Tutorial Article Local Analgesic Techniques for the Equine Head W
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Numb Tongue, Numb Lip, Numb Chin: What to Do When?
NUMB TONGUE, NUMB LIP, NUMB CHIN: WHAT TO DO WHEN? Ramzey Tursun, DDS, FACS Marshall Green, DDS Andre Ledoux, DMD Arshad Kaleem, DMD, MD Assistant Professor, Associate Fellowship Director of Oral, Head & Neck Oncologic and Microvascular Reconstructive Surgery, DeWitt Daughtry Family Department of Surgery, Division of Oral Maxillofacial Surgery, Leonard M. Miller School of Medicine, University of Miami INTRODUCTION MECHANISM OF NERVE Microneurosurgery of the trigeminal nerve INJURIES has been in the spotlight over the last few years. The introduction of cone-beam When attempting to classify the various scanning, three-dimensional imaging, mechanisms of nerve injury in the magnetic resonance neurography, maxillofacial region, it becomes clear that endoscopic-assisted surgery, and use of the overwhelming majority are iatrogenic allogenic nerve grafts have improved the in nature. The nerves that are most often techniques that can be used for affected in dento-alveolar procedures are assessment and treatment of patients with the branches of the mandibular division of nerve injuries. Injury to the terminal cranial nerve V, i.e., the trigeminal nerve. branches of the trigeminal nerve is a well- The lingual nerve and inferior alveolar known risk associated with a wide range of nerve are most often affected, and third dental and surgical procedures. These molar surgery is the most common cause 1 injuries often heal spontaneously without of injury. medical or surgical intervention. However, they sometimes can cause a variety of None of these nerves provide motor symptoms, including lost or altered innervation. However, damage to these sensation, pain, or a combination of these, nerves can cause a significant loss of and may have an impact on speech, sensation and/or taste in affected patients. -

Palatal Injection Does Not Block the Superior Alveolar Nerve Trunks: Correcting an Error Regarding the Innervation of the Maxillary Teeth
Open Access Review Article DOI: 10.7759/cureus.2120 Palatal Injection does not Block the Superior Alveolar Nerve Trunks: Correcting an Error Regarding the Innervation of the Maxillary Teeth Joe Iwanaga 1 , R. Shane Tubbs 2 1. Seattle Science Foundation 2. Neurosurgery, Seattle Science Foundation Corresponding author: Joe Iwanaga, [email protected] Abstract The superior alveolar nerves course lateral to the maxillary sinus and the greater palatine nerve travels through the hard palate. This difficult three-dimensional anatomy has led some dentists and oral surgeons to a critical misunderstanding in developing the anterior and middle superior alveolar (AMSA) nerve block and the palatal approach anterior superior alveolar (P-ASA) nerve block. In this review, the anatomy of the posterior, middle and anterior superior alveolar nerves, greater palatine nerve, and nasopalatine nerve are revisited in order to clarify the anatomy of these blocks so that the perpetuated anatomical misunderstanding is rectified. We conclude that the AMSA and P-ASA nerve blockades, as currently described, are not based on accurate anatomy. Categories: Anesthesiology, Medical Education, Other Keywords: anatomy, innervation, local anesthesia, maxillary nerve, nerve block, tooth Introduction And Background Anesthetic blockade of the posterior superior alveolar (PSA) branch of the maxillary nerve has played an important role in the endodontic treatment of irreversible acute pulpitis of the upper molar teeth except for the mesiobuccal root of the first molar tooth [1, 2]. This procedure requires precise anatomical knowledge of the pterygopalatine fossa and related structures in order to avoid unnecessary complications and to make the blockade most effective. The infraorbital nerve gives rise to middle superior alveolar (MSA) and anterior superior alveolar (ASA) branches. -

Nerves of the Orbit Optic Nerve the Optic Nerve Enters the Orbit from the Middle Cranial Fossa by Passing Through the Optic Canal
human anatomy 2016 lecture fourteen Dr meethak ali ahmed neurosurgeon Nerves of the Orbit Optic Nerve The optic nerve enters the orbit from the middle cranial fossa by passing through the optic canal . It is accompanied by the ophthalmic artery, which lies on its lower lateral side. The nerve is surrounded by sheath of pia mater, arachnoid mater, and dura mater. It runs forward and laterally within the cone of the recti muscles and pierces the sclera at a point medial to the posterior pole of the eyeball. Here, the meninges fuse with the sclera so that the subarachnoid space with its contained cerebrospinal fluid extends forward from the middle cranial fossa, around the optic nerve, and through the optic canal, as far as the eyeball. A rise in pressure of the cerebrospinal fluid within the cranial cavity therefore is transmitted to theback of the eyeball. Lacrimal Nerve The lacrimal nerve arises from the ophthalmic division of the trigeminal nerve. It enters the orbit through the upper part of the superior orbital fissure and passes forward along the upper border of the lateral rectus muscle . It is joined by a branch of the zygomaticotemporal nerve, whi(parasympathetic secretomotor fibers). The lacrimal nerve ends by supplying the skin of the lateral part of the upper lid. Frontal Nerve The frontal nerve arises from the ophthalmic division of the trigeminal nerve. It enters the orbit through the upper part of the superior orbital fissure and passes forward on the upper surface of the levator palpebrae superioris beneath the roof of the orbit . -
Periorbital Sinuses the Periorbital Sinuses Have a Close Anatomical Relationship with the Orbits (Fig 1-8)
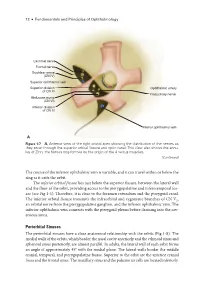
12 ● Fundamentals and Principles of Ophthalmology Lacrimal nerve Frontal nerve Trochlear nerve (CN IV) Superior ophthalmic vein Superior division Ophthalmic artery of CN III Nasociliary nerve Abducens nerve (CN VI) Inferior division of CN III Inferior ophthalmic vein A Figure 1-7 A, Anterior view of the right orbital apex showing the distribution of the nerves as they enter through the superior orbital fissure and optic canal. This view also shows the annu- lus of Zinn, the fibrous ring formed by the origin of the 4 rectus muscles. (Continued) The course of the inferior ophthalmic vein is variable, and it can travel within or below the ring as it exits the orbit. The inferior orbital fissure lies just below the superior fissure, between the lateral wall and the floor of the orbit, providing access to the pterygopalatine and inferotemporal fos- sae (see Fig 1-1). Therefore, it is close to the foramen rotundum and the pterygoid canal. The inferior orbital fissure transmits the infraorbital and zygomatic branches of CN V2, an orbital nerve from the pterygopalatine ganglion, and the inferior ophthalmic vein. The inferior ophthalmic vein connects with the pterygoid plexus before draining into the cav- ernous sinus. Periorbital Sinuses The periorbital sinuses have a close anatomical relationship with the orbits (Fig 1-8). The medial walls of the orbits, which border the nasal cavity anteriorly and the ethmoid sinus and sphenoid sinus posteriorly, are almost parallel. In adults, the lateral wall of each orbit forms an angle of approximately 45° with the medial plane. The lateral walls border the middle cranial, temporal, and pterygopalatine fossae. -

Anatomy of Maxillary and Mandibular Local Anesthesia
Anatomy of Mandibular and Maxillary Local Anesthesia Patricia L. Blanton, Ph.D., D.D.S. Professor Emeritus, Department of Anatomy, Baylor College of Dentistry – TAMUS and Private Practice in Periodontics Dallas, Texas Anatomy of Mandibular and Maxillary Local Anesthesia I. Introduction A. The anatomical basis of local anesthesia 1. Infiltration anesthesia 2. Block or trunk anesthesia II. Review of the Trigeminal Nerve (Cranial n. V) – the major sensory nerve of the head A. Ophthalmic Division 1. Course a. Superior orbital fissure – root of orbit – supraorbital foramen 2. Branches – sensory B. Maxillary Division 1. Course a. Foramen rotundum – pterygopalatine fossa – inferior orbital fissure – floor of orbit – infraorbital 2. Branches - sensory a. Zygomatic nerve b. Pterygopalatine nerves [nasal (nasopalatine), orbital, palatal (greater and lesser palatine), pharyngeal] c. Posterior superior alveolar nerves d. Infraorbital nerve (middle superior alveolar nerve, anterior superior nerve) C. Mandibular Division 1. Course a. Foramen ovale – infratemporal fossa – mandibular foramen, Canal -> mental foramen 2. Branches a. Sensory (1) Long buccal nerve (2) Lingual nerve (3) Inferior alveolar nerve -> mental nerve (4) Auriculotemporal nerve b. Motor (1) Pterygoid nerves (2) Temporal nerves (3) Masseteric nerves (4) Nerve to tensor tympani (5) Nerve to tensor veli palatine (6) Nerve to mylohyoid (7) Nerve to anterior belly of digastric c. Both motor and sensory (1) Mylohyoid nerve III. Usual Routes of innervation A. Maxilla 1. Teeth a. Molars – Posterior superior alveolar nerve b. Premolars – Middle superior alveolar nerve c. Incisors and cuspids – Anterior superior alveolar nerve 2. Gingiva a. Facial/buccal – Superior alveolar nerves b. Palatal – Anterior – Nasopalatine nerve; Posterior – Greater palatine nerves B. -

Anatomy-Nerve Tracking
INJECTABLES ANATOMY www.aestheticmed.co.uk Nerve tracking Dr Sotirios Foutsizoglou on the anatomy of the facial nerve he anatomy of the human face has received enormous attention during the last few years, as a plethora of anti- ageing procedures, both surgical and non-surgical, are being performed with increasing frequency. The success of each of those procedures is greatly dependent on Tthe sound knowledge of the underlying facial anatomy and the understanding of the age-related changes occurring in the facial skeleton, ligaments, muscles, facial fat compartments, and skin. The facial nerve is the most important motor nerve of the face as it is the sole motor supply to all the muscles of facial expression and other muscles derived from the mesenchyme in the embryonic second pharyngeal arch.1 The danger zone for facial nerve injury has been well described. Confidence when approaching the nerve and its branches comes from an understanding of its three dimensional course relative to the layered facial soft tissue and being aware of surface anatomy landmarks and measurements as will be discussed in this article. Aesthetic medicine is not static, it is ever evolving and new exciting knowledge emerges every day unmasking the relationship of the ageing process and the macroscopic and microscopic (intrinsic) age-related changes. Sound anatomical knowledge, taking into consideration the natural balance between the different facial structures and facial layers, is fundamental to understanding these changes which will subsequently help us develop more effective, natural, long-standing and most importantly, safer rejuvenating treatments and procedures. The soft tissue of the face is arranged in five layers: 1) Skin; 2) Subcutaneous fat layer; 3) Superficial musculoaponeurotic system (SMAS); 4) Areolar tissue or loose connective tissue (most clearly seen in the scalp and forehead); 5) Deep fascia formed by the periosteum of facial bones and the fascial covering of the muscles of mastication (lateral face). -

Anatomical Study of the Zygomaticotemporal Branch Inside the Orbit
Open Access Original Article DOI: 10.7759/cureus.1727 Anatomical Study of the Zygomaticotemporal Branch Inside the Orbit Joe Iwanaga 1 , Charlotte Wilson 1 , Koichi Watanabe 2 , Rod J. Oskouian 3 , R. Shane Tubbs 4 1. Seattle Science Foundation 2. Department of Anatomy, Kurume University School of Medicine 3. Neurosurgery, Complex Spine, Swedish Neuroscience Institute 4. Neurosurgery, Seattle Science Foundation Corresponding author: Charlotte Wilson, [email protected] Abstract The location of the opening of the zygomaticotemporal branch (ZTb) of the zygomatic nerve inside the orbit (ZTFIN) has significant surgical implications. This study was conducted to locate the ZTFIN and investigate the variations of the ZTb inside the orbit. A total of 20 sides from 10 fresh frozen cadaveric Caucasian heads were used in this study. The vertical distance between the inferior margin of the orbit and ZTFIN (V-ZTFIN), the horizontal distance between the lateral margin of the orbit and ZTFIN (H-ZTFIN), and the diameter of the ZTFIN (D-ZTFIN) were measured. The patterns of the ZTb inside the orbit were classified into five different groups: both ZTb and LN innervating the lacrimal gland independently (Group A), both ZTb and LN innervating the lacrimal gland with a communicating branch (Group B), ZTb joining the LN without a branch to the lacrimal gland (Group C), the ZTb going outside the orbit through ZTFIN without a branch to the lacrimal gland nor LN (Group D), and absence of the ZTb (Group E). The D-ZTFIN V-ZTFIN H-ZTFIN ranged from 0.2 to 1.1 mm, 6.6 to 21.5 mm, 2.0 to 11.3 mm, respectively. -

Numb Chin Sydrome : a Subtle Clinical Condition with Varied Etiology
OLGU SUNUMU / CASE REPORT Gülhane Tıp Derg 2015;57: 324 - 327 © Gülhane Askeri Tıp Akademisi 2015 doi: 10.5455/gulhane.44276 Numb chin sydrome : A subtle clinical condition with varied etiology Devika SHETTY (*), Prashanth SHENAI (**), Laxmikanth CHATRA (**), KM VEENA (**), Prasanna Kumar RAO (**), Rachana V PRABHU (**), Tashika KUSHRAJ (**) SUMMARY Introduction One of the rare neurologic symptoms characterized by hypoesthesia or Numb Chin Syndrome (NCS) is a sensory neuropathy cha- paresthesia of the chin and the lower lip, limited to the region served by the mental nerve is known as Numb chin syndrome. Vast etiologic factors have been racterized by altered sensation and numbness in the distribu- implicated in the genesis of numb chin syndrome. Dental, systemic and malignant tion of the mental nerve, a terminal branch of the mandibular etiologies have been well documented. We present a case of a 59 year old female patient who reported with all the classical features of numb chin syndrome. On division of trigeminal nerve. Any dysfunction along the course magnetic resonance imaging, the vascular compression of the trigeminal nerve of trigeminal nerve and its branches, intracranially and ext- root was evident which has been infrequently documented to be associated with racranially either by direct injury or compression of the nerve the condition. We have also briefly reviewed the etiology and pathogenesis of 1 numb chin syndrome and also stressed on the importance of magnetic resonance can predispose to NCS. Various etiologic factors have been imaging as an investigative modality in diagnosing the condition. considered of which dental procedures and dental pathologies Key Words: Numb Chin Syndrome, Mental nerve neuropathy, trigeminal nerve root, are the most common benign causes. -

Inferior Alveolar Nerve Trajectory, Mental Foramen Location and Incidence of Mental Nerve Anterior Loop
Med Oral Patol Oral Cir Bucal. 2017 Sep 1;22 (5):e630-5. CBCT anatomy of the inferior alveolar nerve Journal section: Oral Surgery doi:10.4317/medoral.21905 Publication Types: Research http://dx.doi.org/doi:10.4317/medoral.21905 Inferior alveolar nerve trajectory, mental foramen location and incidence of mental nerve anterior loop Miguel Velasco-Torres 1, Miguel Padial-Molina 1, Gustavo Avila-Ortiz 2, Raúl García-Delgado 3, Andrés Ca- tena 4, Pablo Galindo-Moreno 1 1 DDS, PhD, Department of Oral Surgery and Implant Dentistry, School of Dentistry, University of Granada, Granada, Spain 2 DDS, MS, PhD, Department of Periodontics, College of Dentistry, University of Iowa, Iowa City, USA 3 Specialist in Dental and Maxillofacial Radiology. Private Practice. Granada, Spain 4 PhD, Department of Experimental Psychology, School of Psychology, University of Granada, Granada, Spain Correspondence: School of Dentistry, University of Granada 18071 - Granada, Spain [email protected] Velasco-Torres M, Padial-Molina M, Avila-Ortiz G, García-Delgado R, Catena A, Galindo-Moreno P. Inferior alveolar nerve trajectory, mental foramen location and incidence of mental nerve anterior loop. Med Oral Received: 07/03/2017 Accepted: 21/06/2017 Patol Oral Cir Bucal. 2017 Sep 1;22 (5):e630-5. http://www.medicinaoral.com/medoralfree01/v22i5/medoralv22i5p630.pdf Article Number: 21905 http://www.medicinaoral.com/ © Medicina Oral S. L. C.I.F. B 96689336 - pISSN 1698-4447 - eISSN: 1698-6946 eMail: [email protected] Indexed in: Science Citation Index Expanded Journal Citation Reports Index Medicus, MEDLINE, PubMed Scopus, Embase and Emcare Indice Médico Español Abstract Background: Injury of the inferior alveolar nerve (IAN) is a serious intraoperative complication that may occur during routine surgical procedures, such as dental implant placement or extraction of impacted teeth. -

Cranial Neuralgias
CRANIAL NEURALGIAS Presented by: Neha Sharma M.D. Date: September 27th, 2019 TYPES OF NEURALGIAS ❖ TRIGEMINAL NEURALGIA ❖ GLOSSOPHARYNGEAL NEURALGIA ❖ NASOCILIARY NEURALGIA ❖ SUPERIOR LARYNGEAL NEURALGIA ❖ SUPRAORBITAL NEURALGIA ❖ OCCIPITAL NEURALGIA ❖ SPHENOPALATINE NEURALGIA ❖ GREAT AURICULAR NEURALGIA ❖ NERVUS INTERMEDIUS NEURALGIA ❖ TROCHLEAR NEURALGIA WHAT IS CRANIAL NEURALGIA? ❖ Paroxysmal pain of head, face and/or neck ❖ Unilateral sensory nerve distribution ❖ Pain is described as sharp, shooting, lancinating ❖ Primary or Secondary causes ❖ Multiple triggers TRIGEMINAL (CN V) NEURALGIA TRIGEMINAL NEURALGIA ❖ Also called Tic Douloureux ❖ Sudden, unilateral, electrical, shock-like, shooting, sharp pain. Presents affecting Cranial Nerve V; primarily V2 and V3 branches ❖ F>M; 3:1 TRIGEMINAL NEURALGIA ❖ Anatomy of Trigeminal Nerve ❖ Cranial Nerve V ❖ Three Branches: Ophthalmic, Maxillary and Mandibular ❖ Sensory supply to forehead/supraorbital, cheeks and jaw https://www.nf2is.org/cn5.php TRIGEMINAL NEURALGIA – TRIGGERS ❖ Mastication (73%) ❖ Eating (59%) ❖ Touch (69%) ❖ Talking (58%) ❖ Brushing Teeth (66%) ❖ Cold wind (50%) TYPES OF TRIGEMINAL NEURALGIA ❖ Primary/Classic/Idiopathic ❖ Vascular compression of the nerve – superior cerebellar artery ❖ Secondary/Symptomatic ❖ Caused by intracranial lesions ❖ Tumors, Strokes, Multiple Sclerosis (4%) ❖ Typical vs. Atypical ❖ Paroxysmal (79%) vs. Continuous (21%) IASP/IHS & CLASSIFICATIONS OF TRIGEMINAL NEURALGIA ❖ IASP – International Association ❖ Classifications for the Study of Pain ❖ I -

Morphometry of Bony Orbit Related to Gender in Dry Adult Skulls of South Indian Population
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Morphometry of Bony Orbit Related to Gender in Dry Adult Skulls of South Indian Population S. Senthil Kumar1, E. Gnanagurudasan2 1Professor, 2Ph.D Scholar, Department of Anatomy, Sri Ramachandra Medical College and Research Institute, Sri Ramachandra University, Porur, Chennai, Tamil Nadu. Corresponding Author: E. Gnanagurudasan Received: 16/07/2015 Revised: 11/08/2015 Accepted: 12/08/2015 ABSTRACT Introduction: Orbit lodges important structures for vision and allows passage of fine neurovascular structures in it. The knowledge of orbital morphometry helps to protect those structures during various surgical procedures. Aim: To determine the morphometry of bony orbit in dry South Indian skulls related to gender and to compare the results with previous authors. Material and Methods: The material of the present study consists of 100 orbits from 50 skulls (right & left) which are identifiable of their sex. Foetal skulls and skulls with damages in the area of measurement were excluded. All the parameters were examined by a single observer using a vernier calliper, divider and millimetre scale. In each wall of the orbit, a bony landmark is chosen from where the distance of other bony structures is measured. Result: The result of the present study showed significance with respect to gender and side. Conclusion: The data of the present study will be helpful for various surgical approaches around the orbit. Keywords: orbit, South Indian skulls, morphometry. INTRODUCTION pyramidal cavity formed by seven bones The bony orbits are skeletal cavities namely maxilla, palatine, frontal, zygomatic, located on either side of the root of the nose. -

MBB: Head & Neck Anatomy
MBB: Head & Neck Anatomy Skull Osteology • This is a comprehensive guide of all the skull features you must know by the practical exam. • Many of these structures will be presented multiple times during upcoming labs. • This PowerPoint Handout is the resource you will use during lab when you have access to skulls. Mind, Brain & Behavior 2021 Osteology of the Skull Slide Title Slide Number Slide Title Slide Number Ethmoid Slide 3 Paranasal Sinuses Slide 19 Vomer, Nasal Bone, and Inferior Turbinate (Concha) Slide4 Paranasal Sinus Imaging Slide 20 Lacrimal and Palatine Bones Slide 5 Paranasal Sinus Imaging (Sagittal Section) Slide 21 Zygomatic Bone Slide 6 Skull Sutures Slide 22 Frontal Bone Slide 7 Foramen RevieW Slide 23 Mandible Slide 8 Skull Subdivisions Slide 24 Maxilla Slide 9 Sphenoid Bone Slide 10 Skull Subdivisions: Viscerocranium Slide 25 Temporal Bone Slide 11 Skull Subdivisions: Neurocranium Slide 26 Temporal Bone (Continued) Slide 12 Cranial Base: Cranial Fossae Slide 27 Temporal Bone (Middle Ear Cavity and Facial Canal) Slide 13 Skull Development: Intramembranous vs Endochondral Slide 28 Occipital Bone Slide 14 Ossification Structures/Spaces Formed by More Than One Bone Slide 15 Intramembranous Ossification: Fontanelles Slide 29 Structures/Apertures Formed by More Than One Bone Slide 16 Intramembranous Ossification: Craniosynostosis Slide 30 Nasal Septum Slide 17 Endochondral Ossification Slide 31 Infratemporal Fossa & Pterygopalatine Fossa Slide 18 Achondroplasia and Skull Growth Slide 32 Ethmoid • Cribriform plate/foramina