Transcriptome Remodeling in Gradual Development of Inverse Resistance Between Paclitaxel and Cisplatin in Ovarian Cancer Cells
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

University of Wolverhampton
Course Specification Published Date: 14-Sep-2020 Produced By: Laura Clode Status: Validated Core Information Awarding Body / Institution: University of Wolverhampton School / Institute: Wolverhampton School of Sciences Course Code(s): BM021K23UV Sandwich 4 Years UCAS Code: B991 Course Title: BSc (Hons) Biomedical Science with Sandwich Placement Hierarchy of Awards: Bachelor of Science with Honours Biomedical Science, having satisfactorily completed a sandwich placement Bachelor of Science with Honours Biomedical Science, having satisfactorily completed a sandwich placement Bachelor of Science Medical Laboratory Science, having satisfactorily completed a sandwich placement Bachelor of Science Biomedical Science, having satisfactorily completed a sandwich placement Diploma of Higher Education Medical Laboratory Science Certificate of Higher Education Medical Laboratory Science University Statement of Credit University Statement of Credit Language of Study: English Date of DAG approval: 05/Jun/2018 Last Review: 2017/8 Course Specification valid from: 2010/1 Course Specification valid to: 2023/4 Academic Staff Course Leader: Dr Elizabeth O'Gara Head of Department: Dr Elizabeth O'Gara Course Information Location of Delivery: University of Wolverhampton Category of Partnership: Not delivered in partnership Teaching Institution: University of Wolverhampton Open / Closed Course: This course is open to all suitably qualified candidates. Entry Requirements: Entry requirements are subject to regular review. The entry requirements applicable to a particular academic year will be published on the University website (and externally as appropriate e.g. UCAS 240 UCAS points including a science subject at A-level or equivalent. GCSE English and Maths at grade C or above. Distinctive Features of the Course: This course involves the study of a variety of biomedical science disciplines and takes place at an institution where fellow students are undertaking programmes in other disciplines and vocational courses in a wide variety of medicine-related subjects. -

Molecular Diagnostic Testing for Hematology and Oncology Indications Table of Contents Related Coverage Resources
Effective February 15, 2021 Medical Coverage Policy Effective Date.............................................. 2/15/2021 Next Review Date ..................................... 11/15/2021 Coverage Policy Number ................................... 0520 Molecular Diagnostic Testing for Hematology and Oncology Indications Table of Contents Related Coverage Resources Overview ....................................................................... 2 Genetics Coverage Policy ........................................................... 2 Genetic Testing Collateral File General Criteria for Somatic Pathogenic or Likely Pathogenic Variant Genetic Testing ........................... 2 Tumor Profile/Gene Expression Classifier Testing - ...................................................................... 3 Prostate Cancer Screening and Prognostic Tests ..... 6 Tumor Tissue-Based Molecular Assays for Prostate Cancer .......................................................... 6 Hematologic Cancer and Myeloproliferative and Myelodysplastic Disease ............................................ 7 Occult Neoplasms ....................................................... 8 Solid Tumor Cancers .................................................. 9 Other Tumor Profile Testing ....................................... 9 General Background .................................................... 9 General Criteria for Somatic Mutation Genetic Testing ........................................................................ 9 Tumor Profile/Gene Expression Classifier Testing -

BRCA1/2 Mutation Detection in the Tumor Tissue from Selected Polish Patients with Breast Cancer Using Next Generation Sequencing
G C A T T A C G G C A T genes Article BRCA1/2 Mutation Detection in the Tumor Tissue from Selected Polish Patients with Breast Cancer Using Next Generation Sequencing Ewelina Szczerba 1,2, Katarzyna Kami ´nska 1, Tomasz Mierzwa 3, Marcin Misiek 4, Janusz Kowalewski 2 and Marzena Anna Lewandowska 1,2,* 1 The F. Lukaszczyk Oncology Center, Molecular Oncology and Genetics Department, Innovative Medical Forum, 85-796 Bydgoszcz, Poland; [email protected] (E.S.); [email protected] (K.K.) 2 Department of Thoracic Surgery and Tumors, Ludwik Rydygier Collegium Medicum in Bydgoszcz, Nicolaus Copernicus University, 85-067 Torun, Poland; [email protected] 3 The F. Lukaszczyk Oncology Center, Department of Prevention and Health Promotion, 85-796 Bydgoszcz, Poland; [email protected] 4 Swi˛etokrzyskieCancer´ Center, Clinical Department of Gynaecological Oncology, 25-734 Kielce, Poland; [email protected] * Correspondence: [email protected] Abstract: (1) Background: Although, in the mutated BRCA detected in the Polish population of patients with breast cancer, there is a large percentage of recurrent pathogenic variants, an increasing need for the assessment of rare BRCA1/2 variants using NGS can be observed. (2) Methods: We studied 75 selected patients with breast cancer (negative for the presence of 5 mutations tested in the Polish population in the prophylactic National Cancer Control Program). DNA extracted from Citation: Szczerba, E.; Kami´nska,K.; the cancer tissue of these patients was used to prepare a library and to sequence all coding regions Mierzwa, T.; Misiek, M.; Kowalewski, of the BRCA1/2 genes. -

Molecular Effects of Isoflavone Supplementation Human Intervention Studies and Quantitative Models for Risk Assessment
Molecular effects of isoflavone supplementation Human intervention studies and quantitative models for risk assessment Vera van der Velpen Thesis committee Promotors Prof. Dr Pieter van ‘t Veer Professor of Nutritional Epidemiology Wageningen University Prof. Dr Evert G. Schouten Emeritus Professor of Epidemiology and Prevention Wageningen University Co-promotors Dr Anouk Geelen Assistant professor, Division of Human Nutrition Wageningen University Dr Lydia A. Afman Assistant professor, Division of Human Nutrition Wageningen University Other members Prof. Dr Jaap Keijer, Wageningen University Dr Hubert P.J.M. Noteborn, Netherlands Food en Consumer Product Safety Authority Prof. Dr Yvonne T. van der Schouw, UMC Utrecht Dr Wendy L. Hall, King’s College London This research was conducted under the auspices of the Graduate School VLAG (Advanced studies in Food Technology, Agrobiotechnology, Nutrition and Health Sciences). Molecular effects of isoflavone supplementation Human intervention studies and quantitative models for risk assessment Vera van der Velpen Thesis submitted in fulfilment of the requirements for the degree of doctor at Wageningen University by the authority of the Rector Magnificus Prof. Dr M.J. Kropff, in the presence of the Thesis Committee appointed by the Academic Board to be defended in public on Friday 20 June 2014 at 13.30 p.m. in the Aula. Vera van der Velpen Molecular effects of isoflavone supplementation: Human intervention studies and quantitative models for risk assessment 154 pages PhD thesis, Wageningen University, Wageningen, NL (2014) With references, with summaries in Dutch and English ISBN: 978-94-6173-952-0 ABSTRact Background: Risk assessment can potentially be improved by closely linked experiments in the disciplines of epidemiology and toxicology. -

Whole Genome Sequencing in Oncology: Using Scenario Drafting to Explore Future Developments Michiel Van De Ven1†, Martijn J
Ven et al. BMC Cancer (2021) 21:488 https://doi.org/10.1186/s12885-021-08214-8 RESEARCH ARTICLE Open Access Whole genome sequencing in oncology: using scenario drafting to explore future developments Michiel van de Ven1†, Martijn J. H. G. Simons2,3†, Hendrik Koffijberg1, Manuela A. Joore2,3, Maarten J. IJzerman1,4,5, Valesca P. Retèl1,6*† and Wim H. van Harten1,6,7† Abstract Background: In oncology, Whole Genome Sequencing (WGS) is not yet widely implemented due to uncertainties such as the required infrastructure and expertise, costs and reimbursements, and unknown pan-cancer clinical utility. Therefore, this study aimed to investigate possible future developments facilitating or impeding the use of WGS as a molecular diagnostic in oncology through scenario drafting. Methods: A four-step process was adopted for scenario drafting. First, the literature was searched for barriers and facilitators related to the implementation of WGS. Second, they were prioritized by international experts, and third, combined into coherent scenarios. Fourth, the scenarios were implemented in an online survey and their likelihood of taking place within 5 years was elicited from another group of experts. Based on the minimum, maximum, and most likely (mode) parameters, individual Program Evaluation and Review Technique (PERT) probability density functions were determined. Subsequently, individual opinions were aggregated by performing unweighted linear pooling, from which summary statistics were extracted and reported. Results: Sixty-two unique barriers and facilitators were extracted from 70 articles. Price, clinical utility, and turnaround time of WGS were ranked as the most important aspects. Nine scenarios were developed and scored on likelihood by 18 experts. -

The Era of Transformative Molecular Oncology
LURIE CANCER CENTER ONCOSET SYMPOSIUM The Era of Transformative Molecular Oncology Robert H. Lurie Comprehensive Cancer Center of Northwestern University Chairs: Leonidas Platanias, MD, PhD Massimo Cristofanilli, MD Date: March 19, 2021 VIRTUAL EVENT - 9:00 A.M. - 4:30 P.M. CENTRAL TIME | MATERIALS AVAILABLE THROUGH APRIL 2 Lurie Cancer Center OncoSET Symposium: The Era of Transformative Molecular Oncology OPENING REMARKS 9:00 a.m. Welcome Leonidas Platanias, MD, PhD and Massimo Cristofanilli, MD Lurie Cancer Center KEYNOTE ADDRESS 9:05 a.m. The Evolution of Molecular Oncology: Actionable, Druggable, Undruggable? David Hong, MD The University of Texas MD Anderson Cancer Center SESSION 1: Molecularly Targeted Therapies and Immune Therapy Selection Co-Chairs: Amir Behdad, MD and Young Chae, MD, MPH, MBA, Lurie Cancer Center 9:45 a.m. The Central Role of Tumor and Germline DNA Alterations in Cancer Treatment Pamela Munster, MD UCSF Helen Diller Family Comprehensive Cancer Center 10:15 a.m. The Implementation of Precision Medicine in an Academic Center: It Takes a Village Milan Radovich, PhD Indiana University Simon Cancer Center 10:50 a.m. Panel Discussion 11:10 a.m. Break & Exhibits SESSION 2: Evolving Role of Liquid Biopsy: Detection, Monitoring and Early Detection Co-Chairs: Massimo Cristofanilli, MD and Dai Horiuchi, PhD, Lurie Cancer Center 11:40 p.m. Liquid Biopsy in Cancer Diagnostics: Fulfilling the Dream of Earlier Detection? Nickolas Papadopoulos, PhD Johns Hopkins Medicine 12:10 p.m. Precision Medicine Delivery in Metastatic Prostate Cancer: Foresight “2020” Manish Kohli, MD Huntsman Cancer Institute - University of Utah Health 12:50 p.m. -
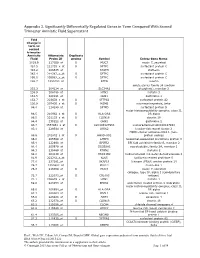
Appendix 2. Significantly Differentially Regulated Genes in Term Compared with Second Trimester Amniotic Fluid Supernatant
Appendix 2. Significantly Differentially Regulated Genes in Term Compared With Second Trimester Amniotic Fluid Supernatant Fold Change in term vs second trimester Amniotic Affymetrix Duplicate Fluid Probe ID probes Symbol Entrez Gene Name 1019.9 217059_at D MUC7 mucin 7, secreted 424.5 211735_x_at D SFTPC surfactant protein C 416.2 206835_at STATH statherin 363.4 214387_x_at D SFTPC surfactant protein C 295.5 205982_x_at D SFTPC surfactant protein C 288.7 1553454_at RPTN repetin solute carrier family 34 (sodium 251.3 204124_at SLC34A2 phosphate), member 2 238.9 206786_at HTN3 histatin 3 161.5 220191_at GKN1 gastrokine 1 152.7 223678_s_at D SFTPA2 surfactant protein A2 130.9 207430_s_at D MSMB microseminoprotein, beta- 99.0 214199_at SFTPD surfactant protein D major histocompatibility complex, class II, 96.5 210982_s_at D HLA-DRA DR alpha 96.5 221133_s_at D CLDN18 claudin 18 94.4 238222_at GKN2 gastrokine 2 93.7 1557961_s_at D LOC100127983 uncharacterized LOC100127983 93.1 229584_at LRRK2 leucine-rich repeat kinase 2 HOXD cluster antisense RNA 1 (non- 88.6 242042_s_at D HOXD-AS1 protein coding) 86.0 205569_at LAMP3 lysosomal-associated membrane protein 3 85.4 232698_at BPIFB2 BPI fold containing family B, member 2 84.4 205979_at SCGB2A1 secretoglobin, family 2A, member 1 84.3 230469_at RTKN2 rhotekin 2 82.2 204130_at HSD11B2 hydroxysteroid (11-beta) dehydrogenase 2 81.9 222242_s_at KLK5 kallikrein-related peptidase 5 77.0 237281_at AKAP14 A kinase (PRKA) anchor protein 14 76.7 1553602_at MUCL1 mucin-like 1 76.3 216359_at D MUC7 mucin 7, -

Cannabinoid Modulation of Cisplatin Induced Neuropathy
University of Mississippi eGrove Electronic Theses and Dissertations Graduate School 2015 Cannabinoid Modulation Of Cisplatin Induced Neuropathy Hannah Marie Harris University of Mississippi Follow this and additional works at: https://egrove.olemiss.edu/etd Part of the Biological Psychology Commons Recommended Citation Harris, Hannah Marie, "Cannabinoid Modulation Of Cisplatin Induced Neuropathy" (2015). Electronic Theses and Dissertations. 1142. https://egrove.olemiss.edu/etd/1142 This Thesis is brought to you for free and open access by the Graduate School at eGrove. It has been accepted for inclusion in Electronic Theses and Dissertations by an authorized administrator of eGrove. For more information, please contact [email protected]. CANNABINOID MODULATION OF CISPLATIN INDUCED NEUROPATHY A Thesis presented in partial fulfillment of requirements for the degree of Master of Arts in the Department of Psychology The University of Mississippi by Hannah Marie Harris December 2015 Copyright Hannah Marie Harris 2015 ALL RIGHTS RESERVED ABSTRACT Endocannabinoid modulation of cancer-related pain is well-documented. Sativex, a cannabinoid extract with a 1:1 ratio of tetrahydrocannabinol (THC) and cannabidiol (CBD) has been shown to alleviate neuropathic pain associated with chemotherapy. This research examined whether THC or CBD alone is effective in attenuating or preventing tactile allodynia associated with cisplatin-administration. Mice (C57BL/6) were given eight doses of 2.3 mg/kg cisplatin or saline solution IP every second day to induce tactile allodynia (Ringers on alternate days). Tactile responses to hind-paws were quantified in g of force using an electric von Frey (eVF) prior to (baseline) and after the cisplatin administration protocol. Separate groups of mice were then given vehicle, 100 mg/kg gabapentin, 2 mg/kg THC or 2 mg/kg CBD IP and tested 60 m later on eVF. -

Human Induced Pluripotent Stem Cell–Derived Podocytes Mature Into Vascularized Glomeruli Upon Experimental Transplantation
BASIC RESEARCH www.jasn.org Human Induced Pluripotent Stem Cell–Derived Podocytes Mature into Vascularized Glomeruli upon Experimental Transplantation † Sazia Sharmin,* Atsuhiro Taguchi,* Yusuke Kaku,* Yasuhiro Yoshimura,* Tomoko Ohmori,* ‡ † ‡ Tetsushi Sakuma, Masashi Mukoyama, Takashi Yamamoto, Hidetake Kurihara,§ and | Ryuichi Nishinakamura* *Department of Kidney Development, Institute of Molecular Embryology and Genetics, and †Department of Nephrology, Faculty of Life Sciences, Kumamoto University, Kumamoto, Japan; ‡Department of Mathematical and Life Sciences, Graduate School of Science, Hiroshima University, Hiroshima, Japan; §Division of Anatomy, Juntendo University School of Medicine, Tokyo, Japan; and |Japan Science and Technology Agency, CREST, Kumamoto, Japan ABSTRACT Glomerular podocytes express proteins, such as nephrin, that constitute the slit diaphragm, thereby contributing to the filtration process in the kidney. Glomerular development has been analyzed mainly in mice, whereas analysis of human kidney development has been minimal because of limited access to embryonic kidneys. We previously reported the induction of three-dimensional primordial glomeruli from human induced pluripotent stem (iPS) cells. Here, using transcription activator–like effector nuclease-mediated homologous recombination, we generated human iPS cell lines that express green fluorescent protein (GFP) in the NPHS1 locus, which encodes nephrin, and we show that GFP expression facilitated accurate visualization of nephrin-positive podocyte formation in -

Transcriptional Recapitulation and Subversion Of
Open Access Research2007KaiseretVolume al. 8, Issue 7, Article R131 Transcriptional recapitulation and subversion of embryonic colon comment development by mouse colon tumor models and human colon cancer Sergio Kaiser¤*, Young-Kyu Park¤†, Jeffrey L Franklin†, Richard B Halberg‡, Ming Yu§, Walter J Jessen*, Johannes Freudenberg*, Xiaodi Chen‡, Kevin Haigis¶, Anil G Jegga*, Sue Kong*, Bhuvaneswari Sakthivel*, Huan Xu*, Timothy Reichling¥, Mohammad Azhar#, Gregory P Boivin**, reviews Reade B Roberts§, Anika C Bissahoyo§, Fausto Gonzales††, Greg C Bloom††, Steven Eschrich††, Scott L Carter‡‡, Jeremy E Aronow*, John Kleimeyer*, Michael Kleimeyer*, Vivek Ramaswamy*, Stephen H Settle†, Braden Boone†, Shawn Levy†, Jonathan M Graff§§, Thomas Doetschman#, Joanna Groden¥, William F Dove‡, David W Threadgill§, Timothy J Yeatman††, reports Robert J Coffey Jr† and Bruce J Aronow* Addresses: *Biomedical Informatics, Cincinnati Children's Hospital Medical Center, Cincinnati, OH 45229, USA. †Departments of Medicine, and Cell and Developmental Biology, Vanderbilt University and Department of Veterans Affairs Medical Center, Nashville, TN 37232, USA. ‡McArdle Laboratory for Cancer Research, University of Wisconsin, Madison, WI 53706, USA. §Department of Genetics and Lineberger Cancer Center, University of North Carolina, Chapel Hill, NC 27599, USA. ¶Molecular Pathology Unit and Center for Cancer Research, Massachusetts deposited research General Hospital, Charlestown, MA 02129, USA. ¥Division of Human Cancer Genetics, The Ohio State University College of Medicine, Columbus, Ohio 43210-2207, USA. #Institute for Collaborative BioResearch, University of Arizona, Tucson, AZ 85721-0036, USA. **University of Cincinnati, Department of Pathology and Laboratory Medicine, Cincinnati, OH 45267, USA. ††H Lee Moffitt Cancer Center and Research Institute, Tampa, FL 33612, USA. ‡‡Children's Hospital Informatics Program at the Harvard-MIT Division of Health Sciences and Technology (CHIP@HST), Harvard Medical School, Boston, Massachusetts 02115, USA. -

CURRICULUM VITAE Mark R. Kelley, Ph.D. Betty and Earl
Mark R. Kelley, Ph.D. CURRICULUM VITAE Mark R. Kelley, Ph.D. Betty and Earl Herr Chair in Pediatric Oncology Research and Professor, Departments of Biochemistry and Molecular Biology and Pharmacology and Toxicology Associate Director, Basic Science Research, IU Simon Cancer Center Director, Program in Molecular Oncology and Experimental Therapeutics Bantz-Petrino Translating Research into Practice Scholar Glenn W. Irwin, Jr., M.D. Research Scholar Associate Director, IU Pancreatic Cancer Signature Center Indiana University School of Medicine 1044 W. Walnut, Cancer Research Institute, R4-Rm 302 Indianapolis, Indiana 46202 Office: 317-274-2755 FAX: 317-274-8046 Email: [email protected] Chief Scientific Founder and Chief Scientific Officer Apexian Pharmaceuticals 20 N. Meridian, Suite 801 Indianapolis, IN 46204 PERSONAL INFORMATION Home address: 4557 Winterspring Crescent Marital Status: Married, 2 children Zionsville, IN 46077 (317) 873-5778 Citizenship: United States EDUCATION B.A. Zoology, 1975 - 1979 DePauw University, Greencastle, IN M.S. Zoology, 1979 – 1981 Louisiana State University, Baton Rouge, LA Director: William R. Lee, Ph.D. Ph.D. Genetics, 1981 - 1984 Louisiana State University, Baton Rouge, LA Director: William R. Lee, Ph.D. Postdoctorate, 1984 – 1987 The Rockefeller University, New York, NY Director: Michael W. Young, Ph.D. 2017 Nobel Prize Winner in Physiology or Medicine HONORS Malpas Trust Scholarship 1975-1979 1 Mark R. Kelley, Ph.D. McClure Research Fellowship 1979 National Sigma XI Research Grant 1982-1983 American Cancer Society Postdoctoral Fellowship 1984-1987 Schweppe Career Development Award 1989-1992 Jonathan and Jennifer Simmons Professor of Pediatrics 2001-2008 Betty and Earl Herr Chair in Pediatric Oncology Research 2008 – Present Innovation to Enterprise Commercialization Award, IUSM 2015 Bantz-Petronio Translating Research Into Practice Award 2017 Education Board Member, American Health Council 2017 Glenn W. -

ABBOTT MOLECULAR ONCOLOGY and GENETICS 2015-2016 Product Catalog
DESCRIPTOR, 9/12, ALL CAPS ABBOTT MOLECULAR ONCOLOGY AND GENETICS 2015-2016 Product Catalog Area for placed imagery Only use imagery that is relevant to the communication CHOOSE TRANSFORMATION See where it will take you at AbbottMolecular.com 2 Please note some products may not be for sale in all markets. Contact your local representative for availability. ASR (Analyte Specific Reagent) Analytical and performance characteristics are not established CE (CE Marked) Conformité Européenne GPR (General Purpose Reagent) For Laboratory use RUO (Research Use Only) Not for use in diagnostic procedures All products manufactured and/or distributed by Abbott Molecular should be used in accordance with the products’ labeled intended use. Products labeled “Research Use Only” should be used for research applications, and are not for use in diagnostic procedures. CEP, LSI, AneuVysion, MultiVysion, PathVysion and Vysis are registered trademarks of Vysis, Inc., AutoVysion, ProbeChek, SpectrumAqua, SpectrumBlue, SpectrumGreen, SpectrumGold, SpectrumOrange, SpectrumRed, TelVysion, ToTelVysion, UroVysion and VP 2000 are trademarks of Abbott Molecular in various jurisdictions. All other trademarks are the property of their respective owners. Please note some products may not be for sale in all markets. Contact your local representative for availability. 3 Abbott Molecular is Transforming Laboratory Partnerships and Productivity—Today and into the Future As a leader in molecular Our commitment to exploring new clinical frontiers is evident in the development and delivery of innovative diagnostics, Abbott is committed systems and assay solutions that aid physicians in the diagnosis of disease, selection of therapies and monitoring to providing solution-oriented of disease. offerings built on FISH and PCR.