State of The
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Living with Mast Cell Activation Syndrome
Anne Maitland, MD, PhD Living with Medical Director, Comprehensive Allergy Mast Cell & Asthma Care Activation Asst Professor, Dept of Medicine – Clinical Immunology Syndrome Icahn School of Medicine at Mt Sinai, New York Got MCAS? Mast Cell mediated disorders are common u 1 out of 2 of us are coping with some chronic immune mediated disorder. o ‘allergies’(rhinitis), sinus infections, hives (urticaria),food allergy/intolerance, skin swelling (angioedema), Anaphylaxis Signs and Symptoms eczema (atopic dermatitis and contact dermatitis), asthma issues, and the prototype of immediate hypersensitivity syndromes, anaphylaxis Why the rise in hypersensitivity disorders? Our genes in this environment! The human race has come to dominate its environment so completely that any analysis of the increase or appearance of a disease has to take changes in our lifestyle into account. In the case of allergic disease [hypersensitivity disorders] changes in our environment, diet, water quality, and personal behavior over the last 150 years have played a dominant role in the specificity of these diseases, as well as in prevalence and severity… it is clear that the consequences of hygiene, indoor entertainment, and changes in diet or physical activity have never been predicted. Thomas A. E. Platts-Mills, MD, PhD, FRS, The allergy epidemics: 1870-2010; J Allergy Clin Immunol 2015;136:3-13. Why? Trauma Stress Infection Connective Tissue Chemical Disorder exposure PIDD -manufactured Autoimmune Dz. -mold, Mastocytosis mycotoxins Hypertryptasemia (naturally Atopic Disorders occuring) Mast cell activation syndrome is easily treated, if it's But most patients with recognized MCAD suffer for Patients with mast cell activation syndrome (MCAS) frequently go for years without an accurate diagnosis… Harding, Reuters Health-New York, 2011 years… It is very common for one hypersensitivity condition to progress/morph into another, be provoked by more triggers. -

Revertant Mosaicism in a Human Skin Fragility Disorder Results from Slipped Mispairing and Mitotic Recombination
Revertant mosaicism in a human skin fragility disorder results from slipped mispairing and mitotic recombination Dimitra Kiritsi, … , Leena Bruckner-Tuderman, Cristina Has J Clin Invest. 2012;122(5):1742-1746. https://doi.org/10.1172/JCI61976. Brief Report Dermatology Spontaneous gene repair, also called revertant mosaicism, has been documented in several genetic disorders involving organs that undergo self-regeneration, including the skin. Genetic reversion may occur through different mechanisms, and in a single individual, the mutation can be repaired in various ways. Here we describe a disseminated pattern of revertant mosaicism observed in 6 patients with Kindler syndrome (KS), a genodermatosis caused by loss of kindlin-1 (encoded by FERMT1) and clinically characterized by patchy skin pigmentation and atrophy. All patients presented duplication mutations (c.456dupA and c.676dupC) in FERMT1, and slipped mispairing in direct nucleotide repeats was identified as the reversion mechanism in all investigated revertant skin spots. The sequence around the mutations demonstrated high propensity to mutations, favoring both microinsertions and microdeletions. Additionally, in some revertant patches, mitotic recombination generated areas with homozygous normal keratinocytes. Restoration of kindlin-1 expression led to clinically and structurally normal skin. Since loss of kindlin-1 severely impairs keratinocyte proliferation, we predict that revertant cells have a selective advantage that allows their clonal expansion and, consequently, the improvement of the skin condition. Find the latest version: https://jci.me/61976/pdf Brief report Revertant mosaicism in a human skin fragility disorder results from slipped mispairing and mitotic recombination Dimitra Kiritsi,1 Yinghong He,1 Anna M.G. Pasmooij,2 Meltem Onder,3 Rudolf Happle,1 Marcel F. -

RD-Action Matchmaker – Summary of Disease Expertise Recorded Under
Summary of disease expertise recorded via RD-ACTION Matchmaker under each Thematic Grouping and EURORDIS Members’ Thematic Grouping Thematic Reported expertise of those completing the EURORDIS Member perspectives on Grouping matchmaker under each heading Grouping RD Thematically Rare Bone Achondroplasia/Hypochondroplasia Achondroplasia Amelia skeletal dysplasia’s including Achondroplasia/Growth hormone cleidocranial dysostosis, arthrogryposis deficiency/MPS/Turner Brachydactyly chondrodysplasia punctate Fibrous dysplasia of bone Collagenopathy and oncologic disease such as Fibrodysplasia ossificans progressive Li-Fraumeni syndrome Osteogenesis imperfecta Congenital hand and fore-foot conditions Sterno Costo Clavicular Hyperostosis Disorders of Sex Development Duchenne Muscular Dystrophy Ehlers –Danlos syndrome Fibrodysplasia Ossificans Progressiva Growth disorders Hypoparathyroidism Hypophosphatemic rickets & Nutritional Rickets Hypophosphatasia Jeune’s syndrome Limb reduction defects Madelung disease Metabolic Osteoporosis Multiple Hereditary Exostoses Osteogenesis imperfecta Osteoporosis Paediatric Osteoporosis Paget’s disease Phocomelia Pseudohypoparathyroidism Radial dysplasia Skeletal dysplasia Thanatophoric dwarfism Ulna dysplasia Rare Cancer and Adrenocortical tumours Acute monoblastic leukaemia Tumours Carcinoid tumours Brain tumour Craniopharyngioma Colon cancer, familial nonpolyposis Embryonal tumours of CNS Craniopharyngioma Ependymoma Desmoid disease Epithelial thymic tumours in -

Dumitras, Cu, MC; Popa, A.; Petca, A.; Miulescu, R.-G. Cutaneous Mastocytosis in Childhood—Update from the Literature
Journal of Clinical Medicine Review Cutaneous Mastocytosis in Childhood—Update from the Literature 1,2 1,3 1,4 1,5, Florica Sandru ,Răzvan-Cosmin Petca , Monica Costescu , Mihai Cristian Dumitras, cu *, Adelina Popa 2, Aida Petca 1,6,* and Raluca-Gabriela Miulescu 1,7 1 “Carol Davila” University of Medicine and Pharmacy, 030167 Bucharest, Romania; fl[email protected] (F.S.); [email protected] (R.-C.P.); [email protected] (M.C.); [email protected] (R.-G.M.) 2 Department of Dermatology, Elias University Emergency Hospital, 0611461 Bucharest, Romania; [email protected] 3 Department of Urology, “Prof. Dr. Theodor Burghele” Clinical Hospital, 061344 Bucharest, Romania 4 Department of Dermatology, “Dr. Victor Babes” Clinical Hospital of Infectious and Tropical Diseases, 030303 Bucharest, Romania 5 Department of Obstetrics & Gynecology, University Emergency Hospital, 050098 Bucharest, Romania 6 Department of Obstetrics & Gynecology, Elias University Emergency Hospital, 0611461 Bucharest, Romania 7 Department of Dermatology, Vălenii de Munte Hospital, 106400 Prahova, Romania * Correspondence: [email protected] (M.C.D.); [email protected] (A.P.); Tel.: +40-722-223223 (M.C.D.); +40-745-787448 (A.P.) Abstract: Mastocytosis (M) represents a systemic pathology characterized by increased accumulation and clonal proliferation of mast cells in the skin and/or different organs. Broadly, M is classified into two categories: Cutaneous mastocytosis (CM) and systemic mastocytosis (SM). In children, CM is Citation: Sandru, F.; Petca, R.-C.; the most frequent form. Unfortunately, pathogenesis is still unclear. It is thought that genetic factors Costescu, M.; Dumitras, cu, M.C.; are involved, but further studies are necessary. As for features of CM, the lesions differ in clinical Popa, A.; Petca, A.; Miulescu, R.-G. -

PROMIS Itch Questionnaire – Children Symptom (PIQ-C-Symptom) Letter of Intent
Clinical Outcome Assessments (COA) Qualification Program DDT COA #000140: PROMIS Itch Questionnaire – Children Symptom (PIQ-C-Symptom) Letter of Intent Section 1. Administrative Structure This project has been led by Amy Paller, MD (PI of sub-study that developed the PIQ-C and co-PI of the PEPR project at Northwestern University) from the Dermatology and Pediatrics departments at Northwestern University (676 N. St. Clair, Suite 1600, Chicago, IL 60611) and Jin-Shei Lai, Ph.D. (contact co-PI of the PEPR project at Northwestern University) from the Medical Social Sciences and Pediatrics departments at Northwestern University (625 N. Michigan Avenue, 21st floor, Chicago, IL 60611). Dr. Paller has had 35 years of experience in caring for children with disorders causing itch. She is Chair of the Dept. of Dermatology, directs the Skin Disease Research Center at Northwestern (now Skin Biology and Diseases Resource-based Center) as well as the Pediatric Dermatology Clinical Research Unit, and has been the PI of more than 100 clinical trials in children with disorders associated with pruritus (atopic dermatitis, epidermolysis bullosa, ichthyosis, psoriasis), most of which involve measuring itch and quality of life. She has authored more than 250 peer-reviewed papers related to these disorders. She has been working on developing and validating PRO tools during the past 5 years, including through this project. Dr. Lai has significant experience in patient reported outcomes, including burden of disease and treatment impact studies across a range of pediatric and adult conditions. She has served as a principal investigator and co-investigator on several federal and foundation funded projects and is the lead developer of several pediatric and adult quality of life and symptom measurement instruments, including the PROMIS Fatigue and Cognition item banks for both adults and children, pediatric Neuro-QoL measurement system, and the pediatric Functional Assessment of Chronic Illness Therapy (pedsFACIT). -

Genodermatoses
GENODERMATOSES Genodermatoses What’s new? Nigel P Burrows C Filaggrin mutations underlie ichthyosis vulgaris and are a risk factor for atopy including eczema, allergic sensitization, asthma, allergic rhinitis and peanut allergy Abstract C A new classification and nomenclature for ichthyoses was Genetic skin diseases encompass a spectrum from the common to the published in 2009, peeling skin syndromes which may be rare. It is important for the clinician to be alert to the possibility that confused for the milder subtypes of epidermolysis bullosa are the patient may be presenting for the first time with one or more features distinct genetic entities of a genetic disease so that appropriate investigation and counselling can C Emerging evidence that pseudoxanthoma elasticum is a meta- take place. Recent discoveries have helped the understanding of many of bolic disorder resulting in calcification of elastic fibres these disorders. A few common and important genodermatoses are high- C Mammalian target of rapamycin (mTOR) inhibitor therapies are lighted in this article. showing promise in tuberous sclerosis complex C Vascular anomalies on the skin may be the presenting feature of Keywords cancer syndromes; collagen; epidermolysis bullosa; filaggrin; inherited syndromes genodermatoses; ichthyosis; keratinization; pseudoxanthoma elasticum; vascular anomalies X-linked recessive ichthyosis In 75% of cases of X-linked recessive ichthyosis (XLRI) (Figure 1), scaling is present in the first week of life and tends to progress into adolescence. In contrast to IV, the flexures may be Genetic skin diseases encompass a spectrum from the common involved. A third of cases are associated with a prolonged labour. (e.g. atopic eczema) to the rare (e.g. -

Urticaria Pigmentosa: a Case Report and Review of Current Standards in the Diagnosis of Systemic Mastocytosis
Urticaria Pigmentosa: A Case Report and Review of Current Standards in the Diagnosis of Systemic Mastocytosis Riddhi J. Shah, DO,* Mark A. Kuriata, DO, FAOCD** *Dermatology Resident, 2nd year, MSUCOM/Lakeland Regional Medical Center, St. Joseph, MI **Dermatology Residency Program Director, MSUCOM/Lakeland Regional Medical Center, St. Joseph, MI Abstract Mastocytosis is a group of diseases that is characterized by mast-cell infiltration of the skin. The cutaneous forms of the disease are most identifiable, yet it is important to recognize the progression to systemic disease due to the eaffect on morbidity and mortality. We Our goal is to describe a case of cutaneous mastocytosis as well as review the current standards in diagnosis and management of systemic mastocytosis. Introduction patient had several bouts of loose stools. This and spleen did not reveal any organomegaly. Mast-cell disease is a rare disorder, primarily was accompanied by bloating and indigestion, Muscle strength and tone appeared to be within of childhood, that is usually self-resolving. which occurred 30 minutes after a meal. A normal limits. There were no palpable lymph Approximately two-thirds of cases are limited to colonoscopy was performed one year prior at an nodes in the neck, axillae or groin regions. outside facility, and it was within normal limits. the skin. The most common forms of cutaneous Our differential diagnosis included systemic However, no biopsies were performed to look mastocytosis include: mastocytoma, urticaria mastocytosis as well as carcinoid syndrome, for mast-cell infiltration of the digestive tract. pigmentosa, telangiectasia macularis eruptiva pheochromocytoma, inflammatory bowel disease, Our patient also had sharp, intermittent, left perstans, maculopapular cutaneous mastocytosis, urticaria, and myeloproliferative disorder. -

Genevista Epidermolysis Bullosa
GeNeViSTA Epidermolysis Bullosa: An Update Neetu Bhari1, Neerja Gupta2 1Department of Dermatology and Venereology, All India Institute of Medical Sciences, New Delhi, India 2Division of Genetics, Department of Pediatrics, All India Institute of Medical Sciences, New Delhi, India Correspondence to: Dr Neerja Gupta Email: [email protected] Abstract Classification and pathogenesis Epidermolysis bullosa (EB) is caused by mutation in Mutation in various components of the basement various components of the basement membrane membrane zone responsible for structural support zone and is characterized by increased fragility of in keratinocytes and adhesion of epidermis and skin and mucous membrane. There are four major dermis, results in different types of epidermol- types based on the level of split at the basement ysis bullosa (Figure 1). The new approach for membrane zone – involvement of basal layer of classification in EB is termed as “onion skinning” epidermis in epidermolysis bullosa simplex (EBS), and sequentially takes account of the level of split lamina lucida in junctional EB (JEB) and sublamina at the dermato-epidermal basement membrane densa in dystrophic EB (DEB) while Kindler syn- zone, phenotypic features and genetic characteris- drome (KS) can exhibit multiple levels of split. More tics such as mode of inheritance, targeted protein than 19 genes have been described resulting in the and its relative expression in the basement mem- various subtypes of these 4 major types giving rise brane zone, the involved gene and the type of to diversity of phenotypic expressions. Diagnosis mutation (Fine et al., 2014). is based on the “onion skin approach” which in- The level of split is the basal layer of the cludes clinical presentation, family history, antigen epidermis in epidermolysis bullosa simplex (EBS) mapping and genetic mutation analysis. -

How to Deal with Skin Biopsy in an Infant with Blisters?
Review How to Deal with Skin Biopsy in an Infant with Blisters? Stéphanie Leclerc-Mercier Reference Center for Genodermatoses (MAGEC Center), Department of Pathology, Necker-Enfants Malades Hospital, Paris Centre University, 75015 Paris, France; [email protected] Abstract: The onset of blisters in a neonate or an infant is often a source of great concern for both parents and physicians. A blistering rash can reveal a wide range of diseases with various backgrounds (infectious, genetic, autoimmune, drug-related, traumatic, etc.), so the challenge for the dermatologist and the pediatrician is to quickly determine the etiology, between benign causes and life-threatening disorders, for a better management of the patient. Clinical presentation can provide orientation for the diagnosis, but skin biopsy is often necessary in determining the cause of blister formations. In this article, we will provide information on the skin biopsy technique and discuss the clinical orientation in the case of a neonate or infant with a blistering eruption, with a focus on the histology for each etiology. Keywords: blistering eruption; infant; skin biopsy; genodermatosis; SSSS; hereditary epidermolysis bul- losa; keratinopathic ichthyosis; incontinentia pigmenti; mastocytosis; auto-immune blistering diseases 1. Introduction The onset of blisters in a neonate or an infant (<2 years old) is a source of great concern for both parents and physicians. Therefore, a precise diagnosis, between benign causes and Citation: Leclerc-Mercier, S. How to life-threatening disorders, is quickly needed for the best management of the baby. Deal with Skin Biopsy in an Infant Several diseases with various backgrounds (infectious, genetic, autoimmune, drug- with Blisters? Dermatopathology 2021, related, traumatic, etc.) can lead to a blistering eruption. -
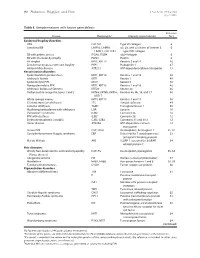

Table I. Genodermatoses with Known Gene Defects 92 Pulkkinen
92 Pulkkinen, Ringpfeil, and Uitto JAM ACAD DERMATOL JULY 2002 Table I. Genodermatoses with known gene defects Reference Disease Mutated gene* Affected protein/function No.† Epidermal fragility disorders DEB COL7A1 Type VII collagen 6 Junctional EB LAMA3, LAMB3, ␣3, 3, and ␥2 chains of laminin 5, 6 LAMC2, COL17A1 type XVII collagen EB with pyloric atresia ITGA6, ITGB4 ␣64 Integrin 6 EB with muscular dystrophy PLEC1 Plectin 6 EB simplex KRT5, KRT14 Keratins 5 and 14 46 Ectodermal dysplasia with skin fragility PKP1 Plakophilin 1 47 Hailey-Hailey disease ATP2C1 ATP-dependent calcium transporter 13 Keratinization disorders Epidermolytic hyperkeratosis KRT1, KRT10 Keratins 1 and 10 46 Ichthyosis hystrix KRT1 Keratin 1 48 Epidermolytic PPK KRT9 Keratin 9 46 Nonepidermolytic PPK KRT1, KRT16 Keratins 1 and 16 46 Ichthyosis bullosa of Siemens KRT2e Keratin 2e 46 Pachyonychia congenita, types 1 and 2 KRT6a, KRT6b, KRT16, Keratins 6a, 6b, 16, and 17 46 KRT17 White sponge naevus KRT4, KRT13 Keratins 4 and 13 46 X-linked recessive ichthyosis STS Steroid sulfatase 49 Lamellar ichthyosis TGM1 Transglutaminase 1 50 Mutilating keratoderma with ichthyosis LOR Loricrin 10 Vohwinkel’s syndrome GJB2 Connexin 26 12 PPK with deafness GJB2 Connexin 26 12 Erythrokeratodermia variabilis GJB3, GJB4 Connexins 31 and 30.3 12 Darier disease ATP2A2 ATP-dependent calcium 14 transporter Striate PPK DSP, DSG1 Desmoplakin, desmoglein 1 51, 52 Conradi-Hu¨nermann-Happle syndrome EBP Delta 8-delta 7 sterol isomerase 53 (emopamil binding protein) Mal de Meleda ARS SLURP-1 -

Adult-Onset Mastocytosis in the Skin Is Highly Suggestive of Systemic
Modern Pathology (2014) 27, 19–29 & 2014 USCAP, Inc. All rights reserved 0893-3952/14 $32.00 19 Adult-onset mastocytosis in the skin is highly suggestive of systemic mastocytosis Sabina Berezowska1, Michael J Flaig2, Franziska Rue¨ff2, Christoph Walz1, Torsten Haferlach3, Manuela Krokowski4, Roswitha Kerler1, Karina Petat-Dutter1, Hans-Peter Horny3 and Karl Sotlar1 1Institute of Pathology, University of Munich, Munich, Germany; 2Department of Dermatology and Allergology, University of Munich, Munich, Germany; 3MLL Munich Leukemia Laboratory, Munich, Germany and 4Institute of Pathology, University of Schleswig Holstein, Lu¨beck, Germany Adult-onset urticaria pigmentosa/mastocytosis in the skin almost always persists throughout life. The prevalence of systemic mastocytosis in such patients is not precisely known. Bone marrow biopsies from 59 patients with mastocytosis in the skin and all available skin biopsies (n ¼ 27) were subjected to a meticulous cytological, histological, immunohistochemical, and molecular analysis for the presence of WHO-defined diagnostic criteria for systemic mastocytosis: compact mast cell infiltrates (major criterion); atypical mast cell morphology, KIT D816V, abnormal expression of CD25 by mast cells, and serum tryptase levels 420 ng/ml (minor criteria). Systemic mastocytosis is diagnosed when the major diagnostic criterion plus one minor criterion or at least three minor criteria are fulfilled. Systemic mastocytosis was confirmed in 57 patients (97%) by the diagnosis of compact mast cell infiltrates plus at least one minor diagnostic criterion (n ¼ 42, 71%) or at least three minor diagnostic criteria (n ¼ 15, 25%). In two patients, only two minor diagnostic criteria were detectable, insufficient for the diagnosis of systemic mastocytosis. By the use of highly sensitive molecular methods, including the analysis of microdissected mast cells, KIT D816V was found in all 58 bone marrow biopsies investigated for it but only in 74% (20/27) of the skin biopsies. -
Blueprint Genetics Comprehensive Immune and Cytopenia Panel
Comprehensive Immune and Cytopenia Panel Test code: IM0901 Is a 642 gene panel that includes assessment of non-coding variants. Is ideal for patients with a clinical suspicion of an inborn error of immunity, such as, Primary Immunodeficiency, Bone Marrow Failure Syndrome, Dyskeratosis Congenita, Neutropenia, Thrombocytopenia, Hemophagocytic Lymphohistiocytosis, Autoinflammatory Disorders, Complement System Disorder, Leukemia, or Chronic Granulomatous Disease. This panel includes most genes from Primary Immunodeficiency, Severe Combined Immunodeficiency, Complement System Disorder, Bone Marrow Failure Syndrome, Hemophagocytic Lymphohistiocytosis, Congenital Neutropenia, Thrombocytopenia, Congenital Diarrhea, Chronic Granulomatous Disease, Diamond-Blackfan Anemia, Fanconi Anemia, Dyskeratosis Congenita, Autoinflammatory Syndrome, and Hereditary Leukemia Panels as well as many other genes associated with inborn errors of immunity. Please note that unlike our other panels, this panel is on our Whole Exome Sequencing platform and cannot be customized. Pricing may vary from our regular panel pricing. About immunodeficiency and cytopenia disorders There is an enormous amount of phenotypic overlap between immunological and hematological disorders, which makes it challenging to know which of these two systems is not functioning properly. Knowing the underlying genetic cause of a person’s clinical diagnosis, especially immunodeficiency, bone marrow failure, neutropenia, thrombocytopenia, autoinflammatory disease, or bone marrow failure can sometime