Shoulder Arthrodesis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
Managing and Recognizing Complications After Treatment of Acromioclavicular Joint Repair Or Reconstruction
See discussions, stats, and author profiles for this publication at: https://www.researchgate.net/publication/272096166 Managing and recognizing complications after treatment of acromioclavicular joint repair or reconstruction Article in Current Reviews in Musculoskeletal Medicine · February 2015 DOI: 10.1007/s12178-014-9255-6 · Source: PubMed CITATION READS 1 182 6 authors, including: Patrick A Smith Matthew J Smith University of Missouri University of Missouri 28 PUBLICATIONS 255 CITATIONS 16 PUBLICATIONS 115 CITATIONS SEE PROFILE SEE PROFILE Seth L Sherman David L Flood University of Missouri University of Missouri 69 PUBLICATIONS 1,378 CITATIONS 3 PUBLICATIONS 21 CITATIONS SEE PROFILE SEE PROFILE Some of the authors of this publication are also working on these related projects: Commentary & Perspective Total Hip Arthroplasty View project Drug Reaction with Eosinophilia and Systemic Symptoms Associated with a Vancomycin-Impregnated Spacer View project All content following this page was uploaded by Xinning Li on 15 February 2015. The user has requested enhancement of the downloaded file. Curr Rev Musculoskelet Med DOI 10.1007/s12178-014-9255-6 SHOULDER SURGERY: COMPLICATIONS (X LI, SECTION EDITOR) Managing and recognizing complications after treatment of acromioclavicular joint repair or reconstruction Richard Ma & Patrick A. Smith & Matthew J. Smith & Seth L. Sherman & David Flood & Xinning Li # Springer Science+Business Media New York 2015 Abstract Complications of the acromioclavicular joint inju- Introduction ries can occur as a result of the injury itself, conservative management, or surgical treatment. Fortunately, the majority Injuries to the acromioclavicular (AC) joint are common, par- of acromioclavicular surgeries utilizing modern techniques ticularly among the young and active population. -

Functional Outcome Oxford Shoulder Score After Modified Weaver Dunn Technique Reconstruction in Patients with Acromioclavicular Injuries
International Journal of PharmTech Research CODEN (USA): IJPRIF, ISSN: 0974-4304, ISSN(Online): 2455-9563 Vol.12, No.03, pp 71-74, 2019 Functional Outcome Oxford Shoulder Score after Modified Weaver Dunn Technique Reconstruction in Patients with Acromioclavicular Injuries Hendra1*, Nino Nasution2, Andriandi3, Asnan Lelo4 1Resident of Orthopaedic and Traumatology, Faculty of Medicine University of Sumatera Utara/ Haji Adam Malik Hospital-Medan, Indonesia 2Consultant of Orthopaedic and Traumatology, Faculty of Medicine University of Sumatera Utara/ Haji Adam Malik Hospital-Medan, Indonesia 3Consultant of Orthopaedic and Traumatology, Faculty of Medicine University of Sumatera Utara/ Haji Adam Malik Hospital-Medan, Indonesia 4Statistic Consultant of Orthopaedic and Traumatology, Faculty of Medicine University of Sumatera Utara/ Haji Adam Malik Hospital-Medan, Indonesia Abstract : Objective : The aim of this study was to compare the clinical outcome of Oxford Shoulder Score in patients with acromioclavicular injuries that were operated with Modified Weaver Dunn Technique Reconstruction compared with the healthy side. Material And Methods : A total of 8 patients with acromioclavicular injuries from 2011 until 2019 that were included into the study that were treated with Modified Weaver Dunn Technique. Age, gender, range of motion and OSS score that was followed for minimum 6 months after surgery (Oxford Shoulder Score [OSS]) were recorded. Results : Patients' gender characteristics totalled three females (3) and five males (5). There weren’t -

Evaluation of the Painful Shoulder
Evaluation of the Painful Shoulder J. Lindsay Quade, MD Clinical Instructor Internal Medicine/Pediatrics, Sports Medicine Michigan Medicine Objectives • To improve physician comfort with obtaining relevant history in the evaluation of the painful shoulder • To improve physician comfort with physical examination of the shoulder, including special testing • To improve physician comfort with diagnosis and management of common causes of shoulder pain The Shoulder • Shoulder pain is common in the primary care setting, responsible for 16% of all musculoskeletal complaints. • Taking a good history can help tailor the physical exam and narrow the diagnosis. • Knowledge of common shoulder disorders is important as they can often be treated with conservative measures and without referral to a subspecialist. Shoulder Anatomy Shoulder Anatomy Shoulder Anatomy Shoulder Anatomy MSK Shoulder Pain Differential • Articular Causes • Periarticular Causes • Glenohumeral (GH) and acromoclavicular • Chronic impingement and rotator cuff (AC) arthritis tendinitis • Ligamentous and labral lesions • Bicep tendinitis • GH and AC joint instability • Rotator cuff and long biceps tendon tears • Osseus: fracture, osteonecrosis, neoplasm, • Subacromial bursitis infection • Adhesive capsulitis Taking Your History • Age • Duration • Grinding or clicking • Hand dominance • Radiation • Weakness • Occupation • Aggravating/relieving • Numbness/tingling factors • Sports/physical activities • Pain • Night pain • Trauma • Effect on shoulder • Onset function • Location • Stiffness/restriction -

Subtalar Joint Version 1.0 Effective June 15, 2021
CLINICAL GUIDELINES CMM-407: Arthroscopy: Subtalar Joint Version 1.0 Effective June 15, 2021 Clinical guidelines for medical necessity review of Comprehensive Musculoskeletal Management Services. © 2021 eviCore healthcare. All rights reserved. Comprehensive Musculoskeletal Management Guidelines V1.0 CMM-407: Arthroscopy: Subtalar Joint Definitions 3 General Guidelines 3 Indications 4 Non-Indications 5 Procedure (CPT®) Codes 5 References 6 ______________________________________________________________________________________________________ ©2021 eviCore healthcare. All Rights Reserved. Page 2 of 6 400 Buckwalter Place Boulevard, Bluffton, SC 29910 (800) 918-8924 www.eviCore.com Comprehensive Musculoskeletal Management Guidelines V1.0 Definitions Red flags indicate comorbidities that require urgent/emergent diagnostic imaging and/or referral for definitive therapy. Clinically meaningful improvement is defined as at least 50% improvement noted on global assessment. General Guidelines Either of the following are considered red flag conditions for subtalar joint arthroscopy: Post-reduction evaluation and management of the subtalar dislocation Septic arthritis in the subtalar joint Although imaging may be normal, prior to subtalar joint arthroscopy, radiographic imaging should be performed and include both of the following: Plain X-rays with one or more views (anteroposterior, lateral, axial, and/or Broden’s) to confirm and differentiate any of the following: Degenerative joint changes Loose bodies Osteochondral lesions Impingement -

In Patients with End-Stage Ankle Arthritis, How Does Total Ankle Arthroplasty Compared to Arthrodesis Affect Ankle Pain and Function?
University of the Pacific Scholarly Commons Physician's Assistant Program Capstones School of Health Sciences 4-1-2020 In Patients with End-Stage Ankle Arthritis, How Does Total Ankle Arthroplasty Compared to Arthrodesis Affect Ankle Pain and Function? Zachary Whipple University of the Pacific, [email protected] Follow this and additional works at: https://scholarlycommons.pacific.edu/pa-capstones Part of the Medicine and Health Sciences Commons Recommended Citation Whipple, Zachary, "In Patients with End-Stage Ankle Arthritis, How Does Total Ankle Arthroplasty Compared to Arthrodesis Affect Ankle Pain and Function?" (2020). Physician's Assistant Program Capstones. 84. https://scholarlycommons.pacific.edu/pa-capstones/84 This Capstone is brought to you for free and open access by the School of Health Sciences at Scholarly Commons. It has been accepted for inclusion in Physician's Assistant Program Capstones by an authorized administrator of Scholarly Commons. For more information, please contact [email protected]. In Patients with End-Stage Ankle Arthritis, How Does Total Ankle Arthroplasty Compared to Arthrodesis Affect Ankle Pain and Function? By Zachary Whipple Capstone Project Submitted to the Faculty of the Department of Physician Assistant Education of the University of the Pacific in partial fulfilment of the requirements for the degree of MASTER OF PHYSICIAN ASSISTANT STUDIES April 2020 Introduction End-stage ankle arthritis is a debilitating degenerative disease commonly located at the tibiotalar joint. The prevalence of symptomatic arthritis is about nine times lower than the rates associated with those of the knee or hip.1 Though less common than knee and hip arthritis, the US estimates greater than 50,000 new cases are reported each year.2 The most common etiology of ankle arthritis is post-traumatic pathology. -

Differences Between Subtotal Corpectomy and Laminoplasty for Cervical Spondylotic Myelopathy
Spinal Cord (2010) 48, 214–220 & 2010 International Spinal Cord Society All rights reserved 1362-4393/10 $32.00 www.nature.com/sc ORIGINAL ARTICLE Differences between subtotal corpectomy and laminoplasty for cervical spondylotic myelopathy S Shibuya1, S Komatsubara1, S Oka2, Y Kanda1, N Arima1 and T Yamamoto1 1Department of Orthopaedic Surgery, School of Medicine, Kagawa University, Kagawa, Japan and 2Oka Orthopaedic and Rehabilitation Clinic, Kagawa, Japan Objective: This study aimed to obtain guidelines for choosing between subtotal corpectomy (SC) and laminoplasty (LP) by analysing the surgical outcomes, radiological changes and problems associated with each surgical modality. Study Design: A retrospective analysis of two interventional case series. Setting: Department of Orthopaedic Surgery, Kagawa University, Japan. Methods: Subjects comprised 34 patients who underwent SC and 49 patients who underwent LP. SC was performed by high-speed drilling to remove vertebral bodies. Autologous strut bone grafting was used. LP was performed as an expansive open-door LP. The level of decompression was from C3 to C7. Clinical evaluations included recovery rate (RR), frequency of C5 root palsy after surgery, re-operation and axial pain. Radiographic assessments included sagittal cervical alignment and bone union. Results: Comparisons between the two groups showed no significant differences in age at surgery, preoperative factors, RR and frequency of C5 palsy. Progression of kyphotic changes, operation time and volumes of blood loss and blood transfusion were significantly greater in the SC (two- or three- level) group. Six patients in the SC group required additional surgery because of pseudoarthrosis, and four patients underwent re-operation because of adjacent level disc degeneration. -

Procedure Coding in ICD-9-CM and ICD- 10-PCS
Procedure Coding in ICD-9-CM and ICD- 10-PCS ICD-9-CM Volume 3 Procedures are classified in volume 3 of ICD-9-CM, and this section includes both an Alphabetic Index and a Tabular List. This volume follows the same format, organization and conventions as the classification of diseases in volumes 1 and 2. ICD-10-PCS ICD-10-PCS will replace volume 3 of ICD-9-CM. Unlike ICD-10-CM for diagnoses, which is similar in structure and format as the ICD-9-CM volumes 1 and 2, ICD-10-PCS is a completely different system. ICD-10-PCS has a multiaxial seven-character alphanumeric code structure providing unique codes for procedures. The table below gives a brief side-by-side comparison of ICD-9-CM and ICD-10-PCS. ICD-9-CM Volume3 ICD-10-PCS Follows ICD structure (designed for diagnosis Designed and developed to meet healthcare coding) needs for a procedure code system Codes available as a fixed or finite set in list form Codes constructed from flexible code components (values) using tables Codes are numeric Codes are alphanumeric Codes are 3-4 digits long All codes are seven characters long ICD-9-CM and ICD-10-PCS are used to code only hospital inpatient procedures. Hospital outpatient departments, other ambulatory facilities, and physician practices are required to use CPT and HCPCS to report procedures. ICD-9-CM Conventions in Volume 3 Code Also In volume 3, the phrase “code also” is a reminder to code additional procedures only when they have actually been performed. -

Knee Arthrodesis After Failed Total Knee Arthroplasty
650 COPYRIGHT Ó 2019 BY THE JOURNAL OF BONE AND JOINT SURGERY,INCORPORATED Current Concepts Review Knee Arthrodesis After Failed Total 04/12/2019 on 1mhtSo9F6TkBmpGAR5GLp6FT3v73JgoS8Zn360/N4fAEQXu6c15Knc+cXP2J5+wvbQY2nVcoOF2DIk3Zd0BSqmOXRD8WUDFCPOJ9CnEHMNOmtIbs3S0ykA== by http://journals.lww.com/jbjsjournal from Downloaded Knee Arthroplasty Downloaded Asim M. Makhdom, MD, MSc, FRCSC, Austin Fragomen, MD, and S. Robert Rozbruch, MD from http://journals.lww.com/jbjsjournal Investigation performed at the Hospital for Special Surgery, Weill Cornell Medicine, Cornell University, New York, NY ä Knee arthrodesis after failure of a total knee arthroplasty (TKA) because of periprosthetic joint infection (PJI) may provide superior functional outcome and ambulatory status compared with above-the-knee amputation. by 1mhtSo9F6TkBmpGAR5GLp6FT3v73JgoS8Zn360/N4fAEQXu6c15Knc+cXP2J5+wvbQY2nVcoOF2DIk3Zd0BSqmOXRD8WUDFCPOJ9CnEHMNOmtIbs3S0ykA== ä The use of an intramedullary nail (IMN) for knee arthrodesis following removal of TKA components because of a PJI may result in higher fusion rates compared with external fixation devices. ä The emerging role of the antibiotic cement-coated interlocking IMN may expand the indications to achieve knee fusion in a single-stage intervention. ä Massive bone defects after failure of an infected TKA can be managed with various surgical strategies in a single- stage intervention to preserve leg length and function. Primary total knee arthroplasty (TKA) is a common procedure suppressive antibiotics for recurrent PJIs are generally reserved with a reported increase of 162% from 1991 to 2010 in the for patients with more severe preoperative disability and United States1,2. From 2005 to 2030, it is projected that the medical comorbidity and those who are not candidates to number of TKA procedures will grow by 673% or 3.5 million. -
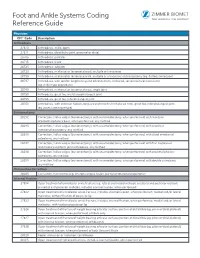
Foot and Ankle Systems Coding Reference Guide
Foot and Ankle Systems Coding Reference Guide Physician CPT® Code Description Arthrodesis 27870 Arthrodesis, ankle, open 27871 Arthrodesis, tibiofibular joint, proximal or distal 28705 Arthrodesis; pantalar 28715 Arthrodesis; triple 28725 Arthrodesis; subtalar 28730 Arthrodesis, midtarsal or tarsometatarsal, multiple or transverse 28735 Arthrodesis, midtarsal or tarsometatarsal, multiple or transverse; with osteotomy (eg, flatfoot correction) 28737 Arthrodesis, with tendon lengthening and advancement, midtarsal, tarsal navicular-cuneiform (eg, miller type procedure) 28740 Arthrodesis, midtarsal or tarsometatarsal, single joint 28750 Arthrodesis, great toe; metatarsophalangeal joint 28755 Arthrodesis, great toe; interphalangeal joint 28760 Arthrodesis, with extensor hallucis longus transfer to first metatarsal neck, great toe, interphalangeal joint (eg, jones type procedure) Bunionectomy 28292 Correction, hallux valgus (bunionectomy), with sesamoidectomy, when performed; with resection of proximal phalanx base, when performed, any method 28295 Correction, hallux valgus (bunionectomy), with sesamoidectomy, when performed; with proximal metatarsal osteotomy, any method 28296 Correction, hallux valgus (bunionectomy), with sesamoidectomy, when performed; with distal metatarsal osteotomy, any method 28297 Correction, hallux valgus (bunionectomy), with sesamoidectomy, when performed; with first metatarsal and medial cuneiform joint arthrodesis, any method 28298 Correction, hallux valgus (bunionectomy), with sesamoidectomy, when performed; with -

Clinical Guidelines
CLINICAL GUIDELINES Joint Services Guidelines Version 1.0.2019 Clinical guidelines for medical necessity review of comprehensive musculoskeletal management services. © 2019 eviCore healthcare. All rights reserved. Regence: Comprehensive Musculoskeletal Management Guidelines V1.0.2019 Large Joint Services CMM-311: Knee Replacement/Arthroplasty 3 CMM-312: Knee Surgery-Arthroscopic and Open Procedures 14 CMM-313: Hip Replacement/Arthroplasty 35 CMM-314: Hip Surgery-Arthroscopic and Open Procedures 46 CMM-315: Shoulder Surgery-Arthroscopic and Open Procedures 47 CMM-318: Shoulder Arthroplasty/ Replacement/ Resurfacing/ Revision/ Arthrodesis 62 ______________________________________________________________________________________________________ © 2019 eviCore healthcare. All Rights Reserved. Page 2 of 69 400 Buckwalter Place Boulevard, Bluffton, SC 29910 (800) 918-8924 www.eviCore.com Regence: Comprehensive Musculoskeletal Management Guidelines V1.0.2019 CMM-311: Knee Replacement/Arthroplasty CMM-311.1: Definition 4 CMM-311.2: General Guidelines 5 CMM-311.3: Indications and Non-Indications 5 CMM-311.4 Experimental, Investigational, or Unproven 9 CMM-311.5: Procedure (CPT®) Codes 10 CMM-311.6: References 10 ______________________________________________________________________________________________________ © 2019 eviCore healthcare. All Rights Reserved. Page 3 of 69 400 Buckwalter Place Boulevard, Bluffton, SC 29910 (800) 918-8924 www.eviCore.com Regence: Comprehensive Musculoskeletal Management Guidelines V1.0.2019 CMM-311.1: Definition -

Everything You Need to Know About Your Surgery at Adena
EVERYTHINGEVERYTHING YOU YOU NEED NEED TO TO KNOW KNOW ABOUTABOUT YOUR YOUR SURGERY SURGERY AT AT ADENA ADENA TOTALTOTAL KNEE SHOULDER JOINT REPLACEMENT REPLACEMENT YOUR PARTNER IN HIGH-QUALITY CARE WE ARE DELIGHTED THAT YOU HAVE CHOSEN ADENA MEDICAL CENTER FOR YOUR TOTAL SHOULDER REPLACEMENT. WE ARE COMMITTED TO PROVIDING BEST-IN-NATION, HIGH QUALITY, PATIENT-CENTERED ORTHOPAEDIC CARE. OUR MISSION: TO HEAL, TO EDUCATE, TO CARE OUR VISION: TO BE THE BEST HEALTHCARE SYSTEM IN THE NATION OUR VALUES: INTEGRITY, COMMUNICATION, TEAMWORK, INNOVATION PAGE - 1 WHY CHOOSE ADENA FOR YOUR SHOULDER REPLACEMENT? OUR DEDICATED PROFESSIONALS ARE PASSIONATE ABOUT HELPING PATIENTS REGAIN THEIR MOBILITY SO THEY CAN ENJOY LIFE. Our medical team includes physical and occupational YOU GET YOUR OWN therapists, nurses, technicians, board-certified PATIENT NAVIGATOR neurologists, physiatrists, sports medicine physicians, orthopaedic surgeons, ortho-spine surgeons and An important part of the joint replacement team is the neuro-spine surgeons. You’ve been living with patient navigator. After you and your orthopaedic debilitating pain, and we want to help you get back surgeon decide that surgery is the best option, you will to enjoying a full and active life. be assigned a patient navigator. This is the person who will help you schedule your appointments before and ADENA HAS THE BEST JOINT after surgery, arrange pre-admission testing and work REPLACEMENT SURGEONS to make sure that all your needs are met. Our orthopaedic surgeons and neuro-spine and ortho-spine surgeons have trained at some of the best programs in the country. They’re at the top of their field and represent the largest group of fellowship-trained physicians in the region. -

Breakthrough in Shoulder Surgery Brings New Hope to Patients
Breakthrough in Shoulder Surgery Brings New Hope to Patients ll her life, Millie has been active – raising six children, bowling in a league, even skating in After a shoulder replacement, Millie Athe roller derby 60 years ago. But when is back to the job she loves at the 81-year-old from Chantilly began Louise Archer Elementary School. experiencing difficulty raising her arms to complete simple tasks such as brushing her hair or reaching up to a shelf, she knew something was wrong. Her limited range of motion also made it hard to do her office job at Louise Archer Elementary School in Vienna. Millie consulted Commonwealth surgeon David Novak, MD, who diagnosed advanced osteoarthritis in both her shoulders. When several months of cortisone shots failed to alleviate her symptoms, she opted for a total shoulder replacement on her left side. This procedure involves replacing the arthritic joint surfaces with a metal and plastic implant. The components come Dr. Novak is among just a handful of surgeons in the area who in various sizes and are either cemented or press fit into the bone. perform this advanced procedure. “Patients like Millie, with end-stage arthritis and intact rotator cuff tendons, who no longer respond to conservative treatment – such Following both of her surgeries, Millie wore a sling for four weeks. as NSAIDs, cortisone or physical therapy – are generally good She spent two months working with a physical therapist on exercises candidates for total shoulder replacement,” Dr. Novak explains. to regain range of motion and strengthen her shoulder joint. It was all part of a rigorous rehabilitation program that every patient goes The surgery restored function to Millie’s left shoulder and she was through.