Acute Encephalitis Is a Neurological Emergency Which Can Lumbar Puncture (LP), Which in Practice Is Often Delayed
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Chasing the Dragon, a Case of Leukoencephalopathy Associated with Heroin Inhalation
Chasing the dragon, a case of leukoencephalopathy associated with heroin inhalation Daniel Cho MD1, Hani Nazha MD2, Kalin Fisher BS2 Author Affiliations: 1. Charleston Area Medical Center, Charleston, West Virginia 2. West Virginia University, Morgantown, West Virginia The authors have no financial disclosures to declare and no conflicts of interest to report. Corresponding Author: Hani Nazha MD West Virginia University Morgantown, West Virginia Email: [email protected] Abstract Although rare, toxic leukoencephalopathy (TLE) associated with heroin inhalation has been reported. “Chasing the dragon” may lead to progressive spongiform degeneration of the brain and presents with a large range of neuropsychological sequelae. This case is an example of TLE in a middle-aged white male with a history of polysubstance abuse. He presented with a three week history of progressive neuropsychological symptoms, including abulia, bradyphrenia, hyperreflexia, and visual hallucinations. He was initially suspected to have progressive multifocal leukoencephalopathy, however, JCV PCR was negative. MRI showed diffuse abnormal signal in the white matter, extending into the thalami and cerebral peduncles. Brain biopsy was performed, which revealed spongiform degeneration, and a diagnosis of TLE was made. The patient was then transferred to a skilled nursing facility. Clinical suspicion based on a thorough history and clinical exam findings is paramount in recognition of heroin-associated TLE. Although rare, heroin-inhalation TLE continues to be reported. As ‘chasing the dragon’ is gaining popularity among drug users, it is important for clinicians to be able to recognize this disease process. Keywords Opioid, Addiction, Heroin, Leukoencephalopathy Introduction Toxic leukoencephalopathy (TLE) associated with heroin abuse was first described in 1982.1 “Chasing the dragon" is a method of heroin vapor inhalation in which a small amount of heroin powder is placed on aluminum foil, which is then heated by placing a match or lighter underneath. -

Viral Encephalitis: a Hard Nut to Crack
Published online: 02.10.2019 THIEME 98 ViralReview Encephalitis Article Shukla et al. Viral Encephalitis: A Hard Nut to Crack Alka Shukla1 Mayank Gangwar1 Sonam Rastogi1 Gopal Nath1 1Department of Microbiology, Viral Research and Diagnostic Address for correspondence Gopal Nath, MD, PhD, Department Laboratory, Institute of Medical Sciences, Banaras Hindu of Microbiology, Viral Research and Diagnostic Laboratory, Institute University, Varanasi, India of Medical Sciences, Banaras Hindu University, Varanasi, India (e-mail: [email protected]). Ann Natl Acad Med Sci (India) 2019;55:98–109 Abstract Viral encephalitis is inflammation of brain that manifests as neurological complication of viral infections. There are quite a good number of viruses, for example, human her- pes virus, Japanese encephalitis, and enteroviruses that can result in such a dreadful condition. Geographical location, age, gender, immune status, and climatic conditions also contribute to the establishment of this disease in an individual. Clinical signs and symptoms include fever, headache, altered level of consciousness, changed mental status, body ache, seizures, nausea, and vomiting. Effective management of this dis- ease relies on timely diagnosis that in turn depends on apt and suitable investigation Keywords techniques. Traditional investigations have thinned out these days owing to the fact ► encephalitis that advanced molecular technologies have been introduced to the diagnostic field. ► viral infection Treatment of viral encephalitis mainly involves symptomatic relieve from fever, mal- ► pathogenesis aise, myalgia along with measures to reduce viral load in the patient. This review men- ► molecular techniques tions about all the possible aspects of viral encephalitis starting from etiology to the ► management management and preventive measures that include immunization and vector control. -

Encephalopathy and Encephalitis Associated with Cerebrospinal
SYNOPSIS Encephalopathy and Encephalitis Associated with Cerebrospinal Fluid Cytokine Alterations and Coronavirus Disease, Atlanta, Georgia, USA, 2020 Karima Benameur,1 Ankita Agarwal,1 Sara C. Auld, Matthew P. Butters, Andrew S. Webster, Tugba Ozturk, J. Christina Howell, Leda C. Bassit, Alvaro Velasquez, Raymond F. Schinazi, Mark E. Mullins, William T. Hu There are few detailed investigations of neurologic unnecessary staff exposure and difficulties in estab- complications in severe acute respiratory syndrome lishing preillness neurologic status without regular coronavirus 2 infection. We describe 3 patients with family visitors. It is known that neurons and glia ex- laboratory-confirmed coronavirus disease who had en- press the putative SARS-CoV-2 receptor angiotensin cephalopathy and encephalitis develop. Neuroimaging converting enzyme 2 (7), and that the related coro- showed nonenhancing unilateral, bilateral, and midline navirus SARS-CoV (responsible for the 2003 SARS changes not readily attributable to vascular causes. All 3 outbreak) can inoculate the mouse olfactory bulb (8). patients had increased cerebrospinal fluid (CSF) levels If SARS-CoV-2 can enter the central nervous system of anti-S1 IgM. One patient who died also had increased (CNS) directly or through hematogenous spread, ce- levels of anti-envelope protein IgM. CSF analysis also rebrospinal fluid (CSF) changes, including viral RNA, showed markedly increased levels of interleukin (IL)-6, IgM, or cytokine levels, might support CNS infec- IL-8, and IL-10, but severe acute respiratory syndrome coronavirus 2 was not identified in any CSF sample. tion as a cause for neurologic symptoms. We report These changes provide evidence of CSF periinfectious/ clinical, blood, neuroimaging, and CSF findings for postinfectious inflammatory changes during coronavirus 3 patients with laboratory-confirmed COVID-19 and disease with neurologic complications. -

TDP-43 Proteinopathy and Motor Neuron Disease in Chronic Traumatic Encephalopathy
J Neuropathol Exp Neurol Vol. 69, No. 9 Copyright Ó 2010 by the American Association of Neuropathologists, Inc. September 2010 pp. 918Y929 ORIGINAL ARTICLE TDP-43 Proteinopathy and Motor Neuron Disease in Chronic Traumatic Encephalopathy Ann C. McKee, MD, Brandon E. Gavett, PhD, Robert A. Stern, PhD, Christopher J. Nowinski, AB, Robert C. Cantu, MD, Neil W. Kowall, MD, Daniel P. Perl, MD, E. Tessa Hedley-Whyte, MD, Bruce Price, MD, Chris Sullivan, Peter Morin, MD, PhD, Hyo-Soon Lee, MD, Caroline A. Kubilus, Daniel H. Daneshvar, MA, Megan Wulff, MPH, and Andrew E. Budson, MD cord in addition to tau neurofibrillary changes, motor neuron loss, Abstract and corticospinal tract degeneration. The TDP-43 proteinopathy Epidemiological evidence suggests that the incidence of amyo- associated with CTE is similar to that found in frontotemporal lobar trophic lateral sclerosis is increased in association with head injury. degeneration with TDP-43 inclusions, in that widespread regions of Repetitive head injury is also associated with the development of the brain are affected. Akin to frontotemporal lobar degeneration chronic traumatic encephalopathy (CTE), a tauopathy characterized with TDP-43 inclusions, in some individuals with CTE, the TDP-43 by neurofibrillary tangles throughout the brain in the relative absence proteinopathy extends to involve the spinal cord and is associated of A-amyloid deposits. We examined 12 cases of CTE and, in 10, with motor neuron disease. This is the first pathological evidence that found a widespread TAR DNA-binding protein of approximately repetitive head trauma experienced in collision sports might be 43 kd (TDP-43) proteinopathy affecting the frontal and temporal associated with the development of a motor neuron disease. -

Encephalopathy
Jounal ofNeurology, Neurosurgery, and Psychiatry 1997;62:51-60 51 Operational criteria for the classification of chronic alcoholics: identification of Wemicke's encephalopathy D Caine, G M Halliday, J J Kril, C G Harper Abstract suggest that there can be a complete resolution Objectives-To establish better opera- of the underlying brain abnormality in tional criteria for the diagnosis of Wernicke's encephalopathy, similar to the res- Wernicke's encephalopathy. Current olution of neuropathology in hepatic criteria for diagnosing Wernicke's encephalopathy. However, unlike hepatic encephalopathy require the presence of encephalopathy, in which the clinical signs are three clinical signs (oculomotor abnor- a precursor of the pathology, many patients malities, cerebellar dysfunction, and an with the neuropathology of Wernicke's altered mental state), although it has encephalopathy do not have recorded signs of often been reported that most patients do the classic triad.' 2 This raises the question of not filfil all these criteria. whether the clinical correlates of the patholog- Methods-The clinical histories of 28 ical lesions are being missed during life or alcoholics with neurological and neu- whether the pathology represents clinically ropsychological assessments and defini- silent lesions. A similar situation is seen in tive neuropathological diagnoses were Alzheimer's disease, in which many non- examined to determine clinical signs for demented aged patients show a similar type use in a screening schedule. Operational and distribution of neuropathology to their criteria were then proposed for differenti- demented counterparts. 12 Recently research ating patients with Wernicke's into the pathophysiology of aging and encephalopathy alone or in combination Alzheimer's disease has been successfully with Korsakoff's psychosis or hepatic advanced by the use of operational criteria encephalopathy. -

Seizures in Encephalitis
Neurology Asia 2008; 13 : 1 – 13 REVIEW ARTICLES Seizures in encephalitis Usha Kant Misra DM, *C T Tan MD, Jayantee Kalita DM Department of Neurology, Sanjay Gandhi PGIMS, Lucknow, India; *Department of Medicine, University of Malaya, Kuala Lumpur, Malaysia Abstract A large number of viruses can result in encephalitis. However, certain viruses are more prevalent in certain geographical regions. For example, Japanese encephalitis (JE) and dengue in South East Asia and West Nile in Middle East whereas Herpes simplex encephalitis (HSE) occurs all over the world without any seasonal or regional variation. Encephalitis can result in acute symptomatic seizures and remote symptomatic epilepsy. Risk of seizures after 20 years is 22% following encephalitis and 3% after meningitis with early seizures. Amongst the viruses, HSE is associated with most frequent and severe epilepsy. Seizures may be presenting feature in 50% because of involvement of highly epileptogenic frontotemporal cortex. Presence of seizures in HSE is associated with poor prognosis. HSE can also result in chronic and relapsing form of encephalitis and may be an aetiology factor in drug resistant epilepsy. Amongst the Flaviviruses, Japanese encephalitis is the most common and is associated with seizures especially in children. The frequency of seizures in JE is reported to be 6.9% to 46%. Associated neurocysticercosis in JE patients may aggravate the frequency and severity of seizures. Other flaviviruses such as equine, St Louis, and West Nile encephalitis can also produce seizures. In Nipah encephalitis, seizures are commoner in relapsed and late-onset encephalitis as compared to acute encephalitis (50% vs 24%). Other viruses like measles, varicella, mumps, influenza and enteroviruses may result in encephalitis and seizures. -

Progressive Multifocal Leukoencephalopathy and the Spectrum of JC Virus-Related Disease
REVIEWS Progressive multifocal leukoencephalopathy and the spectrum of JC virus- related disease Irene Cortese 1 ✉ , Daniel S. Reich 2 and Avindra Nath3 Abstract | Progressive multifocal leukoencephalopathy (PML) is a devastating CNS infection caused by JC virus (JCV), a polyomavirus that commonly establishes persistent, asymptomatic infection in the general population. Emerging evidence that PML can be ameliorated with novel immunotherapeutic approaches calls for reassessment of PML pathophysiology and clinical course. PML results from JCV reactivation in the setting of impaired cellular immunity, and no antiviral therapies are available, so survival depends on reversal of the underlying immunosuppression. Antiretroviral therapies greatly reduce the risk of HIV-related PML, but many modern treatments for cancers, organ transplantation and chronic inflammatory disease cause immunosuppression that can be difficult to reverse. These treatments — most notably natalizumab for multiple sclerosis — have led to a surge of iatrogenic PML. The spectrum of presentations of JCV- related disease has evolved over time and may challenge current diagnostic criteria. Immunotherapeutic interventions, such as use of checkpoint inhibitors and adoptive T cell transfer, have shown promise but caution is needed in the management of immune reconstitution inflammatory syndrome, an exuberant immune response that can contribute to morbidity and death. Many people who survive PML are left with neurological sequelae and some with persistent, low-level viral replication in the CNS. As the number of people who survive PML increases, this lack of viral clearance could create challenges in the subsequent management of some underlying diseases. Progressive multifocal leukoencephalopathy (PML) is for multiple sclerosis. Taken together, HIV, lymphopro- a rare, debilitating and often fatal disease of the CNS liferative disease and multiple sclerosis account for the caused by JC virus (JCV). -

Encephalitis Fact Sheet
Encephalitis Fact Sheet What is encephalitis? Encephalitis is an inflammation (irritation and swelling) of the brain tissue. It can occur as a primary illness or as a result of another illness elsewhere in the body. Frequently caused by an infection with a virus, encephalitis can be mild or severe, but severe cases are rare. Who gets encephalitis? Anyone can get encephalitis, but young children, older adults, and persons with weakened immune systems are more at risk. How is encephalitis spread? Primary encephalitis occurs when a virus directly infects the brain. Viruses that are carried by infected mosquitoes and ticks can cause primary encephalitis. Other viruses can cause an illness and then encephalitis can develop as a complication of the viral illness. When encephalitis develops after another infection, it is called post-infectious encephalitis. Post-infectious encephalitis most commonly follows a bout of chickenpox, mumps, or measles. What are the symptoms of encephalitis? Encephalitis frequently causes headache, fever, confused thinking, seizures, or problems with vision, speech, or movement. Infants and young children might have nausea, vomiting, body stiffness, constant crying, and poor feeding. How soon after exposure do symptoms appear? Encephalitis can occur within two to three weeks after a viral illness. Symptoms begin within a few days to one or two weeks after the bite from an infected mosquito. How is encephalitis diagnosed? Medical evaluation and special tests are needed to confirm the diagnosis. Anyone with a severe headache, fever, and altered mental status should seek medical care immediately. What is the treatment for encephalitis? Doctors might prescribe antiviral drugs, anti-inflammatory drugs, or other treatments for the symptoms as needed. -
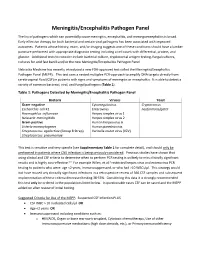
Meningitis/Encephalitis Pathogen Panel
Meningitis/Encephalitis Pathogen Panel The list of pathogens which can potentially cause meningitis, encephalitis, and meningoencephalitis is broad. Early effective therapy for both bacterial and certain viral pathogens has been associated with improved outcomes. Patients whose history, exam, and/or imaging suggests one of these conditions should have a lumber puncture performed with appropriate diagnostic testing including a cell count with differential, protein, and glucose. Additional tests to consider include bacterial culture, cryptococcal antigen testing, fungal cultures, cultures for acid fast bacilli and/or the new Meningitis/Encephalitis Pathogen Panel. Nebraska Medicine has recently introduced a new FDA-approved test called the Meningitis/Encephalitis Pathogen Panel (MEPP). This test uses a nested multiplex PCR-approach to amplify DNA targets directly from cerebrospinal fluid (CSF) in patients with signs and symptoms of meningitis or encephalitis. It is able to detect a variety of common bacterial, viral, and fungal pathogens (Table 1). Table 1: Pathogens Detected by Meningitis/Encephalitis Pathogen Panel Bacteria Viruses Yeast Gram-negative Cytomegalovirus Cryptococcus Escherichia coli K1 Enterovirus neoformans/gattii Haemophilus influenzae Herpes simplex virus 1 Neisseria meningitidis Herpes simplex virus 2 Gram-positive Human herpesvirus 6 Listeria monocytogenes Human parechovirus Streptococcus agalactiae (Group B Strep) Varicella zoster virus (VZV) Streptococcus pneumoniae This test is sensitive and very specific (see Supplementary Table 1 for complete detail), and should only be performed in patients where CNS infection is being seriously considered. Previous studies have shown that using clinical and CSF criteria to determine when to perform PCR testing is unlikely to miss clinically significant results and is highly cost-effective.1-3 For example Wilen, et al.3 restricted herpes virus and enterovirus PCR testing to patients who were: age <2 years, immunosuppressed, or who had >10 WBCs/µl. -

Pharmacologic Treatment of Meningitis and Encephalitis in Adult Patients
Published online: 2019-06-19 THIEME Review Article 145 Pharmacologic Treatment of Meningitis and Encephalitis in Adult Patients Andrew K. Treister1 Ines P. Koerner2 1Department of Neurology, Oregon Health & Science University, Address for correspondence Andrew K. Treister, MD, Department Portland, Oregon, United States of Neurology, Oregon Health & Science University, 3181 SW Sam 2Department of Anesthesiology and Perioperative Medicine, Jackson Park, CR 120, Portland, OR 97239-3098, United States Oregon Health & Science University, Portland, Oregon, (e-mail: [email protected]). United States J Neuroanaesthesiol Crit Care 2019;6:145–152 Abstract Meningitis and encephalitis are two inflammatory, often infectious, disorders of the meninges and the central nervous system. Both are associated with significant morbidity and mortality, and require early and aggressive targeted treatment. This article reviews pharmacologic treatment strategies for infectious meningitis and encephalitis, using Keywords the latest available research and guidelines. It provides an overview of empiric anti- ► meningitis microbial treatment approaches for a variety of organisms, including a discussion of ► encephalitis trends in antibiotic resistance where applicable. Key steps in diagnosis and general ► antibiotic resistance management are briefly reviewed. Introduction care–associated infections are not covered in detail, as they are excellently discussed in a recent guideline statement.4 The terms meningitis and encephalitis comprise a broad array of infectious and inflammatory processes involving the central nervous system (CNS) that carry significant morbidity Literature Review 1,2 and mortality. Meningitis refers to inflammation of PubMed was searched in January 2019 for articles published primarily the meninges, although it may spread to involve the between January 1, 2009, and December 31, 2018. -

Idiopathic Intracranial Hypertension
IDIOPATHIC INTRACRANIAL HYPERTENSION William L Hills, MD Neuro-ophthalmology Oregon Neurology Associates Affiliated Assistant Professor Ophthalmology and Neurology Casey Eye Institute, OHSU No disclosures CASE - 19 YO WOMAN WITH HEADACHES X 3 MONTHS Headaches frontal PMHx: obesity Worse lying down Meds: takes ibuprofen for headaches Wake from sleep Pulsatile tinnitus x 1 month. Vision blacks out transiently when she bends over or sits down EXAMINATION Vision: 20/20 R eye, 20/25 L eye. Neuro: PERRL, no APD, EOMI, VF full to confrontation. Dilated fundoscopic exam: 360 degree blurring of disc margins in both eyes, absent SVP. Formal visual field testing: Enlargement of the blind spot, generalized constriction both eyes. MRI brain: Lumbar puncture: Posterior flattening of Opening pressure 39 the globes cm H20 Empty sella Normal CSF studies otherwise normal Headache improved after LP IDIOPATHIC INTRACRANIAL HYPERTENSION SYNDROME: Increased intracranial pressure without ventriculomegaly or mass lesion Normal CSF composition NOMENCLATURE Idiopathic intracranial hypertension (IIH) Benign intracranial hypertension Pseudotumor cerebri Intracranial hypertension secondary to… DIAGNOSTIC CRITERIA Original criteria have been updated to reflect new imaging modalities: 1492 Friedman and Jacobsen. Neurology 2002; 59: Symptoms and signs reflect only those of - increased ICP or papilledema 1495 Documented increased ICP during LP in lateral decubitus position Normal CSF composition No evidence of mass, hydrocephalus, structural -
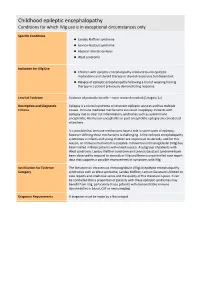
Childhood Epileptic Encephalopathy Conditions for Which Ivig Use Is in Exceptional Circumstances Only
Childhood epileptic encephalopathy Conditions for which IVIg use is in exceptional circumstances only Specific Conditions Landau Kleffner syndrome Lennox‐Gastaut syndrome Atypical rolandic epilepsy West syndrome Indication for IVIg Use Children with epileptic encephalopathy resistant to anti‐epileptic medications and steroid therapy or steroid responsive but dependant Relapse of epileptic encephalopathy following a trial of weaning from Ig therapy in a patient previously demonstrating response Level of Evidence Evidence of probable benefit – more research needed (Category 2a) Description and Diagnostic Epilepsy is a clinical syndrome of recurrent epileptic seizures and has multiple Criteria causes. Immune mediated mechanisms can result in epilepsy. Patients with epilepsy due to clear cut inflammatory syndromes such as autoimmune encephalitis, Rasmussen encephalitis or post encephalitic epilepsy are considered elsewhere. It is possible that immune mechanisms have a role in some cases of epilepsy, however defining these mechanisms is challenging. A few epileptic encephalopathy syndromes in infants and young children are responsive to steroids, and for this reason, an immune mechanism is possible. Intravenous immunoglobulin (IVIg) has been trialled in these patients with mixed success. A subgroup of patients with West syndrome, Landau Kleffner syndrome and Lennox Gaustaut syndrome have been observed to respond to steroids or IVIg and there is uncontrolled case report data that supports a possible improvement of symptoms with IVIg. Justification for Evidence The literature on intravenous immunoglobulin (IVIg) in epileptic encephalopathy Category syndromes such as West syndrome, Landau Kleffner, Lennox Gaustaut is limited to case reports and small case series and the quality of this literature is poor. It can be concluded that a proportion of patients with these epileptic syndromes may benefit from IVIg, particularly those patients with demonstrable immune abnormalities in blood, CSF or neuroimaging.