The Management of Iatrogenic Chylous Ascites
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Laparoscopy As a Diagnostic Tool in Ascites of Unknown Origin: a Retrospective Study Conducted at Kasturba Hospital, Manipal
Research Article Open Access J Surg Volume 8 Issue 3 - March 2018 Copyright © All rights are reserved by Chetan R Kulkarni DOI: 10.19080/OAJS.2018.08.555740 Laparoscopy as a Diagnostic Tool in Ascites of Unknown Origin: A Retrospective Study Conducted at Kasturba Hospital, Manipal Chetan R Kulkarni1*, Badareesh Laxminarayan2 and Annappa Kudva3 1Assistant Professor, Department of Surgery, Kasturba Hospital, Manipal 2Associate Professor, Department of Surgery, Kasturba Hospital, Manipal 3Professor, Department of Surgery, Kasturba Hospital, Manipal Received: February 16, 2018; Published: March 01, 2018 *Corresponding author: Chetan R Kulkarni, Assistant Professor, Department of Surgery, Kasturba Hospital, Manipal, India. Tel: 9535974395;Email: Abstract Background: Laparoscopy as a minimally invasive technique has long played an important role in the evaluation of ascites. Methods: A retrospective analysis was carried out on the record of 80patients who underwent laparoscopy after appropriate investigations had failed to reveal the cause of ascites. Results: Tuberculous peritonitis was reported in 46(57%), malignancies in 18(25%), cirrhosis in 4(5%) and peritonitis of unknown etiology in 8(10%)Conclusion: of patients. Two (2.5%) patients had complications, an Ileal perforation and in other Incisional hernia. Keywords: Ascites;Laparoscopy Diagnostic was Laparoscopy able to diagnose the pathology in 72 (90%) patients with ascites of unknown origin. Introduction Laparoscopy, as a minimally invasive technique has developed rapidly in recent years. Endoscopic examination of conventional laboratory examinations (including ascitic fluid cell count, albumin level, total protein level, Gram stain, culture who termed it as “Celioscopy” [1,2]. The term ‘ascites’ refers to and cytology ) as well as after imaging investigations (including peritoneal cavity was first attempted in 1901 by George Kelling Materialultrasound andand CT Methods scan). -

The Arteriovenous Fistula
DISEASE OF THE MONTH J Am Soc Nephrol 14: 1669–1680, 2003 Eberhard Ritz, Guest Editor The Arteriovenous Fistula KLAUS KONNER,* BARBARA NONNAST-DANIEL,† and EBERHARD RITZ† *Merheim Hospital, Medical Faculty, University of Cologne, Germany; †Department of Nephrology, Med. Klinik IV, Erlangen-Nu¨rnberg, Germany; and ‡Department Internal Medicine, Ruperto Carola University, Heidelberg, Germany. The ground-breaking article by Brescia and Cimino in 1966 (1) side fistula. Flow increased from 21.6 Ϯ 20.8 ml/min to 208 Ϯ revolutionized the creation of the vascular access, and the 175 ml/min immediately after operation. In well-developed fistu- Cimino fistula was soon used in almost all dialysis patients. lae, flow rates may ultimately reach values of 600 to 1200 ml/min. Unfortunately, subsequent wide-spread use of PTFE grafts Flow increases as a result of both vasodilation and vascular instead of AV fistulae occurred because of the ease of the remodeling. The latter has been studied using echo-tracking surgical technique, the immediate availability of the graft for techniques (8). It was found that the diameter of the proximal puncture, the need of high blood flow for high-efficiency, antecubital vein increased progressively while the intima me- short-duration hemodialysis sessions, and because of financial dia thickness remained unchanged. Venous dilation caused disincentives against the AV fistula. PTFE grafts currently reduction of mean shear stress, which had returned to normal account for 80% of primary vascular accesses created in the values by 3 mo. The venous limb of the AV fistula underwent United States (2,3), but they are less frequently used in other excentric hypertrophy as documented by increased wall cross- countries. -

Recurrent Pneumothorax Following Abdominal Paracentesis
Postgrad Med J (1990) 66, 319 - 320 © The Fellowship of Postgraduate Medicine, 1990 Postgrad Med J: first published as 10.1136/pgmj.66.774.319 on 1 April 1990. Downloaded from Recurrent pneumothorax following abdominal paracentesis P.J. Stafford Department ofMedicine, Newham General Hospital, Glen Road, Plaistow, London E13, UK. Summary: A 62 year old man presented with abdominal ascites, without pleural effusion, due to peritoneal mesothelioma. He had chronic obstructive airways disease and a past history of right upper lobectomy for tuberculosis. On two occasions abdominal paracentesis was followed within 72 hours by pneumothorax. This previously unreported complication of abdominal paracentesis may be due to increased diaphragmatic excursion following the procedure and should be considered in patients with preexisting lung disease. Introduction Abdominal paracentesis is a widely used palliative right iliac fossa. Approximately 4 litres of turbid therapy for malignant ascites and is generally fluid was drained over 72 hours. The protein accepted as a procedure with few adverse effects: concentration was 46 g/l and microbiology and pneumothorax is not a recognized complication. I cytology were not diagnostic. Laparoscopy re- report a patient with recurrent pneumothorax vealed matted loops of bowel with widespread apparently precipitated by abdominal paracen- peritoneal seedlings. Histological examination of copyright. tesis. these lesions showed malignant mesothelioma of the epithelioid type. The patient suffered a left pneumothorax within Case report 48 hours ofparacentesis (before laparoscopy). This was treated with intercostal underwater drainage A 62 year old civil servant presented with a 6-week but recurred on two attempts to remove the drain, history ofworsening abdominal distension. -
Intestinal and Multiple Organ Transplantation 1679
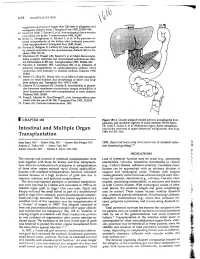
1678 TRANSPLANT ATION euglycemia and survive longer than 200 islets in allogeneic and xenogeneic diabetic hosts. Transplant Proc 1993; 25:953-954. 67. Gotoh M, Maki T, Satomi S, et al: Immunological characteristics of purified islet grafts. Transplantation 1986; 42j387. 68. Klima G, Konigsrainer A, Schmid T, et al: Is the pancreas reo jected independently of the kidney after combined pancreatic renal transplantation? Transplant Proc 1988; 20:665. 69. Prowse 5J, Bellgrau D, Lafferty KJ: Islet allografts are destroyed by disease recurrence in the spontaneously diabetic BB rat. Di abetes 1986; 35:110. 70. Markmann JF, Posselt AM, Bassiri H, et al: Major-histocompat ibility-complex restricted and nonrestricted autoil1'\mune effec tor mechanisms in BB rats. Transplantation 1991; 52:662-667. 71. Navarro X, Kennedy WR, Loewenson RB, et al: Influence of pancreas transplantation on cardiorespiratory reflexes, nerve conduction, and mortality in diabetes mellitus. Diabetes 1990; 39:802. 72. Weber q, Silva FG, Hardy MA, et al: Effect of islet transplan tation on renal function and morphology of short- and long term diabetic rats. Transplant Proc 1979; 11:549. 73. Gotzche 0, Gunderson HJ, Osterby R: Irreversibility of glomer ular basement membrane accumulation despite reversibility of renal hypertrophy with islet transplantation in early diabetes. Diabetes 1981; 30:481. 74. Fung H, Alessini M, Abu-Elmagd K, et al: Adverse effects asso ciated with the use ofFK 506. Transplant Proc 1991; 23:3105. 75. Tzakis AG: Personal communication, 1991. I CHAPTER 185 Figure 185-1. Cluster allograft (shaded portion), including the liver, pancreas, and duodenal segment of small intestine. (From Starzl TE, Todo S. -

Ens Manifestations of Hereditary Hemorrhagic Telangiectasia
569 eNS Manifestations of Hereditary Hemorrhagic Telangiectasia David Sobel, ·2 Hereditary hemorrhagic telangiectasia (HHT) is a familial angiodysplastic disorder. David Norman' Dermal, mucosal, and visceral vascular lesions of this disorder are well known. However, central nervous system (CNS) manifestations, occurring in as many as one-third of patients, have not been well appreciated until recently. The etiology of neurologic symptomatology includes hypoxemia or ischemia secondary to pulmonary arteriovenous shunting, vascular lesions of the brain and spinal cord ranging from aneurysms to arteriovenous malformations, brain abscesses secondary to pulmonary arteriovenous fistulas, and portal systemic encephalopathy. Angiographic and computed tomographic findings in four patients with CNS involvement in HHT are reported. Hereditary hemorrhagic telangiectasia (HHT), or Rendu-Osler-Weber disease, is an uncommon genetic angiodysplastic disorder transmitted as a simple mendel ian dominant character. Characteristic findings first become evident at puberty and include widely scattered dermal and mucosal telangiectases, most common on the skin of the face and neck and on buccal and nasopharyngeal mucous membranes; diffuse visceral vascular lesions; recurrent bleeding; and absence of hematologic disorders other than those secondary to bleeding and/or arteriovenous fistulas (AVFs) [1, 2). The most common presenting symptom is epistaxis from nasomu cosal lesions. Gastrointestinal, genitourinary, pulmonary, and cerebral hemorrhage may all occur. More than 300 families with HHT have been recorded in the literature. Pulmonary AVFs have been reported in 15.4% of patients [4) and are the most frequent visceral lesions. Fifty percent of patients with pulmonary AVFs are cited as having HHT [5) . Vascular malformations of the brain in HHT are much less common and have rarely been documented either angiographically or pathologically [6) . -

Guidelines on the Management of Ascites in Cirrhosis
Downloaded from gut.bmjjournals.com on 25 September 2006 Guidelines on the management of ascites in cirrhosis K P Moore and G P Aithal Gut 2006;55;1-12 doi:10.1136/gut.2006.099580 Updated information and services can be found at: http://gut.bmjjournals.com/cgi/content/full/55/suppl_6/vi1 These include: References This article cites 148 articles, 21 of which can be accessed free at: http://gut.bmjjournals.com/cgi/content/full/55/suppl_6/vi1#BIBL Email alerting Receive free email alerts when new articles cite this article - sign up in the box at the service top right corner of the article Topic collections Articles on similar topics can be found in the following collections Liver, including hepatitis (945 articles) Notes To order reprints of this article go to: http://www.bmjjournals.com/cgi/reprintform To subscribe to Gut go to: http://www.bmjjournals.com/subscriptions/ Downloaded from gut.bmjjournals.com on 25 September 2006 vi1 GUIDELINES Guidelines on the management of ascites in cirrhosis K P Moore, G P Aithal ............................................................................................................................... Gut 2006;55(Suppl VI):vi1–vi12. doi: 10.1136/gut.2006.099580 1.0 INTRODUCTION N Grade 1 (mild). Ascites is only detectable by ultrasound examination. Ascites is a major complication of cirrhosis,1 occurring in 50% of patients over 10 years of N Grade 2 (moderate). Ascites causing moderate follow up.2 The development of ascites is an symmetrical distension of the abdomen. important landmark in the natural history of N Grade 3 (large). Ascites causing marked cirrhosis as it is associated with a 50% mortality abdominal distension. -

Procedure Coding in ICD-9-CM and ICD- 10-PCS
Procedure Coding in ICD-9-CM and ICD- 10-PCS ICD-9-CM Volume 3 Procedures are classified in volume 3 of ICD-9-CM, and this section includes both an Alphabetic Index and a Tabular List. This volume follows the same format, organization and conventions as the classification of diseases in volumes 1 and 2. ICD-10-PCS ICD-10-PCS will replace volume 3 of ICD-9-CM. Unlike ICD-10-CM for diagnoses, which is similar in structure and format as the ICD-9-CM volumes 1 and 2, ICD-10-PCS is a completely different system. ICD-10-PCS has a multiaxial seven-character alphanumeric code structure providing unique codes for procedures. The table below gives a brief side-by-side comparison of ICD-9-CM and ICD-10-PCS. ICD-9-CM Volume3 ICD-10-PCS Follows ICD structure (designed for diagnosis Designed and developed to meet healthcare coding) needs for a procedure code system Codes available as a fixed or finite set in list form Codes constructed from flexible code components (values) using tables Codes are numeric Codes are alphanumeric Codes are 3-4 digits long All codes are seven characters long ICD-9-CM and ICD-10-PCS are used to code only hospital inpatient procedures. Hospital outpatient departments, other ambulatory facilities, and physician practices are required to use CPT and HCPCS to report procedures. ICD-9-CM Conventions in Volume 3 Code Also In volume 3, the phrase “code also” is a reminder to code additional procedures only when they have actually been performed. -

AASLD Position Paper : Liver Biopsy
AASLD POSITION PAPER Liver Biopsy Don C. Rockey,1 Stephen H. Caldwell,2 Zachary D. Goodman,3 Rendon C. Nelson,4 and Alastair D. Smith5 This position paper has been approved by the AASLD and College of Cardiology and the American Heart Associa- represents the position of the association. tion Practice Guidelines3).4 Introduction Preamble Histological assessment of the liver, and thus, liver bi- These recommendations provide a data-supported ap- opsy, is a cornerstone in the evaluation and management proach. They are based on the following: (1) formal re- of patients with liver disease and has long been considered view and analysis of the recently published world to be an integral component of the clinician’s diagnostic literature on the topic; (2) American College of Physi- armamentarium. Although sensitive and relatively accu- cians Manual for Assessing Health Practices and De- rate blood tests used to detect and diagnose liver disease signing Practice Guidelines1; (3) guideline policies, have now become widely available, it is likely that liver including the AASLD Policy on the Development and biopsy will remain a valuable diagnostic tool. Although Use of Practice Guidelines and the American Gastro- histological evaluation of the liver has become important enterological Association Policy Statement on Guide- in assessing prognosis and in tailoring treatment, nonin- lines2; and (4) the experience of the authors in the vasive techniques (i.e., imaging, blood tests) may replace specified topic. use of liver histology in this setting, particularly with re- Intended for use by physicians, these recommenda- gard to assessment of the severity of liver fibrosis.5,6 Sev- tions suggest preferred approaches to the diagnostic, ther- eral techniques may be used to obtain liver tissue; a table apeutic, and preventive aspects of care. -

Intercostal Was Performed, and the Patient Arteriovenous Fistula Recovered Uneventfully
976 Bilton,. Webb, Foster, Mulvenna, Dodd of factor VIII and it also releases plasminogen tion in haemaglobin than when he had activator from endothelial cells.9 previously been admitted for haematemesis. Vasopressin has been used to control bleed- Severe haemoptysis in chronic lung disease ing from oesophageal varices. Its plasma half is uncommon and pressor agents should not Thorax: first published as 10.1136/thx.45.12.976 on 1 December 1990. Downloaded from life is about 24 minutes and it is most effective be used routinely owing to the side effects of when given by infusion. The site of action is water retention and bronchoconstriction. probably arteriolar smooth muscle, through They may, however, have a useful con- an increase in the intracellular concentration servative role in the management of patients of inositol phosphates, which mobilise with cystic fibrosis who have severe lung and intracellular calcium, causing contraction. liver disease. The bronchial and mesenteric arteries both arise directly from the aorta. We hoped to reproduce the effect of pressor agents on the 1 Penketh ARL, Wise A, Mearns MB, Hodson M, Batten JC. mesenteric vasculature in the bronchial cir- Cystic Fibrosis in adolescents and adults. Thorax 1987; culation. The effect of the pressor agents in 42:526-32. 2 King AD, Cumberland DC, Brennan SR. Management of stopping pulmonary bleeding may have been severe haemoptysis by bronchial artery embolisation in a fortuitous; but the immediate termination of patient with cystic fibrosis. Thorax 1989;44:523-4. occasions, 3 Sweezey NB, Fellows K. Bronchial artery embolisation for profuse bleeding on separate severe Hemoptysis in Cystic Fibrosis. -

Aortoiliac Arteriovenous Fistulae Simulating Deep Vein Thrombosis
Case Report J Cardiol & Cardiovasc Ther - Volume 10 Issue 2 April 2018 Copyright © All rights are reserved by Germán J Chaud DOI: 10.19080/JOCCT.2018.10.555782 Aortoiliac Arteriovenous Fistulae Simulating Deep Vein Thrombosis Germán J Chaud*, Filippa A Pablo, Wainscheinker Ezequiel, Parisi Andrés, Guillermo Paladini and Alejandro M Martínez Colombres Department of Cardiovascular Surgery at Hospital Privado Universitario de Córdoba, Argentina Submission: March 05, 2018; Published: April 20, 2018 *Corresponding author: Chaud Germán J, Department of Cardiovascular Surgery at Hospital Privado Universitario de Córdoba, Córdoba, Naciones Unidas 346, Argentina, Tel: ; Email: Abstract Incidence of aorto-caval fistulae is quite low, ranging from 0.22 to 6.04% of all abdominal aortic aneurysm. One of the rare forms of abdominal aortic aneurysm rupture is rupture into great abdominal veins, such as the inferior vein cava (IVC) or the iliac veins. The typical ofclinical atherosclerosis. presentation Correct includes operative abdominal management pain, a pulsatile includes abdominal expeditious mass, control an abdominal of the bleeding, bruit and greater acute care dyspnea. to avoid Morbidity embolization and mortality through willthe be affected by the acute presentation, preoperative recognition of the fistula, the extent of cardiac failure, coronary disease and other risk factors fistula, use of blood salvage, and only selective caval interruption. Introduction Arteriovenous fistula (AVF) of the infrarenal aorta is a well- The control of the venous bleeding from fistula is challenging. useful manoeuvre. The transfemoral insertion of an occlusive known clinical entity. Incidence of aorto-caval fistulae is quite Manual compression distally and proximally to the fistula is a low, ranging from 0.22 to 6.04% of all abdominal aortic aneurysm (A.A.A). -

Clostridial Mycotic Aneurysm Leading to Emphysematous Aortitis
Open Access Case Report DOI: 10.7759/cureus.14136 Clostridial Mycotic Aneurysm Leading to Emphysematous Aortitis Thomas G. Ng 1 , Usha Trivedi 1 , Kajol Shah 1 , Pierre Maldjian 2 1. Internal Medicine, Rutgers University, Newark, USA 2. Radiology, Rutgers University, Newark, USA Corresponding author: Thomas G. Ng, [email protected] Abstract Mycotic aneurysms account for less than 5% of all aneurysms of the aorta, with most cases linked to infection with either Staphylococcus or Salmonella species. Emphysematous aortitis is a rare consequence of mycotic aneurysms and is associated with high morbidity and mortality. It typically occurs from infection superimposed on already damaged endothelium, which is commonly seen in conditions such as atherosclerosis. This report discusses the presentation and relevant imaging findings of a unique case of emphysematous aortitis from Clostridial infection of the thoracic aorta. The patient was a 66-year-old male with a past medical history of end-stage renal disease, arteriovenous fistula for dialysis, hypertension, and diabetes, who presented with tachycardia and tachypnea. Computed tomography of the chest showed inflammatory changes of the thoracic aorta with gas bubbles along the aortic wall, and post-mortem aortic tissue cultures were positive for Clostridium innocuum. Although emphysematous aortitis is rare, the radiographic findings are strikingly characteristic and should prompt immediate and aggressive management. Categories: Cardiac/Thoracic/Vascular Surgery, Infectious Disease, Anatomy Keywords: emphysematous aortitis, clostridium, mycotic aneurysm, rutgers njms, cardiothoracic surgery Introduction Emphysematous aortitis is a rare consequence of underlying mycotic aneurysm, an uncommon cause of arterial dilation resulting from infection of damaged vessel endothelium. A misnomer, mycotic aneurysm is usually caused by bacterial rather than fungal infection, and accounts for 0.7%-1.3% of all surgically treated aneurysms. -

Chyle Leak Post Laparoscopic Cholecystectomy: a Case Report, Literature Review and Management Options
7 Case Report Page 1 of 7 Chyle leak post laparoscopic cholecystectomy: a case report, literature review and management options Ferdinand Ong1, Amitabha Das1, Kheman Rajkomar2 1Department of Upper Gastrointestinal Surgery, Liverpool Hospital, Sydney, NSW, Australia; 2Department of Upper Gastrointestinal Surgery, Bankstown-Lidcombe Hospital, Sydney, NSW, Australia Correspondence to: Dr. Kheman Rajkomar. Eldridge Road, Bankstown-Lidcombe Hospital, Bankstown NSW 2200, Sydney, Australia. Email: [email protected]. Abstract: Chyle leak after a laparoscopic cholecystectomy (LC) is very rarely reported. However, it is needs to be recognised promptly and managed as otherwise it can lead to further metabolic and infective complications. We present the case of a 48 years old man who was admitted with ultrasound proven acute calculous cholecystitis. His vital signs were within normal range but his murphy’s sign was positive. His white cell count (WCC) and liver function tests were within normal limit. He underwent an uneventful standard LC with cholangiography during the same admission with no anomalous biliary or hepatic arterial anatomy noted during the procedure. Post operatively he was noted to have 125 mL of white fluid in his drain. The fluid triglyceride was 23.2 mmol/L, cholesterol level was 2.8 mmol/L, and drain/serum triglyceride of 15.5, hence confirming it to be chyle. He was clinically otherwise very well. He was managed conservatively as a low volume chyle leak with a fat free diet. The triglyceride content in the drain effluent decreased to 1.3mmol/L by day 6 and the fluid turned straw coloured in that interval. The drain was removed and the patient discharged home without any further issues.