Advanced Procedure and Diagnosis Sequencing in ICD-10
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

ABCDE Approach
The ABCDE and SAMPLE History Approach Basic Emergency Care Course Objectives • List the hazards that must be considered when approaching an ill or injured person • List the elements to approaching an ill or injured person safely • List the components of the systematic ABCDE approach to emergency patients • Assess an airway • Explain when to use airway devices • Explain when advanced airway management is needed • Assess breathing • Explain when to assist breathing • Assess fluid status (circulation) • Provide appropriate fluid resuscitation • Describe the critical ABCDE actions • List the elements of a SAMPLE history • Perform a relevant SAMPLE history. Essential skills • Assessing ABCDE • Needle-decompression for tension • Cervical spine immobilization pneumothorax • • Full spine immobilization Three-sided dressing for chest wound • • Head-tilt and chin-life/jaw thrust Intravenous (IV) line placement • • Airway suctioning IV fluid resuscitation • • Management of choking Direct pressure/ deep wound packing for haemorrhage control • Recovery position • Tourniquet for haemorrhage control • Nasopharyngeal (NPA) and oropharyngeal • airway (OPA) placement Pelvic binding • • Bag-valve-mask ventilation Wound management • • Skin pinch test Fracture immobilization • • AVPU (alert, voice, pain, unresponsive) Snake bite management assessment • Glucose administration Why the ABCDE approach? • Approach every patient in a systematic way • Recognize life-threatening conditions early • DO most critical interventions first - fix problems before moving on -

Pre and Post-Thoracostomy Chest X-Ray Taking; Do We Must Do?
www.revhipertension.com Revista Latinoamericana de Hipertensión. Vol. 15 - Nº 1, 2020 Pre and post-thoracostomy chest x-ray taking; do we must do? 71 Radiografía de tórax antes y después de la toracostomía; Qué debemos hacer? Salaminia, Shirvan; Talebi, Shadi; Mehrabi, Saadat 1Assistant Professor of Cardiac Surgery, Clinical Research Development Unit Beheshti Hospital, Yasuj University of Medical Sciences, Yasuj, Iran. [email protected], [email protected], [email protected]. 2General Practitioner, Clinical Research Development Unit Beheshti Hospital, Yasuj University of Medical Sciences, Yasuj, Iran. 3Assistant Professor of Thoracic Surgery, Clinical Research Development Unit Beheshti Hospital, Yasuj University of Medical Sciences, Yasuj, Iran *corresponding author: Saadat Mehrabi, Assistant Professor of Thoracic Surgery, Clinical Research Development Unit Beheshti Hospital, Yasuj University of Medical Sciences, Yasuj, Iran. Email: [email protected] https://doi.org/10.5281/zenodo.4074244 Abstract he prevalence of collision accidents is high in Results: Of the 58 chest tubes with the indication for re- Iran, a developing country. Currently, a plain moval, only one patient needed further observation clini- chest radiograph is routine 6 to 8 hours af- cally after removal. The coincident chest x-ray (CXR) led to ter chest tube removal. In recent years, there have been recurrent chest tube insertion. All thoracostomies had per- doubts about the necessity of routine post-removal chest formed by a trained resident or surgeon. Considering vari- x-ray (CXR) in the absence of clinical symptoms. In chil- able clinical decisions, a comparison of the diagnostic value dren, this is especially imperative because they are more of chest x-ray (CXR) to clinical examination did not differ sensitive to radiation exposure. -

FGM in Canada
Compiled by Patricia Huston MD, MPH Scientific Communications International, Inc for the Federal Interdepartmental Working Group on FGM. Copies of this report are available from: Women's Health Bureau Health Canada [email protected] The Canadian Women's Health Network 203-419 Graham Avenue Winnipeg, Manitoba R3C 0M3 fax: (204)989-2355 The opinions expressed in this report are not necessarily those of the Government of Canada or any of the other organizations represented. Dedication This report is dedicated to all the women in the world who have undergone FGM and to all the people who are helping them live with and reverse this procedure. This report is part of the ongoing commitment of Canadians and the Government of Canada to stop this practice in Canada and to improve the health and well-being of affected women and their communities. Executive Summary Female genital mutilation (FGM), or the ritual excision of part or all of the external female genitalia, is an ancient cultural practice that occurs around the world today, especially in Africa. With recent immigration to Canada of peoples from Somalia, Ethiopia and Eritrea, Sudan and Nigeria, women who have undergone this practice are now increasingly living in Canada. It is firmly believed by the people who practise it, that FGM improves feminine hygiene, that it will help eliminate disease and it is thought to be the only way to preserve family honour, a girl's virginity and her marriageability. FGM has a number of important adverse health effects including risks of infection and excessive bleeding (often performed when a girl is pre-pubertal). -

Prevalence, Clinical Characteristics, and Predictors of Peripheral Arterial Disease in Hemodialysis Patients: a Cross-Sectional Study Radislav R
Ašćerić et al. BMC Nephrology (2019) 20:281 https://doi.org/10.1186/s12882-019-1468-x RESEARCH ARTICLE Open Access Prevalence, clinical characteristics, and predictors of peripheral arterial disease in hemodialysis patients: a cross-sectional study Radislav R. Ašćerić1* , Nada B. Dimković2,3, Goran Ž. Trajković4, Biljana S. Ristić5, Aleksandar N. Janković2, Petar S. Durić2 and Nenad S. Ilijevski3,6 Abstract Background: Peripheral arterial disease (PAD) is common in patients with end-stage renal disease on hemodialysis, but is frequently underdiagnosed. The risk factors for PAD are well known within the general population, but they differ somewhat in hemodialysis patients. This study aimed to determine the prevalence of PAD and its risk factors in patients on hemodialysis. Methods: This cross-sectional study included 156 hemodialysis patients. Comorbidities and laboratory parameters were analyzed. Following clinical examinations, the ankle-brachial index was measured in all patients. PAD was diagnosed based on the clinical findings, ankle-brachial index < 0.9, and PAD symptoms. Results: PAD was present in 55 of 156 (35.3%; 95% CI, 27.7–42.8%) patients. The patients with PAD were significantly older (67 ± 10 years vs. 62 ± 11 years, p = 0.014), more likely to have diabetes mellitus (p = 0.022), and anemia (p = 0.042), and had significantly lower serum albumin (p = 0.005), total cholesterol (p =0.024),and iron (p = 0.004) levels, higher glucose (p = 0.002) and C-reactive protein (p < 0.001) levels, and lower dialysis adequacies (p = 0.040) than the patients without PAD. Multivariate analysis showed higher C-reactive protein level (odds ratio [OR], 1.03; 95% confidence interval [CI], 1.00–1.06; p = 0.030), vascular access by Hickman catheter (OR, 4.66; 95% CI, 1.03–21.0; p = 0.045), and symptoms of PAD (OR, 5.20; 95% CI, 2.60–10.4; p <0.001) as independent factors associated with PAD in hemodialysis patients. -

Iatrogenic Tension Pneumothorax After Surgical Tracheostomy in a Child with Idiopathic Subglottic Stenosis - Case Report
Kosin Medical Journal 2019;34:161-167. https://doi.org/10.7180/kmj.2019.34.2.161 &D VH 5HSRUWV Iatrogenic Tension Pneumothorax after Surgical Tracheostomy in a Child with Idiopathic Subglottic Stenosis - case report Sang Yoong Park, Woo jae Yim, Joon Ho Jeong, Jeongho Kim, Seung-Cheol Lee, So Ron Choi, Jong-Hwan Lee, Chan Jong Chung Department of Anesthesiology and Pain Medicine, Dong-A University College of Medicine, Busan, Korea Tracheostomy is increasingly performed in children for upper airway anomalies. Here, an 18-month-old child (height 84.1 cm, weight 12.5 kg) presented to the emergency department with dyspnea, stridor, and chest retraction. However, exploration of the airways using a bronchoscope failed due to subglottic stenosis. Therefore, a surgical tracheostomy was successfully performed with manual mask ventilation. However, pneumomediastinum was found in the postoperative chest radiograph. Although an oxygen saturation of 99% was initially maintained, oxygen saturation levels dropped, due to sudden dyspnea, after 3 hours. A chest radiograph taken at this time revealed a left tension pneumothorax and small right pneumothorax. Despite a needle thoracostomy, the pneumothorax was aggravated, and cardiac arrest occurred. Car - diopulmonary-cerebral resuscitation was performed, but the patient was declared dead 30 minutes later. This study high - lights the fatal complications that can occur in children during tracheostomy. Therefore, close monitoring, immediate suspicion, recognition, and aggressive management may avoid fatal outcomes. Key Words : Pediatrics, Pneumomediastinum, Tension pneumothorax, Tracheostomy, Thoracostomy Tracheostomy is increasingly being performed swallowing problems, some of which can be in children, leading to improvements in neonatal life-threatening in children. -

Complications Associated with the Use of Autologous Costal Cartilage
Rhinoplasty Aesthetic Surgery Journal 2015, Vol 35(6) 644–652 Complications Associated With the Use © 2015 The American Society for Aesthetic Plastic Surgery, Inc. Reprints and permission: of Autologous Costal Cartilage in Rhinoplasty: [email protected] DOI: 10.1093/asj/sju117 A Systematic Review www.aestheticsurgeryjournal.com Kiran Varadharajan, MRCS, DOHNS; Priya Sethukumar, MRCS (ENT); Mohiemen Anwar, MRCS, DOHNS; and Kalpesh Patel, FRCS Abstract Background: Autologous costal cartilage grafts are common in rhinoplasty. To date, no formal systematic review of complications associated with autol- ogous costal cartilage grafting in rhinoplasty exists. Objectives: The authors review current literature to examine the rates of donor and recipient site complications associated with autologous costal carti- lage in rhinoplasty. Methods: Databases (EMBASE, PubMed, MEDLINE, and Cochrane Database of Systematic Reviews) and references of pertinent articles were searched between January 1980 to July 2014 to find studies evaluating rates of complications with autologous costal cartilage grafting in rhinoplasty. These studies were then screened with specific inclusion/exclusion criteria, and data were extracted from included studies and pooled for analysis. Results: A total of 21 eligible studies were included. Pooled donor site complication incidence was pneumothorax (0.1%), pleural tear (0.6%), infection (0.6%), seroma (0.6%), scar-related problems (2.9%), and severe donor site pain (0.2%). Pooled recipient site complications were as follows: warping (5.2%), infection (2.5%), displacement/extrusion (0.6%), graft fracture (0.2%), and graft resorption (0.9%). Conclusions: Autologous costal rhinoplasty remains a safe procedure, but is associated with not insignificant rates of minor recipient site complications, such as warping. -

Core Curriculum for Surgical Technology Sixth Edition
Core Curriculum for Surgical Technology Sixth Edition Core Curriculum 6.indd 1 11/17/10 11:51 PM TABLE OF CONTENTS I. Healthcare sciences A. Anatomy and physiology 7 B. Pharmacology and anesthesia 37 C. Medical terminology 49 D. Microbiology 63 E. Pathophysiology 71 II. Technological sciences A. Electricity 85 B. Information technology 86 C. Robotics 88 III. Patient care concepts A. Biopsychosocial needs of the patient 91 B. Death and dying 92 IV. Surgical technology A. Preoperative 1. Non-sterile a. Attire 97 b. Preoperative physical preparation of the patient 98 c. tneitaP noitacifitnedi 99 d. Transportation 100 e. Review of the chart 101 f. Surgical consent 102 g. refsnarT 104 h. Positioning 105 i. Urinary catheterization 106 j. Skin preparation 108 k. Equipment 110 l. Instrumentation 112 2. Sterile a. Asepsis and sterile technique 113 b. Hand hygiene and surgical scrub 115 c. Gowning and gloving 116 d. Surgical counts 117 e. Draping 118 B. Intraoperative: Sterile 1. Specimen care 119 2. Abdominal incisions 121 3. Hemostasis 122 4. Exposure 123 5. Catheters and drains 124 6. Wound closure 128 7. Surgical dressings 137 8. Wound healing 140 1 c. Light regulation d. Photoreceptors e. Macula lutea f. Fovea centralis g. Optic disc h. Brain pathways C. Ear 1. Anatomy a. External ear (1) Auricle (pinna) (2) Tragus b. Middle ear (1) Ossicles (a) Malleus (b) Incus (c) Stapes (2) Oval window (3) Round window (4) Mastoid sinus (5) Eustachian tube c. Internal ear (1) Labyrinth (2) Cochlea 2. Physiology of hearing a. Sound wave reception b. Bone conduction c. -
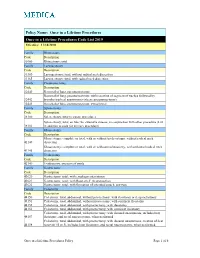
Once in a Lifetime Procedures Code List 2019 Effective: 11/14/2010
Policy Name: Once in a Lifetime Procedures Once in a Lifetime Procedures Code List 2019 Effective: 11/14/2010 Family Rhinectomy Code Description 30160 Rhinectomy; total Family Laryngectomy Code Description 31360 Laryngectomy; total, without radical neck dissection 31365 Laryngectomy; total, with radical neck dissection Family Pneumonectomy Code Description 32440 Removal of lung, pneumonectomy; Removal of lung, pneumonectomy; with resection of segment of trachea followed by 32442 broncho-tracheal anastomosis (sleeve pneumonectomy) 32445 Removal of lung, pneumonectomy; extrapleural Family Splenectomy Code Description 38100 Splenectomy; total (separate procedure) Splenectomy; total, en bloc for extensive disease, in conjunction with other procedure (List 38102 in addition to code for primary procedure) Family Glossectomy Code Description Glossectomy; complete or total, with or without tracheostomy, without radical neck 41140 dissection Glossectomy; complete or total, with or without tracheostomy, with unilateral radical neck 41145 dissection Family Uvulectomy Code Description 42140 Uvulectomy, excision of uvula Family Gastrectomy Code Description 43620 Gastrectomy, total; with esophagoenterostomy 43621 Gastrectomy, total; with Roux-en-Y reconstruction 43622 Gastrectomy, total; with formation of intestinal pouch, any type Family Colectomy Code Description 44150 Colectomy, total, abdominal, without proctectomy; with ileostomy or ileoproctostomy 44151 Colectomy, total, abdominal, without proctectomy; with continent ileostomy 44155 Colectomy, -

Resident Handbook
Duke OHNS Residency Program Handbook Table of Contents • Call Schedules • Communication (Important Numbers) • Compact Between Resident Physicians and Their Teachers • Conference Schedule • Conference Travel Policy • Copier/Fax/Supplies • Core Tenets of Residency Education • Corrective Action and Hearing Procedures • Duty Hour/Fatigue Policy • Extended Leave of Absence • Evaluations • Faculty Supervision Policy • Grievance Policy • Handoff Policy • Harassment Policy • Conflict Resolution • Impairment Policy • Institutional Compliance Modules • Lab Coats/Prescriptions Pads • Leave of Absence Policy • Licensure Requirements • Mailbox and Messages • Society Membership • Otolaryngology In-Training Exam • Required Reading • Home Study Course • ABOto Self-Assessment Modules (SAM) • Moonlighting • Unassigned Patients • Operative Case Logs • Case Coding Guidelines • Overall Policies for Duke University Residents • Policy on Resident Educational Progression and Goals & Objectives • Professionalism • Record Keeping • Reimbursement Policy • Resident Appointment, Reappointment, Promotion and Dismissal • Resident Education Fund • Resident Mentor Program • Supervisory Lines of Responsibility • Surgical Case Review/M&M/QA Conference • Vacation Policy • USMLE Step 3 • Duke Regional Coverage • Duke Raleigh Coverage Compact Between Resident Physicians and Their Teachers Residency is an integral component of the formal education of physicians. In order to practice medicine independently, physicians must receive a medical degree and complete a supervised period of residency training in a specialty area. To meet their educational goals, Resident physicians must participate actively in the care of patients and must assume progressively more responsibility for that care as they advance through their training. In supervising Resident education, Faculty must ensure that trainees acquire the knowledge and special skills of their respective disciplines while adhering to the highest standards of quality and safety in the delivery of patient care services. -

The Greenville Voice Center
The Greenville Voice Center What to Expect: Microlaryngoscopy What is microlaryngoscopy? Surgical microdirect laryngoscopy (MDL) involves putting a hollow metal tube or pipe (called a laryngoscope) into the mouth and down the throat to look at the larynx and the vocal folds. You will be asleep so that you are comfortable. We put a tooth guard over your teeth or a soft pad over your gums if you do not have teeth to protect them from the metal tube. We usually use a microscope or magnifying telescope to allow us to see the vocal cords at high magnification. Thus, the term micro-direct laryngoscopy: we’re using a microscope to look directly at the larynx. Bronchoscopy involves placing a camera between the vocal folds and passing it through the larynx into the airways to look at the trachea and the air passages to the lungs. Esophagoscopy involves placing a metal tube with a camera behind the larynx into the esophagus (swallowing pipe) in order to look at it throughout its length, sometimes as far as the stomach. The day of surgery: The day begins in the preoperative area where you will check in, meet the anesthesia team and OR nurses, speak with me, and have an IV placed in your arm or hand. When it is time for surgery, you will roll back into the operating room where you will see our team there. The instruments will likely be out and waiting for you. Once everything is confirmed and the safety checks are done, the anesthesia team will begin to put you to sleep. -

Advances in Chest Drain Management in Thoracic Disease
Review Article Advances in chest drain management in thoracic disease Robert S. George, Kostas Papagiannopoulos St. James’s University Hospital, Leeds, UK Contributions: (I) Conception and design: None; (II) Administrative support: None; (III) Provision of study materials or patients: None; (IV) Collection and assembly of data: None; (V) Data analysis and interpretation: None; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Mr. Kostas Papagiannopoulos, MD (CTh), MMed Thorax. St. James’s University Hospital, Department of Thoracic Surgery, Level 3 Bexley Wing, Beckett Street, LS9 7TF, Leeds, UK. Email: [email protected]. Abstract: An adequate chest drainage system aims to drain fluid and air and restore the negative pleural pressure facilitating lung expansion. In thoracic surgery the post-operative use of the conventional underwater seal chest drainage system fulfills these requirements, however they allow great variability amongst practices. In addition they do not offer accurate data and they are often inconvenient to both patients and hospital staff. This article aims to simplify the myths surrounding the management of chest drains following chest surgery, review current experience and explore the advantages of modern digital chest drain systems and address their disease-specific use. Keywords: Chest tube; intercostal drain (ICD); digital devices; air leak; pleural effusion Submitted Oct 15, 2015. Accepted for publication Oct 27, 2015. doi: 10.3978/j.issn.2072-1439.2015.11.19 View this article at: http://dx.doi.org/10.3978/j.issn.2072-1439.2015.11.19 Introduction Historical background The pleural cavity is an air-tight closed space that contains In 1965 Hughes advocated the use of closed tube a small amount of pleural fluid. -

GENDER DYSPHORIA TREATMENT Policy Number: 2016T0580A Effective Date: January 1, 2017
UnitedHealthcare® Commercial Medical Policy GENDER DYSPHORIA TREATMENT Policy Number: 2016T0580A Effective Date: January 1, 2017 Table of Contents Page Related Commercial Policy INSTRUCTIONS FOR USE .......................................... 1 Blepharoplasty, Blepharoptosis and Brow Ptosis BENEFIT CONSIDERATIONS ...................................... 1 Repair COVERAGE RATIONALE ............................................. 2 Botulinum Toxin A and B DEFINITIONS .......................................................... 3 Cosmetic and Reconstructive Procedures APPLICABLE CODES ................................................. 4 DESCRIPTION OF SERVICES ...................................... 8 Gonadotropin Releasing Hormone Analogs CLINICAL EVIDENCE ................................................. 8 Panniculectomy and Body Contouring Procedures U.S. FOOD AND DRUG ADMINISTRATION ................... 11 Rhinoplasty and Other Nasal Surgeries CENTERS FOR MEDICARE AND MEDICAID SERVICES ... 11 Speech Language Pathology Services REFERENCES .......................................................... 11 POLICY HISTORY/REVISION INFORMATION ................ 12 Community Plan Policy Gender Dysphoria Treatment Related Optum Guideline Gender Dysphoria INSTRUCTIONS FOR USE This Medical Policy provides assistance in interpreting UnitedHealthcare benefit plans. When deciding coverage, the member specific benefit plan document must be referenced. The terms of the member specific benefit plan document [e.g., Certificate of Coverage (COC), Schedule of