Mucoepidermoid Carcinoma: a Clinico-Pathological Study of 14 Cases
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Mucoepidermoid Carcinoma
PATHOLOGY CLINIC Mucoepidermoid carcinoma Lester D.R. Thompson, MD ' 8 -1 . •, • . A· ~;J. ~ # ,. r:;;; ~ c rV" ~ i} ......l1.lG;y;t; ~ ~ ml· !' ~ ~ tJ " Figure. A: A blending of intermediate, pavemented cells and goblet-type, mucus-filled cells is characteristic ofan MEC. B: Cystic spaces are common in low-grade tumors. This MEC has an intermediate cell population and many mucocytes. Inset: An MEC demonstrates a strong reaction on a mucicarmine stain. Mucoepidermoid carcinoma (MEC) is the most com Cysts of variable sizes are often present, and they usually mon primary salivary gland malignancy, accounting for contain brownish fluid. MEC cells form sheets, islands, approximately 25% of all malignancies. More than half duct-like structures, and cysts of various sizes . The cysts of these cases involve the major saliva ry glands, primarily may be lined with intermediate, mucous , or epidermoid the parotid glands. MEC can also involve a variety of other cells, and they are filled with mucus (figure, A). Papillary sites that have minor mucoserous glands .Women are more processes may extend into the cyst lumina, and this is oc commonly affected than men (3:2), and the mean age at casionally a conspicuous feature. onset is in the 5th decade of life. MEC is also the most The tumor is primarily made up of three cell types in common salivary gland malignancy in children. widely varying proportions: intermediate, mucous, and The tumor usually forms as a painless, fixed, slowly epidermoid. growing swelling of widelyvarying duration thatsometimes goes through a phase of accelerated growth immediately • The intermediate cells frequentl y predominate; their before clinical presentation. -

Oncocytic Mucoepidermoid Carcinoma: a Case Report
Case Report Annals of Clinical Case Reports Published: 16 Jul, 2019 Oncocytic Mucoepidermoid Carcinoma: A Case Report Laurie Hung* Department of Pathology, Medical University of the Americas, Canada Abstract Oncocytes are large epithelial cells characterized by abundant eosinophilic granular cytoplasm containing excessive mitochondria. Mucoepidermoid Carcinoma (MEC) is the most common salivary gland malignancy (10% of all major gland tumors), most commonly found in the parotid gland. Oncocytic Mucoepidermoid Carcinoma (OMEC) is a very rare tumor found most commonly in the parotid gland. This was a case of oncocytic mucoepidermoid carcinoma in a 26 year old Vietnamese male. He initially presented with a painless mass over his left jaw. Biopsy pathology of the mass showed lesion cells with no high-grade features identified; complete excision was recommended for further classification. Microscopic examination showed an ill-defined infiltrative tumor composed predominantly of solid sheets and nests. The tumor cells were predominantly oncocytic characterized by abundant eosinophilic cytoplasm, round nuclei, and prominent nucleoli with focal pleomorphism. Scattered mucocytes were present. To aid in diagnosis, the following stains were done: CK5/6, CK7, CK14, p63, Ki-67, CK903, CK20, GCDFP, SOX10, Androgen receptor, GATA3, PAS-D, and mucicarmine. The stains CK5/6 and p63 were performed to identify oncocytes. PAS-D and mucicarmine were performed to identify mucin and mucous cells. An accurate diagnosis of OMEC can be made using a combination of histological evaluation and the appropriate immunostains and special stains. Equivocal staining results can be further evaluated for MAML2 translocation with RT-PCR or FISH. Introduction Oncocytes are large epithelial cells characterized by abundant eosinophilic granular cytoplasm containing excessive mitochondria [1-3]. -

Intermediate-Grade Mucoepidermoid Carcinoma Arising from Warthin's
Case report 113 Intermediate-grade mucoepidermoid carcinoma arising from Warthin’s tumour of parotid gland Arsheed H. Hakeema, Imtiyaz H. Hakeemc, Fozia J. Wanib aDepartments of Surgical Oncology (Head and Warthin’s tumour (WT), also known as the adenolymphoma, is the second common benign b Neck), Gynaecology and Obstetrics, Apollo neoplasm that mostly occurs in the parotid gland. Malignant transformation of the epithelial or Cancer Institute, Hyderabad, India, cPoplar lymphoid component of the WT has been rarely reported. We describe a case of a 73-year-old Bluff Regional Medical Center, Poplar Bluff, Missouri, USA woman who underwent total radical parotidectomy with modified neck dissection on the left side. The case was diagnosed as intermediate-grade mucoepidermoid carcinoma developed Correspondence to Arsheed H. Hakeem, MBBS, MS, Department of Surgical Oncology in the setting of WT based on histomorphologic findings. Clinical presentation, pathogenesis, (Head and Neck), Apollo Cancer Institute, differential diagnosis and management of the rare malignancy have been discussed briefly. Jubilee Hills, Hyderabad - 500 096, India Tel: 91-40-23607777; fax: 91-40-23545588; e-mail: [email protected] Keywords: Received 26 November 2014 intermediate-grade mucoepidermoid carcinoma, parotid gland, Warthin’s tumour Accepted 7 December 2014 The Egyptian Journal of Otolaryngology Egypt J Otolaryngol 32:113–115 2016, 32:113–115 © 2016 The Egyptian Oto - Rhino - Laryngological Society 1012-5574 Introduction Fine-needle aspiration cytology was suggestive of mucoepidermoid carcinoma. She underwent total Warthin’s tumour (WT) is a benign salivary gland radical parotidectomy with modified neck dissection neoplasm occurring principally in the parotid on the left side. Histopathologic study showed gland of men in the sixth and seventh decades of haphazardly placed mucin-filled cysts and solid life [1–5]. -

Molecular and Cellular Modelling of Salivary Gland Tumors Open New Landscapes in Diagnosis and Treatment
cancers Review Molecular and Cellular Modelling of Salivary Gland Tumors Open New Landscapes in Diagnosis and Treatment Cristina Porcheri * , Christian T. Meisel and Thimios A. Mitsiadis Orofacial Development and Regeneration, Institute of Oral Biology, University of Zurich, Plattenstrasse 11, 8032 Zurich, Switzerland; [email protected] (C.T.M.); [email protected] (T.A.M.) * Correspondence: [email protected] Received: 4 October 2020; Accepted: 20 October 2020; Published: 24 October 2020 Simple Summary: This review elaborates the current knowledge on salivary gland tumors, with a specific focus on classical histological classification, cellular mechanisms and molecular pattern at the origin of the most common glandular malignancies. We dive into novel approaches for modeling, diagnosis and therapy, giving an overview of the biomedical advances for the study of salivary cancers. Thereby this review helps to understand the complexity of these malignancies and paves the way for novel and efficient treatments. Abstract: Salivary gland tumors are neoplasms affecting the major and minor salivary glands of the oral cavity. Their complex pathological appearance and overlapping morphological features between subtypes, pose major challenges in the identification, classification, and staging of the tumor. Recently developed techniques of three-dimensional culture and organotypic modelling provide useful platforms for the clinical and biological characterization of these malignancies. Additionally, new advances in genetic and molecular screenings allow precise diagnosis and monitoring of tumor progression. Finally, novel therapeutic tools with increased efficiency and accuracy are emerging. In this review, we summarize the most common salivary gland neoplasms and provide an overview of the state-of-the-art tools to model, diagnose, and treat salivary gland tumors. -
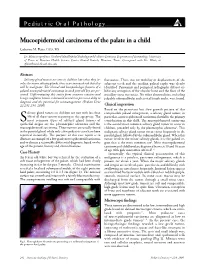
Mucoepidermoid Carcinoma of the Palate in a Child
Pediatric Oral Pathology Mucoepidermoid carcinoma of the palate in a child Catherine M. Flaitz, DDS, MS Dr. Flaitz is a professor, Oral and Maxillofacial Pathology and Pediatric Dentistry, Department of Stomatology, University of Texas at Houston Health Science Center Dental Branch, Houston, Texas. Correspond with Dr. Flaitz at [email protected] Abstract Salivary gland tumors are rare in children but when they in- fluctuance. There was no mobility or displacement of the volve the minor salivary glands, there is an increased risk that they adjacent teeth and the median palatal raphe was clearly will be malignant. The clinical and histopathologic features of a identified. Panoramic and periapical radiographs did not ex- palatal mucoepidermoid carcinoma in an 8 year-old boy are pre- hibit any resorption of the alveolar bone and the floor of the sented. Differentiating this entity from common reactive and maxillary sinus was intact. No other abnormalities, including benign neoplastic lesions is discussed in order to prevent a delay in palpable submandibular and cervical lymph nodes, were found. diagnosis and the potential for mismanagement. (Pediatr Dent 22:292-293, 2000) Clinical impression Based on the persistent but slow growth pattern of this alivary gland tumors in children are rare with less than compressible palatal enlargement, a salivary gland tumor, in 5% of all these tumors occurring in this age group. The particular, a mucoepidermoid carcinoma should be the primary Smost common types of salivary gland tumors of consideration in this child. The mucoepidermoid carcinoma epithelial origin are the pleomorphic adenoma and the is the second most common salivary gland tumor to occur in mucoepidermoid carcinoma. -

Update in Salivary Gland Pathology
Update in Salivary Gland Pathology Benjamin L. Witt University of Utah/ARUP Laboratories February 9, 2016 Objectives • Review the different appearances of a selection of salivary gland tumor types • Establish an immunohistochemical staining pattern to aid in distinguishing between certain tumors • Discuss some newer concepts in salivary gland pathology Acinic Cell Carcinoma • Originally this was considered a benign neoplasm until its malignant potential was described in the 1950s • Later regarded as in between adenoma and carcinoma (acinic cell tumor; WHO 1972) • Finally classified as acinic cell carcinoma in 1991 WHO classification • Diagnosis can be rendered in absence of invasive growth Acinic Cell Carcinoma • Third most common malignancy of major salivary gland (15%) • Most non-parotid ACC (11/14; 80%) actually represent misclassified mammary analogue secretory carcinoma (MASC) - Based upon positivity for S100, mammaglobin - Confirmatory ETV6 t(12;15) translocation by FISH Bishop et al. Am J Surg Pathol. 2013;37(7): 1053-57 Acinic Cell Carcinoma • Neoplasm of cells differentiated towards serous acinar cells • Aside from the zymogen granule rich cells (pathognomonic acinar cells) other cell types frequent these tumors: - Vacuolated cells - Clear cells (non-mucinous, PAS negative) - Nonspecific glandular cells • No grading system exists although high grade transformation is reported Lesion 1: Parotid Mass in 68 year old female Lesion 1: Note clear and vacuolated cells Lesion 2: Parotid mass (3 cm) in 15 year old female PAS-D on Lesion -

2021 Update on Diagnostic Markers and Translocation in Salivary Gland Tumors
International Journal of Molecular Sciences Review 2021 Update on Diagnostic Markers and Translocation in Salivary Gland Tumors Malin Tordis Meyer 1, Christoph Watermann 1, Thomas Dreyer 2, Süleyman Ergün 3 and Srikanth Karnati 3,* 1 Department of Otorhinolaryngology, Head and Neck Surgery, University of Giessen, Klinikstrasse 33, Ebene -1, 35392 Giessen, Germany; [email protected] (M.T.M.); [email protected] (C.W.) 2 Institute for Pathology, Justus Liebig University, Langhansstrasse 10, 35392 Gießen, Germany; [email protected] 3 Institute for Anatomy and Cell Biology, Julius-Maximilians-University Würzburg, Koellikerstrasse 6, 97070 Würzburg, Germany; [email protected] * Correspondence: [email protected]; Tel.: +49-931-3181522 Abstract: Salivary gland tumors are a rare tumor entity within malignant tumors of all tissues. The most common are malignant mucoepidermoid carcinoma, adenoid cystic carcinoma, and acinic cell carcinoma. Pleomorphic adenoma is the most recurrent form of benign salivary gland tumor. Due to their low incidence rates and complex histological patterns, they are difficult to diagnose accurately. Malignant tumors of the salivary glands are challenging in terms of differentiation because of their variability in histochemistry and translocations. Therefore, the primary goal of the study was to review the current literature to identify the recent developments in histochemical diagnostics and translocations for differentiating salivary gland tumors. Keywords: salivary gland tumors; epithelial salivary gland; adenoid cystic carcinoma (ACC); Citation: Meyer, M.T.; pleomorphic adenoma; mucoepidermoid carcinoma; diagnostic markers Watermann, C.; Dreyer, T.; Ergün, S.; Karnati, S. 2021 Update on Diagnostic Markers and Translocation in Salivary Gland Tumors. Int. -

Warthin-Like Mucoepidermoid Carcinoma of the Parotid Gland: a Diagnostic and Therapeutic Dilemma
Article / Clinical Case Report Warthin-like mucoepidermoid carcinoma of the parotid gland: a diagnostic and therapeutic dilemma Vigneshwaran Balasubiramaniyana , Mahesh Sultaniaa , Mukund Sableb , Dillip Mudulya , Madhabananda Kara How to cite: Balasubiramaniyan V, Sultania M, Sable M, Muduly D, Kar M. Warthin-like mucoepidermoid carcinoma of the parotid gland: a diagnostic and therapeutic dilemma. Autops Case Rep [Internet]. 2019 Oct-Dec; 9(4):e2019122. https://doi.org/10.4322/acr.2019.122 ABSTRACT Mucoepidermoid carcinoma (MEC) is the most common malignant salivary gland tumor. Although the parotid gland is the most common site of involvement, other major salivary glands and the minor salivary glands—most commonly of the palate—also can be involved. The management of mucoepidermoid carcinoma depends on the grade of the tumor and the adequacy of resection. We present the case of a 56-year-old female presenting a painless progressive cheek mass over 2 months. Imaging and fine-needle aspiration cytology provided the diagnosis of Mucoepidermoid carcinoma. A superficial parotidectomy was done, and the histopathology revealed a predominantly cystic tumor with a bilayered epithelium of oncocytic and basal cells. Moderate nuclear pleomorphism with infiltration of atypical squamous cells in few glandular cysts was seen. Special staining revealed the presence of intracellular mucin. A diagnosis of Warthin-like variant of MEC was made, based on these findings. After the surgical procedures, the patient is disease-free at 8 months of follow-up. The Warthin-like variant is a rare variant of MEC with fewer than 10 cases described in the English literature. Various differential diagnoses include the malignant transformation of Wartin tumor (WT), squamous metaplasia of WT, and metastasis from a distant primary. -

Adenocarcinomas and Salivary Gland Neoplasms of the Larynx
1999; Vol. 1, Nº 3 Progress in laryngeal pathology 2). 4. Lewis JE, Olsen KD, Sebo TJ. Spindle cell carcinoma of the larynx: Review of greatest concentration of glands is in the saccule (139 glands/cm 26 cases including DNA contentandimmunohistochemistry Hum Pathol 1997; There is a Very low density of glands in the extrinsic laryngeal 28: 664-673. regions. A typical intraepithelial gland is made up of 15-30 mucus- 5. Lane N. Pseudosarcoma (polypoid sarcoma-like masses) associated with secreting cells with a structure like that of goblet cells. They extend squamous cell carcinoma of the mouth, tauces and larynx. Report ot10 cases. from the epithelial surface down toward the basement membrane, Cancer 1957; 10:19-41. on which they may rest, but do not penetrate. Irregularly distributed 6. Ackerman LV. Verrucous carcinoma ofthe oral cavity Surgery 1948; 23: 670- in the larynx, intraepithelial glands are most numerous in the supra- 678. 7. Biller HF, Ogura JH, Bauer WC. Verrucous cancer of the larynx. Laryngoscope glottis and least numerous in the subglottis. 1971; 81:1323-1329. 8. Orvidas LJ, Olsen KD, Lewis JE et al. Verrucous carcinoma of the larynx: A Salivary gland neoplasms review of53 patients. Head Neck 1998; 20: 197-203. With the exception of adenoid cystic carcinomas, salivary-type car- g. Spiro RH. Verrucouscarcinoma, then and now Am JSurg 1998; 176: 393-397. 10. Michaels L. Unusual lorms ot squamous cell carcinoma: Spindle cell carcino- cinomas are rare in the larynx. Even pleomorphic adenomas are ma, verrucous squamous carcinoma, ventriculosaccular carcinoma. In: Ear, almost curiosities in this organ. -

A Case of Mucoepidermoid Carcinoma with Clear Cell Components Occurring in Retromolar Region
Bull Tokyo Dent Coll (2014) 55(1): 25–31 Case Report A Case of Mucoepidermoid Carcinoma with Clear Cell Components Occurring in Retromolar Region Nobuharu Yamamoto1), Yukio Watabe1), Masashi Iwamoto1), Kenichi Matsuzaka2) and Takahiko Shibahara1) 1) Department of Oral and Maxillofacial Surgery, Tokyo Dental College, 1-2-2 Masago, Mihama-ku, Chiba 261-8502, Japan 2) Department of Clinical Pathophysiology, Tokyo Dental College, 1-2-2 Masago, Mihama-ku, Chiba 261-8502, Japan Received 12 April, 2013/Accepted for publication 20 September, 2013 Abstract Mucoepidermoid carcinomas in the minor salivary glands usually originate in the palatine gland, and their occurrence in the retromolar region is rare. We report a rare case of mucoepidermoid carcinoma with clear cell components occurring in the retromolar region. The patient was a 63-year-old woman referred to our hospital with the chief complaint of a painless mass in the right retromolar region initially found during treatment at a local dental clinic. The 20210-mm mass was well-defined, elastic, and flexible. The surface of the mucosa was healthy. The mass was clinically diagnosed as a gingival benign tumor in the right retromolar region. There were no significant findings in the patient’s medical history. The tumor was resected under local anesthesia. Histopathology revealed that squamoid cells, undifferentiated intermediate cells, and clear cells were dominant, with mucus-producing cells in some areas. A mucoepidermoid carcinoma with clear cell components was diagnosed. There were no signs of recurrence or metastasis at 15 months postoperatively and the patient’s progress has been satisfactory. Because the tumor was a painless, slow-growing mass, it was clinically diagnosed as a benign tumor of the gingiva, and resection was performed under local anesthesia without performing a biopsy. -

Characterization of Tumor‑Associated MUC1 and Its Glycans Expressed in Mucoepidermoid Carcinoma
ONCOLOGY LETTERS 22: 702, 2021 Characterization of tumor‑associated MUC1 and its glycans expressed in mucoepidermoid carcinoma EISAKU ISAKA1, TAKANORI SUGIURA1, KAZUHIKO HASHIMOTO2, KAZUTAKA KIKUTA3, UKEI ANAZAWA4, TAKESHI NOMURA1,5 and AKIHIKO KAMEYAMA6 1Department of Oral Oncology, Oral and Maxillofacial Surgery; 2Department of Pathology and Laboratory Medicine, Ichikawa General Hospital, Tokyo Dental College, Ichikawa‑shi, Chiba 272‑8513; 3Department of Musculoskeletal Oncology and Orthopaedic Surgery, Tochigi Cancer Center, Utsunomiya, Tochigi 320‑0834; 4Department of Orthopaedic Surgery; 5Oral Cancer Center, Tokyo Dental College, Ichikawa‑shi, Chiba 272‑8513; 6Cellular and Molecular Biotechnology Research Institute, National Institute of Advanced Industrial Science and Technology (AIST), Tsukuba, Ibaraki 305‑8565, Japan Received March 24, 2021; Accepted June 21, 2021 DOI: 10.3892/ol.2021.12963 Abstract. Mucoepidermoid carcinoma (MEC) is one of the (Hex)2(HexNAc)2(NeuAc)1 and (Hex)2(HexNAc)2(NeuAc)2, most frequently misdiagnosed tumors. Glycans are modulated were found to be significantly abundant glycans of MUC1 by malignant transformation. Mucin 1 (MUC1) is a mucin in MEC. MEC markedly produced MUC1 modified with whose expression is upregulated in various tumors, including sialylated core 2 glycans. These data were obtained from the MEC, and it has previously been investigated as a diagnostic soluble fractions of salivary gland homogenates. These find‑ and prognostic tumor marker. The present study aimed to ings provide a basis for the utilization of MUC1 as a serum reveal the differences in the mucin glycans between MEC and diagnostic marker for the preoperative diagnosis of MEC. normal salivary glands (NSGs) to discover novel diagnostic markers. Soluble fractions of salivary gland homogenate Introduction prepared from three MEC salivary glands and 7 NSGs were evaluated. -
Metastatic Renal Cell Carcinoma to Submandibular Gland
plastol na og A y Melloni, et al., Anaplastology 2015, 4:3 Anaplastology DOI: 10.4172/2161-1173.1000151 ISSN: 2161-1173 Case Report Open Access Metastatic Renal Cell Carcinoma to Submandibular Gland: A Rare Occurrence Carlo Melloni1*, Nino Dispensa2, Adriana Tuttolomondo1, Guglielmo Melloni3 and Adriana Cordova1 1Department of Surgical, Oncological and Oral Sciences, Plastic and Reconstructive Surgery Unit, University of Palermo, Italy 2Department of Medicine, Cardiovascular and Nephrourological Disease – Urology, University of Palermo Italy 3Division of Urology, Department of Surgical Sciences, Molinette Hospital, University of Studies of Turin Italy University of Palermo, Italy *Corresponding author: Carlo Melloni, M.D, Department of Surgical, Oncological and Oral Sciences, Plastic and Reconstructive Surgery Unit, University of Palermo, Italy, Tel: +39 091 6554034; Fax: +39 091 6553720; E-mail: [email protected] Received date: April 25, 2015, Accepted date: September 1, 2015, Published date: September 5, 2015 Copyright: © 2015 Melloni C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Approximately 20-30% of patients affected by renal cell carcinoma (RCC) present with metastatic disease, and 20% to 40% undergoing nephrectomy for clinically localized disease will develop metastases. A 53 years old female patient developed a left submandibular swelling. Four years before she experienced a left radical nephrectomy for a clear cell tumor and two years later right kidney was removed for a cancer having the same histologic subtype. In that circumstance duodenal pancreasectomy was required for infiltration of pancreatic gland.