Food Allergies in the Lactation Dyad
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
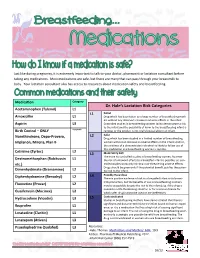
Dr. Hale's Lactation Risk Categories
Just like during pregnancy, it is extremely important to talk to your doctor, pharmacist or lactation consultant before taking any medications. Most medications are safe, but there are many that can pass through your breastmilk to baby. Your lactation consultant also has access to resources about medication safety and breastfeeding. Medication Category Dr. Hale’s Lactation Risk Categories Acetaminophen (Tylenol) L1 L1 Safest Amoxicillin L1 Drug which has been taken by a large number of breastfeeding moth- ers without any observed increase in adverse effects in the infant. Aspirin L3 Controlled studies in breastfeeding women fail to demonstrate a risk to the infant and the possibility of harm to the breastfeeding infant is Birth Control – ONLY Acceptable remote; or the product is not orally bioavailable in an infant. L2 Safer Norethindrone, Depo-Provera, Drug which has been studied in a limited number of breastfeeding Implanon, Mirena, Plan B women without an increase in adverse effects in the infant; And/or, the evidence of a demonstrated risk which is likely to follow use of this medication in a breastfeeding woman is remote. Cetrizine (Zyrtec) L2 L3 Moderately Safe There are no controlled studies in breastfeeding women, however Dextromethorphan (Robitussin L1 the risk of untoward effects to a breastfed infant is possible; or, con- etc.) trolled studies show only minimal non-threatening adverse effects. Drugs should be given only if the potential benefit justifies the poten- Dimenhydrinate (Dramamine) L2 tial risk to the infant. L4 Possibly Hazardous Diphenhydramine (Benadryl) L2 There is positive evidence of risk to a breastfed infant or to breast- milk production, but the benefits of use in breastfeeding mothers Fluoxetine (Prozac) L2 may be acceptable despite the risk to the infant (e.g. -

Breastfeeding Is Best Booklet
SOUTH DAKOTA DEPARTMENT OF HEALTH WIC PROGRAM Benefits of Breastfeeding Getting Started Breastfeeding Solutions Collecting and Storing Breast Milk Returning to Work or School Breastfeeding Resources Academy of Breastfeeding Medicine www.bfmed.org American Academy of Pediatrics www2.aap.org/breastfeeding Parenting website through the AAP www.healthychildren.org/English/Pages/default.aspx Breastfeeding programs in other states www.cdc.gov/obesity/downloads/CDC_BFWorkplaceSupport.pdf Business Case for Breastfeeding www.womenshealth.gov/breastfeeding/breastfeeding-home-work- and-public/breastfeeding-and-going-back-work/business-case Centers for Disease Control and Prevention www.cdc.gov/breastfeeding Drugs and Lactation Database (LactMed) www.toxnet.nlm.nih.gov/newtoxnet/lactmed.htm FDA Breastpump Information www.fda.gov/MedicalDevices/ProductsandMedicalProcedures/ HomeHealthandConsumer/ConsumerProducts/BreastPumps Healthy SD Breastfeeding-Friendly Business Initiative www.healthysd.gov/breastfeeding International Lactation Consultant Association www.ilca.org/home La Leche League www.lalecheleague.org MyPlate for Pregnancy and Breastfeeding www.choosemyplate.gov/moms-pregnancy-breastfeeding South Dakota WIC Program www.sdwic.org Page 1 Breastfeeding Resources WIC Works Resource System wicworks.fns.usda.gov/breastfeeding World Health Organization www.who.int/nutrition/topics/infantfeeding United States Breastfeeding Committee - www.usbreastfeeding.org U.S. Department of Health and Human Services/ Office of Women’s Health www.womenshealth.gov/breastfeeding -

Infant Formula (Breastmilk Substitute) Feeding
Infant Formula (Breastmilk Substitute) Feeding Congratulations on your new baby! If you have made an informed decision not to breastfeed, this handout will provide you with information on the safe preparation of formula (breastmilk substitute) for your healthy full-term infant. If your baby is born early, you will need to follow the specific feeding advice provided by your health care provider. You will probably have many questions about formula feeding. Here are some questions which parents and caregivers often ask: What type of formula should I give my baby? Give your baby a commercial iron-fortified infant formula. How long do I need to give my baby infant formula? Give your baby commercial iron-fortified infant formula until he or she is 9 to 12 months old and is eating a variety of solid foods. Then you can gradually introduce whole cow's milk. For formula-fed babies, the change from iron-fortified infant formula to whole cow’s milk should be completed by around one year of age. At this time, a formula-fed baby should be consuming a healthy diet, including two cups of milk a day, to meet her vitamin D needs. What should I look for when I buy commercial infant formula? • Always buy commercial infant formula with iron. It may be labelled “iron fortified” or “with iron”. Iron helps to keep your baby’s blood healthy. Iron-fortified infant formula does not cause constipation. • Check the expiry date or best before date. These dates may be printed on the bottom or on the side of the package. -

Clinical Update and Treatment of Lactation Insufficiency
Review Article Maternal Health CLINICAL UPDATE AND TREATMENT OF LACTATION INSUFFICIENCY ARSHIYA SULTANA* KHALEEQ UR RAHMAN** MANJULA S MS*** SUMMARY: Lactation is beneficial to mother’s health as well as provides specific nourishments, growth, and development to the baby. Hence, it is a nature’s precious gift for the infant; however, lactation insufficiency is one of the explanations mentioned most often by women throughout the world for the early discontinuation of breast- feeding and/or for the introduction of supplementary bottles. Globally, lactation insufficiency is a public health concern, as the use of breast milk substitutes increases the risk of morbidity and mortality among infants in developing countries, and these supplements are the most common cause of malnutrition. The incidence has been estimated to range from 23% to 63% during the first 4 months after delivery. The present article provides a literary search in English language of incidence, etiopathogensis, pathophysiology, clinical features, diagnosis, and current update on treatment of lactation insufficiency from different sources such as reference books, Medline, Pubmed, other Web sites, etc. Non-breast-fed infant are 14 times more likely to die due to diarrhea, 3 times more likely to die of respiratory infection, and twice as likely to die of other infections than an exclusively breast-fed child. Therefore, lactation insufficiency should be tackled in appropriate manner. Key words : Lactation insufficiency, lactation, galactagogue, breast-feeding INTRODUCTION Breast-feeding is advised becasue human milk is The synonyms of lactation insufficiency are as follows: species-specific nourishment for the baby, produces lactational inadequacy (1), breast milk insufficiency (2), optimum growth and development, and provides substantial lactation failure (3,4), mothers milk insufficiency (MMI) (2), protection from illness. -

Maternal Intake of Cow's Milk During Lactation Is Associated with Lower
nutrients Article Maternal Intake of Cow’s Milk during Lactation Is Associated with Lower Prevalence of Food Allergy in Offspring Mia Stråvik 1 , Malin Barman 1,2 , Bill Hesselmar 3, Anna Sandin 4, Agnes E. Wold 5 and Ann-Sofie Sandberg 1,* 1 Department of Biology and Biological Engineering, Food and Nutrition Science, Chalmers University of Technology, 412 96 Gothenburg, Sweden; [email protected] (M.S.); [email protected] (M.B.) 2 Institute of Environmental Medicine, Unit of Metals and Health, Karolinska Institutet, 171 77 Stockholm, Sweden 3 Department of Paediatrics, Institute of Clinical Sciences, Sahlgrenska Academy, University of Gothenburg, 405 30 Gothenburg, Sweden; [email protected] 4 Department of Clinical Science, Pediatrics, Sunderby Research Unit, Umeå University, 901 87 Umeå, Sweden; [email protected] 5 Department of Infectious Diseases, Institute of Biomedicine, Sahlgrenska Academy, University of Gothenburg, 413 90 Gothenburg, Sweden; [email protected] * Correspondence: ann-sofi[email protected] Received: 10 November 2020; Accepted: 25 November 2020; Published: 28 November 2020 Abstract: Maternal diet during pregnancy and lactation may affect the propensity of the child to develop an allergy. The aim was to assess and compare the dietary intake of pregnant and lactating women, validate it with biomarkers, and to relate these data to physician-diagnosed allergy in the offspring at 12 months of age. Maternal diet during pregnancy and lactation was assessed by repeated semi-quantitative food frequency questionnaires in a prospective Swedish birth cohort (n = 508). Fatty acid proportions were measured in maternal breast milk and erythrocytes. Allergy was diagnosed at 12 months of age by a pediatrician specialized in allergy. -

Breastfeeding Support Credentials
Who’s Who? A glance at breastfeeding support in the United States Lactation support is often needed to help mothers initiate and continue breastfeeding. There are many kinds of help available for breastfeeding mothers including peer counselors, certified breastfeeding educators and counselors, and lactation professionals such as the International Board Certified Lactation Consultant (IBCLC®). Breastfeeding support is valuable for a variety of reasons, from encouragement and emotional support to guidance and assistance with complex clinical situations. Mothers benefit from all kinds of support, and it is important to receive the right kind at the right time. The breastfeeding support categories listed below each play a vital role in providing care to mothers and babies. Breastfeeding Support Prerequisites Training Required Scope of Practice Type • 90 hours of lactation-specific education Recognized health Provide professional, • College level health science professional or evidence based, clinical courses Professional satisfactory completion lactation management; • 300-1000 clinical practice hours (International Board Certified of collegiate level educate families, health Lactation Consultant, IBCLC®) • Successful completion of a health sciences professionals and others criterion-referenced exam offered coursework. about human lactation. by an independent international board of examiners. Certified • 20-120 hours of classroom training Provide education and • Often includes a written exam guidance for families (i.e. Certified Lactation N/A Counselor, Certified or “certification” offered by the on basic breastfeeding Breastfeeding Educator, etc. ) training organization issues. Provide breastfeeding information, Peer Personal breastfeeding • 18-50 hours of classroom training encouragement, and (i.e. La Leche League, WIC experience. Peer Counselor, etc.) support to those in their community. Copyright © 2016 by USLCA. -

MATERNAL & CHILD HEALTH Technical Information Bulletin
A Review of the Medical Benefits and Contraindications to Breastfeeding in the United States Ruth A. Lawrence, M.D. Technical Information Bulletin Technical MATERNAL & CHILD HEALTH MATERNAL October 1997 Cite as Lawrence RA. 1997. A Review of the Medical Benefits and Contraindications to Breastfeeding in the United States (Maternal and Child Health Technical Information Bulletin). Arlington, VA: National Center for Education in Maternal and Child Health. A Review of the Medical Benefits and Contraindications to Breastfeeding in the United States (Maternal and Child Health Technical Information Bulletin) is not copyrighted with the exception of tables 1–6. Readers are free to duplicate and use all or part of the information contained in this publi- cation except for tables 1–6 as noted above. Please contact the publishers listed in the tables’ source lines for permission to reprint. In accordance with accepted publishing standards, the National Center for Education in Maternal and Child Health (NCEMCH) requests acknowledg- ment, in print, of any information reproduced in another publication. The mission of the National Center for Education in Maternal and Child Health is to promote and improve the health, education, and well-being of children and families by leading a nation- al effort to collect, develop, and disseminate information and educational materials on maternal and child health, and by collaborating with public agencies, voluntary and professional organi- zations, research and training programs, policy centers, and others to advance knowledge in programs, service delivery, and policy development. Established in 1982 at Georgetown University, NCEMCH is part of the Georgetown Public Policy Institute. NCEMCH is funded primarily by the U.S. -

Journal of Human Lactation
Journal of Human Lactation http://jhl.sagepub.com Exclusive Breastfeeding: Isn’t Some Breastfeeding Good Enough? Jane Heinig and Kara Ishii J Hum Lact 2004; 20; NP DOI: 10.1177/089033440402000409 The online version of this article can be found at: http://jhl.sagepub.com Published by: http://www.sagepublications.com On behalf of: International Lactation Consultant Association Additional services and information for Journal of Human Lactation can be found at: Email Alerts: http://jhl.sagepub.com/cgi/alerts Subscriptions: http://jhl.sagepub.com/subscriptions Reprints: http://www.sagepub.com/journalsReprints.nav Permissions: http://www.sagepub.com/journalsPermissions.nav Downloaded from http://jhl.sagepub.com at International Lactation Consultant Association on September 29, 2008 ILCA’s INSIDE TRACK a resource for breastfeeding mothers A Publication of the International Lactation Consultant Association Exclusive Breastfeeding: Isn’t Some Breastfeeding Good Enough? By Jane Heinig, PhD, IBCLC, and Kara Ishii, MSW ongratulations on choosing to for at least 3 months. For mothers, exclusive breastfeed your baby! As you know, breastfeeding during the first 6 months means Cmany of the benefits of breastfeeding that more calories are going to make milk (so last a lifetime. You might have heard that health the mother loses weight more quickly, which is organizations, including the World Health Orga- important for her health). Also, mothers who nization, recommend exclusive breastfeeding for exclusively breastfeed often go 9 months with- the first 6 months of life. You may be wondering out a period after their babies are born. Longer if exclusive breastfeeding is truly important or if breastfeeding is also related to greater protec- breastfeeding mixed with bottle feeding is just tion for mothers against breast cancer. -

Factors Affecting Goat Milk Production and Quality
Small Ruminant Research 101 (2011) 55–63 Contents lists available at SciVerse ScienceDirect Small Ruminant Research jou rnal homepage: www.elsevier.com/locate/smallrumres Review article ଝ Factors affecting goat milk production and quality ∗ A.L. Goetsch , S.S. Zeng, T.A. Gipson American Institute for Goat Research, Langston University, P. O. Box 1730, Langston, OK 73050, USA a r t i c l e i n f o a b s t r a c t Article history: Differences between production systems based on grazing and browsing vs. use of har- Available online 5 October 2011 vested feedstuffs in confinement largely depend on specific feedstuffs and plants available and being consumed. Low forage nutrient ingestion should have relatively greater impact Keywords: on tissue mobilization than milk production in early than later periods of lactation, with a Goats transition to proportionally greater change in milk production in late lactation. However, Milk low body condition at kidding would limit tissue energy mobilization and restrict impact Lactation of level of nutrient intake to milk yield and, likewise, tissue mobilization would be less with one vs. two or three milkings per day. As lactation advances after freshening, fat and protein levels decrease with increasing milk yield, and when production declines in mid- to late lactation, fat and protein concentrations increase. Milk production generally peaks at a parity of 3 or 4, thereafter declining slowly. Elevated somatic cell count alone in dairy goats is not a valid indication of mammary infection. Extended lactations offer opportunities to minimize or avoid seasonal fluctuations in milk production and lessen production costs. -

Your Guide to Breastfeeding
Pumping and Milk Storage If you are unable to breastfeed your baby directly, it is important to remove milk during the times your baby normally would feed. This will help you continue to make milk. Before you express breast milk, be sure to wash your hands. Also, make sure the area where you are expressing is clean. If you need help to get your milk to start fow- ing, have one of the following items nearby – a picture of your baby, a baby blanket, or an item of your baby’s clothing that has his or her scent on it. You can also apply a warm moist compress to the breast, gently massage the breasts, or sit quietly and think of a relaxing setting. Ways to Express Your Milk Type How It Works What’s Involved Average Cost Hand You use your hand to UÊRequires practice, skill, and coordination. Free, unless you need Expression massage and com- UÊGets easier with practice; can be as fast as help from a breastfeeding press your breast to pumping. professional who charges remove milk. UÊGood if you are seldom away from baby or for her services. need an option that is always with you. But all moms should learn how to hand express. Manual Pump You use your hand UÊRequires practice, skill, and coordination. $30 to $50 and wrist to operate UÊUseful for occasional pumping if you are a hand-held device to away from baby once in a while. pump the milk. Automatic, Runs on battery or UÊCan be easier for some moms. -

Use of Soy Protein-Based Formulas in Infant Feeding Jatinder Bhatia and Frank Greer Pediatrics 2008;121;1062 DOI: 10.1542/Peds.2008-0564
CLINICAL REPORT Guidance for the Clinician in Rendering Use of Soy Protein-Based Formulas in Pediatric Care Infant Feeding Jatinder Bhatia, MD, Frank Greer, MD, and the Committee on Nutrition ABSTRACT Soy protein-based formulas have been available for almost 100 years. Since the first use of soy formula as a milk substitute for an infant unable to tolerate a cow www.pediatrics.org/cgi/doi/10.1542/ peds.2008-0564 milk protein-based formula, the formulation has changed to the current soy protein isolate. Despite very limited indications for its use, soy protein-based doi:10.1542/peds.2008-0564 formulas in the United States may account for nearly 25% of the formula market. All clinical reports from the American Academy of Pediatrics automatically expire This report reviews the limited indications and contraindications of soy formulas. 5 years after publication unless reaffirmed, It will also review the potential harmful effects of soy protein-based formulas and revised, or retired at or before that time. the phytoestrogens contained in these formulas. The guidance in this report does not indicate an exclusive course of treatment HE AMERICAN ACADEMY of Pediatrics (AAP) is committed to the use of human or serve as a standard of medical care. Variations, taking into account individual Tmilk as the ideal source of nutrition for infant feeding. However, by 2 months circumstances, may be appropriate. of age, the majority of infants in North America are receiving at least some Key Words formula. Soy-based infant formulas have been available for almost 100 years.1 soy protein, infant formula, infant feeding, Despite limited indications, soy protein-based formula accounts for approximately cow milk protein allergy, nutrition, 20% of the formula market in the United States. -

Discontinuing Gerber Graduates Soy, Introduction of Stage 3 Gerber Good Start Soy, and Transitioning to Non-GMO Ingredients Contact: Karen Henry
Announcement 4/21/16 Gerber announces three changes – discontinuing Gerber Graduates Soy, introduction of Stage 3 Gerber Good Start Soy, and transitioning to non-GMO ingredients Contact: Karen Henry Discontinuation of Gerber Graduates Soy Gerber has announced they are discontinuing their soy toddler formula Gerber Graduates Soy. It will stop being manufactured next month (April) but will likely remain available several months afterward. This had been on our rebate contract but fortunately we currently only have 10 participants on the product in the state. Only four agencies have clients on this formula. Within the next couple days, the directors of agencies that have clients on this product will be notified with client info so that the clients can be informed that they will likely stop seeing the product in upcoming months. These participants can ask their physician if the Enfamil Toddler Transitions Soy is a suitable substitute. With a soy toddler contract formula no longer available (the Gerber Graduates Soy), the Enfamil Toddler Transitions soy will be an option without State Approval. If you have clients with new prescriptions for Gerber Graduates Soy, please inquire with the client’s physician if the Enfamil Toddler Transitions Soy is a possible substitute. The physician form on the web is additionally in the process of being updated on azwic.gov. New Stage 3 Gerber Good Start Soy Additionally later this year, Gerber is coming out with a replacement for the Gerber Graduates Soy. It will have limited retail distribution during the 2016 launch period. Not many details are available on this product yet, but will give more info once it becomes available.