Varicose Veins of the Lower Extremities, Treatment For
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Endoscopic Vein Harvest of the Lesser Saphenous Vein in the Supine Position: a Unique Approach to an Old Problem†
Interactive Cardiovascular and Thoracic Surgery 16 (2013) 1–4 NEW IDEAS - ADULT CARDIAC doi:10.1093/icvts/ivs414 Advance Access publication 9 October 2012 Endoscopic vein harvest of the lesser saphenous vein in the supine position: a unique approach to an old problem† C. Phillip Brandt*, G. Clark Greene, Michael L. Maggart, William C. Hall, Lacy E. Harville, Thomas R. Pollard and Chadwick W. Stouffer NEW IDEAS East Tennessee Cardiovascular Surgery Group, Knoxville, TN, USA * Corresponding author: East Tennessee Cardiovascular Surgery Group, PC, 9125 Cross Park Drive, Suite 200, Knoxville, TN 37920, USA. Fax: 865-637-2114; e-mail: [email protected] (C.P. Brandt). Received 8 May 2012; received in revised form 15 August 2012; accepted 20 August 2012 Abstract OBJECTIVES: To obtain a suitable conduit from the lesser (short) saphenous system for use in coronary artery bypass surgery. We wanted to perform this while the patient was in the supine position as to not disrupt the standard operation, and at the same time, util- izing the endoscopic vein harvest technique with its obvious abilities to decrease vein harvest morbidity. We also theorized that through endoscopic techniques instead of the open technique we could harvest greater lengths of conduit, thus providing quality vein segments for additional grafts if needed. METHODS: We were able to perform endoscopic vein harvest while in the supine position with one unique centrally located incision that has not been previously described. RESULTS: The lesser saphenous vein harvested in the described technique provided excellent conduit for our patients that were conduit poor. The endoscopic technique allowed increased length of harvested segments, by giving us the ability to travel under the gastrocnemius muscle with minimal morbidity as opposed to the open technique, where the traditional endpoint is the aforemen- tioned muscle. -

ICD~10~PCS Complete Code Set Procedural Coding System Sample
ICD~10~PCS Complete Code Set Procedural Coding System Sample Table.of.Contents Preface....................................................................................00 Mouth and Throat ............................................................................. 00 Introducton...........................................................................00 Gastrointestinal System .................................................................. 00 Hepatobiliary System and Pancreas ........................................... 00 What is ICD-10-PCS? ........................................................................ 00 Endocrine System ............................................................................. 00 ICD-10-PCS Code Structure ........................................................... 00 Skin and Breast .................................................................................. 00 ICD-10-PCS Design ........................................................................... 00 Subcutaneous Tissue and Fascia ................................................. 00 ICD-10-PCS Additional Characteristics ...................................... 00 Muscles ................................................................................................. 00 ICD-10-PCS Applications ................................................................ 00 Tendons ................................................................................................ 00 Understandng.Root.Operatons..........................................00 -
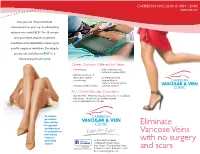
Eliminate Varicose Veins with No Surgery and Scars
CARIBBEAN VASCULAR & VEIN CLINIC www.cvctt.com Now you can show immediate improvement on your legs by eliminating varicose veins with EVLT®. This 45-minute laser procedure requires no general anesthesia or hospitalization, meaning no painful surgery or downtime. Deciding to get the safe and effective EVLT® is a choice everyone will notice. Other Options Offered for Veins • Sclerotherapy • Subfascial Endoscopic Perforator Ligation (SEPS) • COMPASS protocol of ultrasound- guided • Conventional Open sclerotherapy. Surgery (High or CARIBBEAN Sapheno-femoral Ligation • Ambulatory Phlebectomy and Stab Avulsion) VASCULAR & VEIN CLINIC For Other Vascular Disorders • Diabetic feet • Peripheral Vascular disease (poor circulation) • Aneurysms • Dialysis Access for Renal Failure • Carotid interventions for Strokes • 45-minute CARIBBEAN procedure • No scarring VASCULAR & VEIN • No general CLINIC Eliminate anesthesia or hospitalization Varicose Veins • Immediate return to your daily St. Clair Medical Centre, with no surgery routine 18 Elizabeth Street, St. Clair, Port of Spain, Trinidad, West Indies Search: CARIBBEAN VASCULAR & VEIN CLINIC T: (868) 622 9665 • F: (868) 622 9665 and scars E: [email protected] CARIBBEAN VASCULAR & VEIN CLINIC www.cvctt.com About EVLT® EVLT® is a quick, minimally invasive laser procedure that leaves no scar and can be performed in the vascular clinic under local anesthesia. The treatment takes less than one hour. What does EVLT® stand for? Here’s what to expect EndoVenous Laser Treatment • Your doctor uses ultrasound to map out your vein. Varicose Vein Treatment How does the procedure actually work? The images below illustrate varicose vein pictures from • Local anesthetic is applied. A laser fiber is fired inside and along the length of your before and after EVLT® treatment. -

Femoral Nerve Block Versus Spinal Anesthesia for Lower Limb
Alexandria Journal of Anaesthesia and Intensive Care 44 Femoral Nerve Block versus Spinal Anesthesia for Lower Limb Peripheral Vascular Surgery By Ahmed Mansour, MD Assistant Professor of Anesthesia, Faculty of Medicine, Alexandria University. Abstract Perioperative cardiac complications occur in 4% to 6% of patients undergoing infrainguinal revascularization under general, spinal, or epidural anesthesia. The risk may be even greater in patients whose cardiac disease cannot be fully evaluated or treated before urgent limb salvage operations. Prompted by these considerations, we investigated the feasibility and results of using femoral nerve block with infiltration of the genito4femoral nerve branches in these high-risk patients. Methods: Forty peripheral vascular reconstruction of lower limbs were performed under either spinal anesthesia (20 patients) or femoral nerve block with infiltration of genito-femoral nerve branches supplemented with local infiltration at the site of dissection as needed (20 patients). All patients had arterial lines. Arterial blood pressure and electrocardiographic monitoring was continued during surgery, in PACU and in the intensive care units. Results: Operations included femoral-femoral, femoral-popliteal bypass grafting and thrombectomy. The intra-operative events showed that the mean time needed to perform the block and dose of analgesics and sedatives needed during surgery was greater in group I (FNB,) compared to group II [P=0.01*, P0.029* , P0.039*], however, the time needed to start surgery was shorter in group I than in group II [P=0. 039]. There were no block failures in either group, but local infiltration in the area of the dissection with 2 ml (range 1-5 ml) of 1% lidocaine was required in 4 (20%) patients in FNB group vs none in the spinal group. -

Leg Saphenous Vein Stripping with Powered Phlebectomy with Saphenectomy with Greater Saphenectomy Consent Form
Left Right Bilateral Leg Saphenous Vein Stripping With Powered Phlebectomy With Saphenectomy With Greater Saphenectomy Consent Form Patient Name: Date of Birth: Guardian Name (if applicable): Patient ID: Washington State law guarantees that you have both the right and the obligation to make decisions regarding your health care. Your physician can provide you with the necessary information and advice, but as a member of the health care team, you must participate in the decision making process. This form acknowledges your consent to treatment recommended by your physician. 1 MY PROCEDURE I hereby give my consent for Dr. or his/her associates to perform a Left Right Bilateral Leg Saphenous Vein Stripping With Powered Phlebectomy With Saphenectomy With Greater Saphenectomy upon me. I understand the procedure is to be performed at the First Hill Surgery Center. This has been recommended to me by my physician in order to diagnose and/or treat Left Right Bilateral varicose veins. I understand that the procedure or treatment can be described as follows: Removal of the saphenous vein through small incisions, removal of varicose veins using a powered phlebectomy device (Trivex). This procedure requires anesthesia. Either general or spinal anesthetic are appropriate; your anesthesiologist will help determine which is most appropriate for you. 2 MY BENEFITS Some potential benefits of this procedure include: Relief of symptoms associated with superficial venous reflux and elimination of prominent varicose veins. While saphenous vein stripping and powered phlebectomy is often an effective test/treatment for varicose veins and superficial venous insufficiency, not all conditions, diseases or problems can be diagnoses or treated solely by saphenous vein stripping and powered phlebectomy. -

Varicose Vein and Venous Insufficiency Treatments
Medica Policy No. III-SUR.26 UTILIZATION MANAGEMENT POLICY TITLE: VARICOSE VEIN AND VENOUS INSUFFICIENCY TREATMENTS EFFECTIVE DATE: January 18, 2021 This policy was developed with input from specialists in general surgery, vascular surgery and interventional radiology, and endorsed by the Medical Policy Committee. IMPORTANT INFORMATION – PLEASE READ BEFORE USING THIS POLICY These services may or may not be covered by all Medica plans. Please refer to the member’s plan document for specific coverage information. If there is a difference between this general information and the member’s plan document, the member’s plan document will be used to determine coverage. With respect to Medicare and Minnesota Health Care Programs, this policy will apply unless these programs require different coverage. Members may contact Medica Customer Service at the phone number listed on their member identification card to discuss their benefits more specifically. Providers with questions about this Medica utilization management policy may call the Medica Provider Service Center toll-free at 1-800-458-5512. Medica utilization management policies are not medical advice. Members should consult with appropriate health care providers to obtain needed medical advice, care and treatment. PURPOSE To promote consistency between utilization management reviewers by providing the criteria that determines the medical necessity. BACKGROUND Definitions: A. Cyanoacrylate adhesive closure of symptomatic varicose veins is a minimally invasive procedure that uses a specially formulated medical adhesive (glue) that is injected into the vein using the VenaSeal™ closure system. The cyanoacrylate adhesive permanently closes the diseased vein. B. Duplex ultrasonography/Doppler ultrasound are two imaging modalities done sequentially to outline anatomical structure of blood vessels(duplex) and to detect flow, direction of flow and flow velocity of the blood through vessels. -

Selected Treatments for Varicose Veins Final Evidence Report
Selected treatments for varicose veins Final evidence report April 14, 2017 Health Technology Assessment Program (HTA) Washington State Health Care Authority PO Box 42712 Olympia, WA 98504-2712 (360) 725-5126 www.hca.wa.gov/about-hca/health-technology-assessment [email protected] Selected Treatments for Varicose Veins A Health Technology Assessment Prepared for Washington State Health Care Authority Final REPORT April 14, 2017 Acknowledgement This report was prepared by: Hayes, Inc. 157 S. Broad Street Suite 200 Lansdale, PA 19446 P: 215.855.0615 F: 215.855.5218 This report is intended to provide research assistance and general information only. It is not intended to be used as the sole basis for determining coverage policy or defining treatment protocols or medical modalities, nor should it be construed as providing medical advice regarding treatment of an individual’s specific case. Any decision regarding claims eligibility or benefits, or acquisition or use of a health technology is solely within the discretion of your organization. Hayes, Inc. assumes no responsibility or liability for such decisions. Hayes employees and contractors do not have material, professional, familial, or financial affiliations that create actual or potential conflicts of interest related to the preparation of this report. WA – Health Technology Assessment April 14, 2017 Table of Contents EVIDENCE SUMMARY ......................................................................................................................... 1 Summary of Clinical Background -

Our Vascular Surgery Capabilities Include Treatment for the Following
Vascular and EXPERIENCE MATTERS Endovascular The vascular and endovascular surgeons at LVI are highly experienced at performing vascular surgery and Surgery minimally invasive vascular therapies, and they are leading national experts in limb salvage. We invite you to consult with us, and allow us the opportunity to share our experience and discuss the appropriateness of one Our vascular surgery or more of our procedures for your patients. capabilities include treatment for the following conditions: Abdominal Aortic Peripheral Aneurysm Aneurysm Peripheral Artery Aortic Dissection Disease Aortoiliac Occlusive Portal Hypertension Disease Pulmonary Embolism Ritu Aparajita, MD Tushar Barot, MD Atherosclerosis Renovascular Vascular Surgeon Vascular Surgeon Carotid Artery Disease Conditions Chronic Venous Stroke Insufficiency Thoracic Aortic Deep Vein Aneurysm Thrombosis Vascular Infections Fibromuscular Vascular Trauma Disease Medicine Vasculitis Giant Cell Arteritis Visceral Artery Lawrence Sowka, MD Mesenteric Ischemia without limits Aneurysm Vascular Surgeon 1305 Lakeland Hills Blvd. Lakeland, FL 33805 lakelandvascular.com P: 863.577.0316 F: 1.888.668.7528 PROCEDURES WE PERFORM Minimally Angiogram and Arteriogram Endovascular treatment These vascular imaging tests allow our vascular Performed inside the blood vessel, endovascular specialists to assess blood flow through the arteries treatments are minimally invasive procedures to treat invasive and and check for blockages. In some cases, treatments peripheral artery disease. may be performed during one of these tests. Hybrid Procedures for Vascular Blockage surgical Angioplasty and Vascular Stenting Combines traditional open surgery with endovascular Angioplasty uses a balloon-tipped catheter to open a therapy to repair vessels or place stents, when an blocked blood vessel. Sometimes, the placement of endovascular procedure by itself is not possible for treatment a mesh tube inside the artery is required to keep the the patient. -

Imagingadvances
ImagingAdvances VOLUME 5 ISSUE 1 Spring 2013 New Facility Supports More In-Office Procedures by VIVA’s Highly Trained Vascular Surgeons Local Physicians Consult with RAF When Imaging is Vital to Patient Care Diagnostic radiologists are best known for their behind-the-scenes interpretation of medical imaging test results. Yet their collaboration with other medical specialists is equally critical to patient care. David L. Glasser, MD, president of Radiologic Associates of Fredericksburg (RAF), said he and the practice’s other board-certified, fellowship-trained diagnostic radiologists spend a significant part of each day discussing cases and medical imaging tests with patients’ physicians. Typical cases include: • Answering an orthopedic surgeon’s questions about a patient’s imaging tests before surgery to repair a torn meniscus. • Showing an oncologist how a patient’s lymph nodes and tumors are responding to cancer treatment. Dr. D’Addio (right) views real-time medical images to guide a vascular surgery procedure at VIVA. He is assisted by Medical Assistant Stephanie Finley. • Discussing test findings with a patient’s primary care physician When local vascular surgeon Victor J. D’Addio, MD, announced he was joining Radiologic to aid in a diagnosis. Associates of Fredericksburg (RAF) in 2009, some of his patients and medical colleagues Diagnostic Radiology continued page 3 were perplexed. Was Dr. D’Addio switching medical specialties? The answer was “no.” Dr. D’Addio moved his vascular surgery practice to RAF’s interventional radiology and vascular program, Virginia Interventional & Vascular Associates (VIVA), because the two specialties complement each other. In fact, several other radiology groups with interventional radiology sub-specialists in the United States have vascular surgeons as part of their staff. -

RAD-AID Global Curriculum for Interventional Radiology
RAD-AID Global Curriculum for Interventional Radiology Editors: Andrew Kesselman MD, Chad Wilcox MD, Kevin Anton MD, Frances Colgan MBBS FRCR, Bob Dixon MD. Version 2 - January 2021 1 Contents .................................................................................................................................................. 1 RAD-AID Global Curriculum for Interventional Radiology ........................................................... 1 Background ............................................................................................................................ 3 Introduction ......................................................................................................................... 3 Clinical practice and longitudinal care ................................................................................. 3 Limitations in low resource settings ..................................................................................... 3 Purpose .................................................................................................................................. 4 Clinical teaching and experience recommendations ............................................................... 5 Curriculum overview ........................................................................................................... 5 Prerequisites ....................................................................................................................... 5 Clinical Training ................................................................................................................. -

Endovascular Treatment for Iliac Vein Compression Syndrome: a Comparison Between the Presence and Absence of Secondary Thrombosis
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by PubMed Central Endovascular Treatment for Iliac Vein Compression Syndrome: a Comparison between the Presence and Absence of Secondary Thrombosis Wen-Sheng Lou, MD Jian-Ping Gu, MD Objective: To evaluate the value of early identification and endovascular treat- ment of iliac vein compression syndrome (IVCS), with or without deep vein throm- Xu He, MD bosis (DVT). Liang Chen, MD Hao-Bo Su, MD Materials and Methods: Three groups of patients, IVCS without DVT (group 1, Guo-Ping Chen, MD n = 39), IVCS with fresh thrombosis (group 2, n = 52) and IVCS with non-fresh thrombosis (group 3, n = 34) were detected by Doppler ultrasonography, magnetic Jing-Hua Song, MD resonance venography, computed tomography or venography. The fresh venous Tao Wang, MD thrombosis were treated by aspiration and thrombectomy, whereas the iliac vein compression per se were treated with a self-expandable stent. In cases with fresh thrombus, the inferior vena cava filter was inserted before the thrombosis suction, mechanical thrombus ablation, percutaneous transluminal angioplasty, stenting or transcatheter thrombolysis. Results: Stenting was performed in 111 patients (38 of 39 group 1 patients and 73 of 86 group 2 or 3 patients). The stenting was tried in one of group 1 and in three of group 2 or 3 patients only to fail. The initial patency rates were 95% (group 1), 89% (group 2) and 65% (group 3), respectively and were significantly different (p = 0.001). Further, the six month patency rates were 93% (group 1), Index terms: 83% (group 2) and 50% (group 3), respectively, and were similarly significantly Iliac vein compression syndrome different (p = 0.001). -

Ambulatory Phlebectomy INFORMED CONSENT
Ambulatory Phlebectomy INFORMED CONSENT INTRODUCTION: Ambulatory Phlebectomy is a procedure used to remove varicose veins that are near the surface. This procedure is done under local anesthesia. This treatment is used to remove larger veins that are close to the surface. Small stab incisions are made in the skin and the veins are pulled out of these incisions with a small hook. There will be many small incisions in the skin. These will incisions will leave small scars. The incisions may be left open, closed with small pieces of tape or occasionally sutured closed. Occasionally a slightly larger incision will be needed to remove larger veins or in the presence of scar tissue making the dissection more tedious. The pain is usually minor and little scarring is anticipated. A relatively short recovery following the procedure can be expected. The veins being treated are generally removed in one treatment. Additional veins can develop in the areas treated but the vessels removed will not come back. PROCEDURE DESCRIPTION: On the day of your Ambulatory Phlebectomy procedure, staff at The re*be Skin Clinic will answer any last minute questions you might have, and prepare you for the procedure. The skin will be marked to show the location of the veins to be removed. These marks can remain visible on you skin for about 1 week rarely more than that. Hair in the treatment areas may be clipped and the skin will be cleansed. You will be positioned on a power procedure table. Medicated ointment may be applied to your skin to temporarily anesthetize the area being treated.