Letters to the Editor
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
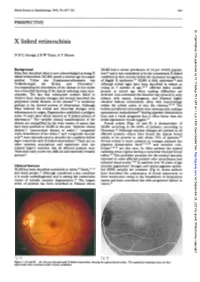
X Linked Retinoschisis
British Joumal of Ophthalmology 1995; 79: 697-702 697 PERSPECTIVE Br J Ophthalmol: first published as 10.1136/bjo.79.7.697 on 1 July 1995. Downloaded from X linked retinoschisis N D L George, J R W Yates, A T Moore Background XLRS had a carrier prevalence of 14 per 10 000 popula- Haas first described what is now acknowledged as being X tion'4 and it was considered to be the commonest X linked linked retinoschisis (XLRS) nearly a century ago in a paper condition in that country before the increased recognition entitled 'Ueber das Zusammenvorkommen von of fragile X syndrome.'5 XLRS is fully penetrant'4 and Veranderungen der Retina und Choroidea'. I although retinal signs have been described in infants as Accompanying his description of the disease in two males young as 3 months of age,'6 17 affected males usually was a beautiful drawing of the typical radiating cystic mac- present at school age when reading difficulties are ulopathy. The fact that subsequent authors failed to detected. Less commonly the disorder may present in early observe these macular changes and instead described the infancy with squint, nystagmus, and bilateral highly peripheral retinal features of the disease2-4 is testimony elevated bullous retinoschisis often with haemorrhage perhaps to his shrewd powers of observation. Although within the schisis cavity or into the vitreous.18 19 The Haas believed the retinal and choroidal changes were bullous peripheral retinoschisis may subsequently undergo inflammatory in origin, Pagenstecher published a pedigree spontaneous reattachment20 leaving pigment demarcation some 15 years later which showed an X linked pattern of lines and a visual prognosis that is often better than the inheritance.5 The variable clinical manifestations of the initial appearance would suggest.2' disease are exemplified by the wide variety of names that Foveal schisis (Figs 1A and B) is characteristic of have been ascribed to XLRS in the past. -

Aspergillus Terreus Postoperative Endophthalmitis
386 Theodossiadis, Koutsandrea, Theodossiadis Figure 3 B scan thus preventing the fluid flow from the optic pit ultrasonography 41/2 years after the operation. Note the to the submacular space (Fig 3). characteristic picture ofthe This procedure should be an alternative solu- silastic sponge as well as the tion for the management of secondary macular height ofthe chorioretinal of optic disc. Br J Ophthalmol: first published as 10.1136/bjo.77.6.386 on 1 June 1993. Downloaded from indentation produced by the elevation caused by the pit the explant at the posterior pole. The location ofthe sponge 1 Gass JDM. Serous detachment of the macula secondary to seems to provide a barrier congenital pit ofthe optic nervehead. Amj Ophthalmol 1969; between the optic nerve pit 67: 821-41. and the macula. 2 Brown GC, Tasman WS. Congenital abnormalities of the optic disc. New York: Grune and Stratton, 1983: 97-126. 3 Lincoff H, Lope R, Kreissig I, Yanuzzi L, Cox M, Burton T. Retinoschisis associated with optic nerve pit. Arch Ophthalmol 1988; 106: 61-7. 4 Theodossiadis G. Evolution of congenital pit of the optic disc with macular detachment in photocoagulated and non- photocoagulated eyes. Am3J Ophthalmol 1977; 840: 620-31. macular hole leading to a rhegmatogenous retinal 5 Theodossiadis GP, Panopoulos M, Kollia AK, Georgopoulos G. Long-term study of patients with congenital pit of the detachment, as happened in our case. This was optic nerve and persistent macular detachment. Acta probably due to a defect ofthe outer retinal layer Ophthalmol (Kbh) 1992; 70: 495-505. 6 Cox MS, Witherspoon CD, Morris RE, Flynn HW. -

OCULAR GENE THERAPY TRIALS ADVANCE Results of the First Phase 3 Trial Were Announced
OCULAR GENE THERAPY TRIALS ADVANCE Results of the first phase 3 trial were announced. BY ARON SHAPIRO INNOVATIONS IN RETINA INNOVATIONS “We used to think that our fate was in our AAV FACILITATES GENE DELIVERY stars, but now we know that, in large measure, The nonpathogenic adeno-associated virus (AAV) has our fate is in our genes.” to date been a safe and effective vector for gene delivery. –James Watson1 The recombinant AAV (rAAV) vector has demonstrated increased specificity and efficiency in ocular AAV-mediated Genetic alterations are known to be respon- gene therapy interventions. Recombinant AAV2 (rAAV2) sible for numerous diseases, and so it follows vectors used for gene therapy are derived from the wild-type logically that the best cures for these diseases virus by deleting the entire viral coding region and replac- might lie in correcting genetic anomalies by the process of ing it with the reporter or therapeutic transgene. Combined gene therapy. This approach involves the introduction of AAV serotypes have also been developed. This diversity genes into existing cells in attempts to prevent or cure a of serotypes may lead to more specific and more efficient wide range of diseases previously thought to be incurable.1 transduction. However, successful and efficient transfection Posterior segment disorders are challenging to treat, and of particular cell types in the eye still depends on other fac- current therapies have numerous shortcomings. Many are tors, such as the AAV titer, the site of injection, the amount invasive, run the risk of complications, offer only short-term of passenger DNA, and the specific gene promoters where relief from symptoms, or are unable to directly treat vision transcription initiation takes place.2 loss. -

The Hereditary Hyalo-Retinopathies
Brit. 7. Ophthal. (I969) 53, 136 Ophthalmological synopsesBr J Ophthalmol: first published as 10.1136/bjo.53.2.136 on 1 February 1969. Downloaded from The hereditary hyalo-retinopathies In the confused spectrum of diseases affecting the vitreous and retina, stretching at the one end from the developmental vitreous anomalies an extreme example of which is persistent hyperplastic primary vitreous-and at the other end to the developmental retinal disorders an extreme example of which are the retinal dysplasias, there lies a group of conditions known as the hereditary hyalo- retinopathies. A clear distinction on clinical grounds in this group of conditions is very difficult because of the diffuseness of the clinical signs, but fortunately distinctions can be drawn on genetic grounds. Four of these conditions, though rare, have been described in the literature. (i) X-linked recessive juvenile idiopathic retinoschisis (Fig. I) has been described under a number of names such as congenital vascular veils in the vitreous and cystic retinal detachment. The condition is characterized by retinoschisis often with large holes in its inner layer, by vitreous membranes and occasional vitreous cords and posterior vitreous detachments, by field defects corresponding to the retinoschisis, by normal visual acuity (unless the macula is affected with cystic change), and by a reduced electroretinogram. copyright. .. e \~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~t .... http://bjo.bmj.com/ F I G. I X-linked recessive juvenile idiopathic FI G. 2 Hyalo-retinopathy of Wagner retinoschisis (2) Autosomal recessive idiopathic retinoschisis with night blindness is rare and is charac- terized by diminished visual acuity due to cystic macular change, retinoschisis with the appropriate field defects and often large holes in the inner layer of the retinoschisis, clumps of pigment in the retina resembling retinitis pigmentosa, degeneration of the vitreous with vitreous cords, an absent electroretinogram, and night blindness. -

Central Serous Chorioretinopathy Towards an Evidence-Based Treatment Guideline
Central serous chorioretinopathy Towards an evidence-based treatment guideline van Rijssen, Thomas J.; van Dijk, Elon H.C.; Yzer, Suzanne; Ohno-Matsui, Kyoko; Keunen, Jan E.E.; Schlingemann, Reinier O.; Sivaprasad, Sobha; Querques, Giuseppe; Downes, Susan M.; Fauser, Sascha; Hoyng, Carel B.; Piccolino, Felice Cardillo; Chhablani, Jay K.; Lai, Timothy Y.Y.; Lotery, Andrew J.; Larsen, Michael; Holz, Frank G.; Freund, K. Bailey; Yannuzzi, Lawrence A.; Boon, Camiel J.F. Published in: Progress in Retinal and Eye Research DOI: 10.1016/j.preteyeres.2019.07.003 Publication date: 2019 Document version Publisher's PDF, also known as Version of record Document license: CC BY Citation for published version (APA): van Rijssen, T. J., van Dijk, E. H. C., Yzer, S., Ohno-Matsui, K., Keunen, J. E. E., Schlingemann, R. O., Sivaprasad, S., Querques, G., Downes, S. M., Fauser, S., Hoyng, C. B., Piccolino, F. C., Chhablani, J. K., Lai, T. Y. Y., Lotery, A. J., Larsen, M., Holz, F. G., Freund, K. B., Yannuzzi, L. A., & Boon, C. J. F. (2019). Central serous chorioretinopathy: Towards an evidence-based treatment guideline. Progress in Retinal and Eye Research, 73, [100770]. https://doi.org/10.1016/j.preteyeres.2019.07.003 Download date: 02. okt.. 2021 Progress in Retinal and Eye Research 73 (2019) 100770 Contents lists available at ScienceDirect Progress in Retinal and Eye Research journal homepage: www.elsevier.com/locate/preteyeres Central serous chorioretinopathy: Towards an evidence-based treatment T guideline Thomas J. van Rijssena,1, Elon H.C. van Dijka,1, Suzanne Yzerb,1, Kyoko Ohno-Matsuic,1, Jan E.E. -

Peripapillary Retinal Splitting Visualized on OCT in Glaucoma and Glaucoma Suspect Patients
RESEARCH ARTICLE Peripapillary retinal splitting visualized on OCT in glaucoma and glaucoma suspect patients Dilraj S. Grewal¤a, Daniel J. Merlau¤b, Pushpanjali Giri, Marion R. Munk, Amani A. Fawzi, Lee M. Jampol, Angelo P. Tanna* Department of Ophthalmology, Northwestern University Feinberg School of Medicine, Chicago, Illinois, United States of America ¤a Current address: Duke Eye Center, Department of Ophthalmology, Duke University Medical Center, Durham, North Carolina, United States of America a1111111111 ¤b Current address: Columbia University, New York, New York, United States of America a1111111111 * [email protected] a1111111111 a1111111111 a1111111111 Abstract Purpose OPEN ACCESS To identify the risk factors for development of peripapillary retinal splitting (schisis) in Citation: Grewal DS, Merlau DJ, Giri P, Munk MR, patients with glaucoma or suspicion of glaucoma Fawzi AA, Jampol LM, et al. (2017) Peripapillary retinal splitting visualized on OCT in glaucoma and glaucoma suspect patients. PLoS ONE 12(8): Setting e0182816. https://doi.org/10.1371/journal. pone.0182816 Glaucoma Clinic, Department of Ophthalmology, Northwestern University Feinberg School of Medicine, Chicago, IL Editor: Demetrios G. Vavvas, Massachusetts Eye & Ear Infirmary, Harvard Medical School, UNITED STATES Methods Received: March 1, 2017 In this institutional cross-sectional study, 495 patients (990 eyes) who had undergone spec- Accepted: July 25, 2017 tral-domain optical coherence tomography (OCT Spectralis HRA-OCT, Heidelberg Engi- Published: August 23, 2017 neering) optic nerve head (ONH) imaging and did not have identifiable optic nerve pits, pseudopits or coloboma were included. OCT scans were reviewed by two observers. Copyright: © 2017 Grewal et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which Main outcome measures permits unrestricted use, distribution, and reproduction in any medium, provided the original Presence of peripapillary retinal splitting identified on OCT raster scans. -

Consanguineous Marriage Resulting in Homozygous Occurrence of X-Linked Retinoschisis in Girls
eCommons@AKU Section of Ophthalmology Department of Surgery 10-2003 Consanguineous marriage resulting in homozygous occurrence of X-linked retinoschisis in girls Azam Ali Aga Khan University, [email protected] Agha Hassan Feroze Zulfiqar H. Rizvi Tausif- Ur -Rehman Follow this and additional works at: https://ecommons.aku.edu/pakistan_fhs_mc_surg_ophthalmol Part of the Ophthalmology Commons Recommended Citation Ali, A., Feroze, A. H., Rizvi, Z. H., -Rehman, T. U. (2003). Consanguineous marriage resulting in homozygous occurrence of X-linked retinoschisis in girls. American Journal of Ophthalmology, 136(4), 767-769. Available at: https://ecommons.aku.edu/pakistan_fhs_mc_surg_ophthalmol/33 FIGURE 1. (A) A red-free fundus photograph reveals several vacuoles within the area of internal limiting membrane peeling (demarcated by white arrows). The arrowhead in the middle shows a vacuole. Horizontal scans using optical coherence tomography 8 months after surgery slightly superior to the fovea (B) and through the fovea (C) show intraretinal vacuoles, largely confined to the middle layers of the retina. silicone oil with eventual deposition of silicone oil within Consanguineous Marriage Resulting in the retina, observable only within the region of ILM peeling. It is possible that the intentional iatrogenic defect Homozygous Occurrence of X-linked created by ILM removal augmented the ability of the Retinoschisis in Girls emulsified oil to penetrate into the retinal tissue. The Azam Ali, MRCOphth, FRCOphth, FRCS(Ed), presence of the silicone droplets could be detected by FRCS(Glas), Agha H. Feroze, MB, BS, ophthalmoscopy and optical coherence tomography. Zulfiqar H. Rizvi, MB, BS, and The anatomic success of macular hole surgery with ILM peeling using intraocular gas as a tamponade is greater than Tausif-Ur- Rehman, MB, BS 90%.4 The success rate for limited head positioning is also very high. -

Gene Therapy for Inherited Retinal Diseases
1278 Review Article on Novel Tools and Therapies for Ocular Regeneration Page 1 of 13 Gene therapy for inherited retinal diseases Yan Nuzbrokh1,2,3, Sara D. Ragi1,2, Stephen H. Tsang1,2,4 1Department of Ophthalmology, Edward S. Harkness Eye Institute, Columbia University Irving Medical Center, New York, NY, USA; 2Jonas Children’s Vision Care, New York, NY, USA; 3Renaissance School of Medicine at Stony Brook University, Stony Brook, New York, NY, USA; 4Department of Pathology & Cell Biology, Columbia University Irving Medical Center, New York, NY, USA Contributions: (I) Conception and design: All authors; (II) Administrative support: SH Tsang; (III) Provision of study materials or patients: SH Tsang; (IV) Collection and assembly of data: All authors; (V) Manuscript writing: All authors; (VI) Final approval of manuscript: All authors. Correspondence to: Stephen H. Tsang, MD, PhD. Harkness Eye Institute, Columbia University Medical Center, 635 West 165th Street, Box 212, New York, NY 10032, USA. Email: [email protected]. Abstract: Inherited retinal diseases (IRDs) are a genetically variable collection of devastating disorders that lead to significant visual impairment. Advances in genetic characterization over the past two decades have allowed identification of over 260 causative mutations associated with inherited retinal disorders. Thought to be incurable, gene supplementation therapy offers great promise in treating various forms of these blinding conditions. In gene replacement therapy, a disease-causing gene is replaced with a functional copy of the gene. These therapies are designed to slow disease progression and hopefully restore visual function. Gene therapies are typically delivered to target retinal cells by subretinal (SR) or intravitreal (IVT) injection. -

Poster Presentations
Poster Presentations 122th Annual AOA Congress & 49th Annual AOSA Conference: Optometry’s Meeting® June 19-23, 2019 Poster Presentations Optometry’s Meeting® • St. Louis, MO • June 19-23, 2019 Screen #7 POSTER SESSION #1 Scientific Abstract Thursday, June 20 from 6- 6:30 p.m. Evaluation of Dynamic Amsler for Estimation of Visual Field in Low Vision Screen #1 Carlos Grandela, OD OD-Ocular Disease Co-Author(s) Electroretinographic Findings in Pityriasis Rubra Pilaris Tapuwa L. Chikwinya, OD, MPH Tracy Matchinski, OD, FAAO Laura Addy, OD Kara Crumbliss, OD, FAAO Co-Author(s) Kaila M. Osmotherly, O.D. Screen #8 OD-Ocular Disease Screen #2 Case Report Abstract An Atypical Case of Retinitis Punctata Albescens OD-Ocular Disease Jeff Rabin, OD, MS, PHD Co-Author(s) Differentiating Subclinical Retinal Detachment, Peripheral Anjli Patel Retinoschisis, and White Without Pressure with Optical Melanie Cadavos, BS Coherence Tomography. Jacob Hansen, BS Jessica Haynes, OD Hiten Patel, BS Co-Author(s) Screen #9 Mohammad Rafieetary, OD OD-Ocular Disease Screen #3 Ocular Complications of Intraconal Cavernous Hemangioma Information Abstract Noor Abushagur, OD Reactivation of Herpes Zoster Co-Author(s) Tony Tran, OD student Jennifer Deakins, OD, FAOO Andrew Kemp, OD, FAAO Screen #4 OD-Ocular Disease Screen #10 OD-Ocular Disease A Case of Polypoidal Choroidal Vasculopathy - Utilizing advanced imaging modalities to appreciate the Pachychoroid Find the Culprit: A Case of Reversible Bilateral Visual Field Spectrum of Diseases Defect and Aripiprazole use Nathan Traxler, OD Karen Choi, OD Screen #6 Screen #11 Scientific Abstract Scientific Abstract Prevalence of Visual Deficits and Dysfunctions associated Sustained IOP Control with Single or Multiple Trabecular with Traumatic Brain Injury (TBI): A Meta- Analyses Micro-Bypass Stents (iStent) Evaluated in Subjects with Open-Angle Glaucoma: 5 Year Outcomes Felix M Barker II OD MS Co-Author(s) Whitney Hauser, O.D. -

Shruti Ravula Outline
I. CASE HISTORY: • Patient demographics: 49 yo African-American male • Chief complaint: Blur @ distance with current bifocal • Ocular History: H/o eye drop prescribed by private provider for “pressure” used 1x/day— pt self discontinued • Family Ocular History: + Glaucoma: Mother, Father & Grandparents • Medical History: Emphysema, H/o Migraine, PTSD, Hyperlipidemia, Sleep Apnea • Medications: Prednisolone 10Mg II. CLINICAL • VA cc 20/40+2 OD, 20/25+2 OS • TA: 36 OU with Goldmann • Confrontational Fields: Restricted OD/OS • Pachymetry: OD: 589, OS: 583 • Gonioscopy: OD: TM 360 w/ 2+ pigment • OS: TM 360 w/ 2+ pigment • HVF 24-2: o OD: Central inferior island of vision remaining o OS: Central inferior island of vision remaining • HVF 10-2: o OD: Superior and Nasal absolute defects. Inferior temporal island of vision remaining: 5H x 6V degree of vision o OS: Superior and Nasal absolute defects. Inferior temporal island of vision remaining: 8H x 7V degree of vision • OCT Macula: o OD: Macula schisis; Deep optic pit and lamina loss evident + ERM o OS: Retinoschisis noted superior to ONH; Deep optic pit and lamina loss evident + ERM III. PHYSICAL: • Dilated Fundus Exam: 0.9R Extremely thin rim 360 Deep Cup OD; 0.9R thinning 360, small areas of nasal rim intact OS. Macula: Retinoschisis OD, Grade 1 ERM with OU with mild macular traction with flat intact macula OU. IV. DIFFERENTIAL DIAGNOSIS: • PRIMARY: Progression of POAG associated with Acquired pits of the Optic nerve and maculoschisis. • SECONDARY: Congenital optic nerve anomaly with associated maculoschisis contributing to progression of POAG. V. DIAGNOSIS & DISCUSSION: • GENERAL: o Optic Neuropathy associated with glaucoma represents a loss of axons of the retinal ganglion cell fibers at the level of the lamina cribosa. -

Peripapillary Schisis in Glaucoma Patients with Narrow Angles and Increased Intraocular Pressure
Peripapillary Schisis in Glaucoma pits, pseudopits, or colobomas, and to discuss the potential association between spontaneous retinal schisis resolution Patients With Narrow Angles and and increased intraocular pressure (IOP). Increased Intraocular Pressure Malik Y. Kahook, Robert J. Noecker, ● CASE 1: A 48-year-old woman with a nine-year history of Hiroshi Ishikawa, Gadi Wollstein, glaucoma presented with IOPs of 31 right eye (OD) and 21 Larry Kagemann, Maciej Wojtkowski, left eye (OS) and occludable angles. Manifest refraction was Ϫ1.00 diopters OD and Ϫ0.75 diopters OS. The OD had Jay S. Duker, Vivek J. Srinivasan, peripapillary retinoschisis extending into the macula with no James G. Fujimoto, and Joel S. Schuman apparent vitreous detachment or optic nerve pit, although there was inferotemporal cupping to the disk margin in the PURPOSE: To describe two cases of peripapillary retinal area of the schisis. Visual field testing was normal in the OS, schisis in patients with glaucoma without evidence of and there was a superior arcuate scotoma in the OD. Standard optic nerve pits, pseudopits, or X-linked retinoschisis. optical coherence tomography (OCT) (StratusOCT; Carl DESIGN: Two observational case reports and literature Zeiss Meditec, Dublin, California, USA) artifactually re- review. ported schisis cavities as retinal nerve fiber layer METHODS: Imaging of the peripapillary nerve fiber layer (RNFL) thickening (Figure 1); Heidelberg retinal tomog- and schisis cavities was completed in two patients, and raphy revealed normal RNFL in the OS and RNFL one patient was followed over time. thinning in the inferotemporal segment of the OD. IOP RESULTS: The first patient, diagnosed with narrow angle improved after bilateral laser peripheral iridectomies and glaucoma, was noted to have peripapillary schisis in the bimatoprost therapy. -

Adeno-Associated Virus 8-Mediated Gene Therapy for Choroideremia: Preclinical Studies in in Vitro Ind in Vivo Models
University of Pennsylvania ScholarlyCommons Publicly Accessible Penn Dissertations 2015 Adeno-Associated Virus 8-Mediated Gene Therapy for Choroideremia: Preclinical Studies in in Vitro ind in Vivo Models Aaron Daniel Black University of Pennsylvania, [email protected] Follow this and additional works at: https://repository.upenn.edu/edissertations Part of the Genetics Commons, Ophthalmology Commons, and the Virology Commons Recommended Citation Black, Aaron Daniel, "Adeno-Associated Virus 8-Mediated Gene Therapy for Choroideremia: Preclinical Studies in in Vitro ind in Vivo Models" (2015). Publicly Accessible Penn Dissertations. 1014. https://repository.upenn.edu/edissertations/1014 This paper is posted at ScholarlyCommons. https://repository.upenn.edu/edissertations/1014 For more information, please contact [email protected]. Adeno-Associated Virus 8-Mediated Gene Therapy for Choroideremia: Preclinical Studies in in Vitro ind in Vivo Models Abstract Choroideremia (CHM) is a slowly progressive X-linked retinal degeneration that results ultimately in total blindness due to loss of photoreceptors, retinal pigment epithelium, and choroid. CHM, the gene implicated in choroideremia, encodes Rab escort protein-1 (REP-1), which is involved in the post- translational activation via prenylation of Rab proteins. We evaluated AAV8.CBA.hCHM, a human CHM encoding recombinant adeno-associated virus serotype 8 (rAAV8) vector, which targets retinal cells efficiently, for therapeutic effect and safety in vitro and in vivo in a murine model of CHM. In vitro studies assayed the ability of the vector to produce functional REP-1 protein in established cell lines and in CHM patient derived primary fibroblasts. Assays included Western blots, immunofluorescent labeling, and a REP-1 functional assay which measured the ability of exogenous REP-1 to prenylate Rab proteins.