Clinical Gait Analysis Biomechanics & Etiology of Common Walking Disorders
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
Pediatrics-EOR-Outline.Pdf
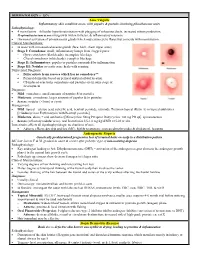
DERMATOLOGY – 15% Acne Vulgaris Inflammatory skin condition assoc. with papules & pustules involving pilosebaceous units Pathophysiology: • 4 main factors – follicular hyperkeratinization with plugging of sebaceous ducts, increased sebum production, Propionibacterium acnes overgrowth within follicles, & inflammatory response • Hormonal activation of pilosebaceous glands which may cause cyclic flares that coincide with menstruation Clinical Manifestations: • In areas with increased sebaceous glands (face, back, chest, upper arms) • Stage I: Comedones: small, inflammatory bumps from clogged pores - Open comedones (blackheads): incomplete blockage - Closed comedones (whiteheads): complete blockage • Stage II: Inflammatory: papules or pustules surrounded by inflammation • Stage III: Nodular or cystic acne: heals with scarring Differential Diagnosis: • Differentiate from rosacea which has no comedones** • Perioral dermatitis based on perioral and periorbital location • CS-induced acne lacks comedones and pustules are in same stage of development Diagnosis: • Mild: comedones, small amounts of papules &/or pustules • Moderate: comedones, larger amounts of papules &/or pustules • Severe: nodular (>5mm) or cystic Management: • Mild: topical – azelaic acid, salicylic acid, benzoyl peroxide, retinoids, Tretinoin topical (Retin A) or topical antibiotics [Clindamycin or Erythromycin with Benzoyl peroxide] • Moderate: above + oral antibiotics [Minocycline 50mg PO qd or Doxycycline 100 mg PO qd], spironolactone • Severe (refractory nodular acne): oral -

Development of a Global Gait Symmetry Score Using Biomechanical Parameters
UNIVERSIDADE DE LISBOA FACULDADE DE MOTRICIDADE HUMANA DEVELOPMENT OF A GLOBAL GAIT SYMMETRY SCORE USING BIOMECHANICAL PARAMETERS Tese elaborada com vista à obtenção do Grau de Doutor em Motricidade Humana na Especialidade de Biomecânica Orientador: Professor Doutor António Prieto Veloso Coorientador: Doutor W. Scott Selbie Júri: Presidente Reitor da Universidade de Lisboa Vogais: Doutor Kevin Deluzio Professor Catedrático, Faculty of Engineering and Applied Sciences, Department of Mechanical and Materials Engineering, Queen’s University (Kingston, ON, Canadá) Doutor António Prieto Veloso Professor Catedrático, Faculdade de Motricidade Humana, Universidade de Lisboa Doutor Alberto Leardini Investigador Principal, Laboratory of Movement Analysis and Functional Clinical Evaluation of Prothesis, Institute Ortopedico Rizzoli (Bolonha, Itália) Doutor Miguel Tavares da Silva Professor Associado, Instituto Superior Técnico, Universidade de Lisboa Sílvia Arsénio Rodrigues Cabral 2016 UNIVERSIDADE DE LISBOA FACULDADE DE MOTRICIDADE HUMANA DEVELOPMENT OF A GLOBAL GAIT SYMMETRY SCORE USING BIOMECHANICAL PARAMETERS Tese elaborada com vista à obtenção do Grau de Doutor em Motricidade Humana na Especialidade de Biomecânica Tese por compilação de artigos, realizada ao abrigo da alínea a) do nº2 do art.º 31º do Decreto-Lei nº 230/2009 Orientador: Professor Doutor António Prieto Veloso Coorientador: Doutor W. Scott Selbie Júri: Presidente Reitor da Universidade de Lisboa Vogais: Doutor Kevin Deluzio Professor Catedrático, Faculty of Engineering and Applied -

Neurologic Outcomes in Friedreich Ataxia: Study of a Single-Site Cohort E415
Volume 6, Number 3, June 2020 Neurology.org/NG A peer-reviewed clinical and translational neurology open access journal ARTICLE Neurologic outcomes in Friedreich ataxia: Study of a single-site cohort e415 ARTICLE Prevalence of RFC1-mediated spinocerebellar ataxia in a North American ataxia cohort e440 ARTICLE Mutations in the m-AAA proteases AFG3L2 and SPG7 are causing isolated dominant optic atrophy e428 ARTICLE Cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy revisited: Genotype-phenotype correlations of all published cases e434 Academy Officers Neurology® is a registered trademark of the American Academy of Neurology (registration valid in the United States). James C. Stevens, MD, FAAN, President Neurology® Genetics (eISSN 2376-7839) is an open access journal published Orly Avitzur, MD, MBA, FAAN, President Elect online for the American Academy of Neurology, 201 Chicago Avenue, Ann H. Tilton, MD, FAAN, Vice President Minneapolis, MN 55415, by Wolters Kluwer Health, Inc. at 14700 Citicorp Drive, Bldg. 3, Hagerstown, MD 21742. Business offices are located at Two Carlayne E. Jackson, MD, FAAN, Secretary Commerce Square, 2001 Market Street, Philadelphia, PA 19103. Production offices are located at 351 West Camden Street, Baltimore, MD 21201-2436. Janis M. Miyasaki, MD, MEd, FRCPC, FAAN, Treasurer © 2020 American Academy of Neurology. Ralph L. Sacco, MD, MS, FAAN, Past President Neurology® Genetics is an official journal of the American Academy of Neurology. Journal website: Neurology.org/ng, AAN website: AAN.com CEO, American Academy of Neurology Copyright and Permission Information: Please go to the journal website (www.neurology.org/ng) and click the Permissions tab for the relevant Mary E. -

Master Thesis, but Also All the Good Times We Have Spent Together These Two Year
Kinetic relationships between ankle plantar flexor and hip flexor power during gait in mildly affected adults with spastic hemiplegic and diplegic cerebral palsy A case series study based on a ballistic strength training rehabilitation program Silje Marie Rydningen Torberntsson Master Program in Health Science – Physiotherapy by Research Department of Global Public Health and Primary Care Autumn 2019 – Spring 2020 1 Preface and acknowledgements First of all, I want to thank my supervisor Silje Mæland and my wonderful college in this project Beate Eltarvåg Gjesdal, who has been great support and made this project possible. I am so thankful for all your advices regarding the master thesis, but also all the good times we have spent together these two year. You spread lots of joy while working which has made it a pleasure to take part in the project. You are absolutely outstanding! Secondly, I am grateful for the kindness and help from Lars Peder Vatshelle Bovim and Bård Erik Bogen in the rehabilitation laboratory Sim Arena, Western Norway University of Applied Science. I truly respect and appreciate everything I have learned from you. Greetings to all the subjects participating in this project. Your effort and encouragement have been important to initiate future research in this field to improve rehabilitation options for individuals in the same position. Thank you so much! And finally, thanks to my fantastic family and friends for always being supportive. Bergen, May 2020 Silje Marie Rydningen Torberntsson 2 Content Preface and acknowledgements -

Tremor, Abnormal Movement and Imbalance Differential
Types of involuntary movements Tremor Dystonia Chorea Myoclonus Tics Tremor Rhythmic shaking of muscles that produces an oscillating movement Parkinsonian tremor Rest tremor > posture > kinetic Re-emergent tremor with posture Usually asymmetric Pronation-supination tremor Distal joints involved primarily Often posturing of the limb Parkinsonian tremor Other parkinsonian features Bradykinesia Rigidity Postural instability Many, many other motor and non- motor features Bradykinesia Rigidity Essential tremor Kinetic > postural > rest Rest in 20%, late feature, only in arms Intentional 50% Bringing spoon to mouth is challenging!! Mildly asymmetric Gait ataxia – typically mild Starts in the arms but can progress to neck, voice and jaw over time Jaw tremor occurs with action, not rest Neck tremor should resolve when patient is lying flat Essential tremor Many other tremor types Physiologic tremor Like ET but faster rate and lower amplitude Drug-induced tremor – Lithium, depakote, stimulants, prednisone, beta agonists, amiodarone Anti-emetics (phenergan, prochlorperazine), anti-psychotics (except clozapine and Nuplazid) Many other tremor types Primary writing tremor only occurs with writing Orthostatic tremor leg tremor with standing, improves with walking and sitting, causes imbalance Many other tremor types Cerebellar tremor slowed action/intention tremor Holmes tremor mid-brain lesion, unilateral Dystonia Dystonia Muscle contractions that cause sustained or intermittent torsion of a body part in a repetitive -

Children with Lower Limb Length Inequality
Children with lower limb length inequality The measurement of inequality. the timing of physiodesis and gait analysis H.I.H. Lampe ISBN 90-9010926-9 Although every effort has been made to accurately acknowledge sources of the photographs, in case of errors or omissions copyright holders arc invited to contact the author. Omslagontwcrp: Harald IH Lampe Druk: Haveka B.V., Alblasserdarn <!) All rights reserved. The publication of Ihis thesis was supported by: Stichling Onderwijs en Ondcrzoek OpJciding Orthopaedic Rotterdam, Stichting Anna-Fonds. Oudshoom B.V., West Meditec B.V., Ortamed B.Y .• Howmedica Nederland. Children with lower limb length inequality The measurement of inequality, the timing of physiodesis and gait analysis Kinderen met een beenlengteverschil Het meten van verschillen, het tijdstip van physiodese en gangbeeldanalyse. Proefschrift ter verkrijging van de graad van doctor aan de Erasmus Universiteit Rotterdam op gezag van de Rector Magnificus Prof. dr P.W.C. Akkermans M.A. en volgens besluit van het College voor Promoties. De openbare verdediging zal plaatsvinden op woen,dag 17 december 1997 om 11.45 uur door Harald Ignatius Hubertus Lampe geboren te Rotterdam. Promotieconmussie: Promotores: Prof. dr B. van Linge Prof. dr ir C.J. Snijders Overige leden: Prof. dr M. Meradji Prof. dr H.J. Starn Prof. dr J.A.N. Verbaar Dr. B.A. Swierstra, tevens co-promotor voor mijn ouders en Jori.nne Contents Chapter 1. Limb length inequality, the problems facing patient and doctor. 9 Review of Ii/era/ure alld aims of /he studies 1.0 Introduction 11 1.1 Etiology, developmental patterns and prediction of LLI 1.1.1 Etiology and developmental pattern 13 I. -

Use of Osteopathic Manipulative Treatment to Manage Compensated Trendelenburg Gait Caused by Sacroiliac Somatic Dysfunction
Editor’s Note: Corrections to this article were published in the March 2010 issue of JAOA—The Journal of the CASE REPORT American Osteopathic Association (2010;110[3]:210). The corrections have been incorporated in this online version of the article, which was posted January 2011. An expla - nation of these changes is available at http://www.jaoa .org/cgi/content /full/110/3/210-a. Use of Osteopathic Manipulative Treatment to Manage Compensated Trendelenburg Gait Caused by Sacroiliac Somatic Dysfunction Adam C. Gilliss, DO; Randel L. Swanson, II, OMS III; Deanna Janora, MD; and Venkat Venkataraman, PhD Gait dysfunctions are commonly encountered in the pri - In the present case report, we provide evidence that com - mary care setting. Compensated Trendelenburg gait is a gait pensated Trendelenburg gait may represent a secondary gait dysfunction that was originally described in patients with dysfunction stemming from somatic dysfunction of the weakness of ipsilateral hip abduction. This condition is sacroiliac joints. We also describe evidence of osteopathic thought to result from neuronal injury or myopathy. No manipulative treatment (OMT) resulting in quantitative treatment modalities currently exist for compensated Tren - improvements in the gait cycle. delenburg gait. The authors present a case in which osteo - pathic manipulative treatment may have improved a Tren - Traditional and Osteopathic Gait Theory delenburg gait dysfunction in a man aged 65 years with The gait cycle is divided into two main phases—stance and multiple sclerosis. Evidence of this improvement was swing, each consisting of numerous subphases. 2,3 Traditionally, obtained with the GaitMat II system for measuring the human gait cycle is considered to have six determinants that numerous gait parameters. -

The Trendelenburg Gait
A Personalised Monitoring and Recommendation Framework for Kinetic Dysfunctions: The Trendelenburg Gait Nikolaos Michalopoulos George E. Raptis Christina Katsini Moment Kinetics Moment Kinetics Moment Kinetics nmichalopoulos@ graptis@ ckatsini@ momentkinetics.com momentkinetics.com momentkinetics.com Theofilos Chrysikos Michail Mamalakis Andrew Vigotsky ECE Department ECE Department Biomedical Engineering Dept. University of Patras University of Patras Northwestern University [email protected] [email protected] [email protected] ABSTRACT bilitative perspective, it is possible to identify the risk of Kinetics and kinematics have been the focus of a lot of re-injury on an individual basis through the application of research throughout the years, and technological advances biomechanical kinematics and kinetics. The identification have contributed towards advanced monitoring and analysing of causality often requires precise analysis, as patients fre- of motion. Focusing on Trendelenburg Gait, an abnormal quently present a plethora of compensatory movement pat- gait, a personalisation framework for monitoring and eval- terns. Such compensatory deficits and impairments are often uating the movement is proposed in this paper based on a more noticeable than the underlying cause [15], making the number of factors, such as individuals' body composition, diagnosis process even more challenging. However, quantify- motion mechanisms, capturing process, analysis tools and ing the mobility state of a medical disorder and determining information -

Hip Arthroscopy PT Protocol
Arthroscopic Hip Surgery Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient’s therapy progression. It is not intended to serve as a recipe for treatment. We request that the PT/PTA/ATC use appropriate clinical decision- making skills when progressing a patient forward. Please call (833) 872-4477 to obtain the operative report from our office prior to the first post-op visit. Please contact our office if there are any questions about the protocol or your patient’s progression. Please keep in mind common problems that may arise following hip arthroscopy: hip flexor tendonitis, adductor tendonitis, sciatica/piriformis syndrome, ilial upslips and rotations, LB pain from QL hypertonicity and segmental vertebral rotational lesions. If you encounter any of these problems, please evaluate, assess, and treat as you feel appropriate, maintaining American Hip Institute’s precautions and guidelines at all times. Gradual progression is essential to avoid flare-ups. If a flare-up occurs, back off with therapeutic exercises until it subsides. Please reference the exercise progression sheet for timelines and use the following precautions during your treatments. Thank you for progressing all patients appropriately. Successful treatment requires a team approach, and the PT/PTA/ATC is a critical part of the team! Please contact AHI at any time with your input on how to improve the therapy protocol. Please send therapy progress notes and renewal therapy prescription requests with the patient or by fax to (630) 323-5625. Notes by fax must be sent 3 days prior to the patient’s visit to internally process this request. -

The Limping Child Future of Pediatrics June 15, 2016
The Limping Child Future of Pediatrics June 15, 2016 Benjamin D. Martin Division of Orthopaedic Surgery The Limping Child • DDX • Normal Gait • Abnormal Gait Patterns • Common causes 2 HOW OLD IS THE CHILD? IS THE CHILD IN PAIN? PAINLESS PAINFUL Coxa vara Perthes DDH SCFE Leg length difference Discoid meniscus Cerebral palsy Transient synovitis Muscular dystrophy Septic arthritis Osteomyelitis JRA DON’T FORGET TO LOOK AT HIP FOR KNEE PAIN!! Toddler Child Adolescent (1-3) (4-10) (11-15) Transient synovitis Transient synovitis SCFE Septic Arthritis Septic Arthritis Dysplasia Toddler’s fx Perthes Tarsal coalition CP Leg length difference DDH Coxa vara JRA Normal Gait Efficient ?? Gait Analysis Toddler vs. Mature Gait step time cadence walking velocity COMMON GAIT PATTERNS Abnormal Gait Patterns • Antalgic • Trendeleburg • Proximal weakness • Spastic • Short limb Antalgic Gait Antalgic gait = shorten stance phase (amount of time affected limp on the ground) PAINFUL quick, soft steps Trendelenburg Gait Lever Arm Trendelenburg gait = body leans over weak abductors NOT PAINFUL* * Trendelenburg + pain = coxalgic gait Proximal Weakness Gait Weak hamstrings = lordosis Weak abductors = Trendelenburg 1st symptom might be toe walking! Spastic Gait Gross Motor & Functional Classification Delayed walkers? Short Limb Gait • Oblique pelvis • ASIS to medial malleolus • Femur vs. tibia vs. both 15 COMMON CONDITIONS Toxic Synovitis vs. Septic Arthritis Toxic Synovitis Septic Arthritis • 4 – 10 yo • Refusal to bear weight • NOT ALLOW MOTION • Hip pain, limp • Fevers (>38.5°) • Recent illness (URI) • WBC (>12K) • ESR (>40) • Low grade temps • CRP (>2) • Slightly elevated labs • Hematogenous spread • Aspirate • NSAIDs – Gram Stain, WBC>50K • Symptoms 1-2 weeks • Surgical emergency!! MOTRIN CHALLENGE ULTRASOUND (both have effusion) ASPIRATION Osteomyelitis subperiosteal abscess - Bone infection - Hematogenous - S. -

Gait Abnormalities in Functional Problems of the Lower Extremities and in Neurological Diseases
48 Review articles GAIT ABNORMALITIES IN FUNCTIONAL PROBLEMS OF THE LOWER EXTREMITIES AND IN NEUROLOGICAL DISEASES M. Becheva, PhD Medical University- Plovdiv, Medical College, Bulgaria, 120Buxton Bros. 4004 Plovdiv Abstract: Gait is a complex, automated and stereotyped motor activity that allows for movement of the body in an upright position. The investigation of gait is an integral part of the pathokinesiological study of the functional problems in any of the segments of the lower limbs. As the stereotype of walking changes at departure, stopping, turning, walking alongside another one, gait should be examined in different situations. In functional problems of the lower limbs and in some neurological diseases, the follow- ing abnormal gaits are detected: arthrogenic gait in extensional contractures of the hip or knee, walking in flexion contractures, "Gluteus maximus" gait, "Gluteus medius"gait, ataxic gait, hemiparetic (hemiplegic) gait, gait in parkinsonism, gait in paresis of plantar flexor, lameness in spasm of m. psoas major, gait in insufficiency of m. quadriceps femo- ris, gait in shortening of a lower limb, steppage gait and scissor gait. Adjusting abnormal gait is especially important to improve the functional condition of the patients in view of procuring a better quality of life. Keywords: abnormal gait, functional problems, neurological diseases. Introduction ground and allows the body to move forward. Gait is a complex stereotyped and auto- Gait is a conscious and volitional motor activity mated motor activity, which allows for move- [3]. ment of the body in an upright position. It 3. A complex coordination action during consists of several components: body movements, to maintain the center of grav- 1. -

Functional Clinical Typology of the Foot and Kinematic Gait Parameters
Acta Gymnica, vol. 46, no. 2, 2016, 74–81 doi: 10.5507/ag.2016.004 Functional clinical typology of the foot and kinematic gait parameters Jitka Marenčáková1,*, Zdeněk Svoboda2, Ivan Vařeka2,3, and František Zahálka1 1Faculty of Physical Education and Sport, Charles University, Prague, Czech Republic; 2Faculty of Physical Culture, Palacký University Olomouc, Czech Republic; and 3Faculty of Medicine, Charles University, Hradec Králové, Czech Republic Copyright: © 2016 J. Marenčáková et al. This is an open access article licensed under the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0/). Background: The foot plays a key role in a standing posture, walking and running performance. Changes in its structure or function may alter upper segments of kinematic chain which can lead to formation of musculoskel- etal disorders. Although functional clinical typology provides a complex view of foot kinesiology there is a lack of knowledge and evidence about influences of different foot types on human gait. Objective: The aim of the study was to analyse differences of kinematic gait parameters of lower extremity joints and pelvis between functional clinical foot types in healthy young men. Methods: Three-dimensional kinematic analysis by the Vicon Motion Capture MX System device in synchronization with 2 Kistler force platforms was used to obtain kinematic data from 18 healthy men (mean age 23.2 ± 1.9 years). The functional clinical foot type was clinically examined and sorted into 3 basic foot type groups – forefoot varus (FFvar), rearfoot varus (RFvar) and forefoot valgus (FFvalg). Peak angular values and range of an angular displacement in all of three movement planes were analysed for pelvis, hip, knee and ankle joint.