclusion. The greater the genetic component, the lower the rate of success on the outcome of orthodontic treatment. The real therapy should be an eventual modification of the gene responsible for the malocclusion; however, this is yet a theoretical proposition. The identification of major genes and determination of their biochemical action to a particular jaw discrepancy is the first approach necessary for the search of a solution. -

Temporomandibular Joint Dysfunction and Orthognathic Surgery: a Retrospective Study Jean-Pascal Dujoncquoy1, Joël Ferri1, Gwénael Raoul1, Johannes Kleinheinz2*
Dujoncquoy et al. Head & Face Medicine 2010, 6:27 http://www.head-face-med.com/content/6/1/27 HEAD & FACE MEDICINE RESEARCH Open Access Temporomandibular joint dysfunction and orthognathic surgery: a retrospective study Jean-Pascal Dujoncquoy1, Joël Ferri1, Gwénael Raoul1, Johannes Kleinheinz2* Abstract Background: Relations between maxillo-mandibular deformities and TMJ disorders have been the object of different studies in medical literature and there are various opinions concerning the alteration of TMJ dysfunction after orthognathic surgery. The purpose of the present study was to evaluate TMJ disorders changes before and after orthognathic surgery, and to assess the risk of creating new TMJ symptoms on asymptomatic patients. Methods: A questionnaire was sent to 176 patients operated at the Maxillo-Facial Service of the Lille’s2 Universitary Hospital Center (Chairman Pr Joël Ferri) from 01.01.2006 to 01.01.2008. 57 patients (35 females and 22 males), age range from 16 to 65 years old, filled the questionnaire. The prevalence and the results on pain, sounds, clicking, joint locking, limited mouth opening, and tenseness were evaluated comparing different subgroups of patients. Results: TMJ symptoms were significantly reduced after treatment for patients with pre-operative symptoms. The overall subjective treatment outcome was: improvement for 80.0% of patients, no change for 16.4% of patients, and an increase of symptoms for 3.6% of them. Thus, most patients were very satisfied with the results. However the appearance of new onset of TMJ symptoms is common. There was no statistical difference in the prevalence of preoperative TMJ symptoms and on postoperative results in class II compared to class III patients. -

Relationship Between Skeletal Class II and Class III Malocclusions with Vertical Skeletal Pattern
original article Relationship between skeletal Class II and Class III malocclusions with vertical skeletal pattern Sonia Patricia Plaza1, Andreina Reimpell1, Jaime Silva1, Diana Montoya1 DOI: https://doi.org/10.1590/2177-6709.24.4.063-072.oar Objective: The purpose of this study was to establish the association between sagittal and vertical skeletal patterns and assess which cephalometric variables contribute to the possibility of developing skeletal Class II or Class III malocclusion. Methods: Cross-sec- tional study. The sample included pre-treatment lateral cephalogram radiographs from 548 subjects (325 female, 223 male) aged 18 to 66 years. Sagittal skeletal pattern was established by three different classification parameters (ANB angle, Wits and App-Bpp) and vertical skeletal pattern by SN-Mandibular plane angle. Cephalometric variables were measured using Dolphin software (Imaging and Management Solutions, Chatsworth, Calif, USA) by a previously calibrated operator. The statistical analysis was carried out with Chi-square test, ANOVA/Kruskal-Wallis test, and an ordinal multinomial regression model. Results: Evidence of associa- tion (p < 0.05) between sagittal and vertical skeletal patterns was found with a greater proportion of hyperdivergent skeletal pattern in Class II malocclusion using three parameters to assess the vertical pattern, and there was more prevalent hypodivergence in Class III malocclusion, considering ANB and App-Bpp measurements. Subjects with hyperdivergent skeletal pattern (odds ratio [OR]=1.85- 3.65), maxillary prognathism (OR=2.67-24.88) and mandibular retrognathism (OR=2.57-22.65) had a significantly (p < 0.05) greater chance of developing skeletal Class II malocclusion. Meanwhile, subjects with maxillary retrognathism (OR=2.76-100.59) and man- dibular prognathism (OR=5.92-21.50) had a significantly (p < 0.05) greater chance of developing skeletal Class III malocclusion. -

CASE REPORT “Surgery-First” Approach with Invisalign Therapy to Correct a Class II Malocclusion and Severe Mandibular Retrognathism
@2019 JCO, Inc. May not be distributed without permission. www.jco-online.com CASE REPORT “Surgery-First” Approach with Invisalign Therapy to Correct a Class II Malocclusion and Severe Mandibular Retrognathism JOY CHANG, BS, DDS, MDS DEREK STEINBACHER, DMD, MD RAVINDRA NANDA, BDS, MS, PhD FLAVIO URIBE, DDS, MDS or patients with severe skeletal jaw discrepancies, the combination of orthodontics with orthognathic surgery is often the only approach that Fcan both harmonize facial esthetics and restore functional occlusion.1 Unfortunately, conventional presurgical orthodontics involves a lengthy de- compensation period that worsens the patient’s facial appearance and ex- acerbates the malocclusion.2,3 Many patients pursuing surgical-orthodontic treatment are adults who wish to avoid a deterioration in their profile and facial appearance during presurgical orthodontics.4 Dr. Chang Dr. Steinbacher Dr. Nanda Dr. Uribe Dr. Chang is a former Resident; Dr. Nanda is Professor Emeritus; and Dr. Uribe is an Associate Professor, Postgraduate Program Director, and Charles J. Burstone Endowed Professor, Division of Orthodontics, Department of Craniofacial Sciences, University of Connecticut School of Dental Medicine, Farmington, CT. Dr. Steinbacher is an Associate Professor of Plastic Surgery, Assistant Professor of Pediatrics, and Director of Dental Services, Oral Maxillofacial and Craniofacial Surgery, Yale School of Medicine, New Haven, CT. Dr. Chang is in the private practice of ortho- dontics in San Jose, CA. Dr. Nanda is also an Associate Editor and Dr. Uribe is a Contributing Editor of the Journal of Clinical Orthodontics. E-mail Dr. Uribe at [email protected]. VOLUME LIII NUMBER 7 © 2019 JCO, Inc. 397 SURGERY-FIRST WITH INVISALIGN TO CORRECT CLASS II MALOCCLUSION Fig. -

Description Concept ID Synonyms Definition
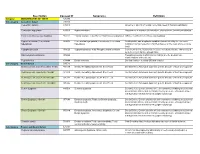
Description Concept ID Synonyms Definition Category ABNORMALITIES OF TEETH 426390 Subcategory Cementum Defect 399115 Cementum aplasia 346218 Absence or paucity of cellular cementum (seen in hypophosphatasia) Cementum hypoplasia 180000 Hypocementosis Disturbance in structure of cementum, often seen in Juvenile periodontitis Florid cemento-osseous dysplasia 958771 Familial multiple cementoma; Florid osseous dysplasia Diffuse, multifocal cementosseous dysplasia Hypercementosis (Cementation 901056 Cementation hyperplasia; Cementosis; Cementum An idiopathic, non-neoplastic condition characterized by the excessive hyperplasia) hyperplasia buildup of normal cementum (calcified tissue) on the roots of one or more teeth Hypophosphatasia 976620 Hypophosphatasia mild; Phosphoethanol-aminuria Cementum defect; Autosomal recessive hereditary disease characterized by deficiency of alkaline phosphatase Odontohypophosphatasia 976622 Hypophosphatasia in which dental findings are the predominant manifestations of the disease Pulp sclerosis 179199 Dentin sclerosis Dentinal reaction to aging OR mild irritation Subcategory Dentin Defect 515523 Dentinogenesis imperfecta (Shell Teeth) 856459 Dentin, Hereditary Opalescent; Shell Teeth Dentin Defect; Autosomal dominant genetic disorder of tooth development Dentinogenesis Imperfecta - Shield I 977473 Dentin, Hereditary Opalescent; Shell Teeth Dentin Defect; Autosomal dominant genetic disorder of tooth development Dentinogenesis Imperfecta - Shield II 976722 Dentin, Hereditary Opalescent; Shell Teeth Dentin Defect; -

The Differential Diagnosis of the Third Class of Malocclusion
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Repository for DZ "DMA" Modern Science — Moderní věda 2019 № 1 THE DIFFERENTIAL DIAGNOSIS OF THE THIRD CLASS OF MALOCCLUSION Ilona Kovach, Doctor of Medical Sciences, Professor, Aleksej Bindiuhin, Department of Pediatric Dentistry, SE "Dnipropetrovsk Medical Academy of the Health Ministry of Ukraine» Annotation. The purpose of this study was to investigate the published evidence regarding the association between the mean values of some cephalometric parameters and their relation to the different types of the clinical formes of mesial bite or third skeletal class of malocclusion. During our investigation we have been improved the efficiency of diagnosis of various clinical forms of me-sial bite by identifying and systematizing of the cephalometric indicators. The study involved 43 pa-tients aged 9 to 32 years (23 females and 20 males) with different clinical forms of the mesial bite (class 3 of malocclusion). In the study used clinical and X-ray methods. Clinical method consisted in examining patients with dentition abnormalities class 3 occlusion anomalies. X-ray method was to study the lateral x-rays of patients and analysis by Bjork, Steiner, Downs, Kim by a computer soft. A comparative analysis of the following parameters: angles ANB, SNA, SNB, ILs / NL, ILi / ML, ILs / Ili, WITS. Based on clinical studies and analysis of X-rays of the patients unable to determine that when clinical forms of third class (progenic mesial bite and progenic neutral occlusion) are ex-pected difference of digital options along with morphological changes that reliably indicates the se-verity of the anomalies based on variants of mutual location of various anatomical struc-tures.Moreover, in the course of the work found that the value of the cephalometric parameters nec-essary for diagnosis when considering teeth anomalies in the sagittal plane are essential to classify the different types of nosology forms of diseases depending on the value of angular parameters. -

Surgical-Orthodontic Treatment for a Patient with Skeletal Class III Deformity and Anterior Open Bite
Volume 30 Issue 3 Article 5 2018 Surgical-orthodontic Treatment for a Patient with Skeletal Class III Deformity and Anterior Open Bite Wei-Chih Hung Department of Dentistry, Songshan Branch, Tri-Service General Hospital, Taipei, Taiwan; Division of Orthodontics and Dentofacial Orthopedics, Department of Dentistry, Tri-Service General Hospital, Taipei, Taiwan Wei-Cheng Lee Division of Orthodontics and Dentofacial Orthopedics, Department of Dentistry, Tri-Service General Hospital, Taipei, Taiwan Yi-Chieh Chen Chicing Plastic Clinic, Taipei, Taiwan Lih-Juh Chou Division of Orthodontics and Dentofacial Orthopedics, Department of Dentistry, Tri-Service General Hospital, Taipei, Taiwan Chung-Hsing Li Division of Orthodontics and Dentofacial Orthopedics, Department of Dentistry, Tri-Service General FHospital,ollow this Taipei, and additional Taiwan" works at: https://www.tjo.org.tw/tjo Part of the Orthodontics and Orthodontology Commons See next page for additional authors Recommended Citation Hung, Wei-Chih; Lee, Wei-Cheng; Chen, Yi-Chieh; Chou, Lih-Juh; Li, Chung-Hsing; and Chen, Gunng-Shinng (2018) "Surgical-orthodontic Treatment for a Patient with Skeletal Class III Deformity and Anterior Open Bite," Taiwanese Journal of Orthodontics: Vol. 30 : Iss. 3 , Article 5. DOI: 10.30036/TJO.201810_31(3).0005 Available at: https://www.tjo.org.tw/tjo/vol30/iss3/5 This Case Report is brought to you for free and open access by Taiwanese Journal of Orthodontics. It has been accepted for inclusion in Taiwanese Journal of Orthodontics by an authorized editor -

In Response to Dr. Rood's
Letter to the Editor Dear Dr. McWilliams: May 12, 1977 - In response to Dr. Rood's "Letter to the Editor" appearing in the July, 1977 edition of The Cleft Palate Journal regarding our article "The Morphology of Musculus Uvulae," which appeared in the January, 1977 The Cleft Palate Journal, we would like to emphasize that in attempting to flatten the soft palate for histological sectioning, some curvature remained since the tissue was already embalmed prior to flattening, we stated that serial sections were cut. The section in Figure 3 was taken from the most superior portion of musculus uvulae and shows horizontally cut muscle fibers. The sections shown in Figures 4 and 5 were taken from inferior portions. Therefore, the muscle fi- bers were cut more obliquely and some even in cross section due to the curvature relative to that portion shown in Figure 3. The photomicrographs were selected from over eight hundred serial sections in order to illustrate the points discussed in the paper. We strongly disagree with Dr. Rood regarding the quality of the photomicrographs. We believe that the printing process of The Cleft Palate Journal did reproduce the photomicrographs exactly as submitted. All the photomicrographs were indeed of superior quality. Sincerely, Nabil A. Azzam, Ph.D. Professor of Anatomy David P. Kuehn, Ph.D. Research Scientist University of Iowa Hospitals and Clinics Department of Otolaryngology and Maxillofacial Surgery The University of Iowa Iowa City, Iowa 52242 331 Book Review BoonrE, DANIEL R., The Voice and Voice Therapy (2nd ed.) Englewood Cliffs: Prentice Hall, Inc., 1977, 250 pages, $10.95. -

Canine Transmigration Accompanying Mandibular Retrognathism Secondary to Osteitis
Open Med. 2015; 10: 566–571 Case Report Open Access Rafał Koszowski, Agnieszka Pisulska-Otremba, Sylwia Wójcik, Joanna Śmieszek-Wilczewska* Canine transmigration accompanying mandibular retrognathism secondary to osteitis DOI: 10.1515/med-2015-0096 received July 29, 2015; accepted October 27, 2015. However, Tarsitano and collegues were the first to define transmigration as the passing of an unerupted tooth Abstract: Transmigration is a tooth pathology in which across the median line [3]. Javid claims that the term the migrating tooth bud passes the median plane. transmigration can be applied when at least half the length Methods: This study is a presentation of the diagnostic of a tooth has passed the median line [4]. Joshi and others and therapeutic outcomes in the cases of 4 stomach teeth consider this view to be incorrect. In their opinion, what is transmigrations diagnosed in 3 patients with mandibular more important is the tendency of a tooth to migrate and retrognathia which was a complication after osteitis in the pass the median plane rather than the distance a tooth has postnatal period and infancy. Results: Extending imaging passed [5]. Howard observed a link between the migration diagnostics to include CT, most preferably CBCT, makes it of a tooth and the angle between the longitudinal axis of possible to precisely evaluate a transmigrated canine’s the impacted canine and the median line. Transmigration position and to plan a course of treatment. Conclusions: does not occur if the angle is 25-30˚. An angle of 30-95˚ Planning of the treatment of teeth in transmigration in promotes transmigration [6].