A Newly Discovered Muscle: the Tensor of the Vastus Intermedius
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
An Intramuscular Injection Is an Injection Given Directly Into The
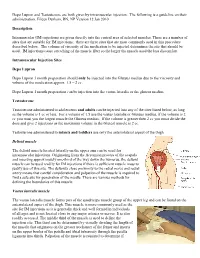
Depo Lupron and Testosterone are both given by intramuscular injection. The following is a guideline on their administration. Eileen Durham, RN, NP Version 12 Jan 2010 Description Intramuscular (IM) injections are given directly into the central area of selected muscles. There are a number of sites that are suitable for IM injections; there are three sites that are most commonly used in this procedure described below. The volume of viscosity of the medication to be injected determines the site that should be used. IM injections cause stretching of the muscle fiber so the larger the muscle used the less discomfort. Intramuscular Injection Sites Depo Lupron Depo Lupron 3 month preparation should only be injected into the Gluteus medius due to the viscosity and volume of the medication approx. 1.5 – 2 cc. Depo Lupron 1 month preparation can be injection into the vastus lateralis or the gluteus medius. Testosterone Testosterone administered to adolescents and adults can be injected into any of the sites listed below, as long as the volume is 1 cc or less. For a volume of 1.5 use the vastus lateralis or Gluteus medius, if the volume is 2 cc you must you the largest muscle the Gluteus medius. If the volume is greater then 2 cc you must divide the dose and give 2 injections as the maximum volume in the Gluteal muscle is 2 cc. Testosterone administered to infants and toddlers use only the anteriolateral aspect of the thigh. Deltoid muscle The deltoid muscle located laterally on the upper arm can be used for intramuscular injections. -

Bacterial Meningitis and Multiple Abscess Formation in the Iliopsoas
Yamada et al. Renal Replacement Therapy (2018) 4:22 https://doi.org/10.1186/s41100-018-0163-x CASEREPORT Open Access Bacterial meningitis and multiple abscess formation in the iliopsoas, erector spinae, and vastus lateralis muscle in a maintenance hemodialysis patient treated with continuous epidural anesthesia for herpes zoster-related pain control: a case report and review of the literature Shunsuke Yamada1, Narihito Tatsumoto1, Noriko Nakamura1, Kosuke Masutani1, Toshiro Maeda2, Takanari Kitazono1 and Kazuhiko Tsuruya1,3* Abstract Background: Infection is the second leading cause of mortality in patients who undergo maintenance hemodialysis. In this population, impairment in both cellular and humoral immunity contributes to the increased incidence of infection and infection-related hospitalization. However, these artificial devices occasionally enhance the risk of deep organ infection including muscle abscess, frequently leading to disability and mortality in hemodialysis patients. Case presentation: A 54-year-old male undergoing maintenance hemodialysis was hospitalized because of the acute onset pain in the back and bilateral legs and declining consciousness which started at 7 days after the treatment of herpes zoster-related neuralgia with continuous epidural anesthesia. Physical examination revealed purulent discharge from the insertion site of the catheter. Serum biochemical tests showed increased inflammatory response and malnutrition. Magnetic resonance imaging revealed meningitis and multiple abscesses in the iliopsoas, erector spinae, gluteus medius, and vastus lateralis muscles, where conventional antibiotic treatment often fails to cure. Staphylococcus aureus was detected in the cerebrospinal fluid. Combination of intravenous antibiotics treatment and aggressive open surgical drainage of the muscle abscesses finally cured meningitis and multiple deep muscle abscesses in this patient. -

Acellular Dermal Graft Augmentation in Quadriceps Tendon Rupture Repair
INNOVATIONS IN PRACTICE Acellular dermal graft augmentation in quadriceps tendon rupture repair Ross M. Wilkins INTRODUCTION cific pain and swelling of the knee indicative of other more nstability of the knee from failure of the extensor frequent soft-tissue maladies such as ligament rupture, mechanism is a debilitating problem. Extensor mechan- partial tears, and the presence of intact medial and lateral 19 ism failure frequently is the result of patellar tendon patellar retinacula and iliotibial band. The purpose of this I retrospective review was to describe a ‘‘stent’’ augmentation rupture, quadriceps tendon rupture, patellar fracture or avulsion of the patellar tendon.1,2 Such failures have method for rupture of the quadriceps tendon and evaluate been linked to underlying pathologies such as diabetes the effects of quadriceps tendon augmentation in both the mellitus, gout, corticosteroid use, autoimmune inflamma- presence and absence of a TKA. tory diseases, hyperthyroidism, obesity and end-stage renal disease.3--8 Often, the treatment of this problem is com- MATERIALS AND METHODS pounded by the presence of a total knee arthroplasty (TKA) Eight knees in seven patients were treated using acellular or the need for a TKA.7 Depending on the root cause of the human dermal matrix, (AHDM; GRAFT JACKETs Matrix, instability, there are a variety of ways to treat this soft-tissue Wright Medical Technology, Arlington TN) for chronic insufficiency. Historically, problems of the extensor me- quadriceps tendon rupture at a single institution. Four chanism have been operatively treated using primary repair, of these patients presented with a TKA, with one patient tendon autografts, fascia, extensor mechanism allografts, having had bilateral TKA. -

Applications of the Pedicled Vastus Lateralis Flap for Patients with Complicated Pressure Sores
Spinal Cord (1997) 35, 437 ± 442 1997 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/97 $12.00 Applications of the pedicled vastus lateralis ¯ap for patients with complicated pressure sores AB Schmidt1, G Fromberg1 and M-H Ruidisch2 1Abt. fuÈr Plastische-, Hand-, Kiefer- und rekonstruktive Mikrochirurgie, BG Unfallklinik Murnau; 2Abt. fuÈr RuÈckenmark- und WirbelsaÈulenverletztungen, BG Unfallklinik Murnau, Germany The vastus lateralis muscle- or musculocutaneous ¯ap is a well established tool in the surgery of pressure sores of the pelvic region. Its size, its constant large axial vascular pedicle originating from the lateral circum¯ex femoral artery, and its ability to carry quite a large skin island from the distal lateral region of the upper thigh makes this ¯ap a very versatile one in the management of dicult situations. The vastus lateralis ¯ap allows the simultaneous closure of defects in the trochanteric and sacral region, a technique which has not been described previously. A pedicled vastus lateralis ¯ap may be the only remaining local salvage procedure for defects due to obstruction of internal and external iliac arteries and aortobifemoral bypass surgery. This is another application which has not yet been described in the medical literature. The outcome of a series of 38 vastus lateralis ¯aps and the complications are shown. The follow-up period ranged from 3 months to 4 years. One ¯ap was lost. More complications were seen at the donor site than at the reconstructed defect. In patients who may be able to walk or stand at a later date, potential impairment of these functions has to be considered. -

A Cadaver Research
Journal of Arthroscopy and Joint Surgery 6 (2019) 114e116 Contents lists available at ScienceDirect Journal of Arthroscopy and Joint Surgery journal homepage: www.elsevier.com/locate/jajs Tensile strength comparison between hamstring tendon, patellar tendon, quadriceps tendon and peroneus longus tendon: A cadaver research * Krisna Y. Phatama a, , Mohamad Hidayat a, Edi Mustamsir a, Ananto Satya Pradana a, Brian Dhananjaya b, Surya Iman Muhammad b a Orthopaedic and Traumatology Department, Lower Extremity and Adult Reconstruction Division, Saiful Anwar Hospital, Jalan Jaksa Agung Suprapto No.2, Klojen, Kota Malang, Jawa Timur, 65112, Indonesia b Orthopaedic and Traumatology Department, Saiful Anwar Hospital, Jalan Jaksa Agung Suprapto No. 2, Klojen, Kota Malang, Jawa Timur, 65112, Indonesia article info abstract Article history: Knee ligament injury is a frequent occurrence. Ligament reconstruction using tendon graft is the best Received 6 December 2018 therapy recommendation in the case of severe knee ligament injury. Tendon graft that is oftenly used are Accepted 15 February 2019 hamstring tendon, patellar tendon (BPTB), quadriceps tendon and peroneus longus tendon have been Available online 19 February 2019 proposed as tendon graft donor. Biomechanically, tensile strength from tendon graft is the main factor that greatly contributes to the success of ligament reconstruction procedure. Numerous researches have Keywords: been done to calculate tensile strengths of hamstring and patellar tendon, but there has not been a Ligament reconstruction research done yet on the comparison of the tensile strengths of peroneus longus tendon, hamstring, Tendon graft Tensile strength patellar tendon and quadriceps tendon. This research will strive to record the tensile strengths of per- oneus longus tendon, hamstring, patellar tendon and quadriceps tendon as well as their comparison. -

Repair of Rectus Femoris Rupture with LARS Ligament
BMJ Case Reports: first published as 10.1136/bcr.06.2011.4359 on 20 March 2012. Downloaded from Novel treatment (new drug/intervention; established drug/procedure in new situation) Repair of rectus femoris rupture with LARS ligament Clare Taylor, Rathan Yarlagadda, Jonathan Keenan Trauma and Orthopaedics Department, Derriford Hospital, Plymouth, UK Correspondence to Miss Clare Taylor, [email protected] Summary The rectus femoris muscle is the most frequently involved quadriceps muscle in strain pathologies. The majority of quadriceps muscle belly injuries can be successfully treated conservatively and even signifi cant tears in the less active and older population, non-operative management is a reasonable option. The authors report the delayed presentation of a 17-year-old male who sustained an injury to his rectus femoris muscle belly while playing football. This young patient did not recover the functional outcome required to get back to running and participating in sport despite 15 months of physiotherapy and non-operative management. Operative treatment using the ligament augmentation and reconstruction system ligament to augment Kessler repair allowed immediate full passive fl exion of the knee and an early graduated physiotherapy programme. Our patient was able to return to running and his previous level of sport without any restrictions. BACKGROUND confi rmed a tear (at least grade 2) in the proximal musculo- The rectus femoris muscle is the most frequently involved tendinous junction of the rectus femoris. The patient had quadriceps muscle in strain pathologies,1 2 principally pain and weakness in the thigh and had been unable to because of its two joint function and high percentage of return to any sport. -

The Role of and Relationship Between Hamstring and Quadriceps Muscle Myofascial Trigger Points in Patients with Patellofemoral Pain Syndrome
The role of and relationship between Hamstring and Quadriceps muscle myofascial trigger points in patients with patellofemoral pain syndrome. By Karen Louise Frandsen Smith A mini-dissertation submitted in partial compliance with the requirements for the Master’s Degree in Technology: Chiropractic at the Durban University of Technology I, Karen Louise Frandsen Smith, declare that this dissertation is representative of my own work in both conception and execution (except where acknowledgements indicate to the contrary). _______________________ ________________ Karen Louise Frandsen Smith Date Approved for Submission _______________________ ________________ Dr Brian Kruger (supervisor) Date M. Tech. Chiro., C.C.S.P. Dedication I dedicate this work to everyone who loves me and have supported me throughout these years of studying and all the difficult times. It is thanks to you that I have reached my dream. Dad, you would be so proud. i Acknowledgements Thank you to the DUT staff, patients, and supervisor, Dr Brian Kruger for making this happen. Thanks to my class mates for making the years fly by, and creating lifelong memories. This dissertation would not have been completed without supportive, generous and helpful people. Special thanks to you, Dr Danella Lubbe for motivating me and thank you so much Dr Charmaine Korporaal for “picking me up” and helping me finish. Endless gratitude goes to you Damon, Cherine, Mom and Viggo. You are / were all my anchors in the storm, and without your belief in me, I would be nowhere. ii Abstract Purpose: Patellofemoral Pain Syndrome is a common condition in all age groups, with a multi- factorial etiology. -

Quadriceps Tendon Rupture Anatomy & Biomechanics
QUADRICEPS TENDON RUPTURE AND SURGICAL REPAIR Page 1 of 6 QUADRICEPS TENDON RUPTURE ANATOMY & BIOMECHANICS Figure 1: Frontal View of Normal Patellar Tendon and Extensor Mechanism. At the top of the patella, the quadriceps tendon is attached. At the top of the quadriceps tendon is the quadriceps muscle. The quadriceps muscle is the large muscle on the front of the thigh. As the quadriceps muscle contracts (shortens), it pulls on the quadriceps tendon, the patella, the patellar tendon, and the tibia to move the knee from a flexed (bent) position to an extended (straight) position. Conversely, when the quadriceps muscle relaxes, it lengthens. This allows the knee to move from a position of extension (straight) to a position of flexion (bent). (Click HERE for a computer animation of basic knee motion (mpg file) courtesy of Rob Kroeger.) http://www.arthroscopy.com/quadrep.htm 9/5/2006 QUADRICEPS TENDON RUPTURE AND SURGICAL REPAIR Page 2 of 6 Figure 2: Lateral View of a Normal Knee with an Intact Quadriceps Tendon. Figure 3: Lateral View of a Normal Knee with an Intact Quadriceps Tendon. INJURY When the quadriceps tendon ruptures, the patella loses its anchoring support in the thigh. Without this anchoring effect of the intact quadriceps tendon, the patella tends to move inferiorly (towards the foot). Without the intact quadriceps tendon, the patient is unable to straighten the knee. If a rupture of the quadriceps tendon occurs, and the patient tries to http://www.arthroscopy.com/quadrep.htm 9/5/2006 QUADRICEPS TENDON RUPTURE AND SURGICAL REPAIR Page 3 of 6 stand up, the knee will usually buckle and give way because the body is no longer able to hold the knee in a position of extension (straight). -

Quadriceps Tendon Repair
Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.MeadowsMD.com Quadriceps Tendon Repair What to Expect The patella is embedded in the quadriceps and patella tendons and acts as a pulley to increase the amount of force that can be generated by the quadriceps muscles to extend the knee. The quadriceps tendon attaches the quadriceps muscles to the patella and the patella tendon connects the patella to the tibial tubercle. These strong tendons can be torn by forceful contraction of the quadriceps muscles during sports, jumping, a fall, or a direct blow to the knee. Surgery is indicated to restore motion and stability to the knee and restore normal gait. The torn tendon is repaired using various techniques involving strong sutures, drill tunnels through the patella, or suture anchors to reattach the tendon to the patella. Chronic tears may be reconstructed using a tendon graft to augment the repair. Appropriate tension is applied to the repair and the repair must be protected to allow the tendon to heal in the first few weeks after surgery. A hinged knee brace is used to control your knee motion to avoid re-tearing the repair before it has completely healed. Appropriate rehabilitation is critical to the success of the procedure. Phase 1 (0 – 2 weeks postop) Goals: Control pain, Diminish swelling, Begin regaining knee motion—achieve full knee extension, Protect the tendon repair • Pain: You will be prescribed pain medication to use after surgery. -

Chapter 10 the Knee Joint
The Knee Joint • Knee joint – largest joint in body Chapter 10 – very complex The Knee Joint – primarily a hinge joint Manual of Structural Kinesiology Modified for Prentice WE: Arnheim’s principles of athletic training , ed 12, New R.T. Floyd, EdD, ATC, CSCS York, 2006, McGraw-Hill; from Saladin, KS: Anatomy &physiology: the unity of forms and function , ed 2, New York, 2001, McGraw- Hill. © 2007 McGraw-Hill Higher Education. All rights reserved. 10-1 © 2007 McGraw-Hill Higher Education. All rights reserved. 10-2 Bones Bones • Enlarged femoral condyles articulate on • Fibula - lateral enlarged tibial condyles – serves as the attachment for • Medial & lateral tibial condyles (medial & knee joint lateral tibial plateaus) - receptacles for structures femoral condyles – does not articulate • Tibia – medial with femur or patella – bears most of weight – not part of knee joint Modified from Anthony CP, Kolthoff NJ: Textbook of anatomy and physiology , ed 9, St. Louis, 1975, Mosby. © 2007 McGraw-Hill Higher Education. All rights reserved. 10-3 © 2007 McGraw-Hill Higher Education. All rights reserved. 10-4 Bones Bones • Patella • Key bony landmarks – sesamoid (floating) bone – Superior & inferior patellar poles – imbedded in quadriceps – Tibial tuberosity & patellar tendon – Gerdy’s tubercle – serves similar to a pulley – Medial & lateral femoral in improving angle of condyles pull, resulting in greater – Upper anterior medial tibial mechanical advantage in surface – Head of fibula knee extension Modified from Anthony CP, Kolthoff NJ: Textbook of anatomy and physiology , ed 9, St. Louis, 1975, Mosby. © 2007 McGraw-Hill Higher Education. All rights reserved. 10-5 © 2007 McGraw-Hill Higher Education. All rights reserved. -

Anatomy of the Lateral Retinaculum
Anatomy of the lateral retinaculum Introduction The lateral retinaculum of the knee is not a distinct anatomic structure but is composed of various fascial structures on the lateral side of the patella. Anatomical descriptions of the lateral retinaculum have been published, but the attachments, name or even existence of its tissue bands and layers are controversial. The medial patellofemoral ligament on the other hand has been more recently re-examined and its detailed anatomy characterised (Amis et al., 2003, Nomura et al., 2005, Panagiotopoulos et al., 2006, Smirk and Morris, 2003, Tuxoe et al., 2002) The first fascial layer is the fascia lata (deep fascia) that continues to envelop the knee from the thigh (Kaplan, 1957). The fascia lata covers the patellar region but does not adhere to the quadriceps apparatus. The iliotibial tract is integral to the deep fascia and is a lateral thickening of the fascia lata. The anterior expansion of the iliotibial band curves forward. It forms a group of arciform fibres and blends with the fascia lata covering the patella. Fulkerson (Fulkerson and Gossling, 1980) described the anatomy of the knee lateral retinaculum in two distinctly separate layers (Figure 1). The superficial oblique layer originates from the iliotibial band and interdigitates with the longitudinal fibres of the vastus lateralis. The deep layer consist of the deep transverse retinaculum with the epicondylopatellar ligament proximally and the patellotibial ligament distally. The patellotibial ligament proceeds obliquely to attach to the lateral meniscus and tibia. The epicondylopatellar ligament was said to be probably the same 1 ligament described by Kaplan. -

Tendon Geometry After Rectus Femoris Tendon Transfer by DEANNA S
COPYRIGHT © 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Three-Dimensional Muscle- Tendon Geometry After Rectus Femoris Tendon Transfer BY DEANNA S. ASAKAWA, PHD, SILVIA S. BLEMKER, MS, GEORGE T. RAB, MD, ANITA BAGLEY, PHD, AND SCOTT L. DELP, PHD Investigation performed at the Department of Mechanical Engineering, Stanford University, Stanford, the Shriners Hospital for Children Northern California, Sacramento, and the Veterans Affairs Palo Alto Health Care System, Palo Alto, California Background: Rectus femoris tendon transfer is performed in patients with cerebral palsy to improve knee flexion during walking. This procedure involves detachment of the muscle from its insertion into the quadriceps tendon and reattachment to one of the knee flexor muscles. The purpose of the present study was to evaluate the muscle-tendon geometry and to assess the formation of scar tissue between the rectus femoris and adjacent structures. Methods: Magnetic resonance images of the lower extremities were acquired from five subjects after bilateral rectus femoris tendon transfer. A three-dimensional computer model of the musculoskeletal geometry of each of the ten limbs was created from these images. Results: The three-dimensional paths of the rectus femoris muscles after transfer demonstrated that the muscle does not follow a straight course from its origin to its new insertion. The typical muscle-tendon path included an an- gular deviation; this deviation was sharp (>35°) in seven extremities. In addition, scar tissue between the transferred rectus femoris and the underlying muscles was visible on the magnetic resonance images. Conclusions: The angular deviations in the rectus femoris muscle-tendon path and the presence of scar tissue be- tween the rectus femoris and the underlying muscles suggest that the beneficial effects of rectus femoris tendon transfer are derived from reducing the effects of the rectus femoris muscle as a knee extensor rather than from con- verting the muscle to a knee flexor.