Blueprint Genetics Nephrolithiasis Panel
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Alternative Splicing of Bicistronic MOCS1 Defines a Novel Mitochondrial Protein
bioRxiv preprint doi: https://doi.org/10.1101/429183; this version posted September 27, 2018. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. Alternative splicing of bicistronic MOCS1 defines a novel mitochondrial protein maturation mechanism Simon Julius Mayr1, Juliane Röper1 and Guenter Schwarz1,2,3,* 1 Institute of Biochemistry, Department of Chemistry, University of Cologne, 50674 Cologne, Germany 2 Center for Molecular Medicine Cologne, University of Cologne, 50931 Cologne, Germany 3 Cluster of Excellence Cluster in Aging Research, University of Cologne, 50931 Cologne, Germany * correspondence: [email protected] Running Title: Mitochondrial MOCS1 protein maturation bioRxiv preprint doi: https://doi.org/10.1101/429183; this version posted September 27, 2018. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. Abstract Molybdenum cofactor biosynthesis is a conserved multistep pathway. The first step, the conversion of GTP to cyclic pyranopterin monophosphate (cPMP), requires bicsistronic MOCS1. Alternative splicing of MOCS1 in exons 1 and 9 produces four different N-terminal and three different C-terminal products (type I-III). Type I splicing results in bicistronic transcripts with two open reading frames, of which only the first, MOCS1A, is translated, whereas type II/III splicing produces two-domain MOCS1AB proteins. Here, we report and characterize the mitochondrial translocation of alternatively spliced MOCS1 proteins. While MOCS1A requires exon 1a for mitochondrial translocation, MOCS1AB variants target to mitochondria via an internal motif overriding the N-terminal targeting signal. -

Supplement 1 Overview of Dystonia Genes
Supplement 1 Overview of genes that may cause dystonia in children and adolescents Gene (OMIM) Disease name/phenotype Mode of inheritance 1: (Formerly called) Primary dystonias (DYTs): TOR1A (605204) DYT1: Early-onset generalized AD primary torsion dystonia (PTD) TUBB4A (602662) DYT4: Whispering dystonia AD GCH1 (600225) DYT5: GTP-cyclohydrolase 1 AD deficiency THAP1 (609520) DYT6: Adolescent onset torsion AD dystonia, mixed type PNKD/MR1 (609023) DYT8: Paroxysmal non- AD kinesigenic dyskinesia SLC2A1 (138140) DYT9/18: Paroxysmal choreoathetosis with episodic AD ataxia and spasticity/GLUT1 deficiency syndrome-1 PRRT2 (614386) DYT10: Paroxysmal kinesigenic AD dyskinesia SGCE (604149) DYT11: Myoclonus-dystonia AD ATP1A3 (182350) DYT12: Rapid-onset dystonia AD parkinsonism PRKRA (603424) DYT16: Young-onset dystonia AR parkinsonism ANO3 (610110) DYT24: Primary focal dystonia AD GNAL (139312) DYT25: Primary torsion dystonia AD 2: Inborn errors of metabolism: GCDH (608801) Glutaric aciduria type 1 AR PCCA (232000) Propionic aciduria AR PCCB (232050) Propionic aciduria AR MUT (609058) Methylmalonic aciduria AR MMAA (607481) Cobalamin A deficiency AR MMAB (607568) Cobalamin B deficiency AR MMACHC (609831) Cobalamin C deficiency AR C2orf25 (611935) Cobalamin D deficiency AR MTRR (602568) Cobalamin E deficiency AR LMBRD1 (612625) Cobalamin F deficiency AR MTR (156570) Cobalamin G deficiency AR CBS (613381) Homocysteinuria AR PCBD (126090) Hyperphelaninemia variant D AR TH (191290) Tyrosine hydroxylase deficiency AR SPR (182125) Sepiaterine reductase -

Enzymatic Encoding Methods for Efficient Synthesis Of
(19) TZZ__T (11) EP 1 957 644 B1 (12) EUROPEAN PATENT SPECIFICATION (45) Date of publication and mention (51) Int Cl.: of the grant of the patent: C12N 15/10 (2006.01) C12Q 1/68 (2006.01) 01.12.2010 Bulletin 2010/48 C40B 40/06 (2006.01) C40B 50/06 (2006.01) (21) Application number: 06818144.5 (86) International application number: PCT/DK2006/000685 (22) Date of filing: 01.12.2006 (87) International publication number: WO 2007/062664 (07.06.2007 Gazette 2007/23) (54) ENZYMATIC ENCODING METHODS FOR EFFICIENT SYNTHESIS OF LARGE LIBRARIES ENZYMVERMITTELNDE KODIERUNGSMETHODEN FÜR EINE EFFIZIENTE SYNTHESE VON GROSSEN BIBLIOTHEKEN PROCEDES DE CODAGE ENZYMATIQUE DESTINES A LA SYNTHESE EFFICACE DE BIBLIOTHEQUES IMPORTANTES (84) Designated Contracting States: • GOLDBECH, Anne AT BE BG CH CY CZ DE DK EE ES FI FR GB GR DK-2200 Copenhagen N (DK) HU IE IS IT LI LT LU LV MC NL PL PT RO SE SI • DE LEON, Daen SK TR DK-2300 Copenhagen S (DK) Designated Extension States: • KALDOR, Ditte Kievsmose AL BA HR MK RS DK-2880 Bagsvaerd (DK) • SLØK, Frank Abilgaard (30) Priority: 01.12.2005 DK 200501704 DK-3450 Allerød (DK) 02.12.2005 US 741490 P • HUSEMOEN, Birgitte Nystrup DK-2500 Valby (DK) (43) Date of publication of application: • DOLBERG, Johannes 20.08.2008 Bulletin 2008/34 DK-1674 Copenhagen V (DK) • JENSEN, Kim Birkebæk (73) Proprietor: Nuevolution A/S DK-2610 Rødovre (DK) 2100 Copenhagen 0 (DK) • PETERSEN, Lene DK-2100 Copenhagen Ø (DK) (72) Inventors: • NØRREGAARD-MADSEN, Mads • FRANCH, Thomas DK-3460 Birkerød (DK) DK-3070 Snekkersten (DK) • GODSKESEN, -

A Gene Expression Resource Generated by Genome-Wide Lacz
© 2015. Published by The Company of Biologists Ltd | Disease Models & Mechanisms (2015) 8, 1467-1478 doi:10.1242/dmm.021238 RESOURCE ARTICLE A gene expression resource generated by genome-wide lacZ profiling in the mouse Elizabeth Tuck1,**, Jeanne Estabel1,*,**, Anika Oellrich1, Anna Karin Maguire1, Hibret A. Adissu2, Luke Souter1, Emma Siragher1, Charlotte Lillistone1, Angela L. Green1, Hannah Wardle-Jones1, Damian M. Carragher1,‡, Natasha A. Karp1, Damian Smedley1, Niels C. Adams1,§, Sanger Institute Mouse Genetics Project1,‡‡, James N. Bussell1, David J. Adams1, Ramiro Ramırez-Soliś 1, Karen P. Steel1,¶, Antonella Galli1 and Jacqueline K. White1,§§ ABSTRACT composite of RNA-based expression data sets. Strong agreement was observed, indicating a high degree of specificity in our data. Knowledge of the expression profile of a gene is a critical piece of Furthermore, there were 1207 observations of expression of a information required to build an understanding of the normal and particular gene in an anatomical structure where Bgee had no essential functions of that gene and any role it may play in the data, indicating a large amount of novelty in our data set. development or progression of disease. High-throughput, large- Examples of expression data corroborating and extending scale efforts are on-going internationally to characterise reporter- genotype-phenotype associations and supporting disease gene tagged knockout mouse lines. As part of that effort, we report an candidacy are presented to demonstrate the potential of this open access adult mouse expression resource, in which the powerful resource. expression profile of 424 genes has been assessed in up to 47 different organs, tissues and sub-structures using a lacZ reporter KEY WORDS: Gene expression, lacZ reporter, Mouse, Resource gene. -

(ESI) for Toxicology Research
Electronic Supplementary Material (ESI) for Toxicology Research. This journal is © The Royal Society of Chemistry 2014 Supplementary data 1 Particle preparation and characterization 1.1 SWCNT preparation The purchased SWCNTs (P2-SWNTs, Carbon Solutions, Inc. CA, USA) have a poor dispersibility and colloidal stability in aqueous medium. To make well-dispersed SWCNTs in aqueous medium with a proper colloidal stability for the duration of the experiments, the purchased SWCNTs were accurately weighted and suspended in dimethyl sulfoxide (DMSO) to 0.125 mg/mL, followed by ultrasonication for 30 minutes in a water bath sonicator (B3510, Branson Ultrasonics, 40KHz). In the last minute of ultrasonication, the SWCNTs-DMSO suspension was rapidly diluted 5 times by injecting a stabilization buffer (5 mg/mL BSA and 10 mM NaCl in MilliQ water). The mixture, referred to as as-dispersed SWCNTs (AD-SWCNTs), resulted in a clear dark-brown suspension. No sedimentation of AD-SWCNTs was observed for weeks at room temperature indicating a good colloidal stability. To remove the majority of DMSO and free BSA, AD-SWCNTs were pelleted by centrifugation at 16,000 g, 4 °C for 30 min followed by three times wash with 10 mM NaCl in MilliQ water under the same conditions. The colloidal stability and surface charge of SWCNTs at each step were monitored by dynamic light scattering analysis (DLS) (see below). The depletion of DMSO and BSA was monitored by UV-Visible absorption analysis (see below). The SWCNTs aggregates and metallic impurities were characterized by TEM and TEM-EDX (see below). After the washing steps, SWCNTs were re-dispersed in MilliQ water with 10 mM NaCl to about 0.4 mg/mL, which was used in the experiments and here referred to as prepared SWCNTs. -

XIST-Induced Silencing of Flanking Genes Is Achieved by Additive Action of Repeat a Monomers in Human Somatic Cells
Minks et al. Epigenetics & Chromatin 2013, 6:23 http://www.epigeneticsandchromatin.com/content/6/1/23 RESEARCH Open Access XIST-induced silencing of flanking genes is achieved by additive action of repeat a monomers in human somatic cells Jakub Minks, Sarah EL Baldry, Christine Yang, Allison M Cotton and Carolyn J Brown* Abstract Background: The establishment of facultative heterochromatin by X-chromosome inactivation requires the long non-coding RNA XIST/Xist. However, the molecular mechanism by which the RNA achieves chromosome-wide gene silencing remains unknown. Mouse Xist has been shown to have redundant domains for cis-localization, and requires a series of well-conserved tandem ‘A’ repeats for silencing. We previously described a human inducible XIST transgene that is capable of cis-localization and suppressing a downstream reporter gene in somatic cells, and have now leveraged these cells to dissect the sequences critical for XIST-dependent gene silencing in humans. Results: We demonstrated that expression of the inducible full-length XIST cDNA was able to suppress expression of two nearby reporter genes as well as endogenous genes up to 3 MB from the integration site. An inducible construct containing the repeat A region of XIST alone could silence the flanking reporter genes but not the more distal endogenous genes. Reporter gene silencing could also be accomplished by a synthetic construct consisting of nine copies of a consensus repeat A sequence, consistent with previous studies in mice. Progressively shorter constructs showed a linear relationship between the repeat number and the silencing capacity of the RNA. Constructs containing only two repeat A units were still able to partially silence the reporter genes and could thus be used for site-directed mutagenesis to demonstrate that sequences within the two palindromic cores of the repeat are essential for silencing, and that it is likely the first palindrome sequence folds to form a hairpin, consistent with compensatory mutations observed in eutherian sequences. -

Molybdenum Cofactor and Sulfite Oxidase Deficiency Jochen Reiss* Institute of Human Genetics, University Medicine Göttingen, Germany
ics: O om pe ol n b A a c t c e e M s s Reiss, Metabolomics (Los Angel) 2016, 6:3 Metabolomics: Open Access DOI: 10.4172/2153-0769.1000184 ISSN: 2153-0769 Research Article Open Access Molybdenum Cofactor and Sulfite Oxidase Deficiency Jochen Reiss* Institute of Human Genetics, University Medicine Göttingen, Germany Abstract A universal molybdenum-containing cofactor is necessary for the activity of all eukaryotic molybdoenzymes. In humans four such enzymes are known: Sulfite oxidase, xanthine oxidoreductase, aldehyde oxidase and a mitochondrial amidoxime reducing component. Of these, sulfite oxidase is the most important and clinically relevant one. Mutations in the genes MOCS1, MOCS2 or GPHN - all encoding cofactor biosynthesis proteins - lead to molybdenum cofactor deficiency type A, B or C, respectively. All three types plus mutations in the SUOX gene responsible for isolated sulfite oxidase deficiency lead to progressive neurological disease which untreated in most cases leads to death in early childhood. Currently, only for type A of the cofactor deficiency an experimental treatment is available. Introduction combination with SUOX deficiency. Elevated xanthine and lowered uric acid concentrations in the urine are used to differentiate this Isolated sulfite oxidase deficiency (MIM#606887) is an autosomal combined form from the isolated SUOX deficiency. Rarely and only in recessive inherited disease caused by mutations in the sulfite oxidase cases of isolated XOR deficiency xanthine stones have been described (SUOX) gene [1]. Sulfite oxidase is localized in the mitochondrial as a cause of renal failure. Otherwise, isolated XOR deficiency often intermembrane space, where it catalyzes the oxidation of sulfite to goes unnoticed. -

Supplementary Materials
Supplementary materials Supplementary Table S1: MGNC compound library Ingredien Molecule Caco- Mol ID MW AlogP OB (%) BBB DL FASA- HL t Name Name 2 shengdi MOL012254 campesterol 400.8 7.63 37.58 1.34 0.98 0.7 0.21 20.2 shengdi MOL000519 coniferin 314.4 3.16 31.11 0.42 -0.2 0.3 0.27 74.6 beta- shengdi MOL000359 414.8 8.08 36.91 1.32 0.99 0.8 0.23 20.2 sitosterol pachymic shengdi MOL000289 528.9 6.54 33.63 0.1 -0.6 0.8 0 9.27 acid Poricoic acid shengdi MOL000291 484.7 5.64 30.52 -0.08 -0.9 0.8 0 8.67 B Chrysanthem shengdi MOL004492 585 8.24 38.72 0.51 -1 0.6 0.3 17.5 axanthin 20- shengdi MOL011455 Hexadecano 418.6 1.91 32.7 -0.24 -0.4 0.7 0.29 104 ylingenol huanglian MOL001454 berberine 336.4 3.45 36.86 1.24 0.57 0.8 0.19 6.57 huanglian MOL013352 Obacunone 454.6 2.68 43.29 0.01 -0.4 0.8 0.31 -13 huanglian MOL002894 berberrubine 322.4 3.2 35.74 1.07 0.17 0.7 0.24 6.46 huanglian MOL002897 epiberberine 336.4 3.45 43.09 1.17 0.4 0.8 0.19 6.1 huanglian MOL002903 (R)-Canadine 339.4 3.4 55.37 1.04 0.57 0.8 0.2 6.41 huanglian MOL002904 Berlambine 351.4 2.49 36.68 0.97 0.17 0.8 0.28 7.33 Corchorosid huanglian MOL002907 404.6 1.34 105 -0.91 -1.3 0.8 0.29 6.68 e A_qt Magnogrand huanglian MOL000622 266.4 1.18 63.71 0.02 -0.2 0.2 0.3 3.17 iolide huanglian MOL000762 Palmidin A 510.5 4.52 35.36 -0.38 -1.5 0.7 0.39 33.2 huanglian MOL000785 palmatine 352.4 3.65 64.6 1.33 0.37 0.7 0.13 2.25 huanglian MOL000098 quercetin 302.3 1.5 46.43 0.05 -0.8 0.3 0.38 14.4 huanglian MOL001458 coptisine 320.3 3.25 30.67 1.21 0.32 0.9 0.26 9.33 huanglian MOL002668 Worenine -
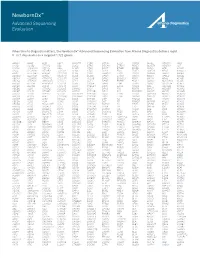
Cldn19 Clic2 Clmp Cln3
NewbornDx™ Advanced Sequencing Evaluation When time to diagnosis matters, the NewbornDx™ Advanced Sequencing Evaluation from Athena Diagnostics delivers rapid, 5- to 7-day results on a targeted 1,722-genes. A2ML1 ALAD ATM CAV1 CLDN19 CTNS DOCK7 ETFB FOXC2 GLUL HOXC13 JAK3 AAAS ALAS2 ATP1A2 CBL CLIC2 CTRC DOCK8 ETFDH FOXE1 GLYCTK HOXD13 JUP AARS2 ALDH18A1 ATP1A3 CBS CLMP CTSA DOK7 ETHE1 FOXE3 GM2A HPD KANK1 AASS ALDH1A2 ATP2B3 CC2D2A CLN3 CTSD DOLK EVC FOXF1 GMPPA HPGD K ANSL1 ABAT ALDH3A2 ATP5A1 CCDC103 CLN5 CTSK DPAGT1 EVC2 FOXG1 GMPPB HPRT1 KAT6B ABCA12 ALDH4A1 ATP5E CCDC114 CLN6 CUBN DPM1 EXOC4 FOXH1 GNA11 HPSE2 KCNA2 ABCA3 ALDH5A1 ATP6AP2 CCDC151 CLN8 CUL4B DPM2 EXOSC3 FOXI1 GNAI3 HRAS KCNB1 ABCA4 ALDH7A1 ATP6V0A2 CCDC22 CLP1 CUL7 DPM3 EXPH5 FOXL2 GNAO1 HSD17B10 KCND2 ABCB11 ALDOA ATP6V1B1 CCDC39 CLPB CXCR4 DPP6 EYA1 FOXP1 GNAS HSD17B4 KCNE1 ABCB4 ALDOB ATP7A CCDC40 CLPP CYB5R3 DPYD EZH2 FOXP2 GNE HSD3B2 KCNE2 ABCB6 ALG1 ATP8A2 CCDC65 CNNM2 CYC1 DPYS F10 FOXP3 GNMT HSD3B7 KCNH2 ABCB7 ALG11 ATP8B1 CCDC78 CNTN1 CYP11B1 DRC1 F11 FOXRED1 GNPAT HSPD1 KCNH5 ABCC2 ALG12 ATPAF2 CCDC8 CNTNAP1 CYP11B2 DSC2 F13A1 FRAS1 GNPTAB HSPG2 KCNJ10 ABCC8 ALG13 ATR CCDC88C CNTNAP2 CYP17A1 DSG1 F13B FREM1 GNPTG HUWE1 KCNJ11 ABCC9 ALG14 ATRX CCND2 COA5 CYP1B1 DSP F2 FREM2 GNS HYDIN KCNJ13 ABCD3 ALG2 AUH CCNO COG1 CYP24A1 DST F5 FRMD7 GORAB HYLS1 KCNJ2 ABCD4 ALG3 B3GALNT2 CCS COG4 CYP26C1 DSTYK F7 FTCD GP1BA IBA57 KCNJ5 ABHD5 ALG6 B3GAT3 CCT5 COG5 CYP27A1 DTNA F8 FTO GP1BB ICK KCNJ8 ACAD8 ALG8 B3GLCT CD151 COG6 CYP27B1 DUOX2 F9 FUCA1 GP6 ICOS KCNK3 ACAD9 ALG9 -

Molecular Diagnostic Requisition
BAYLOR MIRACA GENETICS LABORATORIES SHIP TO: Baylor Miraca Genetics Laboratories 2450 Holcombe, Grand Blvd. -Receiving Dock PHONE: 800-411-GENE | FAX: 713-798-2787 | www.bmgl.com Houston, TX 77021-2024 Phone: 713-798-6555 MOLECULAR DIAGNOSTIC REQUISITION PATIENT INFORMATION SAMPLE INFORMATION NAME: DATE OF COLLECTION: / / LAST NAME FIRST NAME MI MM DD YY HOSPITAL#: ACCESSION#: DATE OF BIRTH: / / GENDER (Please select one): FEMALE MALE MM DD YY SAMPLE TYPE (Please select one): ETHNIC BACKGROUND (Select all that apply): UNKNOWN BLOOD AFRICAN AMERICAN CORD BLOOD ASIAN SKELETAL MUSCLE ASHKENAZIC JEWISH MUSCLE EUROPEAN CAUCASIAN -OR- DNA (Specify Source): HISPANIC NATIVE AMERICAN INDIAN PLACE PATIENT STICKER HERE OTHER JEWISH OTHER (Specify): OTHER (Please specify): REPORTING INFORMATION ADDITIONAL PROFESSIONAL REPORT RECIPIENTS PHYSICIAN: NAME: INSTITUTION: PHONE: FAX: PHONE: FAX: NAME: EMAIL (INTERNATIONAL CLIENT REQUIREMENT): PHONE: FAX: INDICATION FOR STUDY SYMPTOMATIC (Summarize below.): *FAMILIAL MUTATION/VARIANT ANALYSIS: COMPLETE ALL FIELDS BELOW AND ATTACH THE PROBAND'S REPORT. GENE NAME: ASYMPTOMATIC/POSITIVE FAMILY HISTORY: (ATTACH FAMILY HISTORY) MUTATION/UNCLASSIFIED VARIANT: RELATIONSHIP TO PROBAND: THIS INDIVIDUAL IS CURRENTLY: SYMPTOMATIC ASYMPTOMATIC *If family mutation is known, complete the FAMILIAL MUTATION/ VARIANT ANALYSIS section. NAME OF PROBAND: ASYMPTOMATIC/POPULATION SCREENING RELATIONSHIP TO PROBAND: OTHER (Specify clinical findings below): BMGL LAB#: A COPY OF ORIGINAL RESULTS ATTACHED IF PROBAND TESTING WAS PERFORMED AT ANOTHER LAB, CALL TO DISCUSS PRIOR TO SENDING SAMPLE. A POSITIVE CONTROL MAY BE REQUIRED IN SOME CASES. REQUIRED: NEW YORK STATE PHYSICIAN SIGNATURE OF CONSENT I certify that the patient specified above and/or their legal guardian has been informed of the benefits, risks, and limitations of the laboratory test(s) requested. -

Whole Exome Sequencing Identifies Causative Mutations in the Majority of Consanguineous Or Familial Cases with Childhood-Onset Increased Renal Echogenicity
Whole exome sequencing identifies causative mutations in the majority of consanguineous or familial cases with childhood-onset increased renal echogenicity The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters Citation Braun, D. A., M. Schueler, J. Halbritter, H. Y. Gee, J. D. Porath, J. A. Lawson, R. Airik, et al. 2015. “Whole exome sequencing identifies causative mutations in the majority of consanguineous or familial cases with childhood-onset increased renal echogenicity.” Kidney international 89 (2): 468-475. doi:10.1038/ki.2015.317. http:// dx.doi.org/10.1038/ki.2015.317. Published Version doi:10.1038/ki.2015.317 Citable link http://nrs.harvard.edu/urn-3:HUL.InstRepos:29002589 Terms of Use This article was downloaded from Harvard University’s DASH repository, and is made available under the terms and conditions applicable to Other Posted Material, as set forth at http:// nrs.harvard.edu/urn-3:HUL.InstRepos:dash.current.terms-of- use#LAA HHS Public Access Author manuscript Author ManuscriptAuthor Manuscript Author Kidney Manuscript Author Int. Author manuscript; Manuscript Author available in PMC 2016 August 01. Published in final edited form as: Kidney Int. 2016 February ; 89(2): 468–475. doi:10.1038/ki.2015.317. Whole exome sequencing identifies causative mutations in the majority of consanguineous or familial cases with childhood- onset increased renal echogenicity Daniela A. Braun#1, Markus Schueler#1, Jan Halbritter1, Heon Yung Gee1, Jonathan D. Porath1, Jennifer A. Lawson1, Rannar Airik1, Shirlee Shril1, Susan J. Allen2, Deborah Stein1, Adila Al Kindy3, Bodo B. -

Downloaded from the App Store and Nucleobase, Nucleotide and Nucleic Acid Metabolism 7 Google Play
Hoytema van Konijnenburg et al. Orphanet J Rare Dis (2021) 16:170 https://doi.org/10.1186/s13023-021-01727-2 REVIEW Open Access Treatable inherited metabolic disorders causing intellectual disability: 2021 review and digital app Eva M. M. Hoytema van Konijnenburg1†, Saskia B. Wortmann2,3,4†, Marina J. Koelewijn2, Laura A. Tseng1,4, Roderick Houben6, Sylvia Stöckler‑Ipsiroglu5, Carlos R. Ferreira7 and Clara D. M. van Karnebeek1,2,4,8* Abstract Background: The Treatable ID App was created in 2012 as digital tool to improve early recognition and intervention for treatable inherited metabolic disorders (IMDs) presenting with global developmental delay and intellectual disabil‑ ity (collectively ‘treatable IDs’). Our aim is to update the 2012 review on treatable IDs and App to capture the advances made in the identifcation of new IMDs along with increased pathophysiological insights catalyzing therapeutic development and implementation. Methods: Two independent reviewers queried PubMed, OMIM and Orphanet databases to reassess all previously included disorders and therapies and to identify all reports on Treatable IDs published between 2012 and 2021. These were included if listed in the International Classifcation of IMDs (ICIMD) and presenting with ID as a major feature, and if published evidence for a therapeutic intervention improving ID primary and/or secondary outcomes is avail‑ able. Data on clinical symptoms, diagnostic testing, treatment strategies, efects on outcomes, and evidence levels were extracted and evaluated by the reviewers and external experts. The generated knowledge was translated into a diagnostic algorithm and updated version of the App with novel features. Results: Our review identifed 116 treatable IDs (139 genes), of which 44 newly identifed, belonging to 17 ICIMD categories.