Orthopaedics Summary Dec 2014
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Role of Ct in Assessment of Blunt Chest Trauma
Al-Azhar Med. J. Vol. 49(4), October, 2020,2083- 2092 DOI : 10.12816/amj.2020.120663 https://amj.journals.ekb.eg/article_120663.html ROLE OF CT IN ASSESSMENT OF BLUNT CHEST TRAUMA By Ahmed Abouzeid Metwally Mohamed Galal, Abd El-Nabi Bayoumi Mohamed and Ahmed Mohamed Abd El-Ghaffar Zidan Department of Radio diagnosis, Faculty of Medicine, Al-Azhar University Corresponding author: Ahmed Abouzeid Metwally Mohamed Galal, Mobile: (+20) 01017106789, E-mail: [email protected] ABSTRACT Background: Blunt chest trauma is a significant problem affecting mainly young males between 20-40 years and it is usually caused by motor vehicle accidents. It is common and contributes significantly to morbidity and mortality of trauma patients. It has an overall fatality rate of 15-25%. Objective: To evaluate the role of multi-detector computed tomography in assessment of patients with blunt chest trauma. Patients and Methods: This study involved 50 patients; 40 males (70%) and 10 females (30%). Their ages range was 2-75 years (mean age= 51.4 years). They were exposed to blunt chest trauma and referred to the Emergency Radiology Department in Nasr City Hospital and Al-Azhar University Hospitals for multi detector computed tomography (MDCT) of the chest over a period of 6 months starting from November 2019 to April 2020. Results: Multi-planner and 3D reconstruction images were sensitive in the evaluation of different skeletal injuries especially dorsal spine, scapular and sternal fractures. Its high resolution provides more sensitivity in the evaluation of lung contusion that helped in predicting the need for mechanical ventilation. MDCT was more accurate and sensitive in the diagnosis and characterization of different types of pleural and mediastinal injuries. -

Scapulothoracic Dissociation:A Rare Variant: a Case Report
Malaysia Orthopaedic Journal 2014 Vol 8 No 2 Rajat Jangir, et al http://dx.doi.org/10.5704/MOJ.1407.003 Scapulothoracic Dissociation: A Rare Variant: A Case Report Rajat Jangir, MS Orth, Diwakar Misra, DNB Orth Department of Orthopaedics, Rnt Medical College, Udaipur, Rajasthan, India Department of Orthopaedics, Maulana Ajad Medical College, New Delhi, India This article is distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/3.0/), which permits unrestricted use and redistribution provided that the original author and source are credited. ABSTRACT There was massive swelling over the right shoulder with Scapulothoracic dissociation is a rare injury involving abrasions over the scapular region. Distal pulses were palpable. separation of scapula from the thorax along with the upper There was no neurological deficit. The patient was resuscitated extremity. Majority of the patients have concomitant with the ATLS (Advanced Trauma life Support) protocol. neurovascular injury and the prognosis is uniformly poor in such cases. We present a case of scapulothoracic Chest radiograph revealed multiple rib fractures and dissociation with comminuted fracture of scapula and hemothorax. Right shoulder radiograph revealed acromioclavicular joint disruption without neurovascular acromioclavicular disruption, fracture of scapula and deficit. There were associated avulsion fractures of the lateral translation of scapula. Intercostal drainage tubes spinous processes of vertebrae (T3-T5). Such presentation were inserted for hemothorax. The right upper limb was is rare in an already rare scapulothoracic dissociation strapped to the body. The electrocardiograph was suggestive injury. A discussion regarding the probable mechanism of of myocardial ischemia for which echocardiography injury, management and prognosis is presented. -

Clinical Excellence Series Volume V an Evidence-Based Approach to Traumatic Emergencies
Clinical Excellence Series n Volume V An Evidence-Based Approach To Traumatic Emergencies Inside Neck Trauma: Don’t Put Your Neck On The Line Orthopedic Sports Injuries: Off The Sidelines And Into The Emergency Department Blunt Abdominal Trauma: Priorities, Procedures, And Pragmatic Thinking Wrist Injuries: Emergency Imaging And Management Brought to you exclusively by the publisher of: An Evidence-Based Approach To Traumatic Emergencies CEO: Robert Williford President & Publisher: Stephanie Ivy Associate Editor & CME Director: Jennifer Pai • Associate Editor: Dorothy Whisenhunt Director of Member Services: Liz Alvarez • Marketing & Customer Service Coordinator: Robin Williford Direct all questions to EB Medicine: 1-800-249-5770 • Fax: 1-770-500-1316 • Non-U.S. subscribers, call: 1-678-366-7933 EB Medicine • 5550 Triangle Pkwy Ste 150 • Norcross, GA 30092 E-mail: [email protected] • Web Site: www.ebmedicine.net The Emergency Medicine Practice Clinical Excellence Series, Volume V: An Evidence-Based Approach To Traumatic Emergencies is published by EB Practice, LLC, 5550 Triangle Pkwy Ste 150, Norcross, GA 30092. Opinions expressed are not necessarily those of this publication. Mention of products or services does not constitute endorsement. This publication is intended as a general guide and is intended to supplement, rather than substitute, professional judgment. It covers a highly technical and complex subject and should not be used for making specific medical decisions. The materials contained herein are not intended to establish policy, procedure, or standard of care. Emergency Medicine Practice, The Emergency Medicine Practice Clinical Excel- lence Series, and An Evidence-Based Approach to Traumatic Emergencies are trademarks of EB Practice, LLC. -

Spontaneous Fracture of the Scapula Spines in Association with Severe Rotator Cuff Disease and Osteoporosis
Central Annals of Musculoskeletal Disorders Case Report *Corresponding author Hans Van der Wall, CNI Molecular Imaging & University of Notre Dame, Sydney, Australia, Tel: +61 2 9736 1040; Spontaneous Fracture of the FAX: +61 2 9736 2095; Email: [email protected] Submitted: 25 March 2020 Scapula Spines in Association Accepted: 07 April 2020 Published: 10 April 2020 ISSN: 2578-3599 with Severe Rotator Cuff Copyright © 2020 Robert B, et al. Disease and Osteoporosis OPEN ACCESS 1 2 3 Breit Robert , Strokon Andrew , Burton Leticia , Van der Wall Keywords H3* and Bruce Warwick3 • Scapular fracture • Rotator cuff arthropathy 1CNI Molecular Imaging, Australia • Osteoporosis 2Sydney Private Hospital, Australia • Scintigraphy 3CNI Molecular Imaging & University of Notre Dame, Sydney, Australia • SPECT/ CT 4Concord Hospital, Australia Abstract We present the case of a 74 year-old woman with diabetes mellitus and established osteoporosis who initially presented with increasing pain and disability of the shoulders. Investigations showed severe rotator cuff disease. This was treated conservatively with physiotherapy and corticosteroid injection into both joints with good pain relief but no improvement in function. She subsequently presented with increasing posterior thoracic pain with plain films reporting no evidence of rib fracture. Bone scintigraphy showed severe rotator cuff disease and degenerative joint disease at multiple sites. The single photon emission computed tomography (SPECT)/ x-ray Computed Tomography (CT) showed bilateral scapula spine fractures of long standing with a probable non-union on the left side. These fractures are rare and difficult to treat when associated with rotator cuff disease. INTRODUCTION Fractures of the scapula spine are rare, with a reported level of dysfunction remained significant with marked restriction frequency of less than twenty cases in the literature [1-8]. -

Knee Injuries
6/11/2019 Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 8e Chapter 274: Knee Injuries Rachel R. Bengtzen; Jerey N. Glaspy; Mark T. Steele ANATOMY The knee consists of two joints, the tibiofemoral joint and the patellofemoral joint. Within the tibiofemoral joint, the distal femur (comprised of the medial and lateral femoral condyles) articulates with the proximal tibia (comprised of the medial and lateral tibial condyles) (Figure 274-1). The medial and lateral menisci are situated between the articular surfaces, and the menisci provide cushion, lubrication, and resistance to articular wear (Figure 274-2). In the patellofemoral joint, the patella articulates with the distal femur along the anterior depression called the patellofemoral groove during flexion and extension of the knee. The patella is stabilized by the patellar tendon and medial retinaculum. FIGURE 274-1. The supracondylar and condylar areas of the femur, and the medial and subcondylar areas of the tibia. 1/29 6/11/2019 FIGURE 274-2. Ligaments of the right knee joint. The articular capsule and the patella have been removed. 2/29 6/11/2019 There are four ligaments in the knee: the anterior cruciate ligament, the posterior cruciate ligament, and the medial and lateral collateral ligaments (Figure 274-2). These ligaments provide strength and stability to the knee. The posterior aspect of the knee, the popliteal fossa, contains the popliteal artery and vein, the common peroneal nerve, and the tibial nerve (Figure 274-3). FIGURE 274-3. Posterior knee: popliteal fossa anatomy. 3/29 6/11/2019 CLINICAL FEATURES Determine the mechanism of knee injury and review all prior orthopedic injuries or surgical procedures. -

Review Article Fractures of the Scapula
Hindawi Publishing Corporation Advances in Orthopedics Volume 2012, Article ID 903850, 7 pages doi:10.1155/2012/903850 Review Article Fractures of the Scapula Pramod B. Voleti,1 Surena Namdari,2 and Samir Mehta1 1 Department of Orthopaedic Surgery, Hospital of the University of Pennsylvania, 3400 Spruce Street, 2 Silverstein, Philadelphia, PA 19104, USA 2 Department of Orthopaedic Surgery, Washington University in St. Louis, 660 South Euclid Avenue, Campus Box 8233, St. Louis, MO 63110, USA Correspondence should be addressed to Samir Mehta, [email protected] Received 11 August 2012; Accepted 7 October 2012 Academic Editor: Reuben Gobezie Copyright © 2012 Pramod B. Voleti et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. The scapula plays a critical role in the association between the upper extremity and the axial skeleton. Fractures of the scapula account for 0.4% to 1% of all fractures and have an annual incidence of approximately 10 per 100,000 inhabitants. Scapular fractures typically result from a high-energy blunt-force mechanism and are often associated with other traumatic injuries. The present review focuses on the presentation, diagnosis, and treatment of fractures of the scapula. Indications for surgical treatment of glenoid fossa, scapular neck, and scapular body fractures are presented in detail. Finally, the authors’ preferred surgical technique, including positioning, approach, reduction, fixation, and post-operative management, is described. 1. Introduction cause fractures in all regions of the scapula, while indirect force via impaction of the humeral head into the glenoid The scapula plays an integral role in the association between fossa can cause both glenoid and scapular neck fractures. -

Clinical Outcomes and Shoulder Kinematics for the Gray Zone Extra-Articular Scapula Fracture in 5 Patients
Somato Publications ISSN: 2643-2692 International Journal of Orthopedics Research Article Clinical Outcomes and Shoulder Kinematics for the “Gray Zone” Extra-articular Scapula Fracture in 5 Patients Jyoti Sharma1, Candice Maenza2, Andrea Myers3, Erik B. Lehman4, Andrew R Karduna5, Robert L Sainburg2 and April D Armstrong3* 1Department of Orthopaedics, Geisinger Health System/Holy Spirit, Camp Hill, PA, USA 2Department of Neurology, Penn State Health Hershey and Penn State College of Health and Human Development, Hershey, PA, USA 3Department of Orthopaedics and Rehabilitation, Penn State Health Hershey and Penn State College of Medicine, Hershey, PA, USA 4Department of Public Health Sciences, Penn State College of Medicine, Hershey, PA, USA 5Department of Human Physiology, University of Oregon, Eugene, OR, USA *Address for Correspondence: April Armstrong, Department of Orthopaedics and Rehabilitation, Penn State Health Hershey and Penn State College of Medicine, Hershey, PA, USA, E-mail: [email protected] Received: 28 November 2019; Accepted: 06 February 2020; Published: 07 February 2020 Citation of this article: Sharma, J., Maenza, C., Myers, A., B.Lehman, E., Karduna, AR., Sainburg, Rl., Armstrong, AD. (2020) Clinical Outcomes and Shoulder Kinematics for the “Gray Zone” Extra-articular Scapula Fracture in 5 Patients. Int J Orth, 3(1): 01-11. Copyright: © 2020 Armstrong, AD, et al. This is an open access articwle distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Abstract Aims: There is a subset of scapula fractures, which can be considered in the “gray zone,” where treatment guidelines are not clear-cut, based on published Methodsliterature. -

Fracture of the Scapula with Intrathoracic Penetration in a Skeletally Mature Patient
Wright State University CORE Scholar Department of Surgery Faculty Publications Surgery 12-2006 Fracture of the Scapula with Intrathoracic Penetration in a Skeletally Mature Patient Cary C. Schwartzbach Hani Seoudi Amy E. Ross Kimberly M. Hendershot Wright State University, [email protected] Linda Robinson See next page for additional authors Follow this and additional works at: https://corescholar.libraries.wright.edu/surg Part of the Surgery Commons Repository Citation Schwartzbach, C. C., Seoudi, H., Ross, A. E., Hendershot, K. M., Robinson, L., & Maekzadeh, A. (2006). Fracture of the Scapula with Intrathoracic Penetration in a Skeletally Mature Patient. The Journal of Bone and Joint Surgery, 88 (12), 2735-2738. https://corescholar.libraries.wright.edu/surg/198 This Report is brought to you for free and open access by the Surgery at CORE Scholar. It has been accepted for inclusion in Department of Surgery Faculty Publications by an authorized administrator of CORE Scholar. For more information, please contact [email protected]. Authors Cary C. Schwartzbach, Hani Seoudi, Amy E. Ross, Kimberly M. Hendershot, Linda Robinson, and Alireza Maekzadeh This report is available at CORE Scholar: https://corescholar.libraries.wright.edu/surg/198 Schwartzbach.fm Page 2735 Monday, November 6, 2006 2:27 PM 2735 COPYRIGHT © 2006 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Fracture of the Scapula with Intrathoracic Penetration in a Skeletally Mature Patient A CASE REPORT BY CARY C. SCHWARTZBACH, MD, HANI SEOUDI, MD, AMY E. ROSS, MD, KIMBERLY HENDERSHOT, MD, LINDA ROBINSON, MA, MS, AND ALIREZA MALEKZADEH, MD Investigation performed at Inova Fairfax Hospital, Falls Church, Virginia o our knowledge, intrathoracic displacement of a frac- late reconstruction should nonoperative management fail. -

AN ISOLATED NON-TRAUMATIC FIRST RIB FRACTURE in a COLLEGIATE BASEBALL PLAYER Hummel, CH: Ithaca College, Ithaca, NY
AN ISOLATED NON-TRAUMATIC FIRST RIB FRACTURE IN A COLLEGIATE BASEBALL PLAYER Hummel, CH: Ithaca College, Ithaca, NY The objective of this case presentation is to present the unique case of an isolated non- traumatic first rib fracture in a non-pitching baseball player. A 19-year-old male Division III 2nd baseman initially presented with point tenderness at the right pectoralis major insertion at the mid-sternum level following a clean during a team lifting session. On further examination, the athlete was found to have full strength and range of motion. The initial treatment consisted of ice for pain. Prior to each subsequent practice, treatment consisted of heat and pre-modulated electrical stimulation followed by a stretch to the chest and shoulder musculature. The athlete had no limitation or significant complaints until day 24, when he complained of right axilla soreness. Approximately twenty minutes into practice that day, he felt a sharp pain in the axillary region following a single throw (approximately the 30th throw of the day) during the team’s warm-up throwing drills. On physical examination, the athlete complained of extreme pain in the right axillary region, which increased with all head and neck movements and while taking deep breaths. He denied any weakness, numbness or tingling in either extremity. Compression of the scapula and clavicle significantly increased his pain. He was immediately referred to the team physician for evaluation. Differential diagnosis included glenohumeral dislocation, rotator cuff tear, clavicular fracture, pectoralis major tear, humeral fracture, and scapular fracture. An x-ray revealed a fracture to the right first rib. -
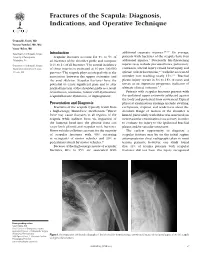
Fractures of the Scapula: Diagnosis, Indications, and Operative Technique
Fractures of the Scapula: Diagnosis, Indications, and Operative Technique 1Pramod B. Voleti, MD 2Surena Namdari, MD, MSc 1Samir Mehta, MD 2-5,9,10 1Department of Orthopaedic Surgery, Introduction additional traumatic injuries. On average, University of Pennsylvania, Scapular fractures account for 3% to 5% of patients with fractures of the scapula have four Philadelphia, PA all fractures of the shoulder girdle and compose additional injuries.6 Potentially life-threatening 1 2Department of Orthopaedic Surgery, 0.4% to 1% of all fractures. The annual incidence injuries may include pneumothorax, pulmonary Washington University in St. Louis, of these injuries is estimated at 10 per 100,000 contusion, arterial injury, closed head injury, and St. Louis, MO persons.2 The scapula plays an integral role in the splenic or liver lacerations,5,6 with the associated association between the upper extremity and mortality rate reaching nearly 15%.3,6 Brachial the axial skeleton. Scapular fractures have the plexus injury occurs in 5% to 13% of cases and potential to cause significant pain and to alter serves as an important prognostic indicator of normal function of the shoulder girdle as a result ultimate clinical outcome.3-5 of malunion, nonunion, rotator cuff dysfunction, Patients with scapular fractures present with scapulothoracic dyskinesis, or impingement. the ipsilateral upper extremity adducted against the body and protected from movement. Typical Presentation and Diagnosis physical examination findings include swelling, Fractures of the scapula typically result from ecchymosis, crepitus, and tenderness about the a high-energy, blunt-force mechanism.3-7Direct shoulder. Range of motion of the shoulder is force may cause fractures in all regions of the limited, particularly with abduction. -

Imaging Review: Modalities and Practice Guidelines Bryan M
Imaging Review: Modalities and Practice Guidelines Bryan M. Bond, BSc, BS, DC, MS, PhD April 7th, 2017 Wichita, Kansas 1 Objectives……. 1. Recognize how the study of human imaging can make the clinician’s evaluation and management of the patient more comprehensive. 2. Discuss and describe the clinical impact of imaging technologies used in musculoskeletal conditions. 3. Describe, compare and contrast the major roles of conventional radiography, magnetic resonance imaging, computed tomography, ultrasound, and bone scintigraphy in clinical decision making. 2 Objectives……. 4. Acquire an ability to transform visually three-dimensional anatomy into two-dimensional radiographic anatomy to enable identification of normal and abnormal anatomical structures on radiographs. 5. Describe and discuss the evidence-informed clinical practice guidelines to promote appropriate imaging or treatment decisions. 3 Goals……… • NOT to teach you A through Z, but….. – Review some information – Add some new knowledge – Stimulate further thinking……………… 4 General Outline • Integration of Imaging into • Diagnostic Imaging Clinical PT Practice Prediction Rules (CPRs) • Special Imaging Techniques • Case-Based Learning • General Principles and Evaluation • Summary of Tissue 5 Integration of Imaging into Physical Therapy Practice 6 Changing Perspectives on Diagnostic Imaging in PT Education 7 The Traditional Model • PT gradually evolved into profession with specialized areas of practice, including primary care, requiring considerable expertise in MSK evaluation – In response, -

Research Article
s z Available online at http://www.journalcra.com INTERNATIONAL JOURNAL OF CURRENT RESEARCH International Journal of Current Research Vol. 12, Issue, 04, pp.10978-10980, April, 2020 DOI: https://doi.org/10.24941/ijcr.38352.04.2020 ISSN: 0975-833X RESEARCH ARTICLE SCAPULA FRACTURES A TWENTY FIVE YEAR EXPERIENCE Efstathios K. Metaxas1,*, Konstantinos Tzelepis2, Ioannis Stamatatos3, Stavroula Amanetopoulou4, Dimitrios Tsiftsis4, Aristotelis K. Stefoudis5, Damon Charalampides5, Dimitrios Klapsakis5, Dimitrios Paschalinos6, Symeon Patsos6, Lazaros Tsiatsios6, Fragkiskos Tzagkarakis6 and Dionysios Louverdis5 1Department of Thoracic Surgery, General Hospital of Nicaea-Piraeus, Greece 2Department of Urology, General Hospital of Nicaea-Piraeus, Greece 3Department of Vascular Surgery, General Hospital of Nicaea-Piraeus, Greece 4Department of Emergency, General Hospital of Nicaea-Piraeus, Greece 5Department of Ortopaedic Surgery, General Hospital of Nicaea-Piraeus, Greece 6Department of General Surgery, General Hospital of Nicaea-Piraeus, Greece ARTICLE INFO ABSTRACT Article History: Background: To determine the importance of the scapula bone fractures upon the causes, sex, age Received 24th January, 2020 groups, associated injuries, morbidity and mortality. Methods: In a 25 year period a retrospective Received in revised form study took place. One hundred and eight (108) patients diagnosed with scapula fracture in General 15th February, 2020 Hospital of Nicaea-Piraeus Agios Panteleimon Thoracic and Orthopaedic Surgery Department. Accepted 08th March, 2020 Results: Between the years 1995 to 2020(25years) 108 patients diagnosed with scapula bone fracture, th Published online 30 April, 2020 81 male (75%) and 27 female (25 %), aged 19-91 years mean age 34 years. Aetiologic factor: Traffic accident 81 (75%), fall from high 24 (22,22 %) and Gunshot injuries 3( 2,777%) patients.