Hematolymphoid-System.Pdf
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

The Ageing Haematopoietic Stem Cell Compartment
REVIEWS The ageing haematopoietic stem cell compartment Hartmut Geiger1,2, Gerald de Haan3 and M. Carolina Florian1 Abstract | Stem cell ageing underlies the ageing of tissues, especially those with a high cellular turnover. There is growing evidence that the ageing of the immune system is initiated at the very top of the haematopoietic hierarchy and that the ageing of haematopoietic stem cells (HSCs) directly contributes to changes in the immune system, referred to as immunosenescence. In this Review, we summarize the phenotypes of ageing HSCs and discuss how the cell-intrinsic and cell-extrinsic mechanisms of HSC ageing might promote immunosenescence. Stem cell ageing has long been considered to be irreversible. However, recent findings indicate that several molecular pathways could be targeted to rejuvenate HSCs and thus to reverse some aspects of immunosenescence. HSC niche The current demographic shift towards an ageing popu- The innate immune system is also affected by ageing. A specialized lation is an unprecedented global phenomenon that has Although an increase in the number of myeloid precur- microenvironment that profound implications. Ageing is associated with tissue sors has been described in the bone marrow of elderly interacts with haematopoietic attrition and an increased incidence of many types of can- people, the oxidative burst and the phagocytic capacity of stem cells (HSCs) to regulate cers, including both myeloid and lymphoid leukaemias, and both macrophages and neutrophils are decreased in these their fate. other haematopoietic cell malignancies1,2. Thus, we need individuals12,13. Moreover, the levels of soluble immune to understand the molecular and cellular mechanisms of mediators are altered with ageing. -

Diverse T-Cell Differentiation Potentials of Human Fetal Thymus, Fetal Liver, Cord Blood and Adult Bone Marrow CD34 Cells On
IMMUNOLOGY ORIGINAL ARTICLE Diverse T-cell differentiation potentials of human fetal thymus, fetal liver, cord blood and adult bone marrow CD34 cells on lentiviral Delta-like-1-modified mouse stromal cells Ekta Patel,1 Bei Wang,1 Lily Lien,2 Summary Yichen Wang,2 Li-Jun Yang,3 Jan Human haematopoietic progenitor/stem cells (HPCs) differentiate into S. Moreb4 and Lung-Ji Chang1 functional T cells in the thymus through a series of checkpoints. A conve- 1Department of Molecular Genetics and nient in vitro system will greatly facilitate the understanding of T-cell Microbiology, College of Medicine, University of Florida, Gainesville, FL, USA, 2Vectorite development and future engineering of therapeutic T cells. In this report, Biomedica Inc., Taipei, Taiwan, 3Department we established a lentiviral vector-engineered stromal cell line (LSC) of Pathology, Immunology and Laboratory expressing the key lymphopoiesis regulator Notch ligand, Delta-like 1 Medicine, University of Florida, Gainesville, (DL1), as feeder cells (LSC-mDL1) supplemented with Flt3 ligand (fms- 4 FL, USA, and Department of Medicine, like tyrosine kinase 3, Flt3L or FL) and interleukin-7 for the development University of Florida, Gainesville, FL, USA of T cells from CD34+ HPCs. We demonstrated T-cell development from human HPCs with various origins including fetal thymus (FT), fetal liver (FL), cord blood (CB) and adult bone marrow (BM). The CD34+ HPCs from FT, FL and adult BM expanded more than 100-fold before reaching the b-selection and CD4/CD8 double-positive T-cell stage. The CB HPCs, on the other hand, expanded more than 1000-fold before b-selection. -

Characterization of Murine Macrophages from Bone Marrow
Wang et al. BMC Immunology 2013, 14:6 http://www.biomedcentral.com/1471-2172/14/6 RESEARCH ARTICLE Open Access Characterization of murine macrophages from bone marrow, spleen and peritoneum Changqi Wang1*†, Xiao Yu1,2†, Qi Cao1, Ya Wang1, Guoping Zheng1, Thian Kui Tan1, Hong Zhao1,3, Ye Zhao1, Yiping Wang1 and David CH Harris1 Abstract Background: Macrophages have heterogeneous phenotypes and complex functions within both innate and adaptive immune responses. To date, most experimental studies have been performed on macrophages derived from bone marrow, spleen and peritoneum. However, differences among macrophages from these particular sources remain unclear. In this study, the features of murine macrophages from bone marrow, spleen and peritoneum were compared. Results: We found that peritoneal macrophages (PMs) appear to be more mature than bone marrow derived macrophages (BMs) and splenic macrophages (SPMs) based on their morphology and surface molecular characteristics. BMs showed the strongest capacity for both proliferation and phagocytosis among the three populations of macrophage. Under resting conditions, SPMs maintained high levels of pro-inflammatory cytokines expression (IL-6, IL-12 and TNF-α), whereas BMs produced high levels of suppressive cytokines (IL-10 and TGF-β). However, SPMs activated with LPS not only maintained higher levels of (IL-6, IL-12 and TNF-α) than BMs or PMs, but also maintained higher levels of IL-10 and TGF-β. Conclusions: Our results show that BMs, SPMs and PMs are distinct populations with different biological functions, providing clues to guide their further experimental or therapeutic use. Keywords: Macrophage, Bone marrow, Spleen, Peritoneum Background macrophage populations could be attributed to their het- Macrophages play an essential role in both innate and erogeneity [4]. -

Collective Cell Migration in Morphogenesis, Regeneration and Cancer
REVIEWS Collective cell migration in morphogenesis, regeneration and cancer Peter Friedl*‡ and Darren Gilmour§ Abstract | The collective migration of cells as a cohesive group is a hallmark of the tissue remodelling events that underlie embryonic morphogenesis, wound repair and cancer invasion. In such migration, cells move as sheets, strands, clusters or ducts rather than individually, and use similar actin- and myosin-mediated protrusions and guidance by extrinsic chemotactic and mechanical cues as used by single migratory cells. However, cadherin-based junctions between cells additionally maintain ‘supracellular’ properties, such as collective polarization, force generation, decision making and, eventually, complex tissue organization. Comparing different types of collective migration at the molecular and cellular level reveals a common mechanistic theme between developmental and cancer research. Invasion The migration of single cells is the best-studied mecha- Defining collective cell migration A hallmark of cancer, nism of cell movement in vitro and is known to contri- Three hallmarks characterize collective cell migration. measured as cells breaking bute to many physiological motility processes in vivo, First, the cells remain physically and functionally con- away from their origin through such as development, immune surveillance and cancer nected such that the integrity of cell–cell junctions is the basement membrane. 1,2 4,6,10 We use this term to mean all metastasis . Single cell migration allows cells to position preserved during movement . Second, multicellular forms of cell movement themselves in tissues or secondary growths, as they do polarity and ‘supracellular’ organization of the actin through three-dimensional during morphogenesis and cancer, or to transiently pass cytoskeleton generate traction and protrusion force for tissue that involve a change through the tissue, as shown by immune cells. -

Cytoselect™ 24-Well Cell Haptotaxis Assay (8 Μm, Fibronectin-Coated, Colorimetric Format)
Product Manual CytoSelect™ 24-Well Cell Haptotaxis Assay (8 µm, Fibronectin-Coated, Colorimetric Format) Catalog Number CBA-100-FN 12 assays FOR RESEARCH USE ONLY Not for use in diagnostic procedures Introduction Cell migration is a highly integrated, multistep process that orchestrates embryonic morphogenesis, tissue repair and regeneration. It plays a pivotal role in the disease progression of cancer, mental retardation, atherosclerosis, and arthritis. The initial response of a cell to a migration-promoting agent is to polarize and extend protrusions in the direction of the attractant; these protrusions can consist of large, broad lamellipodia or spike-like filopodia. In either case, these protrusions are driven by actin polymerization and can be stabilized by extracellular matrix (ECM) adhesion or cell-cell interactions (via transmembrane receptors). Cell Biolabs CytoSelect™ Cell Haptotaxis Assay Kit utilizes polycarbonate membrane inserts (8 µm pore size) to assay the migratory properties of cells, the bottom side of the insert is coated with Fibronectin. The kit contains sufficient reagents for the evaluation of 12 samples. The 8 µm pore size is optimal for epithelial and fibroblast cell migration. However, in the case of leukocyte chemotaxis, a smaller pore size (3 µm) is recommended. Assay Principle The CytoSelect™ Cell Haptotaxis Assay Kit contains polycarbonate membrane inserts (8 µm pore size) in a 24-well plate. The membrane serves as a barrier to discriminate migratory cells from non- migratory cells. Migratory cells are able to extend protrusions towards the gradient of extracellular matrix density (via actin cytoskeleton reorganization) and ultimately pass through the pores of the polycarbonate membrane. Finally, the cells are removed from the top of the membrane and the migratory cells are stained and quantified. -

An Atypical Case of Recurrent Cellulitis/Lymphangitis in a Dutch Warmblood Horse Treated by Surgical Intervention A
EQUINE VETERINARY EDUCATION / AE / JANUARY 2013 23 Case Report An atypical case of recurrent cellulitis/lymphangitis in a Dutch Warmblood horse treated by surgical intervention A. M. Oomen*, M. Moleman, A. J. M. van den Belt† and H. Brommer Department of Equine Sciences and †Companion Animals, Division of Diagnostic Imaging, Faculty of Veterinary Medicine, Utrecht University, Yalelaan, Utrecht, The Netherlands. *Corresponding author email: [email protected] Keywords: horse; lymphangitis; lymphoedema; surgery; lymphangiectasia Summary proposed as a possible contributing factor for chronic The case reported here describes an atypical presentation progressive lymphoedema of the limb in these breeds of of cellulitis/lymphangitis in an 8-year-old Dutch Warmblood horses (de Cock et al. 2003, 2006; Ferraro 2003; van mare. The horse was presented with a history of recurrent Brantegem et al. 2007). episodes of cellulitis/lymphangitis and the presence of Other diseases related to the lymphatic system are fluctuating cyst-like lesions on the left hindlimb. These lesions lymphangioma/lymphangiosarcoma and development appeared to be interconnected lymphangiectasias. Surgical of lymphangiectasia. Cutaneous lymphangioma has been debridement followed by primary wound closure and local described as a solitary mass on the limb, thigh or inguinal drainage was performed under general anaesthesia. Twelve region of horses without the typical signs of progressive months post surgery, no recurrence of cellulitis/lymphangitis lymphoedema (Turk et al. 1979; Gehlen and Wohlsein had occurred and the mare had returned to her former use as 2000; Junginger et al. 2010). Lymphangiectasias in horses a dressage horse. have been described in the intestinal wall of foals and horses with clinical signs of colic and diarrhoea (Milne et al. -

Diagnostic Approach to Congenital Cystic Masses of the Neck from a Clinical and Pathological Perspective
Review Diagnostic Approach to Congenital Cystic Masses of the Neck from a Clinical and Pathological Perspective Amanda Fanous 1,†, Guillaume Morcrette 2,†, Monique Fabre 3, Vincent Couloigner 1,4 and Louise Galmiche-Rolland 5,* 1 Pediatric Otolaryngology-Head and Neck Surgery, AP-HP, Hôpital Universitaire Necker Enfants Malades, 75015 Paris, France; [email protected] (A.F.); [email protected] (V.C.) 2 Department of Pediatric Pathology, AP-HP, Hôpital Robert Debré, 75019 Paris, France; [email protected] 3 Department of Pathology, AP-HP, Hôpital Universitaire Necker Enfants Malades, Université Paris Descartes, 75015 Paris, France; [email protected] 4 Faculté de Médecine, Université de Paris, 75015 Paris, France 5 Department of Pathology, University Hospital of Nantes, 44000 Nantes, France * Correspondence: [email protected] † These authors contributed equally to this work. Abstract: Background: neck cysts are frequently encountered in pediatric medicine and can present a diagnostic dilemma for clinicians and pathologists. Several clinical items enable to subclassify neck cyst as age at presentation, anatomical location, including compartments and fascia of the neck, and radiological presentation. Summary: this review will briefly describe the clinical, imaging, pathologi- cal and management features of (I) congenital and developmental pathologies, including thyroglossal duct cyst, branchial cleft cysts, dermoid cyst, thymic cyst, and ectopic thymus; (II) vascular malforma- Citation: Fanous, A.; Morcrette, G.; Fabre, M.; Couloigner, V.; tions, including lymphangioma. Key Messages: pathologists should be familiar with the diagnostic Galmiche-Rolland, L. Diagnostic features and clinicopathologic entities of these neck lesions in order to correctly diagnose them and Approach to Congenital Cystic to provide proper clinical management. -

In Sickness and in Health: the Immunological Roles of the Lymphatic System
International Journal of Molecular Sciences Review In Sickness and in Health: The Immunological Roles of the Lymphatic System Louise A. Johnson MRC Human Immunology Unit, MRC Weatherall Institute of Molecular Medicine, University of Oxford, John Radcliffe Hospital, Headington, Oxford OX3 9DS, UK; [email protected] Abstract: The lymphatic system plays crucial roles in immunity far beyond those of simply providing conduits for leukocytes and antigens in lymph fluid. Endothelial cells within this vasculature are dis- tinct and highly specialized to perform roles based upon their location. Afferent lymphatic capillaries have unique intercellular junctions for efficient uptake of fluid and macromolecules, while expressing chemotactic and adhesion molecules that permit selective trafficking of specific immune cell subsets. Moreover, in response to events within peripheral tissue such as inflammation or infection, soluble factors from lymphatic endothelial cells exert “remote control” to modulate leukocyte migration across high endothelial venules from the blood to lymph nodes draining the tissue. These immune hubs are highly organized and perfectly arrayed to survey antigens from peripheral tissue while optimizing encounters between antigen-presenting cells and cognate lymphocytes. Furthermore, subsets of lymphatic endothelial cells exhibit differences in gene expression relating to specific func- tions and locality within the lymph node, facilitating both innate and acquired immune responses through antigen presentation, lymph node remodeling and regulation of leukocyte entry and exit. This review details the immune cell subsets in afferent and efferent lymph, and explores the mech- anisms by which endothelial cells of the lymphatic system regulate such trafficking, for immune surveillance and tolerance during steady-state conditions, and in response to infection, acute and Citation: Johnson, L.A. -

Cells, Tissues and Organs of the Immune System
Immune Cells and Organs Bonnie Hylander, Ph.D. Aug 29, 2014 Dept of Immunology [email protected] Immune system Purpose/function? • First line of defense= epithelial integrity= skin, mucosal surfaces • Defense against pathogens – Inside cells= kill the infected cell (Viruses) – Systemic= kill- Bacteria, Fungi, Parasites • Two phases of response – Handle the acute infection, keep it from spreading – Prevent future infections We didn’t know…. • What triggers innate immunity- • What mediates communication between innate and adaptive immunity- Bruce A. Beutler Jules A. Hoffmann Ralph M. Steinman Jules A. Hoffmann Bruce A. Beutler Ralph M. Steinman 1996 (fruit flies) 1998 (mice) 1973 Discovered receptor proteins that can Discovered dendritic recognize bacteria and other microorganisms cells “the conductors of as they enter the body, and activate the first the immune system”. line of defense in the immune system, known DC’s activate T-cells as innate immunity. The Immune System “Although the lymphoid system consists of various separate tissues and organs, it functions as a single entity. This is mainly because its principal cellular constituents, lymphocytes, are intrinsically mobile and continuously recirculate in large number between the blood and the lymph by way of the secondary lymphoid tissues… where antigens and antigen-presenting cells are selectively localized.” -Masayuki, Nat Rev Immuno. May 2004 Not all who wander are lost….. Tolkien Lord of the Rings …..some are searching Overview of the Immune System Immune System • Cells – Innate response- several cell types – Adaptive (specific) response- lymphocytes • Organs – Primary where lymphocytes develop/mature – Secondary where mature lymphocytes and antigen presenting cells interact to initiate a specific immune response • Circulatory system- blood • Lymphatic system- lymph Cells= Leukocytes= white blood cells Plasma- with anticoagulant Granulocytes Serum- after coagulation 1. -

Lympho Scintigraphy and Lymphangiography of Lymphangiectasia
supplement to qualitative interpretation of scintiscans, pulmo 13. Hirose Y, lmaeda T, Doi H, Kokubo M, Sakai 5, Hirose H. Lung perfusion SPECT in nary perfusion scintigraphy will become a more useful tech predicting postoperative pulmonary function in lung cancer. Ann Nuc/ Med 1993:7: 123—126. nique for clinical evaluation of treatment and assessment of 14. Hosokawa N, Tanabe M, Satoh K. et al. Prediction of postoperative pulmonary breathlessness and respiratory failure than the usual one. function using 99mTcMAA perfusion lung SPECT. Nippon Ada Radio/ 1995;55:414— 422. 15. Richards-Catty C, Mishkin FS. Hepatic activity on perfusion lung images. Semi,, Nuci REFERENCES Med l987;l7:85—86. I. Wagner UN Jr. Sabiston DC ir, McAee JG, Tow D, Stem HS. Diagnosis of massive 16. Kitani K, Taplin GV. Biliary excretion of9@―Tc-albuminmicroaggregate degradation pulmonaryembolism in man by radioisotopescanning.N Engli Med 1964;27l:377-384. products (a method for measuring Kupifer cell digestive function?). J Naic! Med 2. Maynard CD. Cowan Ri. Role of the scan in bronchogenic carcinoma. Semin Nuci 1972:13:260—265. Med 1971;l:195—205. 17. Marcus CS, Parker LS, Rose 1G. Cullison RC. Grady P1. Uptake of ‘@“Tc-MAAby 3. Newman GE, Sullivan DC, Gottschalk A, Putman CE. Scintigraphic perfusion pattems the liver during a thromboscintigram/lung scan. J Nuci Med 1983;24:36—38. in patients with diffuse lung disease. Radiology 1982;l43:227—23l. 18. Gates GF, Goris ML. Suitability of radiopharmaceuticals for determining right-to-left 4. Clarke SEM, Seeker-Walker RH. Lung scanning. -
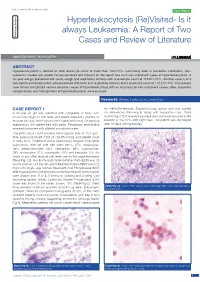
Hyperleukocytosis (Re)Visited- Is It Case Series Always Leukaemia: a Report of Two Pathology Section Cases and Review of Literature Short Communication
Review Article Clinician’s corner Original Article Images in Medicine Experimental Research Miscellaneous Letter to Editor DOI: 10.7860/JCDR/2020/40556.13409 Case Report Postgraduate Education Hyperleukocytosis (Re)Visited- Is it Case Series always Leukaemia: A Report of Two Pathology Section Cases and Review of Literature Short Communication ASHUTOSH RATH1, RICHA GUPTA2 ABSTRACT Hyperleukocytosis is defined as total leukocyte count of more than 100×109/L. Commonly seen in leukaemic conditions, non- leukaemic causes are usually not encountered and thought of. We report two such non-malignant cases of hyperleukocytosis. A six-year old girl presented with fever, cough and respiratory distress with a leukocyte count of 125.97×109/L. Another case is of a two-month old female infant, who presented with fever and respiratory distress and a leukocyte count of 112.27×109/L. The present case thrives to highlight various possible causes of hyperleukocytosis with an emphasis on non-malignant causes. Also, important complications and management of hyperleukocytosis are discussed. Keywords: Benign, Leukocytosis, Leukostasis CASE REPORT 1 for methicillin-resistant Staphylococcus aureus and was started A six-year-old girl was admitted with complaints of fever, non- on intravenous Vancomycin along with supportive care. Serial productive cough for one week and severe respiratory distress for monitoring of TLC revealed a gradual reduction and it returned to the the past one day. There was no other significant history. On physical baseline of 15×109/L after eight days. The patient was discharged examination, the patient had mild pallor. Respiratory examination after 10 days of hospital stay. -

Leukemoid Reaction in a Patient with Acute Lymphoblastic Leukemia Following the Second Chemotherapy
262JCEI / Yokuş et al. Leukemoid reaction in ALL 2013; 4 (2): 262-263 Journal of Clinical and Experimental Investigations doi: 10.5799/ahinjs.01.2013.02.0280 LETTER TO EDITOR Leukemoid reaction in a patient with acute lymphoblastic leukemia following the second chemotherapy Akut lenfoblastik lösemili hastada ikinci kemoterapi sonrası gelişen lökomoid reaksiyon Osman Yokuş1, Murat Albayrak2, Aynur Albayrak3, Habip Gedik4 To the Editor, to 50.000 cells/µL. The examined peripheral blood smear appeared as similar to the chronic phase of The occurrence of persistent neutrophilic leukocy- CML (fig.2). A cytogenetic examination of Philadel- tosis above 50,000 cells/µL for reasons other than phia chromosome [t(9:22] was found to be nega- leukemia is defined as leukemoid reaction. Chronic tive, therefore, CML was excluded in the patient. myelogenous leukemia (CML) and chronic neutro- Hydroxurea was initiated once a day. Leukocytosis philic leukemia (CNL) should be excluded, and un- recovered to normal range after one week (fig.3) derlying diseases or causes should be examined, and bone marrow examination revealed remission. in differential diagnosis. The most commonly ob- Cytogenetic analysis was normal and this leukocy- served causes of leukemoid reactions are severe tosis was determined as reactive leukemoid reac- infections, intoxications, malignancies, severe hem- tion. We aimed to report this case owing to the fact orrhage, or acute hemolysis [1]. J Clin Exp Invest that leukocytosis associated with G-CSF, which is 2013; 4 (2): 262-263 used to increase the leukocyte count during neutro- Rarely, leukemoid reaction can be seen in pa- penia, has been reported previously but it occurred tients with acute leukemia subsequent to chemo- after second chemotherapy without G-CSF [4].